Abstract
Objective
To document the impact of stroke on employment income among people employed at the time of stroke.
Design
Population-based cohort study.
Participants
People hospitalized for stroke in Ontario, Canada (2010–2014) and people without stroke matched on demographic characteristics.
Main measures
Robust Poisson regression to estimate the effects of stroke on the probability of reporting employment income on tax returns over 3 years. Quantile regression difference-in-differences to estimate the changes in annual employment income attributable to stroke.
Results
Stroke survivors were increasingly less likely to report any employment income poststroke, incidence rate ratios (IRR) 0.87 at 1 year (95% confidence intervals [CI]; 0.85–0.88), 0.82 at 2 years (95% CI; 0.81–0.84) and 0.81 at 3 years (95% CI; 0.79–0.82). IRR for reporting at least 50% of prestroke income levels were 0.76 at 1 year (95% CI; 0.75–0.78), 0.75 at 2 years (95% CI; 0.73–0.77) and 0.73 at 3 years (95% CI; 0.71–0.75). IRR for reporting at least 90% of prestroke income levels were 0.72 at 1 year (95% CI; 0.70–0.74), 0.66 at 2 years (95% CI; 0.64–0.68) and again 0.66 at 3 years (95% CI; 0.64–0.68). Relative changes in annual employment income attributable to stroke varied from a decrease of 13.8% (95% CI; 8.7–18.9) at the 75th income percentile to a decrease of 43.1% (95% CI; 18.7–67.6) at the 25th income percentile.
Conclusions
It is important for healthcare and service providers to recognize the impact of stroke on return to prestroke levels of employment income. Low-income stroke survivors experience a more drastic loss in employment income and may need additional social support.
Introduction
Being employed is important for financial reasons and for psychosocial wellbeing.1,2 Chronic impairments after stroke, such as cognitive and physical limitations, can result in difficulty returning to employment.3–5 Following stroke, people may be working at reduced capacities or retire earlier than planned. This can lead to loss of income and financial stress, which adversely affects quality of life.6,7
The percentage of stroke survivors returning to employment is not precisely known. Estimates widely vary but are likely close to 55.7% at 1 year and 67.4% at 2 years poststroke. 8 Estimates vary depending on the operational definitions of employment and length of follow-up poststroke.3,8,9 Return to employment can be influenced by characteristics such as age, gender, area of residence, marital status and having children. Stroke survivors of younger age and men are more likely to return to employment.3,9–12 As well, stroke survivors who are living in more populated areas, are single or have children, are more likely to return to employment.3,9,10,12 Adjusted population-level estimates of the percentage of stroke survivors returning to employment would be useful to better understand current rates and trends in return to employment.
Furthermore, there has been little information on the impact of stroke on employment income over time. We aimed to document this impact by comparing stroke survivors who were employed at the time of stroke with people of similar characteristics who did not have a stroke. We adjusted for characteristics that influence employment, particularly age, since stroke survivors are mostly older people who are likely to be working less over time approaching retirement. 13
Our first objective was to estimate the relative effects of stroke on the probability of reporting employment income over 3 years poststroke. Our second objective was to estimate the changes in annual employment income attributable to stroke.
Methods
We conducted a province-wide retrospective cohort study using hospital and tax data in Ontario, the most populous province in Canada. We used patient record-level data from all hospitals (approximately 167 across Ontario as of 2014) from the Canadian Institute for Health Information Discharge Abstract Database. 14 The hospital data were linked by Statistics Canada to personal income tax returns of the annual T1 Family File collected by the Canada Revenue Agency (Supplemental Table S1). 15
Our sample was people hospitalized for stroke between 2010 and 2014 in Ontario. We included all stroke survivors who filed income tax returns for 3 years poststroke, and reported any employment income during the year prestroke, that is, stroke survivors who were employed prior to their stroke (Supplemental Figure S1). For each unique individual, the index date is the year the stroke occurred. Pre-index refers to the time period prestroke, and post-index refers to the time period poststroke. We set 2014 as the limit to allow for 3 years of post-index follow-up until 2017, the latest year with available data.
