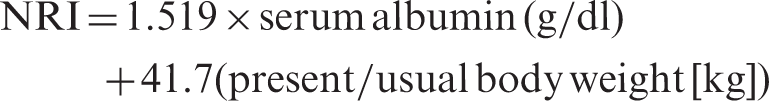Abstract
Objective
To investigate the effects of Ramadan fasting on serum concentrations of immunoglobulin (Ig)G and IgM, and salivary IgA concentrations.
Methods
Blood and saliva samples were collected one week before and during the last week of Ramadan from healthy male volunteers. Albumin, total lymphocyte count, electrolytes, and IgG and IgM concentrations were determined in serum; salivary IgA concentrations were measured. Anthropometric measurements were also recorded.
Results
Samples were collected from 35 subjects (mean age 35.86 years, range 20–59 years). Weight, body mass index, albumin levels and the nutritional risk index decreased significantly during Ramadan fasting compared with before fasting. In addition, Na+ and Cl− electrolyte levels were significantly decreased during Ramadan. Serum IgG concentrations decreased significantly during Ramadan compared with before fasting, but were still within the normal range. Salivary IgA concentrations also decreased significantly, whereas serum IgM levels did not change. Lymphocyte numbers increased significantly, but there was no correlation between Ig levels and lymphocyte count.
Conclusion
Ramadan fasting did not result in severe immunological disturbances.
Keywords
Introduction
Muslims fast from before sunrise to sunset each day during the month of Ramadan, which is the ninth month of the lunar calendar and lasts between 29 and 30 days; each year Ramadan starts 11 days earlier than the year before. The duration of fasting varies between 11 h and 18 h. Fasting during Ramadan is partial: abstention from food and fluid takes place only from sunrise to sunset; intake of both is allowed for the remainder of the day. The obligation to eat and drink only after sunset and the decrease in meal frequency leads to a definite change in daily rhythms during Ramadan, due to altered rest, activity and eating schedules.1–3
Several studies have demonstrated the effects of religious fasting on physiology and disease pathology.4–8 Although limiting the total food intake could potentially weaken the immune system, 9 it is usual for an individual who is fasting during Ramadan to have a balanced eating, resting and sleeping schedule. Together, this should help to maintain adequate immune function. It has been suggested that fasting differentially modulates the immune system. During fasting in animals, immunoglobulin (Ig)A expression in the intestinal mucosa is increased. 10 In addition, catabolism increases because of cellular breakdown, leading to elevated macrophage activity.10,11 Although B cell-mediated immunity increases during fasting, 12 the overall effects on cell-mediated immunity have not been elucidated. Fasting also contributes to an increase in neutrophil (bactericidal) activity and promotes both monocyte killing and natural killer-cell activity. 13 However, little is known regarding the effects of fasting during Ramadan on immunity.
Many infections, including upper respiratory tract infections (URTIs), are initiated at mucosal surfaces protected by antimicrobial proteins, of which secretory IgA is the most abundant.14,15 Since IgA predominates in upper airway secretions, it would appear that its role is important in initial host defences, particularly against viral infection, 16 and IgA present in saliva is an excellent indicator of oral mucosal immune status.17–19 Salivary IgA provides an immunological barrier by neutralizing viral pathogens and preventing them from penetrating the body through the mucosal surfaces.20,21
The objective of the present study was to evaluate whether long-term (∼17 h) partial fasting during Ramadan affects salivary IgA and other B cell-mediated immune responses, as reflected in serum concentrations of IgG and IgM.
Subjects and methods
Subjects
Healthy male volunteers from the staff of the Taksim Training and Research Hospital, Istanbul, Turkey, who indicated that they were going to fast during Ramadan during July 2012 and August 2012 were recruited to the study. Women were excluded from the study since they are prohibited to fast during their menstrual cycle due to religious rules; as all study subjects were required to fast for ∼28 days, this precluded menstruating women. In addition, subjects with any acute or chronic diseases, or those who used medications during the study period, were excluded. The content of the subjects’ diets was similar before and during Ramadan.
The study protocol was approved by the Ethics Committee of the Taksim Training and Research Hospital, Istanbul, Turkey. All study participants provided verbal informed consent.
Subject assessment
All subjects were interviewed using a questionnaire to obtain data regarding age, drug use and medical history. Blood and saliva were collected one week before the beginning of Ramadan (nonfasting period) and during the final week of Ramadan (25th day, fasting period). Blood and saliva samples were taken after a 12-h overnight fast before Ramadan and 12-h after the last meal (eaten before sunrise) in the last week of Ramadan. Anthropometric measurements (height, weight) were performed at the same time as blood and saliva sampling.
At the end of Ramadan, all volunteers were asked whether they had suffered from any URTIs during Ramadan.
