Abstract
Objective:
To compare clinical outcomes between patellar resurfacing and nonresurfacing in total knee arthroplasty (TKA).
Methods:
Data from osteoarthritis patients who underwent TKA and were followed up for ≥ 9 years were analysed retrospectively. Patients were divided into two groups: patellar nonresurfacing group and patellar resurfacing group. In the nonresurfacing group, the partial lateral facet of the patella was removed, the patella was reshaped to match the trochlea of the femoral prosthesis and circumpatellar denervation was performed. In the resurfacing group, the patella was resurfaced with a cemented component. Clinical outcomes included incidence of anterior knee pain, Knee Society Score, patient satisfaction, revision rate and radiographic findings.
Results:
Of the 130 patients included, 71 were assigned to the nonresurfacing group and 59 to the resurfacing group. No significant between-group differences were observed for any clinical outcomes measured. The incidence of anterior knee pain was 14.1% (nonresurfacing group) and 5.1% (resurfacing group). The revision rate was 9.89% (nonresurfacing group) and 3.4% (resurfacing group).
Conclusion:
Clinical outcomes for patellar nonresurfacing, including patelloplasty and circumpatellar denervation, are similar to those for patellar resurfacing, in TKA.
Keywords
Introduction
The decision to perform patellar resurfacing during total knee arthroplasty (TKA) remains controversial.1–16 Many surgeons used to recommend performing patellar resurfacing routinely, in order to decrease the incidence of anterior knee pain (AKP) and the rate of revision caused by patellofemoral problems.1,2,9,12,13 Patellar resurfacing can result in complications (including fracture, patellar component failure, osteonecrosis, instability, tendon rupture and patellar clunk syndrome),17–21 therefore greater attention is being paid to patellar nonresurfacing. Modern prostheses are designed to incorporate the patella in a way that reduces contact stress between them, so that they interact like normal patellofemoral joints, consequently reducing postoperative AKP.22–25 Numerous controlled clinical trials have compared TKA outcomes between patellar nonresurfacing and resurfacing procedures, but results have been inconclusive, particularly regarding AKP and revision rate.1–16 In several uncontrolled trials, compared with other procedures, patellar partial lateral facetectomy and circumpatellar denervation were reported to achieve better therapeutic effects (including improved Western Ontario McMaster Osteoarthritis Index Score, Knee Society Score and patellofemoral symptoms, and slow progression of patellofemoral osteoarthritis), and reduce postoperative AKP in patients with isolated patellofemoral osteoarthritis,26–30 but research into the therapeutic effects of these procedures in TKA is limited.
In the present study, the nonresurfaced patella was treated using partial lateral facetectomy and circumpatellar denervation, and the incidence of AKP, revision rate and knee function between the patellar resurfacing and nonresurfacing groups was compared.
Patients and methods
Study Population
Data from patients with osteoarthritis who underwent primary unilateral TKA at Shengjing Hospital, China Medical University, Shenyang, China, between January 2000 and December 2002, were reviewed retrospectively. The indication for surgery was degenerative osteoarthritis that was severe enough to warrant TKA after an adequate trial of nonoperative therapy. Patients were excluded from this study if they had any of the following: a history of patellar fracture, patellectomy, high tibial or distal femoral osteotomy; any surgery involving the extensor mechanism; septic arthritis of the knee or osteomyelitis; severe deformity (varus angulation, valgus angulation or flexion contracture of > 15°); severe medical disability that limited the patient's ability to walk. Patients with follow-up data of 9 years were enrolled. Those undergoing surgery between January 2000 and November 2000 underwent patellar resurfacing, whereas those undergoing surgery between December 2001 and December 2002 underwent patellar nonresurfacing.
Ethical approval was given by the Medical Ethics Committee of Shengjing Hospital, China Medical University, Shenyang, China (reference no. 20001568). Written informed consent was obtained from all study participants.
Surgical Procedures
All surgical procedures were performed by the same group of three surgeons (B.L., L.B., G.W.). All patients received the same type of cemented posterior cruciate sacrifice prosthesis (press-fit condylar [PFC; DePuy Orthopaedics, Warsaw, IN, USA]). A mid-vastus approach was adopted through an anterior midline skin incision. Bone cuts and soft-tissue balancing were performed in the same sequence. In the nonresurfacing group, patellar osteophytes were removed, partial (1 cm) lateral facetectomy of the patella was performed, the patella was reshaped to match the trochlea of the femoral prosthesis, and the soft tissue around the patella was cauterized using an electroscalpel to destroy the patellar innervation (circumpatellar denervation). In the resurfacing group, patellar resurfacing was performed with a cemented inset PFC Sigma® oval dome component (DePuy Orthopaedics). Heights of the patellae were measured pre- and postoperatively. Optimal patellar tracking was ensured by appropriate soft-tissue balancing. If the patella subluxated during passive testing of the range of movement, a lateral release was performed ≥ 2.5 cm from the lateral patellar border.
