Abstract
Background:
Palliative care research must be inclusive of those with impairments in decision-making to provide a representative evidence base for care and treatment. When capacity to consent to research is impaired, proxies may be asked to support decision-making. However, little is known about how proxies navigate this role or what supports their involvement.
Aim:
To identify, describe, and synthesise empirical evidence on the use of proxies to support the involvement of adults with impaired mental capacity in palliative care research.
Design:
A scoping review conducted and reported following the Joanna Briggs Institute guidance. Data were charted and are reported descriptively, organised by themes.
Data sources:
Ovid Medline, Ovid EMBASE, EBSCO CINAHL, EBSCO Academic Search Ultimate, Scopus, Westlaw, HeinOnline, APA PsycINFO, and Social Sciences Citation Index for studies published between 2007 and 2025.
Results:
Proxy decision-making was found to be context-dependent, shaped by consent models and varying across jurisdictions. Proxies’ confidence and willingness to act were influenced by their understanding of consent requirements, perceived research value and power dynamics. Significant international variation exists in the legal and ethical frameworks that guide proxy involvement.
Conclusion:
Proxy decision-making in research is complex, involving legal, ethical, emotional, relational, and contextual factors. Demands on proxies are particularly pertinent in a palliative care context, where substituted decision making must be balanced alongside personal values and emotional burden. To promote inclusion, accessible, jurisdiction-specific guidance, training for proxies and researchers, and ongoing support mechanisms are essential. In a palliative care context, advance research planning might support proxy decision-making.
Keywords
Where appropriate, proxies can be used to support research participation for adults with impaired mental capacity, particularly in end of life care research.
The process of proxy decision-making is influenced by interpersonal, emotional, and contextual factors, yet comprehensive support for proxies remains limited.
Proxies’ willingness to support research participation is shaped by their understanding of consent processes, perceptions of research value, and relational dynamics with clinical teams.
Evidence suggests that proxies value clarity, early engagement, and practical communication support when asked to make research decisions on behalf of others.
There is an urgent need for updated, jurisdiction-specific guidance and training for both researchers and proxies, especially in palliative care contexts.
Future policy and practice should explore models of early and structured advance research planning to support proxy involvement and uphold participant preferences.
Introduction
The involvement of advocates or “proxy decision-makers” is a familiar concept within palliative care. Many incurable illnesses, and the dying process itself, are characterised by a progressive impairment of cognition, communication or consciousness, and people receiving palliative care are encouraged to plan for who should “speak for them” if mental capacity is impaired. The need for decision making on behalf of another person at the end of life is common; in a large US study of 3746 deaths 42.5% of people required medical decision making near the end of life, 70.3% of whom lacked capacity to do so. 1
Generating the evidence needed to answer important questions about the care of dying patients, such as how to reduce delirium, upper airway secretions, pain and other symptoms at the end of life, requires the inclusion of participants who are unable to provide informed consent. 2 Intervention studies in palliative care are rare compared to other medical specialities and often exclude adults unable to consent to participation. 3 Under-representation of people with impaired capacity in research means that palliative care practice may not be fully evidence based, resulting in a “circular paradox”—where the lack of inclusion of this population limits the evidence needed to improve their care. 4
Whilst supported decision-making is fundamental to ethical inclusion in palliative care research, proxy involvement may offer a vital route to participation in research when conventional consent processes are not possible. This is particularly relevant for older, socially isolated adults and people receiving palliative care who have pre-existing cognitive impairments, such as those with dementia or profound learning disabilities, for whom standard models of consent are often inaccessible.3,5 Recent evidence suggests that study participation, even in the last days of life, can provide a sense of purpose for participants and their informal carers. 6
In most jurisdictions there a consensus that it is ethico-legally permissible, in certain circumstances, for one person to have decisional authority about another’s involvement in research. Despite this, there is little consistency internationally on the legislative procedures and ethical governance that underpin proxy involvement.7,8 Heterogeneity in the terminology, legislation, and ethical frameworks concerning the use of proxies in research can hinder international research collaboration, lead to confusion for the parties involved and may ultimately prevent a person’s wishes about research involvement being honoured at the end of life.7–9 The situation is particularly challenging in the US, where there is state-level variation, and little national consensus despite many people accessing care, treatment and research across state boundaries. 8 In the UK, there is variation across the devolved nations and depending on the type of research study. 10
For consistency, the term “proxies” is used throughout this review to encompass all forms of third-party involvement in supporting or making decisions about research participation involving a person with impaired capacity. This ranges from circumstances in which consent is not possible in any circumstances (e.g. unconsciousness) through to situations in which informed consent might be possible with appropriate information and support. Indeed, understanding how decision making can be supported by a trusted other, without the need for substituted decision making is a key consideration for the preservation of autonomy and human rights of people with disabilities. 11 We acknowledge that the term “proxy” spans different legal and ethical roles, and may encompass unpaid carers, health, social care, legal professionals and those working in an advocacy role.
