Abstract
Background:
Amphetamine-type stimulant (ATS) use is a major public health concern among men who have sex with men (MSM) and transgender women (TGW) in communities worldwide and in Vietnam.
Methods:
A cross-sectional study was conducted on 1000 adult MSM and TGW from 9 community-based organizations in southern Vietnam from March to August 2019. Data on demographics, sexual behaviors, STIs, HIV infection, and substance use were collected with a self-administered questionnaire including the ASSIST tool. Blood and urine samples were collected for HIV and ATS testing.
Results:
The prevalence of lifetime ATS use in the previous three months was 50.5% and 49.4%, respectively. Multivariable analyses showed that ATS use was significantly associated with sex with a transactional partner (aOR [29] = 3.06, 95% CI = 2.13–4.39) who engaged in sex and got paid for it (aOR = 2.78, 95% CI = 1.64–4.73), and purchasing sex (aOR = 2.34, 95% CI = 1.06–5.16). The role in sex with a partner with significant association was ‘insertive and receptive equally vs. insertive only’ (aOR = 1.78, 95% CI = 1.14–2.76).
Conclusion:
ATS use is associated with many sexual behaviors that could be associated with an increased risk of HIV transmission among MSM and TGW populations.
The prevalence of lifetime ATS use in the previous three months was high among men who have sex with men (MSM) and transgender women (TGW) ATS use was significantly associated with having sex with a transactional partner, prostitution, purchasing sex, sex positions. ATS use was significantly associated with a lower age of first sexual intercourse and higher odds of STI.Key Messages:
Chemsex refers to the use of psychoactive substances with the express purpose of engaging in sexual activity because of the substances’ enabling effect on sexual pleasure and performance.
Men who have sex with men (MSM) and transgender women (TGW) are recognized as sensitive and high-risk groups for sexually transmitted infections (STIs), especially HIV infection. In 2020, there were 1.5 million new HIV infections worldwide. The risk of HIV transmission was 25 times higher among MSM and 34 times higher among the TGW. 1 In Vietnam, the percentage of MSM living with HIV in 2020 was approximately 12.3 %. 1
The rate of substance use among transsexuals is 2.5 to 4 times higher than that of non-transgender people. 2 In the United States, 69% of transgender women reported having used illegal drugs in the last six months. The most common drugs reported were marijuana (63%), Ketamine (20%), cocaine (16%), and methamphetamine (13%). 3 Among MSM in China, the drug use rate was 77.3%. 4 In Vietnam, daily smoking was reported by 49.1%, alcohol use by 7.8%, ecstasy use by 18.3 %, heroin use by 15.7%, and methamphetamine use by 6.6% of the population. 5 In addition, 7.1% of respondents who had ever used drugs reported using marijuana.
The MSM and TWG groups worldwide are facing many issues that include being unrecognized in law, 6 discrimination,7–9 sexual abuse, 10 violence, 11 depression and suicide,12–14 drug use, 2 increased risk of sexually transmitted diseases, and HIV infection,15–18 In Vietnam, despite the substantial change in the social acceptance of LGBT populations, this population is still suffering various forms of discrimination. 19
The HIV epidemic is heavily weighted against the MSM and TG. One of the factors related to risk behavior that leads to HIV infection in these groups is substance use.2, 20, 21 Substance use has been identified to be associated with other risk factors for transmission of HIV among the MSM and TGW. 22 Hence, addressing substance use using a comprehensive approach that focuses on promotion, prevention, screening, early detection, treatment, harm reduction, recovery, and rehabilitation is an important strategy to reduce the risk of HIV transmission among MSM and TGW.
Amphetamine tire stimulants have been increasingly becoming a major public health concern in Vietnam. The ATS has been identified as one of the common drugs used for recreation purposes as well as abuse among the MSM and TGW in Vietnam. A sixfold increase in several users of ATS was observed in the country in the year 2020 as compared to 2017. 23 The ATS is the preferred choice of new people who use drugs in large cities. The ATS is one of the most common illicit psychoactive substances associated with chemsex. 24
Designing and implementing effective prevention and control programs for ATS use and HIV infections requires sufficient data on the prevalence, the level of use, and the associated factors of ATS use behaviors. However, there are no existing studies to provide this information in Vietnam. To fill in the gap, our study was conducted in southern Vietnam to ascertain ATS use status and its associated factors among MSM and TGW populations.
