Abstract
Background:
Palliative care is increasingly framed as a public health matter, with a range of new research approaches. However, there is currently no consensus on a research agenda for Public Health & Palliative Care.
Aim:
To set a preliminary consensus-based Public Health & Palliative Care research agenda for the coming decade.
Design:
A mixed-methods Delphi study using qualitative focus groups and quantitative digital surveys using a digital questionnaire. Items were ranked on Likert scales for appropriateness, relevance, feasibility and impact. Research Priority Scores were calculated as mean item scores across criteria and raters. Average Expert Agreement was calculated as mean proportion of raters who scored the mode result on each criterion per item.
Setting/participants:
A snowball sample starting from an initial list of 86 academic experts and people with complementary expertise from 16 countries.
Results:
Sixty-five invited experts responded in Round 1, fifty-one in Round 2. Results found 47 item priorities. Forty-four items had high to very high research priority (≥6/8). Average expert agreement was high (≥70%) for 37 of the 47 items. Priority domains included representation and inclusion (of older people and people in structurally vulnerable positions), access to palliative care and equity in health and wellbeing outcomes, critical knowledge, skills and social networks, and methodological development.
Conclusions:
Findings suggest that future priorities for Public Health & Palliative Care research lie with representation and inclusion, access to palliative care and equity in health and wellbeing outcomes, critical knowledge, skills, social networks and methodological development.
Palliative care is increasingly framed as a public health matter, reflecting a further paradigm shift in our modern responses to the challenges of serious illness, dying and death.
A public health approach to palliative care entails a combination of science, skills and beliefs directed towards improving and maintaining wellbeing of those experiencing the challenges of serious illness, dying and grieving through societal or population-wide interventions/changes.
Delphi-group priority rankings suggest research into (1) representation and inclusion, (2) access to palliative care and equity in health and wellbeing outcomes, (3) impact of critical knowledge, skills and social networks and (4) methodological development in the field are key areas for development.
The presence of service-oriented priorities suggests a bias towards traditional healthcare and palliative care services that should be further investigated.
Our findings suggest that future priorities for Public Health & Palliative Care research lie with representation and inclusion, access to palliative care and equity in health and wellbeing outcomes, critical knowledge, skills and social networks, and methodological development.
Background
Much research has shown that the structural and social determinants of health account for most health outcomes 1 and inequities therein, 2 much more than healthcare services and professionals can address. A recent The Lancet Commission report on the value of death emphasised that this is similarly true for health and wellbeing outcomes around the end-of-life. 3 Additionally, literature shows that merely increasing or improving health is insufficient 4 to address increasing palliative care needs worldwide.5,6 Palliative care offers a vital corrective lens through which these gaps can be addressed.
As a movement in the 60s–70s, palliative care reacted against the highly medicalised and depersonalised way dying had been transformed. 7 As hospice and palliative care mainstreamed, palliative care obtained a specific domain (and power) with the rise of palliative medicine specialities, and creation of specialised palliative care services in different health care settings. With this, palliative care became increasingly associated with terminal care. In response, more emphasis has in recent decades been placed on upstreaming, that is, early initiation of palliative care alongside curative treatment, and on generalists taking up responsibility in palliative care.
Without positioning itself within public health, palliative care cannot possibly address the challenges it faces. However, public health is currently underprepared to address the mounting structural, social, psychological and existential needs of dying, grieving and caregiving populations. This has led to an emerging public health approach within palliative care8,9 – the name for which is still debated, but to which we refer as Public Health & Palliative Care. This perspective signifies a civic and social response to the broader health challenges resulting from serious illness, caregiving, dying and loss, moving beyond, but including health service responses. Public health approaches to palliative care encompass interventions and research focused on direct action targeting the population, advocacy, support and collaboration 10 around end-of-life challenges. It is rooted in the collaboration of specialist and generalist palliative care services with communities and neighbourhoods, and key civic institutions. 11
Applying a public health perspective to palliative care implies a recognition of the importance of policies and practices beyond clinical or health service contexts.8,12 While its’ usefulness is increasingly accepted – as evidenced by the emergence of specific textbooks, 13 journals 14 and conferences 15 focused on Public Health & Palliative Care – there is some debate as to what constitutes a public health approach to palliative care. Cohen 16 tries to reconcile different perspectives by broadly describing a public health approach to palliative care as the combination of sciences, skills and beliefs to improve and maintain wellbeing of those experiencing challenges of serious illness, dying and grieving. It integrates the functions of assurance (i.e. ascertaining adequate and equitable access to quality palliative care and medications, developing an adequately trained workforce and national policy that integrates palliative care services into the national health care system), assessment (i.e. assessing and understanding problems and needs of populations using tools of traditional public health such as epidemiology and policy evaluation) and action (i.e. through health promotion approaches such as asset-based community action and development).
