Abstract
Background:
COVID-19 causes psychological distress and anxiety due to fear of infection and the possibility of worsening symptoms leading to mortality. Public health measures like contact tracing and lockdowns further increase the panic among infected patients and the public. We intended to assess the effect of telecounseling in reducing anxiety in patients admitted to isolation wards.
Methods:
In this multi-center observational study, we administered a Generalized Anxiety Disorder-7 (GAD-7) scale before and after telecounseling. The study group consisted of participants who gave consent for telecounseling, and those who did not give consent constituted the control group. The telecounseling was based on the Psychological First Aid model, due to its simplicity.
Results:
There was a statistically significant decrease in anxiety after telecounseling in the study group (P value ≤ 0.001, effect size = 0.484). There was a statistically significant decrease in anxiety in the study group compared to the control group (P value ≤ 0.001).
Conclusion:
Telecounseling contributed to the reduction in anxiety in COVID-19 patients in isolation wards. Several other factors like severity of the infection, comorbid medical illness, pre-existing mental health issues, individual’s level of coping with stress, and duration and place of admission may have affected the anxiety levels in the patients.
A pandemic has damaging psychological consequences both in the community and in isolation wards. Anxiety can be reduced by providing telecounseling to COVID-19 patients.Key Messages:
COVID-19 patients in isolation wards undergo immense psychological distress, in addition to the ill effects of the disease. 1 Studies in China and elsewhere assessed the psychological issues among the general population, 2 health workers, 3 and students 4 during the pandemic. Sub-syndromal mental health problems were a common response to the COVID-19 pandemic, and a need for more representative research from other affected countries, particularly in vulnerable populations, was stressed. 5 Investigating the need for interventions for the impact of COVID-19 on mental health and working on strategies to improve coping skills and resilience were the need of the hour. 6 No other study from Tamil Nadu has assessed the effect of interventions on the psychological issues in COVID-19 patients. Ours is the first observational study on interventions to reduce anxiety levels in COVID-19 positive patients from the state. We aimed to estimate the efficacy of telecounseling in reducing anxiety among COVID-19 patients in isolation wards.
Materials and Methods
Subjects
COVID-19-positive patients admitted to Government Villupuram Medical College and Hospital and Government Thirunelveli Medical College and Hospital from May 2020 to October 2020 were the participants. Inclusion criteria were (a) age—15 to 80 years, (b) COVID-19-positive patients in isolation wards, and (c) patients with a phone or access to a phone. Exclusion criteria were (a) clinically unstable patients (saturation below 92% and with severe comorbid medical illness) and (b) patients who did not consent to participate in the study.
Materials
The Generalized Anxiety Disorder scale 7 (GAD-7) 7 was used to assess anxiety. The GAD-7 scale was translated into the vernacular language with the help of senior professors of both psychiatry departments. We used forward translation from English to vernacular language at both the centers individually, compared the two drafts, and finalized a draft and the same was used in both the centers.
Procedure
Institutional Ethical Committee appro-val was obtained from both institutions. The Government of Tamil Nadu had instructed the health department to provide telecounseling to COVID-19 patients. The daily list of patient admissions and their phone numbers were obtained from the state-government district administration’s line list. The patients’ cell phone numbers were verified with case records and we confirmed whether the patient had a phone or access to a neighbor’s phone in the ward. Informed consent was obtained orally over the phone. The translated GAD-7 was administered and scored by calling up the patient, once within a day of admission, and again on the day of discharge. Telecounseling was administered 3–4 days after the admission, in a single session. It was based on the Psychological First Aid model (PFA). 8 Both the GAD-7 and the telecounseling were administered by 10 counselors, 2 psychiatrists, 4 trained postgraduate students, and 4 trained psychiatric social workers of the Departments of Psychiatry of the institutions. Brief one-day training, in the form of an interactive session, was given on PFA, explaining its steps, basic details of COVID-19, and the infrastructure and facilities in the hospital isolation wards. It was followed by a demonstration of telecounseling sessions by psychiatrists and role-play rehearsals among the trainees. Each telecounseling session lasted 10–15 minutes. The counselors introduced themselves; informed the patient that they were there to help (contact and engagement); assured them they were safe in the isolation ward (safety and comfort); answered queries on their fears and anxieties; advised them to breathe slowly, pursue pleasurable activities, and eat and rest during their isolation period (stabilization); encouraged them to speak to their loved ones and friends (connection with social supports); helped them to prioritize and restructure their needs; reminded them of how they had tackled an earlier crisis successfully (information on coping); and gave information about food, water, and sanitation services (linkage with collaborative services). Anxiety levels were graded as mild (≤7), moderate (>7 and ≤14), and severe (>14). Anxiety levels among the study and control groups were estimated on admission and discharge. The control group consisted of patients who did not consent to the counseling and to whom counseling was not administered due to worsening symptoms but were administered the GAD-7 on admission and discharge. The scoring sheet did not mention the counseling interview, to eliminate scoring bias between the control and study groups during the administration of the GAD-7 at discharge. Randomization was not done as the design was a multicenter observational study.