Methods
Study Site and Study Participants
The authors conducted a cross-sectional study in Ho Chi Minh City and neighboring provinces in southern Vietnam from March to August 2019. Based upon a established sampling scheme, we collaborated with nine community-based organizations (CBO) that were managed by the Centre for Promotion of Quality of Life. Of these, six CBOs were in Ho Chi Minh City and one CBO each in one of the three following provinces: Dong Nai, Binh Duong, Ba Ria-Vung Tau. Participants were recruited via website advertisement, peer referral, short message service, and community outreach.
The inclusion criteria for the current study were: being men who have sex with men (MSM) or transgender women (TGW); aged 18 or older; having lived for at least three months in the place where the CBOs first approached them; and willing to participate in the study and able to provide written informed consent. On a scheduled day, eligible participants had an appointment with CBOs to complete a self-administered questionnaire on a website. The questionnaire included questions on demographics, sexual behaviors, and substance use history. Participants provided blood samples that were used for HIV tests and urine samples that were used for methamphetamine testing. The participants were offered services related to the management of substance use disorders and HIV based on the existing profile of the CBOs. The study protocol was reviewed and approved by the Biomedical Research Ethics Committee at the University of Medicine and Pharmacy at Ho Chi Minh City, Vietnam (Approval number: 292/DHYD-HDDD)
Measurements
Demographic variables included age (in years), sample distribution (MSM or TGW), education (middle school or lower, high school, or college/university), whether living with a male partner, main occupation (office positions, business/services/entertainment, sex worker, and others), and financial status (full financial autonomy, partial autonomy, based purely on family support).
The clinical variables included sexual behaviors and infection status. The sexual behaviors included: have had sexual intercourse (yes vs. no); age of first sexual intercourse (<18 years old vs. 18 years old or above), having sex with regular/transactional partners (yes vs no/ did not share information), prostitution/purchase sex (yes vs no/did not share information), and role in sex with a male partner (only insertive vs. only receptive, mostly insertive, mostly receptive, and insertive and receptive equally). We asked MSM/ TGW about their behaviors in the previous three months. The HIV infection status was labelled as positive or negative based on participant answers during interviews or on laboratory test results, and STI was labelled as positive or negative/have not been tested over the past year based on participant answers during interviews.
The ATS use was recorded via the ASSIST tool and urine test results of those who took a urine test. This tool not only helped to explore the ATS use status but also assessed the use of other substances, including alcohol and tobacco. ASSIST was designed by the World Health Organization (WHO) to screen, follow, and manage patient use of substances, risk behaviors, and related problems. The tool categorizes the use pattern of all substances as low, moderate, and high risk based on the total score for each substance category.
Laboratory testing included HIV tests using a finger-prick, blood-based rapid diagnostic test (Alere Determine™ HIV 1/2 antibody). Methamphetamine testing was done using a rapid urine test (ABON, Biopham Co. Ltd). Urine samples were collected from the participants for testing for the presence of methamphetamine. Positive status for ATS was determined either by screening positive on the ASSIST-based evaluation or testing positive on the urine test.
Data Analysis
The data were analyzed using the STATA software version 13.0. Descriptive and inferential statistics were used for this purpose. Chi-square tests were used to compare ATS use, categorical demographics, and other clinical variables. In bivariate analyses, odds ratios (OR) with a 95% CI were generated using logistic regression. Multivariable logistic regression was carried out using a stepwise backward selection procedure with a cut-off of
Results
Demographics of Participants
A total of 1,000 MSM and TGW were included in the analysis. The mean age of the study participants was 26.4 ± 5.0 years (range 18–65); the majority were MSM (86.5%), and most had full financial autonomy (74.4%; Table 2). Nearly half of the participants had passed higher education institutes, and 49.2% lived with a male partner. Almost half of the participants (56.4%) were working in the category of business, services, or entertainment, and a few (3.5%) identified themselves as sex workers.