We defined stroke as a brain infarct or a cerebrovascular accident lasting more than 24 hours (Canadian Coding Standards for the International Statistical Classification of Diseases, Tenth Revision). 16 We included the diagnostic codes subarachnoid hemorrhage (I60.X), intracerebral hemorrhage (I61.X), ischemic stroke or cerebral infarction (I63.X) and unspecified stroke (I64). These diagnostic codes have been reported to have high positive predictive value.17,18 We excluded transient ischemic attack (G45.X), defined as a similar neurological deficit lasting less than 24 hours. 16
To compare with stroke survivors, we selected people who did not have a stroke from among all people in Ontario who had filed income tax returns during the same index date 2010–2014, had reported employment income during the year pre-index, and did not have any record of hospitalization during the 3 years pre-index and post-index. We used coarsened exact matching19,20 to select a 10:1 ratio match with stroke survivors on the following characteristics: index date, age, sex, area of residence (urban area with population 15,000+ or rural area with population <15,000), marital status (married or common law, single, separated, divorced, widowed), at least one child under the age of 18 (yes or no), low-income household (yes or no), employment income pre-index and total income pre-index. We defined low-income household according to the Statistics Canada definition of earning less than the low-income measure thresholds. 21 The low-income measure thresholds depend on the year and the household size. For example, in 2017, a one-person household would be considered low-income if the person earned less than $25,397 Canadian dollars (CADs) (£15,200 British pound sterling).22,23
Outcomes and analysis
Our main outcome was employment income, defined according to the Statistics Canada definition, “wages and salaries, commissions from employment, training allowances, tips and gratuities and self-employment income (net income from business, profession, farming, fishing and commissions), Indian exempt employment income, and Indian exempt self-employment income.” 24 We inflated employment income to 2017 Canadian dollars with the Canadian Consumer price, 25 where 1 Canadian dollar = 0.60 British pound sterling (October 2023). 26
For our first objective, we estimated the percentage of people reporting employment income at 3 levels: (a) any employment income, (b) at least 50% of their pre-index employment income and (c) at least 90% of their pre-index employment income. We used robust Poisson regression to estimate the relative effects of stroke on the probability of reporting employment income for each of those levels. We presented the incidence rate ratios (IRR) comparing stroke survivors and the people who did not have a stroke at 1, 2 and 3 years post-index. In addition, we performed stratified analyses by the following subgroups: low-income household (low-income stroke survivors vs. low-income people who did not have a stroke), stroke type (ischemic vs. hemorrhagic vs. unspecified stroke), Charlson Comorbidity Index (0 vs. 1–2 vs. 3+) and total hospital length of stay (LOS; short ≤4 days vs. medium 5–9 days vs. long ≥10 days). 14
For our second objective, we used quantile regression with difference-in-differences to estimate the changes in annual employment income attributable to stroke. This involved calculating the differences in pre-index and post-index annual employment income between stroke survivors and the people who did not have a stroke (example illustrated in Figure 1). To compare changes between lower and higher earners, we performed these analyses in 5 percentile increments from the 25th to the 75th pre-index employment income percentiles. We estimated the absolute changes and the relative changes in annual employment income (3-year average).