Requirements of a proxy within research depends on the model of consent being sought for research (Table 1), which in turn is dictated by study design. Furthermore, there may be variation in the ethical framing of the decision a proxy is asked to support. 9 For example, a proxy may be asked whether they feel a person would wish to take part if able, if able to consent for themselves (“substituted judgement”). Alternatively, a proxy may be asked to consider whether participation would benefit the individual (“best interests”).
Definitions of models of consent.

Researchers have begun mapping the “daunting range of methodological, structural and systemic barriers” to participation of people with impaired capacity across a range of disciplines relevant to end of life research. 14 Clarifying who should act as a proxy, and how best to support them, is essential for improving the ethical inclusion of adults with impaired capacity. Several strategies have been identified to try and address challenges in recruiting adults with impaired capacity into end-of-life research, including advance designation of a proxy before capacity is lost.3,5 However, there is uncertainty about how best to engage proxies, with an expert think tank unable to reach consensus on specific recommendations around their use.3,5 Further research is therefore needed to determine optimal approaches to proxy engagement to enhance the inclusion of adults with impaired capacity in research.
This scoping review was undertaken to identify, describe, and synthesise empirical evidence on the roles of proxies in supporting the participation of people with impaired capacity to consent to research. It also aimed to highlight existing knowledge gaps, with the overarching goal of developing consensus guidance on the ethical and effective use of proxies in palliative care research. Palliative care is one of several specialities where consent challenges and proxy involvement are particularly relevant. Similar issues arise in intensive care, emergency medicine, dementia, and mental health—fields in which impaired capacity is common and standard consent processes may be unworkable.
This review therefore examines proxy involvement across all areas of health and social care research, with a particular focus on interventions and findings applicable to palliative care. It forms part of a wider NHS England research engagement project on structural barriers to research participation for adults with impaired capacity towards the end of life. Our research question was codeveloped through workshops and discussions with people who have lived experience of palliative care, impaired capacity, and proxy decision-making. A scoping review methodology was chosen due to the recognised paucity of evidence in this field. 15 Exploring these complex issues from an international perspective enabled both the challenges and facilitators to be captured from a broad range of jurisdictions and contexts.
A preliminary search of MEDLINE, the Cochrane Database of Systematic Reviews, PROSPERO and Joanna Briggs Institute (JBI) Evidence Synthesis was conducted, and no current or underway systematic reviews or scoping reviews on the topic were identified.
Review question
How can proxies be supported to involve adults with impaired capacity in research towards the end of life?
The following sub questions were addressed:
Who should act as a proxy for a person with impaired capacity to consent to participation palliative care research?
What constitutes “best practice” for the use of proxies in supporting the involvement of adults with impaired capacity in research
What roles do volunteers/independent advocates play in supporting ethically-sound research for those with impaired capacity towards the end of life?
What support or preparation do all potential proxies require to support involvement of adults with impaired capacity in ethically-sound research?
Methods
Design
A scoping review was selected as the most appropriate method to identify the scope of the evidence in this area, which we expected to have significant gaps, breadth and heterogeneity. 16 Given the absence of standardised reporting guidance on proxies in research, we sought to identify the types of evidence available, identifying key concepts/characteristics where possible. We were also interested in practice internationally, to understand how legal and ethical frameworks differ. The scoping review was undertaken in accordance with the Joanna Briggs Institute (JBI) framework. 17
Scoping reviews can be used to inform research agendas and identify implications for policy or practice. The review has been reported in line with the PRISMA extension for scoping reviews (PRISMA-Scr).18,19 The protocol was prospectively registered in Open Science Framework (https://osf.io/etp7g/).
Search strategy
A three-step search strategy was utilised in this review, in consultation with a senior medical librarian (MH). It consistent of three main concepts identified from the research aim: consent, proxies and research. First an initial limited search of MEDLINE (PubMed) and CINAHL (EBSCO) was undertaken to identify articles on the topic. The text words contained in the titles and abstracts of relevant articles, and the index terms used to describe the articles were used to develop a full search strategy (see Supplemental Appendix 1). The search strategy, including all identified keywords and index terms, were adapted for each included database and/or information source.
This scoping review considered all studies published in English since 2007 (when the MCA 2005 came into effect) to January 2025. Ovid Medline, Ovid EMBASE, EBSCO CINAHL, EBSCO Academic Search Ultimate, Scopus, Westlaw, HeinOnline, APA PsycINFO, and Social Sciences Citation Index were searched using identified search terms. The search strategy was structured using the Population, Concept, Context framework. For population, we used terms relating to third party decision maker, such as proxies, consultees, or surrogates. For concept, we used terms relating to consent and decision making in research, such as competency and patient participation. For context, we initially limited our search to palliative care settings, however this yielded few results, so we therefore expanded our search to all relevant health and care settings where research is conducted (e.g. community, primary care, hospices) with a view to having specific regard to findings relevant to palliative care during data analysis. These concepts were combined using Boolean operators (AND/OR), and adapted for each database (MEDLINE, CINAHL, Scopus, etc.). A full search string is provided in Supplemental Appendix 1. We used backward citation searching to identify any potentially relevant studies not captured in database searches.
