Abstract
Background:
Loneliness has been linked to poorer quality of life and worse symptoms in the final weeks prior to death. However, research on prevalence at end of life has yet to be systematically reviewed.
Aim:
To synthesise evidence of prevalence and correlates of loneliness among adults at the end of life.
Design:
Systematic review without meta-analysis, due to high study heterogeneity, registered on PROSPERO (CRD42024581962).
Data sources:
OVID Medline, PsycInfo, Web of Science, PubMed, Social Policy and Practice and Health Management Information Consortium databases were searched up to April 2025. Studies estimating prevalence of loneliness were eligible where the sample (or identifiable sub-sample) were adults with a terminal illness, receiving palliative care or retrospectively identified with a loneliness measure less than 12 months prior to death.
Results:
Fifteen eligible studies were included. Most studies were North American or European, with samples based on clinical diagnosis or palliative care receipt. Prevalence estimates of moderate or worse loneliness ranged from 20% to 73% and high loneliness from 8% to 33% in studies sampling based on clinical diagnosis or care receipt, and 7%–12% and 18.6% respectively, in studies sampling retrospectively based on time to death. However, findings are presented with caution due to significant heterogeneity across studies.
Conclusions:
Evidence suggests loneliness may be a difficulty faced by a significant minority of people at the end of life, requiring support for individuals, within services and communities. Research is needed in a wider range of countries, and to develop and assess effective interventions.
Loneliness has been linked to poorer quality of life and worse symptoms at end of life.
Terminally ill people may experience loneliness related to deteriorating mobility and changes in the quality of important relationships.
Evidence of loneliness prevalence at end of life is needed to inform commissioning of initiatives to address loneliness as a potentially modifiable factor.
Fifteen studies estimated loneliness prevalence among those at end of life, across a range of conditions, care settings and countries.
Prevalence ranged from 20% to 73% (moderate or worse loneliness) and from 8% to 33% (high loneliness) for studies based on diagnosis or receipt of care.
Results are presented cautiously as studies were heterogeneous in their size, design, sample and setting characteristics.
More consistent analysis of correlates, and more research across different countries and conditions, would be beneficial.
Loneliness should be considered as a potential difficulty contributing to worse quality of end of life.
Initiatives to prevent and reduce loneliness at end of life in individuals, within services and communities should be commissioned and evaluated.
Introduction
Loneliness can be defined as the subjective negative feelings that stem from perceived disparities between expected and actual social relationships. 1 Though the mechanisms translating the experience of loneliness to health and wellbeing are the subject of research, 2 loneliness has been linked to reduced quality of life, 3 increasing depressive symptoms, 4 frailty, 5 disturbed sleep, 6 and increased risk of heart failure 7 and other causes of mortality. 8 Community-based healthcare professionals supporting people at the end of life cite loneliness as a common concern in their caseloads,9,10 with implications for their experiences at end of life. For instance, associations have been found between loneliness and use of life support in the last 2 years of life, 11 pain, anxiety and trouble breathing in the last month of life, 12 and greater likelihood of admission to, and dying in, a care home compared to a private home.11,13
End of life is difficult to define and can include individuals with advanced progressive terminal conditions, people who are frail with coexisting conditions and adults who experience a sudden crisis in a pre-existing condition.14–16 Loneliness is common among people with conditions that are major causes of death, such as cancer, 17 dementia 18 and chronic obstructive pulmonary disease. 19 Circumstances that frequently occur near the end of life are also general risk factors for loneliness, including presence of multiple conditions,20,21 deteriorating health and reducing social networks 13 . Experiencing advanced frailty or terminal illness can change social relationships, increase feelings of disconnect with others, and difficulties expressing concerns. 22 For instance, reducing mobility and functional limitations can limit social interactions, or change their quality due to the need to depend on others, introducing the potential for loneliness even in the presence of others. 23 Although loneliness differs from social isolation or living alone, they are related objective measures and are potential risk factors for loneliness.24,25 For instance, having no informal caregiver in the last 6 months of life has been linked to becoming lonely. 26
Loneliness prevalence and risk factors have been recently reviewed among the general and older population21,27–31 and different patient groups, 32 however, only two reviews have addressed these aspects specifically related to end of life. A recent scoping review identified a handful of studies estimating prevalence of loneliness, ranging from 10% to 50%, with limited generalisability due to small samples or limited age range, concluding that there was “no reliable population-based data about the prevalence of loneliness at EOL” 33 (p. 6191). As appropriate for a scoping review, minimal quality assessment of included studies was carried out and new studies have since been published. With regard to correlates of loneliness, limited evidence has been synthesised of at-risk population groups, 33 but there has been greater focus on beliefs, emotional and social support.33,34 A recently developed framework for the causes of loneliness in advanced illness encompasses psychological and existential micro level factors, physical function, mobility and social meso level factors and environmental and societal macro level factors. 34 This provides a structure for understanding potential causes of loneliness among those with advanced terminal illness. However, a gap exists to undertake a systematic review of prevalence data and understand population-based correlates of loneliness among those at end of life, assessing measurement and study quality. This review therefore aimed to 1. synthesise evidence of loneliness prevalence and 2. identify the correlates of loneliness among adults at the end of life.
