Abstract
Gender-based violence (GBV), including intimate partner violence and sexual assault, continues to be a pervasive public health issue globally and in South Africa. One-stop centre (OSC) models have emerged internationally as integrated approaches to service delivery, designed to reduce secondary victimisation and improve access to coordinated medical, legal and psychosocial support for survivors. South Africa’s Thuthuzela Care Centres (TCCs) reflect a local adaptation of this model. However, implementation across provinces is uneven, and minimum service standards are not consistently applied. This systematic review aimed to assess the evidence from low- and middle-income countries (LMICs) on OSC models for GBV response to inform the refinement of minimum standards within the South African TCC framework. A systematic search of five electronic databases (MEDLINE, PubMed, Scopus, CENTRAL, EBSCOhost and Google Scholar) was conducted to identify peer-reviewed articles published between 2010 and 2021. The search strategy was informed by PRISMA 2020 guidelines. Narrative synthesis was conducted, using both preliminary synthesis and thematic analysis. A total of 10 studies met the inclusion criteria. Six were conducted in African countries and four in Asia. Most studies focused on the evaluation of existing OSC models (n = 5) or the implementation of OSC services (n = 4), with one study examining provider responses to GBV. Three major themes emerged from the synthesis: (1) strategies that enable optimal engagement with OSC models; (2) systemic and contextual barriers to access and implementation; and (3) the role of trust and relational agency in survivor–provider interactions. The findings demonstrate that while OSC models offer a promising framework for integrated GBV care, their effectiveness is mediated by relational, institutional and contextual factors. This review supports the need for national guidelines that incorporate survivor-centred principles, cross-sectoral collaboration and relational care practices to ensure equitable and effective service provision.
Keywords
Introduction
Gender-based violence (GBV) is widely recognised as a critical public health concern, both globally and within South Africa, affecting approximately one in every three women during their lifetime (Hicks, 2021; World Health Organization (WHO), United Nations Population Fund (UNFPA) and United Nations High Commissioner for Refugees (UNHCR), 2019). Despite this recognition, victims of GBV continue to face numerous barriers that hinder their willingness and ability to disclose their experiences. These barriers include secondary victimisation, societal stigmatisation, limited awareness of available support programmes and inadequate responses from law enforcement agencies (Muluneh et al., 2020). Collectively, these factors contribute to GBV being described as a ‘hidden pandemic’ (Muluneh et al., 2020).
In response to the shortcomings of traditional, non-integrated approaches to supporting victims of sexual violence, the One-Stop Centre (OSC) model has emerged globally as a more effective, integrated service provision approach for the treatment and care of rape survivors (Colombini et al., 2011; Olson et al., 2020). The OSC model is usually characterised as an interprofessional, health system-based intervention that delivers survivor-centred health services in conjunction with a combination of social, legal, police and/or shelter services. It aims to support survivors of intimate partner violence (IPV) and/or sexual violence (SV) through a coordinated, accessible and holistic response (Olson et al., 2020).
Building on the global shift towards integrated models of care, South Africa has adopted a context-specific response in the form of Thuthuzela Care Centres (TCCs) in line with the One-Stop Centre (OSC) model. TCCs reflect an interprofessional and multi-sectoral approach tailored to the local context. As outlined in the National Strategic Plan on Gender-Based Violence and Femicide, addressing the scourge of GBV in South Africa requires the collaborative engagement of government, civil society and other stakeholders (Department of Women, Youth and Persons with Disabilities (DWYPD), 2020). The National Prosecuting Authority (NPA) initially established TCCs with the primary aim to reduce secondary victimisation, increase conviction rates and expedite case resolution for survivors of sexual violence (National Prosecuting Authority (NPA), 2019; Vetten, 2015). These centres’ aspirational aim is to serve as a ‘one-stop shop’ providing access to psychosocial, health and legal services within a survivor-centred and dignified environment, thereby localising the principles of the OSC model within the South African justice and healthcare systems. The maturation of the TCCs as a response model for crisis and one-stop management of sexual violence has been hailed as a best-practice model of service delivery and has brought about an expanded mandate to include other forms of gender-based violence, such as domestic violence (https://www.gov.za/TCC). Since the expanded mandate, TCCs include working with the South African Police Services Family Violence Units and provide referrals to sheltering options (Dlamini, 2024).
While the TCCs are considered well-functioning on a national scale in South Africa, due to the distinct contexts within and across provinces, the quality and extent of care received by victims vary within and across provinces (Foundation for Professional Development (FPD), 2016). For example, while the TCC Blueprint (see Figures 1 and 2) specifies a suite of services that should be available to victims, there are instances where not all services are provided according to this TCC Blueprint (Foundation for Professional Development, 2016). Furthermore, due to the multi-sectoral nature of the TCC model, coordination and cooperation between stakeholders are challenging. Stakeholders do not share an equal commitment to the quality of services (Foundation for Professional Development, 2016). The multi-sectoral approach attempts to juggle the interests of multiple sectors, which contribute to the increased complexity of services provided to victims within the TCC sector (Vetten, 2015).

TCC blueprint.