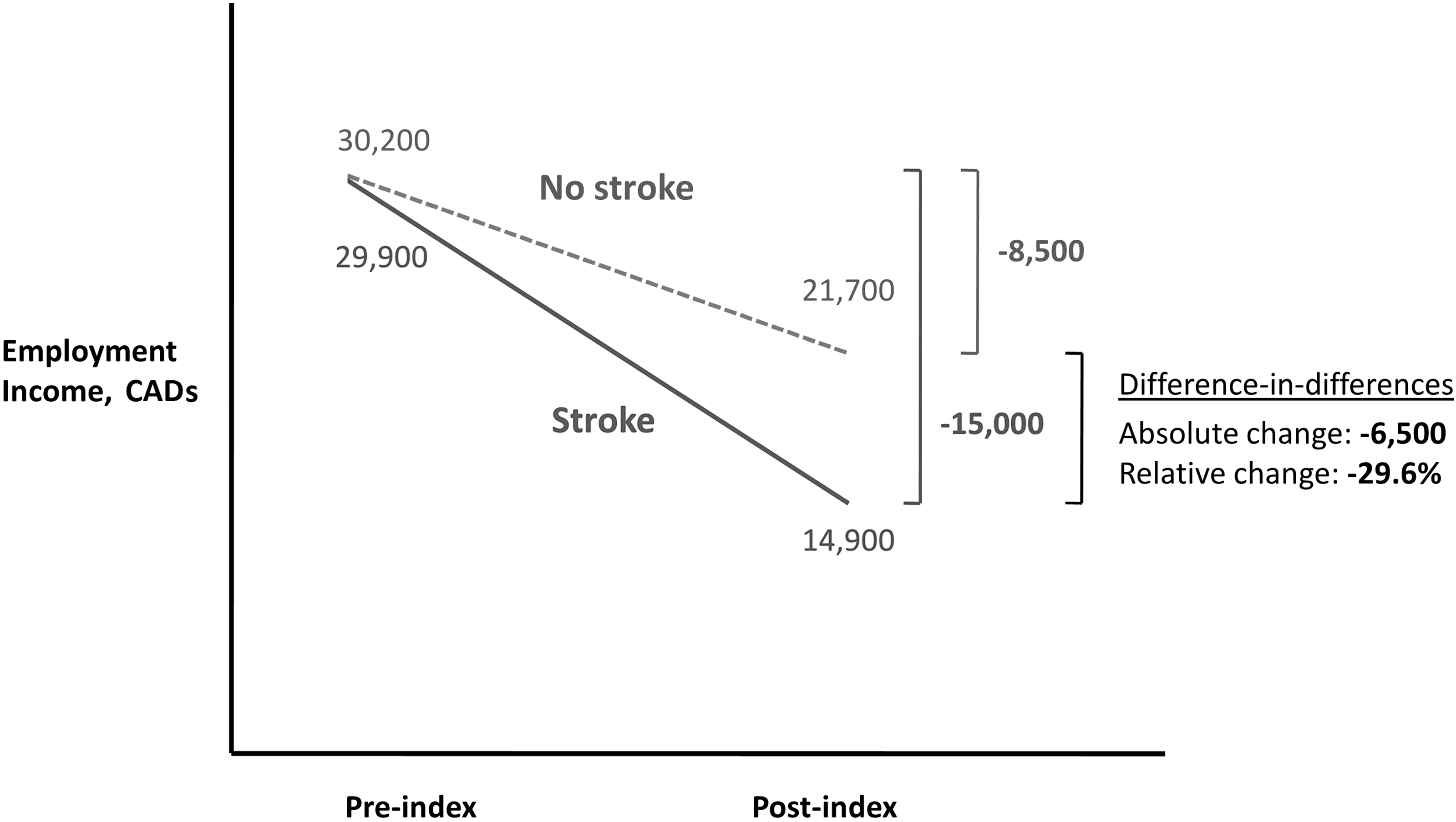
Differences-in-differences change in annual employment income (3-year average) at the 50th (median) pre-index employment income percentile. CADs, Canadian dollars.
We adjusted our estimates by including the following variables in our regressions: index date, age, gender, area of residence, marital status, at least one child under the age of 18, low-income household. We reported estimates with 95% confidence intervals (CI) and statistical tests with
Results
The cohort comprised 12,720 stroke survivors and 125,315 people of similar characteristics who did not have a stroke (Table 1).
Characteristics of the cohort.
