Abstract
Objective
‘Better By Moving’ is a multifaceted intervention developed and implemented in collaboration with patients and healthcare professionals to improve physical activity in hospitalized adults. This study aimed to understand if, how and why ‘Better By Moving’ resulted in higher levels of physical activity by evaluating both outcomes and implementation process.
Design
Mixed-methods study informed by the Medical Research Council guidance.
Setting
Tertiary hospital.
Participants
Adult patients admitted to surgery, haematology, infectious diseases and cardiology wards, and healthcare professionals.
Measures
Physical activity was evaluated before and after implementation using the Physical Activity Monitor AM400 on one random day during hospital stay between 8 am and 8 pm. Furthermore, the time spent lying on bed, length of stay and discharge destination was investigated. The implementation process was evaluated using an audit trail, surveys and interviews.
Results
There was no significant difference observed in physical activity (median [IQR] 23 [12–51] vs 27 [17–55] minutes,
Conclusion
Although implementing ‘Better By Moving’ did not result in significant improvements in outcomes at our centre, the process evaluation yielded important insights that may improve the effectiveness of implementing multifaceted interventions aiming to improve physical activity during hospital stay.
Introduction
Hospitalized adult patients spend up to 87–100% of their time sitting or lying in bed. 1 These low levels of physical activity during hospital stay have been observed in geriatric, surgical, medical and post-stroke patients. 1 There is growing evidence that low levels of physical activity during hospital stay lead to adverse outcomes such as functional decline, prolonged length of hospital stay, institutionalization after discharge and mortality.2–4
Recent evidence revealed that interventions improving physical activity during a hospital stay can help prevent functional decline.5–9 However, patients are still put to bed when admitted, 10 the hospital bed remains to be centrepiece, 11 and very low physical activity levels continue to be observed in hospitalized patients all over the world.1,12 A discrepancy exists between what is known to prevent functional decline and what happens in current hospital care.
To bridge this gap, multifaceted interventions are needed that tackle multiple barriers and effect behavioural and cultural change with respect to physical activity during hospital stay. 13 To date, several multifaceted interventions have been described and these show they can effectuate positive changes regarding the time patients spent lying in bed and sitting,9,14 mobility levels, 8 functional decline, 7 length of hospital stay8,9 and discharge home.9,14 Although these results are promising, most of them lack a process evaluation illuminating how these results occurred and how improvements can be made.
Process evaluations have been conducted concurrently or following a complex intervention to assess whether implementation was successful and to explore if, how and why the intervention had an impact.
15
This insight could assist the interpretation of causality, offer suggestions for improving the implementation of such a multifaceted intervention and explain how the effect of this particular intervention on patient outcomes can be replicated in another context or setting. The United Kingdom Medical Research Council offers a framework consisting of three key functions:
To improve physical activity in hospitalized adult patients admitted to the Amsterdam University Medical Centers, we developed and implemented a theory-driven, multifaceted intervention called ‘Better By Moving’ in close collaboration with patients and healthcare professionals.
17
Insight in if, how and why the ‘Better By Moving’ intervention resulted in higher levels of physical activity will allow us to formulate recommendations for developing and implementing such a multifaceted intervention in another context or setting. Therefore, the aim of this study was to conduct a hybrid evaluation of ‘Better By Moving’, using an outcome and process evaluation to study both the intervention's effectiveness on physical activity and the implementation process in terms of
Methods
Study design
This study used a mixed-methods evaluation study design, and the Medical Research Council guidance on process evaluations 15 was used to guide the hybrid evaluation. To evaluate the effectiveness of the ‘Better By Moving’ intervention on patient outcomes, we collected quantitative data using before-after implementation cross-sectional measurements and longitudinal data from the hospital administrative system. To evaluate the implementation process, we concurrently collected quantitative and qualitative data using an audit trail (i.e. a strategy to trace the process), surveys and interviews. Study reporting followed the Standards for QUality Improvement Reporting Excellence (version 2.0). 18 Ethical approval was granted by the Medical Ethics Committee of the Amsterdam UMC (W17_479 #18.003 and W19_213 #19.258), Amsterdam, The Netherlands. All patients and healthcare professionals provided written informed consent. The study protocol including details on design, implementation process and outcome measures has been published elsewhere. 17
Setting
This study was conducted within five hospital wards of the tertiary university hospital Amsterdam University Medical Centers, location Academic Medical Center, the Netherlands: two gastrointestinal and oncological surgery wards (January 2018 to January 2019), one hematology ward (August 2018 to August 2019), one infectious diseases ward (August 2018 to August 2019) and one cardiology ward (May 2019 to March 2020).
