Abstract

Mental health research in India is still in its infancy. The limited research capacity, lack of adequate mental health professionals (MHPs), insufficient funding, inadequate research training opportunities, and low priority accorded to mental health by the government are some of the barriers to mental health research in India.1-4 Further, administrative barriers include a lack of prompt ethical, scientific, and regulatory review at an institute or government level. 5 Recent scientometric studies point out that a few premier Indian institutes disproportionately dominate the mental health research output in the country. 6 Also, the involvement of the private practitioner in mental health research is minimal due to current regulatory mechanisms which are not conducive to include them in the research ecosystem.
On the one hand, to improve mental health research and address some of the existing barriers, many institutes and professional organizations have taken several innovative steps such as capacity building and research methodology training 7 ; on the other hand, there is the addition of new potential barriers to mental health research. In this article, we aim to discuss the potential impact of the new regulations on various components of mental health research, such as conceptualization and dissemination of findings. We also attempt to provide some feasible solutions.
The Potential Impact of New Regulations and Laws
Practically, the permission from SMHA does not add any additional benefits in terms of protection of rights of a person with mental illness. But these regulations can increase the burden and stress on researchers due to increased administrative paperwork and delay in the approval of research proposal from SMHA. For multi-centric research involving different states, the process can be especially cumbersome to the researcher due to inter-state variation in the research approval process of SMHA. Further, the SMHA has only 6 MHPs (2 psychiatrists) out of 17 members, and voting is based on the final decision rather than scientific merit (section 56 [3]). These, together with the irregular meeting schedule of SMHA (section 56 [1]), can negatively impact the mental health research ecosystem. Postgraduate students of psychiatry and clinical psychology trainees, who are already burdened with clinical work, have to go through this tedious procedure (which will not be applicable for the postgraduate students of other medical disciplines) for getting research approval for their mandatory thesis/dissertation work. It may discourage researchers from studying patients with severe mental illnesses (where the capacity to consent is compromised). Similarly, Indian researchers may face challenges in collaborating with researchers of other countries in multinational projects, due to multiple logistic issues in getting ethics approval. These issues are also relevant for clinical/drug trials conducted on patients with severe mental illness.
In our opinion and experience, the conduct of conferences and webinars on virtual platforms during the COVID-19 pandemic has led to rapid knowledge dissemination surmounting barriers related to costs (e.g., high participation fees, lack of travel support for early career psychiatrists and researchers from many low-to-middle income countries including India) and logistics (difficulties in getting the visa, time constraints for the busy clinician in attending an in-person conference). 15 It has given more opportunities for people to participate and present their research work. The new guidelines are, perhaps, important from a national security perspective. Nonetheless, they will also impede mental health research in many ways, including restricting international training opportunities and posing difficulties in disseminating Indian perspectives and research findings.
Overall, the virtual conference guidelines and section 99 (2, 3) of MHCA, on implementation, can reduce the mental health research in critical areas mentioned above, lead to under-representation of Indian psychiatry at the international level, and increase potential threats of political abuse of mental health researchers working on vulnerable populations (e.g., farmer suicide, marginalized populations). Interactions with the leaders in the field are critical to enhancing opportunities for collaborative work and need to be encouraged by the removal of systemic barriers.
To address these challenges, large institutions and universities may develop a system or employ an individual to help navigate bureaucratic hurdles, but small, rural institutions and independent researchers may need support or suitable modifications and strategies. Given this scenario, we propose a few recommendations aimed at limiting the potential negative impact of these new measures and legislations.
Some Recommendations
In our opinion, the MHPs registered with professional bodies and MHP course trainees must be exempted from having to seek approval from SMHA for research. Indian MHPs are already following various professional, regulatory, and ethical guidelines10,12 and are more proactive and supportive for the rights of persons with mental illness, and there is no evidence that the registered MHPs have violated the rights of persons with mental illness. Further, SMHAs should continue to assess the proposal for research on persons with mental illness, initiated by non-MHPs, for approval.