Methods
Study design
This systematic review followed a published protocol (https://www.crd.york.ac.uk/PROSPERO/view/CRD42024581962), the Preferred Reporting Items for Systematic Reviews and Meta-Analyse, PRISMA, 2020 reporting guidance 35 and as a meta-analysis was not possible due to high study heterogeneity, the Synthesis without Meta-Analysis reporting guideline. 36
Eligibility criteria
Studies were included which were (i) English language primary research studies in any geographic region or setting (ii) where the sample was of adults aged 18 or over and (iii) included a quantitative estimate of loneliness prevalence using any question or scale. Eligibility criteria relating to end of life spanned several different groups aligning to broad definitions used elsewhere.14,15 Eligible studies sampled (iv) adults explicitly defined as end of life, receiving palliative or hospice care or having a terminal diagnosis. Conditions normally considered terminal were confirmed by a clinical researcher with expertise in end-of-life care, including metastatic cancer, end stage liver disease and amyotrophic lateral sclerosis. Retrospective studies of individuals who had died were included where loneliness was measured within the 12 months prior to death.
For studies including only a continuous score for loneliness measured using a validated scale, the author was contacted to request the raw data for estimating prevalence to meet criteria (iii). Studies with samples including a subpopulation of people meeting criteria (iv) were included where the authors could be contacted and agreed to send relevant sub-sample data.
Articles focussed on children and young people under 18 years or measuring living alone, social isolation or social participation, but not loneliness were excluded. Further exclusions included study designs addressing prevalence of loneliness for groups other than patients, for instance carers of people with terminal illness and articles other than empirical research, such as theses or conference abstracts. One original exclusion in the review protocol was removed after searches had been completed: loneliness was not required to be the main outcome of each study.
Search strategy
Six databases were searched up to 29th April 2025 for academic studies (OVID Medline and PsycInfo, Web of Science and PubMed) and grey literature (Social Policy and Practice and Health Management Information Consortium). Scoping for the review established a search strategy including MeSH, subject headings and key words, translated for each database (Supplemental materials, Supplemental Figure S1). Forward and backward citation searching was conducted for included articles and for two relevant reviews.33,37
Screening
Search results were de-duplicated in EndNote then uploaded to Rayyan.ai systematic review screening software (https://www.rayyan.ai/) for independent blind screening of titles and abstracts by two researchers (EM, BH). Following discussion to reach consensus, full text articles were blind reviewed then discussed. Citation searching was undertaken by EM and identified articles reviewed by BH.
Data extraction and assessment of risk of bias
EM and BH undertook independent data extraction using an excel form including author, date, journal and title, stated aims, geography, study type and methodology, sample eligibility, and methodology. Loneliness measure used, statistical analyses, results including prevalence estimate, and where relevant, analysis of correlates were tabulated.
Quality of included studies was assessed by EM using Joanna Briggs Institute guidance for systematic reviews of prevalence and incidence 38 to identify risk of bias. The tool includes nine questions on the appropriateness of sampling frame, sampling method, sample size, response rate, subject and setting description, measure used and statistical analysis. Each study was scored 0–9 and categorised as lower risk of bias (score of 7–9), moderate risk (score of 4–6) or high risk of bias (score of 0–3), following other studies. 39 All studies were included, however, to explore the influence of study quality on prevalence, the range of prevalence estimates was reported first for all studies, then studies assessed as lower risk of bias.
Outcome measure - loneliness
There is no consensus on how loneliness should be measured but several validated scales are available such as the University of California Los Angeles (UCLA) loneliness scale 40 and the De Jong Gierveld Loneliness scale. 41 Scales vary in length and include items related to aspects of loneliness, indirectly asking whether a respondent is lonely. For instance, the three item short form of UCLA loneliness scale asks whether individuals lack companionship, feel left out and are isolated from others hardly ever, some of the time or often. 42 The De Jong Gierveld scale has 11 items relating to emotional and social aspects of loneliness. 43 Although these scales have acceptable reliability and validity,43,44 there are no accepted cut off points to categorise differing intensities of loneliness. Therefore, differing cut-offs used by study authors were categorised according to their original description.27,39 Categories were low loneliness (cut-offs described by study authors as no or low loneliness), moderate loneliness (mild or moderate loneliness) or high loneliness (cut-offs described as very, high, severe, clinically informative or frequent loneliness).
Single direct questions about feeling lonely are also commonly included in surveys, with slightly different wording and response categories, such as “How often do you feel lonely?” or “Do you feel lonely?.” 44 Where loneliness was measured with a direct question and binary response, loneliness was considered to be moderate, following other studies. 39 Validated scale and direct measures of loneliness were analysed separately as low concordance has been found in responses. 45 For instance, men and women may differ in their responses to each question type, 46 and direct loneliness measures may underestimate loneliness due to social stigma. 10
Data analysis
A synthesis without meta-analysis with a structured approach was carried out 36 as four of seven considerations for the appropriateness of meta-analysis were present in the identified studies. 47 Sources of clinical heterogeneity included differing loneliness measurement, study designs and populations (including age ranges, diagnoses, settings and indication of end of life), as well as assessing less than half the studies as lower risk of bias.
To enable different measures to be compared, in addition to translating each loneliness measure to low, moderate and high loneliness, estimates were synthesised separately for studies using validated scales and those using single direct questions, following other systematic reviews of loneliness.27,39 As studies were identified measuring patient loneliness via different groups, a decision was made to analyse studies measuring loneliness by the patient separately from studies using family or health professional proxies, as estimates are influenced by the differing perspectives of these groups. 48 Following initial synthesis, studies were subsequently separated into those identifying their samples by clinical diagnosis or care receipt, and those retrospectively identifying their samples via time to death without other diagnosis or care criteria. This post-hoc grouping enabled separation of studies where not all sample members would know they were nearing the end of life. Prevalence was also narratively summarised by diagnosis where available given known differences in end-of-life experiences between those with malignant and non-malignant disease. 49 The presence or absence and direction of multivariable associations between potential correlates and loneliness for relevant studies were summarised.
