Abstract
Background:
Multi-criteria decision analysis (MCDA) has been used to quantify drug harms in the United Kingdom, the European Union, Australia, and New Zealand. This paper presents the result of an MCDA conducted in Canada, with the aim of informing Canadian drug policy and contributing to public understanding of drugs’ relative harms.
Methods:
A panel composed of 20 experts from six provinces determined 16 drugs to evaluate on 16 dimensions of harm (ten representing harm to people who use the drug; six representing harm to others). At a two-day decision conference, the panel scored each drug on a scale of 0–100 for each harm criterion, then weighted the relative importance of each criterion.
Results:
This analysis of drug harms in Canada found that alcohol causes the most harm overall, with a cumulative weighted score of 79. It was followed by tobacco (45), nonprescription opioids (33), cocaine (19), methamphetamine (19), and cannabis (15). The finding that alcohol causes the most harm is consistent with the results of previous MCDA drug harm studies.
Conclusion:
These harm scores express population-level harm rather than individual-level “harmfulness.” They reflect not only a drug’s pharmacological risk profile but also the current policy context in Canada. The high score for alcohol underscores a failure to adopt policies to address alcohol-related harms, despite the known health harms and the existence of proven policy measures. More broadly, when developing drug policies, governments should consider the harm—both individual and societal—caused by drugs and by the laws and regulations that govern them.
Introduction
Most Canadians use psychoactive substances—drugs—in some form (Health Canada, 2023a, 2023c). People who use drugs report benefits including pleasure, relief of physical or psychological pain, enhanced cognitive functioning, social connection, and meaningful spiritual experiences (Boys et al., 2001; Morgan et al., 2013; Müller et al., 2023). However, the use of drugs is also associated with a range of individual and societal harms. Their net impact in Canada includes approximately 74,000 drug-attributable deaths and nearly $50 billion CAD in social costs annually (Canadian Substance Use Costs and Harms Scientific Working Group, 2023).
