Abstract
Background:
Quantifying palliative care needs and whether they are met is essential for effective service planning and provision. Estimates of palliative care needs are widely reported but less is known about unmet needs, with no accepted definition of this construct or guidance on how to measure it.
Aim:
To investigate how unmet palliative care needs for adults with advanced life-limiting illness have been defined, measured, and reported in the evidence.
Design:
Scoping review following the Joanna Briggs Institute guidelines: protocol registered on Open Science Framework (10.17605/OSF.IO/M8DHA).
Data sources:
In October 2024, we searched MEDLINE, EMBASE, CINAHL, and PsycINFO for quantitative and mixed-methods studies published after 2000, with backward and forward citation and manual searching of grey literature. Data on definitions, measurement and reporting of unmet needs were extracted, charted, and summarised narratively using inductive content analysis and framework synthesis.
Results:
Seventy studies were included: 9 reviews and 61 primary evidence studies from 16 countries. Only 11 (16%) studies explicitly defined unmet palliative care needs. We identified three approaches to measurement of unmet palliative care needs: (1) prevalence of symptoms and concerns; (2) access to services (e.g. specialist palliative care); and (3) sufficiency of service provision to resolve symptoms and concerns.
Conclusions:
This novel review identifies a lack of consensus in defining, measuring and reporting unmet palliative care needs. We propose three distinct approaches to conceptualising unmet palliative care needs and outline their strengths and limitations. Practical guidance on their use is provided to support researchers, clinicians, and policymakers in selecting appropriate approaches for assessment and reporting.
Existing research and policy often report prevalence of palliative care needs with limited consideration to the extent to which needs are met or unmet.
Assessing and quantifying unmet palliative care needs is critical for guiding healthcare planning and delivery, but clear guidance on how this construct should be defined and measured is lacking.
Few studies provide a clear, detailed definition of unmet palliative care needs.
We identify three main approaches to measuring unmet needs in palliative care research, by quantifying: (1) Symptoms and concerns; (2) Access to services; and (3) Sufficiency of service provision to resolve symptoms and concerns.
There is little focus on non-cancer populations and few reports of involvement of patients and carers in studies measuring unmet palliative care needs.
Methodological strengths and limitations of the three identified approaches to measuring unmet palliative care needs are discussed.
To address the knowledge gaps identified, recommendations for reporting of definitions and how these are operationalised are provided.
Background
With population ageing, rising multimorbidity, and increasing health-related suffering,1–4 providing timely and adequate palliative care is becoming a major public health priority. Despite palliative care being recognised as a human right, 5 barriers to access persist, leaving some needs unmet. Assessing and quantifying unmet palliative care needs of a population is essential to inform effective planning and delivery of services and reduce inequitable access,6–8 yet guidance on how best to define and measure this construct is lacking.
Unmet healthcare needs are a concern at individual, group, and societal levels, as they are associated with poorer quality of life, adverse health outcomes, increased risk of hospitalisation and urgent care use, and higher healthcare costs.9–11 In healthcare research, care needs are commonly defined using Bradshaw’s typology as the “ability to benefit from healthcare services.” 12 Care needs can be further categorised as: (1) felt need (individual perceptions of need); (2) expressed need (perceived need resulting in demanded care); (3) normative need (defined by experts and thus largely based on healthcare professionals’ perceptions), and (4) comparative need (needs compared across different groups). 12 While other frameworks for conceptualising need exist, for example, Maslow’s hierarchy of need, Bradshaw’s typology is particularly useful in palliative care as it highlights who determines the need (which influences what is reported as need) rather than simply the what the need is. 13
A needs assessment is a process to determine need for care services in relation to health problems, either at the individual level (e.g. clinical assessments of patients’ healthcare needs) or population-level (e.g. evaluating community needs for care services). 14 A review by Franks et al. 15 identified two main methods for population-level palliative care needs assessment. The first is an epidemiological approach that estimates needs in a patient population based on mortality data of specific life-limiting conditions that may require palliative care and symptom prevalence among patients in advanced stages of these illnesses. The second is an approach based on healthcare service use, which assesses palliative care needs by analysing patterns in service usage data, such as hospice admissions or referrals to home care teams. However, both approaches have limitations. The epidemiological approach relies on mortality and symptom data that might not be readily available and does not specify care required to meet palliative care needs. The service use approach, on the other hand, only captures patients already accessing care, thereby overlooking those not known to palliative services.
It is also vital to understand how many do not have their palliative care needs met. Reported prevalence of unmet palliative care needs in the literature is inconsistent, largely due to methodological variability. A systematic review by Harrison et al. 16 showed that between 1% and 93% of people with cancer have unmet palliative care needs. Similarly wide prevalence estimates across care domains have been reported by Wang et al. 17 The lack of an accepted definition of unmet palliative care needs makes estimations difficult, especially at the population-level.
The present review expands on Franks et al.’s findings by focussing on unmet palliative care needs while broadening the scope beyond prior reviews, which have often focussed on unmet needs in specific patient groups or care settings.18,19 To inform our search strategies for, we constructed operational definitions of “palliative care needs” and “unmet palliative care needs” from definitions of needs and unmet needs in the broader health and care literature20–23 and the World Health Organisation’s classification of palliative care as a holistic care approach to improve the quality of life of patients with life-limiting illness and their families.5,24 To operationalise this, we defined palliative care needs as “the ability for people with life-limiting illness to benefit from available care to manage a range of symptoms and concerns including physical, psychological, social, spiritual, informational, and practical.” These needs can be addressed by specialist and/or generalist palliative care professionals, or a combination of both. 25 We defined unmet palliative care needs as “the difference or gap between required or expected care and actual care received by people with life-limiting illness.”
This review aimed to clarify concepts in the literature by addressing the question: How have unmet palliative care needs for adults with advanced life-limiting illness been defined, measured, and reported in the evidence?
Methods
Design
This scoping review follows the methodological guidelines set out by the Joanna Briggs Institute (JBI) 26 and is reported according to the Preferred Reporting Items for Systematic Reviews and Meta Analyses extension for Scoping Reviews (PRISMA ScR). 27 The review protocol was registered on the Open Science Framework (https://doi.org/10.17605/OSF.IO/M8DHA).
