Abstract

Keywords
Introduction
The swollen lower limb is a common presentation that all clinicians, be they vascular specialists or otherwise, will encounter in their routine clinical practice. Defined as a volumetric increase in the lower limb due to an increase in interstitial fluid volume, oedema stems from a variety of both systemic and localised causes. Systemic causes should be suspected especially if bilateral swelling is present, while localised, vascular causes of swelling usually affect a single limb.
In the assessment and management of patients presenting with a swollen lower limb, a thorough medical history and physical examination is required to determine the likely cause. This will allow for appropriate referrals to other specialities, undertaking further investigations, and targeted management of the underlying cause. This article seeks to highlight the management recommendations from the International Union of Phlebology (UIP), with an accompanying one-page guideline that includes an algorithm that can be followed to investigate and manage a swollen lower limb that can be used by all clinicians and allied health professionals.
Management recommendations
A selection of systemic causes of swollen lower limbs.

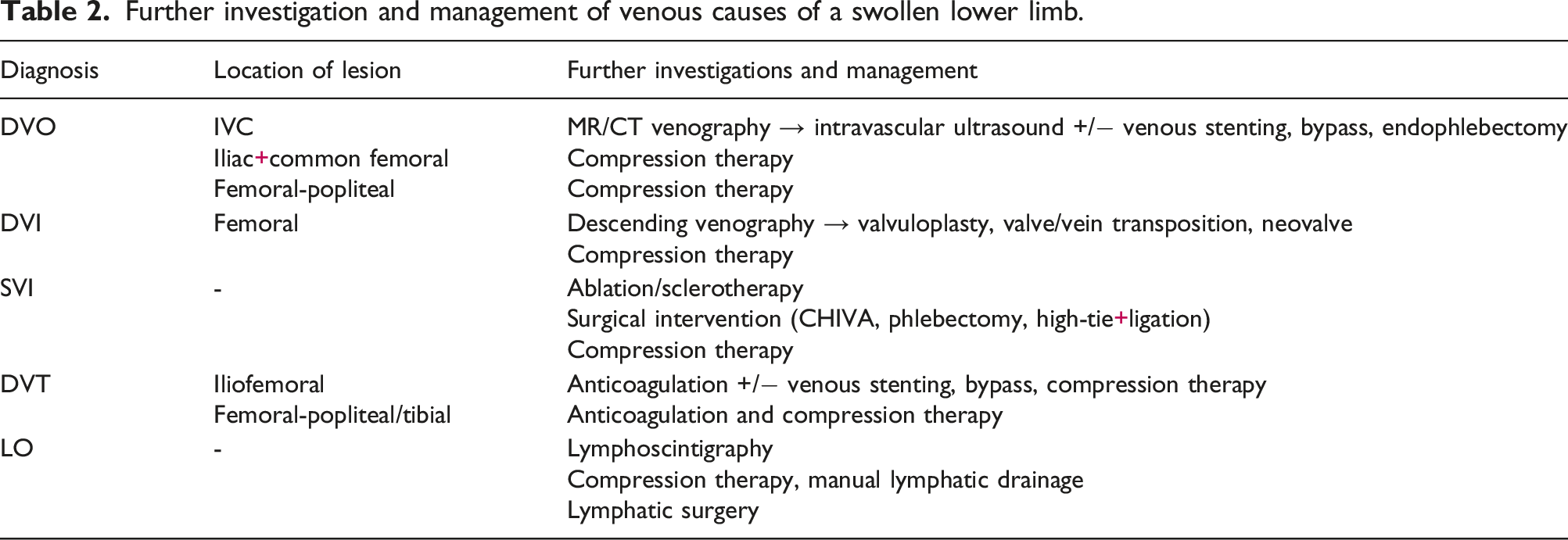
Patients should undergo a duplex ultrasound of the lower limbs to elucidate any venous causes for lower limb swelling. These include deep venous obstruction (DVO), deep venous insufficiency (DVI), superficial venous insufficiency (SVI), or deep venous thrombosis (DVT). If the duplex ultrasound is normal, clinicians should consider further imaging modalities such as computed tomography (CT), magnetic resonance arterial imaging, and trans-abdominal ultrasound (TAUS) of the abdomen and pelvis to rule out intra-abdominal/pelvic compression. If lymphoedema (LO) is suspected, clinicians may consider performing lymphoscintigraphy. 3
Further investigation and management of venous causes of a swollen lower limb.