Sexual Behaviors and HIV/STI Infections
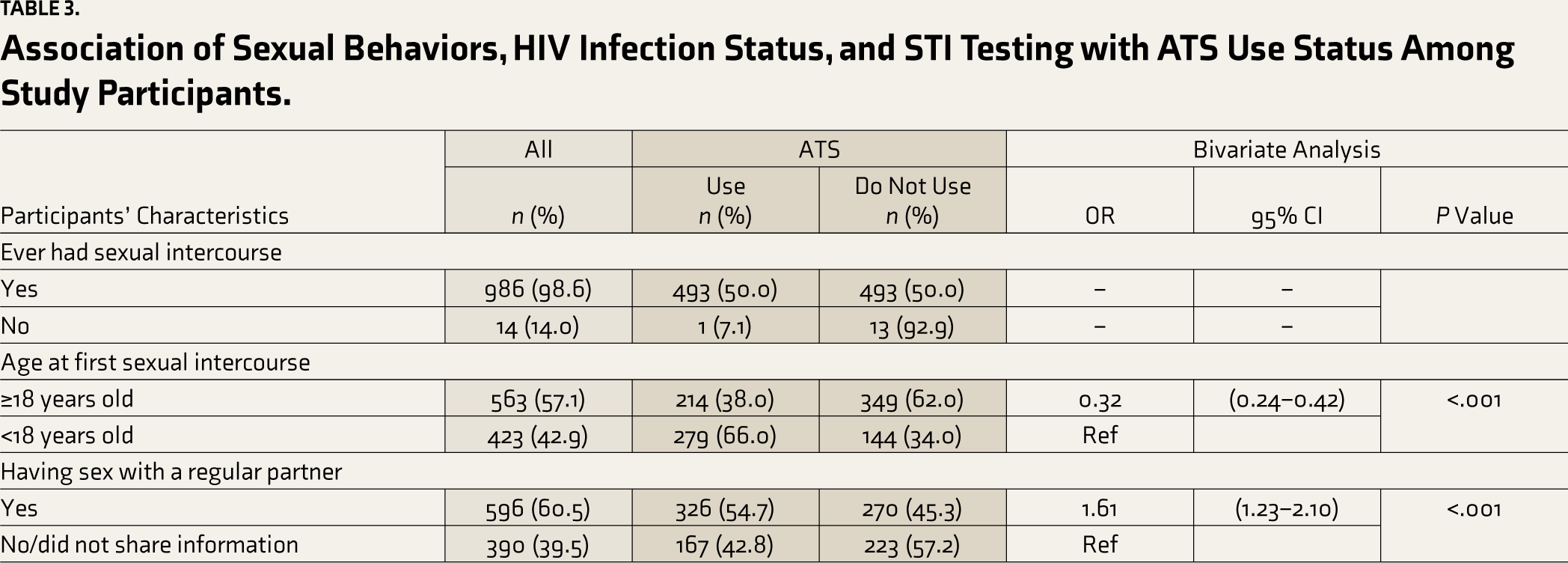
Almost all participants (98.6%) have had sexual intercourse. Less than half of the participants (42.9%) had their first sexual intercourse under the age of 18 years. The percentage of those having sex with regular and transactional partners in the past three months was 60.5% for MSM and 71.6% for TGW. The percentage who engaged in sex work and got paid for it was 13.9%, and the percentage of those purchasing sex was 4.1%. About one quarter each reported only insertive (22.3%), only receptive (24.5%), and insertive and receptive sex equally (26.2%). The order-reported behaviors were mostly insertive (14.0%) and receptive (13.0%; Table 3).
The 79 participants who had been diagnosed with HIV infection prior to the study did not undergo the HIV rapid test. Among the rest, an additional 51 participants had positive results on HIV rapid tests. These individuals were not aware of their HIV status prior to the study. A total of 130 (13.0%) participants had positive HIV serostatus. The prevalence of STI-positive participants was 37.7%. The rest were either not treated or had no history of STI.
ATS and Other Substance Use
The lifetime use prevalence for ATS was 50.5%. Other substance use included alcoholic beverages (82.7%), inhalants (69.0%), tobacco products (47.1%), cannabis (16.9%), hallucinogens (7.9%), sedatives or sleeping pills (6.7%), cocaine (2.3%), and opioids (2.3%; Table 1).
Characteristics of Substance Use, HIV, and STI Infection of the Study Participants.
