Abstract
The possibility to use mobile phones to provide affordable, effective and accessible healthcare solutions has continued to attract significant investments in the application of formal m-health schemes in Africa. However, while the formal m-health schemes in Africa are limited and benefited only a handful of people, a majority of individuals are using their own phones to create an informal m-health ecosystem in an attempt to bridge primary healthcare access gaps. This paper draws on qualitative data from a four-year (2012-2016) anthropological study involving marginalised groups in Sierra Leone to document these health-seeking practices along with the benefits and challenges they create in a complex plural health system. It argues that the informal integration of mobile phones into the plural health system offers opportunities for marginalised individuals to search and secure primary healthcare of their choices, but poor network connectivity, high out of pocket maintenance costs, low digital literacy skills, and the lack of policy to streamline and regulate the practices can promise the effectiveness of the informal m-health system. It concludes by offering suggestions for addressing these challenges in the Sierra Leone context.
Keywords
Introduction
Mobile health solutions in Africa
This study draws on patients and caregivers’ experiences to explore and understand how the informal use of mobile phones in a plural health system shapes and reinforces health seeking behaviours and practices to reduce the access gap in Africa. In the last decade, Africa has continued to experience a phenomenal growth in mobile infrastructures and penetration rates. Current data shows that over 80% of the African populations are now connected to mobile networks (International Telecommunication Union (ITU), 2019). This indicates that the advancement in mobile infrastructural development in Africa far exceeds roads and water, as many rural households now have access to mobile phone services but not pipe borne water (World Bank, 2017).
Research shows that not only are mobile phones increasingly becoming part of ordinary people’s daily communication rituals in Africa, but are believed to also provide effective routes for primary health solutions (known as m-health) in marginalised and unserved rural and urban communities (Bervell and Al-Samarrie, 2019; Opoku et al., 2017). The possibility to use mobile phones to provide affordable, effective and accessible healthcare solutions has continued to attract significant interest in the implementation of m-health schemes in Africa (Daniels, 2014; Hackett et al., 2018; Opoku et al., 2017). A recent systematic review indicates that m-health schemes have been implemented in Africa to support health communication and information dissemination, adhere to treatment prescription routines, facilitate diagnostic care and disease control, as well as promote decision-making on patients’ care services and referrals (Bervell and Al-Samarrie, 2019). M-health interventions are also being used for mobile telemedicine, surveillance, patient record management, information decision support systems and patient monitoring in hospitals and clinics across Africa (Daniels, 2014; Lahti et al., 2020; Hamine et al., 2015; Ngongo et al., 2019). However, while a majority of m-health schemes have the potential to improve health outcomes and processes of care in Africa, the adoption of m-health applications remains limited in scope and coverage (Chib et al., 2015; Mehl and Labrique, 2014). Many m-health schemes in Africa are small scale pilot projects and hardly go beyond the pilot phase (Hampshire et al., 2016; Leon et al., 2012); thus, contributing to high failure of m-health projects to reach a wider African population (Kay et al, 2011; Tomlinson et al., 2013; Watkins et al., 2018).
It has been reported that in the absence of formal m-health schemes in many parts of Africa, people are using their mobile phones informally and creatively to seek healthcare (Hampshire et al., 2015). A number of studies have begun to explore this informal use of mobile phones in biomedical practices, focusing on a set of actions, behaviours and consequences that shape and reinforce the everyday decisions of patients and health workers (Hampshire and Owusu, 2013; Opoku et al., 2017; Watkins, et al., 2018). For instance, a study by Hampshire et al. (2015) reported the consequences of informal mobile phone use by young people to call for clinical help, obtain health-related advice or information, and meet healthcare expenses in Ghana, Malawi and South Africa. Watkins et al. (2018) discussed the patients and health workers’ practices to enhance primary health care, while Chib et al. (2015) articulated the policy dimension of m-health interventions. In all, existing studies focused mainly on the integration of informal mobile phone use into formal biomedical practices to mediate and close primary healthcare gaps in Africa. There is limited evidence on how patients and caregivers use mobile phones informally to enhance primary healthcare from multiple traditional and biomedical providers within a pluralistic healthcare system – a system that forms the genesis of the health therapeutic landscape in most African countries and Sierra Leone (Hampshire and Owusu, 2013; Leach, 2008; Lau et al., 2013; Scott et al., 2014). The present study contributes to filling this gap. It reports on the effective use of mobile phones informally by marginalised individuals 1 to negotiate and seek healthcare in a complex plural health system in Sierra Leone.
Plural health system refers to the coexistence of traditional and biomedical practices as separate but complementary elements, to provide a set of alternatives to meet primary healthcare needs of many people in Africa (Amazat and Razum, 2014; Diaz and George, 2014; James et al., 2018; Hampshire and Owusu, 2013). Biomedical practices involve a set of modern medicine treatments organised through formal government and private healthcare services (Amazat and Razum, 2014; James et al., 2018). Traditional practices on the other hand refer to a combination of indigenous knowledge, skills and experiences of traditional healers divided into herbalists, spiritualists and ritualists, and the use of herbal medicines in treating diseases (Amazat and Razum, 2014; Shim, 2018). In Sierra Leone, research shows that a significant number of people rely on herbal medicines, traditional treatments and traditional practitioners to access primary healthcare alongside the conventional biomedical treatments (Bakshi et al., 2013; Oyerinde et al., 2012; Lau et al., 2013). When a person becomes sick, he/she navigates the multiple healthcare options in the plural health system to seek care (Scott et al., 2014). Often, the decision to seek care from a particular provider rests on factors such as health resource availability, cultural norms, perceived effectiveness, as well as the power relations embedded in the family, household and social relationships (Bakshi et al., 2013; Fleming et al., 2016).