Eligibility criteria
We included studies reporting quantitative data on how unmet palliative care needs of adults (aged 18+ years) with advanced life-limiting illness were defined, measured and reported. Table 1 presents the full inclusion and exclusion criteria. Peer-reviewed quantitative and mixed-methods studies were included, as were systematic and scoping reviews reporting results from quantitative and mixed-methods studies. Grey literature (reports but not published abstracts) that quantitatively measured unmet palliative care needs was also included. Only English-language sources were included. To ensure that the review built on the review by Franks et al., 15 we only included papers and grey literature evidence published in 2001 or after.
Inclusion and exclusion criteria for the literature database searches.
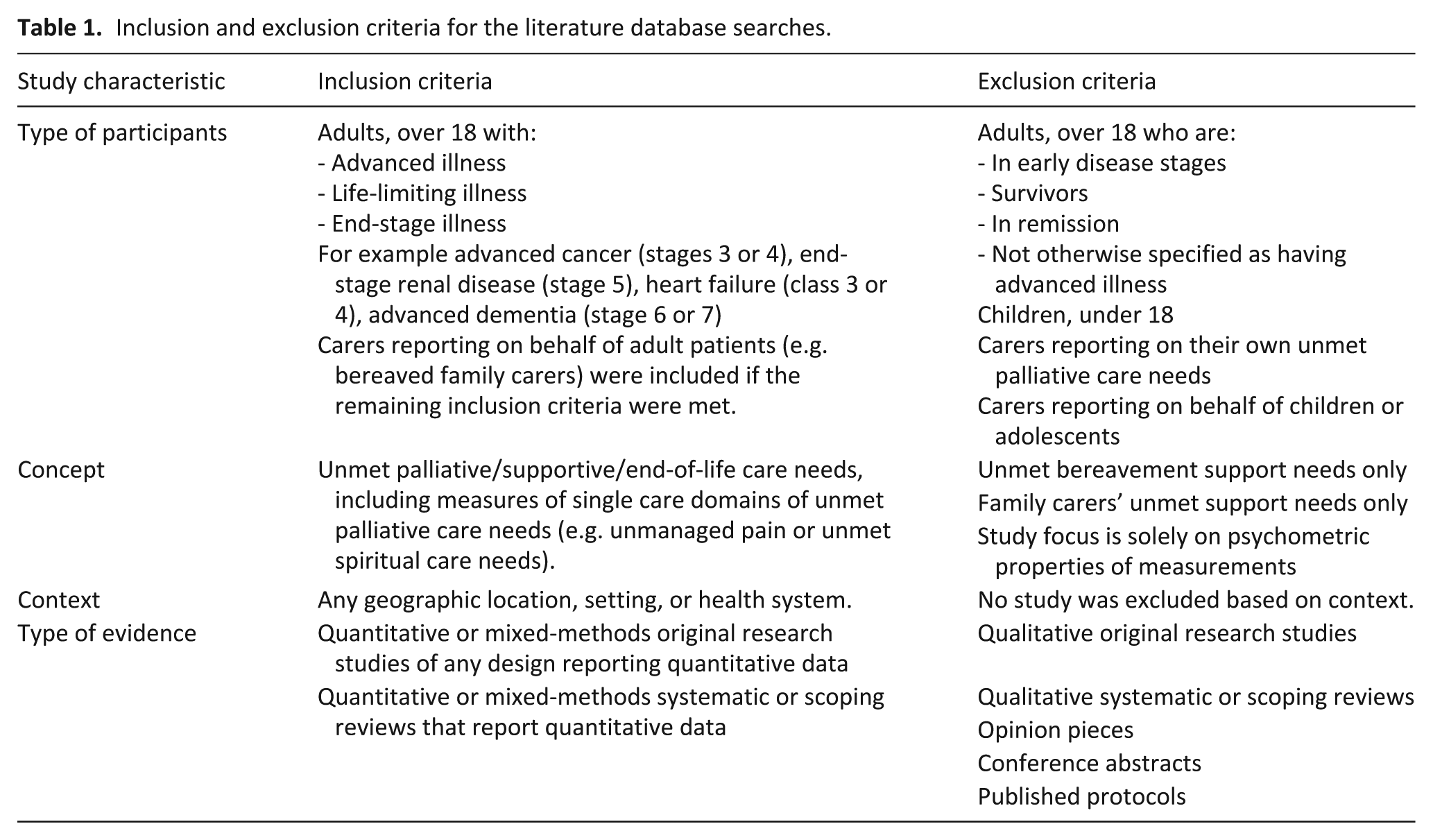
Search strategy
An initial PubMed scoping search of identified relevant published articles and identify target papers. Keywords from titles and abstracts and index terms assigned to the articles from the initial search informed the final search strategy for MEDLINE (Ovid), EMBASE (Ovid), CINAHL (EBSCO) and PsycINFO (Ovid; see Supplemental File 1). The search strategy was developed in collaboration with an information specialist and adapted for each database and/or information source. Target papers for inclusion in the search strategy were set to check the robustness of the search. All databases were searched on 2 October 2024.
Grey literature was hand-searched by one reviewer (MD) across relevant websites (Hospice UK, National Council for Palliative Care, Marie Curie, Macmillan Cancer Support, The Kings Fund, The Nuffield Trust, RAND and RAND Europe, The Lien Foundation, The Health Foundation, The Strategy Unit and World Health Organisation). Additional grey literature was identified through Open Grey and Google Scholar (using the first 100 references). 26 Forward citation searching of included studies was undertaken using Scopus.
Study selection
All papers identified from the searches were imported into Covidence and duplicates removed. Titles and abstracts were screened against the inclusion criteria by a single reviewer (TJ/MD/LF/AF), with a subset of 20% papers independently screened by a second reviewer to ensure screening consistency. Full-text screening was conducted by a single reviewer (TJ/MD), with 20% independently screened by a second reviewer (AF/LF) to check agreement. Any disagreements were resolved through discussion with a third reviewer.
Data extraction and charting
Data from eligible papers and evidence sources were extracted verbatim, where possible, by a single reviewer (TJ/MD/AB) using a bespoke data extraction form in Covidence (see Supplemental File 2). A second reviewer (AB/AF) independently checked 20% of the extracted data for accuracy. Any discrepancies between the reviewers were settled through discussion with a third reviewer.
