Abstract
Background
Computed tomography (CT) and magnetic resonance imaging (MRI) are indicated for use in preoperative planning and may complicate diagnosis and place a burden on patients with lumbar disc herniation.
Purpose
To investigate the diagnostic potential of MRI-based synthetic CT with conventional CT in the diagnosis of lumbar disc herniation.
Material and Methods
After obtaining prior institutional review board approval, 19 patients who underwent conventional and synthetic CT imaging were enrolled in this prospective study. Synthetic CT images were generated from the MRI data using U-net. The two sets of images were compared and analyzed qualitatively by two musculoskeletal radiologists. The images were rated on a 4-point scale to determine their subjective quality. The agreement between the conventional and synthetic images for a diagnosis of lumbar disc herniation was determined independently using the kappa statistic. The diagnostic performances of conventional and synthetic CT images were evaluated for sensitivity, specificity, and accuracy, and the consensual results based on T2-weighted imaging were employed as the reference standard.
Results
The inter-reader and intra-reader agreement were almost moderate for all evaluated modalities (κ = 0.57−0.79 and 0.47−0.75, respectively). The sensitivity, specificity, and accuracy for detecting lumbar disc herniation were similar for synthetic and conventional CT images (synthetic vs. conventional, reader 1: sensitivity = 91% vs. 81%, specificity = 83% vs. 100%, accuracy = 87% vs. 91%;
Conclusion
Synthetic CT images can be used in the diagnostics of lumbar disc herniation.
Introduction
Recent reports reveal that approximately five in 1000 adults experience lumbar disc herniation every year (1,2). During preoperative evaluation of the intervertebral discs of the lumbar segment, computed tomography (CT) and magnetic resonance imaging (MRI) are generally performed at the same time (3). The high resolution of MRI for soft tissue makes it the primary diagnostic modality for most spinal pathologies. MRI possesses good sensitivity and specificity for detecting disc herniation, disc degeneration, and pathological fractures. Therefore, it is routinely used for the diagnosis and surgical planning of spinal pathologies (4,5). However, MRI is not sufficient when high-quality images of the patient's bone structure are also desired, which is the case in detection of disc herniation. Moreover, the simultaneous use of CT and MRI can be burdensome to patients; it also exposes them to ionizing radiation and complicates the diagnostic workflow.
In the past decade, various techniques have been developed to generate synthetic CT (sCT) images based on MRI scans (6–10), which are primarily used for radiation treatment planning (11–13). In this study, we devised an approach to estimate CT-equivalent information from magnetic resonance (MR) images, mainly using technology based on deep learning to reconstruct axial MRI into sCT. This method has been verified clinically for the cervical (14) and lumbar spine (15).
Therefore, the aim of the present study was to compare the diagnostic quality of MRI-based sCT with that of conventional CT for the detection of disc herniation using T2-weighted (T2W) imaging as the standard of comparison. To our knowledge, there is no previous research that has investigated the potential use of sCT images for the diagnosis of lumbar disc herniation in a clinical setting.
Material and Methods
We used a prospective observational design. The study was authorized by the local ethics committee for studies that involved humans, and all participants were provided with written informed consent.
Patients
We recruited patients aged 30–80 years with symptoms of lumbar disc herniation who visited our hospital with lower back pain between January 2019 and February 2020. The exclusion criteria were pregnancy, contraindications to MRI, metallic implants, and an incomplete imaging examination.
MRI and CT protocols
All MRI examinations were performed with a 1.5-T MR scanner (Magnetom, Avanto; Siemens, Germany). The scan parameters for all MR acquisitions were as follows: fast spin-echo T2 sequence without contrast agent injection (TE = 70 ms, TR = 3670 ms, flip angle = 150°, field of view = 180 mm, and image acquisition time = 12 min). The corresponding CT image was acquired using the Siemens Somatom Definition AS with a tube voltage of 120 kV, an exposure current of 300 mA, an in-plane resolution of 0.59 ± 0.5 mm2, and a slice thickness of 1 mm. A total of 47 participants were examined with CT and MRI.
The CT images were rescaled to match the MR image resolution and field of view. A mutual information alignment algorithm was used to align each patient's MRI/CT images.
sCT acquisition
Conventional axial 2D T2W MR images with a slice thickness of 1 mm were used as input for the U-net model (16,17) (Fig. 1), which used a contracting (left) and an expanding (right) path to generate sCT images. To reduce interference from unnecessary information, we cropped the images to 160 × 160, preserving only the spine and surrounding areas. The 2D T2W MR image was imported into U-net and processed in the contracting path through repeated applications of two 3 × 3 convolutions, batch normalization (18), rectified linear unit activation (19), and max-pooling for downsampling. In the expanding path, the number of feature maps was halved after each upsampling operation. The cropped feature map in the shrink path was concatenated to a feature map of the same size in the expanding path. The final step utilized one convolution of 1 × 1 and yielded a 2D sCT image. Thus, two sets of CT images, conventional and synthetic, were acquired for each patient.