The stated objective of Canada’s national drug strategies has generally been to prevent, reduce, or mitigate harms associated with drug use (DeBeck et al., 2009; Health Canada, 2023b; Single, 1995). Addressing harm first requires knowledge of the harms that are occurring. One method to assess drug harms is multi-criteria decision analysis (MCDA), a structured group decision-making technique designed to address complex issues characterized by multiple datasets and conflicting policy objectives. It was first used to systematically quantify drug harms by Nutt et al. (2010) in the United Kingdom. Since then, MCDA has been increasingly recognized as a valuable tool for developing evidence-informed drug policy, and the UK study has been replicated in the European Union (Van Amsterdam et al., 2015), Australia (Bonomo et al., 2019), and New Zealand (Crossin et al., 2023). This paper presents the results of an MCDA quantifying drug harms in Canada. Its aim is to inform Canadian drug policy and contribute to public understanding of drugs’ relative harms.
Methods
Study Design
This study is a multi-criteria decision analysis of drug harms in Canada, based on the methodology developed by Nutt et al. (2010) for their analysis of drug harms in the United Kingdom. MCDA is an analytical method designed to aid decision-making in the context of multiple, competing criteria. It provides a process in which a group of experts can identify relevant criteria, determine their relative importance, and use these elements to appraise and evaluate different options (Marsh et al., 2017). Its inputs are a combination of empirical data and subjective—but informed—judgment (Phillips, 2017).
This study was conducted in three stages: (1) establishment of an expert panel; (2) development of the list of drugs and harm criteria and their definitions; and (3) the “decision conference” at which the MCDA was conducted.
Expert Panel
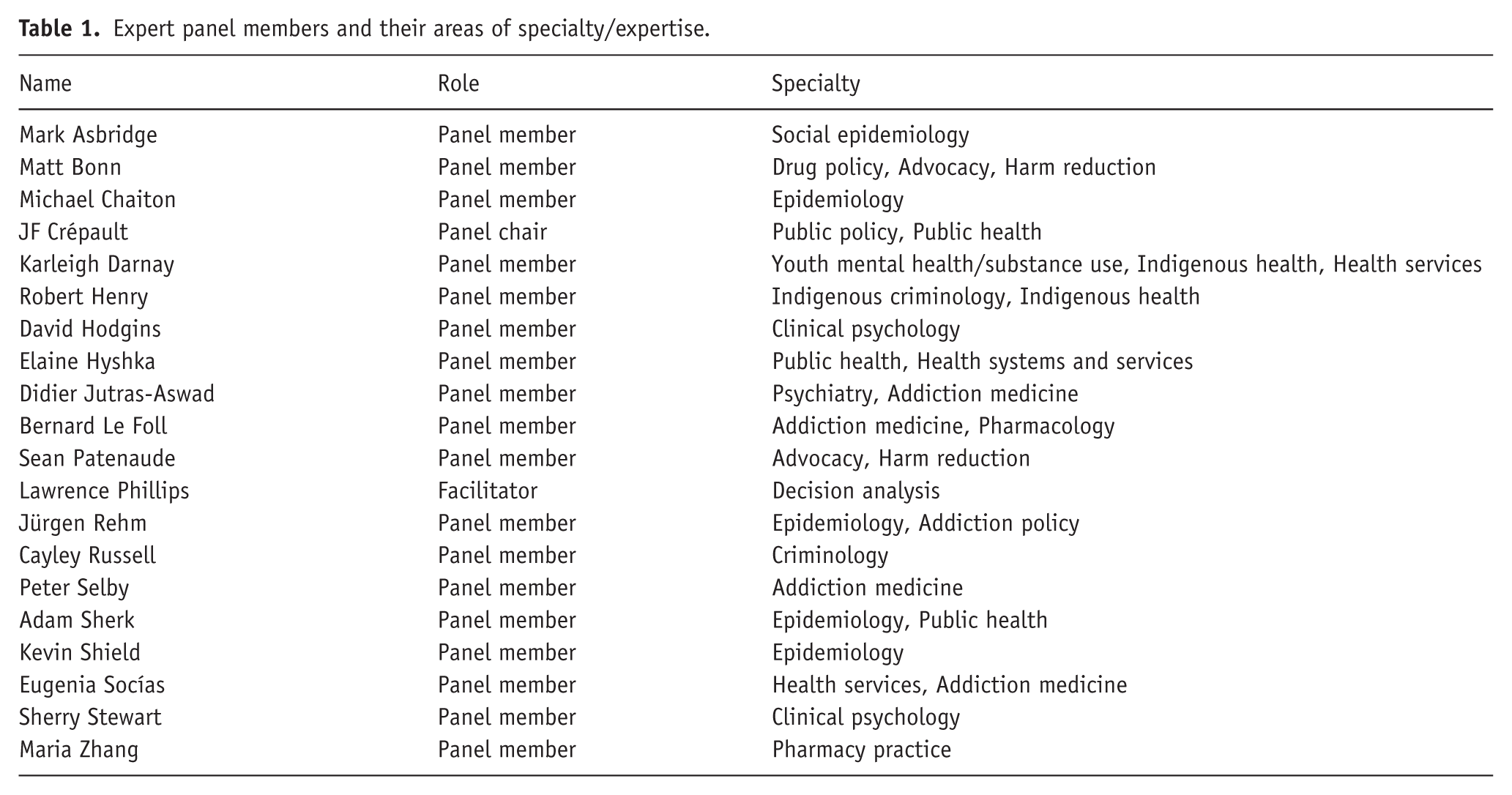
Three co-investigators (JFC, JR, CR) established a multidisciplinary panel of experts from across the country. Expert knowledge is the basis of MCDA, and the coinvestigators approached potential members with a mix of expertise, including clinical, research, and lived experience. The panel was composed of 20 experts from six provinces (see Table 1). All had significant professional experience with substance use, and some disclosed lived experience as well. A variety of disciplines and sectors were represented; the most common specialties were addiction medicine and epidemiology.
Expert panel members and their areas of specialty/expertise.
Drugs and Harm Criteria
