Abstract

Dear Sir,
Healthy Mind for Healthy Nation!
The Government of India’s “National Institution for Transforming India” (NITI) Aayog Health Index (NAHI) is an aspirational step to fulfill the overall goal of achieving prosperity for all. This composite index was released in 2016 1 based on the rationale that poor health status is one of the main factors hindering economic growth. This index is calculated for every state and union territory, based on 23 essential factors clubbed under three groups. 1 This index has been released twice so far, latest in June 2019. This year-on-year index measures the improvement of the states and union territories. This initiative will assist in state-level monitoring of performance and serve as an input for providing performance-based incentives and improving health outcomes.
This article aims to critically analyze NAHI with respect to mental health (MH). The authors also propose a few measurable outcomes of MH to be included in the next version of NAHI.
Critical Analysis
Overall Provisions in the Index
The NAHI was framed to meet the United Nation’s (UN) sustainable development goal (SDG). Goal 3 of SDG exclusively speaks about “good health and well-being,” under which there is mention of promoting mental well-being and addressing the burden of substance use disorders (SUDs). To meet Goal 3 of SDG, NAHI has framed 23 essential factors subgrouped under three domains: health outcomes, governance and information, and critical inputs/processes. It is unfortunate that NAHI has not included mental illnesses and SUDs.
Mismatch with Other Developments in India
The NAHI heavily focuses on physical illnesses and has grossly neglected MH (except for the recommendation of one psychiatrist at district hospitals), whereas National Mental Health Policy, 2014; Mental Healthcare Act 2017; 2 and rapid expansion of National Mental Health Program (NMHP) 3 have all emphasized the burden of MH issues.4, 5
India’s Stand on Mental Health in the International Scenario
India was the first country to advocate MH as the fifth noncommunicable disease (NCD). India fought alone to push psychiatric disorders into the category of NCDs and gained major success in the World Health Organization (WHO) conference on NCD.6, 7 But it is rather surprising to know that NAHI is not in synchrony with these aforementioned developments. One of the likely reasons for this neglect is the misunderstanding that there are no measurable outcome indicators in MH, which is not true.
The Importance of Mental Health in the Indian Scenario