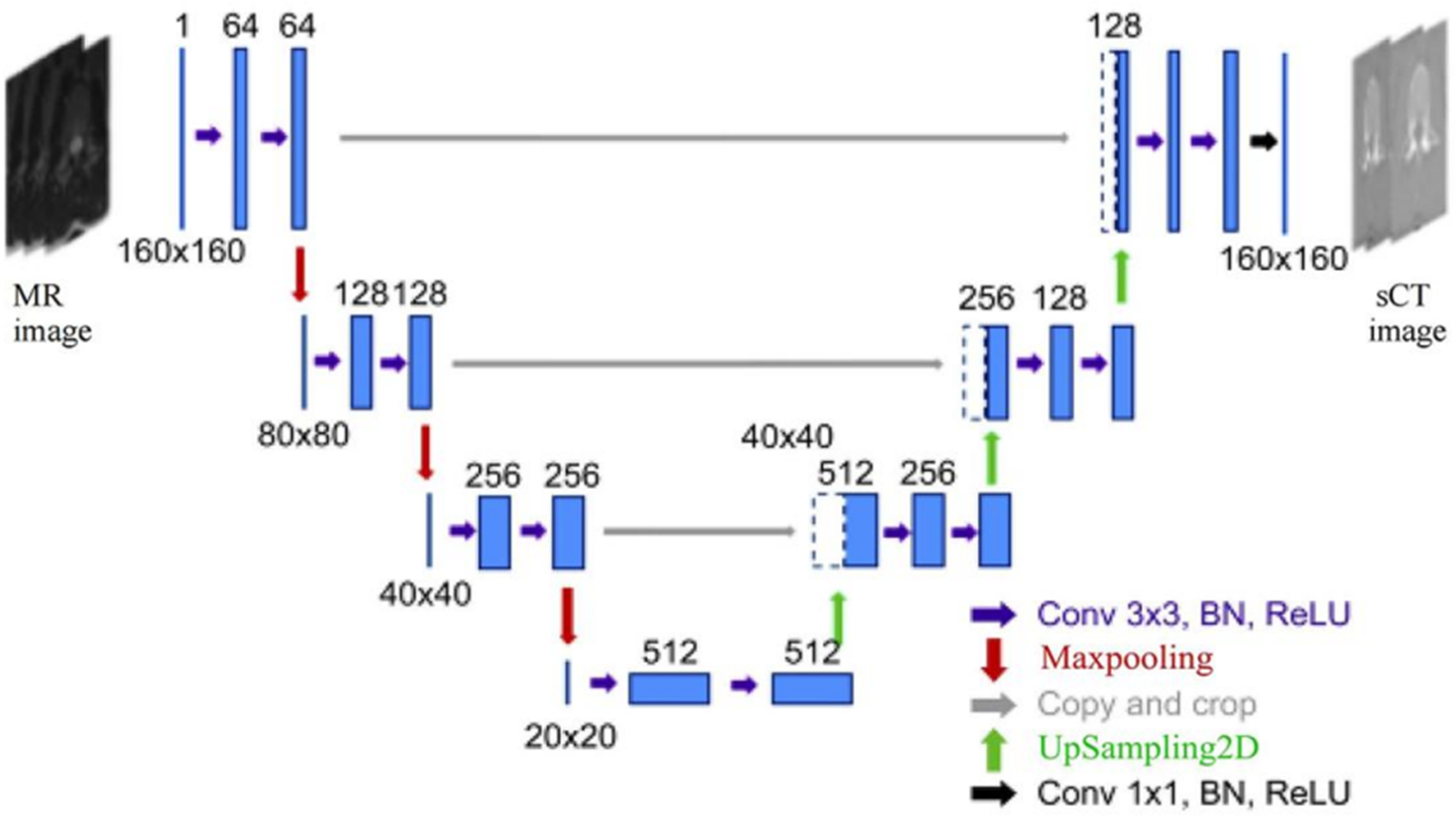
U-net architecture. Maps with multichannel features are depicted as blue boxes; numbers indicate the number of channels. White boxes, copying operations; arrows, different channels; BN, batch normalization; ReLU, rectified linear unit; sCT, synthetic computed tomography.