The coinvestigators collaborated with two main authors of the original UK study (DN, LP) to adapt its list of drugs and harm criteria to the Canadian context. A preliminary list was proposed to the expert panel and refined based on its feedback. The expert panel made additional changes during the decision conference itself.
The final list of 16 drugs is shown in Table 2. Drugs included in some of the previous studies but excluded from this one, due to very low prevalence in Canada, include kava, khat, mephedrone, and nitrous oxide (see Supplemental Material). Though defining drugs is generally straightforward, nonprescription opioids present a unique challenge. Canada is in the midst of a drug toxicity crisis (Public Health Agency of Canada, 2025). While this crisis is most closely associated with fentanyl, nonprescription opioids in Canada typically contain unregulated fentanyls as well as other unregulated psychoactive drugs that amplify opioids’ effects—often other synthetic opioids, benzodiazepines, and veterinary tranquilizers (Russell et al., 2023). While the present study was intended to evaluate individual drugs separately, and fentanyl and its analogs could, in theory, be evaluated, unregulated “opioids” are an ever-changing cocktail of drugs. For that reason, the panel decided to evaluate nonprescription opioids as defined in Table 2.
Drugs evaluated by the expert panel.

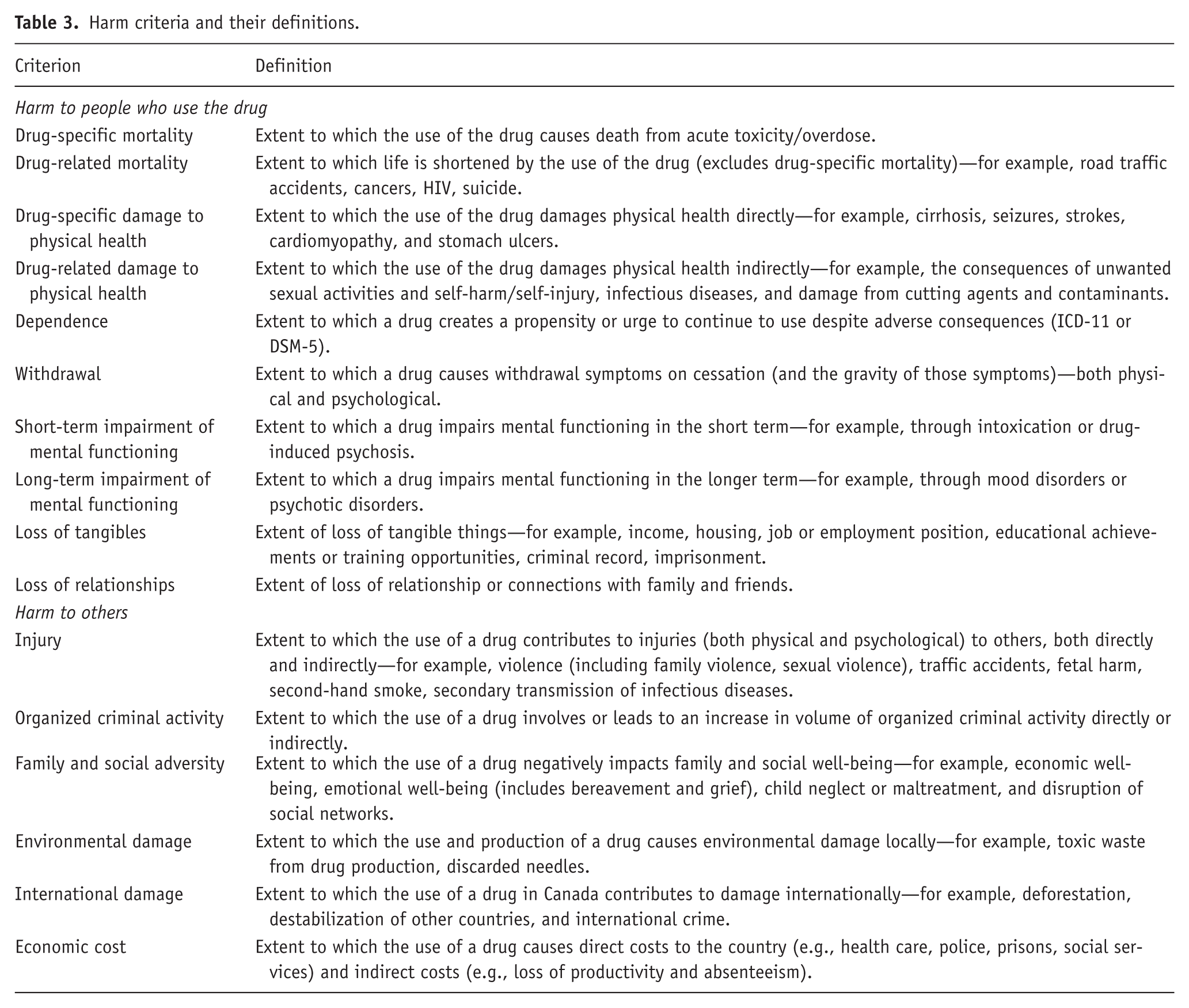
The final list of 16 harm criteria is shown in Figure 1, with definitions in Table 3. They are organized by harms to people who use drugs (“harm to users”) and harms to others, and grouped under physical, mental, and social effects. While the present study began with the original UK harm criteria, the expert panel adopted some minor modifications made by the New Zealand study team (Crossin et al., 2023), and additional changes were made to adapt them to the Canadian context (see Supplemental Material for a detailed comparison). The most substantial changes were cutting one harm criterion that the panel deemed redundant (“Community: Extent to which the use of a drug creates decline in social cohesion and decline in the reputation of the community”), and adding one that the panel decided was missing (“Withdrawal: Extent to which a drug causes withdrawal symptoms on cessation (and the gravity of those symptoms)–both physical and psychological”).
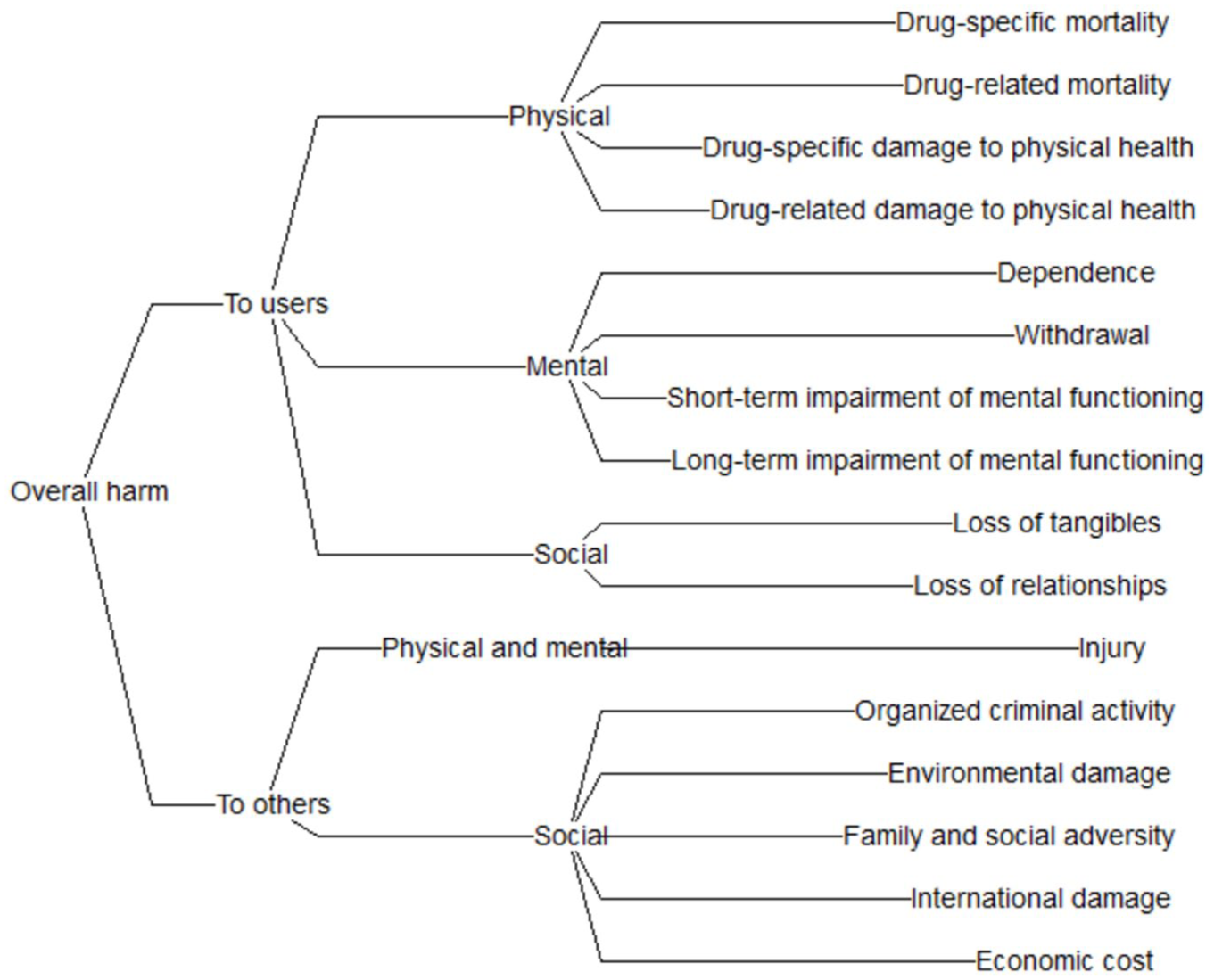
Harm criteria organized by harm to users and harm to others, and clustered under physical, mental, and social effects.