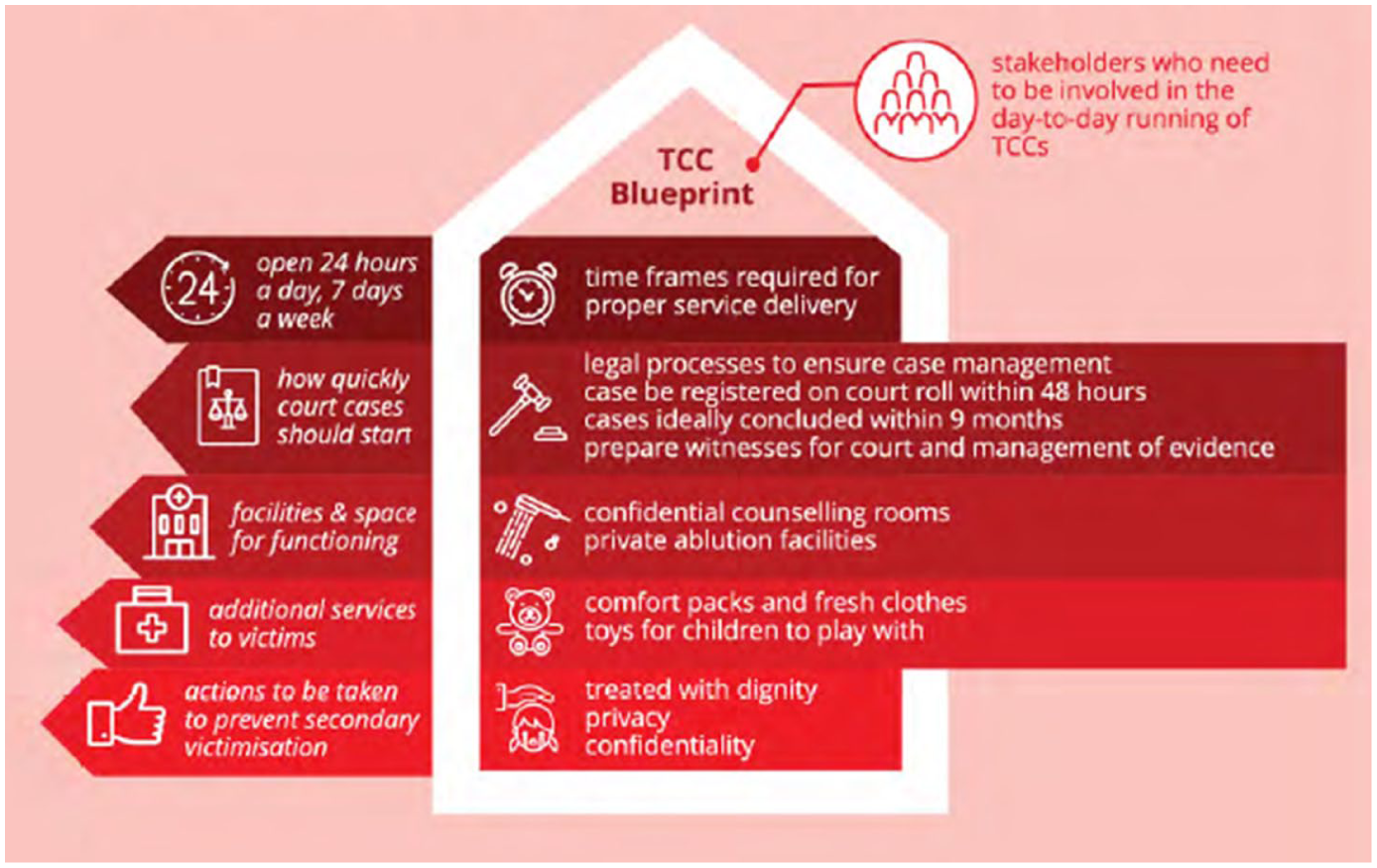
TCC blueprint (cont).
As discussed above, the TCCs in South Africa are based on a one-stop centre (OSC) model that enables the integration of multiple stakeholders to support survivors of sexual violence. However, this multi-stakeholder approach introduces several challenges that may affect accessibility, coordination and overall quality of care. In response, this systematic review aims to examine evidence on the implementation and delivery of OSC models in low- and middle-income countries (LMICs), with the goal of informing service enhancement within the South African TCC framework. To our knowledge, only one prior review (Olson et al., 2020) has focused specifically on the enablers and barriers to OSC implementation in LMICs. However, no review to date has comprehensively examined the operational elements of OSCs, such as roles and responsibilities, service delivery protocols, coordination mechanisms and contextual barriers – with a specific lens on how these may inform the refinement of the TCC model.
The systematic review aimed to assess evidence from LMICs on OSC models broadly, and that findings were used to inform minimum standards for the South African TCC sector. The research questions and outcomes are:
Research questions
What models of OSC service provision exist in LMICs, and how do they function?
What elements are described in these OSC models (e.g. roles and responsibilities, service protocols, coordination and integration) that could inform the South African TCC context?
What factors enable or constrain effective implementation and delivery of services within these OSC models?
Outcomes
Identify existing OSC models in LMICs guided by minimum standards frameworks.
Understand service provision through OSC models and describe relevant elements (e.g. roles and responsibilities, protocols, integration, coordination).
Explore strategies, barriers and enablers that affect optimal engagement with the OSC model.
Methods
A systematic review was conducted to provide a structured and comprehensive synthesis of existing evidence on one-stop centre (OSC) models for gender-based violence services in LMICs. Unlike a scoping review, which maps broad areas of literature, a systematic review applies a focused approach to answering predefined research questions and assesses the quality and relevance of included studies. This review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines to ensure transparency and methodological rigour throughout the review process (Page et al., 2021). The proposal of this study was registered with PROSPERO, the International Prospective Register of Systematic Reviews (registration number: CRD42021268936; available at: http://www.crd.york.ac.uk/PROSPERO).
