Abstract
Determination of test material-induced cutaneous phototoxicity for risk assessment has traditionally been based on visually observed skin reactions such as erythema, edema, and flaking. Because of its role in determining a toxic effect, the use of histopathological evaluation in this determination arises from time to time. However, there is little published information regarding the time course and types of histopathologic changes in the skin after test material-induced phototoxic insult nor any regulatory requirement or precedent for its use. This work evaluated both the visual and histopathological time course of the phototoxic response of the skin of the Long-Evans rat after oral administration of the phototoxins sparfloxacin and 8-methoxypsoralen (MOP) followed by a single exposure to solar-simulated ultraviolet radiation. Both sparfloxacin and 8-MOP elicited visual cutaneous reactions and microscopic changes consistent with a phototoxic response. The visually observed cutaneous time course and elicited histopathologic changes differed in response and extent for each phototoxin, but in both instances, microscopic evaluation did not alter the determination of a phototoxic response based on visual observations. These results indicate that, though histopathologic evaluations may have value for investigating mechanisms of phototoxicity, histopathologic evaluation of the skin is not warranted for determination of phototoxic potential in safety assessment intended for regulatory submission.
Introduction
Phototoxicity is an important component of preclinical drug development, and the determination of a cutaneous phototoxic response to a test material in combination with exposure to ultraviolet radiation (UVR) has traditionally been based on visually observed end points such as erythema, edema, and flaking. While histopathology is a classic tool in evaluating a toxic effect on a tissue, histopathological evaluation of the skin (the primary phototoxicity target tissue) is not included as a criterion for evaluation of phototoxicity in the U.S. Department of Health and Human Services, Food and Drug Administration. Notice Photosafety Evaluation of Pharmaceuticals (2015), the U.S. Department of Health and Human Services, Food and Drug Administration. Notice Note for Guidance of Nonclinical Safety Studies for the Conduct of Human Clinical Trials and Marketing Authorization of Pharmaceuticals (2010a), or the U.S. Department of Health and Human Services, Food and Drug Administration. Notice Nonclinical Evaluation for Anticancer Pharmaceuticals (2010b), all of which define the current regulatory state of photosafety assessments. The genesis of this work was the occasional request for histopathologic evaluation of the skin in preclinical photosafety studies, and the purpose was to determine whether histopathological examination of skin reactions in phototoxicity studies provided additional information for determining the phototoxic potential of test materials for safety assessment. The results of this evaluation using 2 recognized human phototoxins indicated that, though histopathological examination provided meaningful information on the pathology caused by the phototoxic response and could contribute to understanding mechanisms of phototoxicity, it did not add critical information for the determination of a phototoxic response required for photosafety assessment. Inclusion of histopathologic evaluation may add unnecessary complication for data interpretation and is not recommended in photosafety assessments.
Materials and Methods
All works described here involving the care and use of animals were reviewed and approved by the Institutional Care and Use Committee of the Testing Facility.
Animals
Female Crl: Long-Evans (LE) rats were obtained from Charles River Laboratories, NC, and were approximately 12 to 15 weeks of age and approximately 251 g to 275 g at receipt. Fifteen rats/group were assigned to study and socially housed (3/cage) throughout the study using solid bottom caging, corn cob bedding, and shredded paper. Rats were provided commercial certified rodent diet and reverse osmosis membrane water ad libitum. Rats were selected for study based on overall clinical condition, body weight, and skin pigmentation pattern. To delineate the UVR exposure sites, hair was clipped from the back of each rat and a mark was tattooed on the pigmented and nonpigmented skin; the exposure site was caudal to each mark.
Formulation
Sparfloxacin (SigmaAldrich, St. Louis, MO) was prepared daily in 0.5% methylcellulose (400 centipoise, Spectrum Chemical, New Brunswick, NJ) in reverse osmosis membrane deionized water. 8-Methoxypsoralen (MOP; SigmaAldrich, St. Louis, MO) was prepared in corn oil (MP Biomedicals, Santa Ana, CA). The administered doses were 15 mg/kg/day (1.5 mg/ml) for 8-MOP and 150 mg/kg/day (15 mg/ml) for sparfloxacin, at a dose volume of 10 ml/kg. The doses used are those used in sponsored studies and based on data that demonstrate consistent responses at these doses (Dougherty et al. 2013). All formulations were administered to the rats by oral gavage once daily for 3 consecutive days.