Results
Included study characteristics
Database searches identified 668 unique records, see Figure 1. After title and abstract screening, 619 records were excluded leaving 49 articles for full text review and a further 13 from reference and citation searching. Reasons for exclusion with examples are presented in Supplemental Table S1. Following full text review, a total of 15 studies were included.50–64 Risk of bias assessment identified seven studies as having lower risk (scoring 7–8) and eight having moderate risk (scoring 4–6), Supplemental Table S2. The most common sources of bias in the studies were using a single direct question rather than a validated scale measure of loneliness, small sample size and providing no information on response rate.
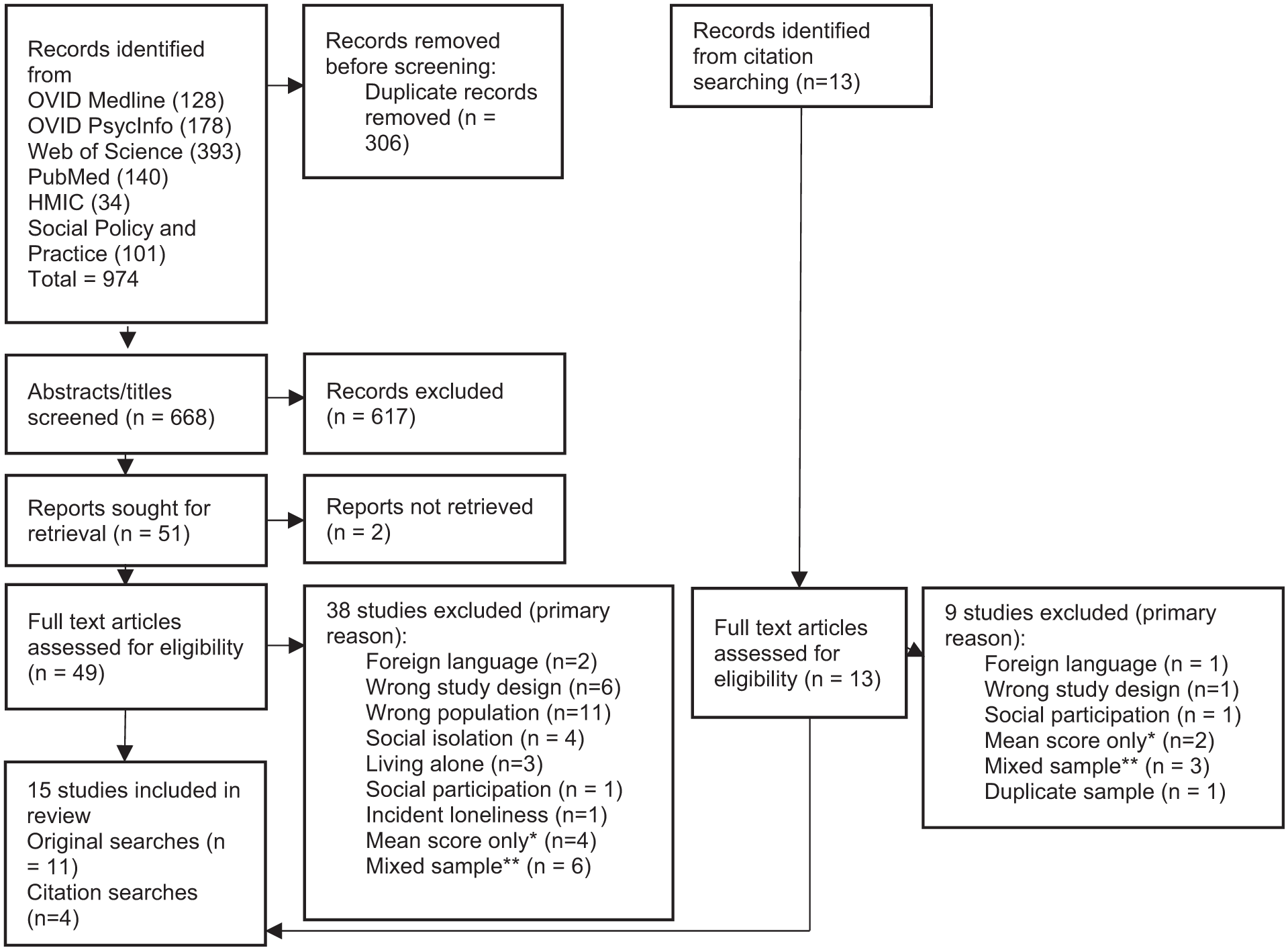
PRISMA diagram literature search.
Table 1 provides details of included study characteristics for studies with samples identified by diagnosis or care receipt. Table 2 provides study details for studies with samples retrospectively identified by time to death. In each table, studies are separated into three categories: patient reported loneliness using 1. scale loneliness measures and 2. direct loneliness measures; and 3. family or health professional reported loneliness. Studies are ordered alphabetically within each category. Across all included studies, most addressed prevalence in North America or Europe: Canada (n = 2), United States (n = 5), Italy (n = 1), Netherlands (n = 3) and Turkey (n = 1), with three studies from other regions: Hong Kong, Israel and South Africa, Tables 1 and 2. Data sources included surveys in hospices and outpatient clinics (n = 9), routinely collected homecare data, including two using similar data (n = 3), nationally representative longitudinal survey data (n = 1) and baseline data for a randomised controlled trial (n = 2). Nine studies were published within the last decade. Relevance to end of life eligibility criterion included prognosis of less than 3 months (n = 1) or 6 months to live (n = 2), receipt of hospice services or palliative care (n = 3), terminal diagnosis (n = 6) and length of time from loneliness measure to death of less than 30 days (n=1), less than 6 months (n=1) and less than 12 months (n = 1). Four of 15 studies aimed to investigate a wide range of symptoms including loneliness, while 11 included loneliness as a specific focus. Study sample size ranged from 37 dying oncology hospice patients to 27,295 cancer decedents who used home care services in their final 6 months of life.