Harm criteria and their definitions.
Decision Conference
The decision conference was held on November 10–11, 2024 in Toronto, Ontario, with all expert panel members physically present. It was informed by certain premises and assumptions, which were discussed by the panel ahead of time and confirmed at the decision conference itself: (1) We were to capture population-level/aggregate harm, not individual-level harm; that is, how much harm a drug does overall rather than how harmful it is, or might be, to an individual; (2) Some of the drugs under consideration may be used medically/therapeutically, but we were only to consider non-medical use; (3) Though polysubstance use is common, we were to consider each drug independently; (4) We were to focus on the harm that would be expected when an “average” person uses a drug through the most common route of administration.
Through open discussion, the expert panel collectively scored each drug on each harm criterion, then weighted the relative importance of each criterion. Scores and weights were entered and calculated using HiView3, an MCDA software program (Catalyze, 2008). These operations were projected onto a screen so that panel members could see and discuss them in real time.
Scoring
Drugs were scored on each harm criterion using a standard scaling technique in which the drug determined by the panel to be causing the most harm on a given criterion was assigned a score of 100, with a score of zero reserved for no harm. Then, all remaining drugs were scored within those limits such that differences in the numbers represented ratios of differences in harms. For example, scoring Drug A at 100 and Drug B at 50 would indicate that Drug A causes twice as much harm as Drug B. This process was informed by panel members’ expertise as well as objective evidence brought forward for discussion (e.g., the number of emergency department visits or motor vehicle collisions attributable to a particular drug). The panel’s scoring considered both the relative severity of the harms and the number of people who use the drug, the latter mainly with reference to the most recent Canadian Alcohol and Drugs Survey (Health Canada, 2023a) and Canadian Tobacco and Nicotine Survey (Health Canada, 2023c), which report prevalence of use among Canadians aged 15 years and older—though for some illegal drugs with no official data, the expert panel estimated prevalence (see Supplemental Material). Accounting for prevalence across all harm criteria (not only harm to users) is both a departure and a natural progression from the previous drug harm studies, as the more recent ones have attempted to address a key criticism of the initial study: its combination of individual- and population-level harm criteria (Caulkins et al., 2011; Rolles and Measham, 2011). 