Abstract
Background:
Socially excluded populations have poorer access to care; however, little attention has been paid to lesbian, gay, bisexual and/or trans* people. Lesbian, gay, bisexual and/or trans* people are at increased risk of certain life-limiting illnesses and may not receive the care and support they need at the end of life and into bereavement.
Aim:
To identify and appraise the evidence of the bereavement experiences of lesbian, gay, bisexual and/or trans* people who have lost a partner and develop an explanatory model of lesbian, gay, bisexual and/or trans* partner bereavement.
Design:
Systematic review (in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines) and thematic synthesis with assessment of reporting and rigour. Quantitative or qualitative articles reporting bereavement experiences of lesbian, gay, bisexual and/or trans* partners were included, excluding articles reporting multiple losses in the context of HIV or AIDS.
Data sources:
PsycINFO, MEDLINE, Web of Science, Scopus, Cochrane Library. Inclusion dates: database inception – 30 April 2015.
Results:
A total of 23 articles reporting on 13 studies were identified. Studies described universal experiences of the pain of losing a partner; however, additional barriers and stressors were reported for lesbian, gay, bisexual and/or trans* people, including homophobia, failure to acknowledge the relationship, additional legal and financial issues and the ‘shadow’ of HIV or AIDS. A novel model was developed to explain how the experience for lesbian, gay, bisexual and/or trans* people is shaped by whether the relationship was disclosed and acknowledged in life and into bereavement and how this impacts upon needs and access to care.
Conclusion:
There is a need for healthcare providers to avoid hetero-normative assumptions; be mindful of additional stressors in bereavement for lesbian, gay, bisexual and/or trans* people; and consider additional sources of support to deliver individualised holistic care.
Socially excluded populations have poorer access to healthcare.
People who identify as lesbian, gay, bisexual and/or trans* (LGBT) have increased risk of certain life-limiting illness, but evidence suggests that they may not access the care and support they need towards the end of life.
LGBT people continue to report discrimination from healthcare providers and fear discrimination in bereavement.
Loss of a partner is associated with universal experiences of grief, pain and struggling to continue with life alone, regardless of sexual identity or gender history.
However, LGBT people face additional barriers and stressors in bereavement, including homophobia, failure to acknowledge their relationship, additional legal and financial issues and the ‘shadow’ of HIV or AIDS.
A new theoretical model is proposed which explores the interaction between disclosure and acceptance of LGBT relationships, and how that may impact upon bereavement experiences.
There is a need for healthcare professionals to avoid assumptions of heterosexuality, explore identity sensitively in line with preferences for disclosure and consider additional sources of support to ensure LGBT people receive the individualised holistic care they need in bereavement.
Introduction
Grief and bereavement are universal human experiences of adjustment after a death. Recent theories of grief have moved beyond a staged or phased understanding,1–3 to models which recognise the active nature of grief as the survivor navigates pain and loss and begins to restore their identity as an individual, 4 and find a new place for the relationship with the deceased. 5 Recent models have also recognised factors that shape the grief experience, including social mediators and concurrent stressors. 6 Social factors that may lead to disenfranchised grief have been recognised, where the deceased had a stigmatised death or where the relationship with the deceased was not acknowledged or publicly recognised, limiting the individual’s access to support and the grieving role. 7
Bereavement heavily impacts those closest to the deceased. 8 Those who performed a caregiving role are 20%–50% more at risk of mental health problems in bereavement than non-caregivers. 9 Individuals who have lost their primary relationship are less likely to seek medical attention where necessary, 10 are at increased odds of worsened or new illness 11 and have increased mortality. 12 Compared to non-bereaved individuals, bereaved people have significantly worse health prior to, and in the year following, bereavement and are significantly less likely to be employed up to 2 years post bereavement. 13
There is increasing recognition that lesbian, gay, bisexual and/or trans* (LGBT) communities represent minority groups with specific healthcare needs.14,15 People who identify as LGBT are at increased risk of life-limiting illnesses, including certain cancers,16–18 and exhibit more risk behaviours linked to experiences of discrimination.19–22 A recent systematic review described a potentially increased need for palliative care among these communities. 23 Isolation is more common among the LGBT communities, particularly among the older generations, 24 who may face additional barriers when accessing healthcare, resulting in a reluctance to share their identity with healthcare professionals. 25 Moreover, experiences of discrimination against LGBT people are still common in healthcare settings.26,27 A recent UK survey of 522 lesbian, gay or bisexual adults identified that 34% had concerns about arranging end-of-life care and 24% expected to face barriers relating to their sexual identity when planning a funeral. 28
In light of the above, and the significant impact of bereavement on those closest to the deceased (partners), the aim of this review was to identify and appraise the evidence of the bereavement experiences of LGBT people who have lost a partner and to develop a new explanatory model of bereavement to aid clinicians in delivering holistic, individually tailored support among the LGBT communities. The specific study objectives were to (1) identify the literature, (2) appraise the quality and reporting, (3) synthesise the literature and (4) build a novel theory of LGBT bereavement experiences from the existing literature.