Image evaluation
The images were independently examined by two specialist radiologists with 15–20 years of experience in musculoskeletal disorders. The readers were blinded to the clinical data. Each reader was provided with training and a handbook containing standard definitions of imaging characteristics. The VolView 3.0 software was used to evaluate the T2W MR and sCT images. The two readers rated the subjective image quality of the synthetic and conventional CT scans on the following four scales: 1 = vertebral body delineation; 2 = soft-tissue delineation; 3 = intervertebral disc visibility; and 4 = artifacts. Image quality was categorized as follows: 4 = excellent (image quality and artifacts were minimal, and the vertebral body/soft tissues/disc were clearly defined); 3 = good (minimal artifacts or poor image quality, suboptimal delineation of either one or both structures mentioned); 2 = acceptable (the image quality was acceptable for diagnostic purposes, although obvious artifacts or other issues were visible on the image); and 1 = poor (the ability to delineate these structures was limited by a large number of artifacts or noise).
Diagnostic criteria for lumbar disc herniation
We used T2W imaging as the reference standard for the diagnosis of lumbar disc herniation, since the difference in diagnostic value between synthetic and conventional CT can be evaluated by comparing them with MRI, which has high soft-tissue resolution. Two musculoskeletal radiologists used both synthetic and conventional CT images to diagnose patients. The absence or presence of lumbar disc herniation was recorded as “normal” (the tissue around the intervertebral disc does not exceed the edge of the vertebral body, score = 0) or “abnormal” (the tissue around the intervertebral disc extends beyond the edge of the vertebral body, score = 1), respectively.
Statistical analysis
The subjective image quality of the conventional and synthetic CT scans was compared using the Wilcoxon test. Each reader's scores were compared in the same manner. The intra- and inter-reader reliabilities were assessed using Cohen's κ statistic (20). The Pearson chi-square test was used to ascertain the presence or absence of lumbar disc herniation. EmpowerStats (http://www.empowerstats.com) and R 3.2.3 (The R Foundation for Statistical Computing, Vienna, Austria) were used for all analyses.
Results
The participants’ characteristics are as summarized in Table 1. Fig. 2 illustrates the inclusion criteria of this study. A total of 15 patients had poor image quality due to motion artifacts; 19 participants (10 men, 9 women) were finally enrolled in the study. The final clinical diagnoses for all 19 participants were disc herniation (n = 19), degeneration (n = 19), and unknown (n = 3).
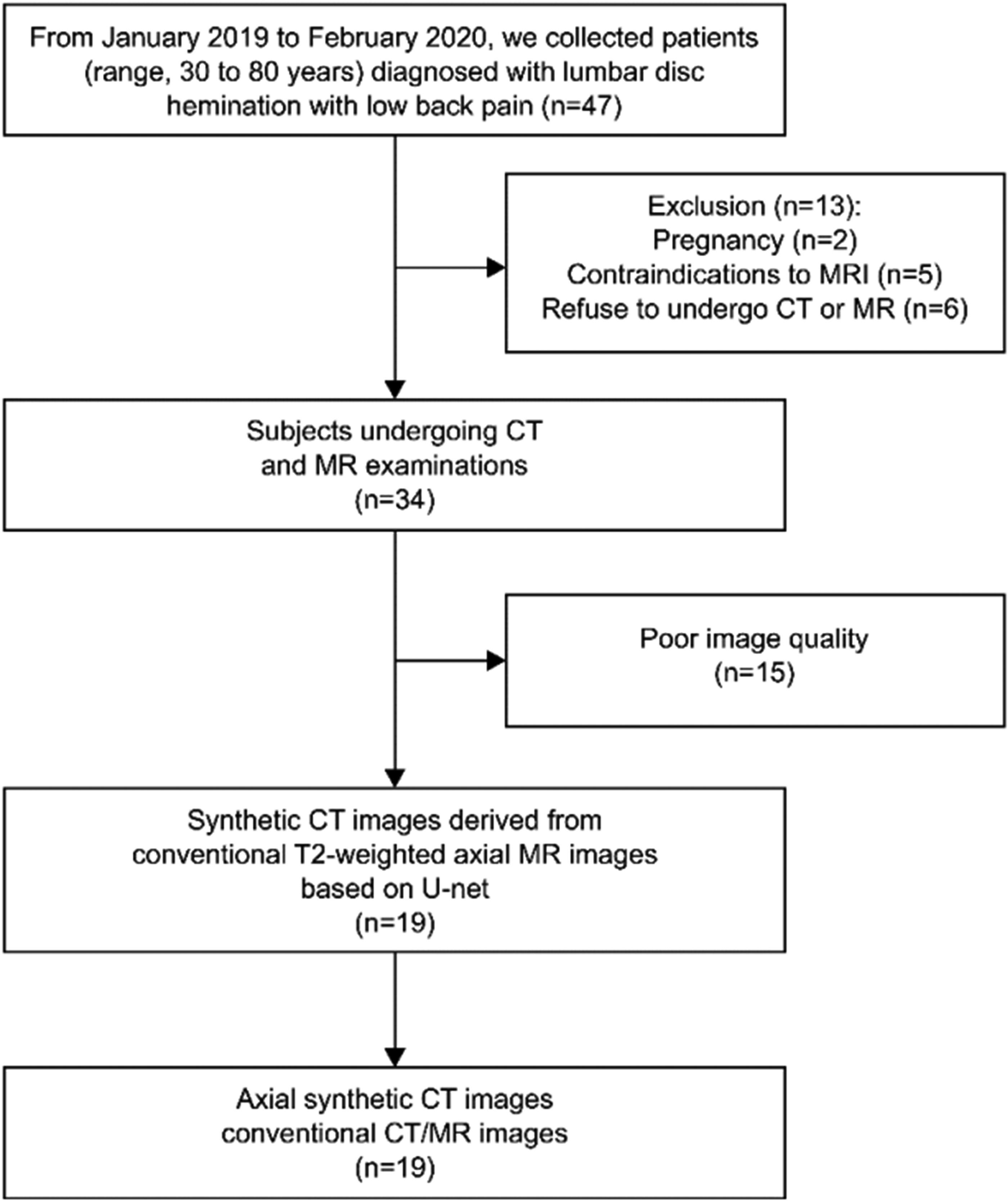
Flow chart for patient inclusion. CT, computed tomography; MRI, magnetic resonance imaging.