1 As a result of this change, the harm scores in the present study express total/aggregate/population-level harm rather than individual-level “harmfulness.”
Weighting
The most harmful drug for each criterion was assigned a score of 100, but those maximum scores do not necessarily represent the same extent of harm across different criteria. The expert panel used swing weighting to make comparative judgments about the extent of harms for the 16 criteria and, separately, how much they matter relative to each other. Weights were first assessed within harm criteria groupings, comparing the harm on one 0–100 scoring scale with the “swing” from 0 to 100 on another scale. For example, weights were assessed for the four harm criteria under the grouping “physical harms to users” (see Figure 1). The expert panel compared the drugs that scored 100 for these four criteria and judged that drug-related mortality was most important, assigning it a score of 100. The other three criteria were assigned lower scores that represented ratios of differences in harms. This process was repeated for the groupings themselves (e.g., physical, mental, and social), and finally, the “harm to users” category was assessed against “harm to others.” A final normalization brought the sum of the final criterion weights to 100, thereby preserving the original ratios of all weights and allowing harm scores to be combined for each drug by adding their weighted scores (Nutt et al., 2010).
Results
The drugs causing the most harm in Canada overall are alcohol (79), tobacco (45), nonprescription opioids (33), cocaine (19), and methamphetamine (19). Figure 2 shows total harm scores for all 16 drugs and the separate contributions of harm to users and harm to others. Figures 3 and 4 show the contributions of each harm criterion to overall scores. Because scores are much higher for some legal drugs (especially alcohol and tobacco) than illegal ones, they are displayed separately.
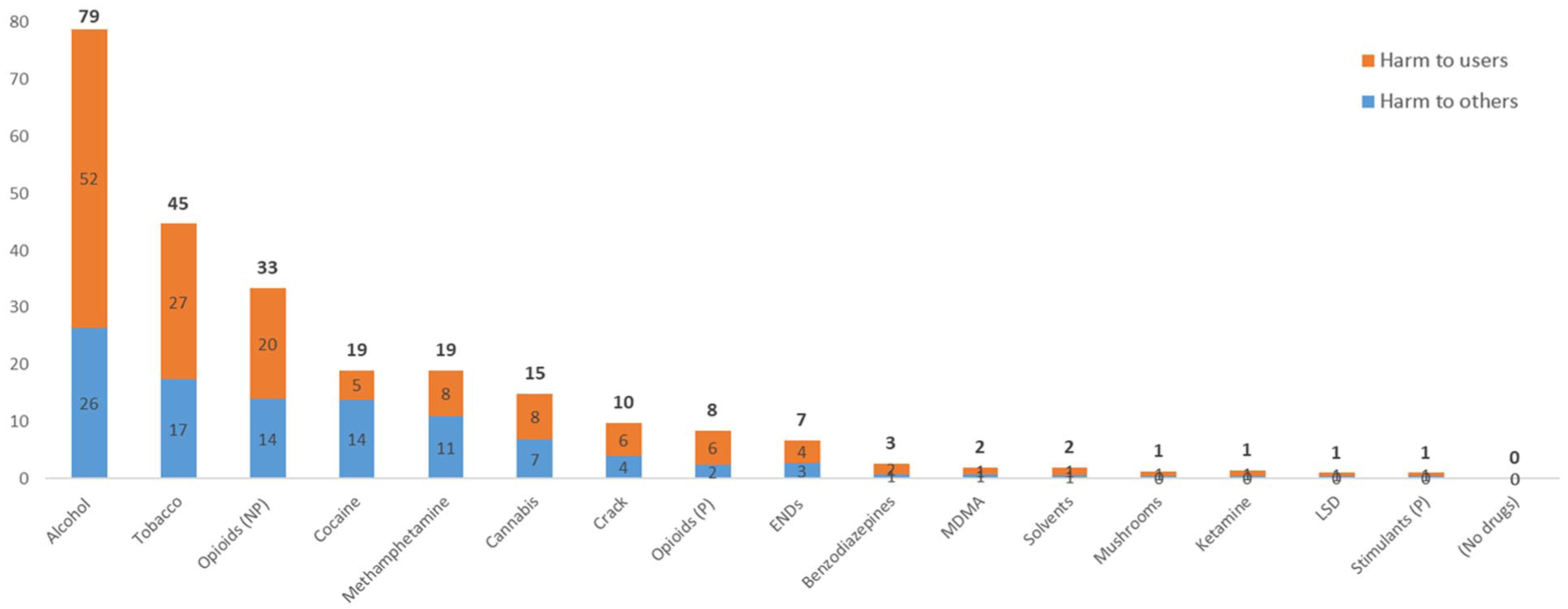
Drugs ordered by overall harm scores, showing separate contributions of harm to people who use the drug and harm to others.*
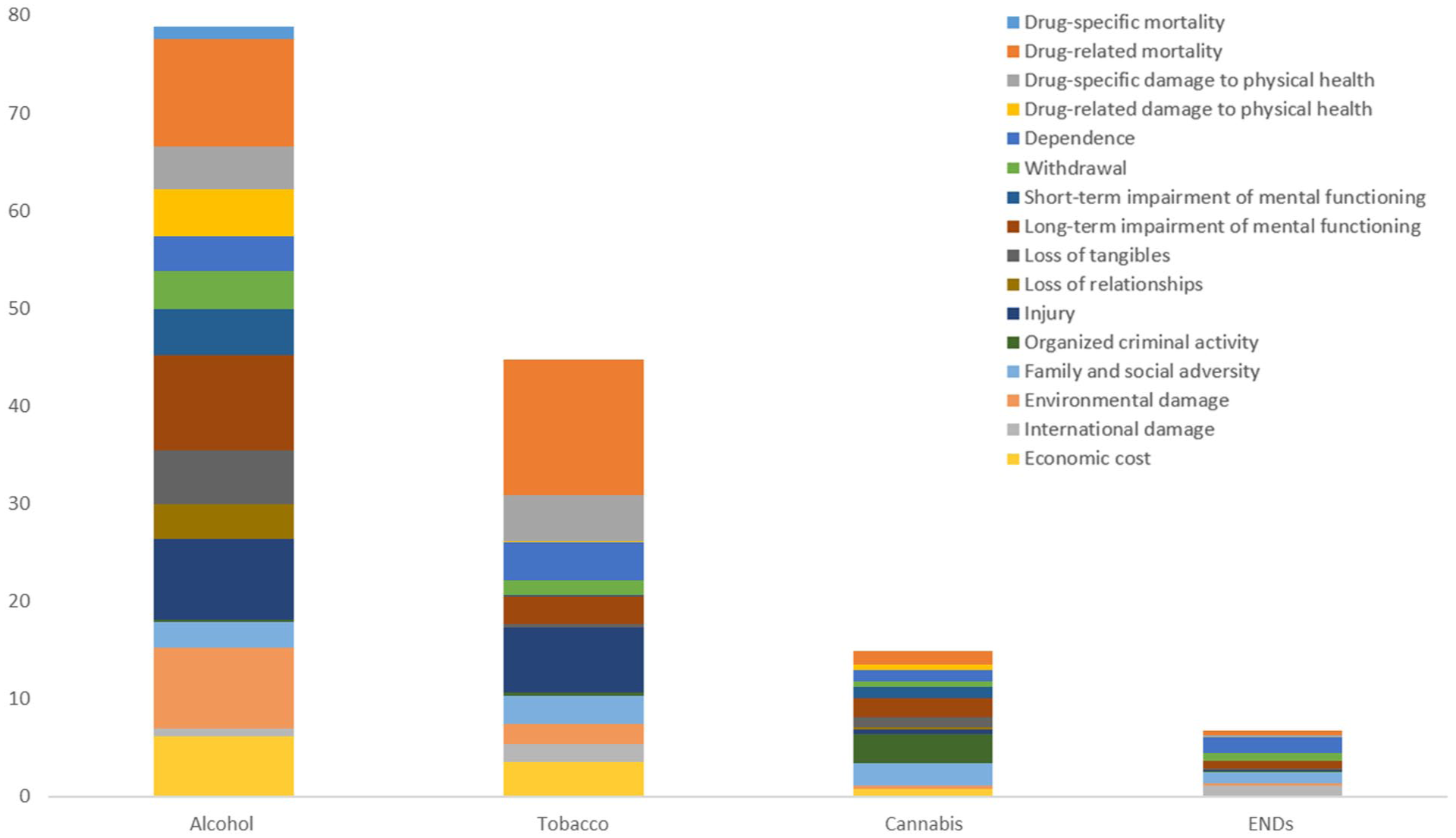
Drugs ordered by overall harm scores, showing individual criterion contributions after weighting (legal/regulated drugs only).