Methods
Search strategy
Our systematic literature review and thematic synthesis, with appraisal of scientific reporting and quality, was undertaken in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. 29 We searched titles, abstracts and keywords of articles indexed within five databases (PsycINFO, MEDLINE, Web of Science, Scopus and Cochrane Library) from database inception to 30 April 2015. Search terms were developed and piloted with an information specialist, to ensure broad inclusivity, and included a combination of the following terms: bereave* OR grief* OR griev* OR mourn* AND lesbian OR gay OR bi*sexual* OR trans*gender* OR homo*sexual*. For articles selected for full-text review, the listed references were hand searched for additional relevant articles.
Inclusion criteria were qualitative or quantitative primary studies reporting the experiences of LGBT people whose partner had died. Exclusion criteria were (1) studies reporting experiences of bereavement outside of the LGBT communities (or studies that did not disaggregate LGBT from heterosexual or cisgender experiences); (2) studies reporting social losses (e.g. employment and financial losses); (3) studies reporting losses of other relationships (friends, siblings, parents, children and other relatives) or that did not separate description of other relationship losses from the loss of a partner; (4) studies reporting multiple losses in the context of HIV or AIDS, rather than loss of the primary relationship; (5) case reports (not research); (6) studies not reporting primary research; (7) studies not published in peer-reviewed journals; and (8) studies not published in English.
Two authors (K.B. and S.M.) screened the titles and abstracts, and articles were excluded according to the exclusion criteria. Full text of the remaining articles was appraised against the inclusion criteria by all authors. Each included article was assessed for reporting by two authors using the consolidated criteria for reporting qualitative research (COREQ) criteria 30 for qualitative articles (K.B. and S.M.) or the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement 31 for quantitative and mixed methods articles (K.B. and R.H.). Each article was assessed for methodological rigour by two authors (K.B. and R.H.) using the Hawker et al. checklist, 32 designed to appraise evidence when reviewing disparate data (rates nine components – very poor 0, poor 1, fair 2 and good 3). Rather than relying on a total score, the checklist enables the reader to make an assessment about the different aspects of the study. Articles were not excluded on the basis of the assessment of rigour. If necessary the senior author (R.H.) adjudicated decisions on inclusion, exclusion, reporting and quality rating.
All text, including quotations reported in the article, under the headings of ‘results’ or ‘findings’ were imported verbatim into Nvivo 10 qualitative data software. A thematic synthesis of the data was performed, 33 using three consecutive phases: (1) line by line coding of the results of included studies; (2) development of descriptive themes encompassing the themes or codes of the primary studies, with particular attention to similarities and differences across and between studies; and (3) development of analytical themes, going beyond presentation of the original data. Findings from the quantitative studies were summarised descriptively and incorporated into the synthesis and thematic framework. The findings from the thematic synthesis were used to develop an original model to explain LGBT experience of partner bereavement.