Statistical Analysis
Sample size calculation was done using the OpenEpi software. Using a study done in southwestern China 9 as our reference, 173 participants were needed (confidence level = 95%).
Anxiety scores on admission and discharge were considered as primary outcome variables. Age and sex were considered as other study-relevant variables. In the study and control groups, for normally distributed quantitative parameters, the mean values were compared using the independent sample t-test (two groups). For non-normally distributed quantitative parameters, the mean values were compared using the Mann–Whitney u test (two groups). Wilcoxon signed-rank test was used to test for the statistical difference between anxiety scores at admission and discharge. Categorical outcomes were compared using the chi-square test and the Mc Nemar test. The repeated measures ANOVA was used to compare the anxiety levels before and after the telecounseling.
P value < 0.05 was considered statistically significant. Data were analyzed using coGuide software, V.1.03. (1) 1 of ADSS Corp. released in 2020 and coGuide Statistics software, Version 1.0 of India ADSS corp.
Results
A total of 574 patients were recruited, out of which 569 were included in the study, with 516 participants in the study group (with telecounseling) and 53 in the control group (without telecounseling). Five participants were not included due to the inability to complete the administration of the GAD-7 on time. In the study group, out of the 516 participants, only 465 were able to complete both the GAD-7 scoring sessions and were included in the final analysis; In the remaining 51, we could not administer the GAD-7 both times.
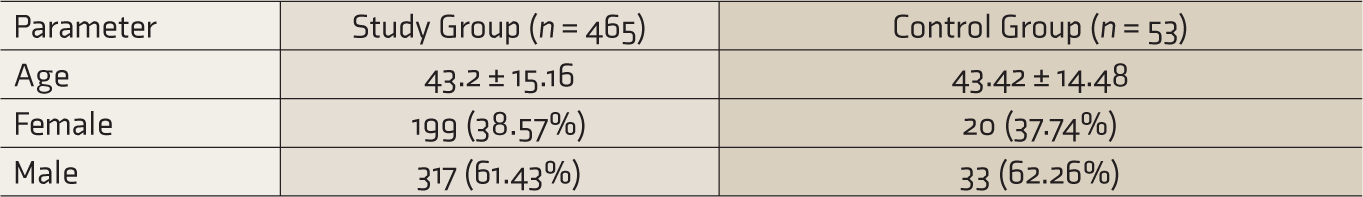
The study and control groups were similar in demographic characteristics of age and sex (Table 1). The overall prevalence of moderate to severe anxiety (GAD 7 score >7) at admission was 36.68%. The prevalence of moderate to severe anxiety levels on admission in the control group was 69.81% and in the study group was 36.26%. There was a statistically significant decrease in mean anxiety levels and grades of anxiety levels in the study group after telecounseling (Table 2). The decrease in grades of anxiety levels in the study group compared to the control group at discharge was statistically significant (Table 3). The grades of anxiety levels at discharge were less than their levels at admission in both the groups.
Comparison of Demographic Parameters.
Decrease in Moderate to Severe Anxiety Levels in the Study Group after Tele-Counseling.
