Abstract

Sir,
Abulia, a distinct lesser-known anatomoclinical syndrome associated with bilateral basal ganglia infarcts, entails the loss of motivation, reduced spontaneity, and blunted affect. 1 Traditionally, the mesolimbic dopaminergic system, localized in the ventral tegmental area with wide projections to the ventral striatum and prefrontal cortex, has been implicated in motivation and reward pleasure. 2 Bilateral lesions of the globus pallidus (GP) have been associated with anhedonia and depression. 3 However, the behavioral features of unilateral GP infarcts are lesser known. Atomoxetine, an inhibitor of the presynaptic norepinephrine transporter, has a widespread effect on the frontal-subcortical system that regulates dopaminergic transmission. 4 We report a novel clinical phenomenon of abulia secondary to an infarct in the left GP with a good response to atomoxetine.
Case Report
A 64-year-old female, homemaker, earlier known to be energetic, talkative, and motivated, presented with an abrupt change of behavior for a week. Her medical history was unremarkable except for hypertension for five years, for which she was on irregular treatment with Telmisartan 40 mg once a day. She had no past or family history of psychiatric or neurological illnesses. She was conscious and oriented. Earlier described as maintaining a high level of interest in family members, she showed a lack of concern about her family and her condition. Although able to follow complex commands, she did not initiate any activities of daily living. She would not initiate verbal communication, although, when coaxed, she would verbalize for brief periods.
She reported no sadness or anxiety but had a significant loss of appetite. Mini-Mental State Examination (MMSE) score was 28, and neurological examination was normal. Geriatric Depression Scale (GDS-15) score was 3. Detailed neuropsychological tests revealed intact attention, language, executive function, memory, and visuospatial functions (Table 