With new paradigms come new questions, priorities and risks that, ideally, translate into a clear research agenda aimed at providing evidence, understanding and support. However, there has been relatively little systematic effort to identify a research agenda or research priorities for Public Health & Palliative Care. Since 2018, the Reference Group on Public Health & Palliative Care of the European Association for Palliative Care has held open meetings where academic, practitioner and community experts have emphasised the need to set research priorities. This inspired efforts to undertake a Public Health & Palliative Care research priority setting exercise.
The aim of this study was to propose a preliminary but distinct and specific research agenda for Public Health & Palliative Care for the next 10 years, through identification of expert consensus-based research priorities. The specific research question was: what research topics should be prioritised, according to Public Health & Palliative Care experts, in Public Health & Palliative Care research over the next 10 years based on their appropriateness, relevance, feasibility and potential impact?
Methods
Design
We conducted a mixed method, international online consensus Delphi study. The Delphi technique is used for consensus building and prioritising research and policy aims, especially when opinions from a range of international experts are to be consolidated in a concise report. 17 The process involved qualitative data collection in the form of idea generation for potential research priorities and open-ended evaluation by expert panellists of these ideas. We also conducted quantitative criteria-based priority evaluations using a digital questionnaire. See Figure 1 for more detail. We followed the CREDES guidelines to design and report this study. 18

Proposed stages of Delphi study adapted from Jünger et al. 17
Population
Our target expert population was defined as people with either research or other complementary expertise in Public Health & Palliative Care. The inclusion criteria used can be found in Box 1.
Inclusion criteria for experts.

Sample and recruitment process
A convenience sample and snowball method were used to recruit participants. The sample consisted of 86 international experts from 16 countries identified by steering group members of the EAPC Reference Group on Public Health & Palliative Care. Through snowballing, 90 additional experts were identified and included in our sample, for 176 experts in total.
Experts were sent an introduction letter outlining the scope, aims, methods of the study. We used ‘Public Health Palliative Care’ as a descriptor for the field during the study. The letter included a link to a digital form which requested the recipient’s voluntary participation, their permission for us to contact them again and a request for each expert to refer us to at least one more research expert and one person with complementary Public Health & Palliative Care expertise. We requested name, country, organisation, types of Public Health & Palliative Care activities and e-mail address of any referral. Suggested experts were sent the same digital form. In total, 83 experts agreed to participate.
Measurements (ranking criteria)
Following Viergever et al.’s 19 guidance on research priority setting exercises, we applied the CHNRI approach 20 which suggests the identification of research priorities based on pooling individual scorings of priorities using ranking criteria. As criteria we decided to use the categories suggested by Okello and Chongtrakul, 21 who suggest most research priorities can be assessed using four criteria: (1) Appropriateness: should we do it?; (2) Relevance: why should we do it?; (3) Feasibility: can we do it?; (4) Impact: what do the stakeholders get out of it? Since we have no prior assumptions regarding the importance of each criterion, we did not use weighting. Table 1 presents the operationalisations employed in the current study and the scale on which they were scored by participants.
Ranking criteria for future European research priorities in Public Health Palliative Care.

Instrument development
The digital Delphi survey questionnaire consisted of two parts. Part 1 asked participants to score a list of thematically categorised items using the ranking criteria, and to provide free-text comments to each item. See Supplemental Appendix 1 for free-text input. Part 2 contained demographic questions.
The questionnaire was cognitively tested for difficulty and clarity of the content, format and functionality with six volunteers across the authors’ affiliated institutions. In Round 1, the questionnaire provided participants with a list of 62 items. In Round 2, the questionnaire provided participants with a list of 47 items. Due to a concern that there may be a ceiling effect, the scale was revised and changed from a 5-point to an 8-point Likert scale between Rounds 1 and 2 to remove a neutral middle point and increase sensitivity. Each scale also added an additional option: ‘I don’t know enough about this topic to rate it’.
Data collection
Data was collected between June 2021 and May 2023. Each data collection round was followed by data analysis informing the next round, as described in Figure 1. All data was pseudonymised before data analysis.