Types of sources
This review considered published, peer reviewed studies and grey literature/policy articles of any intervention that describes the use of proxies in the participation of adults with impaired capacity in research to enable detection of all relevant research. 17
Inclusion/exclusion criteria
The Population, Concept, Context framework was used to determine our key inclusion criteria, as a broader alternative to the conventional PICO (Population, Intervention, Comparator and Outcome 17 ) which is less suited to a scoping review 17 ; our criteria is described in Table 2.
Inclusion and exclusion criteria.

Study selection
Following the search, all identified citations were collated and uploaded into EndNote® and duplicates removed. This set was uploaded to the Rayyan systematic review platform®. Titles and abstracts were screened for assessment against the inclusion criteria for the review. The first 10% of publications were reviewed by two reviewers (CB, MC) to ensure the eligibility criteria are being applied correctly and then these reviewers (CB, MC) completed their share of the remaining screen independently. The full text of selected citations was assessed in detail against the inclusion criteria. Reasons for exclusion of sources of evidence at full text that do not meet the inclusion criteria were recorded and reported. Any disagreements that arose between the reviewers at each stage of the selection process were resolved through discussion.
Data extraction
Data were extracted from papers by two independent reviewers (CB, MC) using a data extraction tool developed by the reviewers (Supplemental Appendix 2). The first 10 papers were cross checked by both reviewers to ensure consistency of data extraction. Data extracted including general study information, (author, year, geography, study methods), study population and details pertinent to context and concept. Data were identified and mapping to a pre-defined list which was developed from key components of the research question(s), the authors’ prior work in this area, and discussions with those with lived experience. These were: models of proxy involvement; education and training needs; challenges and barriers of involvement; known legal, ethical and/or regulatory frameworks. In addition to descriptive data, any outcomes/evaluative findings were also recorded. The two reviewers met regularly to discuss issues encountered or required amendments of the data extraction tool.
Data analysis and presentation
Descriptive data from each paper are presented in tables. Following data extraction, studies were categorised into one or more of our pre-defined themes based on their findings. Over the course of the review, the themes were discussed, and revised with all authors (which includes those with lived experience).
Results