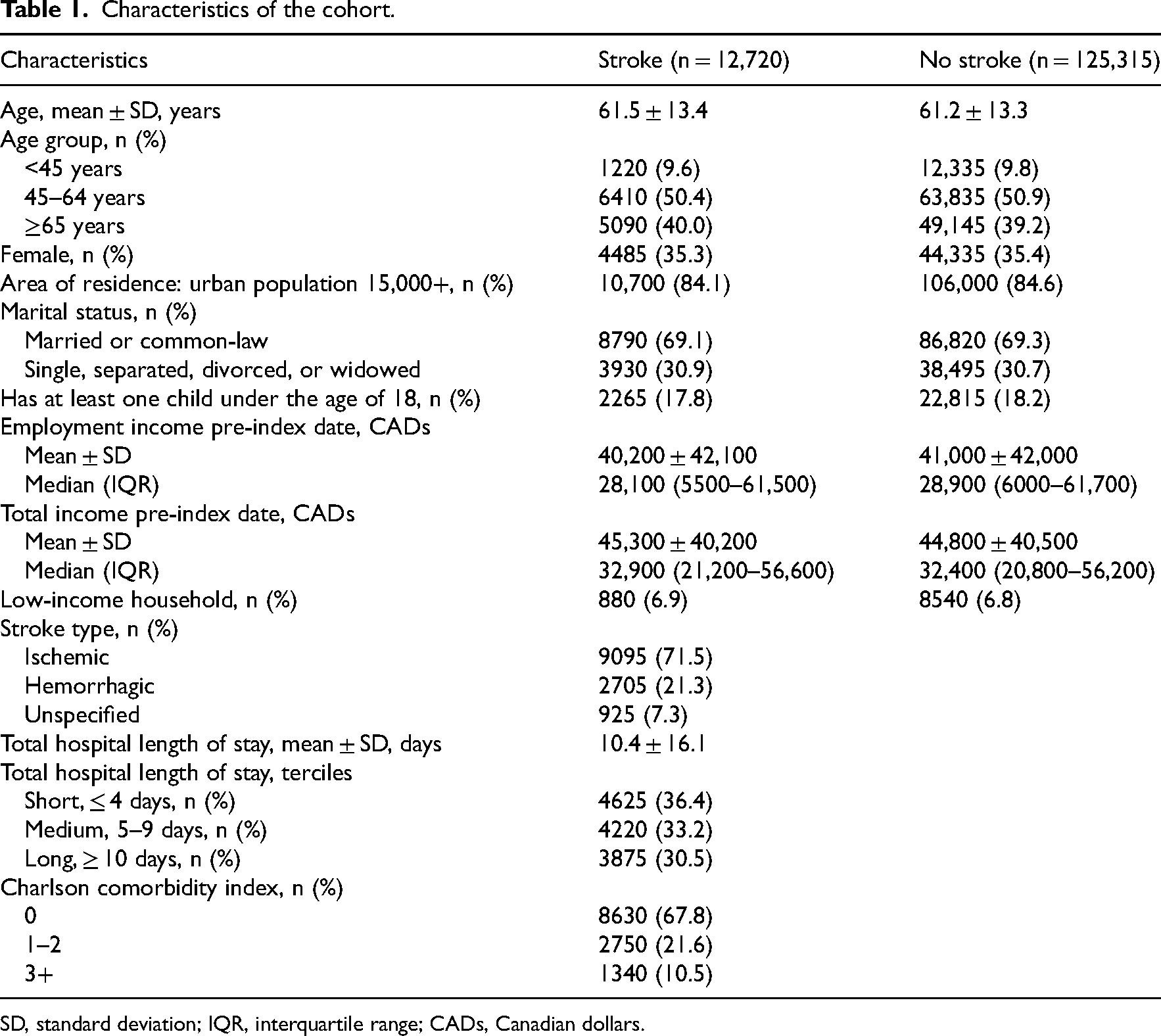
SD, standard deviation; IQR, interquartile range; CADs, Canadian dollars.
Relative effects of stroke on the probability of reporting employment income
The percentage of people reporting employment income decreased over time. The decrease was greater among stroke survivors (Table 2). Stroke survivors had a significantly lower probability of reporting any employment income compared to people who did not have a stroke. Stroke survivors also had a significantly lower probability of reporting at least 50% pre-index employment income and at least 90% pre-index employment income.