Our extraction form was adapted from the JBI template 26 to fit the review aim and capture data on study characteristics (e.g. authors, publication year, study design, population) and how unmet palliative care needs were defined, measured, and reported (e.g. presentation of study findings of prevalence of unmet needs). For included systematic reviews, only review authors’ definitions and operationalisations of unmet palliative care needs, and conclusions regarding its measurement were extracted (excluding primary study results). Data were extracted at study-level; if several papers reported the same study, only one set of data was extracted. Data were recorded and analysed in Microsoft Excel.
Data analysis
Following scoping review guidance, no quality appraisal was conducted, as the aim was to provide a descriptive overview of the available evidence rather than assess study quality.28,29 Data analysis focussed on summarising relevant study findings, both by charting and by narrative summary using inductive content analysis.26,30 Whether studies defined unmet palliative care needs or not was inductively coded as “yes” (a clear explanation of the construct within a palliative or supportive care context), “partially” (addressing unmet needs within a palliative or supportive care context, often using prior research findings suggesting issues with palliative care access, but without explicitly delineating the construct) and “no” (no explanation of the construct).
To identify and map the dimensions of unmet palliative care needs captured in existing measures, we conducted a framework synthesis26,31 based on the domains in Goni-Fuste et al.’s 32 review of comprehensive palliative care needs assessments, encompassing Physical, Psychological, Spiritual, Social, Information, Financial/legal (e.g. preparing wills), Practical (e.g. household tasks), Autonomy (e.g. dependency on others), Role activities (e.g. difficulties with employment), Personal issues (e.g. handling personal affairs), Healthcare (e.g. support from healthcare professionals). Domains were added as needed. 31
Results
The searches and study inclusion are presented in a PRISMA flow diagram in Figure 1. 33 The database searches identified a total of 4513 references after duplicates were removed. Following the title and abstract screening, 274 references were sought for full-text review. After full-text screening against inclusion and exclusion criteria, 75 references were included, reporting on 70 unique studies.
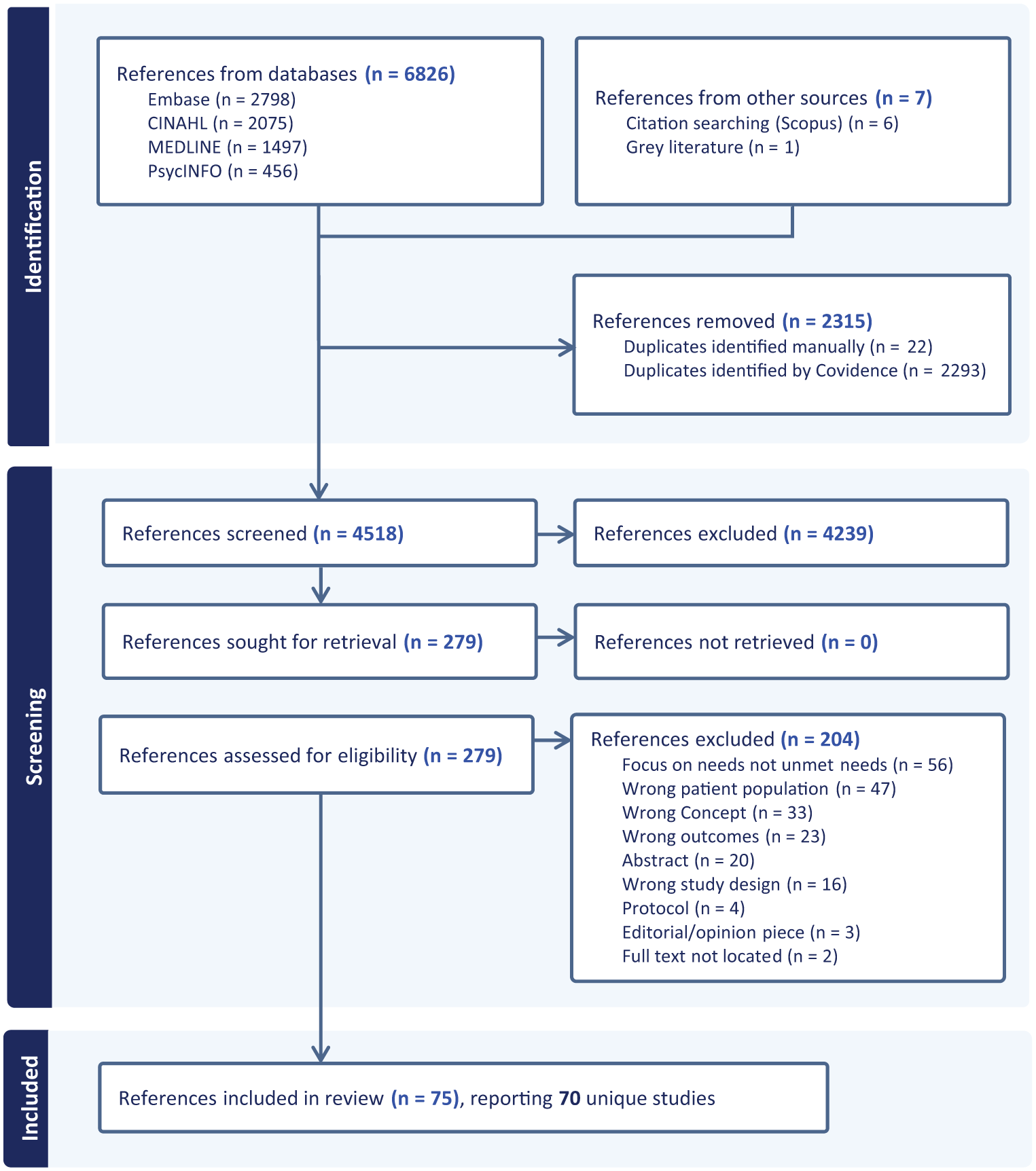
PRISMA flow diagram of study selection.
The 70 included studies were published between 2001 and 2024. In total, 61 were primary evidence studies (i.e. original research),34–95 and nine were reviews.16,17,96–102 The original studies (n = 61) were conducted in 16 countries, primarily Western countries such as the United States (n = 23), Australia (n = 9), Canada (n = 5), and the United Kingdom (n = 5).