The health-seeking practices in the plural health system involve health workers and patients-centred communication and information sharing that may be mediated by the mobile phone, given the prevalence of the technology in Sierra Leone (Lau et al., 2016). However, very limited evidence exists thus far. The aim of this paper is to assess in-depth the patients and caregivers’ experiences of using mobile phones informally to inform the decision-making processes at all levels of health-seeking practices within the plural health system in the rural and urban regions in Sierra Leone. It responds to the following research questions: How and to what extent informal mobile phone use provides a new level of connectivity between individuals and between the patient population and the modern and traditional healthcare providers, and what are the consequences to enhance the delivery of primary healthcare for the marginalised? The paper starts by outlining the composition of the Sierra Leone plural health system and linking it to the informal use of mobile phones. It then describes the methods and analyses the results. It concludes by discussing the results and highlighting key health-seeking practices mediated by mobile phones and their potential health benefits and challenges along with possible solutions.
Composition of the plural health system
Although the plural health system has existed for many years in Sierra Leone, the emergence of its popularity in the country has roots in the decade-long conflict that ended in 2002. During the conflict the already limited health infrastructure was almost destroyed; many government health clinics were completely demolished; and many health professionals relocated elsewhere for greener pastures, leaving a large number of the population, particularly in the rural areas, without reliable formal healthcare services (Wurie et al., 2016). In essence, the cumulative effect of healthcare challenges aggravated by the conflict created an avenue for families and individuals living in the marginalised and unserved regions to explore alternative sources for care services (Mallet, 2014; Scott et al., 2014). This included seeking care from a wide range of available traditional and biomedical service providers, such as community health workers, traditional birth attendants, local drug peddlers, community health centres and traditional healers.
Efforts to address healthcare challenges in the post-conflict development of Sierra Leone have been frustrated by a disease burden related to malaria, diarrhoea, HIV/Aids, TB, and more recently the Ebola epidemic that claimed thousands of lives. In additional to the disease burden, the infrastructure and human capital needed to response and address the health challenges are also in short supply, resulting in an inequitable distribution of effective healthcare services in most parts of the country particularly in the rural areas (Wurie et al., 2016). Studies report that the cumulative challenges and constraints in health care system in Sierra Leone have continued to shape and reinforce the plural health system in the post war era (Fleming et al., 2016; Yansaneh et al., 2014; Scott et al., 2014). This is reflected in practice and national healthcare arrangements, given that most traditional channels are now recognised by the Sierra Leone government along with the biomedical practices as part of an integrated system of national health care.
Plural healthcare and mobile phones in Sierra Leone
Research into the plural health system in Sierra Leone shows that the care seeking practices are flexible and pragmatic and often based on a range of factors linked to people's geographic locations, cultural norms and social and economic status (Fleming et al., 2016; Treacy and Sagbakken, 2015; Scott et al., 2014). Geographic proximity to care providers, together with transport and treatment costs, type of healthcare provision, perceived illness, and perceived friendliness of providers and perceived effectiveness of treatments, characterise and inform health-seeking decisions (Fleming et al., 2016; Scott et al., 2014; Denney and Mallet, 2014). Cultural norms linked to gender, religion and traditional beliefs and practices are also reported to shape health seeking behavioural practices in Sierra Leone (Fleming et al., 2016; Lau et al., 2013). In addition to these factors, the decisions on where and how to seek health care when a person is sick are often made collectively at a house or community level (Scott et al., 2014). These insights are important and add to the understanding of the changing plural medical therapeutic landscape in Africa – from the dominant binary comparison between biomedical and traditional practices for legitimacy to a more fluid set of practices and categories created by caregivers and patients (for detailed discussion see Lambert et al., 2012; Leach et al., 2008; Hampshire et al., 2011).
Relevant to the present study is the informal use of mobile phones to shape and inform health-seeking decisions in the plural health system at an individual and community level, and among networks of family, friends and service providers in Sierra Leone. More broadly, the informal use of mobile phones is emerging as an alternative to formal m-health schemes to disrupt health inequalities in Africa (Hampshire et al., 2016; Watkins et al., 2018). Although not specific to the plural health system, people are ingeniously using their mobile phones in an attempt to secure effective primary healthcare. In South Africa, for example, Watkins et al. (2018) reported that patients and health workers in rural areas are using their mobile phones for a range of healthcare related services, such as reminders to take medications or attend clinic visits, gather health information and recruiting patients with chronic diseases.
It is important to report how such health-seeking practices are facilitated in the Sierra Leone plural health care context through mobile phones. With more than 70% of the Sierra Leone population (about 5.23 million) connected to mobile networks (Thomas, 2018), there is a potential for this technology to inform and transform the actual health-seeking practices of people. In particular, the mobile phones can be used to drive the set of actions, behaviours and norms that inform and reinforce health-seeking decisions of people within the plural health system (Watkins et al, 2018; Head et al., 2013). This includes the practice of how people seek and negotiate care from a wide range of traditional and biomedicine service providers. The focus of this paper is to report findings on these emerging health-seeking practices mediated by the informal use of mobile phones by people in the plural health system.
Methodology
Design – philosophical context
The data presented here come from a large ethnographic study (2012 -2016) in Sierra Leone on mobile phone use and human development. The study design was primarily influenced by Lincoln and Guba’s (1985) conception of Naturalistic Inquiry and Schwandt’s (1998) Interpretive Anthropology. Research findings were literally created as the investigation proceeded (Guba and Lincoln, 1998), and knowledge was gained or created by understanding the context of how the reality of mobile phone use in the everyday world of the marginalised was socially constructed based on individual constructs (Kelly, 1991) and shared (Berger and Luckmann, 1967). Implicitly, the study design built on the understanding that the marginalised people’s construction of reality as individual or group around mobile phone use to articulate their everyday practices coexists in their natural settings. This thinking supports the fundamental epistemic belief that underpins the interpretive anthropology and by extension ethnography (see Mitchell and Charmaz,1998; O’Reilly, 2012; Schwandt, 1998). Thus, the overall ethnographic approach was designed to obtain in-depth insights into marginalised people’s experiences and practices around the everyday use of mobile phones to articulate their livelihoods using participant observation, in-depth interviews and group discussions. Ethical approval was granted from the University of Queensland Ethical Review Committee in Australia.
Research setting
The fieldwork was conducted in two study sites: one rural (Tombo) with little or no basic services and one densely populated urban setting (Wellington) in the western area region with inadequate social services.