UVR Exposure
On the day of UVR exposure (day 3 of study), hair was removed from the backs of the rats before the final formulation administration. After formulation administration, the rats were lightly anesthetized with an intramuscular injection of a mixture of ketamine (50 mg/kg, Henry Schein Animal Health, Dublin, OH) and xylazine (5 mg/kg, Alkorn, Inc., Lake Forest, IL). The rats were restrained and an aluminum foil mask with 2 circular holes, each with a diameter of 1.3 cm, defined the exposure sites on the pigmented and nonpigmented skin sites in the mid-dorsal area. The remaining clipped skin and the eyes of the rats were shielded from UVR exposure using aluminum foil. To minimize irritation during UVR exposure, the eyes of the rats were lubricated with a sterile ophthalmological solution at least once before, immediately after, and 30 ± 5 min following exposure. Rats were monitored until recovery from anesthesia.
UVR Source
The UVR source was a 6.5 kW long-arc xenon water-cooled lamp equipped with a 4-mm thick Schott WG 320 filter. A representative spectrum of the UVR source is included as Figure 1. A dose of 10 J/cm2 of ultraviolet A radiation and 140 mJ/cm2 of ultraviolet B radiation was delivered to each rat over a period of 42 min. The UVR doses were calculated based on absolute power spectrophotometric measurements using a U.S. Food and Drug Administration (FDA) 21 CFR Part 11-validated OL756 High Accuracy UV-visible spectroradiometer (Optronics Laboratories, Orlando, FL), and the incident UVR was monitored using a custom U.S. FDA 21 CFR part 11-validated radiometry monitoring system.
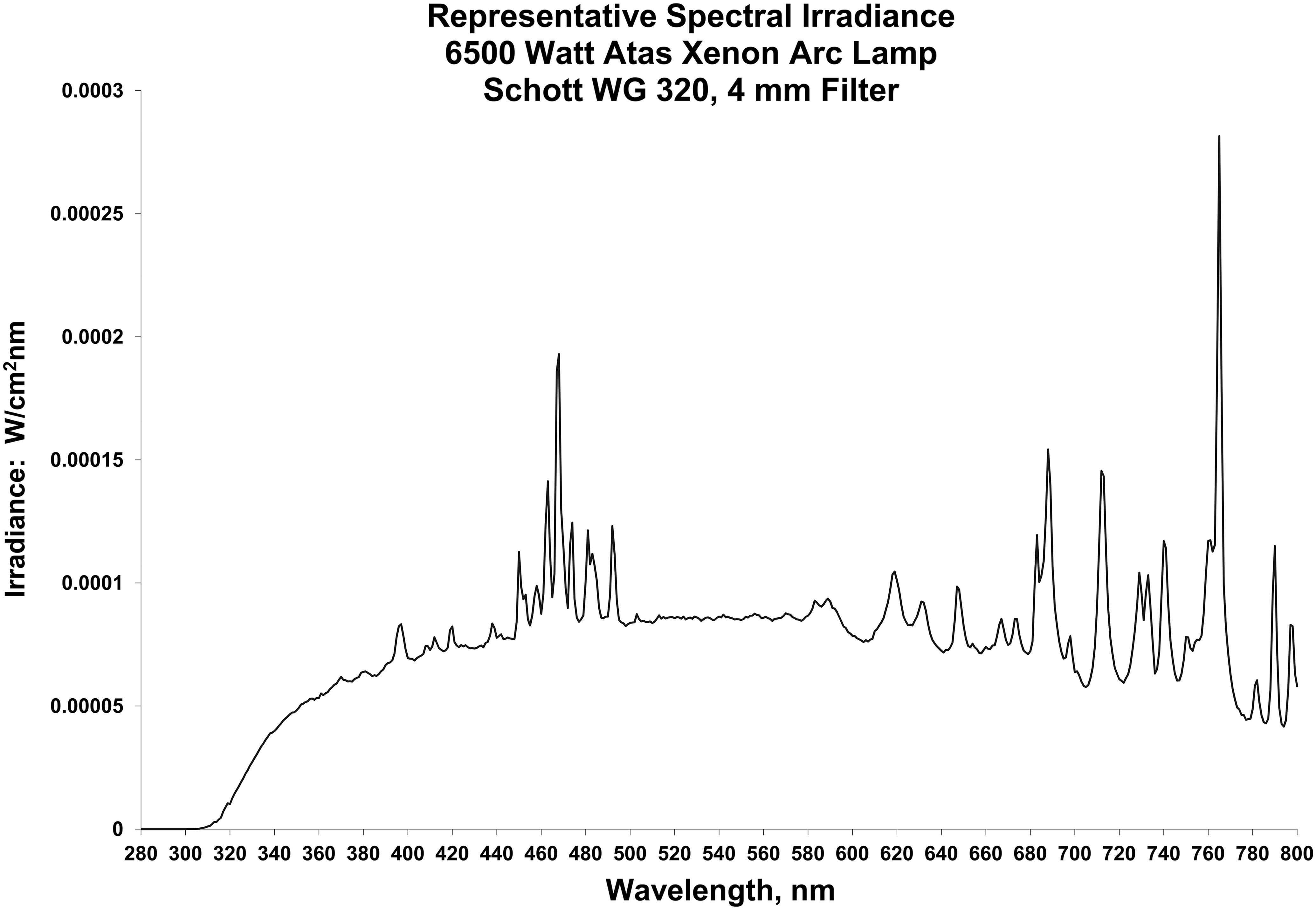
Xenon arc solar simulator spectral distribution.
Clinical and Skin Reaction Observations
Skin reactions observed in the exposed skin sites (erythema grade 1: barely perceptible light redness, erythema grade 2: distinct redness, edema grade 1: raised <1 mm, edema grade 2: raised 1 mm to 2 mm) were recorded approximately 15 min and 4 hr after the end of exposure on the day of exposure and then approximately 24, 48, and 72 hr after exposure. Severity of the skin reactions was evaluated by the use