Nutritional parameters
Nutritional parameters were assessed using the body mass index (BMI) (weight in kg divided by the height in m2) and the nutritional risk index (NRI), which is calculated using the following equation:
Blood analyses
Blood was collected in both plain (5-ml sample) and ethylenediamine tetra-acetic acid (EDTA) tubes (2.5-ml sample). Serum was obtained from the blood in plain tubes by low-speed centrifugation at 1000 g for 15 min at room temperature; samples were immediately separated into aliquots and stored at −80°C until analysed. All serum samples were analysed in a single batch to avoid day-to-day laboratory variations. An automated analyser (Hitachi Modular P800, Roche, Basel, Switzerland) was used to measure serum albumin concentrations, to indicate protein reserves and electrolyte levels (Na+, Cl−), and to determine hydration status. In addition, concentrations of serum IgG and IgM were determined using a Behring Nephelometer BNII Analyser (Behring, Marburg, Germany).
The total lymphocyte count, which can indicate a decrease in immune defences, was measured in fresh EDTA blood samples using a Sysmex® XT-2000i analyser (Sysmex, Hyogo, Japan).
Saliva analysis
Unstimulated saliva was collected by expectoration into sterile 15-ml centrifuge tubes over a 5-min period at a uniform temperature of 33°C after overnight fasting, or 12 h after the last meal and after the mouth had been rinsed with distilled water. Saliva moves anteriorly in the mouth; therefore after initial swallowing, saliva was drained continuously from the lower lip via a funnel into a test tube. Immediately after collection, the saliva samples were centrifuged at 2500 g for 10 min at room temperature. Supernatants were removed and stored at −80°C until analysed. The concentration of salivary IgA was determined using a Behring Nephelometer™ BNII analyser.
Statistical analyses
Results were expressed as the mean ± SD. A paired t-test was used to compare the results in the two groups. Pearson’s correlation coefficient was used to analyse relationships between the variables, and the differences in the means between the variables before and during Ramadan. A p-value of <0.05 was considered to be statistically significant. All statistical analyses were performed using SPSS® software, version 10.0 (SPSS Inc., Chicago, IL, USA).
Results
Anthropometric parameters in healthy male volunteers before and during Ramadan fastin.

Data presented as mean ± SD.
Paired t-test.
Biochemical and haematological parameters in healthy male volunteers before and during Ramadan fastin.

Data presented as mean ± SD.
Paired t-test.
The Na+ and Cl− levels were significantly decreased during Ramadan compared with before fasting (p < 0.001 for both; Table 2), but were still within normal ranges (136–145 mEq/l for Na+ and 98–107 mEq/l for Cl−). There was a significant correlation between the two electrolytes (r = 0.889). There was also a significant correlation between the differences in Na+ and Cl– levels before and during Ramadan (r = 0.801). The total lymphocyte count was significantly increased during Ramadan compared with before fasting (p < 0.001; Table 2), but was still within the normal range (1000–4800 cells/mm3).
Changes in serum and salivary Ig concentrations during Ramadan are given in Table 3 and Figures 1–3. Salivary IgA (p = 0.038) and serum IgG (p = 0.001) concentrations were significantly decreased during Ramadan compared with before fasting (Table 3; Figures 1 and 2); however, there was no significant change in serum IgM levels (Table 3 and Figure 3). The decreased IgG concentration found during Ramadan was still within the normal range (884–1912 mg/dl). There were no significant correlations between Ig levels and the total lymphocyte count. There were also no significant correlations between Ig levels and the NRI or albumin concentration.
Salivary immunoglobulin (Ig)A levels (mg/dl) in healthy male volunteers before and during Ramadan fasting. The bold horizontal lines represent the median, the extremities of the boxes represent the 25th and 75th percentiles and the vertical lines represent the minimum–maximum values. Salivary IgA concentrations decreased significantly (p = 0.038) during Ramadan, compared with before fasting (Pearson’s correlation coefficient). Serum immunoglobulin (Ig) G levels (mg/dl) in healthy male volunteers before and during Ramadan fasting. The bold horizontal lines represent the median, the extremities of the boxes represent the 25th and 75th percentiles and the vertical lines represent the minimum and maximum values. IgG levels decreased significantly (p = 0.001) during Ramadan, compared with before fasting (Pearson’s correlation coefficient). Serum immunoglobulin (Ig) M levels (mg/dl) in healthy male volunteers before and during Ramadan fasting. The bold horizontal lines represent the median, the extremities of the boxes represent the 25th and 75th percentiles and the vertical lines represent the minimum and maximum values. No statistically significant differences were observed (p ≥ 0.05; Pearson’s correlation coefficient). Serum and salivary immunoglobulin (Ig) concentrations in healthy male volunteers before and during Ramadan fastin. Data presented as mean ± SD. Paired t-test. NS, no statistically significant between-group differences (p ≥ 0.05).



