Abstract
Objective
To examine the characteristics and the effectiveness of virtual reality systems on upper limb impairments in children and young adults with cerebral palsy.
Data sources
An electronic search was conducted on PubMed, PEDro, Web of Science, Central, and EMBASE.
Methods
The protocol of this review was prospectively registered in the PROSPERO database (CRD42022302271). Randomized controlled trials that tested the effects of virtual reality-based interventions on the upper limb of participants with cerebral palsy were included. The methodological quality of the studies was measured by the PEDro scale. The certainty of the evidence was assessed using the Grading of Recommendations Assessment, Development and Evaluation. The data of the studies were analyzed in meta-analysis and presented in forest plots and narrative synthesis.
Results
Twenty-two studies involving 746 participants were included. Ten different virtual reality systems were used in the interventions, of which six were designed specifically for rehabilitation and four commercial video games. We found an effect in favor of virtual reality when it was used in combination with conventional therapy for upper limb activity (SMD = 0.65; 95% CI (0.19 to 1.11)). However, the certainty of the evidence of the comparisons ranged from very low to low.
Conclusion
Virtual reality seems to be an effective tool for upper limb activity in children and young adults with cerebral palsy. Nevertheless, future studies should present a better methodological quality, a larger sample size, and well-defined rehabilitation programs to reduce the inconsistency of the evidence in this domain.
Introduction
Cerebral palsy is the leading cause of motor disability in childhood.1–3 Upper limb impairments are common in half of all people with cerebral palsy 4 with an impact on their motor and social activities.5,6 Rehabilitation programs are essential for better utilization of the impaired upper limb and, therefore, for improving their independence in the activities of daily living.5,7,8
In recent years, virtual reality has proven to be an interesting therapeutic tool,9,10 and studies examining its effects on upper limb rehabilitation in children and young adults with cerebral palsy have increased considerably.11–14 Indeed, the characteristics of virtual environments favor the integration of important rehabilitation principles 15 in therapeutic interventions such as repetitive, intensive, and variable practice with increasing difficulty and multisensory feedback. 16 These elements can increase the potential for motor learning and neuroplasticity.17–19 Virtual reality technologies differ from each other depending on the technical specifics of the system, and several types are used in therapeutic interventions. For instance, the systems can be designed specifically for rehabilitation 20 or initially for recreational purposes (e.g. commercial video games).21,22 In addition, the interactive interface of the devices can vary from a joystick to more complex systems using cameras or motion capture sensors. 23 The images can also be viewed on screens or through a virtual reality headset. 24 The virtual experience can therefore be classified as non-immersive, semi-immersive, or fully immersive.25,26
Some systematic reviews have summarized the effects of virtual reality on the therapeutic interventions of individuals with cerebral palsy. For instance, Chen et al. 27 in 2018 and Fandim et al. 28 in 2020 performed reviews interested in the effectiveness of these technologies on the upper limb, but also on the lower limb, ambulation, and postural control. However, this broad scope makes it difficult to draw conclusions regarding the upper limb. Rathinam et al. 29 in 2019 were interested in the effects of all types of virtual reality systems but only on hand function, neglecting the other upper limb joints. Another review conducted in 2020 by Johansen et al. 30 was limited only to the effects of commercial video game systems on the upper limb. In addition, these previous reviews did not address specifically the characteristics of virtual reality systems (e.g. degree of immersion, type of interaction interface, variety of games, necessary adaptations) and how these issues can impact intervention outcomes. For these reasons, the objective of this systematic review was to determine the effectiveness of the different types of virtual reality systems used to improve upper limb impairments in children and young adults with cerebral palsy. To this end, we considered virtual reality systems designed specifically for rehabilitation or recreational purposes with all degrees of immersion. Furthermore, this review aimed to summarize the characteristics of these virtual reality systems used in therapeutic interventions.
Methods
This systematic review followed the recommendations of the Cochrane Handbook 31 and was reported according to the directives and recommendations of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 32 and the PRISMA-S. 33 The protocol of this review was prospectively registered in the International Prospective Register of Systematic Reviews -PROSPERO (registration number: CRD42022302271).
The inclusion criteria were formulated using the PICO approach (Population, Interventions, Comparison, Outcomes). The studies were to include participants diagnosed with unilateral or bilateral cerebral palsy, with all levels of severity, and aged 3 to 18 years. Since some studies included young populations up to 21 years old, we considered selecting them if more than 50% of the participants were younger than 19 years. This decision, which allowed the selection of studies with young adults, was the only deviation from the registered protocol. The studies were to be based on upper limb interventions that used virtual reality systems combined or not with conventional therapy. In this review, we refer to virtual reality as it was defined by Schultheis (p. 298) 34 that is “an advanced form of human-computer interface that provides a multi-sensory context and allows the users to interact and immerse themselves in a computer-generated environment”. Thus, all virtual reality systems were considered, such as those designed for rehabilitation, commercial video games, as well as computer games using all degrees of immersion. The virtual reality-based therapy programs could be compared to interventions based on conventional therapy or no treatment. Given many therapeutic interventions, we considered conventional therapy any activity with therapeutic objectives that do not use virtual reality systems. The outcomes of the included studies were to be measured using validated questionnaires, scales, and tests, based on the three domains of the International Classification of Functioning, Disability and Health 35 : “body functions and structures”, “activity”, and “participation”.
We included only randomized controlled trials reported in full-text articles published in peer-reviewed journals. Inclusion was limited to publications from 1990 onward, as this was the time when virtual reality technologies began to be used in clinical practice, 36 and the period when the key technological developments of virtual reality technology for rehabilitation emerged. 37 We did not impose any language restrictions on the searches. Studies involving participants with mixed etiology (e.g. participants with acquired brain injuries) were excluded unless data from individuals with cerebral palsy were available. Studies based on virtual reality interventions combined with other types of technologies (e.g. virtual reality systems combined with motion assistance devices performed by robots) were also excluded.