of mean sum of scores (MSS), a convenient semiquantitative measure of severity of the elicited reactions for each phototoxin at each time point. Clinical observations and body weights were recorded daily during administration and post-UVR exposure. No adverse clinical observations other than the discussed skin responses or body weight effects were recorded during the study. Group mean body weight loss occurred on the day after UVR exposure, which is a known response of the rats to anesthesia and restraint used for UVR exposure and not considered adverse.
Postmortem Tissue Processing and Histopathologic Evaluation
Rats (3/group) were euthanized by carbon dioxide asphyxiation at each time point after observations were completed and the dorsal skin including the UVR exposure sites was removed and fixed in 10% neutral buffered formalin. Subsections of skin (approximately 1 cm × 0.5 cm) were removed from the exposure sites, embedded in paraffin, processed to slides, and stained using hematoxylin and eosin. Histopathologic evaluation was performed by a board-certified pathologist. Unexposed skin (pigmented and unpigmented) was processed to slide and used to establish baseline microscopic anatomy end points. Microphotographs of exposed skin were generated using Aperio®-scanned images.
Results
Skin Reactions
Skin reactions were not elicited in the group administered the sparfloxacin vehicle and exposed to UVR alone, allowing interpretation of any reaction elicited by an administered formulation to be evaluated without any background reaction to UVR exposure alone. Both 8-MOP and sparfloxacin elicited skin reactions, demonstrating their utility as positive control articles at these doses in phototoxicity studies. However, the time of the responses, the proportion of erythema and edema responses, and the severity of the responses differed between the two phototoxins. Sparfloxacin elicited primarily erythema, with the reactions occurring as early as 1 hr after UVR exposure (Table 1). In comparison, 8-MOP elicited both erythema and edema, but the reactions were first observed 24 hr after UVR exposure (Table 1).
Time Course of Skin Reactions.