Proposed Model of Single Window System
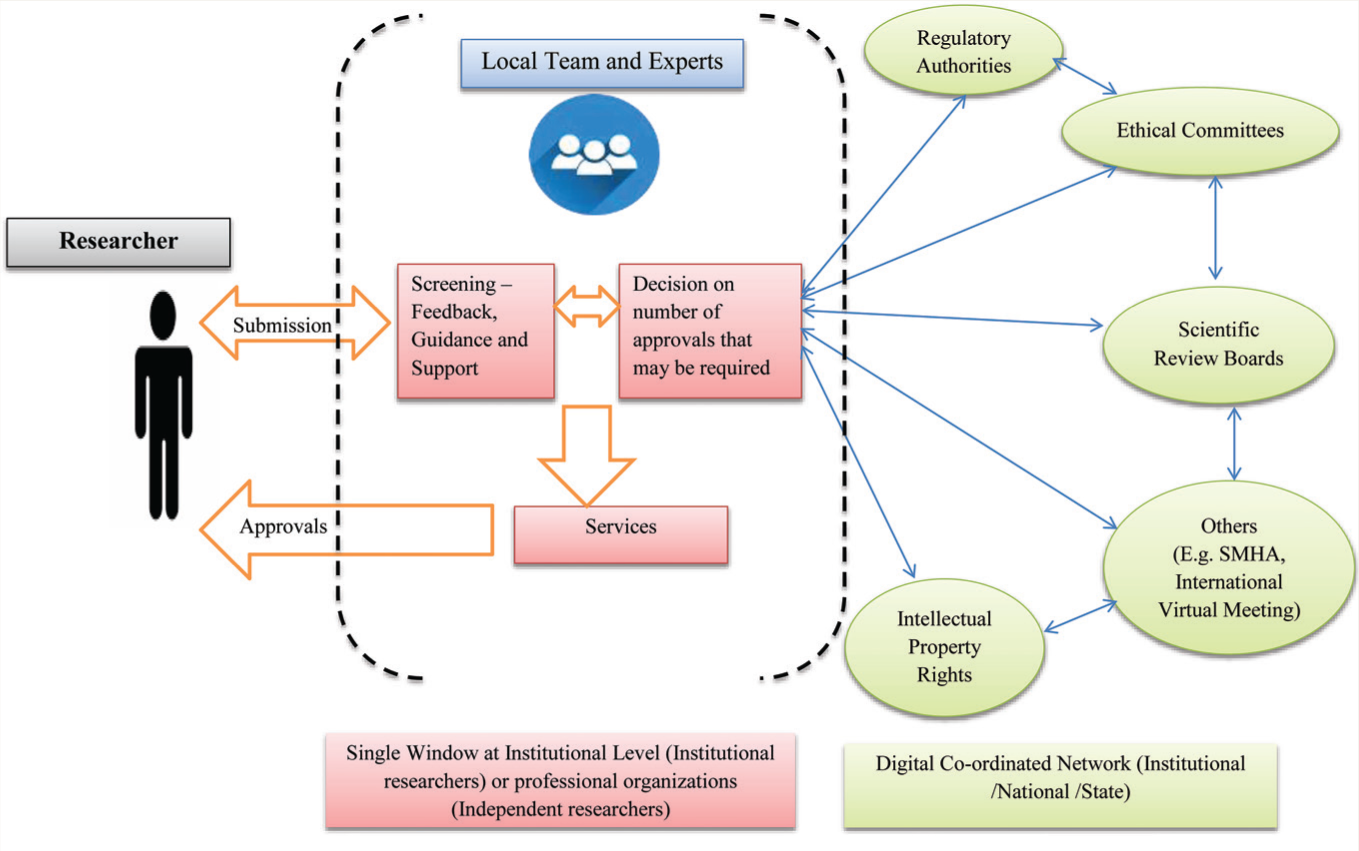
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