Participant characteristics.
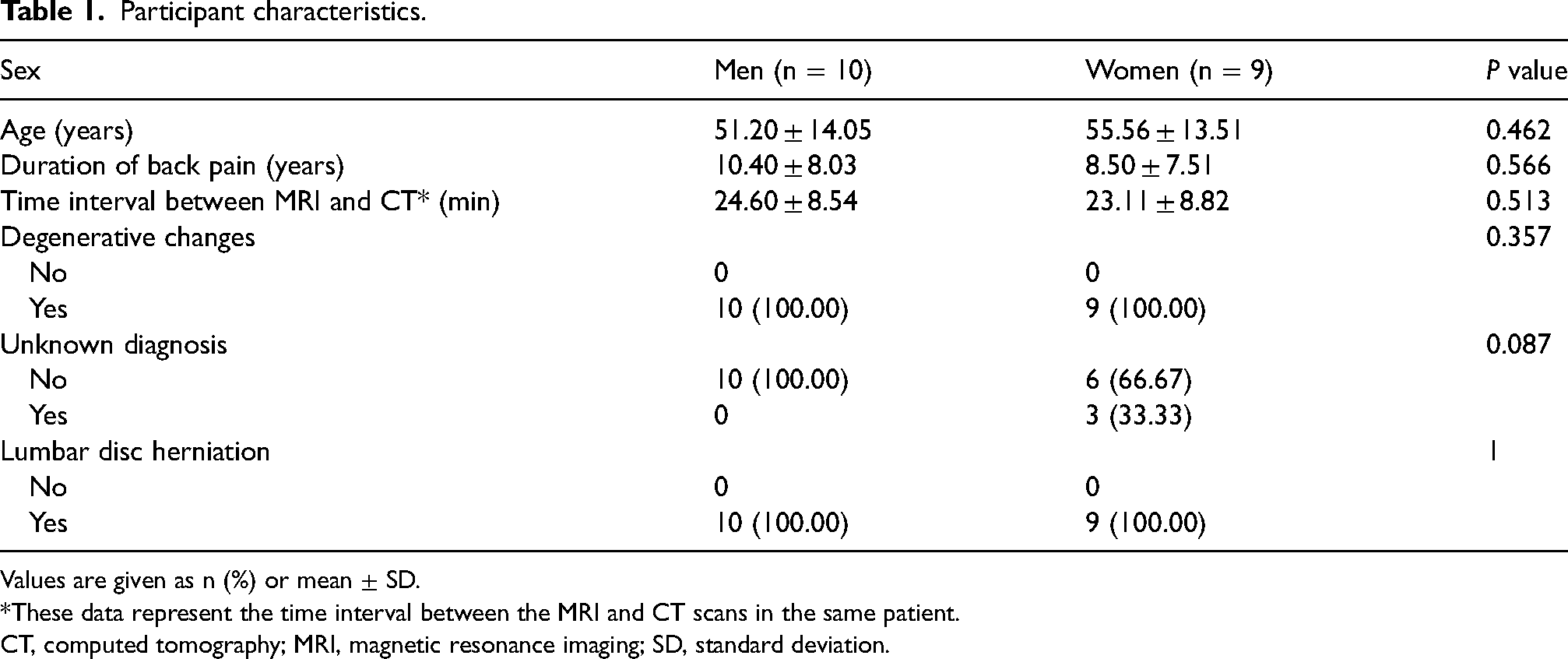
Values are given as n (%) or mean ± SD.