A total of 7082 records were initially identified for inclusion in this review. After the removal of 2875 duplicates, 4072 articles were excluded following title and abstract screening. This left 135 reports for full-text review, from which 42 reports were ultimately included in the final synthesis. The selection process is summarised in Figure 1.
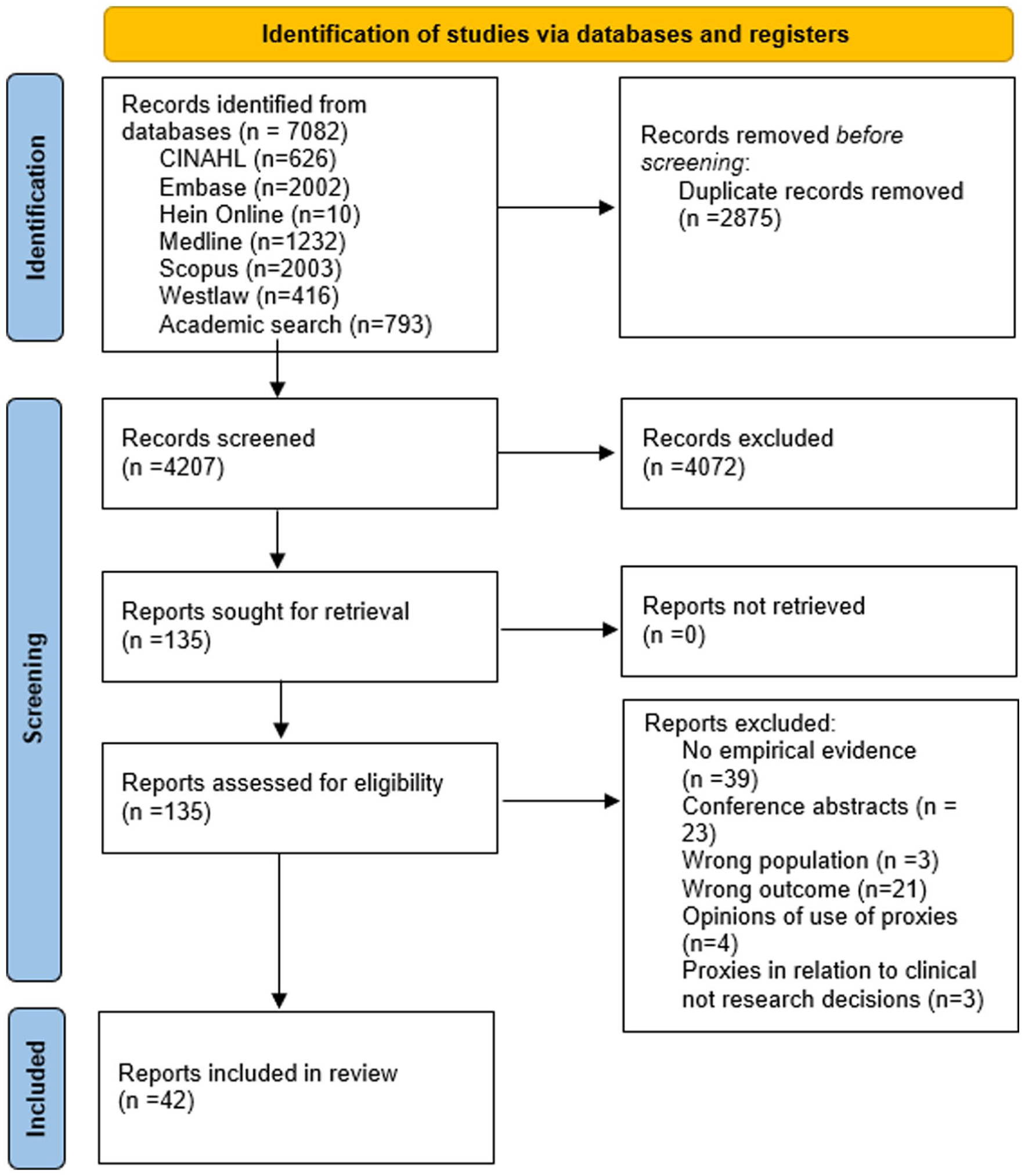
Selection of reports for literature review. 20
Characteristics of included studies
42 studies were conducted across 10 countries; the USA21–37 (n = 17), the UK38–46 (n = 9), Canada47–50 (n = 4), the Netherlands51–53 (n = 3), Australia54–56 (n = 3), India57,58 (n = 2), Switzerland 59 (n = 1) France 60 (n = 1) Germany 61 (n = 1) and Latin America 62 (n = 1). Settings included intensive care (n = 10), care homes (n = 2), emergency care (n = 2) mental health settings (n = 2), acute hospitals (n = 5), research institutions (n = 1), hospice (n = 1) and clinics (n = 1). The remaining 17 studies were conducted with members of the public and were not aligned to a specific health social care setting. This spread highlights the diversity of both geographical contexts and research settings, with a notable concentration of studies in the USA21–37 and acute or intensive care environments.22,30–33,35–37,47–50,52,53,57,59,60 A substantial number of studies also involved public perspectives in predetermined populations,23–25,28,34,38–43,56,61 offering insight into societal attitudes towards proxy decision-making.
Table 3 describes the extent of the geographic distribution and settings of data collection of the included reports in this review.
Characteristics of included studies.
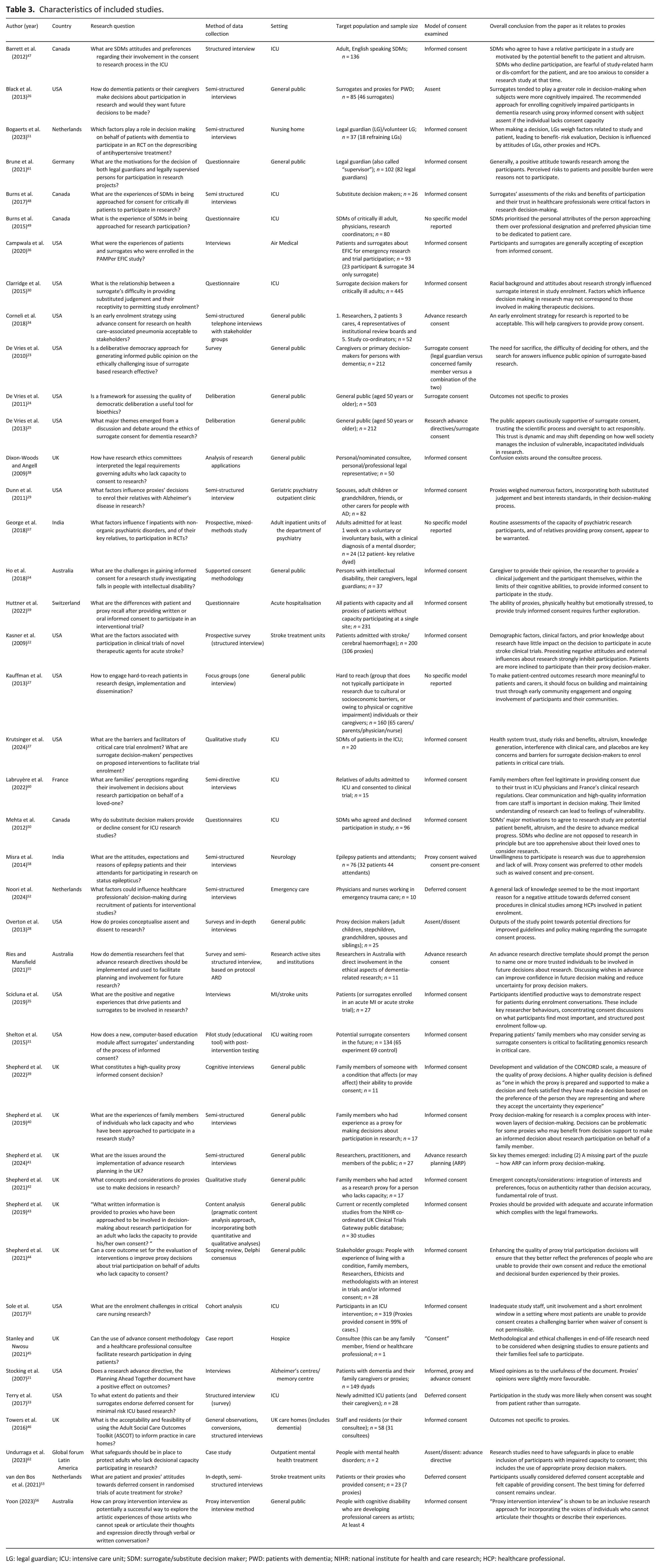
LG: legal guardian; ICU: intensive care unit; SDM: surrogate/substitute decision maker; PWD: patients with dementia; NIHR: national institute for health and care research; HCP: healthcare professional.
The terminology used to describe proxies varied across studies, and countries. Six reports used the term “proxy”: two from USA21,34, two from Australia,55,56 and the others from India 57 and Switzerland. 59 Three reports from Canada47–49 and another from USA 37 used the term “Surrogate Decision Maker,” whilst other reports from USA used the term “surrogate.”26,33,36 Personal consultee or legal representative was the model of proxy involvement in three UK reports38,43,46 with another describing a nominated consultee. 45
The methods of data collection across the included reports were diverse, ranging from hypothetical scenarios examining participants’ attitudes and perspectives,21,23–25,28,29,34,57,58,63,64 to participants’ experiences of research involvement research.30,32,33,35,38,40,43,48,50,56,59 Table 3 provides a detailed overview of the characteristics of these included reports.