Idea generation
One June 17th, 2021, experts were invited to participate in an online moderated idea generation brainstorming session on priority Public Health & Palliative Care research topics for the next 10 years. Thereafter, via an online questionnaire listing resulting themes, to participants were asked to list 1–3 research priorities/themes and add themes they thought were missing. These items were evaluated by all authors for specificity, tacit assumptions and whether they were actionable by research. We formulated all priorities as statements as these were considered clearer than questions. Items were removed if they were (a) clinical, policy or praxis priorities, or (b) were judged as too vague to be understood (see Supplemental Appendix I, Table A.2 for examples). Very similar or identical items were merged. Only minor changes were made to items for rephrasing into statements or to increase clarity.
Delphi survey
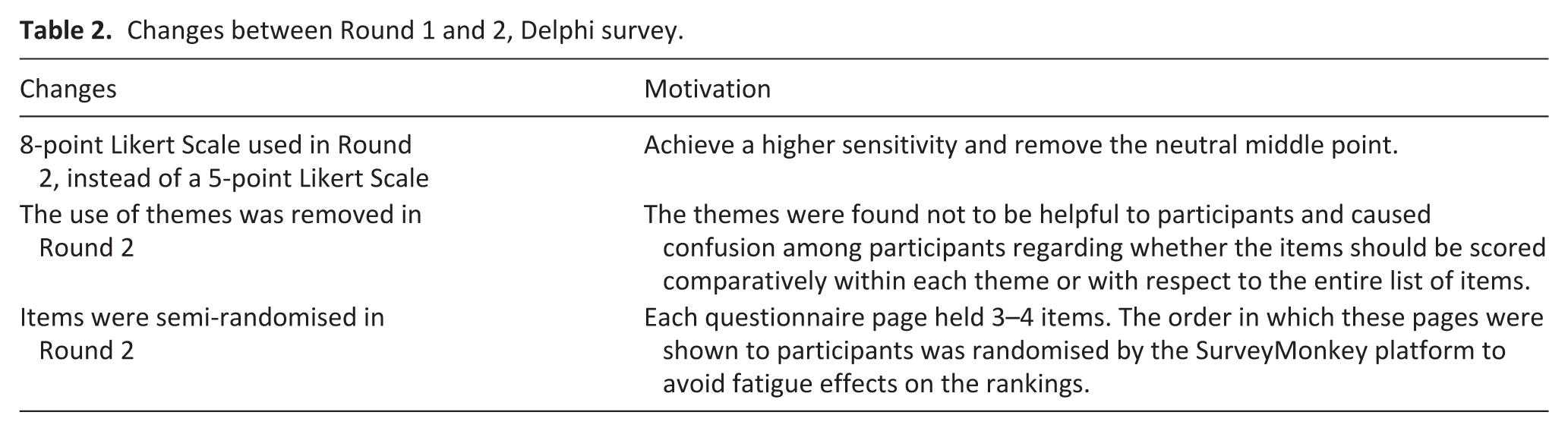
The digital survey questionnaire was sent via e-mail to 83 experts who agreed to participate (47% of identified experts). Survey Round 1 was sent to experts in August 2022. Survey Round 2 was distributed in November 2023, alongside structured feedback from Round 1. Changes were made to the survey between Rounds 1 and 2 (see Table 2).
Changes between Round 1 and 2, Delphi survey.
External validation
The final version of this report was sent to the Board of the European Association for Palliative Care for comments and approval as an EAPC White Paper. Approval was granted on 14 Jul 2025.
Data analysis
Figure 1 clarifies the various approaches to data analysis applied.
Qualitative data analysis
Inductive, thematic 22 analysis was conducted on the qualitative data collected from the two idea generation exercises (Stage 1) and the optional comment field data (Stages 3–4). Data was coded and analysed using NVIVO 12. 23 First author SV categorised specific suggestions for research priorities that emerged from the group discussions into overarching themes. This preliminary analysis was checked by two other researchers (JC, CT) and finetuned based on their feedback. SV added and expanded themes based on participant input and consolidated the collected priorities within each theme into single item statements. This analysis and consolidated list of statements were discussed and fine-tuned with the entire project group (CT, AH, SM, LS, LD, JC). This process resulted in a list of themes, each with priority items, which became the foundation for the survey questionnaire (Stages 2–4).
Quantitative data analysis
Quantitative data was processed using MS Excel and cleaned and analysed using IBM SPSS 26. We performed uni- and bivariate analysis on the quantitative data to calculate priority, consensus and change in agreement between successive survey rounds using Delphi survey data (Stages 3–4).