*These data represent the time interval between the MRI and CT scans in the same patient.
CT, computed tomography; MRI, magnetic resonance imaging; SD, standard deviation.
Inter- and intra-reader agreements
The subjective image quality of the synthetic and conventional images mostly ranged from good to excellent based on the assessments of the two readers, as shown in Fig. 3. The Cohen κ values for inter- and intra-reader agreements are listed in Table 2. The inter-reader κ values (indicating inter-reader agreement) for the conventional CT scans were 0.79, 0.72, and 0.71 for vertebral body delineation, soft-tissue delineation, and intervertebral disc visibility, respectively. The corresponding results for the sCT images were 0.71, 0.73, and 0.57, respectively. The Cohen κ values for intra-reader agreement between the conventional and synthetic CT images were 0.75, 0.59, and 0.47, respectively.
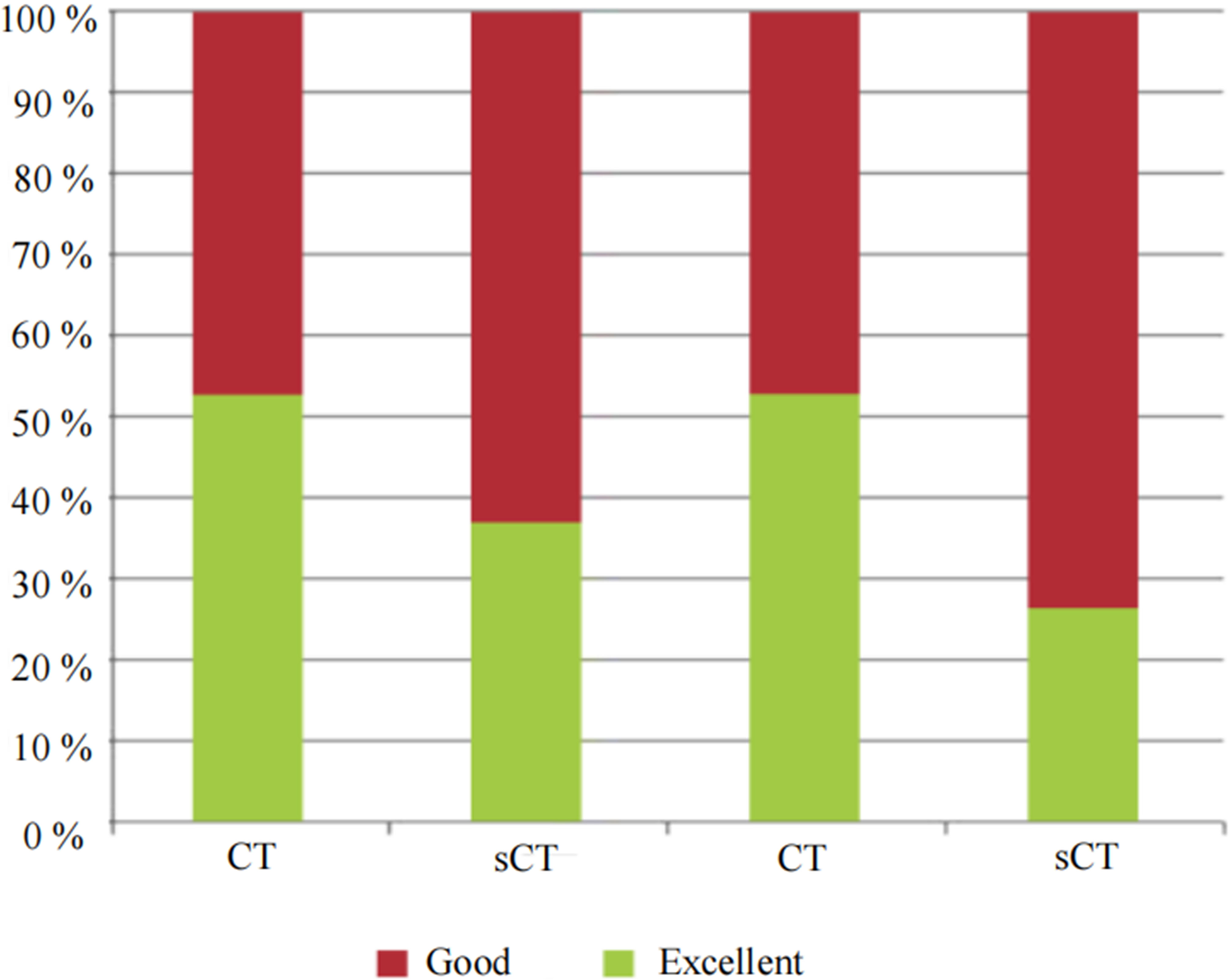
Image quality scores assigned by readers 1 (left) and 2 (right). sCT, synthetic computed tomography.