Eligibility criteria
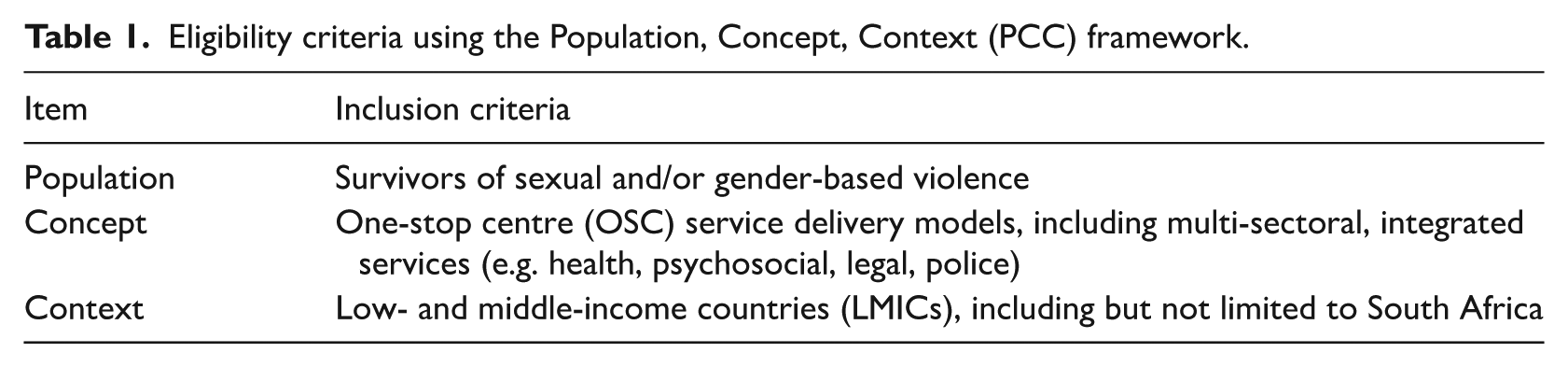
The eligibility of studies was informed by the Population, Concept, Context (PCC) framework, which helped structure the review question and guide inclusion decisions. The PCC approach ensured that selected studies were relevant to the objectives of this systematic review and provided evidence to address the review questions. The criteria are summarised in Table 1.
Eligibility criteria using the Population, Concept, Context (PCC) framework.

Search methods for identification of studies
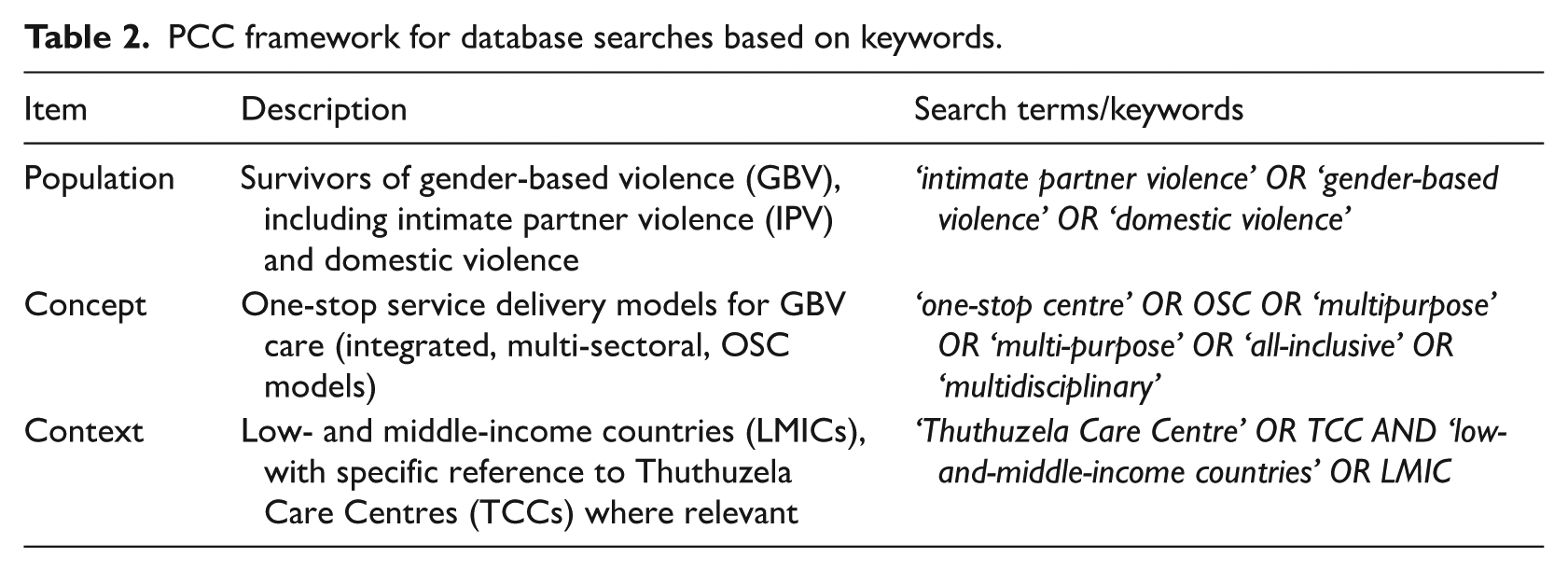
A comprehensive search strategy was developed to identify peer-reviewed research articles published between January 2010 and 2021. The search was designed in collaboration with a librarian to ensure both breadth and precision. Medical Subject Headings (MeSH) terms and relevant keywords were applied in searches of MEDLINE and PubMed. Additional databases searched included Scopus, CENTRAL, EBSCOhost and Google Scholar. EndNote X9 was used to manage references, facilitate the screening process and remove duplicate records prior to title and abstract screening. This primary search was completed by a manual search of articles cited by retrieved articles and on Google, allowing for adding additional articles (see Table 2).
PCC framework for database searches based on keywords.
Charting the data
The retrieved titles were compiled into a Microsoft Excel spreadsheet for initial screening. A three-stage selection process was employed to ensure a systematic and rigorous review. First, titles were screened for relevance by the review team (G.H., B.M., D.S.). Second, abstracts of potentially eligible studies were reviewed. Third, full-text articles were assessed for inclusion based on consensus. Screening was conducted independently at each stage. Discrepancies in title, abstract or full-text assessments were resolved through discussion among the reviewers, with a third reviewer consulted when consensus could not be reached. EndNote 20 was used to manage references and to identify and remove duplicate records. Data were extracted independently using a predefined Microsoft Excel extraction form, which was piloted on five studies to ensure clarity and consistency. Any discrepancies in the extracted data were discussed and resolved collaboratively, ensuring the reliability and accuracy of the synthesis process.