Studies with samples identified by disease or prognosis: Study characteristics, loneliness measure and prevalence estimate.
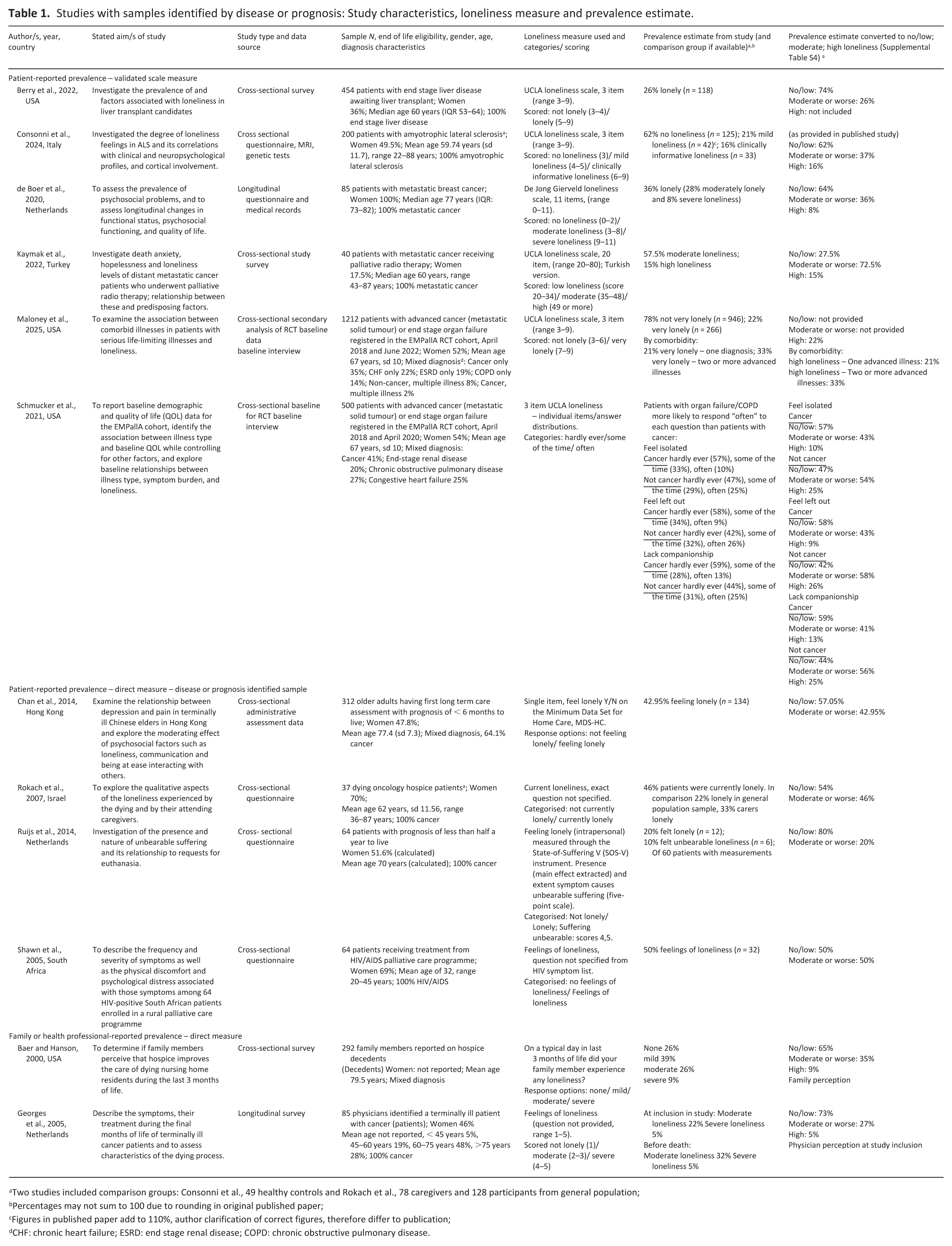
Two studies included comparison groups: Consonni et al., 49 healthy controls and Rokach et al., 78 caregivers and 128 participants from general population;
Percentages may not sum to 100 due to rounding in original published paper;
Figures in published paper add to 110%, author clarification of correct figures, therefore differ to publication;
CHF: chronic heart failure; ESRD: end stage renal disease; COPD: chronic obstructive pulmonary disease.
Studies with retrospectively identified samples based on time to death: Study characteristics, loneliness measure and prevalence estimate.