The ‘Better By Moving’ multifaceted intervention
The primary goal of the ‘Better By Moving’ intervention was to improve physical activity in adult patients during hospital stay. We used a structured, step-by-step implementation plan according to the evidence-based Implementation of Change process model by Grol and Wensing.17,19,20
The first stage to develop the content of the ‘Better By Moving’ intervention was to assess the amount of time patients spent physically active and lying in bed in each ward and to identify the barriers and enablers to improve physical activity from the perspective of patients and healthcare professionals. 17 The Theoretical Domains Framework to identify determinants of behaviour was used to support the exploration of barriers and enablers. 21 The results have recently been published.12,22
Having established the barriers and enablers, the Behaviour Change Wheel
23
was used to select intervention components (e.g. learning how to assist patients in physical activity) and implementation strategies (e.g. information brochures, clinical lessons). This was conducted by ward-specific working groups consisting of physician(s), physician assistant(s), nurses, nursing assistant(s), physical therapists, a program manager (SG) and a senior nurse or team leader.21,23 Convenience samples of patients, caregivers, team leaders and local policymakers provided occasional input. This process is outlined in Appendix 1 and resulted in eight intervention components targeting patients (Table 1) and 15 intervention components targeting healthcare professionals (Table 2). Most intervention components (
Overview of intervention components targeting hospitalized patients.

COM-B: the Capability, Opportunity, Motivation – Behaviour system which forms the hub of the Behaviour Change Wheel; TDF: the Theoretical Domains Framework determinant framework; A: surgery ward #1; B: surgery ward #2; C: haematology ward; D: infectious diseases ward; E: cardiology ward.
Overview of intervention components targeting healthcare professionals.
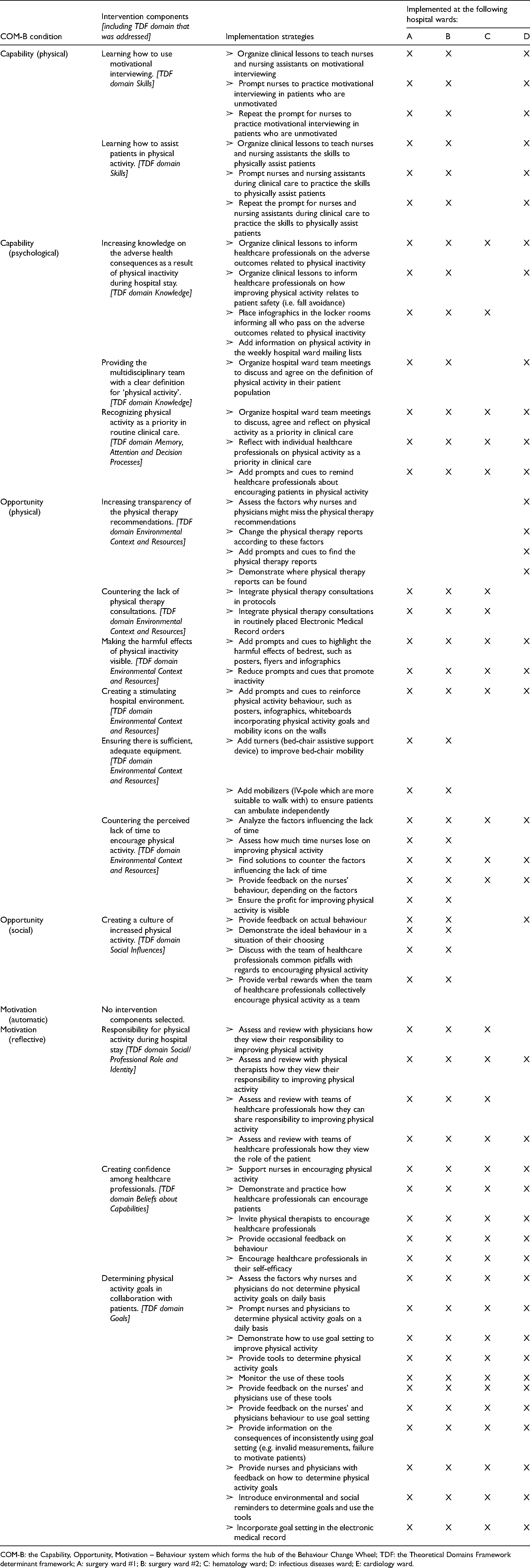

COM-B: the Capability, Opportunity, Motivation – Behaviour system which forms the hub of the Behaviour Change Wheel; TDF: the Theoretical Domains Framework determinant framework; A: surgery ward #1; B: surgery ward #2; C: hematology ward; D: infectious diseases ward; E: cardiology ward.