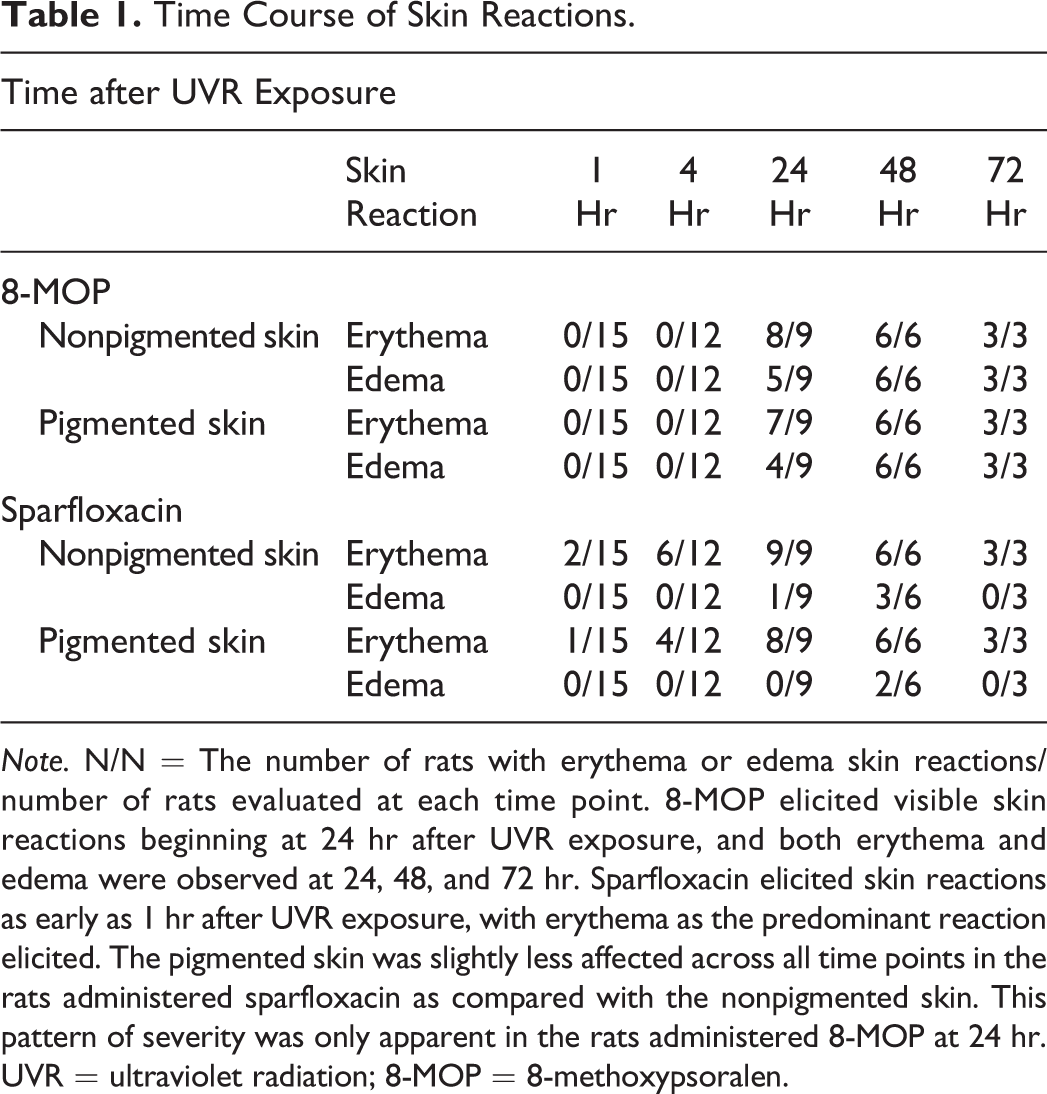
Note. N/N = The number of rats with erythema or edema skin reactions/number of rats evaluated at each time point. 8-MOP elicited visible skin reactions beginning at 24 hr after UVR exposure, and both erythema and edema were observed at 24, 48, and 72 hr. Sparfloxacin elicited skin reactions as early as 1 hr after UVR exposure, with erythema as the predominant reaction elicited. The pigmented skin was slightly less affected across all time points in the rats administered sparfloxacin as compared with the nonpigmented skin. This pattern of severity was only apparent in the rats administered 8-MOP at 24 hr. UVR = ultraviolet radiation; 8-MOP = 8-methoxypsoralen.
