Abstract
In histopathology, the presence of a tissue change that does not represent the tissue’s normal appearance can often lead to an incorrect diagnosis and interpretation. These changes are collectively known as “artifacts” resulting from postmortem autolysis, improper fixation, problems with tissue handling or slide preparation procedures. Most tissue artifacts are obvious, yet some artifacts may be subtle, occur in relatively well-fixed tissue, and demand careful observation to avoid confusion with real biological lesions. The kidney often contains artifacts that may be observed throughout all regions of the renal parenchyma. Cortical tubule artifacts present the greatest challenge when discerning an artifact versus an induced lesion following exposure to a xenobiotic. However, confounding artifacts observed at the tip of the renal papilla may also be problematic for the pathologist. An uncommon artifact involving tinctorial alteration and rarefaction affecting the papillary tip of the rat kidney is described here and differentiated from treatment induced lesions of renal papillary necrosis.
Renal papillary necrosis (RPN) is a serious condition surmised to have contributed to the death of Beethoven in 1827. 1 Renal papillary necrosis may be a consequence to drug abuse of analgesics and nonsteroidal anti-inflammatory drugs but can also be induced in many species of laboratory animals following exposure to a broad range of chemicals and drugs. 2 –4 The identification of RPN has important relevance for clinical risk assessment since many agents that result in RPN in animals have induced RPN in humans under suitable conditions. 5 It is, however, known that certain papillary artifacts may be difficult to distinguish from the early stages of RPN. 6
The rat kidney papillary tip is a relatively small area of simple structure comprised of collecting ducts, medullary interstitial cells, loops of Henle, and capillaries all embedded in a glycosaminoglycan-rich matrix (Figure 1). 2 Papillary epithelium covers the tip of the papilla. 7 Routine sections through the renal papilla can be quite variable. Although it is desirable in rodent toxicology studies to get sections of kidneys which include the tip of the papilla, it is not unusual that one or both kidney sections may be missing the papillary tip (Figure 2).
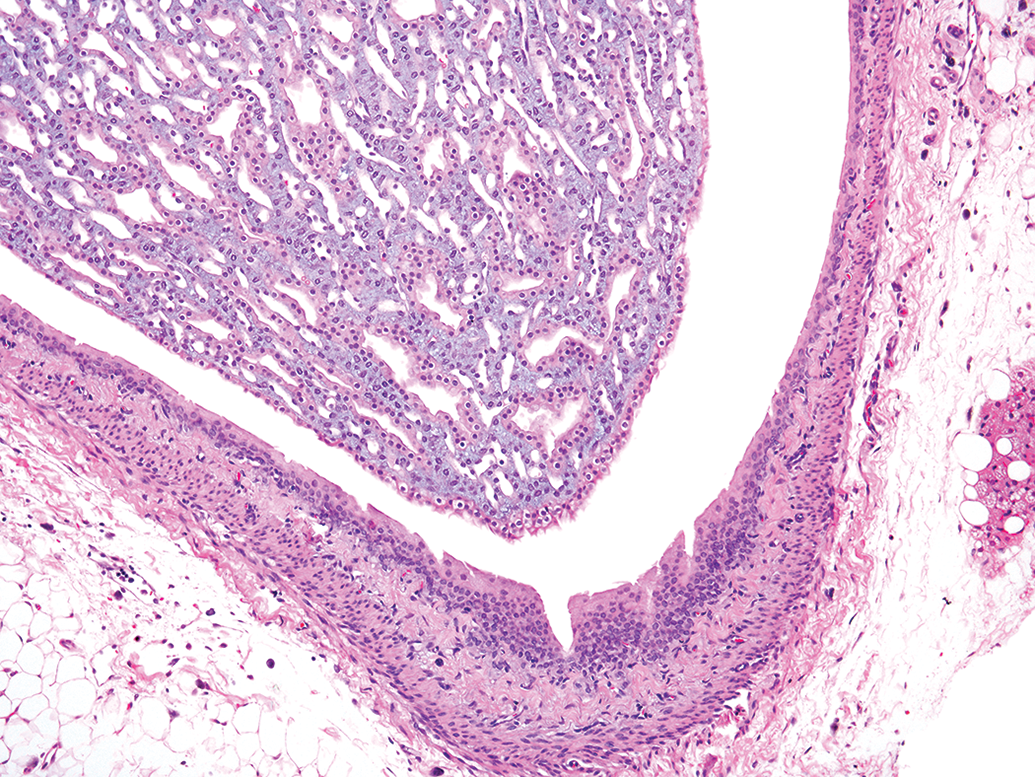
Normal rat renal papillary tip.
