Abstract
Objective:
This retrospective study investigated the predictive role of serum phosphorus concentration for acute renal failure (ARF), defined by the Risk Injury Failure Loss End-stage kidney disease (RIFLE) criteria, after living-donor liver transplantation (LDLT).
Methods:
Perioperative factors, including serum phosphorus concentrations, in LDLT recipients without pre-existing renal dysfunction were retrospectively analysed and compared between patients with or without post-LDLT ARF.
Results:
A total of 45 patients out of 350 (12.9%) met the RIFLE ARF criteria and experienced significantly higher postoperative mortality, longer intensive care unit stay and more frequent graft dysfunction than those patients without post-LDLT ARF. Multivariate logistic regression analyses showed that a serum phosphorus concentration ≥ 4.5 mg/dl on postoperative day 1 (relative risk [RR] 5.31; 95% confidence interval [CI] 2.56, 11.03), a preoperative model for end-stage liver disease score = 20 points (RR 4.17, 95% CI 2.04, 8.52), and packed red blood cell transfusion ≥ 10 units (RR 2.55, 95% CI 1.13, 5.88) were independent risk factors for post-LDLT ARF.
Conclusions:
Hyper -phosphataemia on postoperative day 1 could be an early and simple indicator of ARF occurrence after LDLT.
Keywords
Introduction
Acute kidney injury is one of the most common complications after liver transplantation, particularly in the early postoperative period. The reported incidence of acute kidney injury following orthotopic liver transplantation ranges between 42 and 95%, depending on the definition used.1–4 Acute kidney injury is frequently associated with a prolonged intensive care unit (ICU) or hospital stay, need for postoperative renal replacement therapy, infection and, ultimately, the reduction of graft and patient survival.5,6– 8 In addition to pre-existing renal dysfunction, many perioperative factors may impact on the occurrence of acute renal injury after liver transplantation; known risk factors include intraoperative caval cross-clamping with renal vein outflow obstruction, intra- and postoperative hypotension, high vasopressor requirements, large-volume transfusions and postoperative use of calcineurin inhibitors.9 – 12
Early prediction of acute kidney injury, using practical and reliable indicators, is clinically important for prompt intervention in order to prevent or retard its progression. 13 The serum creatinine concentration is a commonly used marker for renal injury but is known to be slow to respond and insensitive, requiring days to exhibit a change after acute injury. 14 Increases in the serum creatinine concentration are not apparent before renal function has declined by ≥ 50%, meaning that detection of subtle renal injury with this marker is almost impossible. 14 Studies have found that cystatin C, and plasma and urinary neutrophil gelatinase-associated lipocalin, are early markers of acute kidney injury after liver transplantation.14 – 17 The high cost of assays for these markers, however, prohibits their use in routine assessment for early renal impairment. An earlier predictor that is simple to measure and easily accessible in clinical practice is required.
Hypophosphataemia frequently develops after major liver resection.18,19 Although its pathogenesis remains poorly understood, research has suggested that circulatory phosphatonin concentrations increase markedly after hepatic surgery and are connected directly to augmented urinary loss of phosphate.20,21 Kidney injury can impair the metabolism of serum phosphate or phosphatonins, meaning that post-transplant phosphorus concentrations in liver transplant recipients could differ according to the development of acute kidney injury.
The present study investigated the postoperative changes in serum phosphorus concentrations and their relationship with newly developed acute renal failure (ARF), as defined by the Risk Injury Failure Loss End-stage kidney disease (RIFLE) criteria, 22 after living-donor liver transplantation (LDLT). In addition, the study examined the possibility that the serum phosphorus concentration in the immediate postoperative period could serve as a predictor of ARF occurrence after LDLT.
Patients and methods
Study Population
This retrospective study reviewed all medical records of adult patients (aged ≥ 18 years) who underwent LDLT between January 2005 and July 2011 at Seoul St Mary's Hospital, College of Medicine, The Catholic University of Korea, Seoul, Republic of Korea. Donor data and preoperative, intraoperative and postoperative recipient data were retrieved from the hospital's electronic medical record system. The Institutional Review Board of Seoul St Mary's Hospital approved the present study and waived the requirement for written consent from patients, because the study was based on a retrospective review of medical records. Patients with pre-existing renal dysfunction before liver transplantation (including renal replacement therapy support, hepatorenal syndrome, or serum creatinine concentration ≥ 1.5 mg/dl) were excluded from the study.