Priority
The final priority ranking is based on mean Research Priority Score, calculated per statement per participant as follows:
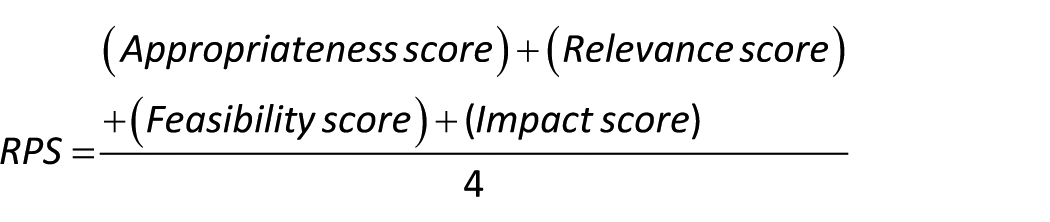

In Round 1 we used a 5-point Likert scale. The scores were interpreted as follows: ⩽2.5 = no or low priority; 2.6–3.5 = uncertain; ⩾3.6 = high to very high priority. In Round 2, we used an 8-point Likert scale. The scores were interpreted as follows: ⩽4 : no or low priority; 4.1–5.9 = uncertain; ⩾6 = high to very high priority.
Consensus
Consensus is defined as Average Expert Agreement, calculated per item as the mean of the proportions of scorers who gave the most frequent response per criterion:
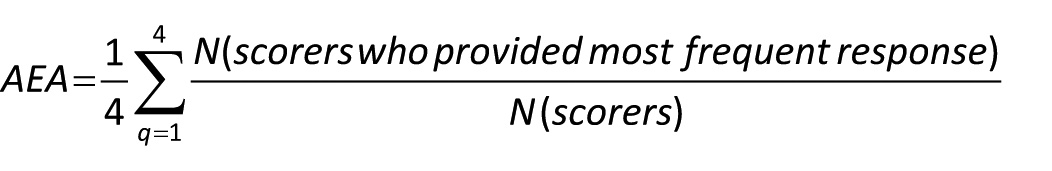
Where q is 1 of the 4 criteria questions used to evaluate competing research priorities.
Agreement scores are presented as percentages and are intended to contextualise the mean Research Priority Score per item. Consensus is often defined as a percentage of agreement. 18 The literature suggests that a threshold of 70% for agreement is appropriate to suggest a high degree of convergence in expert opinion.18,24 Average Expert Agreement is interpreted using the following cut-off scores: <30% = disagreement; 30%—70% = uncertainty; >70% = agreement. In cases of disagreement or uncertainty, changes were made based on respondent suggestions provided via the open-answer questions in the survey.
Results
Idea generation of priority themes
Thirty-eight people from 14 countries participated in the session. Participants mainly came from the UK (24%), Australia (16%), Belgium (13%), Sweden (8%) and Germany (8%). Thematic analysis resulted in the construction of nine themes covering empirical, conceptual and methodological priority topics for international Public Health & Palliative Care research in the next 10 years. The subsequent idea generation survey (see Figure 1) resulted in 122 items in 9 themes (see Table 3).
Themes resulting from the Idea Generation rounds 1 and 2.

In total 46 items were removed, 14 were merged, 41 were changed, and 21 remained unchanged. This resulted in 62 items for ranking. (See Supplemental Appendix I, Table A.3.)
Delphi survey: Socio-demographics
Sixty-five (78%) experts responded in Round 1; fifty-one (62%) responded to Round 2. The majority of respondents were 40–59 years old (56% in Round 1; 63% in Round 2) and women (62% in Round 1; 57% in Round 2). In Round 1, experts were mainly from Australia (16%), the UK (16%), Sweden (14%), Belgium (12%) and Switzerland (12%). Round 2 had less representation from Australia (7%), and more from the UK (24%). Most reported being researchers (61% in Round 1; 50% in Round 2) and clinicians (27% in Round 1; 28% in Round 2). In Round 2, several experts also described a managerial or coordinating involvement in Public Health & Palliative Care (13%). See Table 4 for a demographic overview of the samples.
Demographics per Delphi round.