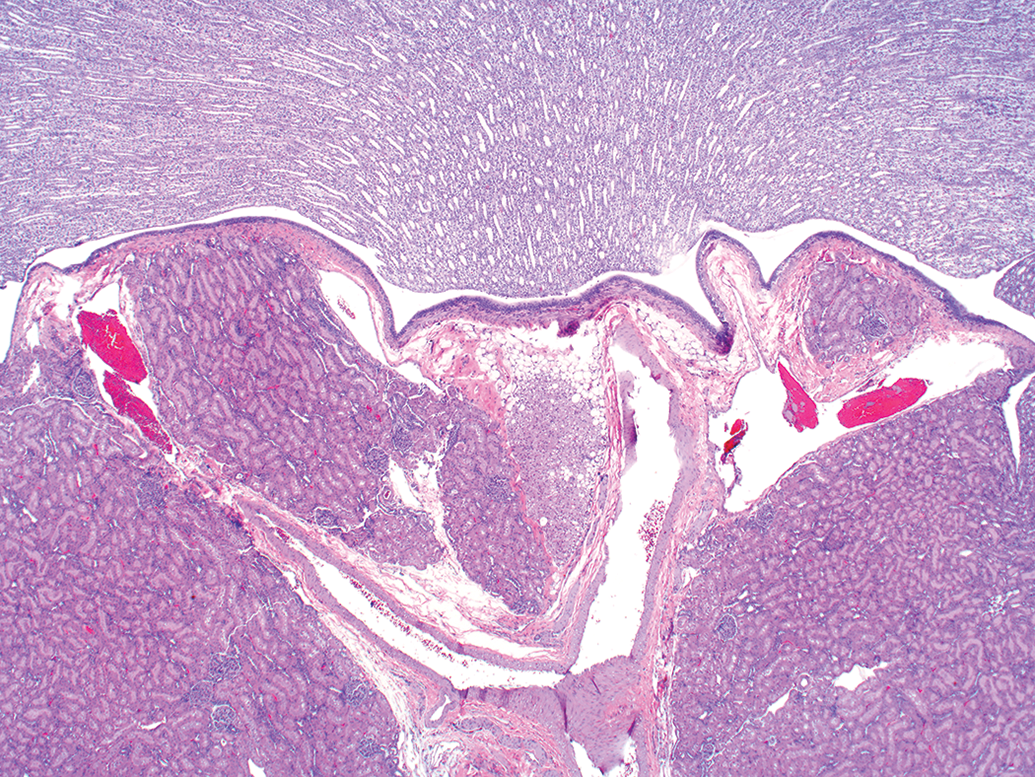
Normal rat missing renal papillary tip due to section variability.
In the early stages of RPN, tissue lesions are restricted to degeneration or necrosis of interstitial cells, small loops of Henle, or small capillaries; interstitial edema or mucoid change; and at a location often limited to or near the papillary tip. 6,8,9 With progression, the lesion tends to involve all components of the papilla with clear evidence of cellular necrosis associated with a spectrum of changes representing expanding vascular injury, the presence of inflammatory cell infiltrates, and degeneration and/or loss of papillary epithelial cells. 10 Unfortunately, cases of early RPN may go unnoticed during the histologic examination due to the missing papillary tip in the renal sections in toxicology studies. 10
Occasionally, during the examination of rodent kidneys from nonclinical studies, pale areas within the papillary tip can be recognized on low-power magnification. These areas appear more frequently in kidneys from animals which have died while on study and often have other renal changes recognized by study pathologists relating to post-mortem autolysis such as the loss of cytoplasmic and nuclear detail, and retraction of tubule cells from basement membranes. 11 However, there are uncommon instances where the kidneys are generally well-fixed from sacrificed animals yet have papillary pale areas in one or both kidneys. These pale renal papillary areas are noted in kidneys from control as well as treated animals and appear morphologically similar without notable time or dose progression. Furthermore, these pale discolored areas contain microanatomical components that abruptly changes their appearance compared to the surrounding tissue in euthanized animals.