A standardized perioperative regimen was used for all patients. In detail, second-generation 3 g/day cephalosporin was injected intravenously for 3 days from 1 day prior to the operation. After surgery, the affected limb was elevated higher than the heart and ice bags were placed around the affected knee. Continuous passive movement was not used postoperatively. Active isometric quadriceps, initiative straight-leg raising and extending–flexing motion was encouraged in the immediate postoperative period. Walking with partial weight bearing was permitted 24 h postoperatively under the supervision of a physical therapist.
Study Assessments
A preoperative evaluation was performed using the Knee Society Pain Score, Knee Society Function Score and Total Knee Society Score. 31 Postoperative follow-up assessments were performed at 3 months and at 1, 2, 3, 5, 7 and 9 years. Data collected at 9 years postoperatively were analysed in the present study. Clinical outcomes were evaluated using the three components of the Knee Society Score mentioned above, 31 the British Orthopaedic Association patient-satisfaction score, 32 X-ray examination findings, the incidence of AKP and the revision rate. Pre-and postoperative clinical evaluations were performed by surgeons (mainly M.H. and J.W.) who were unaware as to whether patients had received patellar resurfacing or nonresurfacing.
Statistical Analyses
All data were analysed using the SPSS® software package, version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. An unpaired Student's t-test was used to compare pre- and postoperative Knee Society Scores between the two groups. Fisher's exact test was used to assess nominal data including incidence of AKP, patient-satisfaction score and revision rate. Differences at a level of P < 0.05 were considered to be statistically significant.
Results
Data from 189 patients were reviewed. Thirty-one patients with at least one of the exclusion criteria were excluded from this study. Of the remaining 158 patients, 28 were followed up for < 9 years and were also excluded. In total, 130 patients were followed up for 9 years and enrolled in the study: 59 in the patellar resurfacing group and 71 in the patellar nonresurfacing group. In the resurfacing group, the difference between pre- and postoperative heights of the patellae was ≤ 2 mm for each patient. There were no statistically significant between-group differences regarding age, gender, body mass index, history of AKP, preoperative Knee Society Scores and duration of follow-up assessments (Table 1). The mean ± SD duration of surgery was 82.3 ± 22.4 min in the nonresurfacing group and 86.7 ± 25.8 min in the resurfacing group; this difference was not statistically significant. Lateral retinacular release was performed in six patients in the nonresurfacing group and in three patients in the resurfacing group, with no significant between-group differences.
Demographic and preoperative data for Chinese patients with osteoarthritis, undergoing total knee arthroplasty with patellar nonresurfacing or resurfacing

Data presented as mean ± SD, or n patients.
No statistically significant between-group differences (P 0.05).
Unpaired Student's t-test,
Fisher's exact test.
The findings of postoperative clinical evaluations are summarized in Table 2. At 9 years postoperatively, there were no significant between-group differences in terms of Knee Society Pain Score, Knee Society Function Score and Total Knee Society Score. According to the guidelines of the British Orthopaedic Association patient satisfaction score, 32 patient satisfaction was assessed before any secondary operation was performed. There was no significant difference between the two groups in the proportion of patients who were satisfied with their treatment or the proportion experiencing postoperative anterior knee pain.
Postoperative patient data comparing Knee Society Scores, incidence of anterior knee pain, patient satisfaction and revision rates following total knee arthroplasty with patellar nonresurfacing versus resurfacing, in Chinese patients with osteoarthritis

Data presented as mean ± SD or n (%) patients.
No statistically significant between-group differences (P 0.05).
Unpaired Student's t-test,
Fisher's exact test.
Superficial redness around the wound occurred in six patients in the nonresurfacing group and in four patients in the resurfacing group. After a 1-week course of oral antibiotics, superficial redness disappeared, with no evidence of infection. One patient in the resurfacing group developed an infection 6 months after surgery and arthroscopic washout was performed to eliminate it. One knee in the nonresurfacing group developed anchylosis 1 year after surgery that required an arthroscopic synovectomy. Seven (9.9%) patients in the nonresurfacing group underwent revision and patellar resurfacing due to postoperative AKP and only four patients obtained a satisfactory outcome. Two (3.4%) patients in the resurfacing group underwent revision due to postoperative AKP and patella fracture, respectively, and both obtained a satisfactory outcome. X-ray examinations showed that there was no radiologic loosening or wearing down of prosthetic components in either group.