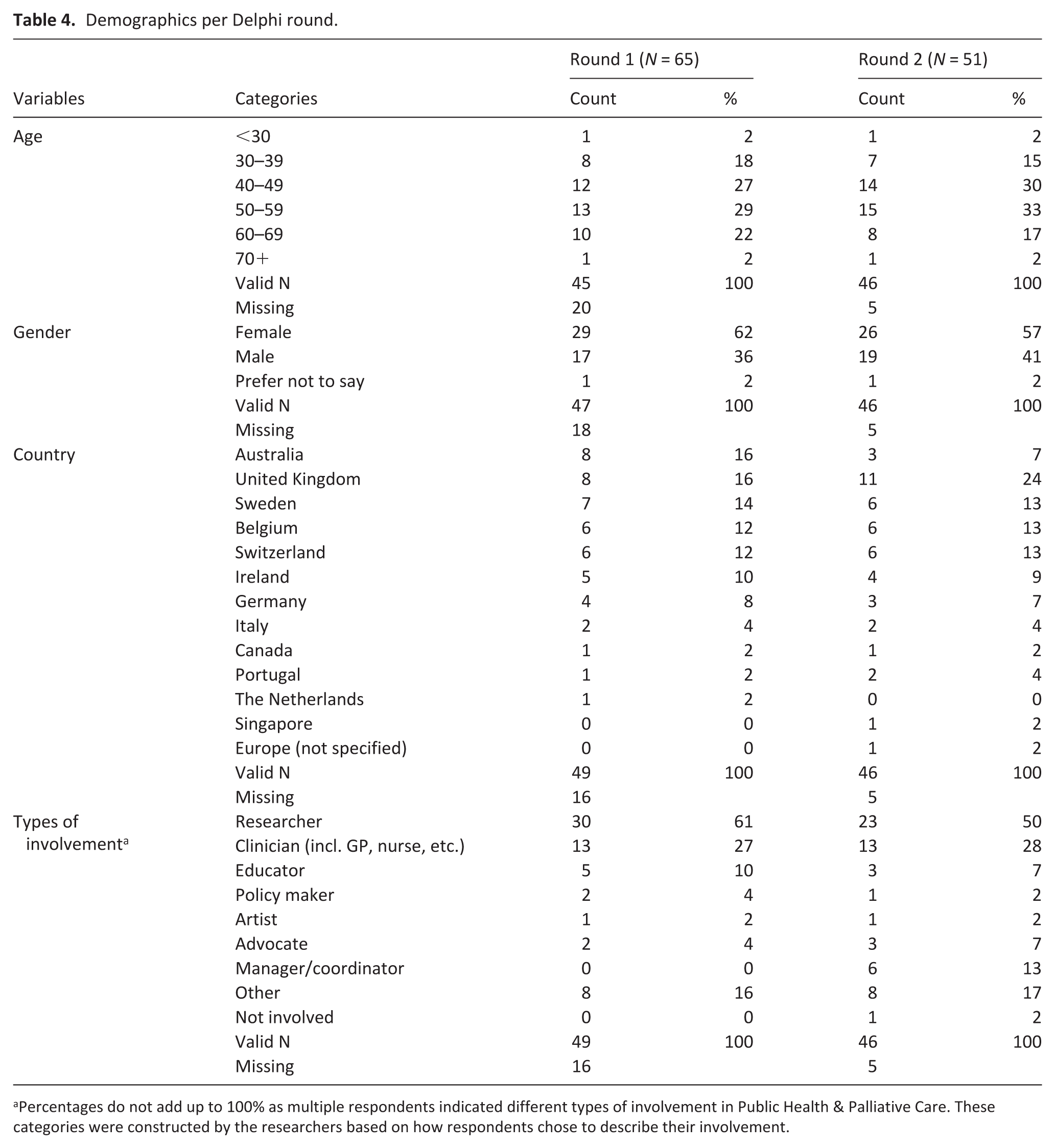
Percentages do not add up to 100% as multiple respondents indicated different types of involvement in Public Health & Palliative Care. These categories were constructed by the researchers based on how respondents chose to describe their involvement.
Delphi survey: Round 1
Research priority and average expert agreement scores
After Round 1, 50 items (81%) had a high to very high Research Priority Score (>3.5), 11 items (17.7%) scored as uncertain (2.5–3.5), and one item scored as low priority (<2.5). Table 5 shows the Round 1 top 10 research priorities based on Research Priority Score. Thirty-six items (58%) achieved an Average Expert Agreement score of 70% or higher, indicating expert agreement regarding their priority and 26 items (42%) scored uncertain agreement (30%—70%). No items indicated disagreement (<30%).
Top 10 research priorities, Delphi Survey Round 1.

RPS: Research Priority Score; AEA: Average Expert Agreement.
Processing of Round 1 items
Based on the Research Priority and Average Expert Agreement scores and the qualitative feedback, the following changes were made between rounds: 17 items were removed, one due to a low priority score (Item 32: ‘Investigate the strengths and limitations in Kastenbaum’s death system model for understanding Public Health & Palliative Care initiatives and their effects/impact’; Research Priority Score of 2.48/5). The other 16 items were removed after merging with other items or because they had vague or leading formulations in the free-text responses. Twenty-seven items were changed based on the qualitative open-answer question data. One item was split into two distinct items. No changes were made to the 18 remaining items. This resulted in a new list of 47 items for Round 2. See Supplemental Appendix I (Table A.4) for the complete list of items with changes made at each step. An overview of the processing of and changes made to items between rounds 1 and 2 were provided to the participants invited to Round 2 as part of the structured feedback.