Two authors (SBC and HB) independently conducted an electronic search using the following databases: PubMed, PEDro, Web of Science, Central (Cochrane Library), and EMBASE. An example of the search strategy conducted in PubMed is provided in Supplemental Material 1. The searches were conducted in January 2022, and again in September 2022, with a second update in May 2023. Moreover, the reference lists of all included studies and previous systematic reviews were screened to identify any other reports not found through electronic searches. The titles and abstracts of the records identified from the search were examined, and irrelevant ones were excluded according to the selection criteria. The full text of the selected reports was then screened for final inclusion of the studies in the systematic review.
The data extraction was performed by two authors (SBC and HB) using a predefined form. This data extraction would include the main author, year of publication, study country, sample size, age range, gender, topographic classification, and degree of cerebral palsy (e.g. I to V),38,39 type of intervention followed by the participants in the experimental and control groups, duration of program and frequency of sessions, location of the study, outcomes, follow-up, and sources of funding of each study. Data related to the characteristics of systems used in the virtual reality group programs were extracted and corresponded to the name of the system and producer, the type of virtual reality, the degree of immersion, the type of task or game, the human-machine interface for interaction, the feedback modality (i.e. visual, auditory, or haptic), the number of movement repetition in each session and the device adaptations.
The methodological quality of the studies was assessed using the PEDro scale developed by the Physiotherapy Evidence Database (www.pedro.org.au). The PEDro scale assesses the methodological quality of randomized clinical trials with a score range of 0 to 10. 40 Studies with a score of 9 to 10 points can be considered of “excellent” methodological quality, 6 to 8 of “good” quality, 4 to 5 of “fair”, and 0 to 3 of “poor” methodological quality. 41 The methodological quality was performed independently by two authors (SBC and HB).
The Grading of Recommendations Assessment, Development and Evaluation (GRADE) was employed to assess the certainty of the evidence of results. 42 The GRADE approach classifies the certainty of the evidence in one of four levels (high, moderate, low, and very low).42,43 The definition of the levels is detailed in Supplemental Material 2. The certainty of evidence can be downgraded for several reasons (domains): (1) inconsistency of results (a significant heterogeneity measure (I2) between studies; downgraded by one level when I2 ≥ 50%, and by two levels when I2 ≥ 90%); (2) indirectness (half of the participants were outside the target group); (3) imprecision (the total number of participants in the comparison was lower than the optimal sample size (>400)); (4) reporting bias (low methodological quality of more than 25% of the studies included in the comparison); (5) publication bias (asymmetry in the funnel plot). 42 The GRADE assessment was performed by one author (SBC) and verified by a second (HB).
We categorized the outcomes of the studies according to three domains of the International Classification of Functioning, Disability and Health. The Review Manager software (RevMan 5.4, The Nordic Cochrane Center, Copenhagen, Denmark) was used to perform the meta-analysis. The studies were pooled according to the proposed rehabilitation program: virtual reality combined with conventional therapy versus conventional therapy only; virtual reality alone versus conventional therapy only; virtual reality versus no treatment. Also, subgroup analyses were conducted to examine whether the results varied according to the characteristics of the virtual reality system: commercial video games versus virtual reality systems designed specifically for rehabilitation; different degrees of immersion; types of commercial video games.
As the studies measured the same outcomes but with different assessment tools, standardized mean differences (SMDs) with 95% confidence interval (CI) were used for continuous outcome measures. Effect sizes were quantified according to the system used by Cohen 44 : a small effect (SMD between 0.2 and 0.5); a medium effect (SMD between 0.5 and 0.8) and a large effect (SMD of 0.8 or higher). For the meta-analysis, the number of participants, the mean value, and the standard deviation of the outcomes in each intervention group were used. 31 When the results were reported as a median, the data were converted to mean and standard deviation according to Hozo et al. 45 The random effects model was used in comparisons that have heterogeneity among the included studies. The Chi2 test and the heterogeneity statistic (I2) were used to evaluate the heterogeneity. 46 This analysis was based on visual inspections of the forest plots.
Results
The search of the five databases identified 1.201 records. After duplication removal, 800 records were examined for eligibility by title and abstract. Of these, 39 full-text reports were screened for eligibility and 20 studies were selected for final inclusion. In addition, 13 records were identified by citations of the included studies and previous systematic reviews, and from this search, two full-text reports were screened for eligibility. Finally, 22 studies47–68 (27 reports) of randomized clinical trial designs published between 2006 and 2023 were included in this review. The study selection process is presented in the PRISMA Flow Diagram (Supplemental Material 3).
The studies included a total of 746 participants aged from 4 to 20 years, diagnosed with cerebral palsy. The sample sizes varied from 6 to 102 participants. Only one study had a crossover design. 68 For this study, the results from the period after the first trial before crossover were used. Only one study was published in Chinese, 60 and all the other twenty-one were published in English. We requested the assistance of a professional translator for the extraction of the relevant information and data from the study in Chinese.
The duration of the programs in the virtual reality and control groups ranged between 3 and 20 weeks, with a frequency of one, two, three, five, or six sessions per week. The intervention sessions in which virtual reality was used alone had a duration of between 30 and 90 min, and those in which the systems were combined with conventional therapy lasted between 30 and 145 min. Table 1 summarizes the characteristics of the participants and the proposed interventions.
Description of studies, participants, interventions, results, and funding.