Percentages of people reporting employment income and incidence ratio ratios (IRR) comparing stroke survivors and people who did not have a stroke a .
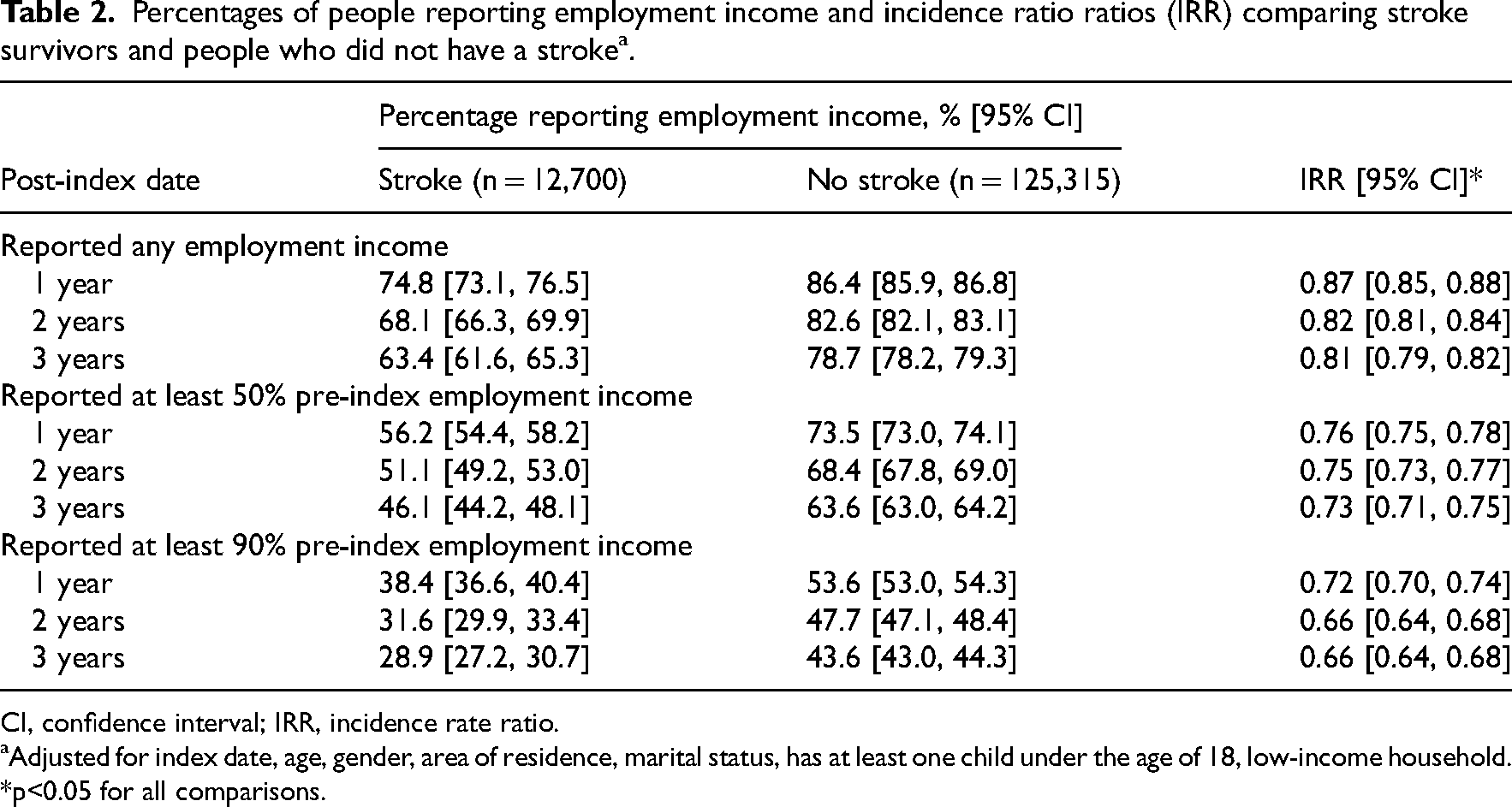
CI, confidence interval; IRR, incidence rate ratio.