Study descriptives
Study designs
Details of study characteristics (n = 70) are presented in Table 2. Most included studies used observational designs: commonly cross-sectional (n = 43, 59%), prospective cohort (n = 8, 11%), and retrospective cohort (n = 6, 9%) designs. The primary evidence studies that directly measured unmet palliative care needs, mostly used convenience samples (n = 49, 80%). Only two primary evidence studies reported on patient and public involvement (PPI): one mentioned PPI input when developing the measure, 91 and one other pilot-tested their questionnaire to ensure it was not too distressing. 36
Characteristics of included studies (n = 70), ordered by study design.
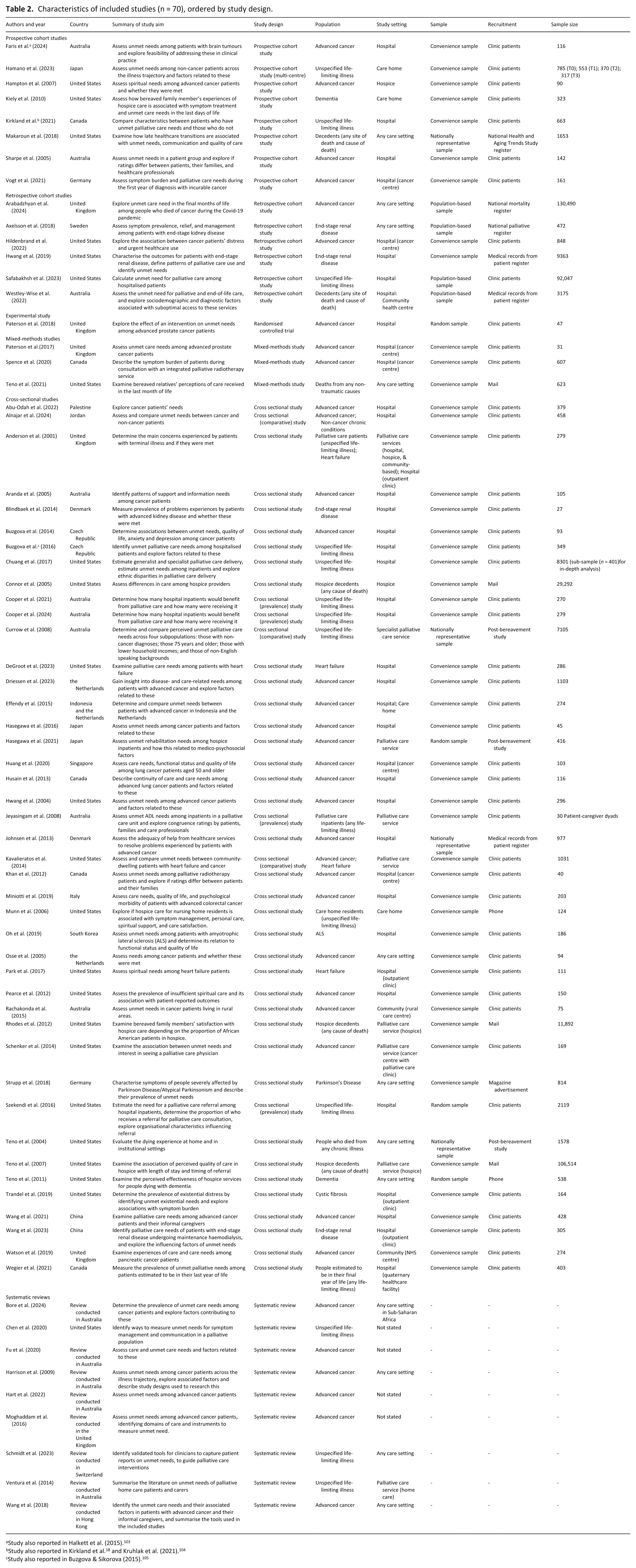
Study also reported in Halkett et al. (2015). 103
Study also reported in Buzgova & Sikorova (2015). 105
Populations and settings
As shown in Table 2, most studies (n = 45, 64%) focussed on unmet palliative care needs within a single disease group, commonly advanced cancer (n = 36, 51%), with three (3%) studies comparing two groups. One-third of studies (n = 23, 33%) included patients or decedents with any life-limiting illness. Study settings varied: most studies used hospital settings (n = 40, 57%; including cancer centres and outpatient clinics), whereas 11 (16%) focussed on palliative care services (including hospices, hospital units, and home care). Eleven (16%) studies included participants from any care setting, and four (6%) did not specify a setting.
Definitions of unmet palliative care needs
Details of how studies defined, measured, and reported unmet palliative care needs are presented in Table 3. Only 11 (16%) studies explicitly provided a definition of unmet palliative care needs, whereas 23 (33%) partially defined the concept – often with reference to prior research on care needs. More than half (n = 36, 51%) provided no definition.
Study definitions, measurement and reporting of unmet palliative care needs in the included studies (n = 70).
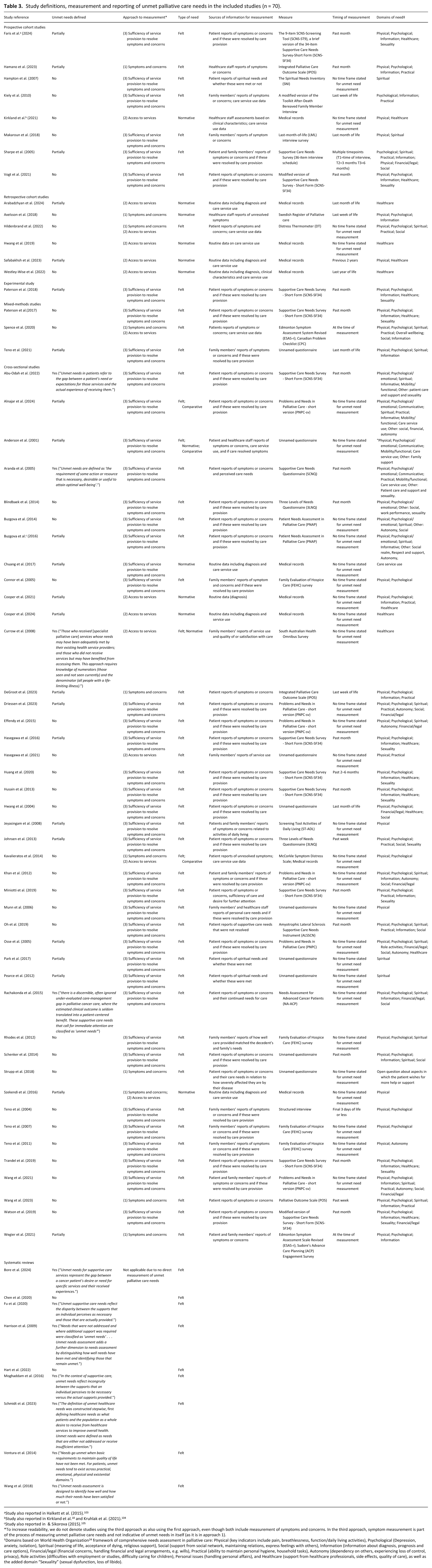
Study also reported in Halkett et al. (2015). 103
Study also reported in & Sikorova (2015). 105
To increase readability, we do not denote studies using the third approach as also using the first approach, even though both include measurement of symptoms and concerns. In the third approach, symptom measurement is part of the process of measuring unmet palliative care needs and not indicative of unmet needs in itself (as it is in approach 1).