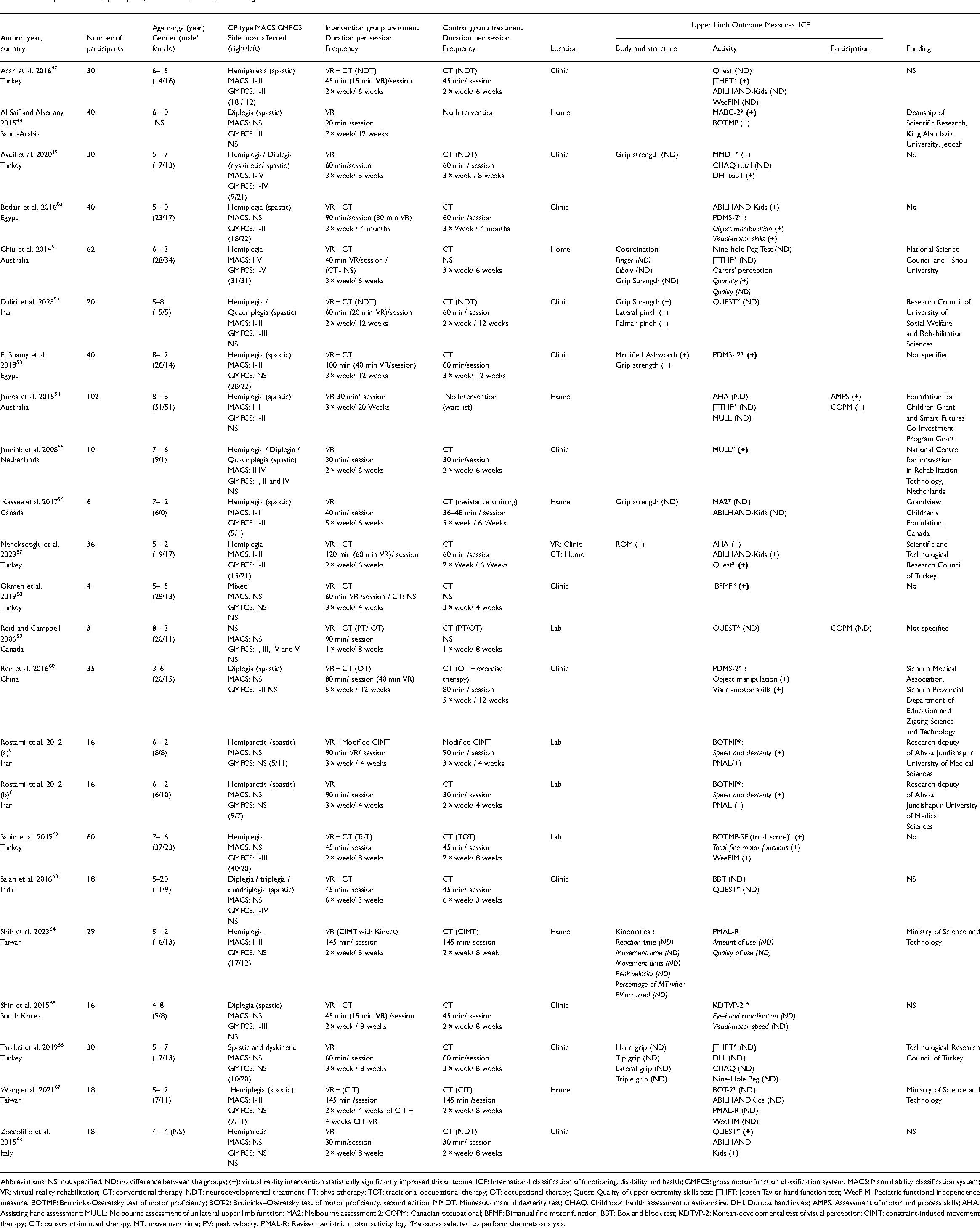
Abbreviations: NS: not specified; ND: no difference between the groups; (+): virtual reality intervention statistically significantly improved this outcome; ICF: International classification of functioning, disability and health; GMFCS: gross motor function classification system; MACS: Manual ability classification system; VR: virtual reality rehabilitation; CT: conventional therapy; NDT: neurodevelopmental treatment; PT: physiotherapy; TOT: traditional occupational therapy; OT: occupational therapy; Quest: Quality of upper extremity skills test; JTHFT: Jebsen Taylor hand function test; WeeFIM: Pediatric functional independence measure; BOTMP: Bruininks-Oseretsky test of motor proficiency; BOT-2: Bruininks–Oseretsky test of motor proficiency, second edition; MMDT: Minnesota manual dexterity test; CHAQ: Childhood health assessment questionnaire; DHI: Duruoz hand index; AMPS: Assessment of motor and process skills; AHA: Assisting hand assessment; MUUL: Melbourne assessment of unilateral upper limb function; MA2: Melbourne assessment 2; COPM: Canadian occupational; BFMF: Bimanual fine motor function; BBT: Box and block test; KDTVP-2: Korean-developmental test of visual perception; CIMT: constraint-induced movement therapy; CIT: constraint-induced therapy; MT: movement time; PV: peak velocity; PMAL-R: Revised pediatric motor activity log. *Measures selected to perform the meta-analysis.
Table 2 summarizes the main characteristics of each virtual reality system. Fifteen studies used commercial video game systems such as Nintendo Wii™,47–49,51,53,56,63,65,67 Microsoft Kinect™ for Xbox™50,68 or computer,62,64 or Sony PlayStation™.55,58 All these commercial consoles can be classified as exergames which are systems that combine physical activity with game mechanics. 69 Six studies used systems designed for rehabilitation such as Fizyosoft games,49,66 Mitii,™ 54 Mandala Gesture Xtreme IREX VR system, 59 E-Link - Evaluation and Exercise System, 61 and Leap Motion Controller games. 52 Menekseoglu et al. 57 did not report the name of the system employed in their study but indicated that it was developed in collaboration with researchers and computer engineers. Ren and colleagues 60 used the Q4 system, but the nature of this system was not indicated.