Patient Management
Living-donor liver transplants were performed using the donors' right hepatic lobes and the piggyback technique without venovenous bypass. In every case, portal vein anastomosis was followed by hepatic artery anastomosis and bile duct reconstruction. A temporary portocaval shunt was applied when high portal vein pressure was diagnosed. All donor liver grafts were prepared using a histidine– tryptophan–ketoglutarate solution. Under standard monitoring, anaesthesia was induced with 2.0 mg/kg propofol, 1 – 2 mg/kg fentanyl and 0.8 mg/kg rocuronium, and was maintained with 1.0 – 1.5 volume% isoflurane and 40% oxygen in air with or without continuous infusion of remifentanil. Muscle relaxation was achieved with an intermittent bolus of vecuronium or continuous infusion of 5 – 12 mg/kg per min atracurium. Intraoperative patient management was guided by the LDLT protocol of Seoul St Mary's Hospital. Packed red blood cells (PRBCs) were administered to maintain a haematocrit of 25 – 30%. Vasopressors were administered when mean arterial pressure was < 65 mmHg or decreased by > 20% of the original range, as determined by invasive haemodynamic monitoring. Patients received furosemide intravenously when oliguria continued despite adequate fluid resuscitation and vasopressor coverage; calcium chloride was given when serum calcium concentrations dropped to < 80% of the normal lower limit. When vital signs were unstable and the serum pH was < 7.25 despite an adequate increase in minute ventilation, use of sodium bicarbonate was indicated. After completion of surgery, oral feeding was started on postoperative days 3 – 4. Total parenteral nutrition was not initiated unless a patient required prolonged care with a mechanical ventilator. Intravenous phosphorus replacement was not performed during the early postoperative period. Immunosuppression was initiated by intravenous administration of 20 mg basiliximab within 2 h of surgery. Prior to reperfusion of the liver graft, patients received 250 mg prednisolone intravenously, with the dose being tapered on postoperative days 1 – 4, and replaced with prednisolone orally on day 5. The daily oral dose of prednisolone was reduced from 60 mg to 10 mg within 1 month after surgery. All patients received either 100 mg cyclosporine or 2 mg tacrolimus orally or by nasogastric tube twice a day from postoperative day 2. Doses of calcineurin inhibitors were adjusted according to blood levels. Mycophenolate mofetil (500 mg orally) was co-administered twice a day from postoperative day 2 and continued unless side-effects occurred.
Definition of ARF
Acute renal failure was defined according to the RIFLE criteria as a > 200% increase in serum creatinine or an absolute serum creatinine concentration ≥ 4 mg/dl (with an acute rise of 0.5 mg/dl), and a decrease in urine output to < 0.3 ml/kg/h during 24 h or anuria during 12 h. 22 Patients requiring renal replacement therapy, irrespective of the serum creatinine concentration, were deemed to have ARF. The occurrence of ARF was evaluated until postoperative day 30.
Perioperative and Serum Phosphorus Data
The following preoperative data were recorded: age; gender; body mass index (BMI); bone mineral density (measured by X-radiography within 1 month of surgery); aetiology of liver disease; model for end-stage liver disease (MELD) score; 23 Child–Pugh–Turcotte classification' 24 accompanying systemic diseases other than liver disease (hypertension, diabetes and heart disease); presence of ascites ≥ 1 l; history of abdominal surgery; spontaneous bacterial peritonitis; preoperative application of a molecular absorbent recirculating system; incidence of emergency transplantation. Laboratory tests were conducted within 1 day of surgery and included measurements of haematocrit, platelet count, estimated glomerular filtration rate (eGFR) using the Modification of Diet in Renal Disease equation, 25 prothrombin time, arterial pH, and total bilirubin, alanine transaminase, albumin, sodium, phosphorus and creatinine concentrations. Donor factors recorded included age, BMI, graft-to-recipient weight ratio and incidence of graft macrosteatosis ≥ 20%.
Intraoperative variables recorded were surgical time, duration of anhepatic phase, units of transfused PRBCs, hourly urine output, use of vasopressors, serum lactate change, last arterial pH and administered drugs (including furosemide, calcium chloride and sodium bicarbonate). A hypotensive episode was defined as a systolic arterial blood pressure < 70 mmHg for > 15 min.