The model of consent described in the studies also demonstrated wide variation. In most of the included reports, informed consent was the primary model of consent discussed, appearing in 24 reports.22,29–32,35–40,42–44,46–48,50,51,54,56,59–61 Data relating to guidance or information used to help inform and/or prepare proxies on the optimal way to support involvement of adults with impaired capacity in research was extracted alongside views and experiences of proxies. This data is reported in our Supplemental materials (Supplemental Appendix 3).
Our analysis identified five themes, with international relevance to researchers undertaking work with populations at risk of impaired capacity towards the life, where proxies may be required to support involvement:
Communicating Value: understanding role, importance and relevance of research
Respectful Responsiveness: Getting the timing right
Trust and Connexion: Ensuring the right people are involved
Balancing Power and Reciprocity in decision making
Navigating uncertain legal, ethical and policy contexts
Communicating value: Understanding the role, importance & relevance of research
Twenty-seven reports identified knowledge and understanding as key influences on proxy decisions to support research participation. Being informed about the research project, in terms of benefits, risks and burdens to the participant, and the proxy, was a central theme in this review.24,27,29–33,35–40,44,46,48,50–57,59–61 Understanding cannot be assumed; sub-optimal communication, complex study materials and poor timing of discussions can result in proxies lacking knowledge or confidence to make an informed decision about the study.35,50,53,57,60 In a 2022 study of proxy recall after written or verbal consent for an intervention trial, only 36% recalled the purpose of the trial, with regression analysis demonstrating no association between recall, time spent question asking or consent modality. 59
Proxies emphasised the need for accessible, clear information with “everyday” references to help their own understanding, and to support decision making of the person with impaired capacity. 54 This includes emphasising that participation in research is voluntary, that consent/participation can be withdrawn at any point, and that refusal will not affect ongoing care.31,33,34,36,49 Additionally, proxies often reported needing clarity about their role in the research process, such as what is expected of them and what role they have in decision-making.35,38–40,43,45 For example, distinguishing between whether they are being asked to provide information about a person’s prior wishes or preferences about research, whether they are being asked to support the decision making by the person in question or whether they are being asked to determine whether research participation might benefit the individual, on their behalf.