Tombo is predominantly a small fishing rural settlement situated in the Western rural district. Residents in Tombo relied on one poorly resourced community health centre for biomedical care and a wide range of informal and traditional providers. Wellington, on the other hand, had a small under resourced government health centre and few private hospitals and clinics, but the prohibitive cost of private healthcare treatment pushed a majority of the poor to seek care from alternative informal sources (healers/medicine sellers). Both research sites had relatively good mobile network connectivity, and were situated within 12 – 43km of the national maternity referral hospital in Sierra Leone – Christian Maternity Hospital.
The choice of Tombo and Wellington settings was critical for interpreting the socially constructed meanings of mobile phone use by individuals who are excluded from the periphery of society. Ethnography deals with individuals in their natural contexts, to understand how they articulate their daily lives, make meaning and construct or reconstruct their world in a way that is relevant to them (O’Reilly, 2012). The description of both sites alluded to this ethnographic principle. Tombo and Wellington offered critical sites to map detailed contexts of mobile phone use in marginal settings; understand how the marginalised negotiate the social and economic challenges of everyday life including health care; and determine the role technology plays as they try to make ends meet.
Selecting research participants
The research participants were marginalised individuals (N = 50) who experienced or were at the verge of experiencing a wide range of socio-cultural economic and political deprivations, including the lack of access to quality education, employment and healthcare services. Participants’ ages ranged predominantly between 18 and 35 years, and 60 percent were male and 40 percent female. A majority (65%) were engaged in some kind of informal income generating activities such as petty trading, bike riding, mobile airtime and accessories street trading, fishing and labourer or menial jobs, etc., while the rest (35%) were unemployed. The participants were recruited through a snowballing approach, as it allows for recruiting acquaintances that experience similar challenges in their social networks. The targeted settings and popular hangouts of the targeted people were visited, existing participants were asked for referrals, and permission was obtained from community informants and organisations that may have dealt with these groups. Each participant read and signed ethical consent forms before participating in the study.
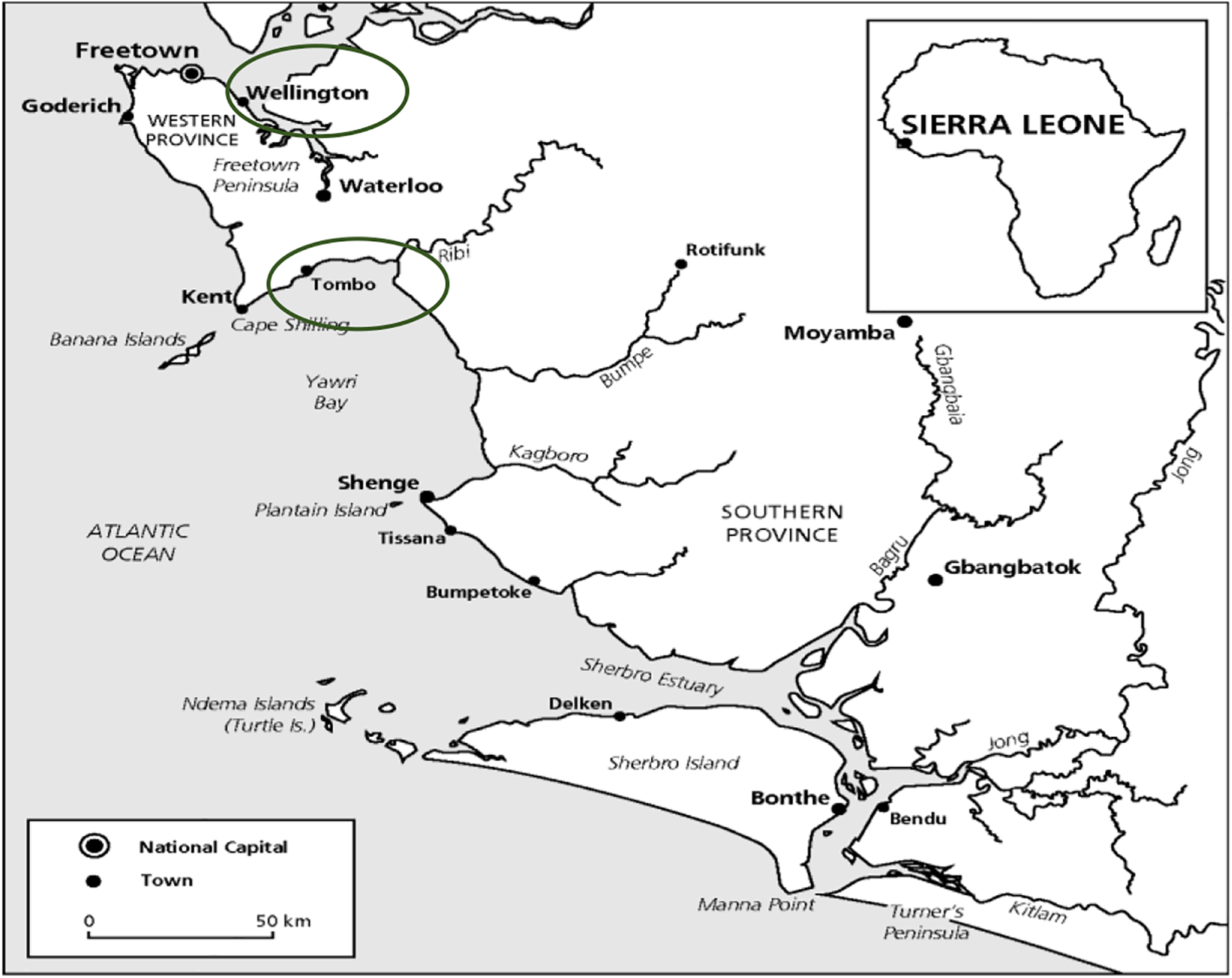
Map of Sierra Leone showing Tombo and Wellington field sites.
2.4 Data collection
As mentioned above, data collection involved participant observation, focus group discussions and in-depth interviews with the research participants in each research setting.
The data collection process was holistic and iterative in nature, and it conformed to typical traditional ethnographic practice (O’Reilly, 2012). Each method was integrated where necessary into the data collection process, which involved moving back and forth between the research questions, data collection and analytical field notes until the needed data were collected to answer all the research questions.
