Abstract

Telepsychiatry Practice in Sikkim Manipal Institute of Medical Sciences
Sikkim is a state in north-eastern India sharing borders with China and Bhutan. This least populous and second smallest state in India has 14 consultant psychiatrists and 5 psychiatry postgraduate trainees. As per the 2011 Indian census, Sikkim has a population of around 610,577. 6 Based on the reliable population data, there are 2.3 psychiatrists per 100,000 in Sikkim, which is well above the national average of 0.75 per 100,000. 7
Telepsychiatry services from the Department of Psychiatry in our hospital, Sikkim Manipal Institute of Medical Sciences (SMIMS), began on March 25, 2020, at the commencement of the nationwide lockdown. Patients who have had their prior consultations with the psychiatrists at the hospital before the lockdown constitute the majority of those who sought telepsychiatry services. All five psychiatrists of the hospital were involved in the handling of telepsychiatry consultations for both new as well as follow-up cases. These patients have been calling or messaging their psychiatrists on their mobile numbers and also connecting with them on social media platforms. The new cases connected to the psychiatrist either by calling the hospital or through a person who has already visited or is known to these psychiatrists. All follow-up cases contacted the psychiatrist directly as they already had the contact numbers or obtained it from the hospital. The telepsychiatry consultations were done with the help of audio and video modes. Video mode was utilized for all new cases and, where List A medications like antipsychotic, antidepressant, etc.,
5
needed to be prescribed for the first time (
As of May 26, 2020, there have been a total of 78 teleconsultations (
We had six acute cases. For all of these, we guided the caregiver for a referral to a nearby hospital or to come to our institute. We received no cases of child and adolescent psychiatry for telepsychiatry consultation.
Challenges We Faced
Though an informal consent was taken before starting any consultation, it was difficult to get a formal written consent as suggested in the telepsychiatry guideline (Appendix 2, last part). 