Respectful responsiveness: Getting the timing right
In non-acute settings, early engagement in the research process may increase participation.21,25,27,34,40,41,45 In both acute and non-acute contexts, the stage of a person’s illness influences decisions about research participation; with participation more likely if someone is judged to be in a stable condition.47,51,52,55 The exceptions to this are emergency and intensive care, where a study may be perceived as more acceptable if it confers a potential survival benefit in a critical situation. Spending time to explain the research, pre, during and post study was important to proxies, as was the ability to delay decision making if more time was needed. 44
Where considered, there was a strong interest in how early conversations about advance research planning41,55 and advance consent 45 might support research participation for people who go onto to development impairments in mental capacity. The need for tools to help people involve family members in these discussions has been identified, not least because such individuals may go onto to provide the practical support and care needed to participate in research. 41 Targeted educational initiatives around advance research planning (e.g. during will writing or as part of advance care planning activities) might increase public awareness. 25 Evidence suggests that advance research planning or advance consent can facilitate research inclusion, particularly in dementia care 55 and hospice settings. 45
Trust and connexion: Ensuring the right people are involved
A proxy’s decision to support research participation is shaped by relational factors, including their interpersonal and prior experiences with the person they represent, family dynamics, and their connexion, new or existing, with the research team.25,28,41–43,48 Proxies reported greater willingness to participate when they had access to someone they could ask questions and receive updates from.24,27,29,39,44 Building rapport is particularly important for people with cognitive impairments and their carers, to enable the carers to contribute to a supportive environment for discussion, based around that person’s communication requirements. 56 Inclusive community engagement may help widen opportunities to engage with research, particularly around advance research planning. 41
Proxies valued researcher attributes such as kindness, confident tone, an unhurried communication style, and openness to questions. 48 A 2015 Canadian study found that proxies prioritised these personal qualities over the researcher’s professional designation. 49 Proxy suitability depends on multiple factors, including the research context, availability of a trusted individual, legal frameworks, and the consent model used. An Ethiopian case study highlighted the complexity of proxy roles in mental health trials, where carers’ treatment priorities and involvement in coercive practices (e.g. restraint) created ethical tensions. 62
Legal frameworks include the use of independent advocates to support individuals without family or friends in medical and social care decisions,65,66 but we found no evidence of equivalent advocacy roles in other jurisdictions for supporting research involvement. Across studies, proxies were almost exclusively family or unpaid carers,21,24,29–32,40,42,43,45,60 highlighting a critical gap in ethical infrastructure for people with impaired capacity who have no informal support network.
We were unable to answer our research question from the literature to determine who should act as a proxy. Given the complexity of proxy decision-making and its reliance on trust, motivation, and ethical sensitivity, how and why a proxy is involved may matter more than who the proxy is.
Balancing power and reciprocity in decision making
Acting as a proxy can be emotionally challenging, especially when being asked to take responsibility for making decisions on behalf of someone with impaired capacity.24,40,49,50,60 In addition to emotional strain, practical burdens related to the study itself also affect proxy decisions.26,46,51,54,55,61 Ries and Mansfield noted that even when an advance research directive is in place, proxies still bear logistical burdens like arranging transport to research sites. 55
Five reports identified concerns about potential coercion from clinicians during the research consent process.26,37,49,60,62 Power imbalances can influence proxy views, a known issue under many forms of mental capacity legislation, where healthcare professionals often serve as decision makers for health and care decisions. 66 These power dynamics may be subtle; for example, one study found that proxies were more likely to agree to participation in research, if asked immediately after a clinical update from a medical professional. 47 Favourable attitudes towards research were associated with high level of trust in clinicians. 30 Proxies may also be guided by their own values rather than the patient’s wishes. 28
Terminology is important; whilst the use of “participants” was common, for others, this was perceived as reducing them passive subjects, disconnected from the study processes and demeaning of their valuable contributions to research. Respectful engagement was seen as critical to maintain trust and ethical involvement. 27
Navigating uncertain legal, ethical and policy contexts
This review of international literature highlights heterogeneity in the legal and ethical frameworks governing research across countries. Studies from the Netherlands and France suggest that high trust in national legislation is associated with greater participant willingness to consent to research.51,52,60 The development of policies to support proxy decision-making may further facilitate ethical participation23,28,40,62
Conversely, it was identified that inconsistencies or inaccuracies in the way that statutory and regulatory bodies (such as research ethics committees) viewed, reviewed or interpreted proxies in research had the potential to exclude people who may be eligible to be consulted.38,40,60
Irrespective of the prevailing ethico-legal framework in the country where they reside, proxies often weigh their own hopes, needs, and expectations28,44,48 alongside the perceived wishes and best interests of the patient.25,28,32,34,39–45,48,50,55 Nine studies reported that both potential individual and societal benefits factored into decision-making, with societal benefit often carrying more weight25,26,29,33,37,40,42,50,51
No definitive guidance exists on how proxies should decide about research participation for people who are unable to provide informed consent, nor how to determine the person’s wishes. Many aspects of “best practice” may vary by study design and jurisdiction. Key challenges include the setting in which consent is sought,32,33,35,47,52,53 the communicator’s approach,32,35,48,49,53 and the often time-sensitive nature of these decisions.22,32,35,37,47,49,50,52,53,57
What support or preparation do all potential proxies require? A consensus statement on involving proxies in end-of-life research 5 highlighted structural and procedural improvements, like early involvement, clear role definition, and national support, but it does not fully elaborate on how proxies can be trained or supported to optimise the involvement of the person they represent. This is a notable gap, especially considering that international human rights treaties 11 call for reasonable adjustments and communication supports to enable the person’s own preferences and participation to the greatest extent possible, which logically extends to supporting proxies to enable this.