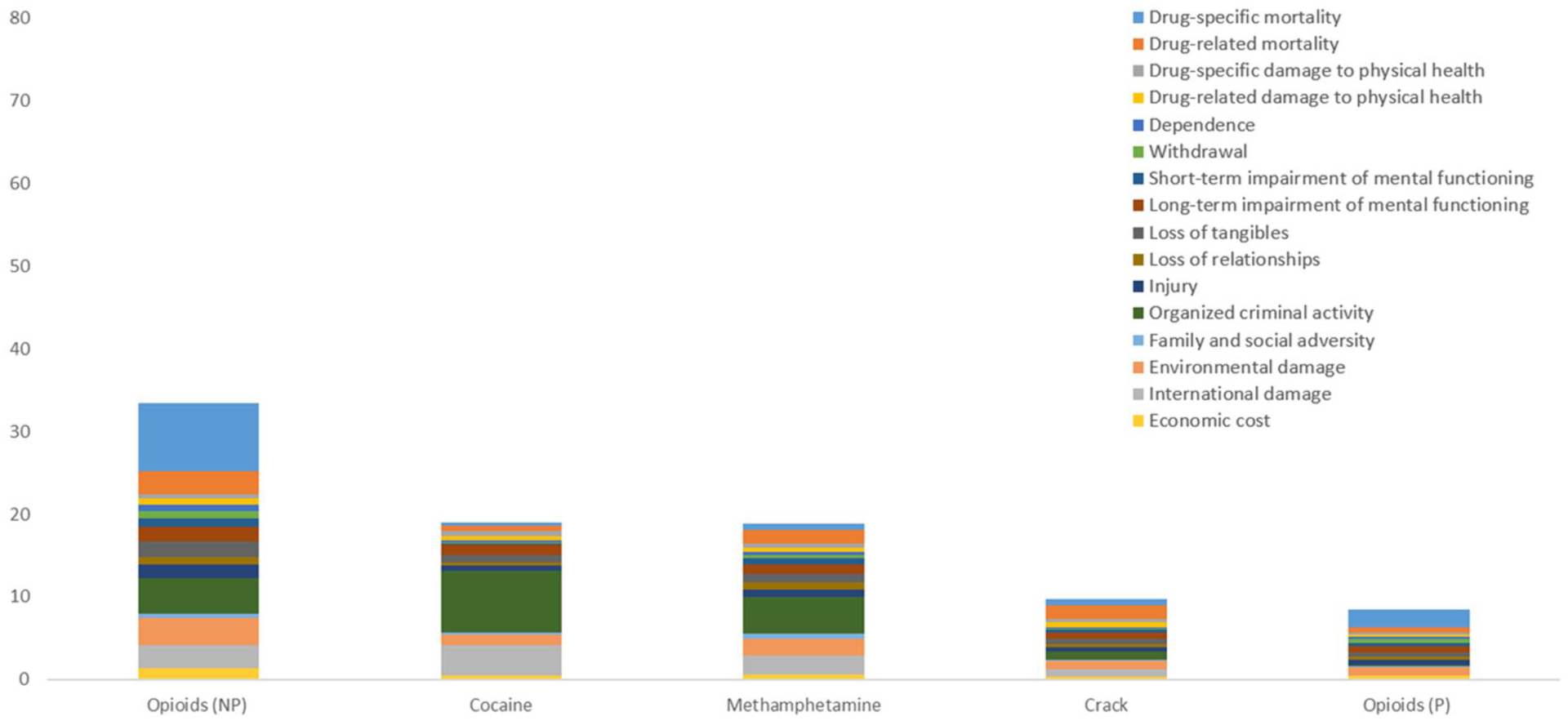
Drugs ordered by overall harm scores, showing individual criterion contributions after weighting (five highest-scoring illegal drugs).
Alcohol ranked first in 9 of the 16 harm categories: drug-related damage to physical health, withdrawal, short-term impairment of mental functioning, long-term impairment of mental functioning, loss of tangibles, loss of relationships, injury, family and social adversity, and economic cost. Alcohol has a much higher prevalence of use than other drugs; it is also associated with a variety of acute and chronic health harms and is known to have a causal role in more than 200 disease and injury conditions (Babor et al., 2023). A growing body of research suggests that there is no level of alcohol consumption that does not lead to health harms (Anderson et al., 2023; Paradis et al., 2023). Risk assessments using margin of exposure—the ratio between harmful levels of exposure and estimated normal consumption—have found alcohol to be riskier than most illegal drugs (Lachenmeier and Rehm, 2015).
Tobacco ranked first in 4 of the 16 harm categories: drug-related mortality, drug-specific damage to physical health, dependence, and environmental damage. It is responsible for a majority of drug-attributable deaths in Canada (Canadian Substance Use Costs and Harms Scientific Working Group, 2023). In addition to the well-known health harms, tobacco has a substantial negative environmental impact, from cultivation and processing to cigarette manufacturing to post-consumer waste (World Health Organization, 2022). Some studies have found nicotine to be the drug with the highest probability of causing dependence, as measured by the percentage of users who transition from use to dependence (Anthony et al., 1994; Lopez-Quintero et al., 2011). This is applicable to electronic nicotine delivery systems (ENDS) as well. ENDS were considered separately from tobacco products; two harm categories (dependence and environmental impact) accounted for nearly half of their weighted score.
Nonprescription opioids ranked first in one harm category: drug-specific mortality. Opioids directly contribute to more than 80% of drug toxicity deaths (Gomes et al., 2023). Opioid toxicity deaths usually involve unregulated fentanyl, but more than 60% of opioid toxicity deaths involve other substances, mainly unregulated stimulants and benzodiazepines (Public Health Agency of Canada, 2025). Prescription opioids were considered separately. For both types of opioids, drug-related mortality accounted for 25% of their weighted scores.
Cocaine and methamphetamine had nearly identical scores (18.98 and 18.88, respectively). They are the only two drugs with higher weighted scores for harm to others than harm to users. Cocaine ranked first in two harm categories: organized criminal activity and international damage. According to the federal government (Criminal Intelligence Service Canada, 2023), cocaine is by far the drug with which organized crime groups operating in Canada are most involved, followed by methamphetamine. While the cocaine trade has long been associated with violence, this seems to have been increasing in the past decade, with South America particularly affected (United Nations Office on Drugs and Crime, 2023). Methamphetamine ranked lower than cocaine in harms to others, but higher for almost all harms to users—especially drug-related mortality—despite having a lower use prevalence. Crack was considered separately; it had higher weighted scores than cocaine for drug-related mortality, drug-specific mortality, and short-term impairment of mental functioning—despite its use also being less prevalent than cocaine.