Domains based on World Health Organization 24 framework of comprehensive needs assessment in palliative care: Physical (key indicators include pain, breathlessness, function/daily living activities), Psychological (Depression, anxiety, isolation), Spiritual (meaning of life, acceptance of dying, religious support), Social (support from social network, maintaining relations, express feelings with others), Information (information about diagnosis, prognosis and care options), Financial/legal (financial concerns, handling financial and legal arrangements, e.g. wills), Practical (ability to maintain personal hygiene, household tasks), Autonomy (dependency on others, experiencing loss of control, privacy), Role activities (difficulties with employment or studies, difficulty caring for children), Personal issues (handling personal affairs), and Healthcare (support from healthcare professionals, side effects, quality of care), as well as the added domain “Sexuality” (sexual dysfunction, loss of libido).
Definitions varied but often emphasised a perceived discrepancy between the care required or desired and the care received, such as “the disparity between the supports that an individual perceives as necessary and those that are actually provided.” 98 Other definitions highlighted presence of unfulfilled care needs, for example, “needs that are either not addressed or receive insufficient attention.” 101 Some studies focussed on specific outcomes, for example, conceptualising unmet palliative care needs as lacking “the requirement of some action or resource that is necessary, desirable or useful to attain optimal well-being” 38 or “when basic requirements to maintain quality of life have not been met.” 102
Partial definitions were usually presented as part of the study rationale, to suggest that care needs in specific patient groups or care settings might not be met. One study stated that “problems in the quality of life are not always correctly identified, and needs for care sometimes remain unmet.” 93 Other studies implied that known issues of under-utilisation of palliative care meant that care needs might not be met, such as arguing that “Deficits in [palliative] care in any domains may result in multidimensional, unmet needs”. 48
Where studies specified care services that can help address unmet palliative care needs in their definition, few were explicit about which these services were or made any distinction between specialist and generalist palliative care.
Measurement of unmet palliative care needs
Approaches to measurement
While few studies defined unmet palliative care needs, most described the approach used to measure it (i.e. the operationalisation), whether explicitly or implicitly. We identified three main approaches to measuring unmet palliative care needs: (1) Symptoms and concerns (studies using symptom prevalence to indicate unmet palliative care needs, without explicitly determining whether these symptoms were addressed or not); (2) Access to services (studies focussing on measuring service referrals or contacts, with little consideration of care outcomes); and (3) Sufficiency of service provision to resolve symptoms and concerns (studies addressing a perceived gap between the care provided and care deemed necessary to resolve symptoms and concerns). These approaches were not mutually exclusive and occasionally combined to varying degrees. Examples of each approach are presented in Box 1.
Examples of approaches to measuring unmet palliative care needs in the included studies.

Symptoms and concerns
The first approach to measurement of unmet palliative care needs relates to identifying and reporting the presence of one or more symptoms or concerns. Descriptions of what constituted a symptom or concern varied. Some studies narrowly focussed on certain levels of specific symptoms, for example, prevalence of pain being operationalised as having unmet need for pain relief. 39 Other studies acknowledged accumulation of several symptoms or concerns, or these being present across various domains as indicating unmet needs,48,52 while others included anything that the patient deemed a problem or concern. 81 Studies focussing on symptoms and concerns were often based on self- or proxy- reports of felt needs (in contrast to normative needs).
Access to services
The second approach to measurement of unmet palliative care needs relates to the access to or provision of care. This includes absence of referral to specific services (such as specialist palliative care) for people who might benefit from this care, for example, due to having specific diagnoses or other clinical characteristics. Access to palliative services (whether generalist or specialist) was generally presumed to meet needs and often described in terms of maintaining or improving quality of life, whereas lack of contact with palliative services was indicative of unmet needs. These studies were often larger-scale studies using medical records 78 or clinical screening tools, for example, the Palliative Care and Rapid Emergency Screening (P-CaRES) tool, 66 to make inferences about people missing out on palliative care receipt at cohort- or population- level. As such these largely represent normative needs, that is, as determined by professionals. 12 This approach seldom distinguished between types of palliative care services, for example, studies reporting overall rates of palliative care referrals.45,47,82 Availability of palliative care services was generally assumed, with only one study explicitly considering the lack of services across geographical regions. 80
Sufficiency of service provision to resolve symptoms and concerns
Most studies’ approaches to measuring unmet palliative care needs related to insufficient care provision. This included the presence of symptoms, concerns or problems that were either not addressed at all, not adequately addressed (according to the patient or their family), or not satisfactorily resolved (for which the patient wanted further professional attention). This approach emphasises a gap or discrepancy between a desired or expected standard of care and what has been provided. Studies often measured insufficient provision of care by asking patients or proxies (usually patients’ families or, less commonly, healthcare professionals) first whether a problem or concern was present and then the extent to which it was adequately provided for and addressed, thus primarily capturing felt need. 12 This approach was primarily used by small-scale survey studies using convenience samples to describe patients’ perspectives on the presence of unresolved issues, although some were larger scale.56,84
Sources of information for measuring unmet palliative care needs in primary evidence studies
Among primary evidence studies (n = 61) that measured unmet needs, methods for measurement varied in terms of who and what was the source of information for the assessment (see Table 3). Most studies used self-reported data (n = 39, 68%) collected using research questionnaires or patient reported or patient-centred outcome measures (PROMs or PCOMs). Proxy-reported data by bereaved family members, for example, using mortality follow-back surveys were also common (n = 15, 25%). These methods largely capture felt needs (i.e. an individual’s perceived need for care). Clinical assessments by healthcare professionals (often through use of screening tools; n = 8, 11%) or researchers (n = 8, 11%) were less common, representing normative need. 12
Instruments and timing of measurement in primary evidence studies
As shown in Table 3, named instruments or measures were used in 42 (69%) of the primary evidence studies, whereas nine (15%) used unnamed questionnaires, and one (2%) used an unnamed structured interview. The most commonly used named measure was the Supportive Care Needs Survey - Short Form (SCNS-SF34; n = 8, 13%), followed by the Problems and Needs in Palliative Care-short version (PNPC-sv; n = 5, 8%), both of which were initially developed for cancer patients. Unmet palliative care needs were estimated using administrative medical records in nine (15%) studies.