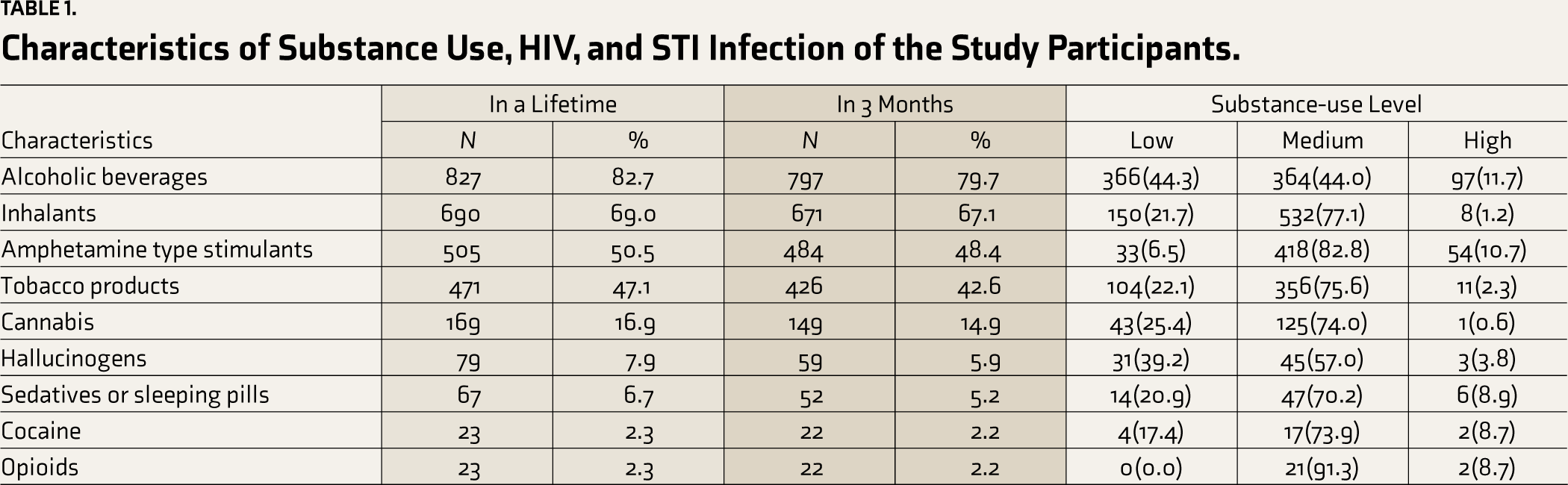
Individual substance use prevalence in the previous three months was almost the same as lifetime use prevalence. The percentages for three months prior were ATS (49.4%), alcoholic beverages (79.7%), inhalants (67.1%), tobacco products (42.6%), cannabis (14.9%), hallucinogens (5.9%), sedatives or sleeping pills (5.2%), cocaine (2.2%), and opioids (2.2%; Table 1).
Moderate and high levels of substance use were most commonly reported. Among the ATS users, 82.8% have a high-risk level associated with the use pattern.
The prevalence of moderate- and high-risk use was 44.0% and 11.7% for alcoholic beverages; 77.1% and 1.2% for inhalants; 82.8% and 10.7% for amphetamine-type stimulants; 75.6% and 2.3% for tobacco products; 74.0% and 0.6% for cannabis; 57.0% and 3.8% for hallucinogens; 70.2% and 8.9% for sedatives or sleeping pills; 73.9% and 8.7% for cocaine; and 91.3% and 8.7% for opioids (Table 1).
Of the 1,000 participants who reported using ATS in the past 3 months, 484 self-reported via the ASSIST tool, and an additional 10 participants had their urine samples tested positive for ATS. Hence, 494 (49.4%) participants used ATS (Table 1).
Association Between ATS Use and Demographics, Sexual Behaviors, and HIV/STI Infections
Results from univariate analyses showed that all demographic characteristics, sexual behavior, and HIV/STI infection variables were associated with ATS use (
Association of Demographics with ATS Use Status Among Study Participants.