Cannabis’ highest weighted score was for organized criminal activity. Though more than 70% of Canadians who purchase cannabis now do so through legal sources (Statistics Canada, 2024), organized criminal groups are heavily involved in the remaining illegal cannabis market, from production to distribution (Criminal Intelligence Service Canada, 2023). Cannabis also scored relatively high for mental harms to users (dependence, withdrawal, short- and long-term impairment of mental functioning), ranking third in that combined category.
A low score does not mean that a drug causes no harm. Solvents are not widely used but cause much harm in some communities in Canada (Dell et al., 2011), and non-medical use of prescription benzodiazepines is associated with substantial adverse outcomes in some Canadian populations as well (Murphy et al., 2016). Psychedelics such as LSD, MDMA, and mushrooms can cause adverse psychological or physical symptoms (Schlag et al., 2022). For the lowest-ranked drugs, scores represent a combination of relatively lower risk and lower prevalence.
Discussion
This analysis of drug harms in Canada found that alcohol causes the most harm overall. This finding is consistent with the results of drug harm studies conducted in the UK, EU, Australia, and New Zealand, which all ranked alcohol first (Bonomo et al., 2019; Crossin et al., 2023; Nutt et al., 2010; Van Amsterdam et al., 2015). Beyond alcohol, results differ. In Canada, the drugs causing the most harm following alcohol are tobacco, nonprescription opioids, cocaine, and methamphetamine. The UK and EU ranked heroin second, while Australia and New Zealand ranked methamphetamine second. The third-ranked substances were methamphetamine in the UK and EU, heroin in Australia, and synthetic cannabinoids in New Zealand. The lower ranking of tobacco in the other studies is likely because they did not take prevalence into account when scoring harm to users. In the Australian study’s supplementary analysis incorporating prevalence, the adjusted scores moved cigarettes from fifth to second place (Bonomo et al., 2019).
Our findings are also consistent with the conclusions of the most recent Canadian Substance Use Costs and Harms study (2023), which estimated that alcohol accounts for 40% of total drug-attributable costs (healthcare, lost productivity, criminal justice, etc.), followed by tobacco, opioids, cocaine, amphetamine/methamphetamine, and cannabis. The top six rankings in that study correspond with the top six rankings in this MCDA, lending face validity to our findings.
In a commentary on the original UK drug harms study, Rolles and Measham (2011) described drug-related harm as “pharmacology translated through a complex prism of social, behavioral, and environmental variables, in turn influenced by a range of differing policy regimes, from prohibition through to legal regulation.” Indeed, the harm score for each drug reflects not only its pharmacological risk profile but also the current policy context in Canada. For example, alcohol is the most commonly used drug and is associated with a variety of acute and chronic health harms, but independent of its pharmacological properties, the way it is (or is not) regulated can cause additional harm. Alcohol’s availability, price, and promotion drive its consumption—and as population-level consumption increases, so does harm (Babor et al., 2023). Over the past two decades, governments across the country have loosened regulations to make alcohol more affordable and more available, and in many cases, these changes have been associated with increases in deaths, hospitalizations, and economic costs (Giesbrecht and Myran, 2024). In the case of illegal drugs, prohibition impacts how people use them, encouraging risky practices like using alone (which increases the risk of mortality) or sharing equipment (which increases the risk of infectious disease) (Papamihali et al., 2020). It also impacts the production chain of the drugs themselves, creating an unregulated supply in which the content, quality, and potency of drugs are variable and not readily known (Csete et al., 2016). The consumption of opioids, cocaine, and methamphetamine comes with inherent pharmacological risks, and while those risks are reflected in this study’s harm scores, so are the external factors influencing the composition of the drug supply and the consumption patterns of people who use them.
Several limitations of MCDA have been outlined by the authors of the first drug harm ranking studies (Nutt et al., 2010; Van Amsterdam et al., 2015) and their critics (Caulkins et al., 2011; Rolles and Measham, 2011). This study only considers harms and does not account for any benefits a drug may have at the individual or societal level. It does not account for individual differences: drug harms differ depending on the person, the setting, the route of administration, and many other factors, and this study does not shed light on those elements. Since this analysis focuses on the general population aged 15+, it does not provide insight into the harms to youth or specific sub-populations. It does not consider medical/therapeutic use or polydrug consumption. Importantly, it rests on the current state of knowledge and experience. Many questions remain unanswered about the harms associated with some drugs, and even the prevalence of some drugs remains unclear; the expert panel had to generate its own prevalence estimates for some illegal drugs due to the lack of objective prevalence data. There are also important regional differences in drug markets and drug use patterns. For example, drug poisoning deaths are decreasing in western and central Canada but increasing in the east of the country (Fischer et al., 2025). Expert panel members also noted that crack is common in Ontario, Québec, and the Maritimes but much less so in western Canada; conversely, methamphetamine appears to be much more common in the Prairies and British Columbia than in most of eastern Canada (O’Keefe-Markman et al., 2022). Some members of the panel felt that our prevalence estimate for methamphetamine was too low. Increasing it would have moved methamphetamine into fourth place in the rankings, above cocaine. And finally, the decision to account for prevalence limits this drug harm study’s comparability to the ones that came before it. However, this change addresses a key methodological criticism of the previous studies; further, we believe it makes the present rankings more policy-relevant, because public policy—including health policy—is designed based on desired aggregate outcomes and evaluated against aggregate indicators (Kingdon, 1984; Rose et al., 2008). Total harm is thus more relevant to policymakers than individual-level harmfulness.