Upon closer examination, the renal papilla appears normal except for a washed-out area confined to the papillary tip that can best be described as an area of “rarefaction” (lessening of tissue density; Figures 3 and 4). Other changes, as detailed in Table 1, support the assumption that this change represents an artifact. In contrast, the aforementioned RPN is characterized by a well-demarcated area of degeneration and necrosis involving most cellular components in this area of the papilla. Additional features of RPN include variable findings of hyperemia or small hemorrhages, the presence of necrotic debris, mineralization, and sloughing or loss of papillary epithelium (Figures 5 and 6).
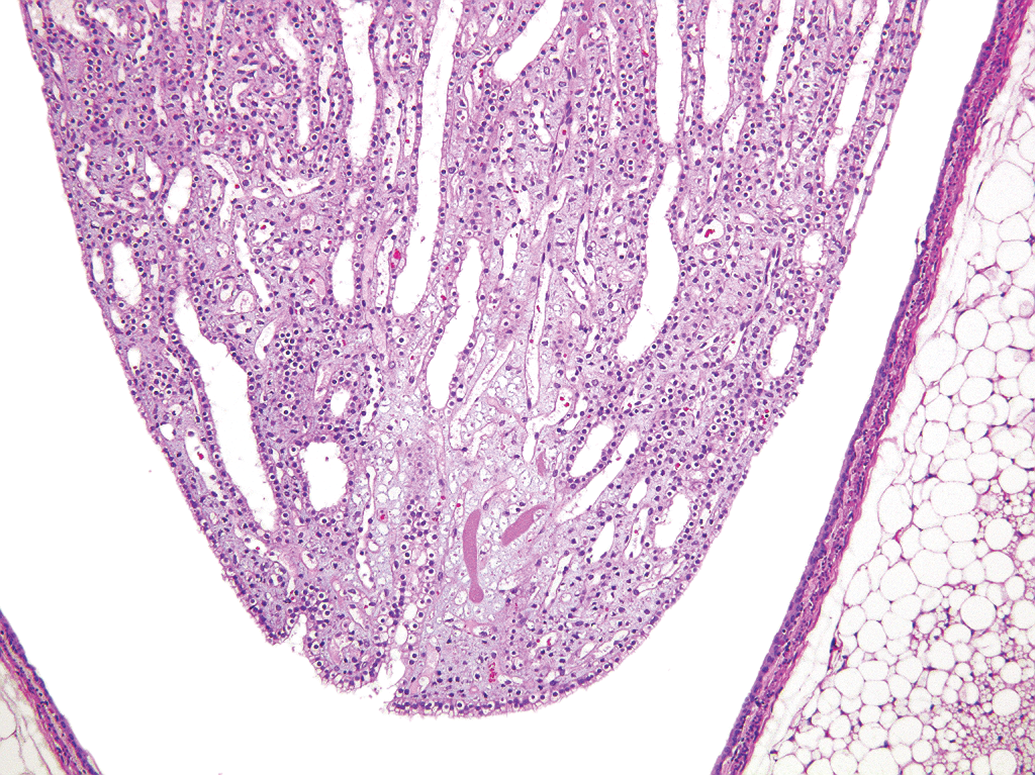
Note pale focal area representing rarefaction with interstitial “ghost cells” in an otherwise normal appearing rat renal papilla.