Discussion
This article provides a one-page clinical practice guideline summarising the clinical management of patients presenting with a swollen lower limb. It is part of a series of publications for the UIP One-Page Guidelines which are aimed at ensuring that patients with venous disease receive timely and appropriate care based on current best evidence and expert consensus (Figure 1). The one-page guideline.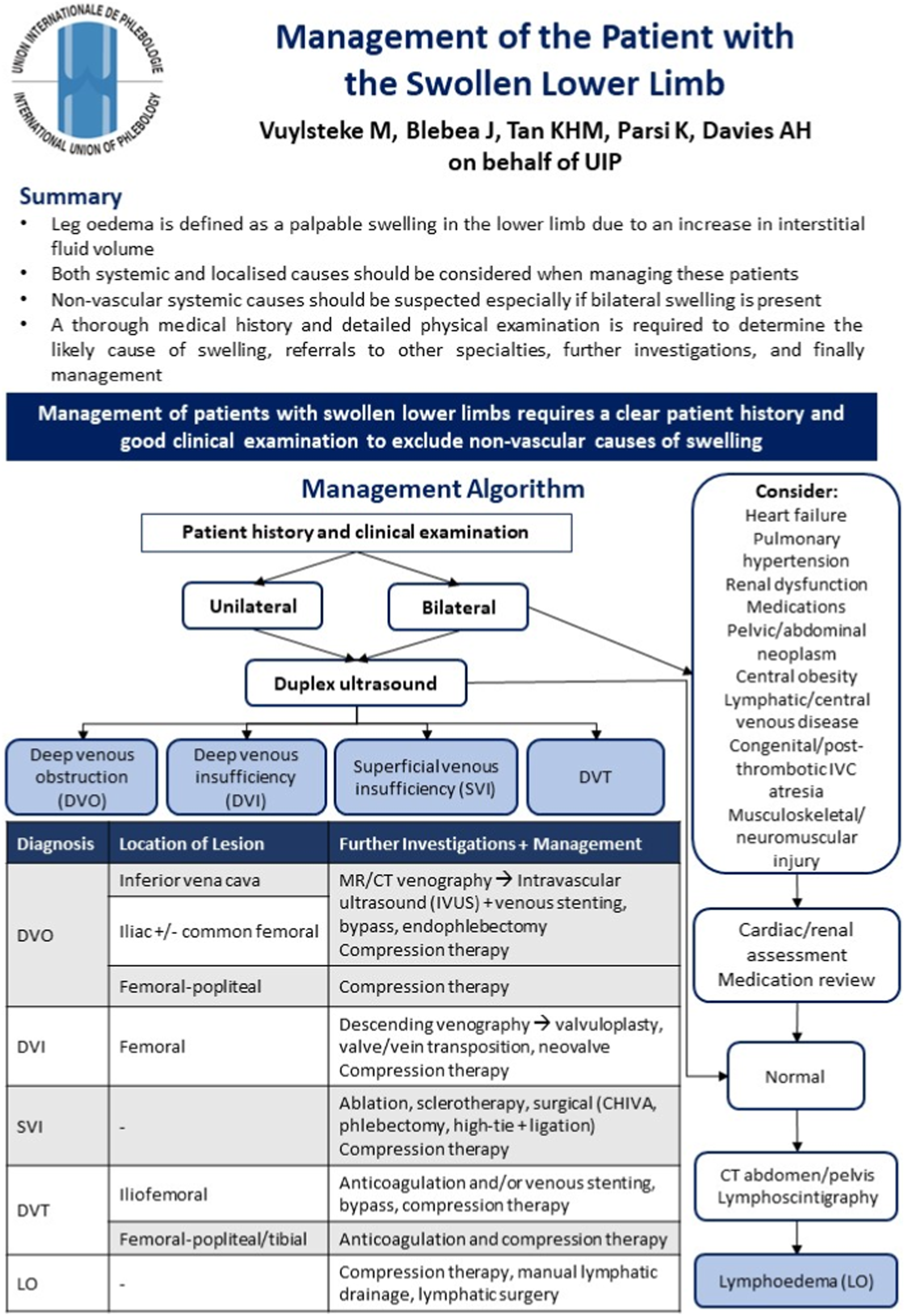
Oedema, of one or both lower limbs, is a common problem and can represent up to half the referrals to any vascular practice. 2 When facing such a presentation, vascular specialists should be reminded not to restrict their assessment to the vascular system but instead maintain a wide differential diagnosis until medical history and examination findings narrow this down. Often, the diagnosis for patients’ oedema can be identified from these findings, for example, a patient with heart failure will also report other symptoms such as breathlessness on exertion or on lying flat. However, if there is any persisting uncertainty, the differential can be further refined by targeted investigations to include or exclude diagnoses. If a venous or lymphatic cause is identified, further investigations should be performed and treatments initiated according to evidence-based practice guidelines, for example, the other publications in this series of UIP One-Page Guidelines.
Footnotes
Author contributions
K.P. and A.H.D. conceptualised the design of the short report and one-page guideline. M.V. and J.B. contributed to the literature review and formulation of the recommendations. M.T. contributed to the formatting and layout of the one-page guideline (![]() ) and wrote the initial draft of the short report. All authors reviewed the short report prior to submission.
) and wrote the initial draft of the short report. All authors reviewed the short report prior to submission.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Guarantor
Professor Alun Davies on behalf of the UIP.