2.4.1 Participant observations
Participant observation was employed to build rapport and engage in informal interactions with the research participants to learn about their everyday lives and behavioural patterns around mobile phone use (O’Reilly, 2012). How and what to observe was dictated by the research objectives, research questions and the theoretical approach adopted to explain the research problems. It was also driven by the events or situations that unfolded at a given point in time during observation. Participant observation was guided by Spradley’s (1980, p.73) three observation techniques: descriptive, focus, and selective observation. The descriptive observation was employed to capture the broader behavioural practices around the mobile phone use, while the focus and selective observations allowed for detailed observation of emerging issues in the data. During the descriptive observation phase, the everyday activities of the participants, major features of the settings, major things that took place, behavioural acts or activities such as the feeling that people had and the goals that they intended to achieve in their everyday routines were all observed, together with I also observed how the participants interacted with each other in their social settings and their experiences in adopting and using mobile phones differently to articulate their everyday routines. Descriptive observation carried out was followed by written field notes and reflection to inform the next two observation phases, which focused on structural and contrasting questions to acquire an in-depth understanding of emerging topics from multiple views of the participants.
Semi-structured Interviews
In each rural and urban setting, semi-structured interviews were conducted with marginalised individuals (N = 50). The interviews were designed to clarify or confirm detailed information obtained from participant observation, and further elicit in-depth information on the mobile phone usage culture and behavioural practices. This included how they use mobile phone informally to seek primary healthcare from multiple traditional and biomedical providers within the plural health system. Participants were carefully recruited based on the sampling techniques described above. Pseudonyms were used to represent the names of all the respondents and also some places and offices to protect privacy, personal information and safety of the research participants.
The interviews were conducted on a rolling basis—some were one off (45 minutes- 120 minutes) and others at an interval of 45– 60 minutes in two or more sessions to exhaust the interview guide. Open questions were asked based on the interview guide, which comprised of a list of topics implicit to the research objectives, questions and conceptual framework. In addition, followed-up questions were asked to clarify emerging thoughts that needed further in-depth enquiry. All interviews were conducted in the local language spoken and understood and also convenient for the participants to express themselves better. Each interview started by either introducing or reintroducing the study; read or gave ethical consent form; agreed on terms and respondents signed ethical form either by writing or using thumb print.
Focus group
The focus group discussion was adopted to engage the marginalised in a structured conversation with each other to define key concepts and learn about their differing experiences, ideas and concepts that exist among them (Barbour, 2011; Roper and Shapira, 2000). It was designed to clarify and gain collective insights into the participants’ knowledge, perceptions, beliefs and practices regarding the use of mobile telephony to articulate their everyday practices, including health-seeking behavioural practices. Five focused group discussions were conducted, each comprising 3-8 participants (Barbour, 2011; Boeren, 1992). The composition of the group was homogeneous; it reflected diversity built on shared characteristics in terms of background, belief, values and knowledge of group members (Barbour, 2011). The discussions were flexible and incorporated innovative approaches, such as seminar-like sessions and communication tree activities, to encourage free and open discussions and elicit important data.
Data analysis
During fieldwork, the focus group discussions and interviews were audio-recorded and transcribed into English and shared with the participants to seek their validation (Guba and Lincoln, 1998). The transcripts and observation documents were analysed following the guidelines of thematic analysis (Braun and Clarke, 2006; Roper and Shapira, 2000). First, the whole data set was read and reread several times to familiarise with it, taking relevant notes on initial ideas. Next, the data were coded iteratively (doing line-by-line coding) to generate themes by moving back and forth between the data set, research questions, research theoretical framework and existing literature around emerging themes (LeCompte and Schensul, 1999). This was to: (i) avoid getting locked into patterns quickly and missing additional understanding from the part not analysed, and (ii) clarify any ambiguities and enrich understanding (Roper and Shapira, 2000)). After the coding was completed, categories of codes were organised into smaller groups that were similar or different by comparing codes to identify patterns and themes. The patterns and themes were closely examined for differences, similarities and recurring relationships that explained the complex picture and nuances of everyday mobile phone usage culture and consequences on the participants’ lives in their social settings. Finally, the resulting themes were collated into five broad coherent themes and sub-themes to represent the data accurately and inform the writing up of the results.
Summary of research themes.
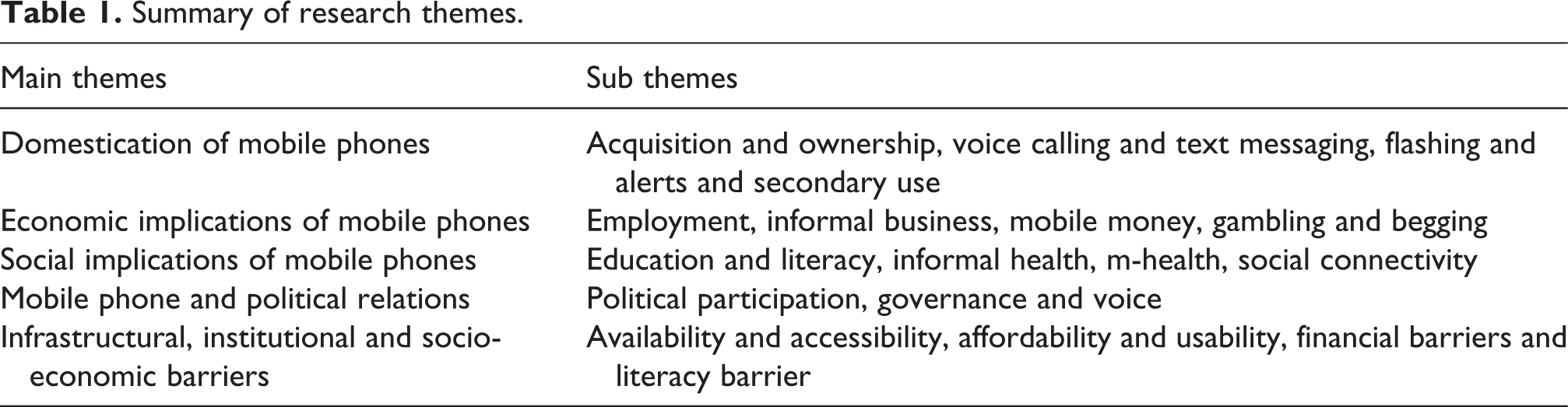

The analysis in this paper draws on the social implication theme, with a specific focus on the informal health usage theme and further five sub-themes (presented in the results analysis) that emerged inductively from the data set to answer the research questions.