The serum phosphorus concentration was measured 1 day before surgery and monitored until postoperative day 30. Early postoperative outcomes (such as mortality, duration of ICU stay and mechanical ventilator support), early allograft dysfunction and cardiac complications (including ischaemic heart disease, cardiomyopathy or arrhythmia more severe than ventricular premature complex) were also monitored until postoperative day 30. Early allograft dysfunction was defined as the presence of one or more of the following: serum bilirubin concentration ≥ 10 mg/dl on postoperative day 7, an international normalized ratio (INR) ≥ 1.6 on post -operative day 7 or an alanine or aspartate aminotransferase concentration > 2000 U/l within the first 7 days. 26
Statistical Analyses
All statistical analyses were performed using the SPSS® statistical package, version 18.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Data were expressed as mean ± SD, median (interquartile range) or n (%). To compare patients with and without ARF, continuous data were analysed using the unpaired t-test or Mann–Whitney U-test, and categorical data were analysed using the χ2-test. The Shapiro–Wilk test was used to confirm normal distribution. Perioperative recipient factors, donor factors and serum phosphorus concentrations were compared between patients with or without ARF. Factors that showed a potential association with ARF in the univariate intergroup comparison were selected for inclusion in analyses to establish a predictive model for ARF. When multiple factors were significantly correlated, the most significant factor from the clinical point of view was chosen. Postoperative serum phosphorus concentrations were also compared between patients with and without ARF, and diagnostic values for ARF occurrence were evaluated by the area under the receiver operating characteristic curve (AUC). The serum phosphorus variable with the highest AUC value was entered in the next step of analysis.
The predictive functions of perioperative factors for ARF occurrence were determined using a logistic regression model. Before multivariate analysis, continuous variables selected in intergroup comparisons were dichotomized using median, quartile or clinically meaningful cut-off points. After univariate logistic regression, multivariate analysis was performed using forward and backward stepwise logistic regression modelling processes, with variables shown to be significant by univariate logistic regression. The intercorrelation among the predictors from multivariate analysis was analysed by Spearman's rank correlation coefficient test. The sensitivity and unbiased estimate of the multivariate logistic model were evaluated using AUC analysis. A P-value < 0.10 was considered statistically significant in the univariate comparison of donor and preoperative and intraoperative recipient characteristics between patients with or without ARF. Otherwise, a P-value < 0.05 was considered statistically significant.
Results
During the study period, 429 adult patients underwent LDLT at Seoul St Mary's Hospital. Of these patients, 75 were excluded due to preoperative renal replacement therapy, hepatorenal syndrome or a serum creatinine concentration ≥ 1.5 mg/dl before transplant surgery. Four patients were not included in the analysis because of incomplete or missing data regarding ARF definition, leaving 350 evaluable patients.
A total of 45/350 patients (12.9%) met ARF criteria during the first month after liver transplantation. Preoperative serum creatinine concentrations and eGFR in patients with or without ARF were within normal ranges and did not differ between the two groups (Table 1). Through postoperative day 30, peak serum creatinine concentrations were higher in patients with, than in those without, t ARF (2.97 ± 1.11 mg/dl versus 0.93 ± 0.45 mg/dl, respectively; P < 0.001) and nadir eGFRs were lower (26.4 ± 11.8 ml/min versus 102.4 ± 52.0 ml/min, respectively; P < 0.001). A total of 28 patients with ARF required renal replacement therapy during the month following surgery. The median timepoint for ARF occurrence was postoperative day 3 (range 1 – 25 days) after liver transplantation.
Comparison of donor and preoperative recipient characteristics between patients with or without acute renal failure (ARF), as defined by Risk Injury Failure Loss End-stage kidney disease criteria, after living-donor liver transplantation

Data presented as mean ± SD, median (interquartile range) or n (%) of patients.
Continuous variables analysed using unpaired t-test or Mann–Whitney U-test; categorical variables analysed using χ2-test.
BMI, body mass index; MELD, model for end-stage liver disease; CPT, Child–Pugh–Turcotte; MARS, molecular absorbent recirculating system; eGFR, estimated glomerular filtration rate using the Modification of Diet in Renal Disease equation; INR, international normalized ratio; NS, not statistically significant (P ≥ 0.10).
Age, gender, BMI and bone mineral density did not differ between the liver transplant recipients with or without ARF (Table 1). The most common indication for liver transplantation was hepatitis B virus-related liver disease; no intergroup difference was found regarding the aetiology of liver disease. Liver disease was more severe in patients with, than in those without, ARF (as indicated by significantly higher MELD scores and a significantly higher incidence of Child–Pugh–Turcotte class C; P < 0.001 for both comparisons). Preoperatively, patients with ARF were diagnosed with hypertension less frequently than those without ARF (P = 0.071), and exhibited significantly higher total bilirubin concentrations (P = 0.001) and INR of prothrombin time (P = 0.004) than patients without ARF. Platelet counts were significantly lower in patients with, than in those without, ARF (P = 0.003), but hepatic alanine transaminase concentrations did not differ between the two groups. There were no significant differences in donor-related factors between groups, except that patients with ARF received grafts from younger donors than those without ARF (P = 0.068).