The severity of the responses was greater in the rats administered 8-MOP as measured by the extent of the skin reactions in the exposed skin, as compared with the reactions elicited by sparfloxacin. This severity is reflected in the MSS, a convenient semiquantitative measure of the visual observations for each phototoxin and time point (Tables 2 –4). For all rats evaluated at each time point (Table 2), the MSS show the increased severity of the 8-MOP responses, as compared with the sparfloxacin responses. For both phototoxins, the peak of severity was 48 hr after UVR exposure. This response pattern is also demonstrated by the MSS of the 3 rats evaluated histopathologically at each time point (Table 3) and the MSS of the 3 rats over time in each group that were evaluated at 72 hr (Table 4), demonstrating the consistency of the responses across all rats in each group.
Mean Sum of Skin Reaction Scores of All Rats Evaluated at Each Time Point.
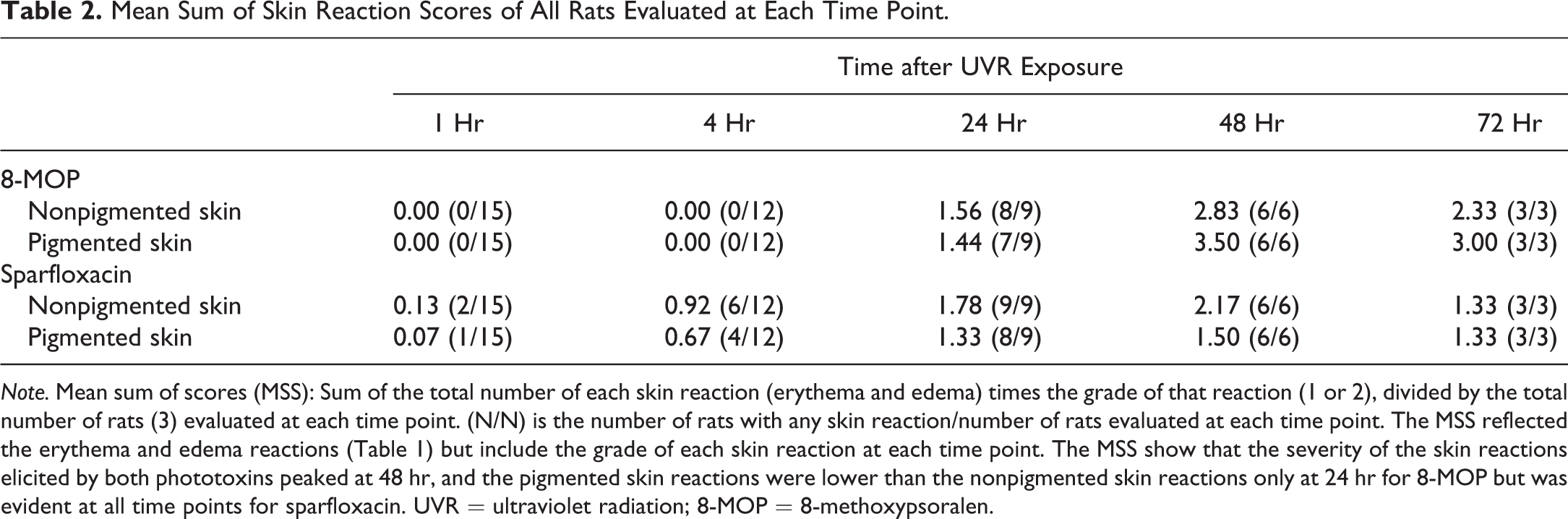
Note. Mean sum of scores (MSS): Sum of the total number of each skin reaction (erythema and edema) times the grade of that reaction (1 or 2), divided by the total number of rats (3) evaluated at each time point. (N/N) is the number of rats with any skin reaction/number of rats evaluated at each time point. The MSS reflected the erythema and edema reactions (Table 1) but include the grade of each skin reaction at each time point. The MSS show that the severity of the skin reactions elicited by both phototoxins peaked at 48 hr, and the pigmented skin reactions were lower than the nonpigmented skin reactions only at 24 hr for 8-MOP but was evident at all time points for sparfloxacin. UVR = ultraviolet radiation; 8-MOP = 8-methoxypsoralen.
Mean Sum of Skin Reaction Scores Over Time for the Three Rats Evaluated at Each Time Point.