Almost half of the studies did not report the time period during which unmet palliative care needs were measured (n = 30, 49%). Of those that specified a time interval, self-reported unmet needs commonly related to the past month (n = 15, 25%). In studies using samples of decedents, the time interval of interest was usually the last month of life (n = 4, 7%) or last week of life (n = 3, 5%). Only three studies reported longitudinal measurements of unmet palliative care needs over time.52,88,94
Reporting of unmet palliative care needs in primary evidence studies
Some of the 61 primary evidence studies reported unmet palliative care needs at the item-level, usually as the proportion of patients with a specific unresolved symptom or concern.39,44,85 Most, however, reported unmet needs at the domain-level by combining responses to several items related to a specific domain of care (e.g. Oh et al. 70 and Pearce et al. 74 ). Our mapping of the unmet care needs reported in the primary evidence captured 11 distinct domains of needs (Table 3). Ten of these were identified in the framework by Goni-Fuste et al., 32 with the addition of “Sexuality” which was reported in 14 (23%) studies. Of the 52 primary evidence studies that measured unmet palliative needs using a questionnaire or interview, most used multi-domain measures that allowed a holistic assessment of unmet palliative care needs: 38 (73%) captured three dimensions or more, while only four (8%) focussed solely on one domain (spiritual needs53,71,74 and physical function 61 ).
In total, 26 studies (43%) reported one single metric of unmet palliative care needs, usually as a percentage of participants needing palliative care but not adequately receiving it. These rates ranged from 10% in a 2023 study of hospitalised patients in United States 78 to 30% among people with non-cancer conditions in a 2008 health omnibus survey in Australia. 47 Other studies calculated unmet palliative care needs by aggregating items and/or domains from the measure used, which was commonly reported as prevalence of having one or more unmet needs (e.g. “71.8% of patients reported at least one unmet supportive care need” 88 ), sometimes with reference to severity (e.g. “48% reported one or more moderate or high unmet needs” 91 ). Some studies presented a mean or median number of unmet palliative care needs within the group (e.g. “The median number of total unmet needs identified was 3” 79 ).
Discussion
Key findings
This scoping review examines how existing evidence has defined, measured and reported unmet palliative care needs across disease groups and care settings. Only 11 out of 70 (16%) defined the theoretical construct of unmet palliative care needs. The review also found variability in approaches to measurement and reporting across studies, identifying three main approaches to measuring unmet palliative care needs: (1) the presence or severity of symptoms and concerns; (2) the level of access to palliative care services; and (3) symptoms and concerns that remain unresolved despite service provision.
Unmet palliative care needs were commonly identified using self-reported data about the presence of symptoms and concerns and whether these were resolved by the care provided. Similar to previous reviews on unmet palliative care needs in the emergency department 106 and in nursing homes, 107 we found that the lack of explicit definition hinders consistent measurement and comparisons across studies, making it difficult to determine how best to measure or estimate unmet needs at the population-level. This lack of clarity creates ambiguity about what is being assessed and risks conflating unmet palliative care needs with related concepts, such as satisfaction with care or quality of life. There is also a conceptual distinction between unmet palliative care needs as outcomes (e.g. inadequate pain relief), and reasons for unmet needs (e.g. not accessing to palliative care services), which was rarely noted in the included studies.
Expanding on the findings of Franks et al. 15 on population-level assessments of palliative care needs, our review identifies three approaches to measuring unmet needs in the existing international literature.
The first approach, Symptoms and concerns, involves quantifying prevalence or burden of problems. This approach corresponds to Franks et al. 15 epidemiological approach and is not dependent on whether patients are known to services or not. Patient-reported or patient-centred outcome measures (PROMs and PCOMs) can be very helpful for collecting these data and, depending on how many domains a measure captures, this approach enables a holistic assessment of palliative care needs. For example, the Integrated Palliative care Outcome Scale (IPOS) is a valid and reliable measure for multi-domain symptoms and concerns, allowing evaluation of the complexity of needs for care. 108 Wide international use of PROMs and increasing integration with patient record systems further aids access to comparable data for research. Nevertheless, this approach has limitations, as presence of unresolved symptoms or concerns does not necessarily mean professional help is desired, and it may not clarify which professionals or services should meet any unmet needs identified.