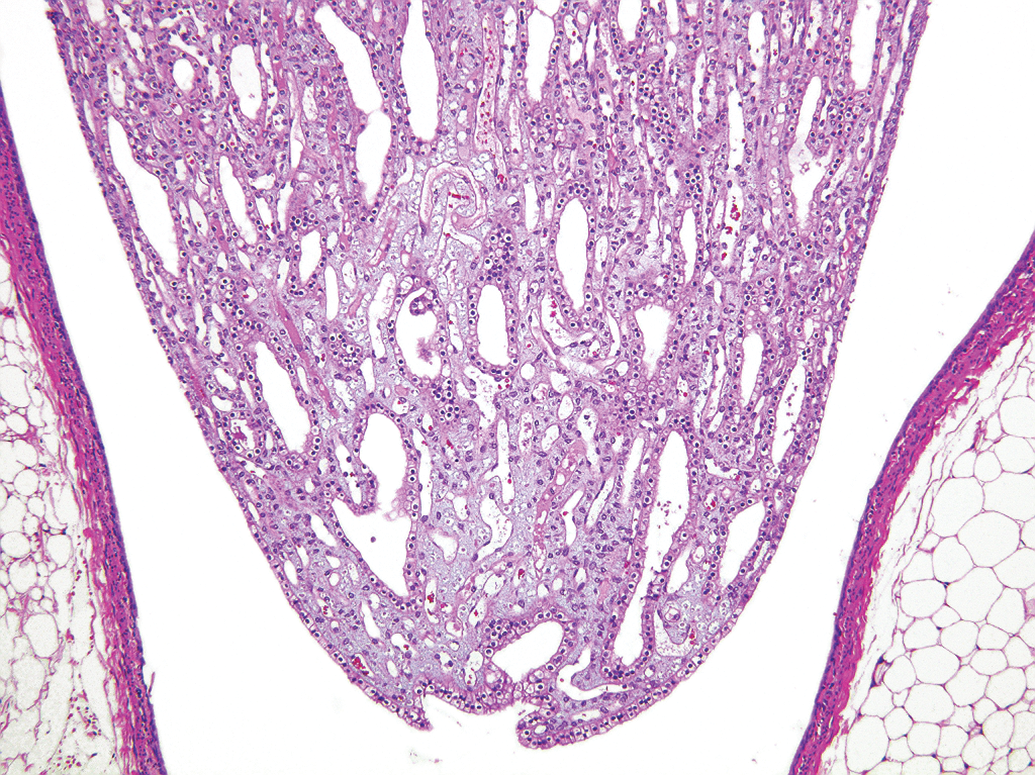
Example of another kidney processed at the same time as the kidney shown in Figure 3 with a similar histological appearance of the renal papilla.
Criteria Associated with Rat Renal Papillary Artifacts Termed “Rarefaction.”

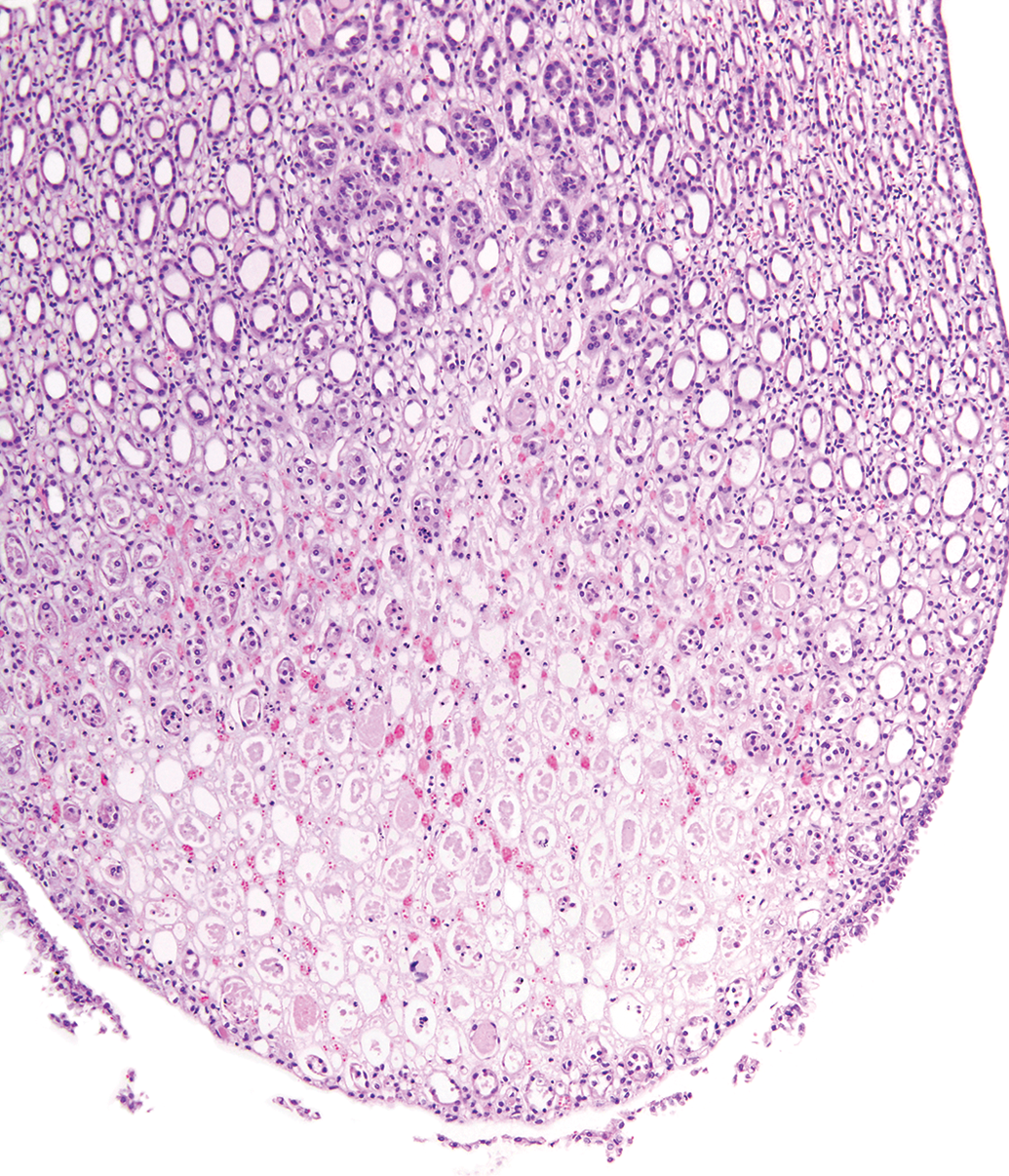
An early stage of RPN in a rat characterized by a well-demarcated area of cellular necrosis involving both collecting ducts and interstitial cells, the presence small hemorrhages, and papillary epithelial sloughing. (Image Courtesy of the US National Toxicology Program.) RPN indicates renal papillary necrosis.
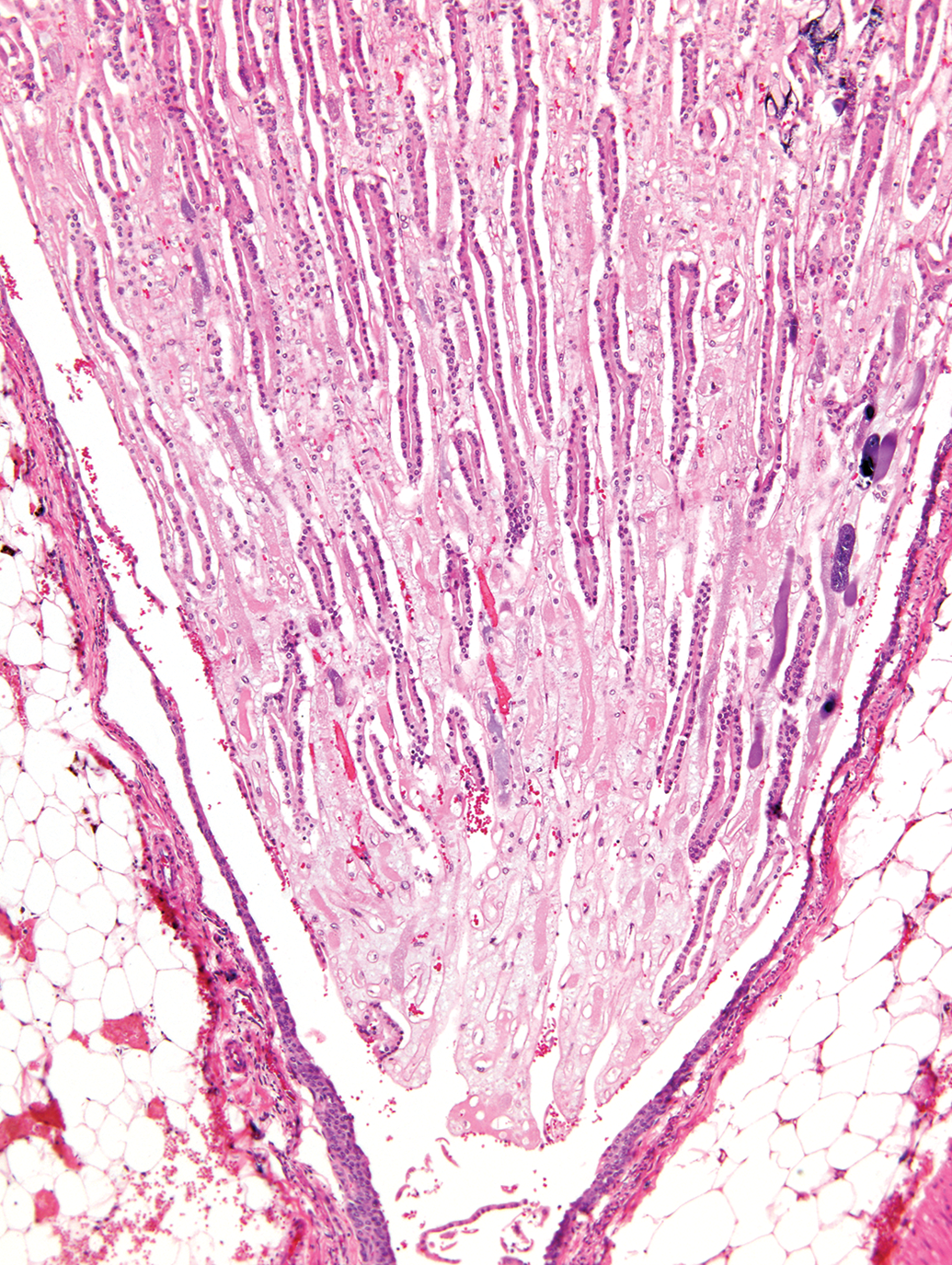
Another kidney with an early stage of RPN in a rat characterized by a well-demarcated area of collecting duct and interstitial cellular necrosis, vascular congestion, dystrophic mineralization, and loss of the papillary epithelium. (Reprinted with permission from Toxicologic Pathology. 10 RPN indicates renal papillary necrosis.
It should be noted that the hallmarks of RPN, discussed and illustrated above, are distinctly lacking within the rarefaction artifact, and that there no associated clinical pathology alterations in urine or clinical chemistry parameters with rarefaction. Furthermore, unlike RPN, there is no apparent progression to degeneration, necrosis, inflammation, mineralization, demarcation, or repair, within rarefaction or an increase in the severity with dose and/or study duration.