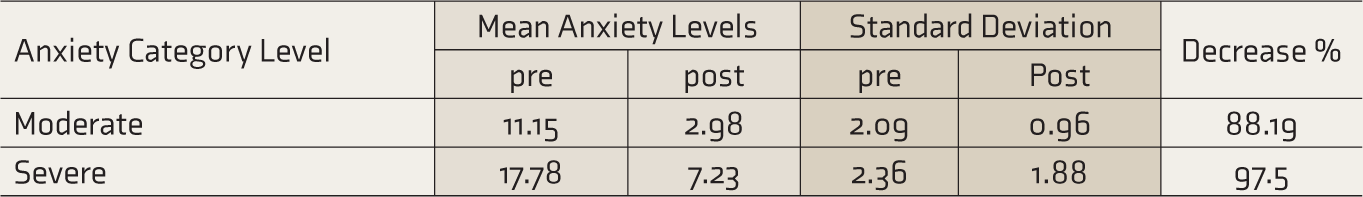
P Value ≤ 0.001, Effect Size = 0.48.
Moderate to Severe Anxiety Levels at Discharge in the Study and Control Groups.
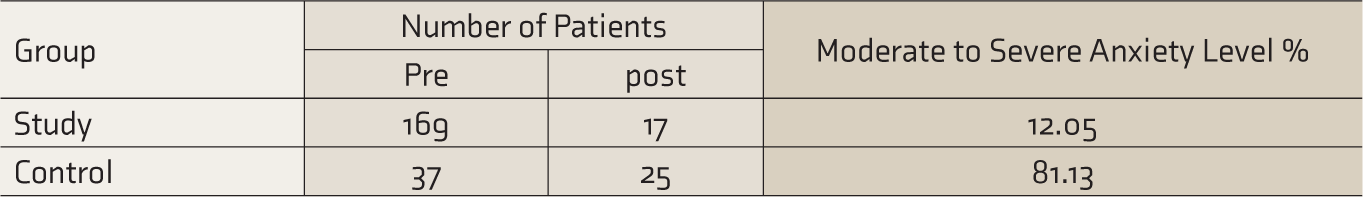
P Value ≤ 0.001.
In the study group, severe anxiety levels decreased by 97.5% and moderate anxiety levels by 88.19% at discharge (Table 2). In the control group, severe anxiety levels decreased by 33.3% and moderate anxiety levels remained the same at discharge. The repeated measures ANOVA with a Greenhouse–Geisser correction determined that the mean anxiety score of the study group had a statistically significant difference between time points [F (1, 465) = 435.5, P < 0.005, effect size = 0.484]. Post hoc analysis with a Bonferroni adjustment revealed that in the study group, anxiety scores had a statistically significant decrease from before telecounseling levels [5.1(95%CI, 4.6 to 5.6) P < 0.0005]. Mauchly’s test of sphericity indicated that the assumption of sphericity has been violated [χ2(2) = 3.343, P = 0.188]. We found that the fear of the infection and its possible morbidity contributed to the patients’ anxiety. Staying away from family in a closed ward for prolonged periods was another cause of anxiety.
Discussion
In our study, the overall prevalence of moderate to severe anxiety at admission was 36.68%, that is, 208 among the 567 patients had anxiety, which is almost three times that of the prevalence of anxiety levels in the general population during the COVID-19 pandemic, 12.9%. 9 The high prevalence may be due to the prevalence of anxiety being measured in the COVID-19 positive patients who were isolated in the isolation wards in a hospital, compared to measuring the prevalence in the unaffected persons in the general population.