Description of virtual reality systems.
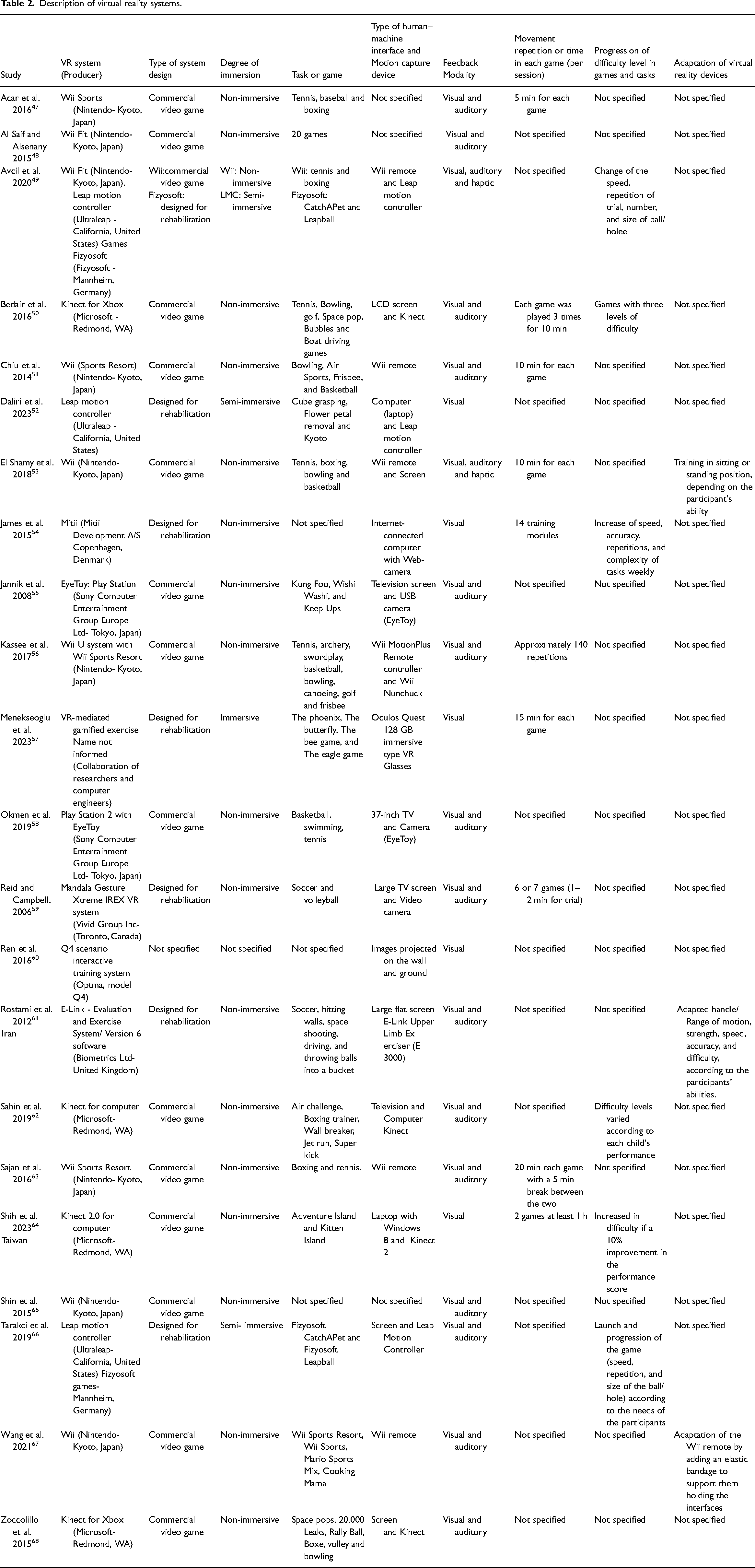
Relative to the reproduction of the images of the games, eight studies50,53,55,58,59,61,62,66 reported using televisions or screens connected to systems. Only one study used a virtual reality glass 57 and three used computer screens.52,54,64 The other studies did not specify the type of human-machine interface used. However, it is known that commercial video games require the use of a screen to reproduce the images of the games. A single study 60 reported using a device with images projected on a wall and ground with the Q4 system.
Regarding motion capture to play the games, four studies utilized the Kinect system.50,62,64,68 The Kinect contains a sensor that incorporates various sensing hardware such as a depth sensor, color camera, and microphone array that provides 3D motion capture and facial recognition. 70 Six studies that used Nintendo Wii™ reported the use of Wii controller49,51,53,56,63,67 which is the joystick included in this console for interaction and motion capture. Two studies55,58 used Sony PlayStation™ with the EyeToy application, which is a camera that detects the user's body movements and reproduces them in images, allowing interaction with games. 71 In addition, three studies49,52,66 used Leap Motion Controller which is a low-cost optical hand tracking with declared submillimeter accuracy.72,73 One study 54 used a computer for interaction with the Mitti™ system which is a web-based multimodal therapy program delivered in the home environment. Mitti™ detects and tracks bodily movements by a web camera using tracking bands worn on the hands of users. 54 One study 59 reported using a simple motion capture system camera.