To implement the ‘Better By Moving’ intervention, each working group developed and executed an implementation plan for the intervention components they deemed feasible and effective at their hospital ward. The taxonomy of 93 Behaviour Change Techniques was used to specify implementation strategies. 23 Throughout the implementation, working groups strived for optimal integration within routine hospital care. The implementation strategies linked to the intervention components are shown in Tables 1 and 2.
Outcome evaluation
The primary outcome was the difference in amount of physical activity of patients before-after implementation. Physical activity was assessed on one random day during hospital stay between 8 am and 8 pm using the Physical Activity Monitor AM400. 24 The Physical Activity Monitor AM400 is a 2-cm-wide coin attached to the ankle, and validly measures three-dimensional accelerations as a derivative for Metabolic Equivalent Tasks to determine the time patients spent physically active in minutes (>1.4 Metabolic Equivalent Tasks).24,25 Metabolic Equivalent Tasks express the energy cost of physical activities. Eligible patients are 18 years or older, can communicate in Dutch or English, and are admitted for at least 24 h. Exclusion criteria were: insufficient Dutch or English speaking and reading skills, inability to perform independent bed-to-chair transfer before hospital admission, delirium, obligatory bed rest, receiving end-of-life care and discharge before 12 am on the day of observations. Eligible patients were approached one or two days prior to observation in a random order using a computer-generated list based on the room numbers. Each patient could only be enrolled once throughout the study.
Secondary outcomes were time spent lying on bed, length of hospital stay and proportion of patients discharged home instead of a temporarily institution. Time spend lying in bed was assessed over the same time period as the primary outcome using a behavioural mapping protocol. 26 Length of stay and proportion of patients discharged home were assessed in all patients admitted for three days or longer to one of the hospital wards using an Interrupted Time Series approach over 30 months (i.e. 12 months before, 12 months during and 6 months after implementation). 27 This approach allowed us to assess the effect over time by comparing the slopes (i.e. trends) before-during-after implementation and to assess the immediate effect by comparing the level changes at implementation start (month 0) and stop (month 13). 27 Discharge destination was categorized as (1) home with or without homecare, and (2) discharged to a temporary institution (i.e. temporary nursing home, geriatric rehabilitation center, or medical rehabilitation center). Discharges to permanent nursing homes, other hospitals, end-of-life care facilities or patients who passed away were omitted. The data were obtained as de-identified data from the hospital administrative system.
Process evaluation
Process outcomes were defined as
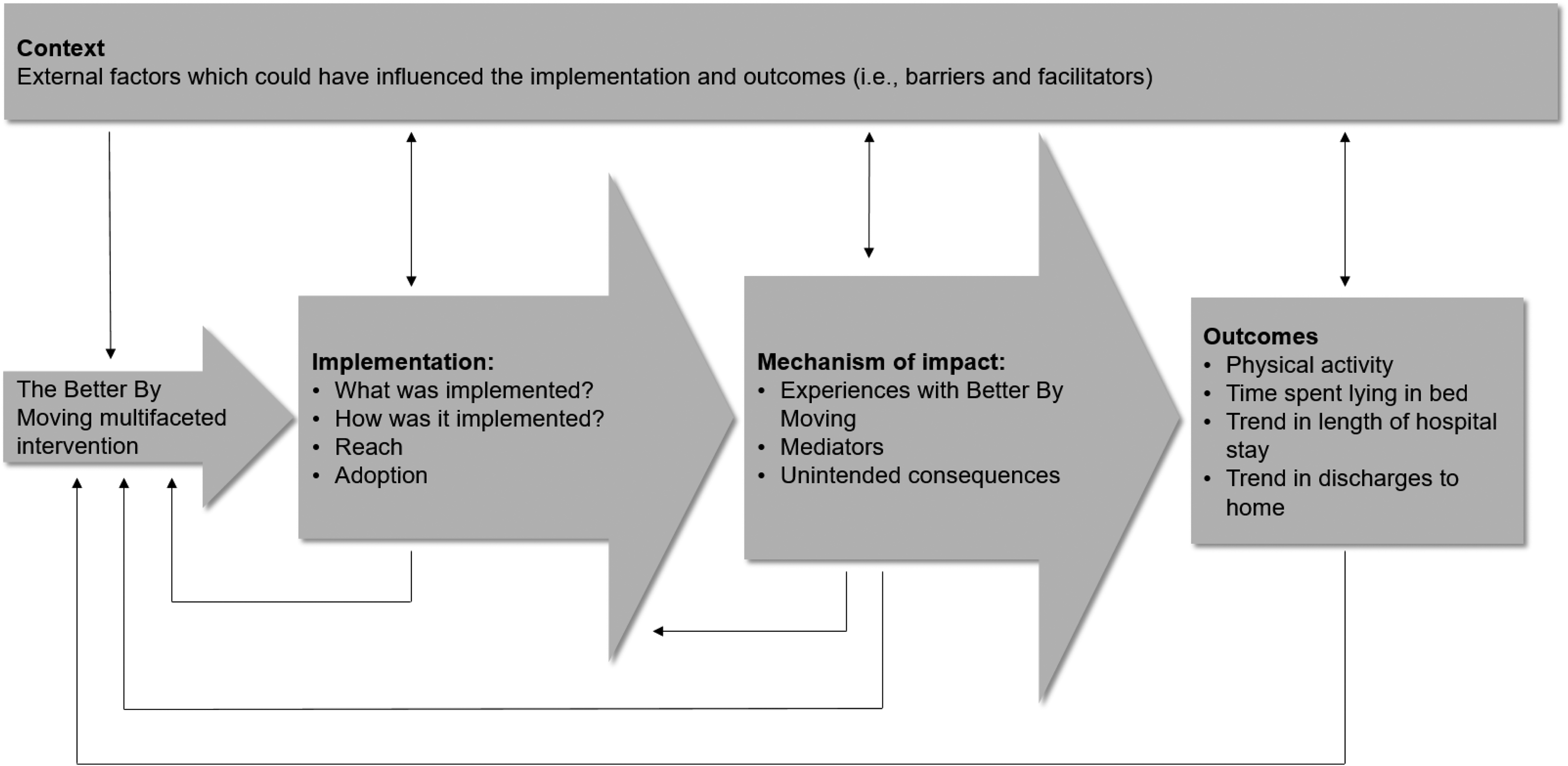
Key functions of the ‘Better By Moving’ intervention process evaluation and relations among them (after UK Medical Research Council guidance. 15 )
For the process evaluation, all hospitalized patients were asked to complete the questionnaire one day after the day of observation. Furthermore, healthcare professionals employed for at least 70% of full-time equivalent at one of the five wards were asked to complete the questionnaire after implementation. After the questionnaire, we conducted semistructured interviews with healthcare professionals to provide a more in-depth understanding of the survey responses concerning all three process outcomes. We aimed to include a heterogeneous group with respect to working group participation, working experience and profession.