The second approach, Access to services, infers unmet palliative care needs from access to services, aligning with Franks et al.’s 15 healthcare utilisation approach. Service use is usually documented in medical records and often readily available in national patient registers, which facilitates their use in research, policymaking, and commissioning. While evaluating access to services, for example, referrals, can elucidate care gaps or inequities indicative of underserved populations, this approach requires that patients are correctly identified as having palliative care needs in the first place. 109 Moreover, uptake of palliative care services might not reflect actual needs for care, 47 and access to services alone cannot indicate whether needs are met or if the care delivered improves the patient’s situation. 95
The third approach identified in this review, Sufficiency of service provision to resolve symptoms and concerns, is the most comprehensive as it combines aspects of the first two in operationalising unmet palliative care needs (presence of symptoms and concerns but also whether services adequately addressed these). This approach is also the only that captures forgone care. Studies using this approach more often distinguished between having an unmet problem and desire for care, showing that patients did not necessarily want professional attention even for serious problems, especially within social, sexual, and spiritual domains.62,74,93 This approach is helpful for evaluating outcomes of care and person-centredness, 110 that is, not only determining whether symptoms are present or if care is delivered, but whether the care meets individual needs. However, focussing on the gap between desired and received care can risk overestimating unmet palliative care needs if expectations of symptom relief at the end of life are unrealistic. For example, a symptom like fatigue 111 is known to be common towards the end of life but difficult to fully relieve even with optimal currently available treatment. Studies adopting this approach must consider the subjective nature of measurement and how the person making the assessment might influence estimations of unmet need, since reports of symptom relief can vary between family members and healthcare professionals. 112
Each approach has its strengths and limitations, and all can help estimating unmet palliative care needs, depending on context and research question. For example, the Symptoms and concerns approach is well suited for intervention studies to assess changes in needs over time in response to a care intervention. The Access to services approach is helpful for service mapping studies, and the Sufficiency of service provision to resolve symptoms and concerns approach could be used to inform future post-bereavement survey research. Appropriateness of the approaches may also vary according to the healthcare system from which the evidence is derived. 113 As already mentioned, the approaches do not distinguish between which services should meet which level of unmet palliative care needs. Future research should examine how variation in service use might be associated with management of unmet needs across the physical, psychological, spiritual and social domains. The high proportions of unmet palliative care needs reported in the included studies also raise questions about “acceptable” levels of unmet needs at the population-level. While the goal should be to prevent suffering, achieving complete resolution of all symptoms and concerns for every individual is unlikely given finite care resources. Some degree of unmet needs may therefore be inevitable. The definitions of unmet palliative care needs presented in this review cover a wide span, ranging from care required for optimal well-being 38 to basic requirements for maintaining quality of life, 102 and provide little clarity about what constitutes a feasible standard.
What this review adds
Resource limitations invariably mean that specialist palliative care access is prioritised for the most urgent and complex cases, 114 and it is not surprising that the existing research has focussed on identifying specialist palliative care needs. However, better understanding of whether specialist palliative care services meet patients’ needs is crucial to inform decision-making about funding, planning and delivering high-quality care. 115 Despite 25 years since Franks et al.’s 15 review highlighted poor-quality and inconsistent population-level estimates of palliative care needs, the literature is still largely based on cross-sectional studies using self-reported data from convenience samples, with few studies using population-based or representative samples.
To provide a comprehensive understanding of unmet palliative care needs, multi-domain multi-level assessments like those presented in the third approach to measurement are well-suited to capture both felt and normative need, particularly when combining objective data sources, like service provision, and subjective experiences of the care received. In Box 2 we provide further recommendations for advancing research, policy and practice and building a more robust evidence-base for estimating the prevalence of unmet palliative care needs in the general population. Additional considerations of data collection methods are provided in Supplemental File 3.
General and audience-specific recommendations based on the review findings.
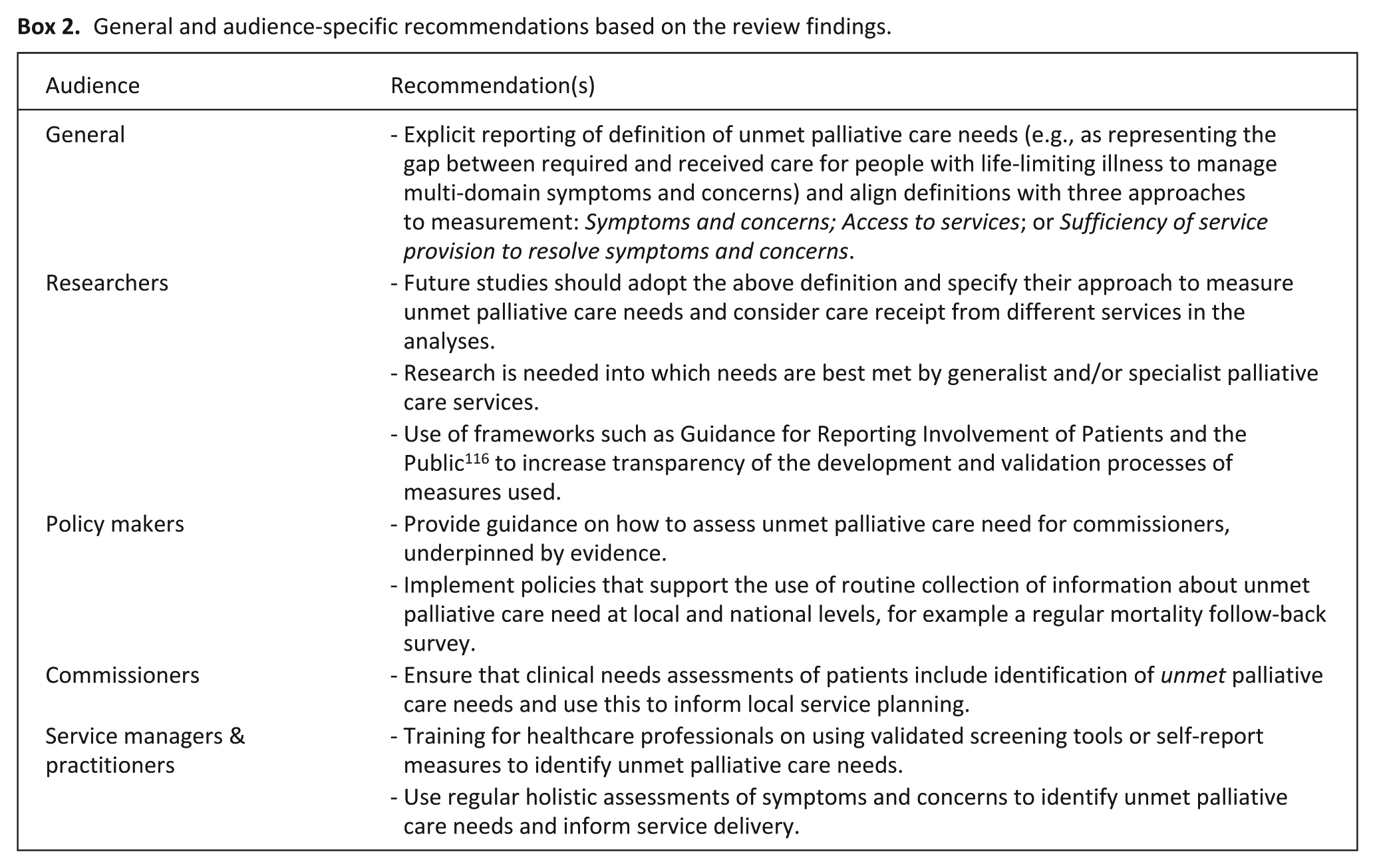
Routine data collection from continuous multi-domain needs assessments is crucial to advance the understanding of unmet palliative care needs at the population-level and inform policymakers and commissioners in the planning and delivery of palliative and end-of-life care.23,117 For studies using administrative data from medical records, standardising the use of clinical variables in screening tools would enhance consistency in identification of unmet palliative care needs. Challenges remain, however, regarding how needs are disclosed, as limited awareness of available services or resources can hinder people from recognising they have unmet palliative care needs, 118 and lack of trust and power imbalances can hinder requests for support, particularly for potentially sensitive topics such as mental health issues, living situations, or family relationships. 79
Strengths and limitations
This is the first scoping review to summarise how unmet palliative care needs has been defined, measured and reported in existing literature. While prior reviews have focussed on the psychometric properties of measures of unmet palliative care needs,18,19,119 this review contributes with new knowledge about overarching theoretical and operational aspects of the existing evidence on unmet palliative care needs.