Intraoperatively, patients with ARF had a significantly longer surgical time and required more units of PRBC transfusion than patients without ARF (P < 0.001 for both comparisons; Table 2). There were no significant differences between the two groups with respect to duration of the anhepatic phase, hourly urine output, last arterial pH, incidence of vasopressor usage or hypotensive episodes. The administered quantities of furosemide, calcium chloride and sodium bicarbonate were significantly higher in patients with ARF than in those without ARF (P < 0.001 for all comparisons). Compared with patients without ARF, the serum lactate concentration was increased in patients with ARF during surgery (P = 0.006).
Comparison of intraoperative factors between patients with or without acute renal failure (ARF), as defined by Risk Injury Failure Loss End-stage kidney disease criteria, after living-donor liver transplantation

Data presented as mean ± SD, median (interquartile range) or n (%) of patients.
Continuous variables analysed using unpaired t-test or Mann–Whitney U-test; categorical variables analysed using χ2-test.
PRBC, packed red blood cells; NS, not statistically significant (P ≥ 0.10).
Preoperatively, no difference was observed in the serum phosphorus concentration between patients with or without ARF (Fig. 1). Serum phosphorus concentrations started to increase from postoperative day 1, peaked on postoperative day 2 and decreased thereafter, reaching a plateau on day 5 in patients with ARF. In contrast, serum phosphorus concentrations did not increase markedly during the immediate period after liver transplantation in patients without ARF. The differences in serum phosphorus concentrations between patients with or without ARF were significant until postoperative day 7 (P < 0.05 for all comparisons). AUC values of the serum phosphorus concentration for ARF occurrence on postoperative days 1, 3 and 5 were 0.759, 0.758 and 0.756, respectively. The serum phosphorus concentration on postoperative day 1 had the highest AUC value and was selected for inclusion in univariate and multivariate logistic regression analyses.
Comparison of changes in serum phosphorus concentrations from the preoperative value through to postoperative day 30 between patients with acute renal failure (ARF group) and without ARF (non-ARF group), as defined by the Risk Injury Failure Loss End-stage kidney disease criteria, after living-donor liver transplantation. Data presented as mean ± SD. *P < 0.05 versus non-ARF group on respective postoperative day (determined by unpaired t-test)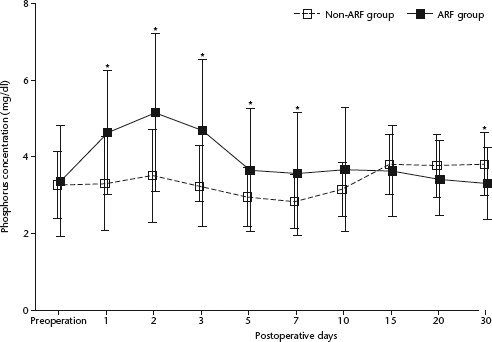
Table 3 lists all perioperative and serum phosphorus concentration variables that were entered into the logistic regression analyses. In univariate logistic regression, a long surgical time (≥ 10 h) and the administration of intraoperative drugs (such as furosemide and calcium chloride) were associated with a greater than five-fold relative risk for ARF occurrence. Stepwise multivariate logistic regression analysis, however, identified three significant independent predictors for ARF occurrence after LDLT: serum phosphorus concentration ≥ 4.5 mg/dl on postoperative day 1; MELD score ≥ 20 points; intraoperative PRBC transfusion ≥ 10 units. The relative risk for ARF in LDLT recipients was increased more than five-fold if the serum phosphorus concentration was ≥ 4.5 mg/dl on postoperative day 1, but the phosphorus concentration was not correlated with the MELD score and intraoperative PRBC transfusion ≥ 10 units (correlation coefficient r < 0.3 for both variables). AUC analysis indicated that this model had a clinically suitable accuracy to predict ARF after LDLT (AUC 0.788; 95% CI 0.714, 0.863; P < 0.001).
Logistic regression analyses to establish a predictive model for acute renal failure, as defined by Risk Injury Failure Loss End-stage kidney disease criteria, after living-donor liver transplantation

Dichotomized using median, quartile or clinically meaningful cut-off points.