The study by Menekseoglu et al. 57 was the only one that reported the use of an immersive virtual reality system through Quest 128 glasses. Three studies49,52,66 used the Leap Motion Controller considered a semi-immersive technology. The other studies did not report the degree of immersion, but due to the type of console or human-machine interface reported by the authors, we classified them as non-immersive virtual reality. 74
The items of the quality assessment of the studies using the PEDro scale are presented in Supplemental Material 4. A single study 51 was considered excellent methodological quality with a score of 9 points. Nine52–54,61–64,66,67 presented good quality with a score between 6 and 8. Ten studies47,49,50,55,57–60,65,68 presented a fair quality with a score between 4 and 5, and two48,56 received a score between 0 and 3 points with poor methodological quality.
Regarding outcome measures, only two studies54,59 assessed the participation domain of the International Classification of Functioning, Disability and Health. Of these two, only the study by James et al. 54 showed a significant effect in favor of virtual reality using the assessment tools “Canadian Occupational Performance Measure”, and the “Assessment of Motor and Process Skills”. Nine studies49,51–54,56,57,64,66 assessed body functions and structures domain. Six49,51–53,56,66 assessed grip strength but only the studies by Daliri et al. 52 and El-Shamy et al. 53 demonstrated a significant effect in favor of virtual reality interventions for this outcome. This latest study 53 also reported significant results when assessing spasticity measured by the “Modified Ashworth Scale”. Menekseoglu et al. 57 found significant results in favor of virtual reality in assessing the upper limb range of motion. All studies used measures to assess upper limb outcomes relative to the activity domain. Thus, for the comparisons with meta-analysis, we used the outcome measures the most employed in studies on upper limb activity. The list of all measures selected to perform the meta-analyses, as well as all outcomes of the included studies, are presented in Table 1.
Effects of the interventions are presented from the results of the comparisons performed by meta-analysis with the assessment of the certainty of the evidence by the GRADE approach for each analysis. The complete summary of the results of the certainty of evidence for all comparisons is presented in Supplemental Material 5.
We pooled 15 studies47,50–53,57–63,65,67,68 (479 participants) that compared virtual reality combined with conventional therapy versus conventional therapy performed alone in the improvement of upper limb activity after the intervention period up to 4 weeks follow-up. This comparison showed a medium effect in favor of virtual reality (SMD = 0.65; 95% CI 0.19, 1.11; Figure 1). The analysis of the certainty of the evidence for this comparison was low (downgraded by risk of bias and inconsistency). Publication bias was assessed using the funnel plot only for this comparison, as the others included fewer than ten studies, however, this analysis did not indicate asymmetry. Only three studies51,57,61 (109 participants) assessed upper limb activity in the short-term (up to 3 months after the intervention) in the same preceding comparison. There was no difference between the groups receiving virtual reality combined with conventional therapy and conventional therapy only (SMD = 0.73; 95% CI −0.28, 1.74; Figure 1). The certainty of evidence for this comparison was low (downgraded by inconsistency and imprecision). No study has assessed the effects of intervention over a long term (i.e. 6-month follow-up or more).
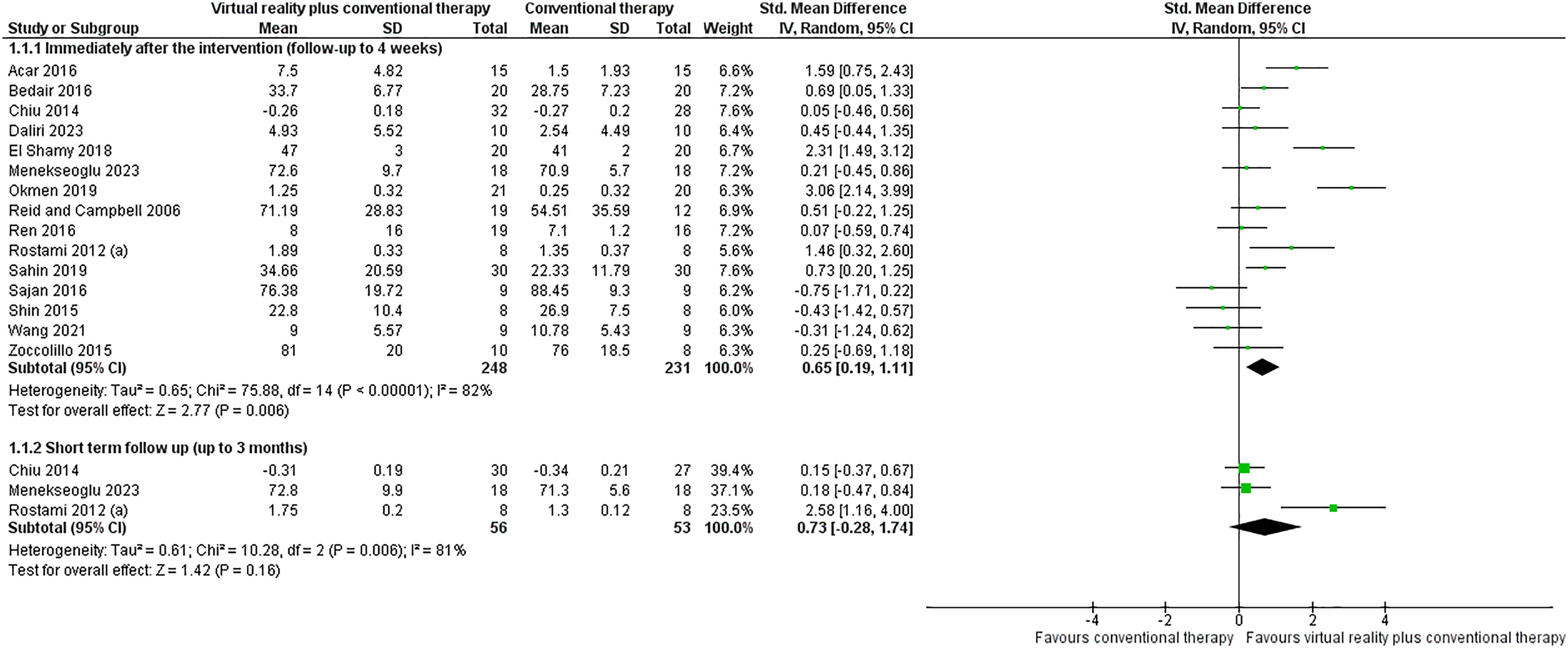
Forest plot of the meta-analyses: virtual reality plus conventional therapy compared to conventional therapy immediately after the intervention period (follow-up to 4 weeks) (1.1.1), and after 3 months of follow-up (1.1.2).