Inter- and intra-reader agreement for the evaluated structures.
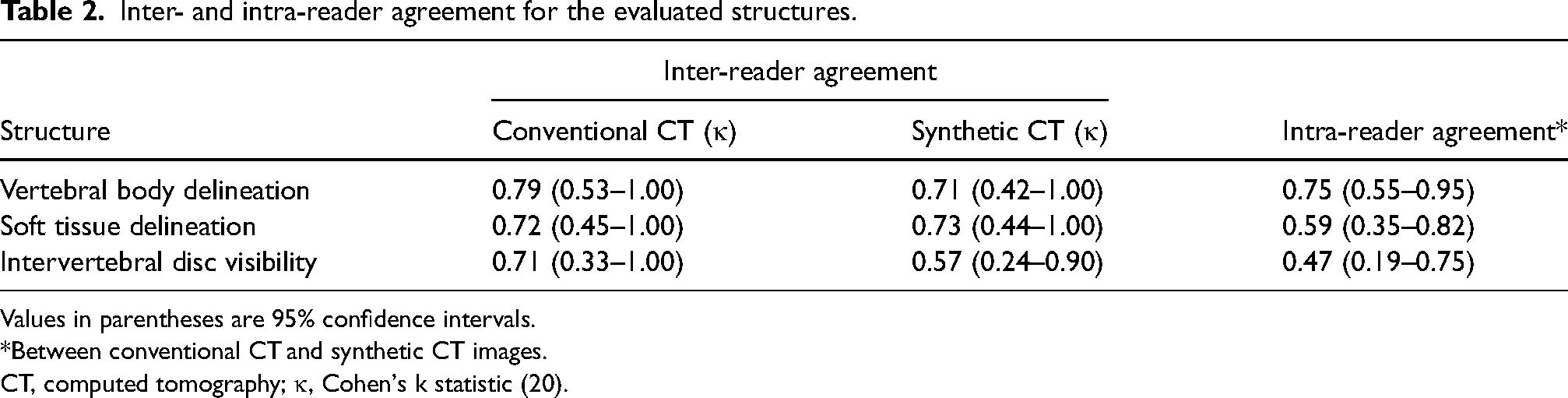
Values in parentheses are 95% confidence intervals.
*Between conventional CT and synthetic CT images.
CT, computed tomography; κ, Cohen's k statistic (20).
Diagnostic performance of sCT and conventional CT for lumbar disc herniation
Fig. 4 provides examples of lumbar disc herniation, as visualized on T2W imaging, sCT, and CT. Table 3 summarizes the results of the sensitivity, specificity, and accuracy analyses of conventional and sCT imaging, using T2W imaging as the reference standard. The sensitivity, specificity, and accuracy of CT for the detection of lumbar disc