Data analysis
No a priori sample size calculations were performed. Financial and logistic resources allowed us to include a pragmatic sample with an estimated size of
Descriptive statistics were derived to describe the patient characteristics. Normality was evaluated with the Kolmogorov–Smirnov test and Q–Q plots. A negative binomial regression model was used to assess the difference in physical activity before-after implementation, with the presence of urinary catheter used as a covariate.12,17 An analysis of covariance was performed to assess the difference in time spent lying on bed and included the same covariate. In the published protocol,
17
independence in mobility was also mentioned as covariate; however, due to a significant difference (
Qualitative data were analyzed using the thematic analysis approach as described by Braun and Clark.17,28 The research team participated in refining the preliminary themes and member checking was used with the participants to ensure the credibility of the data analysis. MAXQDA Analytics Plus 2018 (VERBI Software) supported the analysis.
Results
Due to the COVID-19 crisis, the implementation of the ‘Better By Moving’ intervention in the Cardiology ward was put on hold in March 2020 and, as a result, the cardiology ward is not included in the hybrid evaluation.
Outcome evaluation
Participant characteristics
In total, 88 and 85 patients, respectively, were included before-after implementation. Patient characteristics of both groups are presented in Table 3. No significant differences in patient characteristics before-after implementation were observed (
Primary and secondary outcomes
After implementation, there was no significant difference observed in physical activity between 8 am and 8 pm compared to before implementation (median [IQR] 23 [12–51] minutes before vs 27 [17–55] minutes after,
Before-after implementation differences in patient characteristics.

IQR: interquartile range.
Score of 20 when using questions 1–5 Activity Measure for Post-Acute Care (AM-PAC) Basic Mobility.
Urine catheter presence.
Process evaluation
Participant characteristics
In total,
Implementation
Tables 1 and 2 show which intervention components were implemented and how they were implemented per hospital ward. In summary, clinical lessons to increase knowledge (attendance 61% [
Reach among patients varied from 26% (
Adoption among patients who were reached varied from 19% (
Mechanisms of impact
In total, 43.8% (
The majority (59.7%,
Context
We identified five barriers influencing the implementation and outcomes from the perspective of healthcare professionals. Firstly, the inability of nurses to consistently participate in the working groups. Secondly, the lack of active involvement of physicians in the working group. Thirdly, the lack of resources to facilitate working group participants to spend more time on implementing intervention components or to finance more substantive changes to the wards’ environment. Fourthly, an imminent renovation or relocation of the wards, preventing more permanent environmental changes from being allowed. Lastly, the working group participants at some wards perceived a lack of support from leadership and the multidisciplinary team, caused by the multiplicity of different projects.