Five studies49,55,56,61,66 (92 participants) compared virtual reality used alone versus conventional therapy immediately after the intervention period up to 4 weeks of follow-up. There was no difference between these groups (SMD = 0.74; 95% CI −0.32, 1.81; Supplemental Material 6(a)). The analysis of the certainty of the evidence for this comparison was very low (downgraded by risk of bias, inconsistency, and imprecision). Two studies48,54 (131 participants) compared virtual reality to no treatment, but this meta-analysis showed no difference (SMD = 1.61; 95% CI −1.34, 4.55; Supplemental Material 6(b)). The certainty of evidence for this comparison was very low (downgraded by one level because of risk of bias, and imprecision, and two levels because of inconsistency (I2 = 97%)).
We compared in a subgroup analysis the commercial video games47,50,51,53,58,62,63,65,67,68 with virtual reality systems designed specifically for rehabilitation52,57,59,61 when used as an adjunct to conventional therapy, but we found no difference between the subgroups (P = 0.62; Figure 2). However, when analyzed separately, both commercial video games (SMD = 0.72; 95% CI 0.06, 1.39) and systems designed for rehabilitation (SMD = 0.52; 95% CI 0.08, 0.96) were more effective than conventional therapy. A second subgroup analysis showed no difference between the commercial video games55,56 and the virtual reality systems designed for rehabilitation61,66 when used alone (P = 0.28; Supplemental Material 7). When analyzed separately, the two systems were no more effective than conventional therapy.
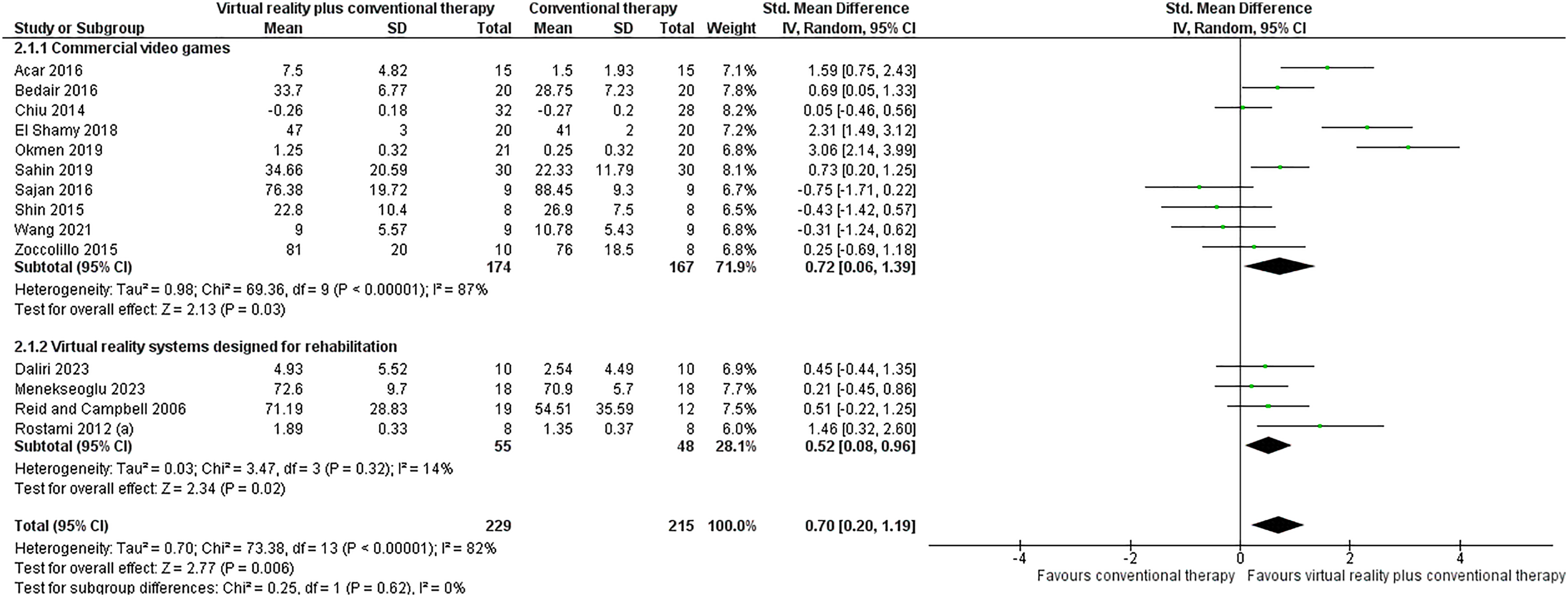
Forest plot of the subgroup analyses of commercial video games (2.1.1) or virtual reality systems designed specifically for rehabilitation (2.1.2) when combined with conventional therapy compared to conventional therapy.