herniation for reader 1 were as follows: conventional CT versus sCT; sensitivity = 91% versus 81%; specificity = 83% versus 100%; and accuracy = 87% versus 91%;
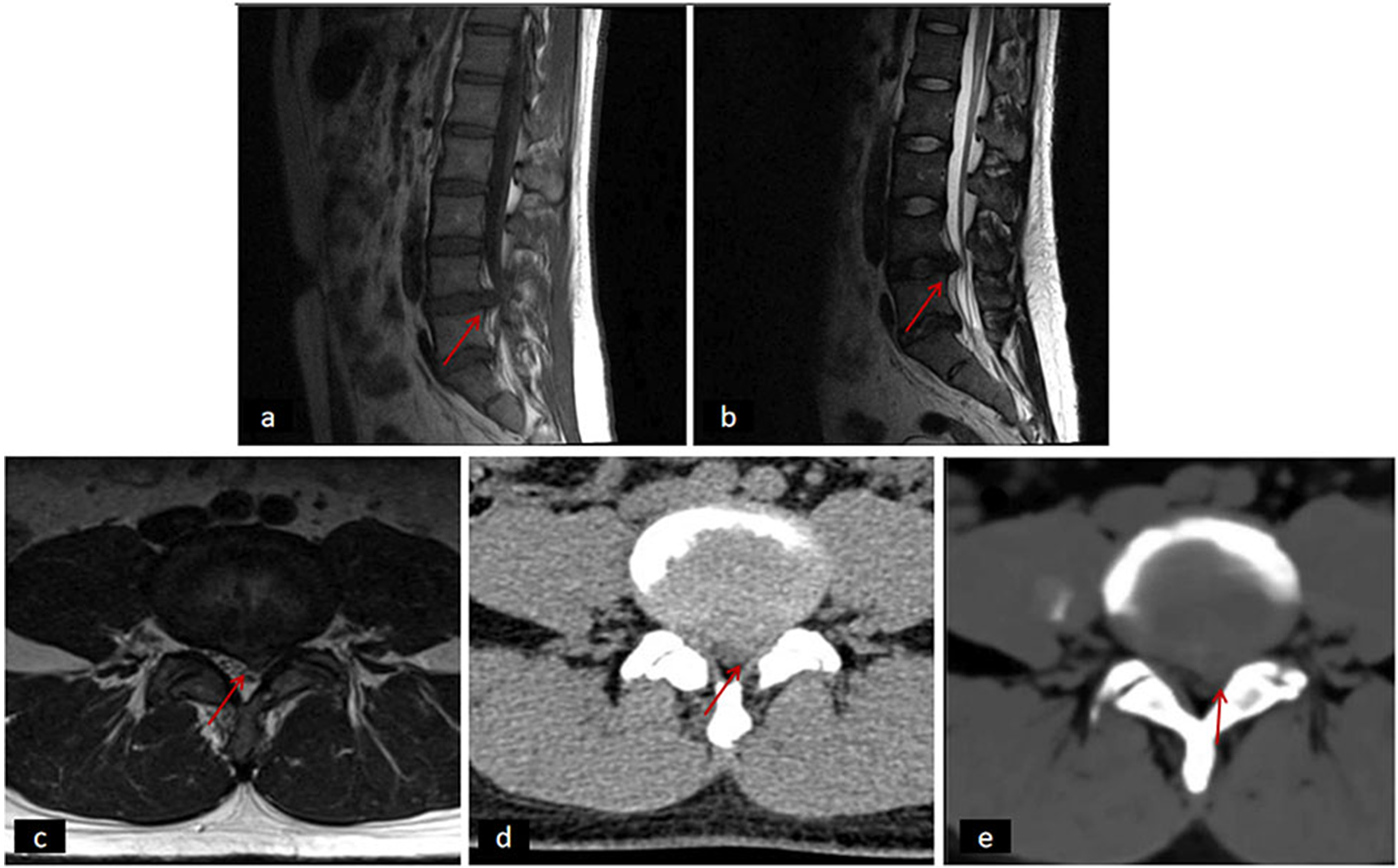
Imaging of a 37-year-old man with lumbar 4/5 disc herniation. (a) T1W imaging, sagittal view; (b) T2W imaging, sagittal view; (c) T2W imaging, axial view; (d) conventional CT scan; and (e) synthetic CT scan. Arrows, lumbar disc herniation. CT, computed tomography. T1W, T1-weighted; T2W, T2-weighted.
Estimated diagnostic value of conventional and synthetic CT images using T2-weighted imaging as the reference standard.
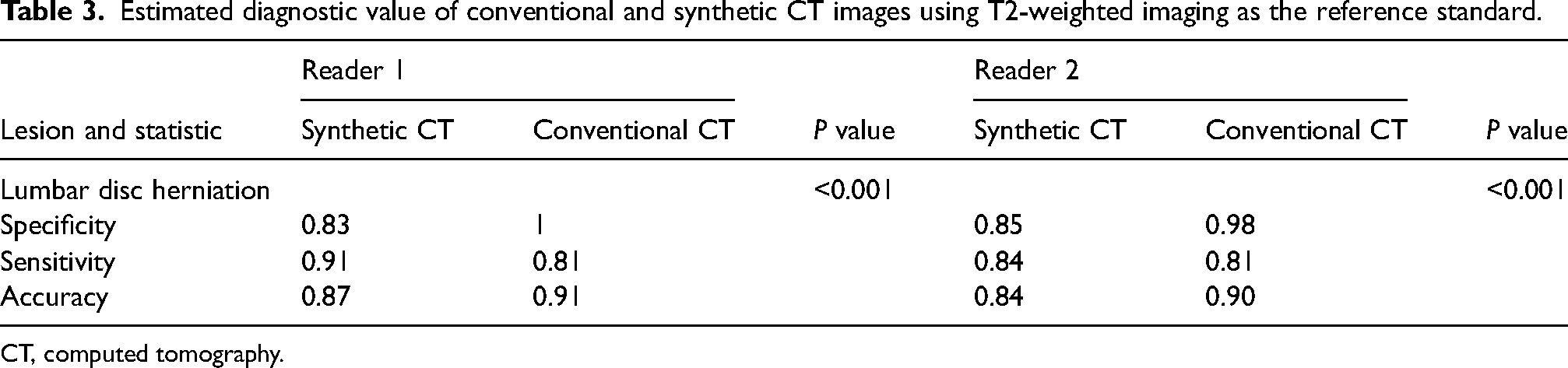
CT, computed tomography.