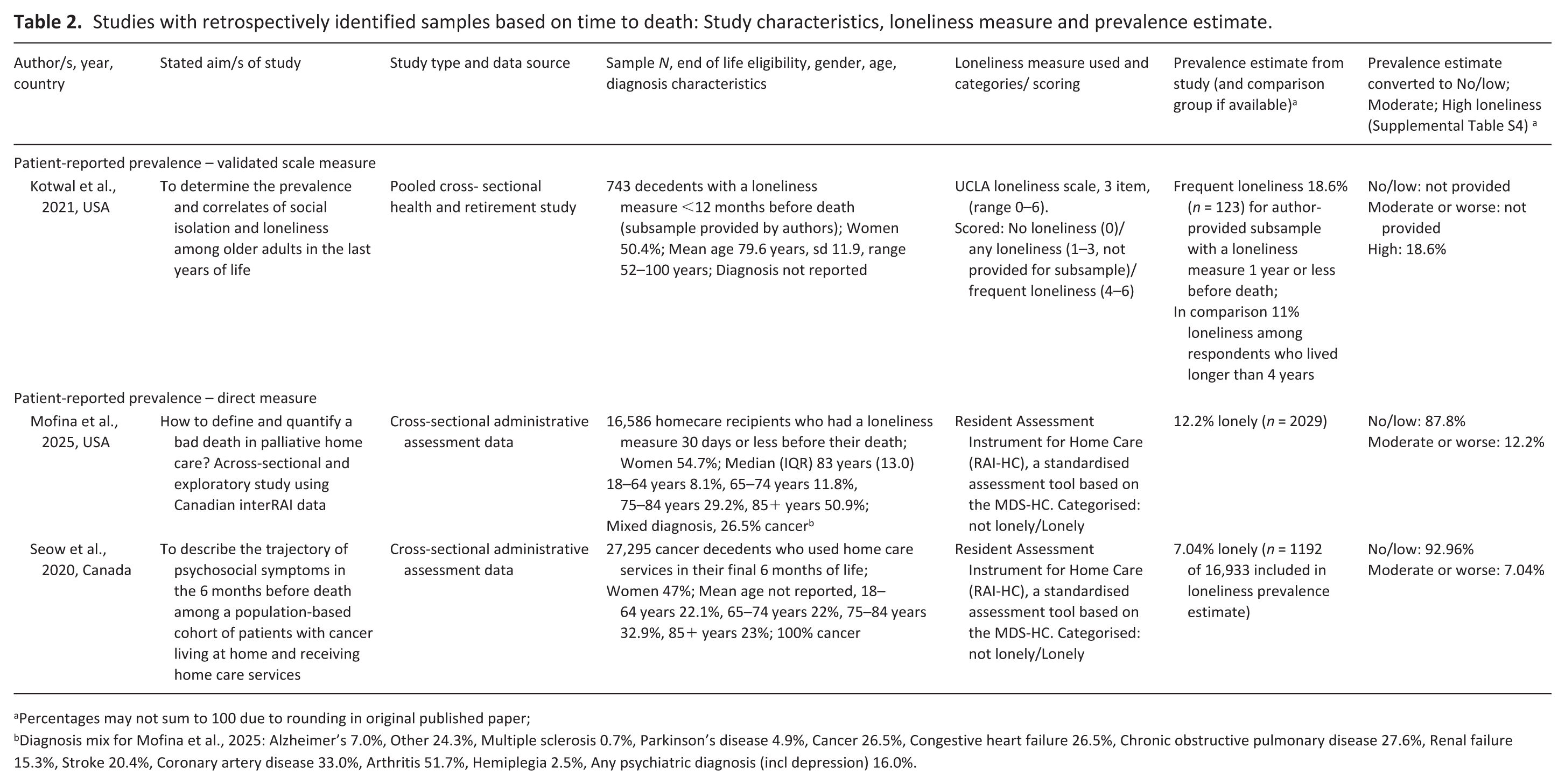

Percentages may not sum to 100 due to rounding in original published paper;
Diagnosis mix for Mofina et al., 2025: Alzheimer’s 7.0%, Other 24.3%, Multiple sclerosis 0.7%, Parkinson’s disease 4.9%, Cancer 26.5%, Congestive heart failure 26.5%, Chronic obstructive pulmonary disease 27.6%, Renal failure 15.3%, Stroke 20.4%, Coronary artery disease 33.0%, Arthritis 51.7%, Hemiplegia 2.5%, Any psychiatric diagnosis (incl depression) 16.0%.
Study population characteristics included disease type: cancer patients (n = 6), patients with end stage liver disease (n = 1), HIV/AIDS (n = 1) and Amyotrophic lateral sclerosis (n = 1) and six studies not including details of patient diagnosis or including mixed diagnoses. The proportion of women among the sample, ranged from 36% to 100% (weighted proportion 50%). Weighted mean age was 70.7 years (data available from seven studies). Ethnicity and socioeconomic status data where available is reported in Supplemental Table S3.
Measurement of loneliness
Among studies of patient-reported loneliness (n = 13, total of 47,588 patients), scale measures were used in 7 studies: three-item UCLA loneliness scale (n = 5), 20-item UCLA loneliness scale (n = 1), and 11-item De Jong Giervald loneliness scale (n = 1). Six studies used patient-reported direct questions asking about being or feeling lonely with binary response options. Studies measuring loneliness via health professional or family-respondent used direct questions with 3 or 5 response options (n = 2) estimated from 85 professionals and 292 family members, Table 1. Supplemental Table S4 presents the mapping of each study’s loneliness measure to the framework of low, moderate and high loneliness.
Studies with samples identified by diagnosis/care receipt and patient-reported prevalence – validated scale measure
Four out of six studies estimating patient-reported prevalence using a scale measure were assessed as having lower risk of bias (scores of 7) and two studies a moderate risk of bias (scores of 4), Supplemental Table S2. Prevalence of moderate or worse loneliness ranged from 26% to 73% (26%–58% among studies with a lower risk of bias), Table 1. There was less variation in estimates of high loneliness, ranging from 8% to 33%.
