Abstract
Objective
To determine interleukin (IL)-17 concentrations in serum and synovial fluid from patients with knee osteoarthritis, and evaluate their correlation with disease severity.
Methods
Serum and synovial fluid were collected from patients with primary knee osteoarthritis; age- and sex-matched healthy control subjects provided serum samples. This study was conducted retrospectively. IL-17 was quantified by enzyme-linked immunosorbent assay. Osteoarthritis severity and grade were assessed using the Lequesne index and Kellgren and Lawrence (KL) grading system, respectively.
Results
Serum IL-17 concentrations were significantly higher in patients (n = 98) than in controls (n = 50). In the patient group, the synovial fluid IL-17 concentration increased significantly with KL grade and was significantly positively correlated with Lequesne index (r = 0.6232).
Conclusions
The synovial fluid IL-17 concentration could represent a useful biochemical marker to reflect knee osteoarthritis severity and progression.
Introduction
Osteoarthritis is a chronic, degenerative joint disease characterized by the progressive destruction of articular cartilage, joint-space narrowing, subchondral bone remodelling, joint marginal osteophyte formation and synovitis. 1 Osteoarthritis causes joint pain, stiffness, swelling and reduced range-of-motion in middle-aged and older people, and has a serious impact on health-related quality-of-life. 2 Osteoarthritis can be diagnosed by the presence of joint irregularities and deformities on X-radiographic images, with the grade of joint degeneration being reflective of disease severity. 3 Noninvasive biochemical analyses have been developed to evaluate disease progress and severity, and provide a nonradiographical alternative for the early detection of osteoarthritis.4–6 Although the aetiology and pathophysiology of osteoarthritis are both poorly understood, it is believed that secreted inflammatory molecules (such as proinflammatory cytokines) are among the critical mediators of the disturbed processes implicated in osteoarthritis pathophysiology. 7 Proinflammatory cytokines have been reported to contribute to osteoarthritis pathogenesis by increasing cartilage degradation and inducing hyperalgesia via a number of direct and indirect actions. 8
The proinflammatory cytokine interleukin (IL)-17 is implicated in both the induction of local inflammation and the joint destruction that characterize the synovial tissue of rheumatoid arthritis.9,10 IL-17 is present at increased concentrations in serum, synovial fluid and synovium samples from patients with rheumatoid arthritis, 11 and has been shown to induce and perpetuate chronic inflammation, cartilage damage and bone erosion. 12 Osteoarthritis shares several characteristics with rheumatoid arthritis, including joint destruction and synovitis. 13 In addition, IL-17 has been shown to be present in synovial fluid from patients with osteoarthritis, 14 but the relationship between serum and synovial fluid IL-17 concentrations and severity of primary knee osteoarthritis remains to be clarified.
The aim of the present retrospective study was to investigate IL-17 concentrations in serum and synovial fluid samples from patients with primary knee osteoarthritis, and assess their possible relationship with disease severity.
Patients and methods
Study population
The retrospective study included serum and synovial fluid samples from Han Chinese patients with primary knee osteoarthritis, who attended the Department of Orthopaedic Surgery, Zhongnan Hospital, Wuhan, China for diagnosis and treatment, between 1 January 2008 and 31 December 2012. Diagnosis of osteoarthritis was performed according to criteria of the American College of Rheumatology. 14 Exclusion criteria were: (i) symptoms suggestive of any other chronic inflammatory disease; (ii) diabetes; (iii) history of corticosteroid treatment; (iv) any other form of arthritis; (v) cancer; (vi) family history of osteoarthritis.
Serum samples from age- and sex-matched healthy subjects were used as controls; these samples had been provided by members of the local population and medical staff of Zhongnan Hospital who were attending the hospital for routine medical checks. The control subjects were ethnically matched and had no symptoms suggestive of gout, rheumatoid arthritis, trauma, diabetes or any orthopaedic disease.
The study protocol was approved by the Ethics Committee of Wuhan University Zhongnan Hospital, Wuhan, China, and all participants provided written informed consent.
IL-17 quantification
Whole blood (5 ml) was collected in serum separator tubes, allowed to clot for 30 min and centrifuged for 15 min at 1000
Grading and assessment of osteoarthritis
Osteoarthritis was graded based on weight-bearing anteroposterior X-radiographs of the affected knee, according to the Kellgren and Lawrence (KL) grading system3 as follows: grade 0, no radiological changes; grade 1, doubtful narrowing of joint space and possible osteophytic lipping; grade 2, definite osteophytes and possible narrowing of joint space; grade 3, moderate multiple osteophytes, definite narrowing of joint space, some sclerosis and possible deformity of bone contours; grade 4, large osteophytes, marked narrowing of joint space, severe sclerosis and definite deformity of bone contours. 14 For the purposes of this study, patients were required to have KL grade ≥2 in at least one knee. Disease severity was assessed using the standardized Lequesne algofunctional index, which evaluates pain/discomfort, maximum distance walked and activities of daily living. 15
Statistical analyses
Continuous variables were presented as mean ± SD, and compared using two-tailed Student’s t-test or one-way analysis of variance. Relationships between variables were examined using nonparametric Spearman correlation coefficients. Statistical analyses were performed with SPSS® version 15.0 (SPSS Inc., Chicago, USA) for Windows®. P-values < 0.05 were considered statistically significant.