Results
Search yield
Our search yielded 697 articles. After removal of duplicates (233), 426 articles were excluded according to the stated criteria. A total of 38 articles were retained for full-text review, after which a further 17 were excluded. Two further articles were added from the references of included articles (see Figure 1 for the PRISMA flow diagram).
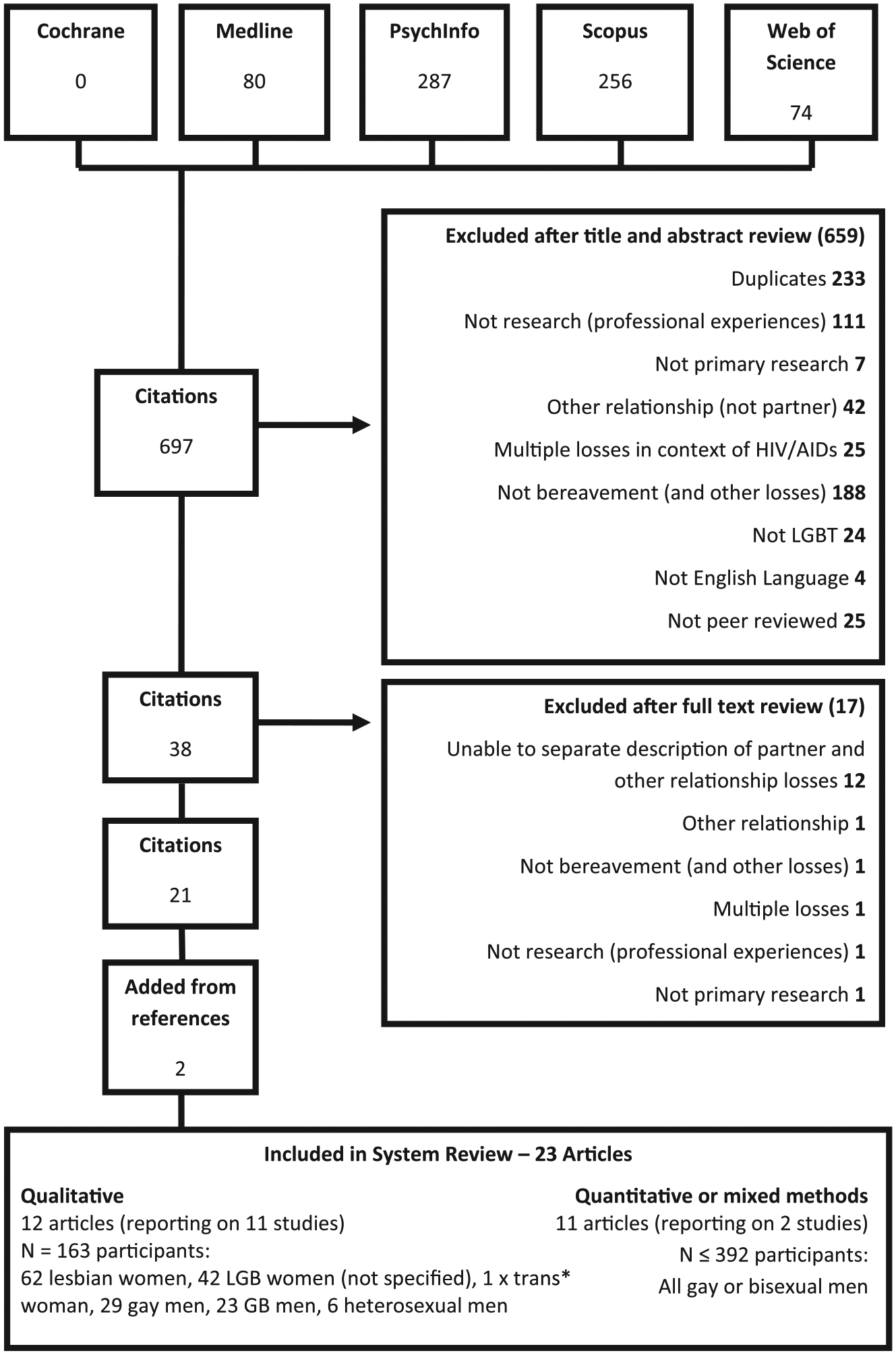
PRISMA flow diagram of study selection and exclusion.
Study descriptions
A total of 23 articles were included in the review:34–56 12 qualitative, 10 quantitative and 1 mixed methods. The articles report on 13 studies (see Table 1) and the experiences of 555 individuals (as 10 articles are from the same study, the University of California San Francisco (UCSF) coping project,46,48–56 the participants are not discrete samples and derive from the same data set. Therefore, the total participants in the quantitative studies (Figure 1) are taken from the first article from the UCSF coping project which reported the total number at study entry 46 (n = 314), and the figure reported in the Multicenter AIDS Cohort Study (MACS; n = 78). 47 Similarly, the participants described in the two Irish qualitative articles38,40 represent the same sample, so they are counted only once in the total participants for qualitative studies (n = 163)).
Articles included in the systematic review and thematic synthesis.

LGB: lesbian, gay or bisexual; UCSF: University of California San Francisco.
Of the qualitative studies, six were from the United States, two from Canada, one from Ireland and two from the United Kingdom. Both quantitative studies were from the United States. Overall, the qualitative studies were more recent – all except two articles were published in the last decade (since 2006), while the majority of the quantitative articles were published in the mid-late 1990s (Table 1). No quantitative studies were identified reporting bereavement experiences of LGBT partners outside of the context of HIV or AIDS.
The qualitative studies utilised varied methods of data collection: eight used interviews, two used surveys or questionnaires and one used focus groups. Methods of analysis included grounded theory or constant comparative approaches; phenomenology; narrative analysis, thematic or content analysis; and approaches described as ‘qualitative’, ‘descriptive’ and ‘exploratory’. The two quantitative studies were part of larger longitudinal prospective observational studies, utilising measures to assess mood, behaviours, psychosocial resources and coping, including the Centers for Epidemiology Scale–Depression (CES-D); 57 the Profile of Mood States (POMS) questionnaire; 58 the 12-item Life Orientation Test; 59 the Ways of Coping Scale; 60 the Dyadic Adjustment Scale; 61 the Social Support Questionnaire; 62 the Positive State of Mind Scale; 63 Bradburn’s Affect Balance Scale; 64 the Structured Clinical Interview for Diagnostic and Statistical Manual of Mental Disorders (3rd ed., rev.; DSM-III-R; SCID); 65 the Daily Hassles Scale; 66 and the Impact of Event Scale. 67
Methods were poorly described in some studies. For qualitative articles, details regarding the personal characteristics of the researcher, relationship with the participants prior to the study, number of coders, data saturation, description of coding tree and participant checking were rarely described (see Online Supplementary Table 1).