Discussion
Although TKA achieves a high rate of clinical success, data reviewed in Table 31–16 highlight the controversy that remains regarding whether the procedure should include patellar resurfacing. The present study compared the clinical outcomes of two treatment regimens: patellar resurfacing and patellar nonresurfacing. No differences were found in relation to AKP, revision rate and knee function between the two methods.
Review of prospective studies comparing patellar nonresurfacing with patellar resurfacing (retention/resurfacing; R/R) in total knee arthroplasty
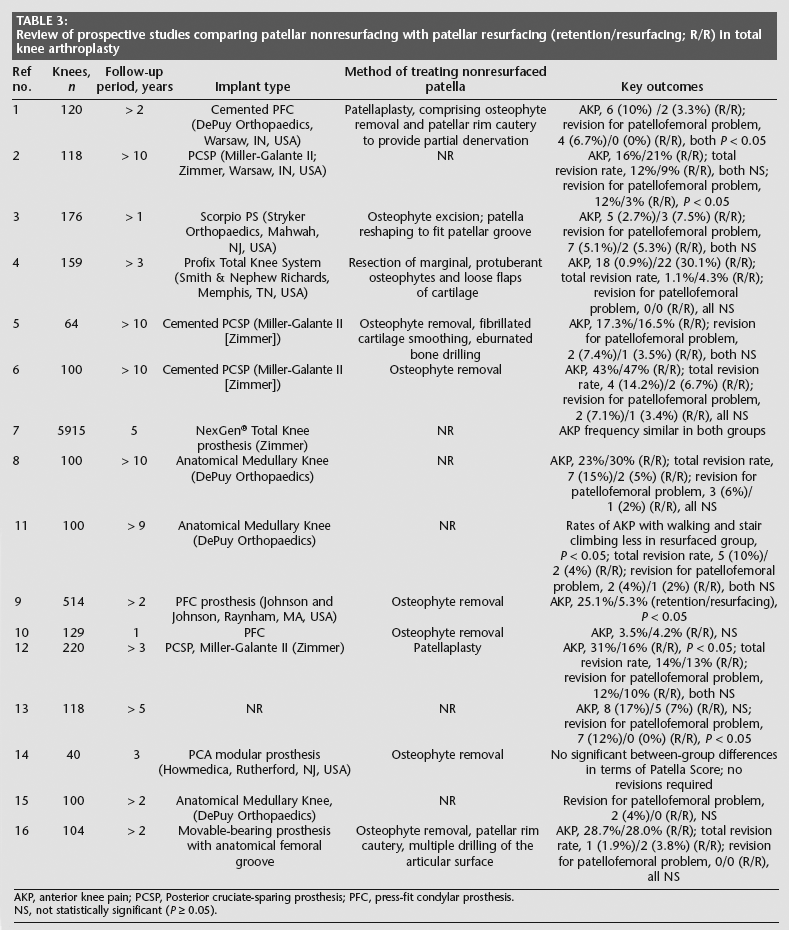
AKP, anterior knee pain; PCSP, Posterior cruciate-sparing prosthesis; PFC, press-fit condylar prosthesis.
NS, not statistically significant (P ≥ 0.05).
Anterior knee pain is a key search term when looking for literature describing optimal patellar treatment in TKA. Search results show varying incidences of AKP:1–16 2.7% – 43% with the patellar nonresurfacing regimen and 3.3% – 44% with the patellar resurfacing regimen. The postoperative AKP rate in the present study was 14.1% in the nonresurfacing group and 5.1% in the resurfacing group. The incidence of AKP in published trials is so varied that it becomes difficult to collect and analyse AKP data, in order to identify optimal treatment of the patella during TKA. We believe that the variation in outcomes may be attributed to differences in patient demographics, design of the total knee prostheses, operating technique and data examiners. Additional factors that may contribute to the different outcomes between this study and other published studies1–16 are discussed in the following paragraphs.