Two studies of baseline data from a randomised controlled trial comparing models of palliative care addressed prevalence estimates by disease type 60 and for multimorbidity. 63 The first study found patients with non-cancer diagnoses (congestive heart failure, end stage renal disease or chronic obstructive pulmonary disease) reported the three items in the UCLA scale more frequently than patients with cancer diagnoses. For instance, feeling isolated often, 10% for cancer patients and 25% for non-cancer patients, Table 1. 60 The second study found higher prevalence of high loneliness among patients with two or more of cancer or end stage organ failures (33%), compared to patients with only one condition (21%). 63 However, the same pattern was not found when comparing estimates from studies of single diseases. Two small studies of cancer patients (N = 40 and 80) estimated moderate or worse loneliness as 36%–73% and high loneliness 8%–15%. Two studies of end stage liver disease patients and patients with amyotrophic lateral sclerosis estimated moderate or worse loneliness as 26%–37% and high loneliness 16%. Studies differed by country, setting, design and sample characteristics.
Studies with samples identified by diagnosis/care receipt and patient-reported prevalence – direct measure
All four studies estimating patient-reported prevalence using a direct loneliness question were assessed as having a moderate risk of bias (scores of 4–6), Supplemental Table S2. Prevalence of moderate or worse loneliness ranged from 20% to 50%, Table 1. Only one study compared loneliness prevalence to those not at the end of life, finding higher loneliness among oncology hospice patients (46%) compared to the general population (22%) and carers (33%). 58 Prevalence ranged from 20% to 46% in studies of cancer patients and was 50% in patients with HIV/AIDS.
Studies with samples identified by diagnosis/care receipt and family or health professional-reported prevalence – direct measure
Both studies estimating family or health professional-reported prevalence with a direct loneliness question were assessed as having a moderate risk of bias (scores of 5), Supplemental Table S2. Studies estimated moderate or worse loneliness among patients at 27%–35% and high loneliness between 5% and 9%, Table 1.
Studies with retrospective samples identified by time to death
One of three studies with retrospective samples estimated patient-reported prevalence using a scale measure. The study was assessed as having lower risk of bias (score of 8), Supplemental Table S2, and prevalence of high loneliness was estimated at 18.6%, Table 2. This study compared loneliness prevalence to those not at the end of life, finding significantly lower loneliness among an age- and sex-matched group living for more than 4 years after their loneliness measurement (11%). 57 The remaining two studies estimated patient-reported prevalence using a direct measure and were assessed as lower risk of bias (scores of 7), Supplemental Table S2. Prevalence of moderate or worse loneliness was estimated as 7%–12% in these studies, Table 2.
Correlates of loneliness
Seven studies carried out multivariable analysis of correlates of loneliness. The presence, absence and direction of the associations found are presented in Figure 2. Four studies were rated lower risk of bias (scores of 7) and three rated moderate risk of bias (scores of 4 or 5). There was little consistency in covariates analysed, though sociodemographic, physical and mental health and social factors were most frequently included. Analytic methods included multiple linear and logistic regression.
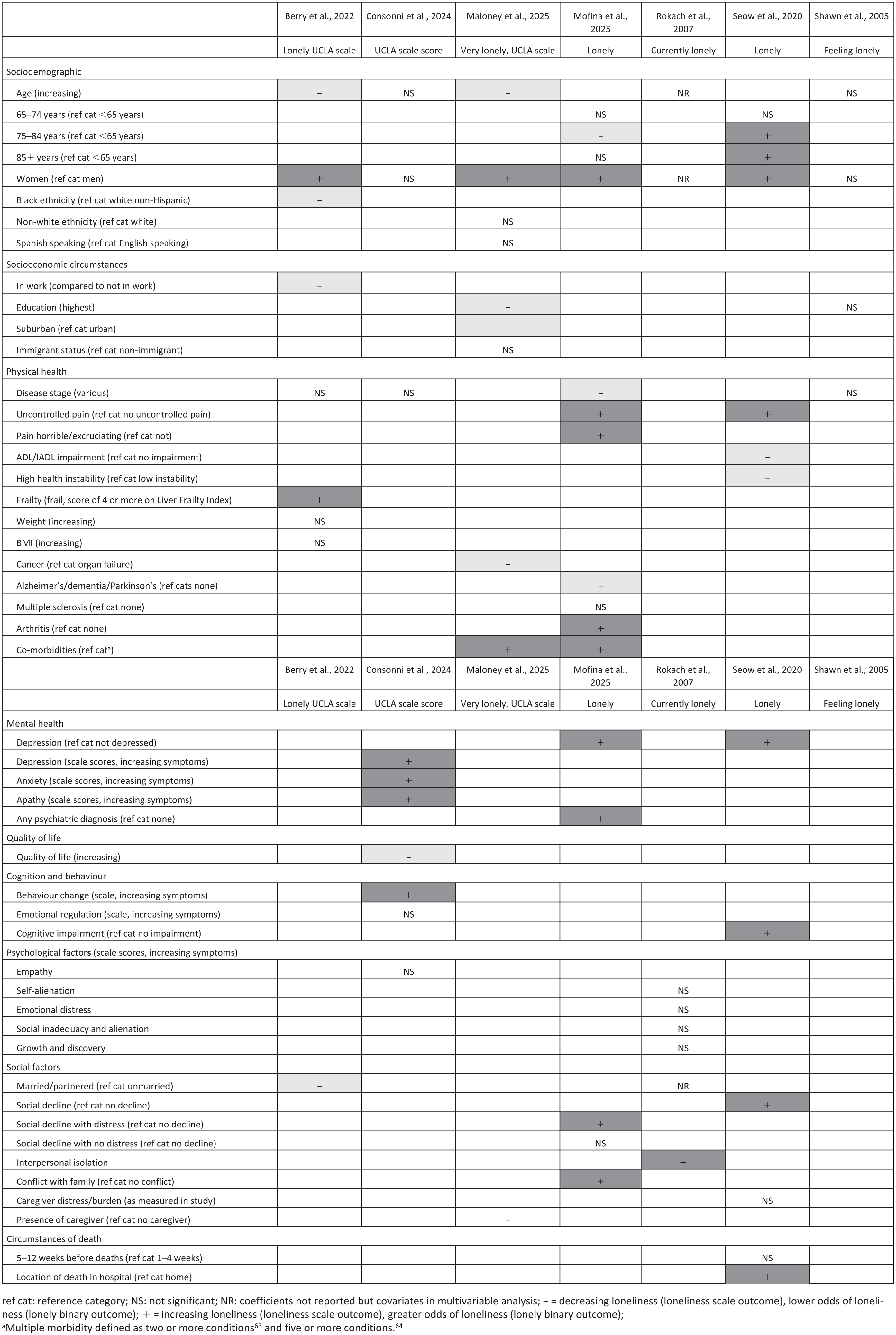
Correlations with loneliness: Presence or absence of association and direction.