For the quantitative articles, the design was rarely described in the title or abstract, and details regarding the sample size calculations, management of missing data and loss to follow-up were often absent (see Online Supplementary Table 2).
Comprehensiveness of study reporting
The comprehensiveness of reporting was variable across the studies (Online Supplementary Tables 1 and 2). All articles reported the number of participants and key demographics (e.g. age, ethnicity and education). However, sexuality was often poorly defined with many studies favouring grouped identifies (‘gay or bisexual men’, ‘LGB people’ and ‘same-sex partners’). The experiences of bisexual people were absorbed within the broader grouped identities, with no exploration of their experiences independently. The experiences of trans* people were poorly represented with just one study including a trans* participant, and no exploration in the article of how her trans* identity shaped her experiences.
Quality of included studies
An assessment of rigour was undertaken for each study according to the Hawker et al. 32 checklist. The main areas where articles were found to be of lower quality included the criteria of consideration of ethics, bias and sampling (particularly for older quantitative articles from the 1990s) and demonstration of transferability or generalisability (qualitative articles). Also, a number of articles failed to include a clear descriptive title or adequate abstract (see Online Supplementary Table 3).
Synthesis
Findings from the 23 articles could be separated into two broad emergent themes: universal or generic bereavement experiences at the loss of a partner and LGBT-specific bereavement experiences (see Figure 2 for themes and sub-themes and Table 2 for illustrative quotes).
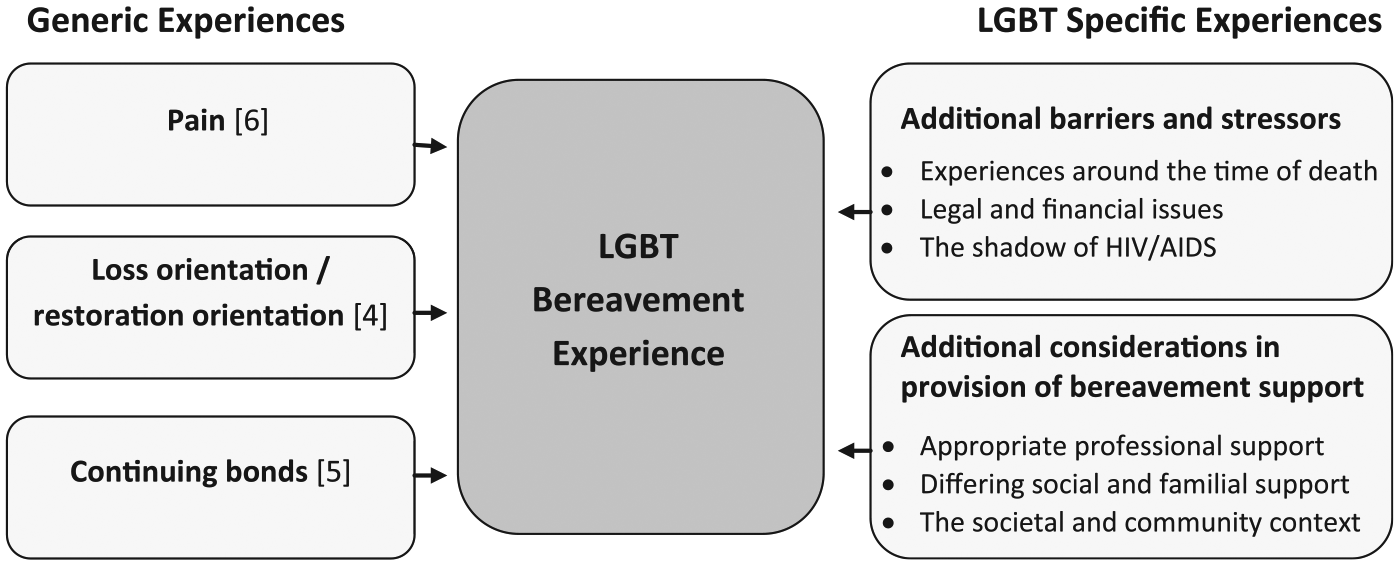
Generic and LGBT-specific bereavement experiences.
Example quotes from thematic synthesis of the literature.

Generic bereavement experiences
The loss of the primary relationship is, to some extent, a universal experience, regardless of sexual identity or gender history. The death of the person who you are closest to, and have shared your life and future plans with, is associated with generic experiences of pain, loss, restoration of individual identity and continuing bonds with the deceased, as recognised in previous literature.4–6 Participants in the included studies described an overwhelming sense of loss and grief, after the loss of their partner, and the totality and physicality of the pain (quote 1). They also described loss of purpose and a need to distract themselves with necessary death related tasks. However, they also depicted the struggle to rebuild their identity alone (quote 2) and find a place for the relationship with the deceased as they continue their life alone.