Inclusion and exclusion criteria
Studies were included if they (1) assessed integrated or multi-sectoral service provision models for sexual or gender-based violence survivors in LMICs; and (2) presented empirical evidence of coordination, delivery or integration of services aligned with the OSC model (e.g. medical, psychosocial, legal, police). Studies that were excluded focused solely on IPV screening or provider responses without a systems or service-delivery model focus.
Quality assessment
To assess the quality of the included studies, we used the Lockwood et al. (2015) critical appraisal tool developed as part of the Joanna Briggs Institute (JBI) methodology for qualitative research synthesis. This tool was selected because a significant portion of the included studies employed qualitative or mixed-methods designs, for which standard tools like AMSTAR (focused on RCTs) or ROBIS (designed for systematic reviews of interventions) are not well suited. The Lockwood tool evaluates methodological congruence between the research questions, study design, data collection and interpretation of findings.
Data extraction and synthesis
The data extraction methodology was first piloted using five studies to ensure consistency and relevance of the extraction process. Following completion of the quality appraisal, the authors independently extracted data from the included studies using a predefined Microsoft Excel data extraction form, based on the approach outlined by Lucas et al. (2007). This form captured key study characteristics, methodological features and relevant findings. Any discrepancies in extracted data were discussed and resolved through consensus to ensure accuracy and reliability. This process supported a systematic and transparent synthesis of evidence across studies.
We now reference Table 1 to guide readers to a descriptive summary of the included studies. A narrative synthesis of the findings was undertaken to provide a textual response to the review questions, integrating both qualitative and quantitative evidence. Following the approach outlined by Lucas et al. (2007), the synthesis involved two key stages: (1) preliminary synthesis and (2) thematic analysis. The preliminary synthesis included the extraction and tabulation of key study characteristics such as author names, year of publication, participants, study location and design, aims, methods appraisal, setting, sampling strategies and key findings. This table served as the basis for a textual summary of study features. Thematic analysis was then applied to identify and organise core patterns across studies, allowing the review to draw out overarching themes related to service provision, coordination, barriers and enablers within OSC models in LMICs.
Results
Search results
The initial database search yielded a total of 2,716 records. After removing duplicates (n = 2), 2,714 records were screened by title and abstract. Of these, 2,627 records were excluded for not meeting the inclusion criteria. A total of 57 full-text articles were assessed for eligibility. Following full-text screening, 47 articles were excluded for the following reasons: (1) the study did not focus on one-stop centre (OSC) models or (2) the study setting was not within a low- or middle-income country (LMIC). A total of 10 studies were included in the final review. The study selection process is reported according to the PRISMA 2020 guidelines and is illustrated in Figure 3.
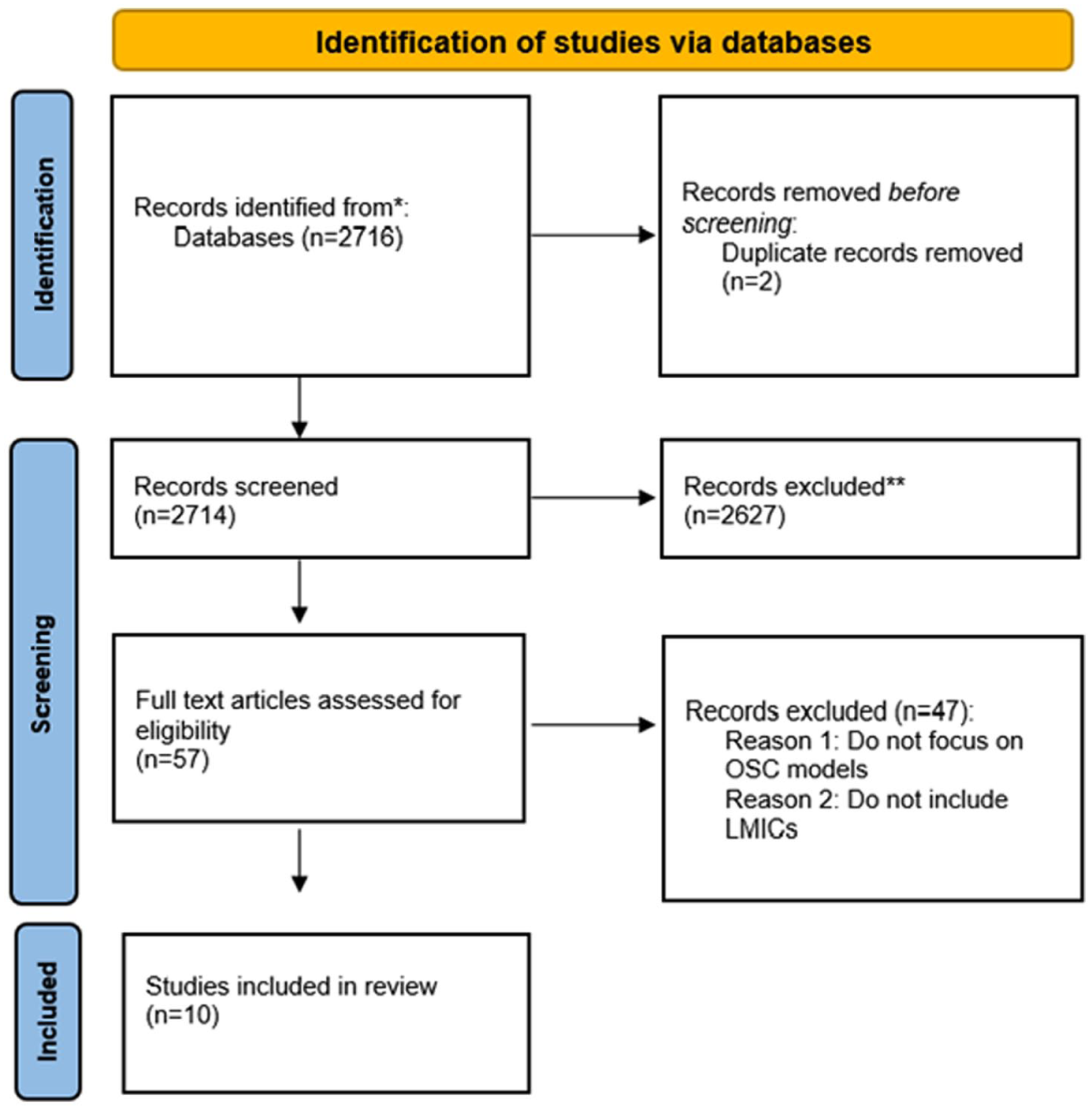
PRISMA flow diagram.