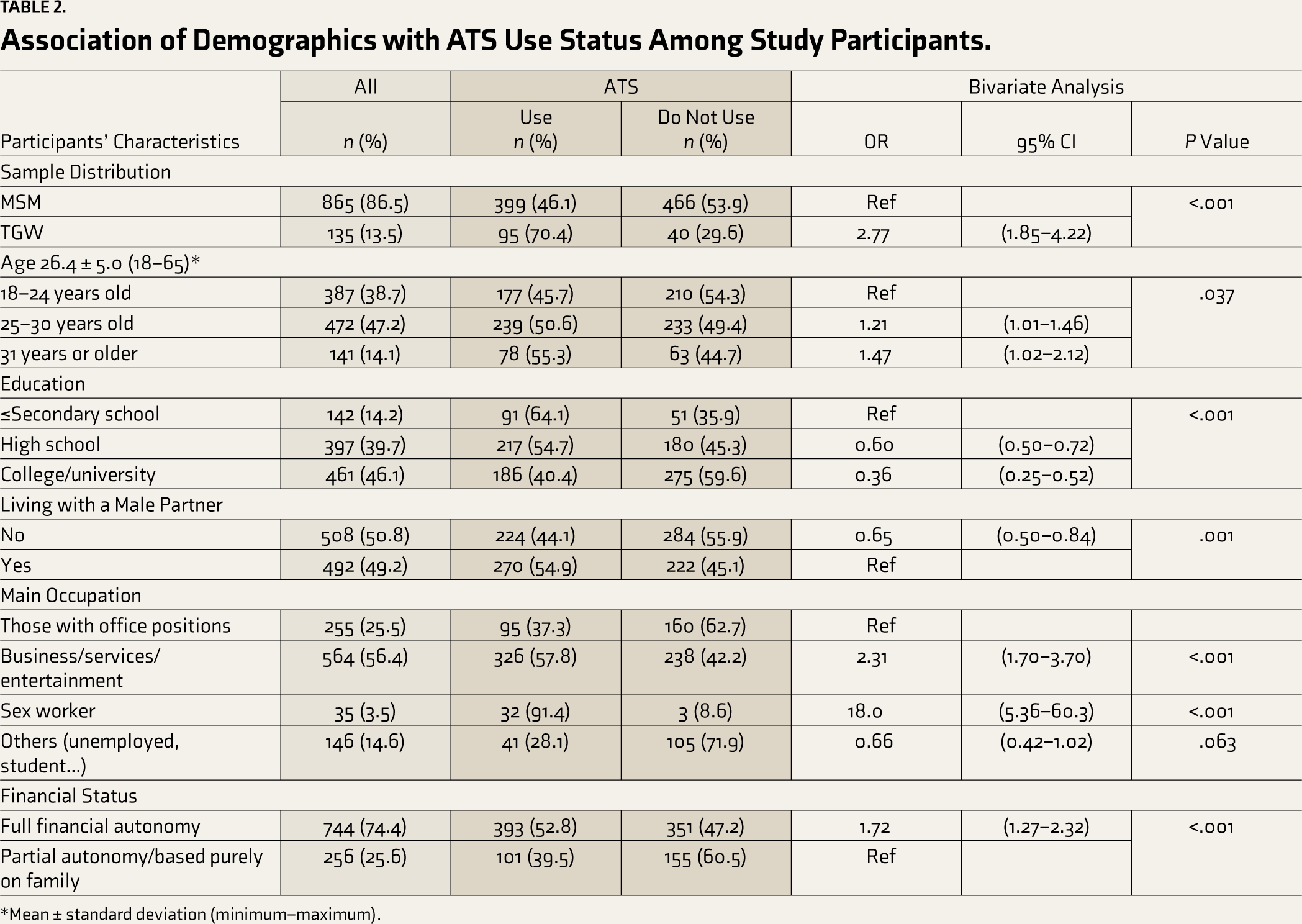
*Mean ± standard deviation (minimum–maximum).
Association of Sexual Behaviors, HIV Infection Status, and STI Testing with ATS Use Status Among Study Participants.

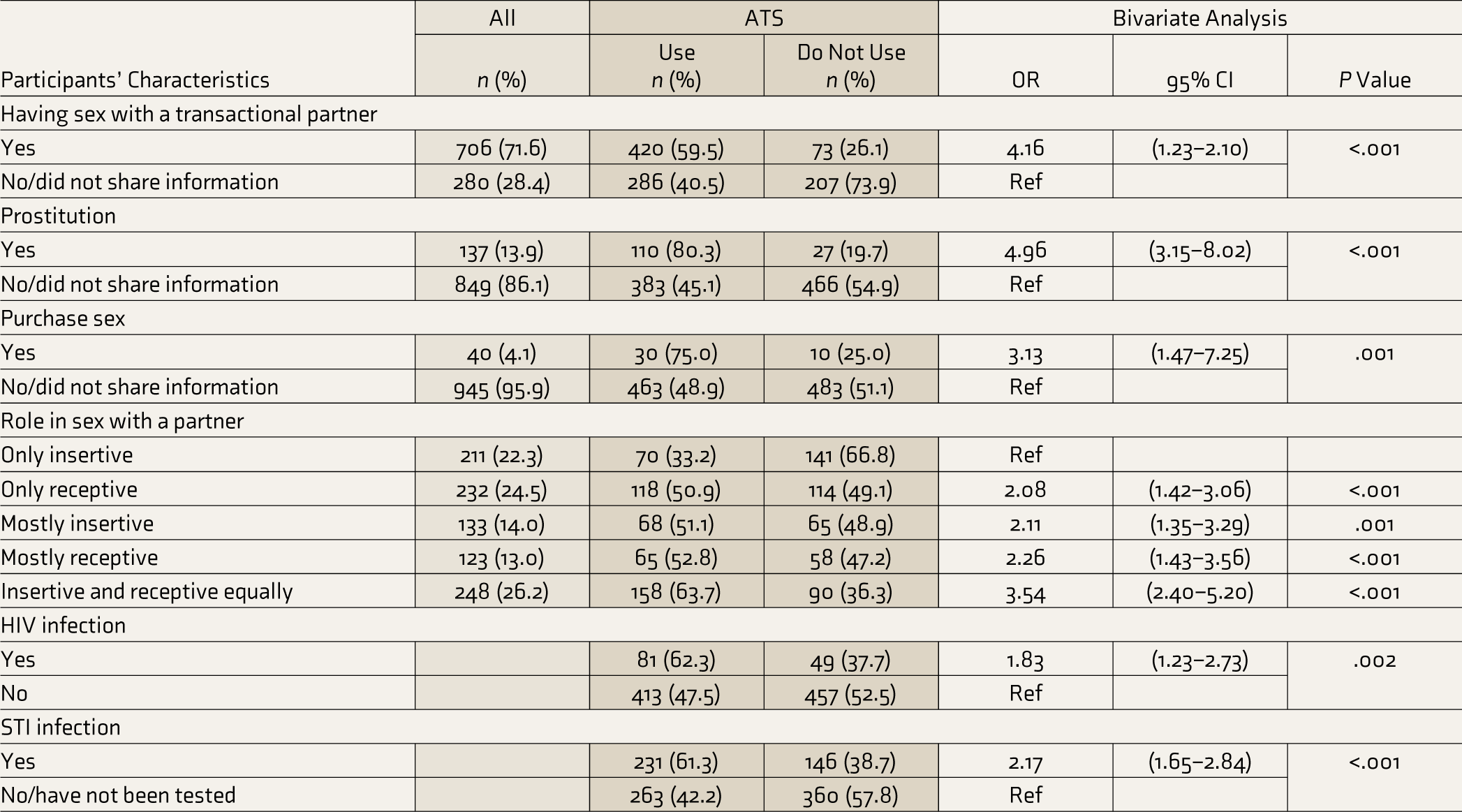
Multivariable analyses showed that ATS use was significantly associated with three sexual behaviors with partners and one role pair in sex with a partner. The specific sexual risk behaviors were sex with a transactional partner (aOR [29] = 3.06, 95% CI = 2.13–4.39), who engaged in sex and got paid or it (aOR = 2.78, 95% CI = 1.64–4.73), and purchasing sex (aOR = 2.34, 95% CI = 1.06–5.16). The role in sex with a partner with significant association was ‘insertive and receptive equally vs. insertive only’ (aOR = 1.78, 95% CI = 1.14–2.76). The multivariable analyses also showed that ATS use was significantly associated with higher financial status (aOR = 1.80, 95% CI = 1.24–2.60). Moreover, ATS use was also significantly associated with the lower age of first sexual intercourse (≥ 18 years old vs. < 18 years old; aOR = 0.41, 95% CI = 0.30–0.56) and main occupation (Those with office positions vs. Business/services/ Entertainment ‘aOR = 1.46, 95% CI = 1.01–2.10’ and others: unemployed, student…‘aOR = 0.53, 95% CI = 0.31–0.93’). In addition, ATS use was associated with higher odds of STI -infection (aOR = 1.67, 95% CI = 1.22–2.27) but not HIV infection. (Figure 1).
Multivariable Correlates of ATS Use Status Among Study Participants (
N
= 947).