Results
Use of mobile phones to search for providers
In both Tombo and Wellington, patients and caregivers were very clear about their mobile phone usage to seek care from multiple providers. With mobile phones, patients and caregivers were able to search and contact healthcare providers to seek advice, make appointments, request support (e.g. advice on drug administration, treatment and side effect), call for help, and sometimes request for referrals. This is narrated in the two quotes: ‘Because we live very far away from the community health centre, any time my children get sick, I will first use my mobile phone to call one nurse that I know very well at the Centre. The nurse would advise me to come to the health centre or prescribe some drugs for me to buy from a local medicine store close to our house’ (Aminata, female, 32, fishmonger). ‘My daughter had an eye infection […] I used my mobile phone to call Pa Kamara (a traditional healer) in the neighbouring village for herbal treatment. Few hours later he called me from his phone to go and collect the medicine. During the treatment of my daughter’s eye, he provided additional instructions on administering the medicinal treatment through this (pointing to her mobile phone)’ (Mary, female, 29, petty trader).
The mode of communication was largely voice calls compared to text messaging. Although the reason for this may be linked to high illiteracy, some participants reported that the voice call is more trustworthy than text messaging, and that it can facilitate instant responses and replicate a typical face-to-face form of oral communication that dominates the communication patterns in most African countries. ‘Anything that has to do with sickness, I don’t think text message work best, because you won’t know if the person receive the message or not. But with the voice call, you talk directly with the doctor or nurse just like face-to-face communication […]. You get immediate reply to decide whether to go to the health centre or ‘medicine man’ (traditional healer) for treatment’ (James, male, 30, top-up seller).
The information obtained from the participants indicates that all mobile phones used were entirely owned and maintained by patients or caregivers. There was no evidence of any m-health schemes for facilitating health care search. Equally, although few people reported to have received calls from health providers, almost all calls related to health care search were initiated and facilitated by patients or caregivers.
The mode of the calls was most time urgent, culminating in either an abrupt or hasty end. According to the participants, the underlining reason for the urgency reflected in calls relates to high maintenance cost, which includes cost for airtime, repairs and recharging phone batteries. When a question was asked to the participants during interviews and group discussions about who bears the cost of mobile phone use for seeking healthcare, responses vary and depend on each person’s position in the households. For most married women and younger generations, the head (often men) of the household bears the financial responsibility for healthcare related mobile phone usages. However, for other participants who did not have such a social protection, buying airtime was reported as a financial burden. In Sierra Leone, where airtime is expensive relative to incomes and living expenses, some participants mentioned instances where the lack of airtime prevented them to make critical calls to healthcare providers for their loved ones ailment.
In addition to the financial burden, the participants were also concerned about network failure. Poor network connectivity was reported as one of the major issues in the Tombo community. This was considered problematic, particularly when they needed to contact health providers during an emergency. One participant recalled an instance when she almost lost her sick daughter because of poor network to contact providers for treatment. ‘It was in the middle of the night when my child got sick. My husband was on a fishing trip. I called him several times for advice but the calls were not going through. I tried calling my mother in the nearby village but it was the same problem. I phoned a nurse living about 20 minutes away from us, the call was still not going through. To safe my child’s life, I had to knock on my neighbour’s door, who assisted me with an Okada (a motorcycle taxi) to take her to the nurse’ (Hawa, 25, female, housewife).
However, in spite of the challenges mentioned, care-seeking behaviours reported in this study revealed that the mobile phone enabled patients and caregivers to search for the healthcare preferences available to them. Almost all participants regarded the act of searching through mobile phones essential for facilitating communication, speeding up instant decision making on appropriate care choices and maximising recovery. This is further explained in the following result sections.
Lowering barriers to access health care
Most participants reported that a range of important access-related barriers preventing them to seek health services from preferred choices. This included vast distance and high travelling costs to public health centres, particularly in rural areas; high search cost for appropriate care; long queues at care centres; cost of service and the inability of the population to financially access service. However, almost all mobile phone uses reported in this study, to some extent, involved lowering these barriers. For example, the participants who have contact numbers of health-workers at existing centres explained instances in which they used their own mobile phones to call and seek advice or assurance first before visiting the centres. According to them, this was instrumental to avoid long queues at the centres or unnecessary travelling costs. As mentioned above both Tombo and Wellington have only one government health centre each. Some participants mentioned that access to these centres was limited due to lack of geographical proximity, particularly for those living in unserved suburbs that require transportation to the centres.
Even in the case of alternative providers such as herbalists, religious healers and pepeh doctas, the distance to desired providers was considered problematic for some participants as well. Although alternative providers are diverse in Sierra Leone, some patients and caregivers are tied to specific providers whom they believed can offer better medicinal treatments, as well as social and emotional support that cannot be easily attained from government health centres (Fleming et al., 2016; Scott et al., 2014). It was reported that some of the preferred traditional health providers are difficult to reach in person due to geographical distance, but with the mobile phones, they were able to communicate and seek advice or treatment support. We grew up knowing Pa Foday Bangura as a good native doctor (Herbalist) who can cure several illnesses […]. Even though he lives far away from us now, we still trust Pa Bangura to provide care for me and my children. For example, when my daughter got sick two months ago, I phoned and explained the sickness symptoms to him. He recommended herbal treatments through the phone. […], so distance is not really a problem to us now because of the mobile phone (Mada, male, 31, handcart driver).
Like this father, some participants mentioned instances where they have witnessed patients being treated through mobile phones without the need to travel to any health providers. Information on treatment methods, medications (including preparing and administering herbal treatments) and worries about side effects were communicated to caregivers or patients’ relatives via mobile phones. It was also claimed that some patients received treatment through mobile phones by religious pastors whom they perceived as having spiritual healing power.