LGBT-specific experiences
Other experiences of bereavement described within the 13 studies were specific to LGBT communities, including additional barriers and stressors or social mediators and concurrent stressors, 6 regarding care during and around the time of death, legal and financial issues and the ‘shadow’ of HIV or AIDS. However, they also described experiences which reflect the potential additional considerations when supporting bereaved LGBT people: professional support, social and familial support and societal and community support.
Additional barriers and stressors in bereavement
Experiences around the time of death
Experiences of bereavement for LGBT partners were often shaped by interactions with healthcare professionals prior to, and at the time of, death. Some participants described feeling well supported, with healthcare professionals recognising the depth of their relationship and their need to be supported together, as a couple (quote 3). Specifically, recognition of the partner’s needs, and asking about their well-being, as well as the patient’s, was a source of great support for individuals.
However, other participants described additional stressors around the time of death. Homophobia was a concern for some couples, whether experienced through rudeness and hostility or expected and feared. Other participants described being excluded from discussions and decision-making and a lack of acknowledgement of their relationship (quote 4). These experiences of exclusion also extended for some to the time of death, being unable to be with their partner when they died or with the body after death. This had a profound effect on individuals at the time and into bereavement, as they felt denied the opportunity to say goodbye (quote 5).
Additional legal and financial issues
Additional barriers described by bereaved LGBT participants included legal and financial issues. While these differ greatly across the countries of origin of the participants and have changed over time to move towards more parity with heterosexual couples in recent years, there remains an additional layer of complexity to the financial entitlements of same-sex couples compared to their heterosexual peers. Moreover, among the LGBT communities, estrangements or strained relationships with biological family are more common, which in turn presents additional possibilities of contesting of wills and assets around the time of death (quote 6). Such legal and financial battles with families heightened the bereavement experience of the participants, creating an additional layer of stress and discomfort.
Shadow of HIV or AIDS
HIV or AIDS remains a ‘shadow’ over the bereavement experiences of gay and bisexual men and is prominent within the literature from the 1990s. The two quantitative studies identified additional challenges or risk factors for men who had lost their partner to HIV or AIDS, often related to social isolation and stresses in bereavement. High levels of depression were identified among bereaved partners, with mean depression score above the cut-off for ‘at risk of major depressive disorder’ from 3 months before bereavement to 7 months after the loss. Also, HIV+ status, longer relationships, pre-bereavement distancing and experiencing bereavement hassles were predictors for unrelieved depressive mood. 46 Those experiencing initially high levels of depression, and those with high levels of hopelessness and daily stress, were also more likely to have depressive symptoms up to a year post bereavement. 55 Positive states of mind, optimism and low levels of cognitive escape avoidance at 1 month post bereavement were associated with greater likelihood of recovery. 49 At 3 years post bereavement, mean levels of depressive mood remained elevated compared to the general population.
Those having lost a partner to HIV or AIDS also reported increased sexual risk taking in the first year after bereavement, 48 and higher levels of suicidal ideation, particularly among those who felt burdened by caregiving, and described low levels of support or social integration. 54 High levels of spirituality were reported among the participants, 53 maintained 3–4 years after bereavement, 52 and there was no difference in psychological and social resources between HIV− and HIV+ bereaved partners.50,51 Critically, for gay and bisexual men living with HIV or AIDS themselves who had lost a partner to HIV or AIDS, immune changes relevant to HIV progression were evident less than 1 year after the bereavement, which were not explained by risk behaviours (alcohol, smoking and drug use) or antiretroviral medication, 47 suggesting a physical, as well as psychological impact, of losing a partner to HIV or AIDS.
In the qualitative data, gay and bisexual men described the stigma associated with losing a partner to HIV or AIDS. However, for those whose partners died of other causes, participants described assumptions that the deceased had died of HIV or AIDS and the need to explain the death in more detail than they would have chosen to at that time, to avoid such assumptions (quote 7). These assumptions were also extended to the bereaved partner and impacted upon the support they received. When a partner was lost to HIV or AIDS, some individuals described disenfranchisement, 7 being forced to conceal the nature of the loss and of the relationship, for fear of the impact on their support network and job (quote 8).
Additional considerations in provision of bereavement support
Appropriate professional support
Participants also described their experiences of accessing professional support, particularly bereavement support groups, after their partner had died. For some, this was a positive experience, feeling well supported and that their loss was recognised and acknowledged. However, for others, the fear of lack of acceptance, or homophobia from other members of the group, created a barrier, preventing them attending (quote 9). Indeed, some participants who did attend were treated with hostility or lack of understanding from other group members (quote 10). For others, the discrimination was more subtle, with hetero-normative discussions and little or no consideration of other relationship configurations (quote 11).