Delphi survey: Round 2
After Round 2, 44 items (94%) had a high to very high Research Priority Score (>6), 3 items (6%) scored as uncertain (4–6), and none scored low (<4). Item 21 had the highest Research Priority Score: ‘Represent and involve older people with care needs and their caregivers in palliative care research’ (7.02/8). Item 39 had the lowest Research Priority Score: ‘Investigate how climate change affects access to, delivery and quality of palliative and End-of-Life care’ (4.99/8). Thirty-seven items (79%) achieved Average Expert Agreement scores of 70% or higher, indicating expert agreement regarding their priority, whereas 10 items (21%) scored between 30% and 70%, indicating uncertainty and none scored <30%. Table 6 shows the research priority ranking from Round 2.
Research priority ranking by RPS and AEA, Delphi Survey Round 2.
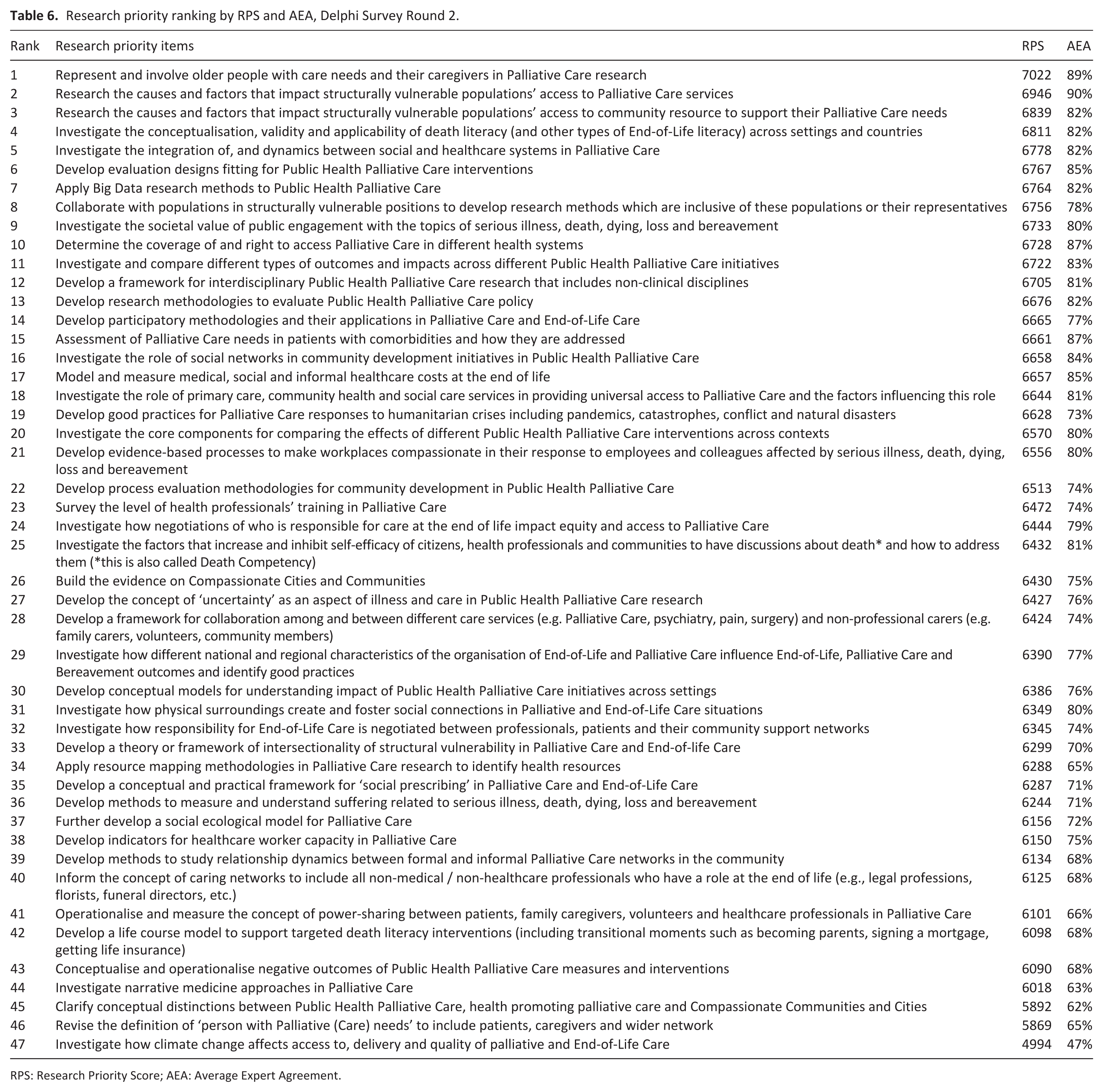

RPS: Research Priority Score; AEA: Average Expert Agreement.