Geographical distribution of studies
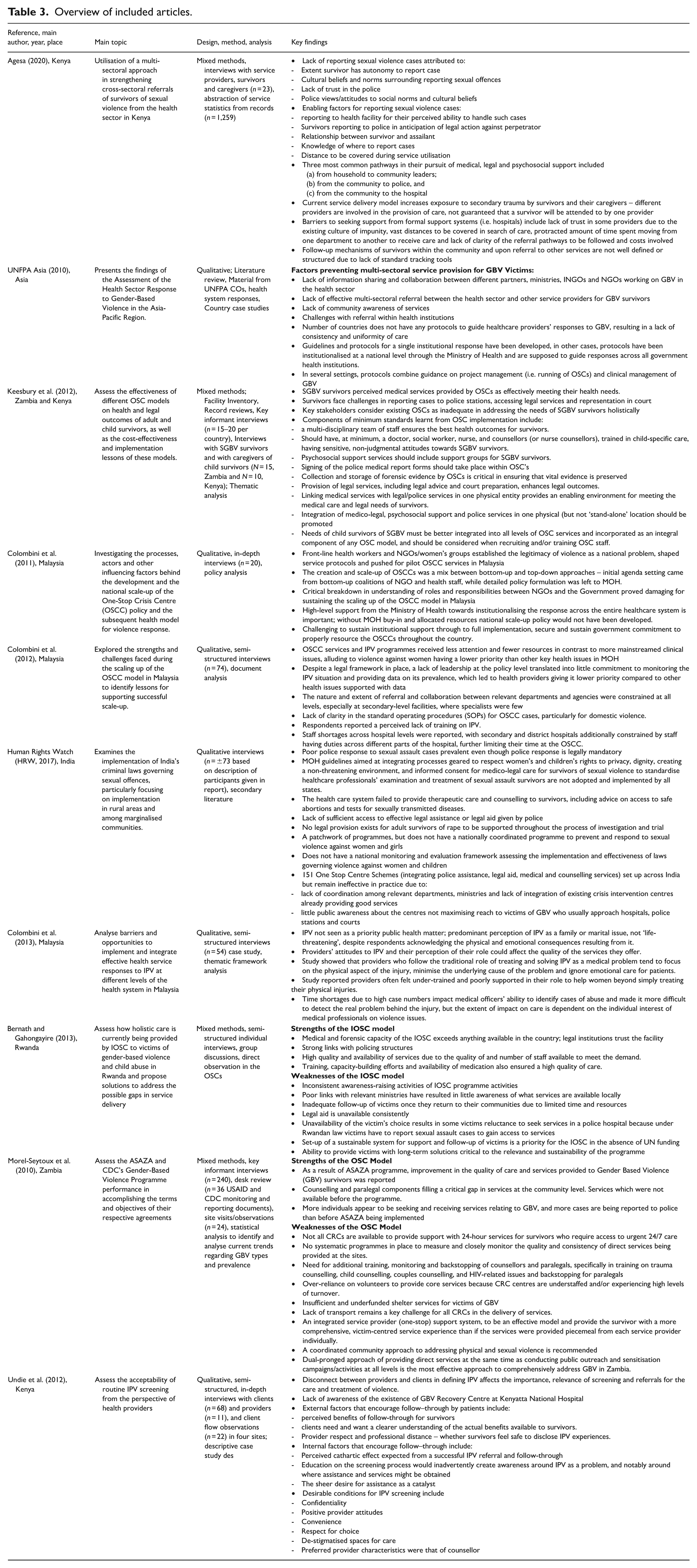
Of the 10 included studies (see Table 3), six were conducted in African countries and four in Asia. The African studies were conducted in Kenya (n = 1), Zambia (n = 1), Rwanda (n = 1) and one cross-country study involving Kenya and Zambia. The Asian studies were conducted in Malaysia (n = 3), with one study spanning multiple regions, including Asia, categorised as cross-continental.
Overview of included articles.
Main topic/s studied
The 10 studies included in this review focused on various components related to service provision for victims of sexual and gender-based violence in LMICs. Specifically, five studies focused on evaluating or assessing existing one-stop centre (OSC) models. Four studies explored the implementation of OSC services in different contexts.
While the central focus remained on OSCs, we included studies that examined multi-sectoral or partially integrated approaches where no standalone OSC existed but elements of the OSC model (e.g. coordination across health, legal, psychosocial domains) were present and documented. This was particularly necessary due to the scarcity of direct OSC studies within LMICs.
Methods/designs used
Of the 10 studies, six used qualitative methods and four employed mixed-methods designs. In terms of specific classifications, the studies included a descriptive case study (n = 1), a cross-sectional study (n = 1), a comparative case study (n = 1), a policy analysis (n = 1), a document analysis (n = 1) and a thematic framework analysis (n = 1). Several studies employed more than one methodological approach, reflecting the complexity of evaluating one-stop centre (OSC) service delivery in diverse contexts.
Synthesis of findings and thematic analysis
This section presents the thematic analysis of the 10 studies included in this systematic review. The analysis was guided by a narrative synthesis approach and structured around recurring themes that emerged from the data. These themes reflect the range of experiences, implementation strategies, barriers and enablers associated with OSC models for gender-based violence response in LMICs. The findings are presented to provide a deeper understanding of the components and conditions that shape OSC service delivery, with the aim of informing the development and refinement of minimum standards for TCCs in South Africa.