A facilitator was the availability of a project manager to manage, facilitate and keep an overview of the quality improvement process during all phases at the different wards. The multidisciplinary approach was also commonly noted as a facilitator to develop intervention components that were not only related to one profession. Furthermore, the extensive exploration of barriers and enablers and the bottom-up approach to select and implement intervention components meeting the needs of the wards were noted as facilitators. Both contributed to making the healthcare professionals feel heard and to creating ownership among working group participants. They also indicated the project did not increase the nursing workload. Support of the leadership and involvement of patients and caregivers in selecting intervention components were specifically reported as facilitators by workgroup participants. Lastly, having small multidisciplinary projects focusing on improving physical activity prior to the ‘Better By Moving’ intervention and aligning intervention components with routine clinical care or other running projects (e.g. the involvement of patients’ caregivers in postoperative care) were perceived as facilitators.
Discussion
The aim of this study was to conduct a hybrid evaluation of ‘Better By Moving’, a newly developed theory-informed multifaceted intervention to improve physical activity in hospitalized adult patients. The findings of our outcome evaluation indicate that implementing the ‘Better By Moving’ intervention on four different wards of the Amsterdam University Medical Centers was not associated with significant improvement in physical activity, reduction of time spent lying in bed or length of hospital stay or increase in discharges home. These results are in contrast with previous studies that reported improved patient outcomes after implementing a multifaceted intervention during hospital stay.7–9,14,29 To obtain insight in why the ‘Better By Moving’ intervention was not associated with significant improvement in physical activity and secondary outcomes, we concurrently conducted a process evaluation. Based on this process evaluation, we hypothesize that moderate reach and low adoption contributed to the lack of effectiveness of the ‘Better By Moving’ intervention. By using a bottom-up co-creational approach to select, tailor and implement the intervention components, 17 we intended to establish ownership among healthcare professionals and leadership. 30 Apparently, this was not achieved, likely due to the lack of support in terms of priority, resources and involvement, both at staff- and ward level. Other reasons for different outcomes compared to previous studies may be the amount and variety in intervention components,7–9,14,29 difference in outcome evaluation (e.g. procedures, analyses),7–9,14,29 difference in patient population7,8,29 or difference in context (e.g. local hospital admissions and discharge policies).7,8,29
To date, two previous multifaceted interventions to improve in-hospital physical activity included a process evaluation29,31 and only one of these evaluated reach and adoption of their intervention components. 31 With reach and adoption varying from 54% to 86%, 31 they observed a significant decrease in time spent lying in bed and number of discharges to a rehabilitation setting after implementation. 14 This contrasts with our findings indicating that significant improvements in patient outcomes are likely depending on the level of reach and adoption of each intervention component. 15 Therefore, we recommend that reach and adoption should be monitored during implementation. A recent study performed by Khadjesari et al. 32 provides guidance on how to measure reach and adoption validly and reliably during implementation.
Further, statistically significant differences in several
Even though it is commonly assumed that multifaceted interventions lead to more effective changes when compared to single-component interventions, compelling evidence is still lacking. 33 Given the moderate reach and low adoption, we agree with the suggestion made by previous researchers that fewer components with a clear hierarchical structure may help to increase effectiveness31,33 because a narrow focus ensures that more attention and effort can go to implementing the intervention components (i.e. improving reach and adoption). An example of such intervention is the multifaceted intervention study conducted by Cohen et al. 7 focusing on implementing the 900-step mobility goal to prevent hospitalization-associated functional decline among older adults. Video clips, in-personal communication, brochures, posters and staff-training were all used to support achieving this walking-dose benchmark in as many patients as possible.
Finally, implementing a multifaceted intervention may have different effects in different contexts even if its implementation does not vary. 15 Through the implementation of the ‘Better By Moving’ intervention in the Amsterdam University Medical Centers, we identified five contextual barriers and eleven contextual facilitators, with the level of support in terms of priority, resources and involvement—both at staff- and ward level—appearing to be the common denominator. Context includes anything external to the intervention, 15 but this does not necessarily mean that contextual factors cannot be influenced. This has recently been highlighted by Geerligs et al., 30 who recommend to consider factors relating to the staff and system (e.g. ward) as active components that can be influenced during intervention development and implementation.
Strengths and limitations of the study
A major strength of this study is the integration of outcome and process evaluation. 15 Another strength of this study was the combination of different theoretical approaches used to address various implementation and evaluation challenges in the ‘Better By Moving’ intervention.15,19,21,23 Lastly, an important strength of this study is the implementation of usual care in a heterogeneous hospital population.