Participants noted that mobile phones were also particularly instrumental in instances where caregivers or patients’ relatives have to search and seek care from preferred providers among a range of traditional and biomedical practices within the plural health system. Traditionally, most participants mentioned that the process involved time and high cost, as caregivers are compelled to ask relatives, friends and neighbours in person or travel with the patient from one provider to another. But with the mobile phone, they are able to accomplish this easily using minimal time and cost.
Another critical use of mobile phones reported by participants was that some caregivers were able to simultaneously negotiate care services and costs to enable them make informed decisions on preferred care choices. In Sierra Leone, where a majority of the population live on under UN/World Bank poverty threshold of $1.25 a day, high out of pocket fees often prohibit access to essential health care services. Despite the introduction of the free health care services for under-five children and insurance, most of the vulnerable population in this study indicated their inability to financially access health services. As a result, they mentioned that the mobile phone provided a useful way for them to first contact and agree on care cost before making any care decision.
Timely and life-saving decision making from patients’ networks
Care-seeking behaviours reported in this study revealed that the decisions on where and how to treat a sick person were rarely made individually. Instead, health-seeking decisions were made collectively by a network of family members, older people, friends and/or neighbours. Depending on the sick person’s gender, social relations or economic status in the household or community, health-seeking decisions were often socially negotiated through face-to-face meetings, informal visits or mobile phones. Such practices are led by male family heads, who often provide the financial resources to support care services (Mallet, 2014). According to most participants, the mobile phone was more preferable to mediate the networking relations because it can leverage instant responses and decisions. ‘Our mother was sick two months ago. I used my mobile phone to call all family members in Freetown and the provinces to agree on where to take her for treatment. The process was quick and fast compare to what we used to do – send a person to deliver the message to relatives and convene a meeting before making decisions’ (Fatima, female,32, trader).
Similarly, some participants expressed that having mobile phones reduced the time required to report illness and receive immediate care-seeking decisions from family members and other supporting actors living at distance.
Furthermore, other participants noted instances where caregivers use mobile phones to coordinate networks of family, friends and neighbours to seek instant decisions during health emergence. The instrumental use of mobile phones in emergencies involved channelling urgent collective decisions on choosing a care provider and organising transport for a sick person. For example, one participant described how the mobile phone aided in organising emergency care for her sick daughter. My daughter had an appendicitis that needed an urgent medical attention. I phoned the father, other relatives, friends and neighbours to seek an urgent advice on the best possible care provider. After hours talking to all these people, I finally decided to seek medical help from the nearby private hospital with financial support from the father and relatives (Mariam, female, 35, Secretary).
Further analysis also revealed a substantial use of mobile phones to collectively organise transport for sick people during emergencies. Most participants mentioned that poor road networks, lack of adequate and effective public transport system, expensive vehicle hiring cost and ineffective ambulance system serve as major barriers during health emergencies in Sierra Leone. Like Hawa’s case mentioned earlier, some participants explained instances where Okadas (motorcycle taxis) or hammocks (makeshift stretchers) were used, especially in the rural and unserved areas, to transport sick relatives to care centres during emergencies. It was reported that organising this set of transport systems, though informal, also involved negotiations between a sick person’s networks or households and the transport providers or individuals through mobile phones.
Arranging informal health care for family members
Results show considerable instances where mobile phones were used to make informal care arrangements for family members by relatives perceived to have high social and economic status. Typically to the Sierra Leone cultural norms, it is common (and to some extent compulsory) for perceived wealthy family members to provide healthcare support to extended relatives. This is largely because a majority do not have a formal social safety net including national healthcare coverage (Kamara, 2008). According to the participants, healthcare support received ranged from paying for simple pain killer medicines, arranging care treatments with local care providers, to covering hospital treatment for serious illnesses for both long-distance and close family members.
Analysis showed an instrumental role of mobile phones in the organisation and mediation of this family-led healthcare support system in Sierra Leone. Some participants reported using mobile phones to facilitate quick and effective ways to organise a timely and life-saving healthcare treatment for families and friends. James, an NGO employee in Wellington, provided an example of how he used the mobile phone to negotiate and prearrange informal healthcare service with local medical personnel and drug peddlers (Pepeh Doctas) for his family living with him in Wellington and extended relatives in the provinces. According to him, one of the useful functionalities of the mobile phone was that the technology enabled him to organise and coordinate lifesaving care treatment for relatives and friends from the comfort of his office. I make all healthcare arrangements for my family here and those in the village with my mobile phone. I used it to pay for treatment and buy medicine without the need for me to see them…(James, Male, 46, Project Officer).
For James, and also other participants interacted with in Wellington and Tombo, the perceived easiness the mobile phone creates to arrange care and the reduction in travelling time is life changing in terms of how people in the rural and unserved areas received care and treatment particularly for life threating illnesses.
Risk of seeking care from wrong providers
While a majority of participants expressed optimism regarding the range of possibilities offered by mobile phone phones to expand and increase healthcare access, some participants were also concerned about the risks associated with the use of the technology in the plural health system. Results revealed that mobile phone use within the plural health system increased people’s vulnerability to seek care from the wrong providers for certain illnesses, especially during health emergencies or infectious disease outbreaks. It was reported that during health emergencies, some patients or caregivers contact providers that they can easily access with their mobile phones, irrespective of whether such providers have the required training or skills. A particular reference was repeatedly made to the Ebola outbreak that claimed about 3,955 lives in Sierra Leone in 2014 (World Health Organisation (WHO), 2016). Participants claimed that during the early phase of the Ebola outbreak, many local residents used mobile phones to easily contact informal healthcare channels than the government-controlled treatment centres. Others mentioned instances where the mobile phone was used by patients or caregivers to reach out to traditional healers, such as herbalists or religious leaders, as the first point of contacts for advice or treatment.