The WHO endorses the slogan of “No health without mental health.” According to Global Burden of Disease Study 2010, MH and SUD’s were the leading causes of years lived with disability worldwide. 8 The National Mental Health Survey of India also reported that the point prevalence of psychiatric disorders was 10.6%. Mortality among patients with mental illness is significantly higher too, with a pooled relative risk of 2.22. 9 Despite this high prevalence, morbidity, and disability, the treatment gap range is as high as 83% for mental disorders. 10
Cost of Mental Disorders in India
Health regulates the productivity, expenditure, retirement, and dependency in a country. NCDs, including mental illness, are raising concerns because of their significant impact on economic expenditure. Mental illness leads to a decline in the number of family members who can work. The Global Economic Burden of NCDs 2011 report by the World Economic Forum and Harvard School of Public Health envisaged that MH alone would cost India $1.03 trillion between 2012 and 2030. The WHO reports that treating common mental disorders will eventually increase national income. 11 NITI Aayog has considered the aforementioned point in its health index but has still excluded psychiatric disorders. 12
Suggestions
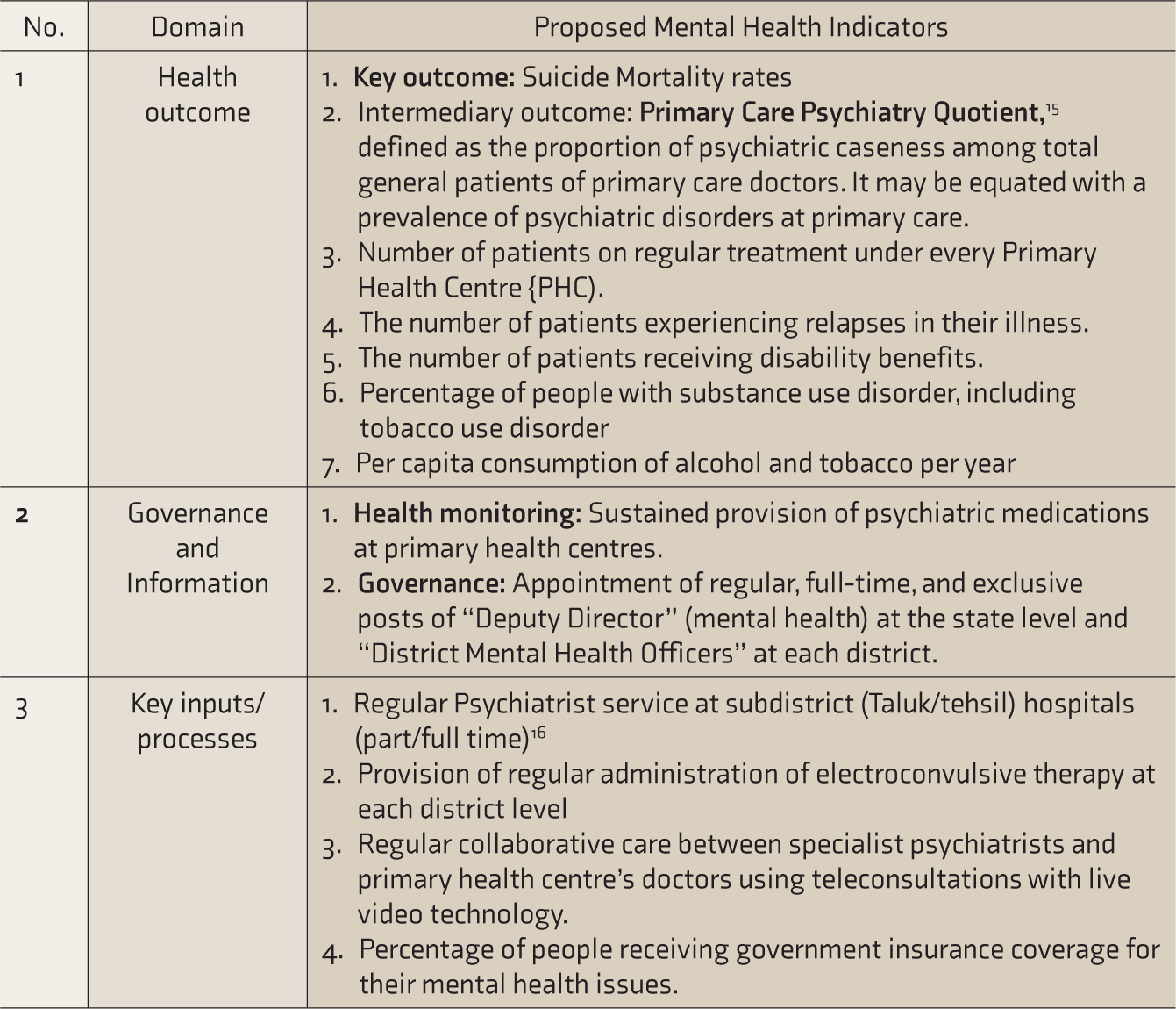
The authors suggest a proportionate increase in the importance given to MH in the subsequent versions of NAHI. We propose a few possible measurable outcome indicators of MH within its three domains ( Table 1 ). One of the most important indicators would be suicide mortality rates. Reasons for suicide are much beyond just psychiatric illness. They include multiple socioeconomic factors such as poverty, unemployment, etc., which in turn can impact MH. So, suicide rate is a good indicator of the overall MH of the community, and the same is mentioned in Goal 3 of SDG also. 13 Another indicator we propose is primary care psychiatry quotient (PCPQ). 15 PCPQ is defined as the percentage of primary care attendees having psychiatric disorders receiving first line treatment among total outpatients. 15 Studies have already shown that 17% to 46% 14 of patients attending primary health centers have psychiatric illnesses; so, PCPQ of at least 30% will indicate fair which in turn will mean a fair number of patients being pulled into the treatment loop. 15 Another indicator is the number of patients with mental illness receiving regular treatment and disability-related benefits. However, the proposed indicators need to be studied further for its feasibility and validity.
Measurable Outcome Indicators of Mental Health to be Added in NITI Aayog Health Index

Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