Variables shown to be significant (P < 0.05) analysed using forward and backward stepwise logistic regression.
CI, confidence interval; MELD, model for end-stage liver disease; PRBC, packed red blood cell; NS, not statistically significant (P ≥ 0.10).
Patients with ARF had a 10-times higher mortality rate at 30 days (P < 0.001) and stayed significantly longer in the ICU than patients without ARF (P = 0.024, Table 4). A significantly higher incidence of reintubation (P = 0.001) and a requirement for a significantly longer postoperative mechanical ventilation period (P = 0.011) were observed in patients with, compared with those without, ARF. The rate of early allograft dysfunction in patients with ARF was three-times higher than that recorded in those without ARF (P < 0.001). There was no significant difference in the postoperative cardiac complication rate between the two groups.
Comparison of postoperative outcomes between patients with or without acute renal failure (ARF), as defined by Risk Injury Failure Loss End-stage kidney disease criteria, after living-donor liver transplantation

Data presented as mean ± SD or n (%) of patients.
Continuous variables analysed using unpaired t-test; categorical variables analysed using χ2-test.
ICU, intensive care unit; NS, not statistically significant (P ≥ 0.05).
Discussion
Using the RIFLE criteria for the diagnosis of ARF, the present study found that hyperphosphataemia on postoperative day 1 could be used as an early predictor of ARF occurrence after LDLT. Patients with hyperphosphataemia (serum phosphorus concentration ≥ 4.5 mg/dl) on postoperative day 1 had a more than five-fold greater risk for newly developing ARF than those without hyperphosphataemia.
Several studies have evaluated the impairment of renal function following liver transplantation, but appropriate comparison among these studies is difficult due to the adoption of different definitions of ARF. To standardize definitions, many recent reports have used RIFLE or the Acute Kidney Injury Network (AKIN) criteria to describe acute kidney injury following liver transplantation.6,9,14,16,17,27 The RIFLE ARF criteria have been evaluated under various clinical settings and proven to be associated with serious clinical consequences.27– 31 Validation of the RIFLE and AKIN criteria has not, however, been fully described in patients with liver disease, as highlighted by a study evaluating the impact of acute kidney injury definition on outcomes following liver transplantation. 5
The incidence of ARF in the present study was 12.9%, which is lower than previously reported in studies that evaluated kidney dysfunction following liver transplantation, using the RIFLE ARF criteria.6,27,30 This finding indicates that patients undergoing LDLT sustained lower rates of renal injury than patients undergoing deceased-donor liver transplantation, as reflected by lower MELD scores in the LDLT recipients.14,32 There are several reasons why renal injury may be less severe in LDLT. These include the use of a piggyback technique in the liver transplantation itself, as performed in the present study, which avoids occlusion of renal venous outflow and so may reduce renal injury during the anhepatic phase. 33 Furthermore, there is evidence that patients undergoing LDLT also have markedly lower pre- and postoperative concentrations of inflammatory markers. 34
The present study is consistent with previous reports that have shown ARF after liver transplantation to be associated with significantly higher postoperative mortality, longer ICU stays and more frequent graft dysfunction.6,27 Animal experiments have demonstrated that acute kidney injury is not an isolated event, but results in remote organ dysfunction involving the heart, lungs, liver, intestines and brain. 35 It has been proposed that acute kidney injury induces liver dysfunction by increasing small intestinal production of the proinflammatory cytokine interleukin-17A, which induces hepatic inflammation, necrosis and apoptosis with subsequent cytokine flow via the portal circulation. 35
Phosphorus is an essential mineral that, in nature, is usually found combined with oxygen as phosphate. 36 Phosphate is a vital component of cell membranes and other intracellular compounds, such as nucleic acids and nucleoproteins. The amount of intracellular phosphate is 100-times higher than that of extracellular phosphate, and most intracellular phosphate exists as organic phosphate compounds such as creatine phosphate, adenosine triphosphate and 2,3-diphosphoglycerate. Phosphorus is an essential component of tissue metabolism, therefore it has been assumed that hypophosphataemia following major hepatectomy is due to utilization of large amounts of phosphate during liver regeneration. 37 Simple calculations based on the recovery rates of liver mass and intracellular and plasma phosphate concentrations have, however, shown this explanation to be seriously flawed: the rate of phosphate uptake required by a rapidly recovering liver following hepatectomy cannot account for the observed severity of hypophosphataemia.20,21,38 Accordingly, studies have evaluated the association between hypophosphataemia and increased urinary phosphorus loss caused by liver regeneration.20,21 The factors underlying urinary phosphate loss following hepatic surgery remain unclear, but an increase in circulatory phosphaturic factors (phosphatonins) has been suggested to be an important aetiological factor in hypophosphataemia. Matrix extracellular phosphoglycoprotein is a putative phosphatonin and is activated by cathepsin B released by the injured liver. 39
In the present study, early postoperative serum phosphorus concentrations were higher than preoperative concentrations in patients with ARF, but not in patients without ARF. Differences in the extent of urinary phosphorus excretion between patients with or without ARF were likely to be responsible for this observation in early postoperative concentrations, although this was not directly measured. This assumption cannot, however, explain why overall phosphorus concentrations did not decrease below preoperative values, following transplant surgery in patients without ARF. These data might be attributed to the difference between transplant surgery and major hepatectomy. Hepatectomized livers may begin to regenerate as soon as surgical insults cease. In contrast, liver grafts endure an ischaemic period, become reperfused during transplant surgery, and undergo a degree of transient graft dysfunction during the early postoperative period until the damage from ischaemia/reperfusion injury disappears. The consumption of phosphorus for regeneration may, therefore, be less effective in a transplanted liver than in a hepatectomized liver.