Although other factors, such as costs and perceived effectiveness, etc., may inform this type of health seeking behaviours, some participants also believed that the presence of the mobile phone is reinforcing health-seeking behavioural practices. When a question was asked on what the participants think about the impact of this health-seeking behaviour on patients, mixed responses were received. A number of them believed that having a mobile phone can enable one to contact and receive immediate responses from the health providers they can easily access or at least have their numbers. Others acknowledged that seeking care from random providers who may not have the appropriate knowledge of the illness is likely to subject patients to risk. This is because the patients may not receive the appropriate diagnoses or treatments in time. According to them, this may also involve waste of time and money because the caregivers or patients may look for another provider. As one of the participants explained: ‘I remembered when my wife got sick two years ago, I phoned my pastor whom we believed to have a spiritual healing power […]. We prayed for several days with him and use the anointing oil provided but my wife situation got worst. I was advised by my uncle to call a native doctor in the nearby suburb. I did and he provided some herbal medicines, but wife health still did not improve […]. After wasting time and money on all other accessible treatment sources nearby and did not see any improvement, my neighbour’s friend who came to visit him advised me to take her to Connaught Hospital in Freetown. He gave me a phone number of a nurse at the hospital. I called and arranged for my wife to be transfer to the hospital, where she eventually received treatment and recovered’ (Abu, male, 35, petty trader).
Abu’s story suggests that having a mobile phone is not a sufficient condition to access immediate healthcare treatments. Patients and caregivers should have an awareness of appropriate care providers for certain illness types.
Similar consequences were also notable in treatments conducted through mobile phones. While most acknowledged the convenience and cost effectiveness of this approach, a few noted that patients are likely to face the risk of receiving improper care because treatments are prescribed without the providers’ adequate knowledge of the patients’ illness status. Furthermore, in cases where advice was sought through mobile phones on administering drugs, especially herbal medicines, some participants confirmed the difficulty to determine the exact dosage and patient health progress without the presence of a provider.
Discussion
The results of this study suggest that introducing the mobile phone into the multiplicity of healthcare providers appears to be very instrumental to expand and augment the capability of the unserved population to search, negotiate and seek care of their choice. Health seeking behaviours in the Sierra Leone plural health system are multi-faceted, complex and culturally laden (Treacy and Sagbakken, 2015; Yansaneh et al., 2014). Strategies to seek health care for patients are dynamic and involved an ongoing consultation, problem solving and decision making among multiple actors at household or community level (Lau et al., 2013; Scott et al., 2014). For instance, health-seeking decisions for a patient needing treatment outside the home involve where and how to treat the patient; sourcing and allocating financial resources and support systems (e.g. organising transport, carrying the sick person and manning household tasks) for the patient; and taking the patient to a healer or clinic (Scott et al., 2014). Research reports that these practices are traditionally slow, time consuming and risky for patients requiring emergency or critical treatment due to the difficulty to make instant individual and collective decisions for care (Fleming et al., 2016; Treacy and Sagbakken, 2015). However, findings from this study show that the mobile phone is emerging as a strategic tool for the marginalised to ease communication and expedite timely and life-saving decision making and care. Most participants used the mobile phone to reduce healthcare traveling and search time and replicate face-to-face meeting, which traditionally dominates health-seeking decision making processes in Sierra Leone (Scott et al., 2014). Explicitly, the use of the mobile phone in this respect suggests the extent to which the technology can expand people’s capability and the freedom to make collective, timely decisions to seek primary health healthcare of their choice. This is important for responding to emergency or critical illnesses in Sierra Leone, where health-seeking decisions are shaped by cultural norms, social networks and the power relations embedded in the households or communities.
Additionally, results suggest that the trust embodied in mobile phones to facilitate a two-way communication process and generate instant response increases the likelihood of informal health-seeking behaviours and practices. Sierra Leone, like many sub-Saharan African countries, relies overwhelmingly on oral rather than written communication, particularly in the rural settings. Oral communications go beyond mere exchange of messages or information to provide space for maintaining and strengthening traditional social networks in the Africa (Slater and Kwami, 2005). In this context, the channels through which the message is conveyed hold great importance in the communication process. And such channels have to be genuine and trustworthy and cater for an opportunity for face-to-face communication and immediate feedback mechanisms (Obijiofor, 1998). It is against this understanding that the mobile phone is assumed to facilitate a reliable and trustworthy informal health-seeking communication process in Sierra Leone. This finding differs significantly from other studies where health-seeking behaviours and practices in the plural health system were dictated by the trust patients and caregivers placed in healthcare providers and care services (Haenssgen and Ariana, 2017, Oyerinde et al., 2013, Scott et al., 2014). Here, the trust is embodied in the communication channel facilitated by mobile phones.
Findings further indicates that in the absence of formal m-health schemes at the time of this study in Wellington and Tombo, patients and caregivers ingeniously used their own mobile phones to augment primary healthcare within their capability. A systematic review by Bervell and Al-Samarrie (2019) showed that most m-health initiatives identified the mobile phone as a tool to mediate between patients and care providers. However, my study reveals that the mobile phone can also be seen as a self-created individualised virtual clinic for most people living outside the coverage of area of actual physical healthcare structures such as hospitals or clinics (Hampshire et al., 2011). In addition to seeking health information and advice, most participants rely on this virtual mobile phone health clinic for drug administration and treatment, specific diagnosis, making appointments and calling for help during emergence. In consistent with Watkins et al., (2018) and Hampshire et al., (2016), patients and caregivers’ use of mobile phone reinforces and shape local healthcare delivery and management in unserved communities in Sierra Leone.
The study also highlights that although the primary healthcare landscape in Sierra Leone is diverse in terms of multiplicity of formal and informal providers, it continues to presents significant challenges and barriers for a majority of the poor and marginalised individuals. Limited human resource and health infrastructure and prohibitive cost for people accessing primary healthcare, coupled with the lack of universal healthcare coverage and health financing, are indicative of barriers preventing health care access (Moshabela, 2012; Oyerinde et al., 2013, Scott et al., 2014). While the informal use of mobile phone cannot address all challenges, there are signs to suggest that the technology can make a significant contribution to lower some of these barriers and speed up care delivery. For example, health-seeking contacts and treatments conducted via mobile phones were reported to save time and travelling costs to preferred care providers; increased the possibility of taking timely medication for critical illnesses; and enabled patients and caregivers to compare and seek care within their financial means. These findings corroborate existing research such as Bervell and Al-Samarraie, (2019), Cilliers et al, (2018), and Noordam et al. (2011), where mobile phones are reportedly used to increase health care access, promote information for treatment, and serve as an effective tool for reminders towards adherence.