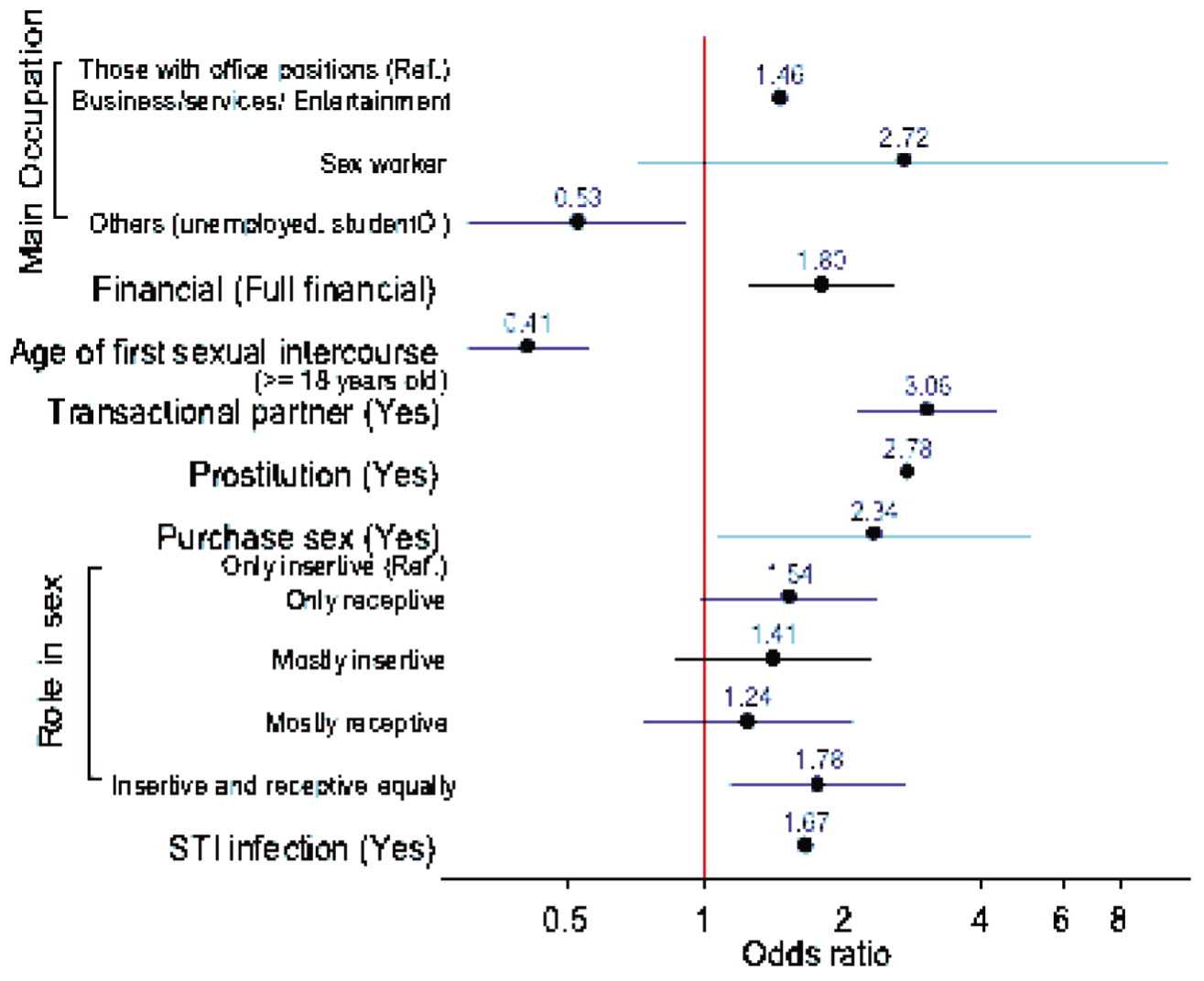
Discussion
Our study examined the prevalence and the level of ATS use among MSM and TGW in Southern Vietnam. The present study reported that 50.5% of participants used ATS at least once in their lives, and 49.4% used it in the past three months. The percentage of ATS use was much higher than in previous studies in Vietnam, the US, and China. The rates have varied from 24.7%–30.4% in the previous studies from Vietnam,25, 26 21.5% in the USA, 27 and 1.5% in China. 28 Besides, the moderate and high-risk level of ATS use among MSM and TGW was 93.5%, which was close to that reported in a previous study (90.5%). 25 It had been wisely postulated that Southeast Asia had become the hot spot for ATS trade and consumption in the past few years. In addition, because of its lower price and ease of use, the ATS has become increasingly popular in Vietnam. Consequently, the use of ATS has become one of the most commonly used substances among young people, especially MSM and TGW.