Sociodemographic factors included age, gender and ethnicity, with no consistent associations found across all studies. However, women were more often lonely than men in studies assessed as having lower risk of bias. Few physical health factors were included in more than one study, with the exceptions of various disease stage measures (predominantly not associated with loneliness), arthritis and pain (both associated with being lonely). All studies including measures of poorer mental health (such as depression, anxiety and apathy) found associations with loneliness. Associations were also found between social factors such as not being married and experiencing social decline, but consistency across studies was again limited and no studies included living arrangements, such as lone living or living in a care home in their analyses.
Discussion
This review synthesised evidence from 15 studies, encompassing a variety of conditions, care settings and countries, and indicating loneliness may be experienced by a significant minority of people at the end of life, though with wide variation. Prevalence of moderate or worse loneliness was estimated to be 20% or over in all except two studies. Among studies with samples based on diagnosis or care receipt, prevalence ranged from 26% to 73% (mid-range or higher loneliness scale scores) and 20%–50% (based on answering yes to a direct loneliness question). High loneliness estimates ranged from 8% to 33% in these studies (upper range loneliness scale scores). Among studies based on samples identified retrospectively by time to death, respective estimates were 7%–12% and 18.6%. Where directly compared, loneliness was more common among patients with non-cancer diagnoses compared to cancer diagnoses, and multiple conditions compared to one condition. The same pattern was not found when comparing estimates from studies of single diseases, though the samples, countries and methods also differed. There was no clear difference in estimates from direct or scale measurements. However, direct loneliness estimates from two studies with retrospective samples based on time to death were notably lower (7% and 12%) compared to estimates from studies with clinically identified samples (20%–50%). Caution is required in interpreting these findings due to heterogeneity in measurement of loneliness and study details such as sample size and characteristics, country and care setting.
These findings can be viewed in the context of the many changes to individuals’ physical, social and internal worlds with approaching end of life. Although individuals respond in different ways, declining health and mobility can impose unpredictable constraints on social activities, roles and relationships. 65 Indirect pressures arise through uncertain trajectories of illness and care 66 and fragmented support.67,68 Approaching end of life may lead to feelings of separateness, lost connections, regrets or shame, connected to existential loneliness – deeper feelings of aloneness.22,65,69 However, these deeper feelings are not captured in widely used short loneliness measures, though longer scales do exist. 70
Comparing prevalence of loneliness among people at end of life and among those living longer can provide insights into differing needs across life stages. In this review, one study found higher loneliness among those in their last year of life compared to those living for more than 4 years. 57 In the wider literature, a recent systematic review found pooled prevalence of loneliness among older adults ranged from 11.1% in western Europe to 27.7% in eastern European countries, measured as 6 or more on the de Jong Gierveld loneliness scale. 27 This is equivalent to moderate loneliness for scale measures in this review and lower than our estimation of 26%–73% among those at end of life. Similar pooled prevalence was found for high loneliness among older adults, measured as 6 or more on the UCLA loneliness scale, as among adults at end of life in this review (6%–19% for older adults; 8%–26% for people at end of life in this review). These comparisons give some indication that loneliness among people at the end of life may be higher than among the general older adult population, at least at moderate levels. However, general prevalence estimates vary across and between regions, likely influenced by differing demographic, health, social and welfare contexts. 27 Future studies could compare people at end of life with general population estimates within the same country.
Differing loneliness prevalence by diagnosis was found in two studies of baseline data from a randomised controlled trial.60,63 Greater prevalence of loneliness was found among patients with non-cancer diagnoses compared to cancer diagnoses, and with multimorbidity compared to one diagnosis. However, the same pattern was not seen when comparing prevalence across studies of patients with single diseases. People with cancer are more likely to be referred to, or die in, hospices compared to people with non-cancer end stage disease. 71 This may mean people with cancer receive more support to maintain important relationships and find meaning towards the end of their lives. 72 Differing symptoms and management of illnesses also vary in their impact on an individual’s life and social functioning. 34 In relation to multimorbidity, the challenges of managing multiple conditions may reduce opportunities to meet others or increase perceived differences with others.21,23 More studies are needed comparing prevalence by diagnosis to add to this emerging evidence base and to carry out multivariable analysis of correlates to help disentangle the effects of underlying individual differences between patients, disease-specific factors and potentially modifiable aspects such as access to support.