Differing social and familial support
The fragility of biological family relations for LGBT people was described frequently in the studies, with many participants experiencing a degree of estrangement. For some, who were not ‘out’ with their own families, the lack of support, due to not being able to share the loss, was an additional barrier. Others described fear of sharing too much with family, with whom they were ‘out’, at the risk of pushing them away (quote 12). Participants also described relationships with the deceased partner’s biological family. Some were able to maintain a close relationship, which was a source of support, comfort and reassurance for the future (quote 13). However, others experienced challenges including guilt imposed on them due to their relationship, or complete withdrawal of the partner’s family, with whom they had been close for many years (quote 14). The importance of ‘chosen family’ was well recognised within the interviews. Participants described the essential support they received from the LGBT community and the closeness they felt for their chosen family (quote 15). However, others described challenges of reengaging with the LGBT community after bereavement (quote 16).
Societal and community context
Experiences of bereavement were also influenced by interactions with society and community more broadly, shaped by the degree to which the participant’s relationship was accepted by society and individuals, and if it was disclosed openly. The interaction between acceptance and disclosure, and their influence on the bereavement experience of LGBT people, has been delineated in Figure 3 – the ‘acceptance–disclosure model’ of LGBT partner bereavement experiences – a new model informed by the findings of this synthesis and the previous literature. Individuals can be plotted onto this model, to inform clinical considerations in line with their needs.
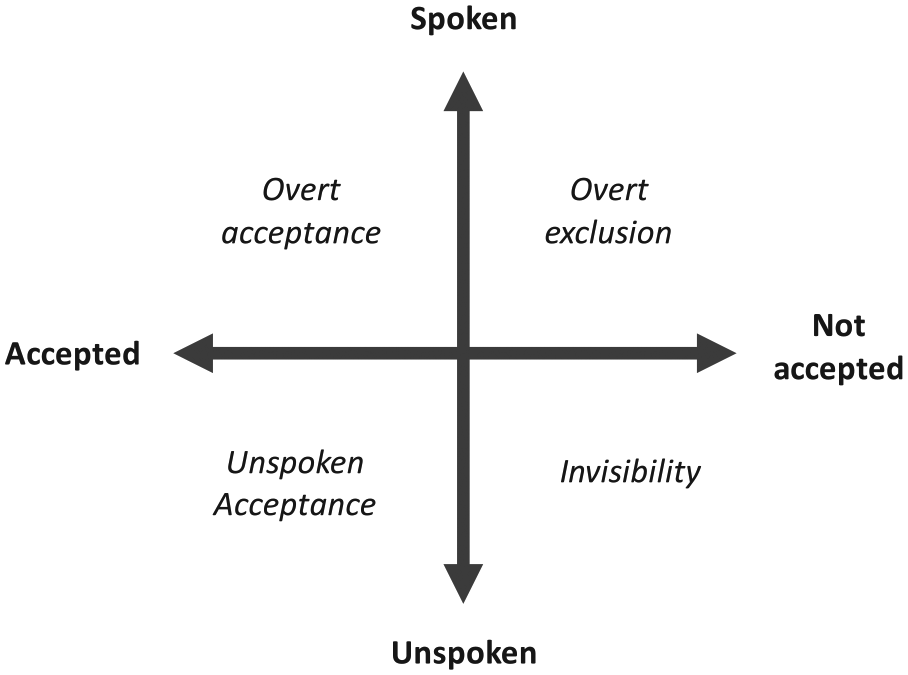
Acceptance–disclosure model of LGBT bereavement experiences.
Model: the ‘acceptance–disclosure model’ of LGBT partner bereavement experiences
Those who are ‘out’ within their community and have their relationship acknowledged and accepted within society would be identified in the top left of this model, in the position of overt acceptance. In contrast, those whose relationship is accepted but not openly disclosed would be identified in the bottom left, in the position of unspoken acceptance, a condition also described previously as tacit acknowledgement. 38 Individuals who are ‘out’ within their community but have experienced estrangement or lack of acceptance of their relationship would occupy the position of overt exclusion in the top right of this model. Finally, those for whom their relationship is neither disclosed nor acknowledged or accepted would be identified in the bottom right in the position of invisibility.
All those occupying positions outside of overt acceptance could be at risk of disenfranchisement, 7 where the relationship with the deceased is either stigmatised or unrecognised, or adverse grief outcomes. Each area of the model is described in more detail below, with examples from the data from the included studies, and discussion of the implications for bereavement and support.
Overt acceptance (accepted+, spoken+)
Some participants experienced acceptance and acknowledgement from the community, and institutions, recognising their loss and treating them with respect (quote 17) enacted through talking openly and supportively about their relationship.