Discussion
This review offers an international perspective on proxy involvement in research with adults impaired capacity, revealing considerable variation in consent models, data collection methods, and legal-ethical frameworks across jurisdictions. While previous studies have explored proxies’ views and ethical issues,9,40 this is the first to systematically synthesise the structures and mechanisms required to support proxies in this role.
This review highlights substantial international variation in proxy involvement, reflecting diverse legal, ethical, and cultural frameworks that govern research. Perceptions of research importance also vary culturally. For instance, a French study described participation as a “citizens’ duty,” 60 while a Korean–U.S. survey of institutional review boards found Korean respondents prioritised communal benefit, whereas U.S. respondents emphasised individual rights. 64 In palliative care, where person-centred, individualised decision-making is central, these ethical and cultural differences must be navigated with sensitivity.3,5,67
Differences also emerged between acute and non-acute settings. In non-acute settings, proxies expressed a need for clear contacts and ongoing updates.27,29,39,42 Barriers included indecision, risk aversion, and emotional burden.45,46,58 Researchers can address these through thoughtful study design, including building rapport through physical presence, providing clear information about the research team, and offering consistent contact points. 44 In hospice settings, which may lack dedicated research teams, exploring partnerships with volunteers or advocates, common in palliative care, may offer a valuable future strategy.
Proxies frequently reported being guided by the previously expressed wishes and values of the people they represent.25,28,34,39–45,55 This underscores the importance of early engagement in research discussions, ideally initiated while the individual retains capacity.21,25,27,34,41,43,45,55 Community awareness initiatives were also identified as valuable in preparing both potential participants and proxies for future involvement. 27 A phased approach to introducing advance research planning, starting with “priority” populations in whom it is most likely to be relevant (e.g. conditions characterised by progressive cognitive impairment) has been recommended, whilst taking care to avoid any sense of a moral obligation to participate. 55 In palliative care, where relatives or carers are often already involved in broader conversations about future care preferences, advance research discussions with potential proxies may offer a practical and ethically sound extension of existing practices. However, there is a need for more guidance and tools to support all those involved in advance research planning activities.
The burden placed on proxies emerged as a significant concern across multiple studies.26,46,51,54,55,61 Researchers must acknowledge and address this burden by developing protocols that support proxies as well as participants. In palliative care, this support should extend beyond the participant’s lifetime and into bereavement. Consideration should be given to how and when research findings are communicated to bereaved relatives, with sensitivity to timing, content, and emotional impact.
Education and understanding about the research and its potential effects consistently emerged as a key theme across the literature, serving both as a barrier and an enabler to participation.24,27,29–33,35–40,44,46,48,50–57,59–61 A systematic review reinforces that adequate knowledge and comprehension significantly influence willingness to participate, while insufficient understanding can undermine the validity of informed consent. 68 Furthermore, education plays a critical role in addressing the “gatekeeping” phenomenon frequently observed in palliative care settings, where clinical staff may hesitate to approach potential participants or proxies for research involvement.3,5
Although providing clear and accurate information to proxies is essential to support participation, this is not always achieved in practice. International variation in statutory and ethical procedures may hinder the development of consensus guidance which might support proxy involvement, with some jurisdictions having out of date guidance leading to further uncertainty. 69 Understanding how study materials might meet the requirements of research ethics boards, whilst remaining comprehensible and accessible for people with cognitive impairments, and their proxies is a key consideration.
Best practice for involving proxies in supporting research participation for adults with impaired capacity requires an approach that is adaptive, multidimensional, and responsive to context. 70 The Context and Implementation of Complex Intervention Framework offers a valuable lens for understanding the range of contextual determinants that influence proxy decision-making. This framework comprises of three interacting dimensions; context, implementation and setting, with context further divided into seven domains: geographical, epidemiological, socio-cultural, socio-economic, ethical, legal, and political. 71 Each domain operates at micro, meso, and macro levels, from national policy to interpersonal relationships.
Applying the Context and Implementation of Complex Intervention Framework to proxy decision-making in palliative care research helps generate hypotheses about the determinants of inclusion, revealing how broader, macro-level policies and governance structures shape individual decisions at the point of care. We propose that these hypotheses be further explored in future empirical research to inform evidence-based recommendations for practice.