Few studies carried out multivariable analysis of correlates of loneliness and there was limited consistency in included covariates. Associations with sociodemographic, socioeconomic and physical health factors mirrored those in the wider literature, where evidence is mixed. 29 Associations found in this review with poorer mental health, and to some extent social circumstances, are consistent with risk factors identified for the general and older population29,30 and among those with advanced terminal illness. 34 Surprisingly, no studies assessed living arrangements, such as living alone and future research could include these important variables in analyses.
Limitations of the studies included in the review
Although included studies were diverse, some settings were noticeably absent, including care homes. Currently almost a quarter of deaths occur in care homes in England 73 and care homes are projected to be the most common place of death in England and Wales by 2040. 74 Pooled prevalence of loneliness among care home residents has been estimated at up to 61% for moderate loneliness. 39 Only two studies, using data from a randomised controlled trial, compared loneliness across people with differing or multiple diagnoses, limiting our understanding of how loneliness may differ by condition at end of life. Methodologies and loneliness measurements differed across studies, there was wide variation in sample size and for the studies assessing correlates, there was inconsistent adjustment for covariates. Further, no study included a loneliness measure incorporating aspects of existential loneliness, of particular relevance to end of life populations. 22
Strengths and limitations of the review
Strengths of the review include the structured narrative approach, guided by accepted standards, and use of a broad definition of end of life, to capture the diversity of settings, conditions and uncertainty of timing. 16 Nevertheless, the broad definition may mean some studies were either missed or incorrectly included. Further, where studies retrospectively identified their sample by date of death, estimates of loneliness included individuals whose deaths were accidental and unrelated to terminal illness. Finally, we conducted a narrative review due to heterogeneity among studies. This resulted in reporting ranges of prevalence, considered preferable to producing a point estimate from studies with few similarities.
Implications for further research, policy and practice
Estimates of loneliness prevalence across a wider range of country contexts, care settings and conditions warrant further exploration. The 10 year health plan for England sets out an ambition for three radical shifts in how health care is delivered, including moving care into the community, rather than hospital settings. 75 This type of health system reform is occurring in other contexts globally. 76 It will be important to extend understanding of loneliness to all those dying at home, not only those receiving state-funded home care, and to institutional settings including care homes. 77 Exploration of how loneliness prevalence differs by condition and better understanding potential population risk factors is also important. With these priorities in mind, future research might investigate possibilities to modify a standardised loneliness measurement tool to incorporate existential loneliness, adapting the tool to better measure loneliness at end of life. This could include applicability across cultures, settings and with different patient groups. This review focussed on loneliness among people at the end of life, however, reviewing the literature specifically for carers at end of life would be beneficial.
For policy and practice, the review highlighted loneliness as an important consideration for the care and support of people at end of life. Loneliness is increasingly recognised as a societal issue in need of coordinated action 78 and the needs of people with advanced illness should be acknowledged in new policies and strategies. An integrative review of loneliness at end of life identified potentially modifiable factors to reduce or mitigate loneliness at end of life, operating at different levels. 27 At the individual level, these include interventions such as befriending services; at the meso level, opportunities to make care homes, hospitals and hospices more home-like environments; and at the macro level, compassionate communities to better support lonely individuals. 27 Tailored interventions need to be developed for diverse groups. 28 Underpinning evidence of loneliness prevalence and at-risk end of life population groups is critical to making the case for developing and funding these approaches and raising awareness among health and social care providers in community settings where palliative care may be less common. Evidence indicates integrated approaches are important, necessitating support at multiple levels, from staff training to recognise the signs of loneliness to mobilisation of community resources through compassionate communities.79,80
Conclusions
Evidence indicates a significant minority of adults at the end of life experience moderate or high loneliness. There is emerging evidence of higher loneliness among individuals with non-cancer compared to cancer conditions and multiple morbidity, though there are currently only two comparative studies. Correlates of loneliness at the end of life may include poorer mental health and some social and physical health factors. However, there was significant heterogeneity in study quality, loneliness measurement, country, care settings and conditions investigated, which limits interpretations across studies. Further research is needed in more countries and settings, and to assess the effectiveness of supportive interventions, better informing evidence-based approaches to recognising and mitigating loneliness at the end of life.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163261428936 – Supplemental material for Loneliness among adults at the end of life: A systematic review of prevalence and correlates
Supplemental material, sj-docx-1-pmj-10.1177_02692163261428936 for Loneliness among adults at the end of life: A systematic review of prevalence and correlates by Emma Maun, Clare Gardiner, Tracey McConnell, Kathy Seddon, Andy Woodhead and Briony Hudson in Palliative Medicine
Footnotes
Acknowledgements
We would like to acknowledge Irena Cenzer and Ashwin Kotwal for agreeing to provide subsample data from their original study, and Kate Maitland for providing advice on diagnoses indicating terminal illness.
Ethical considerations
This research reviewed published literature and did not require ethics approval.
Consent to participate
This research reviewed published literature and did not require participant consent.
Author contributions
EM and BH designed the study. EM, CG, TM and BH developed the search strategy, EM conducted the searches, EM and BH screened the records and extracted the data. EM assessed the risk of bias, carried out the narrative synthesis and prepared the manuscript. All authors provided critical input to the analysis and manuscript drafts. All the authors have read and approved the final version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors. EM and BH’s roles are funded by Marie Curie.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Clare Gardiner is a member of the editorial advisory board for Palliative Medicine.
Data availability statement
Data collated for this review are available from the authors on request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