First, in the present study, the lateral patellar facet was excised in the nonresurfacing group. This method is effective for treating patellofemoral osteoarthritis,26–28 although we have not found any published studies that report this technique for TKA. In patellofemoral osteoarthritis, the patella tilts laterally due to the loss of cartilage on the lateral facet, which increases the pressure in the lateral patellofemoral joint. 27 The lateral part of the patella and the eroded part of the bone are excised to eliminate bone articulation, which allows pressure to decrease in the lateral patellofemoral joint. Partial lateral facetectomy is suggested to be an effective treatment of isolated patellofemoral osteoarthritis, to relieve AKP.26–28 The beneficial effects of this procedure have been documented to continue even at 10-year follow-up examinations. 26
Secondly, in the current study, circumpatellar electrocautery was performed in all patients. Immunohistochemical research on the innervation of peripatellar soft tissues has shown the presence of substance-P nociceptive afferent fibres. 33 These pain receptors are destroyed by electrocautery, to reduce postoperative AKP. An observational study comparing two groups of patients (n = 131 each) undergoing patellar nonresurfacing in TKA, with or without circumpatellar electrocautery, 34 found that the incidence of AKP was significantly lower in the group receiving circumpatellar electrocautery than in the other group. In two prospective studies, circumpatellar electrocautery was performed in both patellar resurfacing and patellar nonresurfacing TKA. The incidence of AKP in the two studies was 10% and 28.7% with regard to patellar nonresurfacing TKA, and 3.3% and 28.0% with regard to patellar resurfacing, respectively.1,16 The marked differences in AKP between the two studies might be due to the differences in the total knee prostheses used. The total knee prosthesis used in the present study was the same as that used by Patel et al. 1 , and the incidence of AKP was similar in both studies.
Thirdly, patients in the aforementioned prospective studies1,16 were from Western populations, in whom patellofemoral joint morphological features are not completely consistent with those observed in the Chinese patients included in the present study. It is reported that patellar thickness in the Chinese is less than that of Western populations, with the thinnest part being only 13 – 14 mm. 35 In clinical practice, we find that anterior femoral condyles of Chinese patients are thinner than those of Western patients and we believe, therefore, that the pressure in the patellofemoral joint is lower in Chinese than in Western patients due to these slight differences in morphological features of the joint, although this difference has not been proven to be statistically significant in any study.
Revision due to patellofemoral problems is another common feature to consider when selecting optimal treatment of the patella in TKA. Some trials have reported significant differences in revision rates due to patellofemoral problems between the resurfacing and nonresurfacing TKA,1,2,13 whereas others have found no such differences.3–12,14 –16 The current study did not reveal any significant differences in revision rates between the resurfacing or nonresurfacing techniques. The main cause of revision in patients undergoing patellar nonresurfacing is AKP. In patients undergoing patellar resurfacing, multiple factors can cause revision (including component loosening, patellar instability, patellar necrosis, patellar fracture and AKP).1–16 Two studies2,13 reported that the revision rate was significantly lower in the patellar resurfacing groups than in the nonresurfacing groups, while AKP rates were similar between both groups. It seems that, in patients undergoing patellar nonresurfacing TKA, there is an opportunity to undertake revisions to resurface the patella when AKP recurs. Not all patients with patellofemoral problems after patellar nonresurfacing TKA benefit from secondary patellar resurfacing, however. Three patients in the present study were dissatisfied with the outcome following revision surgery, due to recurrence of AKP. Perhaps many factors might affect the revision outcome, and the aetiology of AKP remains to be further explored.
The main limitations of the present study were that it was not a randomized, controlled trial, and the data were collected retrospectively. The study did, however, include an adequate number of patients treated during a similar time period, whose demographic features were matched between the two groups. Patients were divided into the two groups based two measures: on the time of the operation, and on whether patellar resurfacing or nonresurfacing was performed. Patellar resurfacing was performed in the early part of the study (between January 2000 and November 2000), whereas patellar nonresurfacing was performed during the later period (between December 2001 and December 2002). In other nonrandomized trials, however, patients were usually grouped according to only one measure (i.e., the main treatment method). By allocating patients into study groups on the basis of length of the operation time, the present study enabled patients' states of health to be more uniform within each group, compared with other nonrandomized studies. Consequently, this minimized selection bias in the present trial. Another limitation was that the degree of diseased articular patellar cartilage was not graded. We believe that this may not influence the accuracy of the conclusions drawn, because several other authors have reported that the status of the patellar cartilage does not influence clinical outcomes (including AKP), regardless of whether or not patellar resurfacing or nonresurfacing has been performed.8,13
In conclusion, the present study suggested that compared with patellar nonresurfacing TKA, patella resurfacing TKA has no advantages in terms of relieving pain, lowering revision rate and improving knee function during a minimum 9-year follow-up. Patellar nonresurfacing (including removal of patellar osteophytes, patellar partial lateral facetectomy and circumpatellar denervation) can obtain satisfactory outcomes in TKA. In addition, patellar nonresurfacing can easily be converted to patellar replacement, if AKP recurs.
Footnotes
Acknowledgement
The authors gratefully acknowledge the financial support of the Natural Science Foundation of China (NSFC), reference no. 81171716.
The authors had no conflicts of interest to declare in relation to this article.