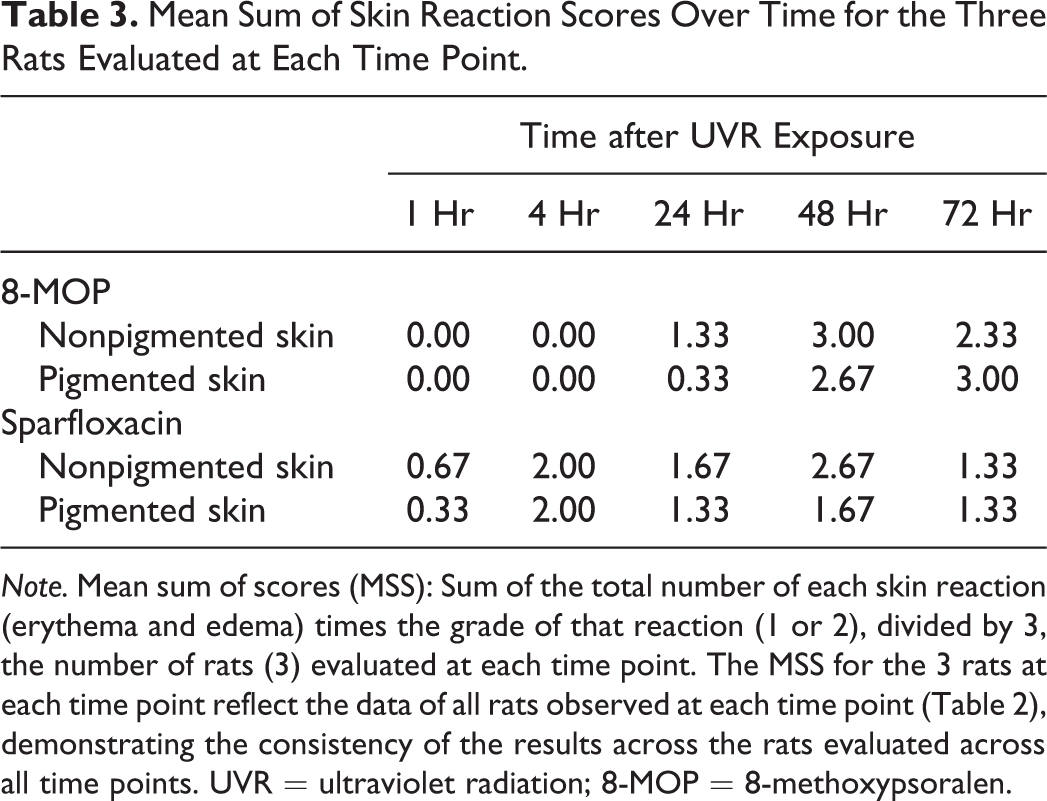
Note. Mean sum of scores (MSS): Sum of the total number of each skin reaction (erythema and edema) times the grade of that reaction (1 or 2), divided by 3, the number of rats (3) evaluated at each time point. The MSS for the 3 rats at each time point reflect the data of all rats observed at each time point (Table 2), demonstrating the consistency of the results across the rats evaluated across all time points. UVR = ultraviolet radiation; 8-MOP = 8-methoxypsoralen.
Mean Sum of Skin Reaction Scores Over Time for the Three Rats Histopathologically Evaluated at 72 Hr.