Adjusted for index date, age, gender, area of residence, marital status, has at least one child under the age of 18, low-income household.
p<0.05 for all comparisons.
Additional results for stratified analyses by low-income household, stroke type, Charlson Comorbidity Index and hospital length of stay are available in the supplemental material (Supplemental Tables S2–S5). Low-income household stroke survivors had significantly lower probabilities of reporting employment income compared to low-income household people who did not have a stroke. The different stroke types (ischemic, hemorrhagic and unspecified stroke) had comparable probabilities. Stroke survivors with Charlson Comorbidity Index of 0 had significantly higher probabilities of reporting employment income compared to stroke survivors with Charlson Comorbidity Index of 3+. Stroke survivors with short hospital length of stay (≤4 days) had significantly higher probabilities of reporting employment income compared to stroke survivors with long hospital length of stay (≥10 days).
Changes in annual employment income attributable to stroke
The pre-index and post-index changes in annual employment income (3-year average) are shown in Table 3. For stroke survivors at the 50th percentile (median), pre-index employment income was $29,900 and post-index employment income was $14,900. The change in annual employment income attributable to stroke was −$6400 (−29.6%). The relative changes were larger at lower employment income percentiles (Supplemental Figure S2). The largest relative change was −52.2% at the 30th percentile and the smallest relative change was −13.8% at the 75th percentile.
Pre-index and post-index changes in annual employment income (3-year average) a .
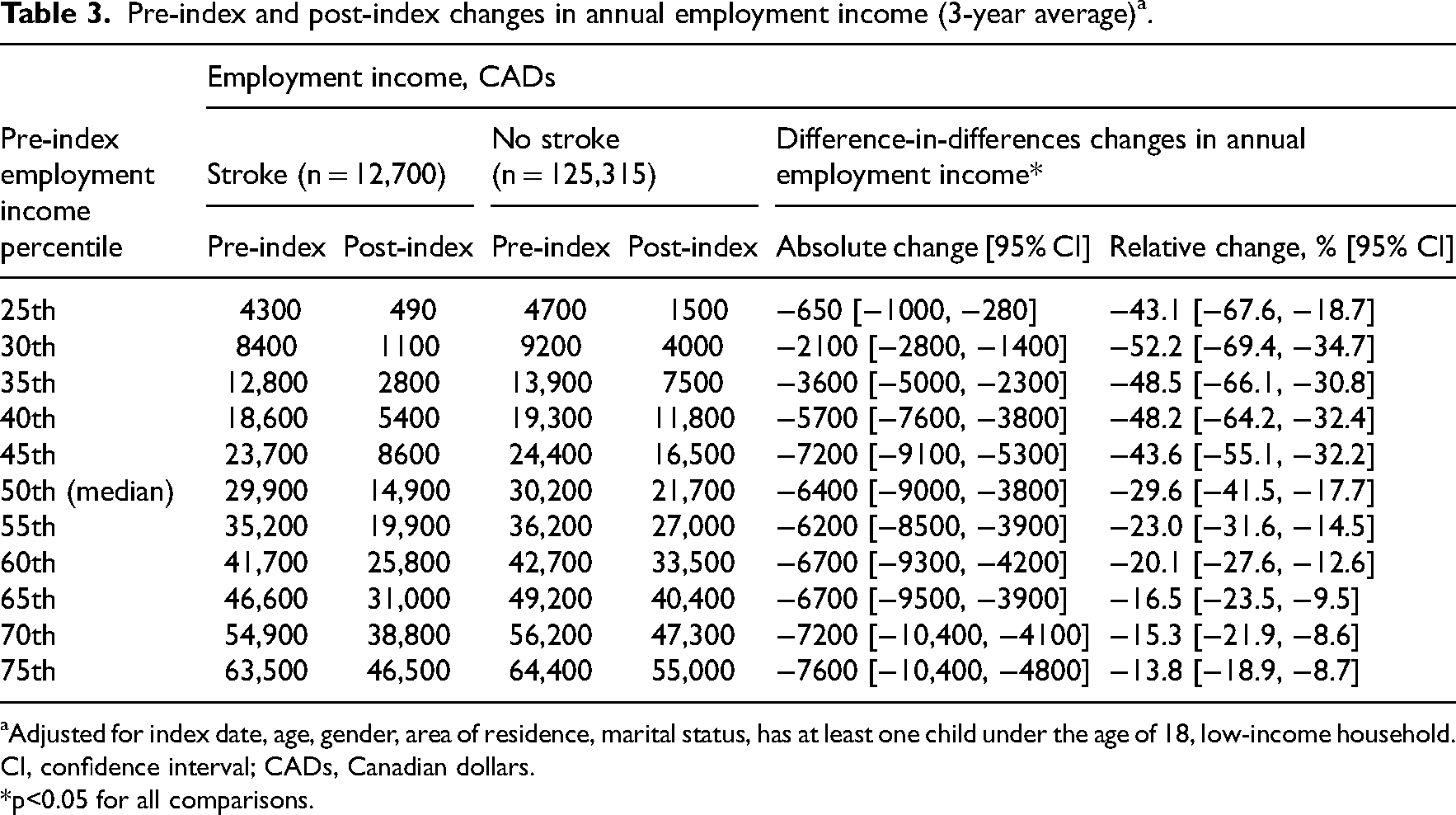
Adjusted for index date, age, gender, area of residence, marital status, has at least one child under the age of 18, low-income household.
CI, confidence interval; CADs, Canadian dollars.
p<0.05 for all comparisons.
Discussion
In this cohort study, we used hospital and tax data to examine the impact of stroke on employment income. To this end, we examined the income that stroke survivors reported on their tax returns during the time periods before and after stroke, and we compared this to the income reported by people of similar characteristics who did not have a stroke during the same time periods.
Our results showed that the percentage of people reporting employment income decreased over time. Among the people who did not have a stroke, this decrease most likely reflects the age-related decline in employment due to transition to retirement. The relative differences, between stroke survivors and people who did not have a stroke, indicate that stroke had negative effects on the probability of reporting employment income, as could be seen with the IRR that decreased each year. These findings suggest that stroke survivors experience increasingly more difficulty maintaining employment and earning prestroke levels of income over time. Offering interventions to assist stroke survivors early could be beneficial, such as modifying work duties and reducing work hours to part-time before gradually increasing to full-time.10,29–31