ATS acts as a stimulant on the central nervous system. High doses or long-term use can affect mental health and can specifically cause psychosis symptoms. However, with ATS in the community being mixed with many impurities, mental health is affected more seriously. In addition, ATS, with its increased ‘pleasure effect,’ can lead to risky behaviors (such as collective and condomless sex), resulting in risk for STIs and HIV infection. ATS places MSM and TGW as vulnerable groups that are facing social inequalities, discrimination, and barriers to accessing health care services. Therefore, it is necessary to have interventions on substance use for MSM and TGW, especially for those who have risky patterns of using ATS.
Regarding other substances, alcohol, solvents, and tobacco were commonly used at rates of 79.7%, 67.1%, and 42.6%, respectively. The results were consistent with many other studies in Vietnam and China.5, 25, 28 This high use rate can be explained by the fact that alcohol and tobacco are legal and available in Vietnam and other countries and are often the initially used substances.
In the multivariable analysis, the correlates of ATS use status were main occupation, financial status, sexual behaviors with partners, age of first sexual intercourse, and STI -infection, but not HIV infection.
We found that participants who were unemployed or students had a lower percentage of ATS use than those who held some kind of office job. This can be explained because the unemployed and students do not have a stable income, so ATS may not be readily accessible to them, which is not the case with those with office jobs. Similarly, participants in other occupations that provided a steady income also had a higher percentage of ATS use.
Concerning sexual behaviors, the study found an association between the age of first sexual intercourse and the prevalence of ATS use. Those who had sex for the first time at the age of 18 years or more had a lower rate of ATS use than those aged less than 18 years.
Like a previous study from China, the sex role of the sexually active partner was related to the use of substances, with participants in both an insertive and receptive role being more susceptible to ATS use than those whose role was only insertive. 28 Similarly, the participants who had sex with a transactional partner had a higher rate of using ATS. Often, during sexual intercourse with transactional partners, ATS was used to increase sexual pleasure. There was also a link between the participants who used prostitution or purchased sex and a higher ATS use rate. This may be to prolong sex with multiple partners or ATS being forced upon them. Besides, when the participants had sex with their paid/bought partners, the majority of participants were not aware of HIV and STI infection, and so when using ATS, they were likely to easily accept sex without using condoms even with the high risk of HIV and STI infection transmission.
The study showed a statistically significant association between ATS use and STI infection. The participants who used ATS had a higher rate of HIV-positive status than those who did not use ATS, but this difference was not statistically significant. This was similar to the previous research on TGW in Vietnam. 25 In another study, the HIV-positive rate among MSM and TGW was 13%, much higher than the general population. Currently, the main trend of HIV and STI transmission in the community is by high-risk sexual behaviors that ATS can contribute to by increasing pleasure, increasing libido, and prolonging the duration of sexual acts,
Limitations
The cross-sectional research is unable to identify a causal relationship, so it was not possible to identify whether the participants acquired HIV infection before or after initiation of ATS use. The results show that the use of ATS, being a major factor related to HIV and STI- infection, is a real concern among the MSM and TGW communities.
In the context of potential limitations, all the participants were recruited from xxx city and neighboring provinces. Hence, it might only be generalizable to some MSM and TGW nationwide. It is also difficult to derive causal relationships between ATS use and other factors from the cross-sectional analysis.
Conclusions
This study found that the association between ATS use and sexual behaviors is notable in Vietnam. Integrated HIV interventions that target substance use among MSM and TGW shall be more relevant than programs that only focus on HIV alone. Thus, it is essential to implement more effective interventions targeted at harmful patterns of ATS use among MSM and TGW communities.
Footnotes
Acknowledgements
The authors would like to thank all MSM and TGW participants in this study, and the individuals and institutions that made this research possible. From the community-based organizations in southern Vietnam, the authors thank Pham Hong Son (CBO1), Trang Van Toan (CBO2), Le Khuong (CBO3), Sa Liem (CBO4), Nguyen Ngoc Tuan (CBO5), Le Hong Thai (CBO6), Tong Van Nam (CBO7), Le Trong Minh (CBO8), and Le Trung Hieu (CBO9).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Declaration Regarding the Use of Generative AI
None used.
Ethical Approval
The study protocol was reviewed and approved by the Biomedical Research Ethics Committee at the University of Medicine and Pharmacy at Ho Chi Minh City, Vietnam (Approval number: 292/DHYD-HDDD).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this study was provided by the USAID Enhanced Community HIV Link-Southern Project for HIV testing, and the Vietnam HIV Addiction Technology Transfer Center via the Substance Abuse and Mental Health Services Administration.