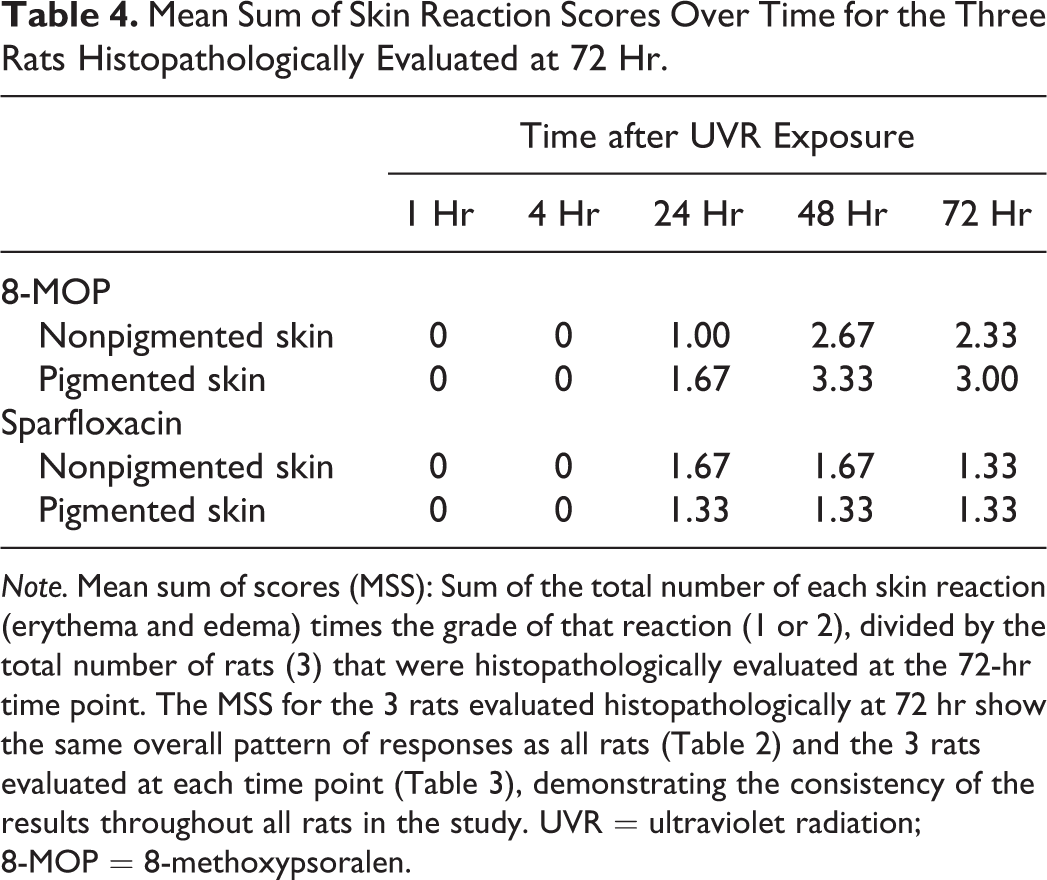
Note. Mean sum of scores (MSS): Sum of the total number of each skin reaction (erythema and edema) times the grade of that reaction (1 or 2), divided by the total number of rats (3) that were histopathologically evaluated at the 72-hr time point. The MSS for the 3 rats evaluated histopathologically at 72 hr show the same overall pattern of responses as all rats (Table 2) and the 3 rats evaluated at each time point (Table 3), demonstrating the consistency of the results throughout all rats in the study. UVR = ultraviolet radiation; 8-MOP = 8-methoxypsoralen.
The LE rat is used in this assay in part because of the concern that melanin binding could affect a phototoxic reaction (Hamanaka et al. 1999; U.S. Department of Health and Human Services, Food and Drug Administration. Notice 2015). However, the conventional thinking is that melanin is protective against UVR-induced damage. The rats administered sparfloxacin demonstrated a slightly lower extent of reaction in the pigmented skin sites across all time points as compared with the nonpigmented skin sites (Tables 2 –4). In the rats administered 8-MOP, a lesser effect in the pigmented skin sites was only apparent at 24 hr; at 48 had 72 hr, the MSS were higher in the pigmented skin sites. The reason(s) for this seemingly inconsistent reaction pattern is not known.
Histopathology
Unless otherwise noted, there was no difference in the findings of the nonpigmented and pigmented skin (Figure 2). Histopathological evaluation of the skin of rats administered the sparfloxacin vehicle demonstrated essentially normal LE rat dermal microarchitecture (Figure 3). In the group administered 8-MOP, at 1 hr and 4 hr after exposure, no pathological findings were recorded. Twenty-four hours after UVR exposure, in 3 of the 3 animals, mild, epidermal single cell necrosis and minimal-to-mild mixed inflammatory cell dermal infiltrates were observed (Figure 4). Forty-eight hours after UVR exposure, moderate mixed inflammatory cell dermal infiltrates and moderate-to-marked ulceration, minimal-to-moderate dermal and/or epidermal edema, minimal-to-moderate epidermal infiltrates of neutrophils (pustules), mild-to-moderate epidermal necrosis, and minimal dermal hemorrhage were also observed (Figure 5). Seventy-two hours after UVR exposure, the findings were the same as those seen on day 2, with the additional finding of minimal regeneration of the epidermal epithelium (Figure 6). The regenerating epidermis indicates that the lesions, while severe, had the potential for healing.