Discussion
The aim of the present study was to compare the diagnostic value of sCT with that of conventional CT images for patients with suspected lumbar disc herniation. sCT exhibited better sensitivity for the diagnosis of lumbar disc herniation than did conventional CT. However, its specificity and accuracy were slightly inferior to that of conventional CT. The respective inter- and intra-observer reliabilities for sCT and CT were comparable for vertebral body delineation. Conventional and synthetic CT images showed moderate consistency for delineating soft tissues and depicting the intervertebral discs.
Previous studies in other anatomical locations have shown that the diagnostic value of synthetic and conventional CT images is comparable (21–24). Morbée et al. (15) reported that sCT is equivalent to conventional CT for obtaining geometric measurements of the lumbar spine. Additionally, sCT can be used in conjunction with MRI for the diagnosis and planning of surgical procedures without exposing the patient to ionizing radiation. However, Morbée et al. did not investigate the possibility of using sCT for diseases of the lumbar spine. Some studies (25,26) have compared MRI-based sCT and conventional CT for the quantitative evaluation of hip bone morphology and demonstrated good equivalence. Recent studies have explored the generation of radiograph- and CT-like images from MRI data for the diagnosis of related diseases. Jans et al. (27) found that compared to conventional T1-weighted (T1W) MRI, sCT was more effective for the diagnosis of structural lesions within the sacroiliac joint in patients with suspected sacroiliac arthritis. The same technique was applied to the lumbar spine in the present study. Gersing et al. (28) compared MRI-derived CT-like images and simulated radiographs with conventional radiographs in patients with benign and malignant bone tumors. They used 3D T1W gradient echo sequences as the basis for CT-like image generation. However, this method requires postprocessing to obtain CT-like bone contrast, and quantitative tissue parameters are not available from this method. Argentieri et al. (29) and Breighner et al. (30) showed good agreement between CT images of the spine and hips and the corresponding MRI-based CT-like images. However, their method requires specific scanning hardware that is not available in routine clinical practice. On the contrary, the sCT postprocessing based on deep learning is fully automated, does not require user input, and as an added advantage, requires only standard MRI hardware. Some studies have shown that exploiting the 3D ultrashort echo time method to generate CT-like bone contrast in the shoulder and cervical spine is associated with powerful imaging performance (31,32). However, compared with the deep learning-based method used here, the former is more prone to motion artifacts, and requires extensive supplementary MRI hardware.
Here, the comparison of the axial lumbar position on conventional and synthetic images found no statistically significant differences in overall image quality. sCT was highly consistent with conventional CT for imaging the lumbar vertebrae, which may be related to the deep learning method utilized in this study. Since the lumbar spine is a rigid structure, it does not undergo deformation easily during image conversion. Both sCT and CT possessed moderate intra- and inter-reader reliability for paravertebral soft tissue and intervertebral discs; the image quality of sCT was sufficient for the imaging diagnosis of lumbar disc herniation.
The sensitivity, specificity, and accuracy of sCT images for the diagnosis of lumbar disc herniation exceeded 80%, which proves that sCT images have the potential for application in the diagnosis of lumbar disc herniation. Moreover, sCT also demonstrated greater diagnostic sensitivity than did conventional CT. This shows that the sCT image generated by deep learning technology does not compromise the visibility of the lesions; rather, it enhances it. In addition, MRI-based sCT eliminated the need for conventional CT scans, which potentially reduces patient radiation exposure and simplifies the diagnostic workflow. This study generated corresponding sCT images from standard T2W MR images using deep learning, a method that is distinct from other studies based on T1W imaging (33).
The present study had some limitations. First, the comparison between axial synthetic and conventional CT images for the evaluation lumbar disc herniation was not identical to the evaluation of the intervertebral disc in present-day clinical settings. Second, patient selection may have impacted the results because all participants were referred by tertiary hospitals, and a control group comprising healthy individuals was not used for comparison. Third, our study estimated diagnostic accuracy based on populations with the same disease prevalence; therefore, the results are applicable only to such populations. Finally, the participants only underwent imaging with a 1.5-T scanner, which limits the generalizability of our results to a single field strength.
In conclusion, synthetic and conventional CT images showed considerable agreement in the assessment of the lumbar spine. Thus, sCT images can be useful for the diagnosis of lumbar disc herniation.
Supplemental Material
sj-zip-1-acr-10.1177_02841851231169173 - Supplemental material for Clinical feasibility of MRI-based synthetic CT imaging in the diagnosis of lumbar disc herniation: a comparative study
Supplemental material, sj-zip-1-acr-10.1177_02841851231169173 for Clinical feasibility of MRI-based synthetic CT imaging in the diagnosis of lumbar disc herniation: a comparative study by Gan Cao, Yafen Li, Shibin Wu, Wen Li, Jia Long, Yaoqin Xie and Jun Xia in Acta Radiologica
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