This study also has some limitations. Firstly, our uncontrolled before-after study design does not allow us to conclude direct causation. 34 Secondly, the limited power of our before-after evaluation of physical activity and time spent lying in bed may have caused a type II error (i.e. false negative results). 17 Thirdly, although the ‘Better By Moving’ intervention may have been effective on individual hospital wards, lack of statistical power in this quality improvement project did not allow a ward-specific analysis. Fourthly, this is a single-site study in a university hospital in the Netherlands, limiting the generalizability of the results.
Conclusions
Although implementing the ‘Better By Moving’ intervention did not result in significant improvements in physical activity and secondary outcomes at our center, the process evaluation of ‘Better By Moving’ yielded valuable information that may improve the effectiveness of implementing future multifaceted interventions aiming to improve physical activity during hospital stay. Future research should focus on investigating the effectiveness of using a more flexible and iterative approach to improve physical activity during hospital stay.
Multifaceted interventions to improve in-hospital physical activity are more likely to be successful when they include a limited amount of components with a clear hierarchical structure, implementation teams closely monitor reach and adoption during implementation, and implementation teams are sufficiently supported in terms of priority, resources and involvement.Clinical messages
Footnotes
Author contributions
SJGG, RHHE and MvdS were responsible for study conception and study design. SJGG was also responsible for data collection, data analyses, data interpretation, drafting the manuscript and reviewing the manuscript. BMG contributed by collecting process evaluation data, analyzing the process evaluation data, editing the manuscript and reviewing the manuscript. FN contributed in study conception, editing the manuscript and reviewing the manuscript. CV and RHHE contributed in study design, data interpretation, editing the manuscript and reviewing the manuscript. MvdS contributed to data interpretation, quality control, editing the manuscript and reviewing the manuscript. All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Amsterdam UMC (grant number Unrestricted internal innovation fund).
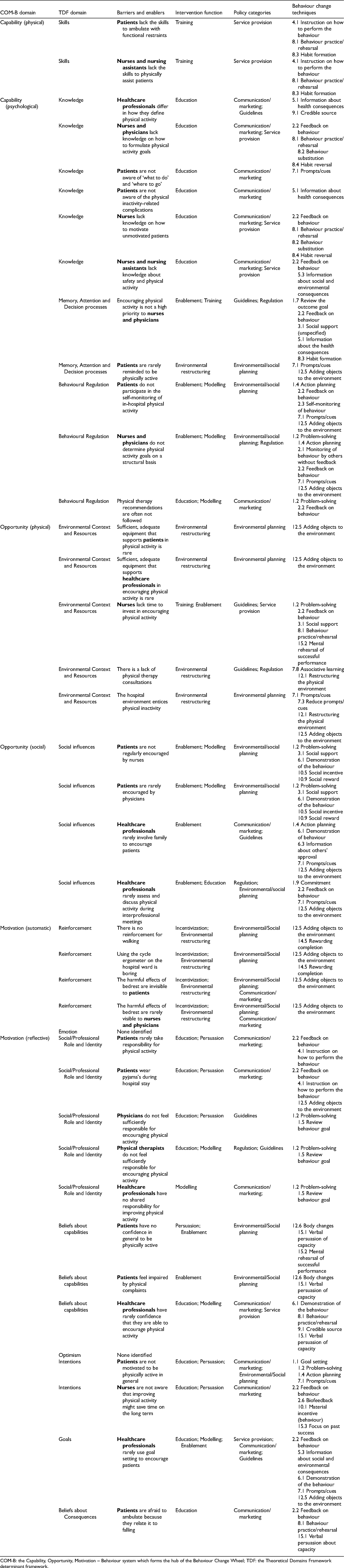
An overview of the perceived barriers and enablers with linked intervention functions and BCTs.