Theme 1: strategies that enable optimal engagement of the OSC model
Collaboration between healthcare workers and NGOs
As mentioned above, various strategies focused on evaluating and/or assessing existing OSCs in different LMICs. As part of their evaluations, this group of studies highlighted key strategies that enable optimal engagement of the OSC model. Two out of five studies highlight the importance and influence of collaboration between healthcare workers and NGO groups in prioritising GBV/IPV as a national priority. In Malaysia, front-line health workers and NGOs/women’s groups established the legitimacy of violence as a national problem, shaped service protocols and pushed for pilot One-Stop Crisis Centre services. Similarly, in the South African context, NGOs partnered with the government, and specifically the NPA to establish the TCCs. This pattern of collaboration has continued as integral to the growth of TCCs nationally in SA.
Linkages with policing structures, high-quality services and staff
Strong linkages with policing structures, providing high-quality services and having high-quality staff and staff capacity available to meet demand alongside training and capacity-building strategies were also reported to be key to effective OSC service delivery. For example, in Rwanda, a health-based, hospital-owned OSC model emerged as providing the best legal outcomes for survivors. The Isange One-Stop Centres medical and forensic capacity of the centre exceeds anything else available in the country, which has meant that legal institutions trust the facility. The centre is also reported to have high quality and availability of service due to the quality and number of staff available to meet the demand. Training and capacity-building efforts and the availability of medication have also ensured a high quality of care. Linkages with policing structures are central to the TCC Model. In the first TCC established in South Africa, the police were 100 m away from the health care centre which ensured communication and strengthened collaboration between the NPA, health and police services. In rural communities, it is a lot harder for police, the prosecution team and health services to work together because of the distances between services.
Integrated service provider response
In addition, providing survivors with integrated service provider response at the community level while simultaneously conducting public outreach and sensitisation campaigns/activities has also been found to be effective in Zambia. For example, a particular strength of Zambia’s programme is the way it has fully integrated local community-based public outreach, awareness and support into the core work of the ASAZA Coordinated Response Centres. Activities have included local radio talk show programmes, IEC materials, community conversations, men’s network activities, engaging with local and traditional leaders, survivor support groups, youth programmes, training local stakeholders, participation in local events, mobile clinics and training of community caregivers to provide referrals and victim support. In the larger research study, community outreach was identified as a weakness in the implementation of the TCC Model in SA.
Theme 2: systematic barriers to accessing care
Follow-up and referral pathways
The mandate of one-stop centres is for a multi-disciplinary team to respond immediately and in one location to the management and treatment of sexual violence and other forms of GBV. However, the initial service provision is only successful if the follow-up treatment is coordinated and continues to focus on the reduction of secondary trauma. Follow-up management and treatment include the investigation of the case by the local detective, as well as connecting the survivor to psychosocial support beyond the immediate crisis counselling services (that are stationed at the OSC) and then the court trial. Similarly, the TCC Model implements a referral system. In communities with many NGOs and social support services, referral is a lot smoother and external support for survivors is a lot stronger. In addition, in LICs, particularly in rural communities, the services are separated by far distances, which makes sustained referral pathways difficult and inconsistent. Many service providers reported inadequate follow-up communication and underdeveloped referral networks, compounded by a limited range of referral options available to survivors. These challenges are further exacerbated by long travel distances to access care, difficulty locating appropriate services, prolonged waiting times due to interdepartmental transfers, ambiguity surrounding referral pathways and associated costs – all of which negatively influence survivors’ willingness to engage in follow-up and referral processes.
A lack of standardised follow-up mechanisms within communities and primary healthcare centres, as well as poor inter-agency referrals, was attributed to the absence of reliable tracking tools and ineffective communication systems. For example, in Kenya, it has been noted that while verbal referrals are commonly employed by service providers, there is often no subsequent follow-up to confirm whether survivors accessed the referred services. In addition, resource constraints, limited time and inadequate multi-sectoral collaboration further hinder consistent follow-up with survivors. The absence of standardised tracking tools and the lack of coordination between providers also mean that critical information about a survivor’s care journey is often lost or fragmented. The research that this paper is based on surfaced similar challenges in the SA TCC Model. There was no clear monitoring, tracking and evaluation tool. This means that survivors are burdened with navigating multiple service points, often across long distances, at great cost and with little assistance. This increases the likelihood that they disengage from care, especially when dealing with trauma or fear.
In Malaysia, staff shortages and the multitasking of personnel across various departments were reported to constrain referral processes and interdepartmental collaboration, particularly within secondary-level facilities where specialist availability is limited. In states such as Penang and Kelantan, high caseloads were reported to reduce medical officers’ capacity to detect cases of abuse and to identify the underlying causes of injury. Notably, the effectiveness of care was often influenced by the personal interest of individual medical professionals in issues related to violence. Moreover, the unavailability of 24-hour support services posed significant limitations for survivors requiring urgent care outside of standard working hours or during weekends. The Malaysian context shows that despite the legal framework in place, a lack of leadership at the policy level has translated into little commitment to monitoring the IPV situation and providing data on its prevalence, thus leading to health providers giving it lower priority compared to other health issues supported with data.
Guidelines and/or protocols for the provision of care
The absence or inadequacy of guidelines and protocols for the provision of care has been identified as a significant barrier to effective service delivery and has compromised the quality of care for survivors of GBV. In the Asia-Pacific region, many countries lack standardised protocols to guide healthcare providers in responding to GBV. In some contexts, institutional-level guidelines have been developed, such as the protocols implemented by the Formed Police Unit in the Maldives, or those introduced as part of pilot initiatives in countries like China and Mongolia. In contrast, several other countries in the region have institutionalised national-level protocols through Ministries of Health to guide responses across public health systems.
These protocols often integrate guidance on both project management-such as the operation of One-Stop Crisis Centres and the clinical management of GBV cases. However, gaps in implementation and clarity persist. In Malaysia, for instance, there is a notable lack of clarity regarding standard operating procedures (SOPs) for handling cases, particularly those involving domestic violence. The TCC Model experiences similar challenges in implementation, while some TCCs are aware of the blueprint and supporting guidelines, other TCCs are not aware of the blueprint and accompanying guidelines for implementation and care which results in different standards of care across the TCCs.