A related finding demonstrated the socio-cultural relevance of mobile phone use to mediate and reinforce traditional forms of healthcare coverage and financing for family or friends in Sierra Leone. This included the use of mobile phones by perceived wealthy individuals to organise informal care arrangements with providers for people who do not have any source for healthcare coverage or financing. The practices are inherent in the notion of ‘Ubuntu’ — that is, collective caring and sharing culture entrenched in most African societies (Nyamnjoh, 2004). In Sierra Leone, the socio-cultural practice embodies looking after one’s relatives, family members or friends by providing welfare and economic assistance, household and livelihood resources, as well as health care support (Kamara, 2008). This practice is not only common, but it is also perceived as an obligation for certain family kinships. Demonstrated in this study is that the integration of mobile phones into the healthcare domain of this cultural practice adds to the cultural repertoires (as discussed in Lau et al., 2013; Scott et al., 2014; Treacy and Sagbakken, 2015) that shape health-seeking behaviours and practices in Sierra Leone among marginalised individuals.
Finally, while it is clear that mobile phones are becoming increasingly important in shaping the local health care delivery, the findings also agree with Hampshire et al., (2016) that the informal use of the technology in the plural health system comes with serious risks for patients. The research data suggest that perceived ease of mobile phone use to simultaneously seek healthcare from multiple biomedical and traditional providers at random meant that patients are at risk of duplicating care treatment, misdiagnoses, incorrect medication, false consultation from unqualified practitioners and questionable mobile phone treatment and care advices (Wardle and Adams, 2014). For example, the participants expressed instances where misdiagnoses and advices received through mobile phones result in economic risks and health complications for patients. Particularly worrying for the participants were the waste of already limited financial resources on unproductive care and the unregulated treatment provided by healers for serious illnesses like TB and HIV/AIDS, as well as critical care related to pregnancy, delivery and child care. While this alludes to similar findings demonstrated in Hampshire et al.’s (2015) study in Ghana, Malawi and South Africa, the risks add potential uncertainty to the use of mobile phone informally for primary healthcare and opportunity for control and regulation.
Conclusion and Implication
This paper contributes to emerging bodies of research on the informal use of mobile phones to improve healthcare access in a medical pluralism system in Africa. It focuses specifically on patients and caregivers’ experiences in rural and urban settings in Sierra Leone. The overall research result offers important insights into the potential and capability of informal m-health to reduce access gaps and cushion some of the challenges and barriers confronting the poor and marginalised people to access primary healthcare in remote rural and unserved communities. It also highlights an important indication of mobile phone usefulness for integrating the informal health sector into the formal healthcare system to improve healthcare access and delivery without comprising quality.
In general, while the study contributes to academic literature, it has a number of implications for policy and practice in Sierra Leone. First, the study contributes to the understanding of the complexity embedded in the informal health seeking behaviours and practices mediated through mobile phones by marginal groups, and generates the most needed data for policy and practice. Sierra Leone, like many countries in sub-Saharan Africa, needs a comprehensive health information management system to augment the limited health infrastructure and improve primary healthcare access for the poor and marginalised. Learning from the informal use of mobile phone is critical for mitigating these challenges in ways that reflect the actual therapeutic and health-seeking practices of patients and caregivers. This may involve developing, streamlining and regulating a standard mobile-enabled ecosystem (m-health) that bridges the biomedical and traditional healthcare services. Such a system should be comprehensive and focus on providing high quality and easily accessible care at lower costs for all.
Second, the study data suggest an increase in the use of mobile phones as a new frontier to reinforce and strengthen familiar health support schemes, as an alternative for healthcare coverage. National health financing is very limited and only a handful of citizens can afford private health insurance in Sierra Leone. Equally, most individuals who rely on family or friends for healthcare support live in rural or impoverished urban settings with limited healthcare access. Having a mobile phone to channel health financing and coordinate care meant that a majority of the marginalised can receive from basic to urgent life-changing medical treatments. This is important because it can pave a way for understanding and facilitating policy and practical interventions in citizen-led insurance scheme and mobile phone health financing scheme for the marginalised.
Third, the analysis of the research data shows that improved access and effective use of mobile phones requires basic digital literacy skill sets, quality network coverage and financial resources to acquire and maintain the technology. Over the course of the study, high maintenance cost and poor mobile network impacted on people’s health-seeking practices. Government should adopt a proactive approach to invest in technology infrastructure and promote an ‘absolute use’ – that is, a simultaneous process of developing digital skill sets, facilitating access and linking the technology use to high quality healthcare delivery.
Finally, while the study reported the benefits of informal mobile phone use to facilitate healthcare, it also demonstrated several risks. Current policy interventions in Sierra Leone make very little provision for the traditional healthcare sector. How and what medicines and treatments are delivered by traditional care providers are often not scrutinised or regulated (Scott et al., 2014). Equally, lapses also exist in the biomedical sector particularly in the pharmaceutical sector. Illegal treatments, as well as sales of prescription and counterfeit or sub-standard drugs, are common among citizens with no medical qualifications or permission from the state (Pieterse and Lodge, 2015). Collectively, what this study has revealed is that these challenges can be seen to pose significant health threats for people who reply on the informal use of mobile phones to seek primary health care within the plural health system. Therefore, as the informal phone health-seeking practices multiply, so does the need for the government to mitigate these risks through robust policy, regulatory and public education interventions.
All in all, research into the informal mobile phone use by the people and marginalised to mediate healthcare access and delivery in Africa is emerging in the m-health field that has been dominated by a lot of studies and application of former m-health applications and initiatives (e.g. Bervell and Al-Samarrie; Opoku et al., 2017). While this study provides an essential insight into patients and caregivers’ experiences in Sierra Leone, it is subject to a potential limitation relating to a comprehensive health system research. The data analysis is based on the subjective and contextual interpretation of the participants’ experiences and knowledge of using their own mobile phones to search and seek care within the plural health system in a rural and urban setting. It excludes data from health workers’ experiences and policymakers. To provide a comprehensive understanding of the operationalisation of the informal m-health ecosystem in the Sierra Leone context, a more rigorous health system study involving biomedical and traditional health workers and policymakers could be of significant benefit in the future.