Results
Baseline demographic and clinical characteristics of Han Chinese patients with primary knee osteoarthritis and matched healthy control subjects included in a study investigating the association between IL-17 and severity of knee osteoarthritis.

Data presented as mean ± SD or n.
KL, Kellgren and Lawrence grading system; 3 BMI, body mass index.
No statistically significant between-group differences (P ≥ 0.05; Student’s t-test or one-way analysis of variance).
Inkerleukin (IL)-17 concentrations in serum samples from healthy control subjects, and serum and synovial fluid samples from Han Chinese patients with primary knee osteoarthritis.

Data presented as mean ± SD.
KL, Kellgren and Lawrence grading system; 3 NT, not tested.
Serum IL-17 concentrations: aP < 0.05 vs control group, bP < 0.05 vs KL grade 2, cP < 0.05 vs KL grade 3; Synovial fluid IL-17 concentrations: dP < 0.05 vs KL grade 2, eP < 0.05 vs KL grade 3; Student’s t-test or one-way analysis of variance.
Synovial fluid IL-17 concentrations were significantly higher in patients with grade 3 or 4 osteoarthritis than in those with grade 2, and significantly higher in patients with grade 4 than those with grade 3 disease (P < 0.05 for each comparison; Table 2).
Synovial fluid IL-17 concentrations were significantly positively correlated with Lequesne index (r = 0.6232, P < 0.05; Figure 1). There was no correlation between serum IL-17 concentrations and Lequesne index, however.
Correlation between interleukin (IL)-17 concentration in synovial fluid and Lequesne index of disease severity
15
in Han Chinese patients with primary knee osteoarthritis (n = 98).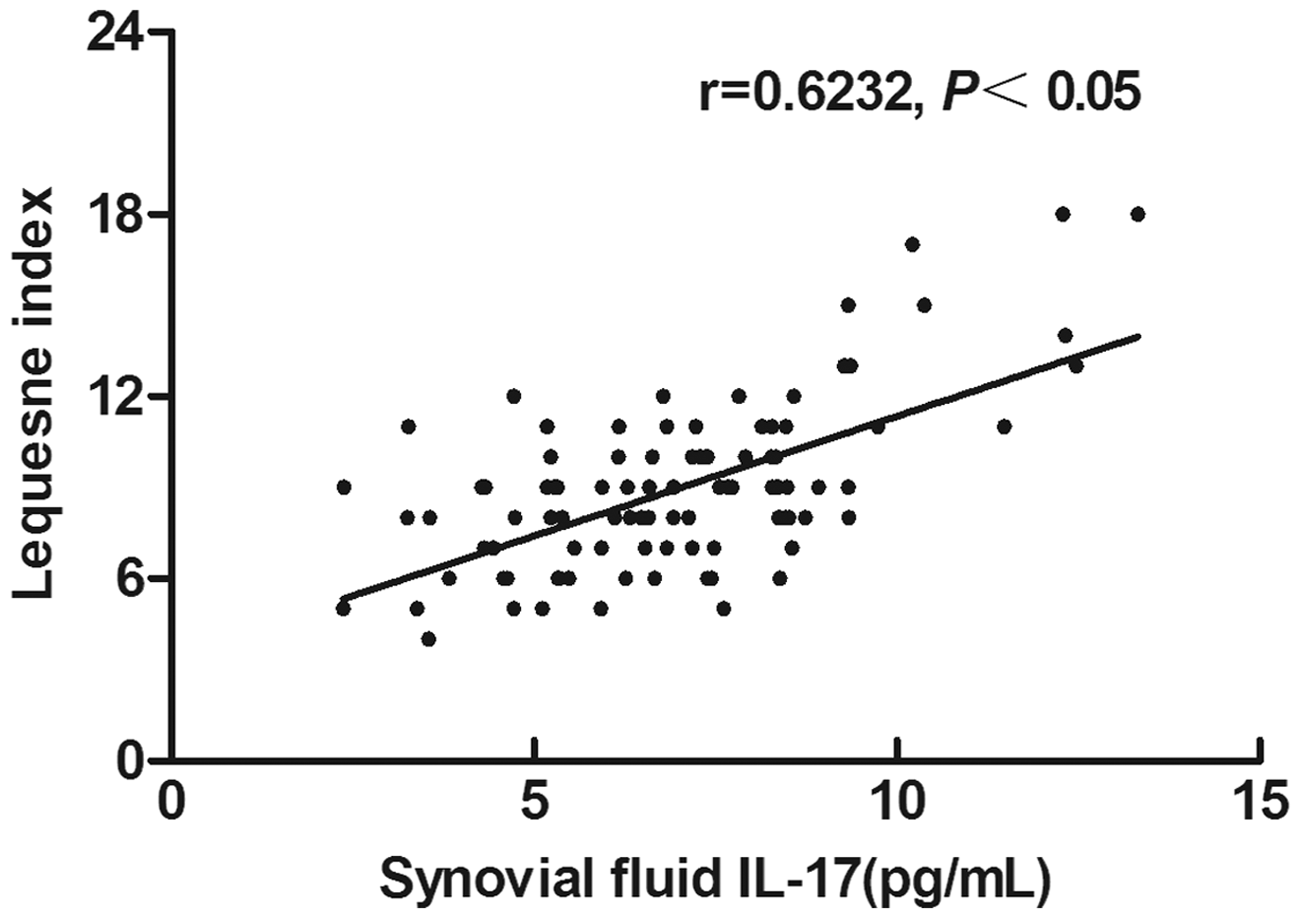
Discussion
The current study demonstrated that IL-17 was detectable in serum and knee synovial fluid samples from patients with knee osteoarthritis, and found a positive association between the severity of knee osteoarthritis (KL grade) and the IL-17 concentration. In addition, synovial fluid IL-17 concentrations were positively correlated with Lequesne index, 15 suggesting that IL-17 may play an important role in the pathogenesis of osteoarthritis.