Access to services including justice and police
A recurring theme in the literature reviewed is the limited access to effective legal assistance, legal aid and responsive police services, all of which constitute significant service-related barriers to justice for survivors of gender-based violence (GBV). In the Indian context, for example, the absence of a national monitoring and evaluation framework to assess the implementation and impact of laws addressing violence against women and children has been highlighted as a major gap. Furthermore, there are no legal provisions to ensure that adult survivors of rape receive continuous support throughout the investigation and trial process. Although the law mandates a police response in cases of sexual harassment, the actual response by law enforcement remains inadequate and inconsistent.
In contrast, Rwandan law requires that survivors report sexual assault to access services; however, this mandatory reporting requirement, which limits survivor autonomy, has been associated with reluctance among victims to seek support. Similar challenges have been documented in Zambia and Kenya, where survivors encounter difficulties in reporting incidents to the police, accessing legal services and securing legal representation in court. A pervasive lack of trust in the police has been linked to law enforcement officers’ attitudes, which are often shaped by prevailing social norms and cultural beliefs surrounding sexual violence. These attitudes contribute significantly to the underreporting of such cases.
Service providers’ attitudes, responsibilities and training towards handling IPV cases
The studies included in this review consistently demonstrate that service provider attitudes towards IPV significantly influence the quality of care delivered to survivors. In many contexts, IPV is not recognised as a public health issue and is often deprioritised by healthcare providers. This is largely due to prevailing perceptions of IPV as a private or familial matter rather than a life-threatening condition. despite its well-documented physical and psychological consequences. Consequently, negative attitudes among providers hinder the provision of comprehensive medical and psychosocial support. The degree to which care is effectively delivered often depends on individual healthcare providers’ personal interest or commitment to addressing violence-related issues.
For example, in Malaysia, providers who adopt a traditional biomedical approach to IPV tend to focus narrowly on the physical injuries while minimising the underlying causes and neglecting the emotional needs of survivors. In Kenya, the quality of provider-patient interactions, particularly the respect shown by providers and their ability to maintain professional boundaries, was identified as a key factor influencing survivors’ willingness to disclose IPV experiences and adhere to treatment plans.
A lack of formal IPV training among service providers emerged as a major barrier to effective care across multiple settings. Providers often reported feeling inadequately trained and unsupported in addressing IPV beyond treating physical injuries. In India, for instance, the healthcare system was criticised for failing to offer therapeutic services, including counselling, guidance on safe abortion and testing for sexually transmitted infections. In Zambia, there remains an urgent need for enhanced monitoring and targeted training of counsellors and paralegals in trauma, child and couples counselling, as well as in HIV-related issues. In the South African context, most of the training has been on dealing with sexual violence and not IPV which means that many staff are skilled in dealing with survivors of sexual assault but less so when dealing with survivors of IPV. Furthermore, in SA, staff are chosen to work in TCCs because of their skill in working compassionately with survivors of GBV.
This fragmented approach to care means that:
Survivors must retell their stories multiple times, which can exacerbate trauma.
Some services are unavailable at key points in time (e.g. after hours).
No single provider feels ownership of the survivor’s care journey.
Survivors are left to navigate complex systems alone, often with minimal support or understanding of what services are available or appropriate.
Coordination, integration and multi-sectoral collaboration
One of the most consistent issues across settings is the absence of effective multi-sectoral collaboration. In theory, GBV response should involve healthcare systems, law enforcement, legal aid, social welfare and community-based organisations. However, these entities often operate in silos, with little communication or coordination. In the Asia-Pacific region, UNFPA (2010) notes that poor information sharing between ministries, NGOs and INGOs working on GBV contributes to duplication, delays or complete gaps in care. In Kenya, Agesa (2020) found that survivors are often referred from one sector to another (e.g. from the community to police, or from police to hospital), but with no guarantee that information or support follows them through the system. In South Africa, even where systems are developed, nurses’ individual agency tends to compensate for the lack of institutional integration (Sprague et al., 2020).
Variability in institutional commitment and resources
Even when national or organisational protocols exist, their implementation is uneven. Some facilities may have operationalised referral guidelines, while others have not – even within the same country. The presence or absence of champions, staff training and local leadership often determines the extent of collaboration. Malaysia provides an example where staff shortages and competing demands on staff time make it difficult to coordinate responses across departments, especially in secondary-level facilities, where the need for specialist input is highest. Health providers themselves may be unaware of services outside their facility, leading to either under-referral or inappropriate referral.
Theme 3: the role of trust and relational agency
This theme underscores the foundational role of trust and relational agency in the provision of services to survivors of GBV/IPV. The review found that beyond institutional frameworks, survivors’ access to and engagement with services were profoundly influenced by the quality of their interpersonal interactions with healthcare providers. Trust emerged as a key prerequisite for disclosure and help-seeking. Survivors were more likely to disclose experiences of violence when they perceived the healthcare environment as safe, supportive and non-judgmental. In such contexts, trust facilitated open communication, enabling providers to uncover the underlying causes of injuries and offer more accurate, personalised and timely care and referrals.
Relational agency, in this context, refers to the provider’s capacity to co-construct meaning and solutions with survivors in a manner that is responsive, respectful and empowering. This extends beyond technical competence to include empathy, emotional intelligence, responsiveness to the survivor’s cues and preferences, and a deep respect for survivor autonomy and dignity. The presence of interpersonal continuity, where survivors interact consistently with the same provider, was found to be particularly valuable in fostering emotional safety. Such continuity minimises the risk of re-traumatisation by reducing the need for survivors to repeatedly recount their experiences to different professionals, thereby mitigating feelings of institutional distrust or dismissal.