Rarefaction is a term used in pathology descriptions which refers to “the condition of becoming less dense”. 12 In light of the totality of histological evidence, the terminology of “rarefaction” seems appropriate in these cases to indicate a change in which the pathogenesis is not known but suspected to represent an artifact. If renal papillary rarefaction is diagnosed, we recommend that the study pathologist provides a compelling argument for why the observed change is consistent with the rarefaction artifact and not a treatment-related change, if the issue becomes important to the overall study findings.
There are many definitions but one that seems to be widely accepted is that artifacts represent any structure, feature, or tissue alteration that has been produced by tissue handling or by the inappropriate processing of a tissue. 13,14 Artifacts can be introduced at any time during necropsy, tissue fixation, tissue trimming, or during histological processing and staining. Therefore, the highest necropsy and histology quality standards should be applied to avoid and minimize tissue artifacts.
The exact cause of the here described papillary rarefaction is not known but loss of cytological detail and staining intensity is just one of the many possible artifacts encountered during the preparation of microscopic tissue slides. 11,13 Rarefaction could also represent one of the earliest changes associated with postmortem autolysis since the rodent papillary tip caps the end of a single (unipapillate) long papilla supported by a poor blood supply compared to humans (multipapillate). Therefore, it is not surprising that one of the main differential diagnoses of RPN is autolysis. 10
In summary, we are describing an uncommon renal artifact that can be very subtle and its interpretation requires the knowledge of experienced pathologists who understand the spectrum of variation seen in processed renal tissues and who are able to distinguish artifactual alterations from treatment induced lesions. 15 Pathology texts often do not contain discussions or illustrations of unusual tissue artifacts. Therefore, it is important to bring difficult diagnostic observations like the described rat renal papillary rarefaction to the attention of veterinary pathologists, reading or reviewing nonclinical rodent studies.
Footnotes
Acknowledgments
The authors are grateful to Michelle McCrimmon for reference retrieval, Emily Singletary for image support, and Donna Turner for manuscript preparation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