In our stratified analyses, we found that low-income household stroke survivors were less likely to report employment income than low-income household people who did not have a stroke. Low-income stroke survivors face unique challenges that may be linked to the type of employment at the time of stroke. People who experience stroke are more likely to be self-employed, doing part-time or contract work with no benefits and are more likely to be employed in manual labor with demands that are more difficult to meet after stroke.32–35 We did not find significant differences between ischemic, hemorrhagic and unspecified stroke. The stroke type did not have a large effect after adjusting for other variables. Other studies have reported mixed findings on whether people with ischemic stroke or hemorrhagic stroke are more likely to return to employment.9,36 We found differences when stratified by Charlson Comorbidity Index and total hospital length of stay. Stroke survivors with lower comorbidity and shorter hospital length of stay were more likely to report employment income. Lower comorbidity and shorter hospital length of stay have been associated with better functional outcomes and more favorable return to employment.9,10,36
Regarding changes in annual employment income attributable to stroke, we observed larger relative changes at lower prestroke employment income percentiles. The largest relative change was a decrease of 52.2% at the 30th percentile. This highlights a disparity, that people earning less employment income prestroke further experience a disproportionately greater loss of employment income poststroke. This can result in difficulty meeting basic expenses, such as housing, food, medication and accessible transportation, which in turn can lead to poor health outcomes.32,34,35,37,38
The findings of our study compliment another Canadian cohort study by Garland
Given these findings, further research is needed with special attention to people with low income. It is concerning that these people are less likely to be employed poststroke while also confronted with more substantial relative loss of income. Low-income stroke survivors in particular may be less able to navigate community resources and have greater difficulty accessing employment and income support programs. 32 Future studies should investigate what proportion of low-income versus high-income stroke survivors receive income supports, what amounts they are receiving and what challenges they face with accessing income support and programs designed to help them return to work. While considering regional socioeconomic differences, this research would be an important first step in better understanding whether the social support system is effectively providing assistance to stroke survivors in need and could help shape future policy on improving the provision of those services.