See Supplemental Appendix I for details on the individual ranking criterion scores. All criteria showed improvements from Round 1 to Round 2.
Discussion
Main findings
This Delphi study resulted in 47 items that represent potential future international priorities for Public Health & Palliative Care research based on the input and rankings by experts in the field from 16 countries. Forty-four (94%) items had high to very high priority scores. Overall, experts displayed high agreement for 37 (79%) of the 47 items. Prominent priority domains included representation and inclusion (of older people and people in structurally vulnerable positions), access to palliative care and equity in health and wellbeing outcomes, critical knowledge, skills and social networks, and methodological development for Public Health & Palliative Care. We reflect on each of these below.
Strengths and limitations
This study involved a broad and highly international network of Public Health & Palliative Care experts, including researchers, practitioners, community developers, educators, advocates and more, and boasts response rates of 78% (Round 1) and 62% (Round 2). We applied an extensive brainstorming process and several opportunities for experts to provide qualitative feedback. The instrument was fine-tuned between rounds to increase scoring sensitivity. Finally, the paper was reviewed and approved by the EAPC Board, an international authority in palliative care. Although tailoring between rounds improved Research Priority and Average Expert Agreement scores, it made comparing scores for specific items impossible. Additionally, data suggested that after Round 2 the list still had room for further refinement. The priorities presented here are therefore a first iteration of a research agenda for the Public Health & Palliative Care field, intended to inspire discussion. Approximately 30% of panel experts were from countries outside Europe as the EAPC and EAPC Reference Group on Public Health & Palliative Care membership is not limited to Europe. Additionally, we identified many research priorities in Public Health & Palliative Care with high to very high Research Priority Scores.
Several important limitations should also be considered. First, it may have been interesting to compare priority scores and agreement between academic experts and non-academic experts. Unfortunately, we do not have complete data on types of involvement of participants in Public Health & Palliative Care. Next, we do not know how many respondents only responded to Round 1 versus only to Round 2. Third, demographic data collection was limited during idea generation, and we did not gather data on languages spoken or other linguistic factors. It is possible that the results were influenced by being framed in English terms and that English speakers were overrepresented in the results. Next, the Delphi methodology itself has limitations. Priority setting often reflects established experts’ interests rather than a forward-looking Public Health & Palliative Care research agenda. The presence of service-oriented priorities suggests that Public Health & Palliative Care is still shaped by experts with a background in traditional healthcare and palliative care services. Furthermore, our panel consisted primarily of experts from higher-income countries, yet access to palliative care remains a major issue in Lower- and Middle-Income countries. The dominant framings of public health issues are likely to have also influenced the set priorities, creating a circular problem as described by Tannahill. 25 However, Delphi methods can also offer a way to look beyond the constraints of prior and present funding of established priorities. Finally, quantitative measures are inherently limited in representing the significance of priorities and should be complemented by more nuanced qualitative insights going forward. It should therefore be remembered that presentation of these data is a first preliminary step in a hitherto unexplored area.
Key research domains
As the differences in scores between items were small, we consider the prominent priority domains in the ranking (in bold below) to make sense of the general priorities represented here.
Several highly rated items emphasised representation and inclusion, particularly of older people 27 and those in positions of structural vulnerability, 28 aligning with recent research on participation in health 26 and equity in palliative care. 27 This emphasis on participatory research approaches and collaboration between researchers and these target populations aligns with much of the Public Health & Palliative Care literature focusing on community-based approaches to end-of-life challenges (e.g. Compassionate Communities, 28 ageing and dying in place 29 and the decolonisation of the end of life 30 ).
The priority given to access to palliative care and equity in health and wellbeing outcomes is closely tied to the previous domain. Echoing the report by The Lancet Commission on the Value of Death, 3 identifying the factors driving disparities in access to services and support remains a key research concern. This aligns with existing work highlighting how social determinants of health shape palliative care accessibility.29,31,32 These items also emphasise access to supportive environments (e.g. workplaces, schools) when faced with End-of-Life challenges as an important avenue for research.