1). MRI revealed an infarct in the ventral part of the left GP, involving both the external and internal segments (Figure 1). She was treated with atomoxetine, at an initial dose of 18 mg per day for one week, without any clinical worsening, and the dose was escalated up to 72 mg per day over two weeks. At four weeks of follow-up, there was improved initiation and spontaneity, with euthymia, active participation in cognitive testing, improved scores of fluency and problem-solving, and normalized appetite. Although spontaneous recovery is a possible consideration, it seems unlikely considering the recurrence of symptoms when a discontinuation trial was tried. The antihypertensives were optimized by the cardiologist at discharge.
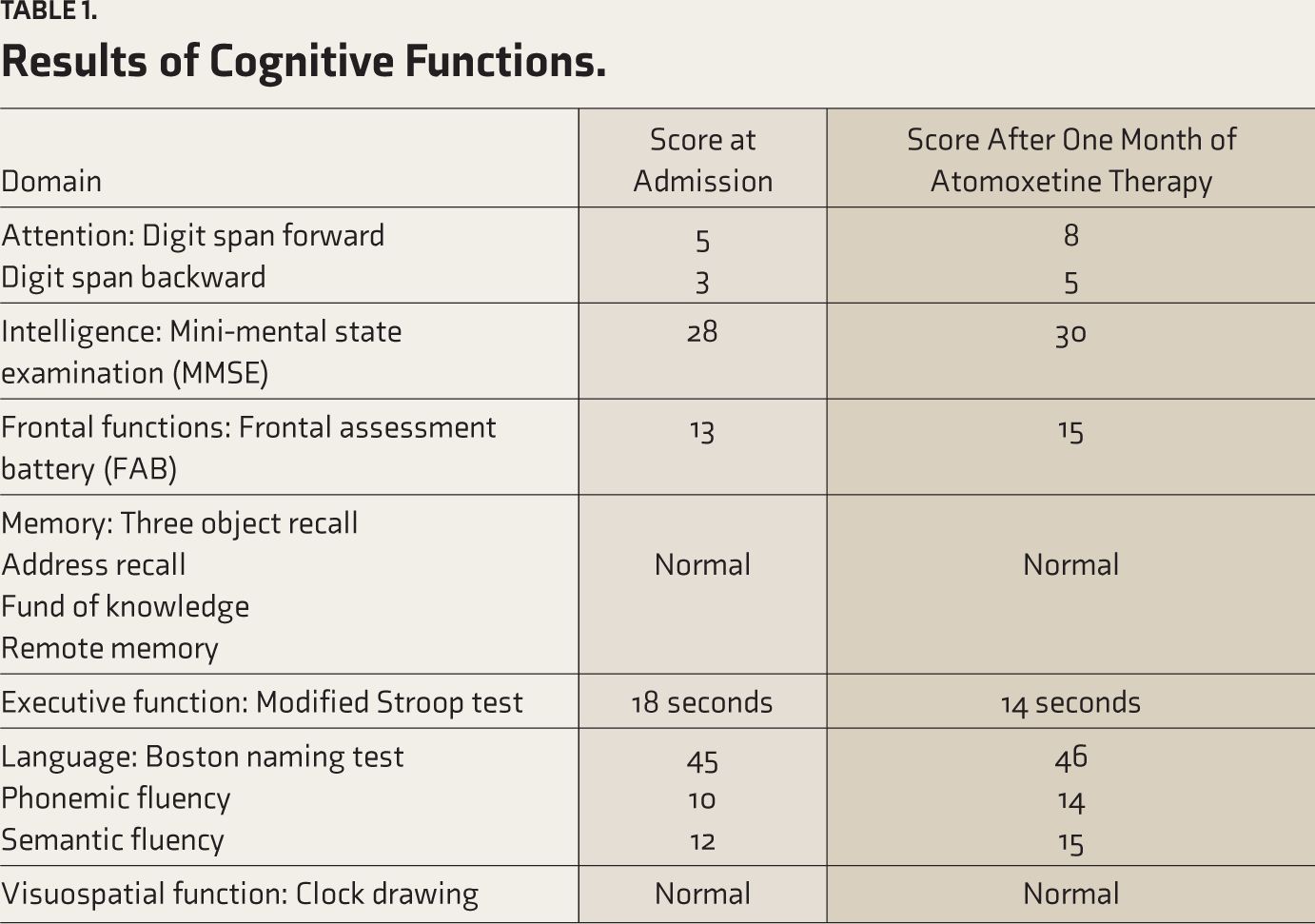
Results of Cognitive Functions.
Diffusion-weighted Imaging and ADC Mapping Showing Acute Infarct in the Left Ventral Globus Pallidus.
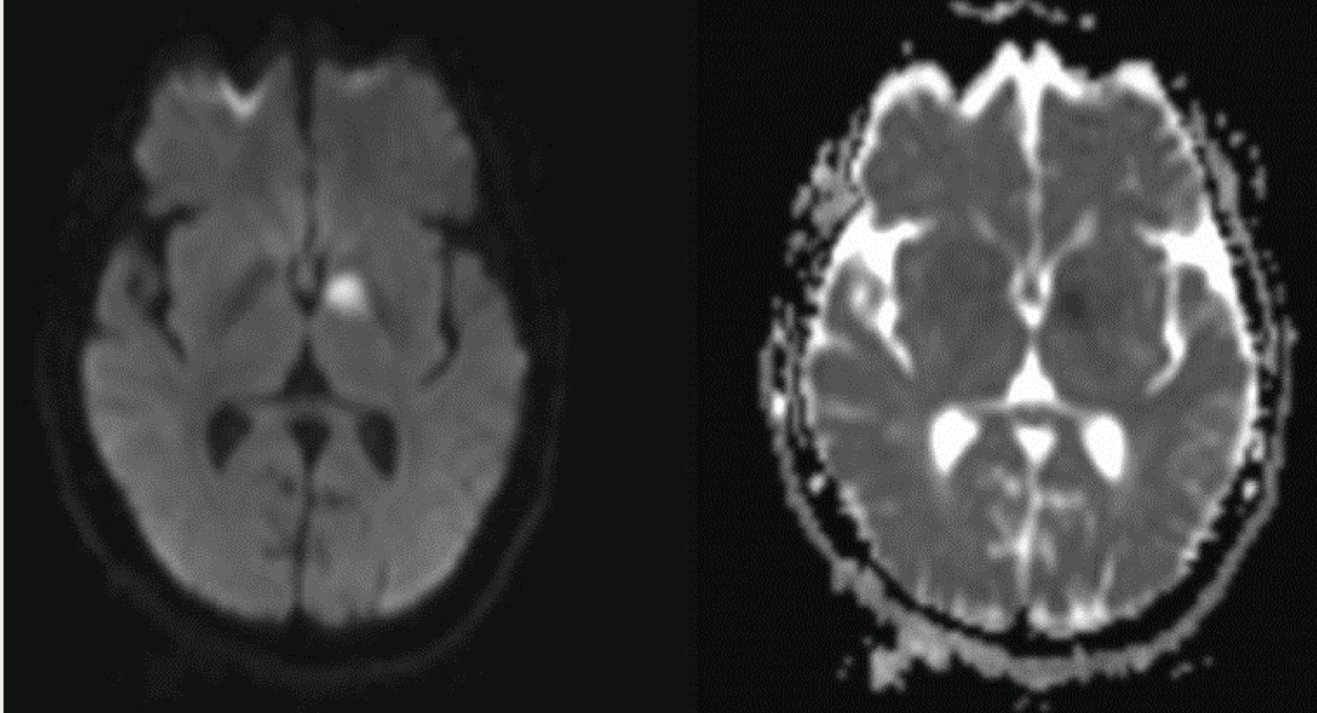
Discussion
Often interchangeably used with apathy, abulia is a moderate form of diminished motivation, with apathy being mild and akinetic mutism being more severe on the clinical spectrum of Disorders of Diminished Motivation (DDM). 5 Dopaminergic dysfunction has been found to result in abulia with growing evidence of the pivotal role played by the mesolimbic system in motivation. 6 Various behavioral consequences of bilateral GP damage following hypoxia and carbon monoxide poisoning have been reported, including anhedonia, depressed mood, and social isolation.7, 8 Because those cases resulted from metabolic insults, diffuse neuronal damage cannot be excluded as the cause of the behavioral symptoms, unlike our patient who had a focal cerebral infarction. Cognitive impairment primarily involving attention, fluency, and verbal memory that has been reported in left GP infarcts 9 was conspicuously absent in this patient.