None of the study participants reported URTIs during the study period.
Discussion
During Ramadan, Muslims refrain from eating and drinking between sunrise and sunset, although they are permitted to eat during the remaining time periods. The Islamic Hijri calendar is a lunar calendar; therefore Ramadan occurs at different times during the seasonal year over a 33-year cycle. It has been established that a well-balanced diet is essential to maintain immune function.23,24 The purpose of the present study was to assess the effects of fasting during Ramadan on serum IgG and IgM and salivary IgA levels.
Ramadan fasting has been shown to modulate certain aspects of the immune system. 25 Although the immunoregulatory effects of low-caloric diets on various components of the immune system have been demonstrated, 26 the effects of Ramadan fasting on immune system function have not yet been adequately characterized. Al-Jewari et al. 27 examined the effects of Ramadan fasting on serum IgA, IgG and IgM levels in healthy subjects and patients with type 2 diabetes mellitus. They found that serum Ig levels were slightly decreased towards the end of Ramadan. In the present study, serum IgG levels significantly decreased during Ramadan compared with before the fasting period, but were still within the normal range, whereas there was no significant change in serum IgM levels. Ramadan is a partial and controlled fast; therefore, IgM-mediated acute immune responses may not be affected. The significant decline in IgG may have been due to immunomodulation. Moreover, salivary IgA concentrations also decreased significantly during Ramadan compared with before the fasting period. Temporary dietary regimens, such as fasting for several days, can have subtle effects on mucosal function and potentially on mucosal activity. 28 The results of the present study suggest that Ramadan fasting, which is controlled, partial and consecutive, has a cumulative negative effect on the level of salivary IgA.
The methodological care with which salivary samples were collected (in a fasted state at an approximately consistent time of day, depending on the time of the last meal) was one of the strengths of the present study. Since the factors that influence the concentration of salivary IgA have not always been controlled and standardized in published reports, this may partly explain the inconsistencies found in the literature.29–31 A circadian rhythm has been reported in serum IgG and IgM concentrations.32–34 In clinically healthy subjects, peak concentrations of IgG and IgM occur in the early to late afternoon.32–34 In the present study, the blood and saliva collection time was kept consistent to remove the effects of circadian rhythms.
Fluctuations in some haematological parameters during Ramadan have been reported. 35 El-Hazmi et al. 36 found that the lymphocyte count increased during Ramadan. In the present study, the number of lymphocytes in the peripheral blood increased but remained within the normal range. This elevation was accompanied by decreased levels of serum IgG. One possible explanation for this finding is that cellular immunity increases, whereas humoral immunity decreases, during Ramadan fasting. This needs to be confirmed by further research.
In a study of professional athletes, Neville et al. 37 examined the relationship between salivary IgA and URTIs. They reported that a significant decline in salivary IgA concentrations occurred during the 3 weeks before a URTI episode, with levels returning to baseline by 2 weeks after the URTI. These authors concluded that the decline in an individual’s relative salivary IgA concentration appeared to contribute to the risk of URTI, depending on the magnitude of the decrease, independent of the absolute salivary IgA level. 37 The time-lag between the decrease in salivary IgA concentration and the increased risk of URTI may, in part, explain the lack of infection in subjects who fasted during Ramadan in the present study despite the fall in salivary IgA.
Although significant decreases in albumin levels and NRI were seen during Ramadan in the present study, there were no significant correlations between Ig levels and the NRI or albumin concentrations. The NRI remained >100 during Ramadan, indicating that there was no malnourishment. Similar to other studies,23,38–41 a significant decrease in BMI was observed during Ramadan fasting. Although there were no restrictions on the types of food consumed, the time during which food intake was permitted was limited: this may explain the reduction in weight and BMI during Ramadan.
The effects of fluid restriction during fasting in Ramadan were assessed in the present study. Na+ and Cl− levels were significantly decreased (within normal ranges) during Ramadan, and there was a significant correlation between the two electrolytes. This decrease in serum electrolyte levels is likely to be due to the state of dehydration induced by Ramadan fasting.
There has been much discussion regarding the benefits of fasting in relation to health and immunity. 42 Fasting can be beneficial in the treatment of some allergic and inflammatory conditions, because the process of ketosis decreases the availability of the fatty acid, arachidonic acid, which tends to increase inflammation. 43 The present study focused specifically on whether Ramadan fasting altered Ig concentrations in the serum and saliva. Decreased concentrations of serum IgG and salivary IgA were seen during Ramadan compared with levels before the fasting period. Although the serum IgG concentration declined during Ramadan, it remained within the normal range; a reference range is not available for salivary IgA concentrations. It can be concluded that Ramadan fasting did not lead to severe immunological disturbances or have a detrimental effect on health. Further studies on larger and more varied groups should be performed, in order to confirm these outcomes.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.