Moreover, when providers foster trust, they are better positioned to deliver holistic care, including psychosocial support and appropriate referrals, and are more likely to identify indirect or non-verbal signs of abuse. Importantly, the empathetic and trusting relationships developed between survivors and healthcare providers can also enhance survivors’ own sense of agency, their ability to make decisions, seek justice and regain control. This is particularly significant in contexts where survivors often feel disempowered, stigmatised or blamed. Thus, relational dynamics are not merely supportive elements of care but are essential to the effectiveness and ethical quality of OSC service delivery.
Discussion
This review has identified several critical elements necessary for the optimal functioning of One-Stop Centres (OSCs), such as South Africa’s Thuthuzela Care Centres (TCCs), and has provided key considerations for establishing guidelines and/or a minimum standards framework for care within such facilities. Central to effective OSC service delivery is sustained high-level governmental support. The institutionalisation of care for survivors within the broader healthcare system requires political will, resource allocation and policy alignment.
Consistent with Olson et al. (2020), our findings reaffirm the central role of sustained high-level governmental support. The institutionalisation of survivor care within the health system requires political will, stable funding and coherent policy frameworks. The Malaysian OSCC experience illustrates the value of a hybrid approach in which early advocacy by NGOs and health professionals catalysed policy development and scale-up by the Ministry of Health – an example of effective government–civil society collaboration that aligns with Olson et al.’s emphasis on intersectoral coordination as an enabler. South Africa experienced a similar partnership between NGO/s and the government in the establishment and rollout of the TCCs. In rural communities, this partnership is less established because there are fewer established NGOs in these rural communities.
An integrated, victim-centred service model emerged as another key component. OSCs that offer a comprehensive suite of services, including medical care, psychosocial support, legal assistance and referrals, can provide more holistic, long-term support to survivors. For instance, the ASAZA Coordinated Response Centres in Zambia demonstrate how combining integrated services with community outreach and sensitisation efforts can enhance public awareness of available services and contribute to shifts in societal attitudes towards sexual and gender-based violence.
Equally important is the configuration and interlinkage of multi-sectoral actors within the OSC ecosystem. Ensuring that OSCs are adequately resourced with personnel trained specifically in GBV care is fundamental. A minimum standard team typically includes medical practitioners, social workers, nurses and counsellors, including some with expertise in child-sensitive and trauma-informed care. This approach has strengthened the SA TCC Model, regardless of the turnover of staff. The literature affirms that staff attitudes play a decisive role in survivors’ willingness to report cases. Unsupportive, judgmental or culturally biased responses, particularly from police and court personnel, erode trust in the system and act as a barrier to disclosure. This highlights the urgent need for targeted training in empathy, cultural competence and trauma-informed approaches for police, legal officers and court staff. Olson et al. (2020) also identified inadequate staffing, lack of GBV-specific training and unsupportive attitudes as high-confidence barriers, with police and legal sector staff attitudes frequently cited as deterrents to reporting.
Staffing adequacy and manageable caseloads also emerged as important operational factors. Evidence suggests that excessive workloads can hinder clinicians’ ability to accurately identify signs of abuse, potentially compromising the diagnostic process and survivor outcomes. Effective service delivery thus requires not only appropriate staff composition but also attention to workload management and resource planning.
Infrastructure and operational efficiency, highlighted in both reviews, further influence OSC performance. Olson et al. (2020) emphasised the importance of private consultation spaces, adequate medical supplies and streamlined intake processes to minimise survivor movement between service points. Our findings echo this, noting that excessive case volumes and fragmented service delivery can compromise assessment quality and survivor engagement.
Finally, the accessibility and responsiveness of OSCs significantly influence survivor engagement with care pathways. Geographic distance, fragmented service delivery, unclear referral systems and associated costs can all deter survivors from following through with services and legal processes. Therefore, designing OSCs that are agile, survivor-friendly and easy to navigate is essential. When facilities are well-staffed, strategically located and staffed by competent and compassionate professionals, they can provide high-quality, empowering care that encourages survivor participation and supports long-term recovery.
Conclusion
This review has highlighted the multifaceted requirements for the effective functioning of One-Stop Centres (OSCs) such as Thuthuzela Care Centres (TCCs), drawing attention to the structural, operational and relational components that shape service delivery. High-level governmental support, cross-sectoral collaboration, integrated service provision and trauma-informed, victim-centred approaches are all critical to ensuring that survivors of GBV receive comprehensive and dignified care. Furthermore, the availability of trained personnel, attention to staff well-being and caseload management, and the establishment of clear, accessible care pathways significantly influence survivors’ willingness to seek help and remain engaged in the justice and recovery process. The review identified that an efficient and effective monitoring, tracking and evaluation system is necessary to ensure a quality service delivery to survivors that maintains a sense of urgency that prioritises the needs of survivors.
Across the review, different contexts can support some elements more effectively than others. However, protocols and guidelines are necessary to confirm government support, collaboration and management. By investing in minimum standards of care that are contextually relevant and survivor-informed, policymakers and practitioners can strengthen the capacity of OSCs to respond effectively to GBV. While this review attempted to discuss a comprehensive set of elements for minimum standards, it could not cover all the aspects necessary. We hope that this paper will complement and provide further guidance for the adoption of minimum standards of care in South Africa’s TCC model, but also more generally to other countries wanting to consolidate guidelines on minimum standards of care.
Some recommendations for government and policymakers include resourcing rural OSC, which are usually under resourced. In villages and in communities where infrastructure is lacking or inadequate, consider the use of mobile clinics, a coordination and monitoring system and an accompanying responsible committee to ensure effective functioning of the model, and finally separate minimum standards of care for children and adults. For practitioners, strengthen referrals to shelters and counselling services, open communication channels and strengthen relationships between practitioners. Finally, researchers can review and assess minimum standards of care for children and, in countries where it is possible, focus on developing integrating systems for LGBTIQ persons. Future efforts must therefore focus not only on expanding the reach of such centres but also on deepening the quality, coordination and sustainability of services provided.
Footnotes
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