Implications for bereavement and support
Individuals in this position within the model are more likely to be well supported in their relationship and into bereavement, and therefore, additional supportive needs may be minimal. However, in bereavement, individuals may experience a shift from overt acceptance to a less favourable position (quote 10), due to negative experiences. Importantly, as with other positions in the model, participants will experience varying degrees of acceptance and acknowledgement enacted through individual interactions, and their proximity to other areas of the model will shift with each experience.
Unspoken acceptance (accepted+, spoken−)
In contrast, some participants described receiving support in bereavement, despite their relationship not being openly disclosed, a condition previously described as tacit acknowledgement 38 (quote 18). Although preferred by some participants, the risk of this unspoken acceptance includes lack of recognition of the loss, failure to assess bereavement needs and a risk of tacit exclusion 38 (quote 19). This indirect neglect of the relationship is further compounded by society’s inadequate lexicon to describe the loss of a civil partner or same-sex married partner (quote 20).
Implications for bereavement and support
Individuals occupying the position of unspoken acceptance may need additional consideration in bereavement. The lack of communication about their relationship may impact upon their access to support services, as they may be overlooked by healthcare professionals who fail to recognise that they have lost their primary relationship.
Overt exclusion (accepted−, spoken+)
Other participants described overt exclusion from their community and disenfranchisement. 7 While the relationship was acknowledged, it was not accepted or supported (quote 21). The lack of opportunity to take comfort in sharing their bereavement experience, with friends and family, further compounded their grief.
Implications for bereavement and support
Those occupying the position of overt exclusion may be at increased risk of adverse bereavement outcomes due to the additional barriers and stressors they experience and, therefore, may need additional support. In addition, for some individuals, due to historical factors, such as having lived through a period when homosexuality was illegal, there may be an expectation of homophobia or assumption of overt exclusion, even if this is not actualised in interactions with healthcare professionals.
Invisibility (accepted−, spoken−)
Finally, some participants described invisibility in their bereavement, within society and the community, resulting in disenfranchisement, 7 and an inability to access support (quote 22). This also excluded them from the vital experience of celebrating and commemorating their relationship at funeral and memorial services – an important part of grieving (quote 23).
Implications for bereavement and support
Those identifying within the position of invisibility will rely on sensitivity from the clinical team to recognise the depth and nature of the relationship in order to access the support they need. Their disenfranchised status increases their risk of adverse bereavement outcomes, and careful consideration of potential additional sources of support will be needed, in line with their preferences for disclosure. For some individuals, however, the isolation of grief within an invisible relationship may be overwhelming, and they may be forced to ‘come out’ in bereavement, in order to access support (quote 24), perhaps resulting in a move into overt exclusion (quote 25). These individuals are particularly vulnerable, and such experiences are associated with increased stress at a critical time and potential additional or increased supportive care needs.
In practice, the ‘acceptance–disclosure model’ can be used by clinical teams as a tool to plot and consider an individual’s, or couple’s, position in relation to acceptance and disclosure. This in turn may prompt consideration of the potential additional barriers and stressors that LGBT individuals may face in bereavement, to enable proactive assessment of needs, identification of sources of support, planning and interventions, to mitigate against complicated grief and adverse grief outcomes.
Discussion
This systematic review aimed to identify and appraise the evidence of the bereavement experiences of LGBT people who have lost a partner and to develop a new explanatory model to improve care for bereaved LGBT individuals. Loss of the primary relationship is a universal experience, regardless of sexual or gender identity. Participants described the previously recognised pain of loss, 6 processes of loss and restoration orientation, 4 as well as continuing bonds 5 with the deceased as they learned to find a new place for the relationship in bereavement. However, participants also described social mediators and concurrent stressors 6 specific to the LGBT communities. These shaped the bereavement experience and highlighted potential additional considerations for healthcare professionals providing that support.
Disenfranchisement has previously been described 7 where the relationship with the deceased is either socially stigmatised or not recognised and accepted. Moreover, the relevance of whether a relationship is openly disclosed, and how this may shape bereavement experiences, 38 has also been described. However, evidence from this synthesis, and the model devised, suggests an important interaction between acceptance and disclosure – from a position of complete invisibility to overt acceptance. The position an individual occupies in the model shapes not only the bereaved individuals access to support but also their access to the role of ‘widow’ and the social capital, norms, expectations and entitlements that role encapsulates. Importantly, it is also recognised that an individual’s position within the model is not static and may shift during bereavement due to the additional barriers and stressors and interactions they experience. Critically, an individual’s previous negative experiences, or historical factors, such as having lived through a period when homosexuality was illegal, may increase fears and expectations of homophobia and force them to assume a position of exclusion, unless professionals overtly, and adequately, demonstrate acknowledgement and acceptance.