The main strength of our study was the large, population-based sample. This together with the multiple years of data allowed for more precise estimation of the impact of stroke on employment income over time. There were limitations to consider. We strived for a population-based sample of stroke survivors who were employed in Ontario. Our sample included all people hospitalized for stroke but did not include people who were not admitted to the hospital following assessment in the emergency department (approximately 14%). 41 It may be reasonably assumed that these people had mild strokes that would not largely impact their ability to work. Since they were not included in our sample, we may have slightly underestimated poststroke employment and income. As well, our sample did not include people who did not file their income tax returns. However, it may be assumed that these people were not earning employment income. Lastly, we were not able to adjust for other variables that could have potentially influenced employment, such as education, type of occupation, years of employment, functional level and social support,3,9,10,33,36 as these variables were not available in our datasets.
This population-based study showed that stroke has a considerable negative impact on employment income. Stroke survivors were increasingly less likely to report earning prestroke levels of employment income over 3 years. As well, stroke survivors with lower prestroke employment income were seen to have greater relative losses in poststroke employment income. Low-income stroke survivors may be more financially disadvantaged and most in need of assistance.
Clinical messages
Stroke survivors are increasingly less likely over 3 years to report earning prestroke levels of employment income. Providing interventions early to assist with returning and maintaining employment could be beneficial.
Low-income stroke survivors may need additional social support because they experience a greater relative loss in employment income.
Supplemental Material
sj-pdf-1-cre-10.1177_02692155241249345 - Supplemental material for The impact of stroke on employment income: A cohort study using hospital and income tax data in Ontario, Canada
Supplemental material, sj-pdf-1-cre-10.1177_02692155241249345 for The impact of stroke on employment income: A cohort study using hospital and income tax data in Ontario, Canada by Patrick Duong, Mary Egan, Matthew Meyer, Tricia Morrison and Katrine Sauvé-Schenk in Clinical Rehabilitation
Supplemental Material
sj-pdf-2-cre-10.1177_02692155241249345 - Supplemental material for The impact of stroke on employment income: A cohort study using hospital and income tax data in Ontario, Canada
Supplemental material, sj-pdf-2-cre-10.1177_02692155241249345 for The impact of stroke on employment income: A cohort study using hospital and income tax data in Ontario, Canada by Patrick Duong, Mary Egan, Matthew Meyer, Tricia Morrison and Katrine Sauvé-Schenk in Clinical Rehabilitation
Footnotes
Author Contributions
Patrick Duong and Mary Egan designed the study. Patrick Duong collected and analyzed the data and drafted the manuscript with input from all authors. Mary Egan supervised the project. All authors contributed to the interpretation of the findings, revised the manuscript critically for important intellectual content, and approved the final version for publication.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Access to the datasets for this study was approved through the Statistics Canada Microdata Access Portal. The data were accessed at a university-based Research Data Centre. Although the research and analysis are based on data from Statistics Canada, the opinions expressed do not represent the views of Statistics Canada.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by funds to the Canadian Research Data Centre Network from the Social Sciences and Humanities Research Council, the Canadian Institute for Health Research, the Canadian Foundation for Innovation, and Statistics Canada. Patrick Duong was a recipient of the Canadian Research Data Centre Network Emerging Scholars Grant in 2021.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