| COM-B domain | TDF domain | Barriers and enablers | Intervention function | Policy categories | Behaviour change techniques |
|---|---|---|---|---|---|
| Capability (physical) | Skills | Training | Service provision | 4.1 Instruction on how to perform the behaviour |
|
| Skills | Training | Service provision | 4.1 Instruction on how to perform the behaviour |
||
| Capability (psychological) | Knowledge | Education | Communication/marketing; Guidelines | 5.1 Information about health consequences |
|
| Knowledge | Education | Communication/marketing; Service provision | 2.2 Feedback on behaviour |
||
| Knowledge | Education | Communication/marketing | 7.1 Prompts/cues | ||
| Knowledge | Education | Communication/marketing | 5.1 Information about health consequences | ||
| Knowledge | Education | Communication/marketing; Service provision | 2.2 Feedback on behaviour |
||
| Knowledge | Education | Communication/marketing; Service provision | 2.2 Feedback on behaviour |
||
| Memory, Attention and Decision processes | Encouraging physical activity is not a high priority to |
Enablement; Training | Guidelines; Regulation | 1.7 Review the outcome goal |
|
|
|
Memory, Attention and Decision processes | Environmental restructuring | Environmental/social planning | 7.1 Prompts/cues |
|
|
|
Behavioural Regulation | Enablement; Modelling | Environmental/social planning | 1.4 Action planning |
|
|
|
Behavioural Regulation | Enablement; Modelling | Environmental/social planning; Regulation | 1.2 Problem-solving |
|
|
|
Behavioural Regulation | Physical therapy recommendations are often not followed | Education; Modelling | Communication/marketing | 1.2 Problem-solving |
| Opportunity (physical) | Environmental Context and Resources | Sufficient, adequate equipment that supports |
Environmental restructuring | Environmental planning | 12.5 Adding objects to the environment |
| Environmental Context and Resources | Sufficient, adequate equipment that supports |
Environmental restructuring | Environmental planning | 12.5 Adding objects to the environment | |
| Environmental Context and Resources | Training; Enablement | Guidelines; Service provision | 1.2 Problem-solving |
||
| Environmental Context and Resources | There is a lack of physical therapy consultations | Environmental restructuring | Guidelines; Regulation | 7.8 Associative learning |
|
| Environmental Context and Resources | The hospital environment entices physical inactivity | Environmental restructuring | Environmental planning | 7.1 Prompts/cues |
|
| Opportunity (social) | Social influences | Enablement; Modelling | Environmental/social planning | 1.2 Problem-solving |
|
|
|
Social influences | Enablement; Modelling | Environmental/social planning | 1.2 Problem-solving |
|
|
|
Social influences | Enablement | Communication/marketing; Guidelines | 1.4 Action planning |
|
|
|
Social influences | Enablement; Education | Regulation; Environmental/social planning | 1.9 Commitment |
|
| Motivation (automatic) | Reinforcement | There is no reinforcement for walking | Incentivization; Environmental restructuring | Environmental/Social planning | 12.5 Adding objects to the environment |
|
|
Reinforcement | Using the cycle ergometer on the hospital ward is boring | Incentivization; Environmental restructuring | Environmental/Social planning | 12.5 Adding objects to the environment |
|
|
Reinforcement | The harmful effects of bedrest are invisible to |
Incentivization; Environmental restructuring | Environmental/Social planning; Communication/marketing | 12.5 Adding objects to the environment |
|
|
Reinforcement | The harmful effects of bedrest are rarely visible to |
Incentivization; Environmental restructuring | Environmental/Social planning; Communication/marketing | 12.5 Adding objects to the environment |
| Emotion | None identified | ||||
| Motivation (reflective) | Social/Professional Role and Identity | Education; Persuasion | Communication/marketing; | 2.2 Feedback on behaviour |
|
| Social/Professional Role and Identity | Education; Persuasion | Communication/marketing; | 2.2 Feedback on behaviour |
||
| Social/Professional Role and Identity | Education; Persuasion | Guidelines | 1.2 Problem-solving |
||
| Social/Professional Role and Identity | Education; Modelling | Regulation; Guidelines | 1.2 Problem-solving |
||
| Social/Professional Role and Identity | Modelling | Communication/marketing; | 1.2 Problem-solving |
||
| Beliefs about capabilities | Persuasion; Enablement | Environmental/Social planning | 12.6 Body changes |
||
| Beliefs about capabilities | Enablement | Environmental/Social planning | 12.6 Body changes |
||
| Beliefs about capabilities | Education; Modelling | Communication/marketing; Service provision | 6.1 Demonstration of the behaviour |
||
| Optimism | None identified | ||||
| Intentions | Education; Persuasion; | Communication/marketing; Environmental/Social planning | 1.1 Goal setting |
||
| Intentions | Education; Persuasion | Communication/marketing | 2.2 Feedback on behaviour |
||
| Goals | Education; Modelling; Enablement | Service provision; Communication/marketing; Guidelines | 2.2 Feedback on behaviour |
||
|
|
Beliefs about Consequences | Education | Communication/marketing | 2.2 Feedback on behaviour |
COM-B: the Capability, Opportunity, Motivation – Behaviour system which forms the hub of the Behaviour Change Wheel; TDF: the Theoretical Domains Framework determinant framework.
Before-after implementation differences in physical activity and time spent lying in bed between 8 am and 8 pm.