To promote the ethical inclusion of this underserved group, future work should focus on the development of co-produced, context-specific complex interventions that reflect the diverse legal and cultural contexts in which proxy decision-making occurs. 72
Limitations
As a scoping review, this study aimed to map the breadth and nature of existing literature rather than critically appraise study quality. Despite a comprehensive search, some relevant evidence may have been missed due to publication bias, database limitations, or language restrictions. No formal risk of bias assessment was conducted, limiting conclusions about study quality. Variations in consent models, data collection methods, and healthcare contexts contribute to heterogeneity, so findings may not be fully transferable to palliative care settings. Furthermore, due to the inherent variation observed across jurisdictions, our ability to produce definitive generalisable conclusions is limited.
The Context and Implementation of Complex Interventions framework 71 is a conceptual tool for organising understanding of context, implementation, and intervention complexity, rather than an analytical method. Caution is needed to avoid “retrofitting” findings to the framework instead of creating themes inductively.
Conclusion
This review underscores the urgent need for clearer guidance, targeted education, and ethical support for proxies making research decisions on behalf of adults with impaired capacity. Proxy decision-making is complex, involving legal, ethical, emotional, relational, and contextual factors. Variations in consent models place differing demands on proxies as they interpret and apply the person’s wishes and interests, often while managing personal values and emotional burden. To promote equitable research inclusion, accessible, jurisdiction-specific guidance, training for proxies and researchers, and ongoing support mechanisms are essential.
These challenges are especially pronounced in palliative care, where individuals may experience rapid or progressive loss of capacity due to conditions such as advanced cancer, dementia, or neurological disease. In such contexts, proxy involvement may be the only viable route to research participation, underscoring the need for sensitive and timely support.
However, efforts to address these challenges may be hampered by a lack of legal reform or updating of the ethical and professional codes which govern this area of research. For example, in England and Wales where the authors of the review are located, the delayed update of the Mental Capacity Act 2005 Code of Practice highlights the pressing need for practical, comprehensive guidance to support ethical, inclusive research and clarify proxy roles in evolving legal frameworks. We only have one opportunity to ensure people receive the best care at the end of their life. If palliative care research is to be “fit for purpose” to provide the best evidence for care at the end-of-life care, there is a pressing need for practical, comprehensive guidance to support ethical, inclusive research and clarify proxy roles in evolving legal frameworks.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163261431100 – Supplemental material for Proxy decision-making about participation in palliative care research: A scoping review
Supplemental material, sj-docx-1-pmj-10.1177_02692163261431100 for Proxy decision-making about participation in palliative care research: A scoping review by Caroline Barry, Miriam Craske, Matthew Hawkes, Guy Peryer, Karen Bunning, Rob Heywood, Martyn Patel and Victoria Shepherd in Palliative Medicine
Supplemental Material
sj-docx-3-pmj-10.1177_02692163261431100 – Supplemental material for Proxy decision-making about participation in palliative care research: A scoping review
Supplemental material, sj-docx-3-pmj-10.1177_02692163261431100 for Proxy decision-making about participation in palliative care research: A scoping review by Caroline Barry, Miriam Craske, Matthew Hawkes, Guy Peryer, Karen Bunning, Rob Heywood, Martyn Patel and Victoria Shepherd in Palliative Medicine
Supplemental Material
sj-xlsx-2-pmj-10.1177_02692163261431100 – Supplemental material for Proxy decision-making about participation in palliative care research: A scoping review
Supplemental material, sj-xlsx-2-pmj-10.1177_02692163261431100 for Proxy decision-making about participation in palliative care research: A scoping review by Caroline Barry, Miriam Craske, Matthew Hawkes, Guy Peryer, Karen Bunning, Rob Heywood, Martyn Patel and Victoria Shepherd in Palliative Medicine
Footnotes
Author contributions
CB conceptualised the study idea, goals and aims with input from VS, GP, KB and RH. CB, VS, GP, KB, MH and RH developed the methodology and search strategy. CB and MC screened abstracts and extract the data. CB and MC wrote the initial draft. All authors were involved with reviewing, editing and approving the final version of the paper. All authors approved the final version. CB is the guarantor.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by NHS England Research Engagement Network Grant, November 2023 – July 2025. The views expressed are those of the author(s) and not necessarily those of NHS England or the Department of Health and Social Care.
This study is supported by the National Institute for Health and Care Research (NIHR) Applied Research Collaboration East of England (NIHR ARC EoE) at Cambridgeshire and Peterborough NHS Foundation Trust. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
CB is funded, and GP is supported by the National Institute for Health and Care Research (NIHR) Applied Research Collaboration East of England (NIHR ARC EoE) at Cambridgeshire and Peterborough NHS Foundation Trust. VS is supported by an NIHR Advanced Fellowship funded by Health and Care Research Wales (NIHR-FS(A)-2021)
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