5 The service users needed to be explained about the regulations of telepsychiatry. However, they were not very keen to listen about it during the initial stage of consultation, and, also, did not have the logistics to take a printout and send an image of the signed consent form. In some follow-up cases who were higher doses of the medications, refilling the doses without actual physical examination was a tricky affair. A routine OPD consultation gives the chance to build a relation, both for the attending psychiatrist and the patients as well as their caregivers; the virtual consultation may not have the same effect, especially for the new cases where the patients/caregivers are in contact with a stranger on a small screen and may not like disclosing everything about their life.
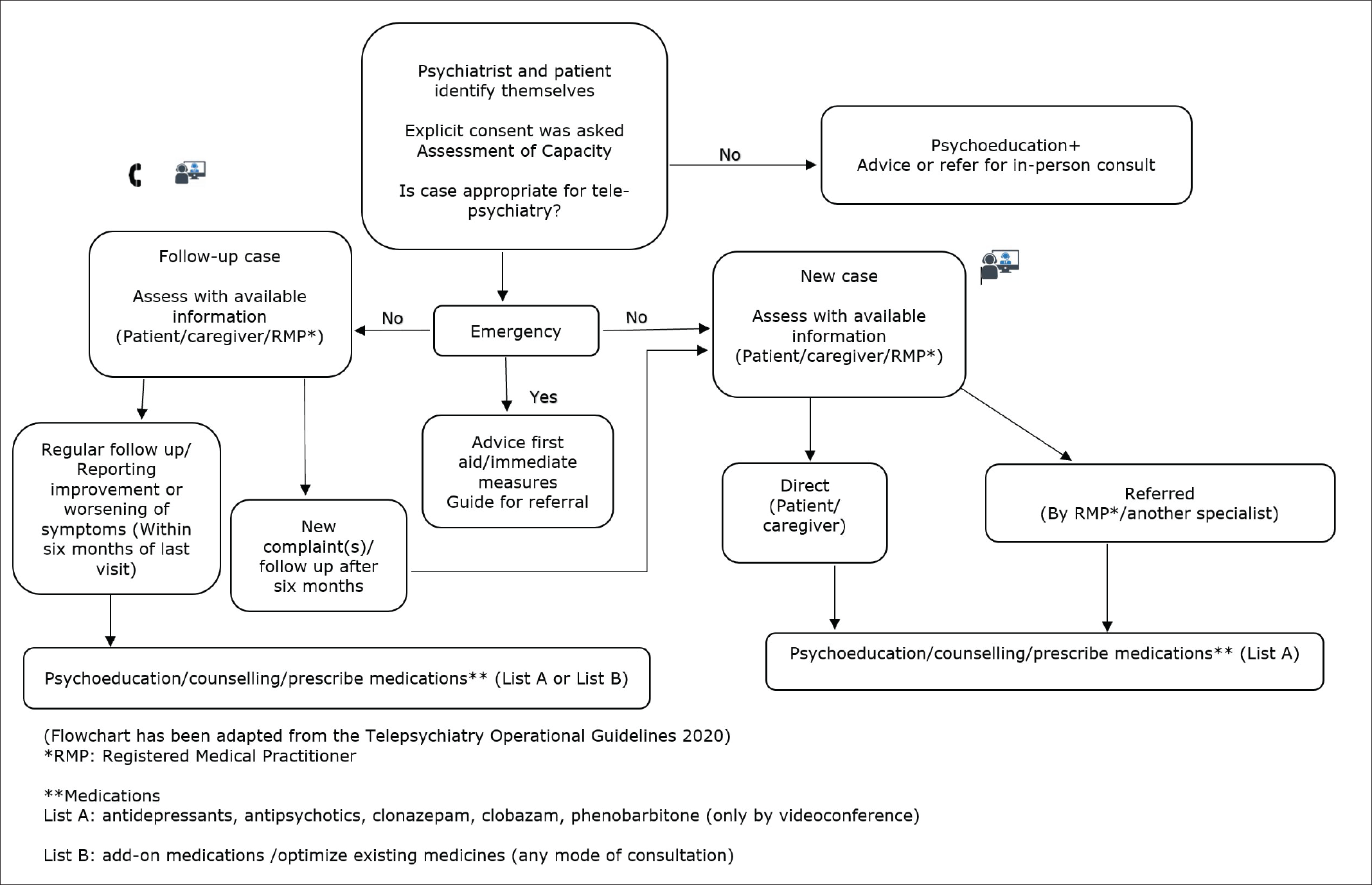
Flowchart Showing Steps of Telepsychiatry Consultations
Characteristics of Telepsychiatry Service Users
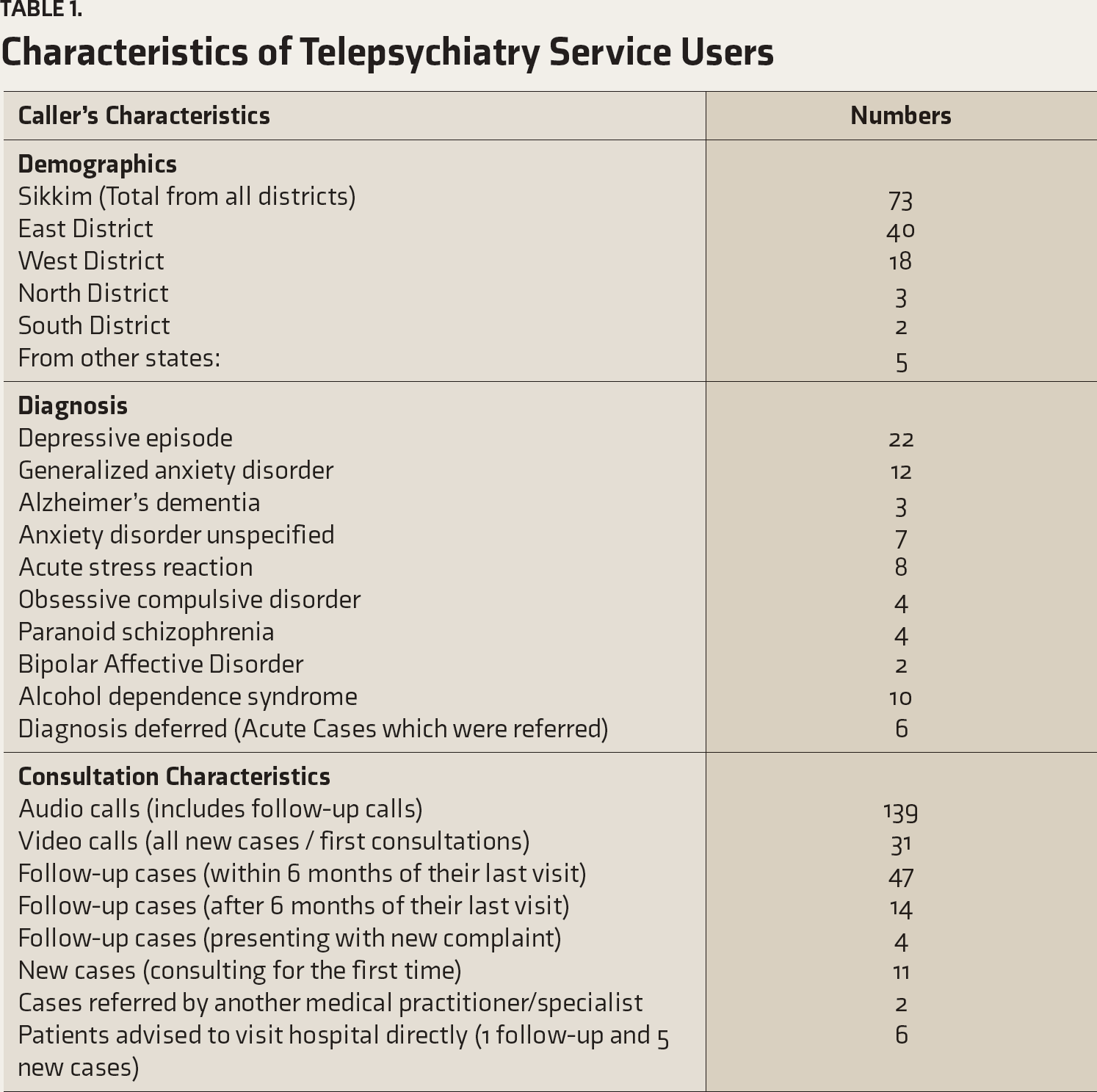
Future Considerations
For telehealth to be effective during the current COVID-19 pandemic and similar future events, it needs to be appropriately integrated into health service and treated as a “business as usual” modality, unless we want to experience the same failure as that of more developed countries who tried implementing it. 8 To make telehealth a mainstream component of the health system, the authors propose the following measures:
Adequate education and training of all health professionals in telemedicine, even consider including it in the curriculum of the trainees.
Initiate telehealth accreditation for health professionals.
Adequate funding to cover the cost of delivering telehealth.
Restructure clinical models of patient care.
Support to all stakeholders with an effective communication and change management strategy
Ascertain systems to manage telehealth services on a regular basis.
Conclusion
The COVID-19 crisis and global pandemic may be the defining moment for digital mental health. One of the definite solutions to continue delivering mental health support within this pandemic from a safe distance is telepsychiatry. According to our preliminary experience, telepsychiatry services are realistically possible and apt to help patients and caregivers not only now during the pandemic but also in the future. This would help to decrease the inflow of regular OPD consultations and hence minimize exposure to novel corona virus now and save transportation and other logistic costs for the patients and their caregivers in the future too.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