As with any minority population, there is a need for sensitivity and consideration of the political, social and historical context for the LGBT communities when providing care after death. Although the recent raft of legislative changes have resulted in improvements for lesbian, gay, bisexual and trans* people, it is important to be mindful that many older individuals in same-sex relationships will have lived through a time when such a relationship was highly stigmatised or indeed illegal. 68 Moreover, legislative changes largely occur in advance of changes in attitudes.
The recognition that the needs of the LGBT communities may differ from those of the general population was undoubtedly hastened by the advent of HIV or AIDS and a recognition that an individual’s sexuality may shape their particular health needs. 15 However, the ‘shadow’ of HIV or AIDS in the LGBT bereavement literature is disproportionately large. Quantitative research into the bereavement outcomes of people who identify as LGBT and have lost a partner is entirely dominated by studies in the context of the HIV or AIDS pandemic or studies which focus on those who have experienced multiple losses in the context of HIV or AIDS. Indeed, a recent review of studies funded by the National Institute for Health found that after excluding studies focusing on HIV or AIDS and sexual health matters, just 0.1% of studies concerned LGBT health, 69 despite conservative estimates that LGBT individuals represent 3.4%–7% of the population.70,19 Similarly, a review in 2002 found that just 0.1% of articles published in the preceding 20 years addressed the public health needs of LGBT people, 71 suggesting that the needs of LGBT people continue to be under-researched. In 2010, the US Department of Health and Human Services quoted LGBT health equity as one of its 10-year goals for 2020; however, it is also important to ensure that funding for research within the LGBT communities is more equally distributed, with the vast majority (86%) currently allocated to research into gay and bisexual men’s health. 69
Limitations
It was not possible to include articles not published in English; therefore, studies reporting the experience of LGBT bereavement in other languages may have been omitted. However, through piloting the search terms, and taking guidance from information specialists, we were able to reduce other limitations of the search strategy, increasing the comprehensiveness of this review. The decision to include only peer-reviewed articles may mean we omitted some valuable research which had not yet made it to publication. However, it is important in systematic reviews to focus on findings that have been peer reviewed.
Additionally, although the studies were assessed for quality and reporting, they were not weighted or excluded based on these assessments. However, given the predominance of qualitative research within the review, the divergent study designs and methodologies and the contentious nature of quality assessment in qualitative research,72,73 this was considered the most appropriate decision.
The review, and subsequent modelling, was also limited by the paucity of research with the trans* and bisexual communities and poor reporting of sexual identity, both of which need to be addressed in future studies. Finally, the study was also limited by the selection bias of research within hard to reach communities, as it only reports the experiences of those who openly disclose their LGBT identity.
Future research
A notable finding from this review is the scarcity of literature exploring the experiences of bereaved bisexual and trans* people. Sexuality was also often poorly described, with individuals described as ‘LGB people’ or ‘same-sex partners’, and the experience of the trans* participants were not described separately in relation to their gender identity. It is essential that reporting of sexual and gender identity in research is congruent with individuals’ self-identity and expression. In addition, researchers need to be cautious when using LGBT as a descriptor for participants, which can be misleading particularly when bisexual and trans* people are underrepresented within the sample.
Challenges remain in accessing communities and recruiting within minority groups. There is a need for more thorough documentation of successful and unsuccessful recruitment processes to inform future study designs. In addition, the majority of included studies were from the United States and urban settings, where experiences would undoubtedly differ from more rural settings.
In addition, methods and methodology were often poorly described. A particularly notable absence from the literature is research into psychological and other outcomes for LGBT people who have been bereaved, outside of the context of HIV or AIDS. Given the additional barriers and stressors outlined in this review, and discrimination and negative experiences described by LGBT people in healthcare more generally,25–27 there is a need for more focused quantitative research in this area, particularly using patient reported outcome measures of grief and depression, comparing outcomes with the general population.
Conclusion
Loss of a partner is associated with universal experiences, regardless of sexual identity or gender history. However, people who identify as LGBT face additional barriers and stressors when grieving the loss of a partner, may have additional or different care needs from their heterosexual or cisgender peers and may be at risk of heightened or prolonged bereavement. There is a need for careful exploration of the relationship and the bereaved individual’s identity, including the degree to which the relationship was disclosed and acknowledged in life. By integrating careful questioning about who is important to an individual into routine practice, avoiding assumptions of heterosexuality, and not being afraid to ask sensitively about identity, clinicians can be enabled to deliver holistic individually centred care. This may include thinking about alternative sources of support from chosen family, or the LGBT community more broadly, and moving away from biologically focused models of understanding ‘family’. It is also vital to be mindful of the cultural and historical factors which may make individuals less inclined to share their identity, or proactively seek out the care and support they need, and the increased potential for isolation among the LGBT communities. Finally, fostering an environment of acceptance, recognition and support, working closely with community groups and seeking out training and education where necessary are key to delivering high-quality individualised care to bereaved LGBT people.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This work was supported by the Marie Curie Research Grants Scheme, grant [MCCC-RP-14-A17159].
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