The present data are in accordance with others, who found that increased synovial fluid IL-17 concentrations were correlated with arthritis disease activity and matrix metalloproteinase expression in synovial fibroblasts, suggesting a role for this cytokine in cartilage destruction.16,17 In addition, IL-17 has been shown to induce the release of chemokines (such as IL-1β and tumour necrosis factor [TNF]-α) by chondrocytes and synovial fibroblasts, contributing to cartilage breakdown and synovial infiltration in osteoarthritis. 13 Others demonstrated that IL-17 inhibited proteoglycan synthesis in rat cartilage, and increased nitrogen monoxide production. 18 Although the aetiology and pathogenesis of osteoarthritis are poorly understood, it is possible that IL-17 may be among the critical mediators of the disturbed processes implicated in osteoarthritis pathophysiology.
Activated memory CD4+ T-cells are the primary secretors of IL-17, which then binds to specific receptors that are expressed by virtually all cells and tissues. 9 Increasing evidence suggests a pathogenic role for IL-17 in the structural damage of rheumatoid arthritis, 19 promoting cartilage and bone destruction by acting as potent inductor of matrix metalloproteinase and receptor activator of nuclear factor κB ligand expression in rheumatoid synoviocytes and osteoblasts.10,20,21 In addition, data suggest that IL-17 may be important in recruiting monocytes into the joints of patients with rheumatoid arthritis, and in promoting the secretion of inflammatory cytokines and chemokines from rheumatoid arthritis synovial tissue. 10 There is evidence to suggest that IL-17 plays a key role in the synergistic or additive effects of TNF-α and IL-1 in rheumatoid arthritis.22,23 The disease process of osteoarthritis begins with cartilage degradation, which triggers the inflammatory cascade, resulting in similar symptoms to rheumatoid arthritis. Although rheumatoid arthritis and osteoarthritis have different aetiologies, the diseases share several common characteristics including destruction of articular cartilage, joint space narrowing and synovitis. 24
The concentration of IL-17 in synovial fluid, but not serum, was found to correlate significantly with Lequesne index (an objective assessment of osteoarthritis severity) in the current study. The increased IL-17 concentrations in synovial fluid may be attributable to the increased local and systemic production of IL-17 by synovial cells and chondrocytes in local and extra-articular tissues. Inflamed synovial tissue and stimulated chondrocytes may stimulate increased IL-17 production, which could then contribute to the initiation or worsening of synovial inflammation, leading to a vicious cycle. 25
This is a small article and the study design may be simple. Nevertheless, in this article we have attempted to express the correlation between knee osteoarthritis severity and IL-17 concentration, and we acknowledge that further studies are necessary to validate these findings. Such studies might investigate, for example, random samples taken from patients from multiple centres, mRNA expression of IL-17 in synovial fluid mononuclear cells according to KL grade, relationship between inflammation and osteoarthritis, as well as studying the differences between osteoarthritis and rheumatoid arthritis. In addition, we acknowledge that ethical concerns meant that it was not possible to obtain synovial fluid from the knee joints of control participants, which may have led to a potential bias.
In conclusion, the present study findings demonstrate a positive correlation between disease severity (Lequesne index) and IL-17 concentrations in synovial fluid from the affected joint of patients with primary knee osteoarthritis. Synovial fluid IL-17 could represent a useful biochemical marker to reflect knee osteoarthritis severity and progression. In addition, blocking IL-17/IL-17 receptor signalling may be a novel therapeutic approach to the control of osteoarthritis symptoms and the prevention of joint destruction.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research was supported by grants from the Natural Science Foundation of China (81201401 and 30973539) and the Fundamental Research Funds for the Central Universities (303274010).