There was a statistically significant decrease in mean anxiety levels and grades of anxiety levels in the study group after telecounseling. The telecounseling served as an effective means to reduce anxiety with a medium effect size of 0.484. During the telecounseling session, we encouraged the patients to talk to their family members, friends, and counselors, instead of using social media. A study in the general population during the outbreak showed that the time spent focusing on COVID-19 (≥ 3 hours per day) was associated with Generalized Anxiety Disorder. 10 We conveyed the test results of family members, to allay the patients’ fears. A total of 75.2% of the general population were worried about their family members contracting COVID-19. 2 We reiterated the importance of precautionary measures like hand washing and wearing a mask. Many patients were constantly seeking clarification of posts on social media and news, during our telecounseling. We encouraged the patients to watch reliable news on TV channels than on social media. Specific, up-to-date, and accurate health information (e.g., treatment, local outbreak situation) and particular precautionary measures were associated with a significantly lower psychological impact of the outbreak and lower levels of stress, anxiety, and depression. 2 Telecounseling as an intervention also acted as a supportive measure that allowed patients to speak out about their anxieties and obtain relief. Studies among college students showed social support was negatively correlated with the level of anxiety. 4 We encouraged sleep hygiene and prescribed benzodiazepines in certain instances. A study had shown the need for interventions for insomnia among medical staff during the pandemic. 3 The decrease in anxiety levels in the study group may also have been due to other factors like asymptomatic COVID-19, shorter duration of admission, individual’s level of coping with stress, administration of anxiolytics, and in-person visits of physicians and counselors. In cases where members of the same family were admitted, we arranged for them to be in the same ward whenever possible. Adequate rest and timely serving of good food in the isolation wards could have also contributed to the decrease in anxiety. These observations need to be studied further and verified. The decrease in grades of anxiety levels at discharge was significantly higher in the study group. Though this decrease could have been due to the telecounseling, it could have also been due to the relative increase in the grades of anxiety levels at discharge in the control group. The patients who suffered worsening in COVID-19 symptoms or comorbid illnesses after administration of the GAD-7 on admission were shifted to step-up wards and were not available for telecounseling. On improvement, some of them were stepped down to isolation wards and were administered the GAD-7 at discharge. These patients came under the control group and could have scored higher on the GAD-7 at discharge due to worsening symptoms and having witnessed morbidity and death in the step-up wards. This needs to be verified by further studies.
We based our telecounseling on the Psychological First Aid model 8 as it was easy to administer, required less time, had fewer sessions, and could be administered by nonprofessionals with minimum training, compared to models based on cognitive behavior therapy. The patients in the isolation wards were admitted for 10–14 days. They remained in isolated cubicles, leaving them only for food, water, and toilet use. Their cell phones were their only source of communication, information, and entertainment. The conversation with the counselors was a welcome interaction for most patients, though a few were annoyed. This is in agreement with a study that showed that brooding about family members in their absence and the possibility of the infection spreading to them were causes of anxiety. 1 Telecounseling also served as a means to address patients’ grievances, which were resolved in coordination with the hospital administration.
Limitations
The control group was small, with only 53 patients. The study and control groups were not comparable, as the baseline anxiety levels were different. The absence of standard psychological intervention guidelines and formal training for the counselors 11 could have led to variability in the anxiety scores and the quality of telecounseling. The GAD-7 was not validated on COVID-19 patients. Problems like the nonavailability of cell phones, not knowing how to use the cell phone, network and connectivity issues, and hearing disability in the older adults might have influenced the effectiveness of telecounseling. We obtained only age and sex from the patient details of the district administration line list. We were unable to obtain complete demographic and clinical data for all the patients due to pandemic restrictions in the isolation wards and this has narrowed the scope of our study. Digital psychological interventions such as text messages, chat lines, applications, blogs, and forums could have been considered.12, 13
Conclusion
Telecounseling contributed to reducing anxiety levels in COVID -19 patients admitted to the isolation ward. During a pandemic, telecounseling can be important in addressing psychological issues such as anxiety. Factors such as asymptomatic COVID19, duration of admission, individual’s level of coping with stress, administration of anxiolytics, and in-person visits of physicians and counselors may have influenced the effect of telecounseling in reducing the anxiety levels in the infected patients.
Footnotes
Acknowledgements
We are thankful to the below mentioned for their contribution in tele-counseling and administering the anxiety scale:
Miss Rosalla, MSW psychiatric social worker Mr Arun, MSW psychiatric social worker Mr Pavithran, MSW psychiatric social worker Mrs Anbuselvi, MSW psychiatric social worker Dr Usha Nandhini Dr Srikrithika Dr Niranchanadevi
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