Conclusion
This study is the first to apply MCDA to quantify drug harms in Canada. It evaluated 16 drugs on 16 dimensions of harm, generating scores representing the total (aggregate) harm caused by each drug in Canada. It found that alcohol causes the most harm overall, underscoring a failure to adopt policies to address these harms, despite the existence of proven interventions (Crépault et al., 2024; Rehm et al., 2023). Alcohol was followed by tobacco, nonprescription opioids (like fentanyl), cocaine, methamphetamine, and cannabis. Harm scores for each drug reflect not only their pharmacological risk profile but also the current policy context in Canada.
MCDA could be used to shed further light on how drugs impact specific populations (e.g., the New Zealand drug harms study (Crossin et al., 2023) developed separate rankings for youth) or to draw out differences within drug categories (e.g., particular cannabis products or specific opioids). Future research could also attempt to incorporate drugs’ benefits. In the meantime, when developing drug policies, governments should consider the harm—to the individual and to society—caused by drugs and by the laws and regulations that govern them.
Supplemental Material
sj-docx-1-jop-10.1177_02698811251409147 – Supplemental material for Drug harms in Canada: A multi-criteria decision analysis
Supplemental material, sj-docx-1-jop-10.1177_02698811251409147 for Drug harms in Canada: A multi-criteria decision analysis by Jean-François Crépault, Cayley Russell, Mark Asbridge, Matthew Bonn, Michael Chaiton, Karleigh Darnay, Robert Henry, David C. Hodgins, Elaine Hyshka, Didier Jutras-Aswad, Bernard Le Foll, Sean Patenaude, Peter Selby, Adam Sherk, Kevin D. Shield, M. Eugenia Socías, Sherry H. Stewart, Maria Zhang, Farihah Ali, Rose Crossin, Lawrence Phillips, David Nutt and Jürgen Rehm in Journal of Psychopharmacology
Footnotes
Acknowledgements
The authors wish to thank Shannon Lange for her assistance in the early planning of the project.
ORCID iDs
Author Contributions
Conceptualization: Crépault, Crossin, Nutt, Phillips, Rehm, Russell. Methodology: Crépault, Nutt, Phillips, Rehm, Russell. Software: Phillips. Validation: Crépault, Nutt, Phillips, Rehm, Russell. Formal analysis: Crépault, Phillips. Investigation: Asbridge, Bonn, Chaiton, Crépault, Darnay, Henry, Hodgins, Hyshka, Jutras-Aswad, Le Foll, Nutt, Patenaude, Phillips, Rehm, Russell, Selby, Sherk, Shield, Socías, Stewart, Zhang. Data curation: Crépault, Phillips. Writing – original draft: Crépault. Writing – review & editing: Ali, Asbridge, Bonn, Chaiton, Crépault, Crossin, Darnay, Henry, Hodgins, Hyshka, Jutras-Aswad, Le Foll, Nutt, Patenaude, Phillips, Rehm, Russell, Selby, Sherk, Shield, Socías, Stewart, Zhang. Visualization: Crépault, Phillips. Supervision: Rehm. Project administration: Crépault, Russell. Funding acquisition: Rehm.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors acknowledge funding from the Ontario Node of the Canadian Research Initiative in Substance Matters (CRISM) through the Canadian Institutes for Health Research (CIHR) (grant #REN-181677) and from a CIHR Planning and Dissemination Grant – Institute Community Support (PI: Dr. Shannon Lange; grant #PCS-197316). David C. Hodgins’ position at the University of Calgary is partially supported by funding from the Alberta Gambling Research Institute. Elaine Hyshka’s research is supported in part by funding from the Canada Research Chairs Program, in the form of a Canada Research Chair in Health Systems Innovation. Bernard Le Foll is supported by CAMH, Waypoint Centre for Mental Health Care, a clinician-scientist award from the department of Family and Community Medicine of the University of Toronto and a Chair in Addiction Psychiatry from the Department of Psychiatry of University of Toronto. Didier Jutras-Aswad holds a senior clinical research scholar award from the Fonds de Recherche du Québec – Santé. Sherry H. Stewart is supported through a CIHR Tier 1 Canada Research Chair in Addictions and Mental Health at Dalhousie University. The funding sources had no role in the design of this study, nor its execution, analyses, or interpretation of data.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Bernard Le Foll has obtained funding from Indivior for a clinical trial sponsored by Indivior. He has in-kind donations of placebo edibles from Indivia. He has obtained industry funding from Canopy Growth Corporation (through research grants handled by the Centre for Addiction and Mental Health and the University of Toronto). He has participated in a session of a National Advisory Board Meeting (Emerging Trends BUP-XR) for Indivior Canada and is part of Steering Board for a clinical trial for Indivior. He has been consultant for Shinogi and ThirdBridge. He is part of a scientific advisory board for NFL Biosciences. He received travel support to attend an event by Bioprojet. Didier Jutras-Aswad received study materials from Cardiol Therapeutics for a clinical trial funded by the Québec Ministry of Health and Social Services (2022–23). David Nutt via Imperial College London has received research support from the following entities with an interest in the psychedelic space: Compass Pathways, Usona, Beckley Psytech and Multidisciplinary Association for Psychedelics (MAPS). He is a paid member of the management team as part-time chief research officer for Awakn Life Sciences, a biotech company that is developing novel ketamine and MDMA therapies, and also advises Alvarius, Algernon Pharmaceuticals and Neural Therapeutics. He is an unpaid ambassador for Mind Medicine Australia and teaches unpaid on their training course. Peter Selby reports receipt of research support from Pfizer Inc. He reports that through an open-tender process, Johnson & Johnson (now Kenvue), Haleon, and Pfizer Inc. are vendors of record for having provided smoking cessation pharmacotherapy for research studies at free or discounted rates. M. Eugenia Socías has received partial support from Indivior’s Investigator-Initiated Study programme. Sherry H. Stewart acknowledges that she has received grant funding in the past from the Alcoholic Beverage Medical Research Foundation. All of the above pertain to activities outside of and unrelated to the current study.
Supplemental Material
Supplemental material for this article is available online.