We also performed a subgroup analysis to compare immersive, 57 non-immersive,59,61 and semi-immersive 52 virtual reality systems. In this comparison, all these systems were designed for rehabilitation and were combined with conventional therapy. This subgroup analysis showed no significant difference (P = 0.50; Figure 3), and when analyzed separately, these three virtual reality systems were no more effective than conventional therapy. We also analyzed the commercial video games type when used as an adjunct to conventional therapy with three subgroups: studies that had used the Nintendo Wii™,47,51,53,63,65,67 those that used the Kinect™50,62,68 for Xbox™ or computer, and one that used the Sony PlayStation™. 58 There was a difference in this subgroup analysis (P < 0.00001; Supplemental Material 8). When analyzed separately only the Kinect™ (SMD = 0.64; 95% CI 0.27, 1.01), and the PlayStation™ (SMD = 3.06; 95% CI 2.14, 3.99) were more effective than conventional therapy. The analyses of the certainty of evidence for all subgroup tests ranged from low to very low.
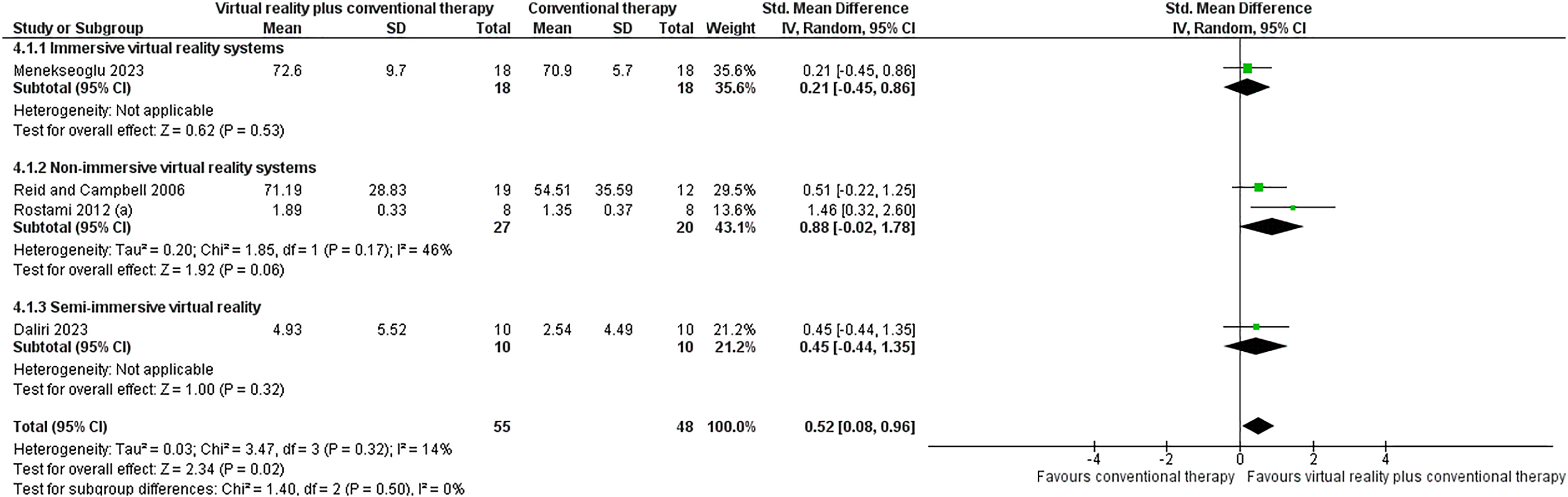
Forest plot of the subgroup analyses of virtual reality systems designed for rehabilitation: immersive (4.1.1), non-immersive (4.1.2), or semi-immersive (4.1.3) when combined with conventional therapy and compared to conventional therapy only.
Discussion
This systematic review included 22 studies that examined the effectiveness of virtual reality systems on upper limb impairments in children and young adults with cerebral palsy. The meta-analysis showed an effect in favor of virtual reality when it was combined with conventional therapy to improve upper limb activity. However, the certainty of the evidence for this analysis assessed by the GRADE was low due to the high risk of bias and heterogeneity among studies. No differences were found between virtual reality used alone when compared to conventional therapy or no treatment. These two comparisons showed a very low certainty of evidence.
Our findings are consistent with those reported by Fandin and colleagues 28 in 2020 in their meta-analysis that also found an effect of virtual reality when combined with conventional therapy. However, for this analysis, the effect size we found (SMD = 0.65) was less than that obtained by these authors (SMD = 1.06). Chen and colleagues 27 in 2018 also found a large effect (SMD = 0.83), yet they combined in the same meta-analysis the results of thirteen studies in which virtual reality was used alone or added to conventional therapy. This combination of different programs in the same analysis may make it difficult to understand the effects found in this review published in 2018. Our review aimed to perform an update of the existing evidence considering studies that were published after the last search,49,52,57,64,67 as well as some previously published research56,60,65,66 that were not included in either of these two previous reviews.27,28 Nevertheless, even including new studies, we reach a similar conclusion to these two other reviews regarding the need for future research with a low risk of bias, larger sample sizes, and less heterogeneity in study design to increase the strength of evidence in this field.
We identified ten different virtual reality systems employed in the interventions, of which six were designed specifically for rehabilitation and four were commercial video games. It should be noted, however, that 15 studies used commercial video games, compared to only seven that employed specialized systems. Subgroup analysis showed no differences when these two types of systems were compared, either when they were used in combination with conventional therapy or alone. However, both types of systems were effective when used in addition to conventional therapy. The Cochrane review by Laver and colleagues 75 found similar results when comparing the two types of systems of stroke patients.
Although the differences between commercial video games and specialized systems are not demonstrable, some authors15,16,29 emphasize that devices designed for rehabilitation may be better adapted to the needs of treatments. For example, Demers et al. 16 considered that specialized systems are developed in considering the user's disabilities and present a more adapted game difficulty and target training. Two other reviews76,77 summarized the recommendations for designing virtual reality systems for rehabilitation and highlighted the importance of collaborative work between virtual reality experts, engineers, and researchers and end-user engagement, such as clinicians and patients. The main disadvantage of these specialized systems is probably their cost. 78 This is why commercial video games can provide simple, low-cost,27,78 and motivating solutions thanks to the playfulness and variety of the games.79,80 These systems can also be more easily employed for home interventions.