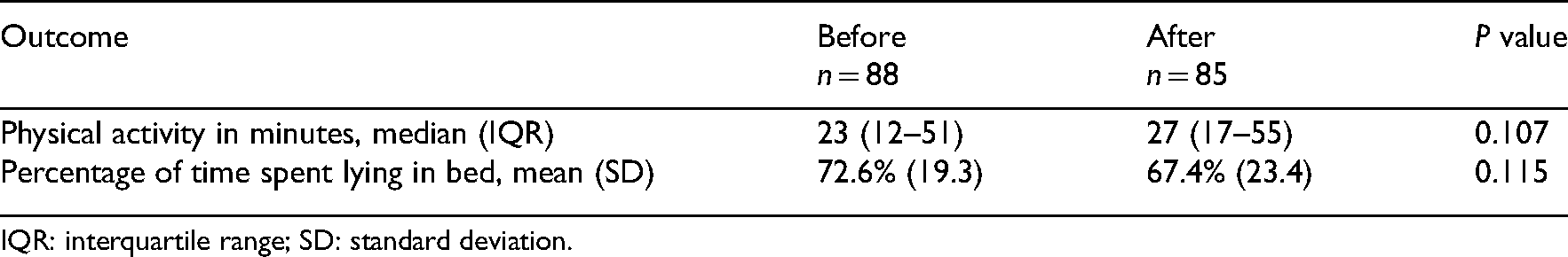
| Outcome | Before | After | |
|---|---|---|---|
| Physical activity in minutes, median (IQR) | 23 (12–51) | 27 (17–55) | 0.107 |
| Percentage of time spent lying in bed, mean (SD) | 72.6% (19.3) | 67.4% (23.4) | 0.115 |
IQR: interquartile range; SD: standard deviation.
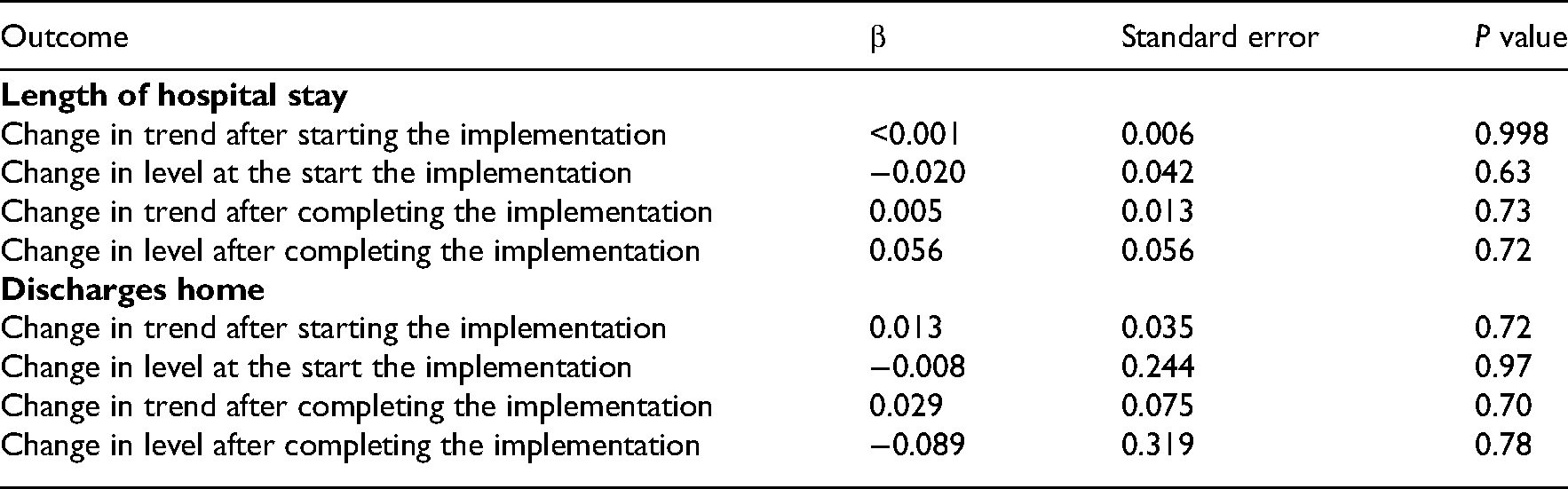
Trend and level changes over time in length of hospital stay and proportion of patients discharged home.
| Outcome | β | Standard error | |
|---|---|---|---|
|
|
|||
| Change in trend after starting the implementation | <0.001 | 0.006 | 0.998 |
| Change in level at the start the implementation | −0.020 | 0.042 | 0.63 |
| Change in trend after completing the implementation | 0.005 | 0.013 | 0.73 |
| Change in level after completing the implementation | 0.056 | 0.056 | 0.72 |
|
|
|||
| Change in trend after starting the implementation | 0.013 | 0.035 | 0.72 |
| Change in level at the start the implementation | −0.008 | 0.244 | 0.97 |
| Change in trend after completing the implementation | 0.029 | 0.075 | 0.70 |
| Change in level after completing the implementation | −0.089 | 0.319 | 0.78 |