A strength of this review is the inclusion of grey literature as well as use of forward and backward citation searches to mitigate the risk of omitting relevant sources. We present data at the study-level, thereby avoiding double counting duplicate data sets across sources. 29 Although the methodological variation of included studies hindered conclusions to be drawn regarding prevalence of unmet palliative care needs, this is not a limitation for the current scoping review since the aim was to identify and describe the breadth of existing evidence and not synthesise study findings. 120
By not limiting our inclusion criteria to specific disease groups or care settings, we provide a comprehensive overview of how unmet palliative care needs has been researched in various contexts, regardless of diagnosis, with the objective to expand on the work of Franks et al. 15 and further the understanding of how prevalence of unmet palliative needs are measured. However, our review also has limitations. Including only quantitative or mixed-methods studies and reviews reduces the range of evidence sources and may limit the completeness of the findings, as we might have missed important conceptual work from qualitative sources. The lack of quality appraisal and risk of bias assessment is another inherent limitation to scoping reviews, 121 but also allows for a more rapid review process.
Conclusion
This is the first scoping review to summarise the existing literature on how unmet palliative care needs have been defined, measured and reported across disease groups and care settings. Even though quantification of unmet palliative care needs is crucial for planning and equitable delivery of palliative care services, our review demonstrates that studies rarely explicitly define the construct and there is considerable variation in how unmet palliative care needs are measured and reported. Clear reporting of definitions and operationalisations of unmet palliative care needs is required to harmonise the evidence base and subsequently enable estimation of the proportion of people with unmet needs at the population-level. We identify three distinct approaches to measurement of unmet palliative care needs – (1) symptoms and concerns; (2) access to services; and (3) sufficiency of service provision to resolve symptoms and concerns – and provide guidance on their use for various end-users.
Supplemental Material
sj-docx-1-pmj-10.1177_02692163261416279 – Supplemental material for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence
Supplemental material, sj-docx-1-pmj-10.1177_02692163261416279 for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence by Therese Johansson, Melanie F. J. Diggle, Anne Finucane, Joanna M. Davies, Irene J. Higginson, Katherine E. Sleeman, Lorna K. Fraser, Fliss E. M. Murtagh and Anna E. Bone in Palliative Medicine
Supplemental Material
sj-docx-2-pmj-10.1177_02692163261416279 – Supplemental material for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence
Supplemental material, sj-docx-2-pmj-10.1177_02692163261416279 for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence by Therese Johansson, Melanie F. J. Diggle, Anne Finucane, Joanna M. Davies, Irene J. Higginson, Katherine E. Sleeman, Lorna K. Fraser, Fliss E. M. Murtagh and Anna E. Bone in Palliative Medicine
Supplemental Material
sj-docx-3-pmj-10.1177_02692163261416279 – Supplemental material for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence
Supplemental material, sj-docx-3-pmj-10.1177_02692163261416279 for Defining and measuring unmet palliative care needs among people with life-limiting illness: A scoping review of international evidence by Therese Johansson, Melanie F. J. Diggle, Anne Finucane, Joanna M. Davies, Irene J. Higginson, Katherine E. Sleeman, Lorna K. Fraser, Fliss E. M. Murtagh and Anna E. Bone in Palliative Medicine
Footnotes
ORCID iDs
Ethical considerations
Ethical approval was not required for this review as there was no direct patient contact or access to individual participant data.
Author contributions
T.J. and M.D. were responsible for the design of the study, with critical input from all authors. M.D. and T.J. developed the search strategy, M.D. conducted the searches. T.J., M.D., A.F, and L.F. screened articles for inclusion. T.J., A.B., A.F., and M.D extracted data. T.J. charted the data; A.B., T.J and M.D. conducted qualitative synthesis. All authors contributed to analysis and interpretation of data. T.J. drafted and revised the manuscript. All authors critically revised the manuscript for intellectual content, and read and approved the final manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was conducted as part of the DUE_Care (Defining and estimating unmet palliative care needs in the UK) project, which is funded by the end-of-life charity, Marie Curie, and carried out by King’s College London (grant MCCRP-23-02). Marie Curie supports research into palliative and end of life care to improve the care that is provided to people affected by any terminal illness. For more information visit ![]() . I.J.H. is an UK National Institute for Health and Care Research (NIHR) Senior Investigator (Emeritus), F.E.M.M is an NIHR Senior Investigator, and L.K.F is an NIHR Research Professor. The views expressed in this article are those of the authors and not necessarily those of the UK NIHR, or the UK Department of Health and Social Care. AF is funded by a Marie Curie Senior Research Fellowship (MCRFS-20-101). K.E.S. is the Laing Galazka Chair in palliative care at King’s College London, funded through an endowment from Cicely Saunders International and the Kirby Laing Foundation.
. I.J.H. is an UK National Institute for Health and Care Research (NIHR) Senior Investigator (Emeritus), F.E.M.M is an NIHR Senior Investigator, and L.K.F is an NIHR Research Professor. The views expressed in this article are those of the authors and not necessarily those of the UK NIHR, or the UK Department of Health and Social Care. AF is funded by a Marie Curie Senior Research Fellowship (MCRFS-20-101). K.E.S. is the Laing Galazka Chair in palliative care at King’s College London, funded through an endowment from Cicely Saunders International and the Kirby Laing Foundation.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