Additionally, several items point to the priority of studying the development and impact of critical knowledge, skills, and social networks as individual and community resources in End-of-Life support. The explicit inclusion of the concepts of Death Literacy 33 and Death Competency 34 underscores a growing need to understand how well prepared and supported individuals and populations feel in providing End-of-Life support and how this preparedness can affect End-of-Life experiences and outcomes. The proliferation of literacy concepts in Public Health & Palliative Care research (e.g. Grief Literacy, 35 End-of-Life Health Literacy 36 ) reflects the rising interest in literacy as a critical resource for public health. Future research should adapt these concepts to diverse socio-cultural contexts, including lower- and middle-income countries.
Finally, several items emphasised the need for methodological development for Public Health & Palliative Care. Given the field’s interdisciplinary nature, establishing appropriate frameworks for evaluating interventions, programmes or policies 37 is essential. Some initial efforts into transdisciplinarity, include Bakelants et al. 38 who identified implementation science frameworks suitable for Compassionate Communities evaluations. Further methodological advancements should consider complexity-aware mixed-methods research to capture quantitative outcomes, qualitative experiences and systems-based approaches that account for the complex interactions between health, social care, and community networks.
Future research
Future studies should apply methodologies that seek innovation beyond what is already known. Researchers may consider a broader review of the literature at the intersection of Public Health and Palliative Care, synthesising research recommendations (e.g. Riffin et al. 39 ) and classifiers that signal ignorance (known unknowns; e.g. Boguslav et al. 40 ) from review and consensus documents to complement the current agenda. Decision support techniques, such as the analytic hierarchy process (Lambooij and Hummel 41 ) are uniquely suited to explore innovation preference structures among and between different stakeholder groups. Such methods may help uncover why our research priorities consistently scored lowest on the feasibility ranking criterion, which may have implications for policy and educational initiatives. Additionally, this priority-setting exercise should be done in different languages and language communities to broaden the research agenda. Finally, to uncover the real ‘known unknowns’ and ‘unknown unknowns’, real innovation will need to come from transdisciplinary, cross-sectoral collaboration and increased attention in research to real-world complexity.
Conclusion
Our findings suggest that prominent future priorities for Public Health & Palliative Care research are focused on representation and inclusion (of older people and people in structurally vulnerable positions), access to palliative care and equity in health and wellbeing outcomes, critical knowledge, skills and social networks, and methodological development for Public Health & Palliative Care. Our findings provide a foundation for advancing Public Health & Palliative Care research by identifying key thematic priorities. However, this study should be viewed as a starting point for ongoing discussions rather than a definitive research agenda. Future work should further refine and expand these priorities, incorporating diverse perspectives, including those from Lower and Middle Income Countries, different language communities, diverse stakeholders and community-based practitioners.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163261418440 – Supplemental material for EAPC White Paper: What are the priorities for Public Health & Palliative Care research in the coming decade? Results from an International Delphi study
Supplemental material, sj-docx-1-pmj-10.1177_02692163261418440 for EAPC White Paper: What are the priorities for Public Health & Palliative Care research in the coming decade? Results from an International Delphi study by Steven Vanderstichelen, Carol Tishelman, Agnes van der Heide, Sonja McIlfatrick, Libby Sallnow, Luc Deliens and Joachim Cohen in Palliative Medicine
Footnotes
Acknowledgements
We would like to acknowledge the Board of the European Association for Palliative Care evaluating and approving the manuscript, and the entire steering committee of the EAPC Reference Group on Public Health & Palliative Care who commissioned this work and were the driving factors behind it.
Ethical considerations
This study was commissioned by the European Association for Palliative Care (EAPC) reference group on Public Health & Palliative Care. Approval was sought from the EAPC Board, and from the Commission for Medical Ethics (CME) of the executive researchers’ host institution (Vrije Universiteit Brussel). The protocol was sent to the CME of the University Hospital of Brussels and approval was granted on 27 October 2022 (B.U.N. 1432021000565). Approval for amendments to extend the period of data collection was received on 09 November 2022 and 19 July 2023 respectively.
Consent to participate
Consent to participate and for the publication of their responses as study findings was assumed upon completion and return of the questionnaire.
Author contributions
All authors (SV, CT, AvdH, SMc, LS, LD and JC) (i) made a substantial contribution to the concept or design of the work; or acquisition, analysis or interpretation of data, (ii) drafted the article or revised it critically for important intellectual content, (iii) approved the version to be published and (iv) have participated sufficiently in the work to take public responsibility for appropriate portions of the content.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was in part supported by a Senior Postdoctoral Fellowship from the Flemish Research Foundation (FWO) under grant nr 1200424N.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data are kept by the corresponding author and will be shared only upon reasonable request.*
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