The ventral GP and nucleus accumbens receive dopaminergic fibers from the ventral tegmental area and these comprise the motivation and reward circuit. Disruption of this circuit resulted in the abulia. Furthermore, exposure to stimuli associated with reward triggers neuronal firing in the ventral GP. 8 The patient’s diminished pleasure in the family may have been related to the impaired effect of social rewards. Lack of extrapyramidal signs indicates sparing of the dorsal GP, which is involved in motor behavior. 8
We optimized the dose of atomoxetine in the current patient based on a previous report where, in a patient with right anterior cerebral artery infarction, atomoxetine, with a dose optimized up to 72 mg per day, given for eight weeks, had led to clinical improvement, with increased cerebral glucose metabolism in both the premotor and visual association cortices. 10
Stimulation of the noradrenergic brainstem nuclei enhancing the function of the premotor and prefrontal cortices, with indirect influence on the subcortical dopaminergic system, 4 could have been the mechanism of clinical improvement in my patient.
This is the first case report of abulia in association with unilateral GP infarct; hence, whether atomoxetine hastened the natural course of recovery is difficult to comment upon. However, literature on cognitive impairment in GP infarcts suggests sequelae at three months.6, 9 No scale was utilized to document the improvement of abulia since no validated scales are currently in use. The improvement was determined from a consensus of a team of a neurologist, nurses, physical and occupational therapists, and patients’ family members.
This case report suggests a beneficial effect of atomoxetine. However, to confirm the efficacy, additional controlled studies with larger samples are necessary. The development of a rating scale for abulic symptoms, to quantify the efficacy of pharmacological interventions, is also needed.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent has been taken from the patient’s son for the patient information and images to be published.