We can highlight some limitations in conducting our review. Since we only included randomized controlled trials, there is a risk that several virtual reality systems that are used for rehabilitation but were examined in other types of study designs (e.g. non-randomized, observational, and feasibility studies) could not be identified and included in this review. Moreover, we did not analyze the adverse events (e.g. dizziness, headache, eye fatigue, and motion sickness) 81 of the proposed virtual reality programs. Taking these events into account could help identify the limits to the use of virtual reality.
In addition, we can discuss some limitations of the studies included in our review from a methodological and outcome assessment standpoint. For example, some risks of bias assessed by the PEDro scale could be avoided. In studies examining the effects of technology-based interventions, it is very difficult to blind participants and therapists to the therapy being performed. However, it is possible to blind the assessor, although this was performed in only half of the studies included in this review.49,51–53,59,61–64,66–68 In addition, few studies used intention-to-treat analysis,47,51,52,54,61,62,64 and more than half had PEDro scores lowered because concealed allocation was not mentioned or was unclear.47–49,55–61,65,68 To ensure robustness, future research should consider these risks of bias as well as others assessed by the PEDro scale when designing randomized controlled trials. Regarding the strategies employed to assess the outcomes, all studies performed analyses immediately after the completion of the programs, and only three51,57,61 followed up on short-term results (up to 3 months after the intervention). It would be important for studies to be interested in the long-term effects of interventions (e.g. 6 months follow-up or more). Moreover, most studies were interested in assessments related to the activity domain of the International Classification of Functioning, Disability and Health, and few reported results related to the areas of body functions and structures, or participation. Assessments highlighting these last two domains should also be considered in future research to discuss the impact of virtual reality interventions on these aspects. 82
It should also be noted that only one study used an immersive virtual reality system. 57 The subgroup analysis does not allow a conclusion to be drawn on the absence of a difference in the comparison between immersive, semi-immersive, and non-immersive systems. Consequently, it appears that more research is needed to examine the benefits of more immersive technologies and their adverse effects.
Our findings also offer some suggestions for clinical practice. Virtual reality systems have proven to be effective when added to conventional therapy. This is consistent with Novak and colleagues 83 who systematically described in 2019 the best evidence for interventions in cerebral palsy, and considered virtual reality technologies as adjunctive therapies that can increase the benefits of rehabilitation. Yet, as the studies in our analysis are heterogeneous in terms of session length, some programs may have been more intense than others in integrating virtual reality. It is to be noted that the amount of practice may be the key element of virtual reality. Indeed, the use of virtual technologies in rehabilitation is based on motor learning elements, 18 and thus can be useful as a tool that integrates the aspects of repetition and intensity into therapy. In addition, other aspects considered challenging for conventional therapy seemed to be employed in some virtual reality systems, such as difficulty adjustment and goal-oriented tasks. 15 Some commercial video games and specialized systems can record performance data at each session, and the more advanced can perform kinematic and muscle strength measurements (e.g. E-Link - Evaluation and Exercise System). 61 Virtual reality can also add the fun factor to the intervention, one of the F-words (i.e. functioning, family, fitness, fun, friends, and future) suggested as a necessary focus in childhood disability, 84 and thus could facilitate the patients’ engagement in therapy.
From a practical standpoint, the virtual reality systems analyzed in this review integrate some principles necessary for rehabilitation but differ from each other in terms of the technology and interface employed, type of interaction, variety of games, degree of immersion, and how the system is designed. At this stage, it is still difficult to determine which system is the most effective for upper limb rehabilitation in children and young adults with cerebral palsy. However, our findings could guide clinicians to identify the characteristics of different virtual reality systems and decide if this is the best tool to include in their rehabilitation programs, depending on the needs, the resources, the intervention environment, or the profile of their patients. In this case, the choice for the system can be made according to the rehabilitation context, the patient's preferences, and the clinician's knowledge. These results are important to health professionals that use evidence-based practice in their decision-making.85,86
Clinical messages
Different types of virtual reality systems are used in therapeutic interventions for children and young adults with cerebral palsy.
Virtual reality combined with conventional therapy was effective in improving upper limb activity.
The certainty of the evidence ranged from very low to low limiting the confidence in the effect estimates found.
Supplemental Material
sj-docx-1-cre-10.1177_02692155231187858 - Supplemental material for Effectiveness of virtual reality interventions of the upper limb in children and young adults with cerebral palsy: A systematic review with meta-analysis
Supplemental material, sj-docx-1-cre-10.1177_02692155231187858 for Effectiveness of virtual reality interventions of the upper limb in children and young adults with cerebral palsy: A systematic review with meta-analysis by Simone Burin-Chu, Héloïse Baillet, Pascale Leconte, Laure Lejeune, Régis Thouvarecq and Nicolas Benguigui in Clinical Rehabilitation
Footnotes
Author contributions
SBC; NB; PL; HB; LL were involved in the conception and design of the review. SBC and HB performed study selection, data extraction, quality, and certainty of the evidence assessment of the studies. SBC performed the statistical analysis and the forest plots. All authors were involved in the interpretation and discussion of results. NB monitored the review progress. SBC drafted the manuscript, and all authors revised the draft. All authors edited the manuscript and approved the last version submitted for publication.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This review was supported by “RV rééduc” European project, co-funded by the Normandy County Council and the European Union in the framework of the ERDF-ESF operational program 2014-2020.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