The importance of the intraoperative period on the occurrence of postoperative acute kidney injury is being increasingly recognized.9,14 Cross-clamping of the portal vein and inferior vena cava during the anhepatic phase interrupts venous return of the lower extremities and splanchnic bed. Consequently, it may result in decreased cardiac output and blood pressure, increased systemic vascular resistance and reduced perfusion to vital organs. 13 Reduction in organ perfusion may lead to renal hypoperfusion and potential ischaemic injury. To elucidate intraoperative risk factors for postoperative ARF, the current study analysed patients without preoperative renal dysfunction. Preoperative creatinine concentrations and eGFR were within normal ranges and did not differ between patients with or without post-LDLT ARF.
In the present study, PRBC transfusion of ≥ 10 units was identified as an independent risk factor for postoperative ARF occurrence. Using univariate analyses, other retrospective studies have also confirmed that PRBC transfusion is a risk factor for ARF occurrence.6,9 Furthermore, in a retrospective study analysing patients with normal renal function, postoperative renal dysfunction after liver transplantation was independently associated with units of PRBC transfusion by multivariate analysis. 40 The extent of intraoperative transfusion is also known to be independently associated with outcome after orthotopic liver transplantation.41,42 Despite these published findings, it would still be premature to conclude that PRBC transfusion is an independent predictor of the postoperative occurrence of acute kidney injury following liver transplantation. Rather, the data should be understood within the context of unstable haemodynamics. The results of univariate analyses in the present study indicated indirectly that haemodynamics were compromised intraoperatively in patients with ARF; these patients showed more severe lactate change and required greater intraoperative administration of rescue drugs (such as diuretics, calcium chloride or sodium bicarbonate) for poor vital signs. Preoperative MELD score was also identified as another independent risk factor for postoperative ARF occurrence, in the present study. Previous research has shown that a high preoperative MELD score is associated with renal impairment following liver transplantation.43,44
The present study had several limitations. First, the study was susceptible to bias due to its retrospective design. Surgical techniques, perioperative management and postoperative immunosuppression were not uniform even though guidelines existed. Secondly, more than 50 perioperative variables were included in the analysis, meaning that it was not possible to consider all potential risk factors in one model. For example, factors such as cold ischaemic time and occurrence of postreperfusion syndrome were not included in the current analyses because of insufficient or inaccurate data. Thirdly, the exact serological cause of early postoperative hyperphosphataemia in patients with ARF could not be ascertained due to the study design.
In conclusion, using the RIFLE criteria to define ARF following LDLT, the present study found that perioperative outcomes were poorer in patients who developed ARF in the postoperative period, compared with outcomes in those who did not develop ARF. Multivariate logistic regression analyses demonstrated that a serum phosphorus concentration ≥ 4.5 mg/dl on postoperative day 1, a MELD score of ≥ 20 points and PRBC transfusion of ≥ 10 units were independent predictors of the development of ARF after LDLT. Of these risk factors, early hyperphosphataemia was associated with the highest relative risk for ARF and may represent an early and simple indicator for its occurrence after LDLT. A further prospective study is needed to identify the detailed and direct causes of hyperphosphataemia in patients with ARF after LDLT.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