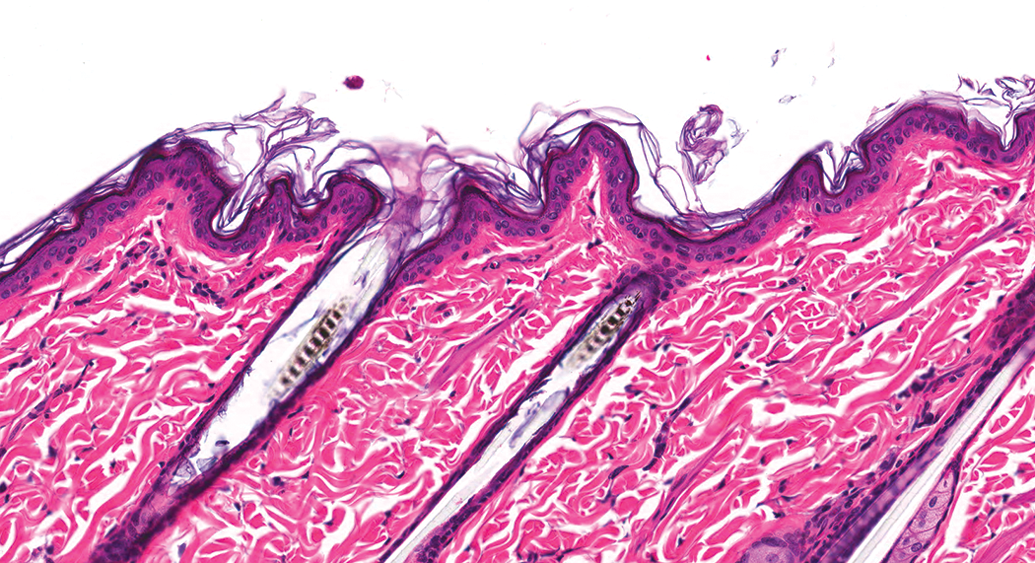
Normal (unirradiated) Long-Evans rat skin (pigmented skin). This image is of pigmented skin and, other than the presence of melanin in the hair shafts and melanocytes in the basilar epidermis, is similar to that of unpigmented skin. Hematoxylin and eosin, original objective used was 20×.
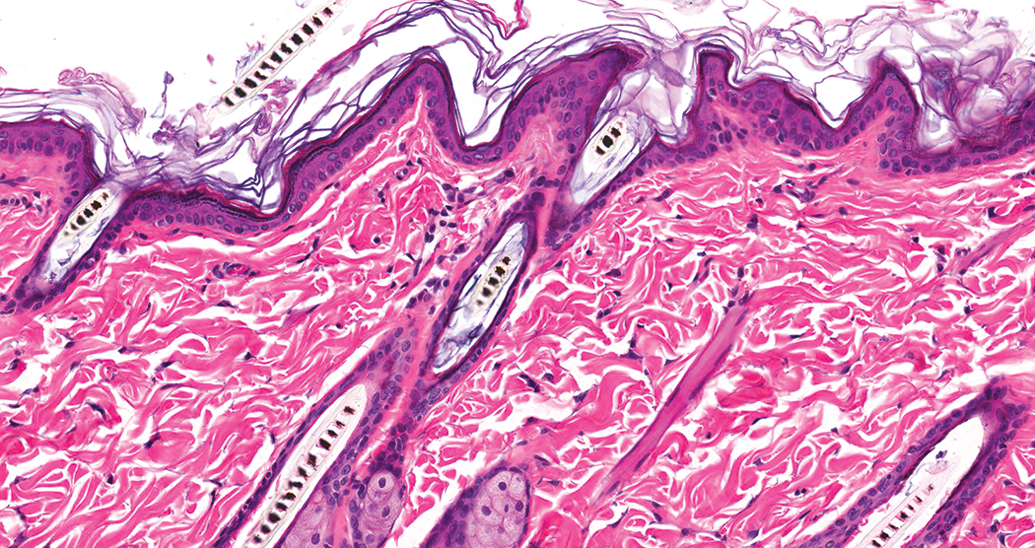
Sparfloxacin vehicle, day 4 (pigmented skin). There is very little difference in microarchitecture as compared with the unirradiated illustrated in Figure 2. Hematoxylin and eosin, original objective used was 20×.
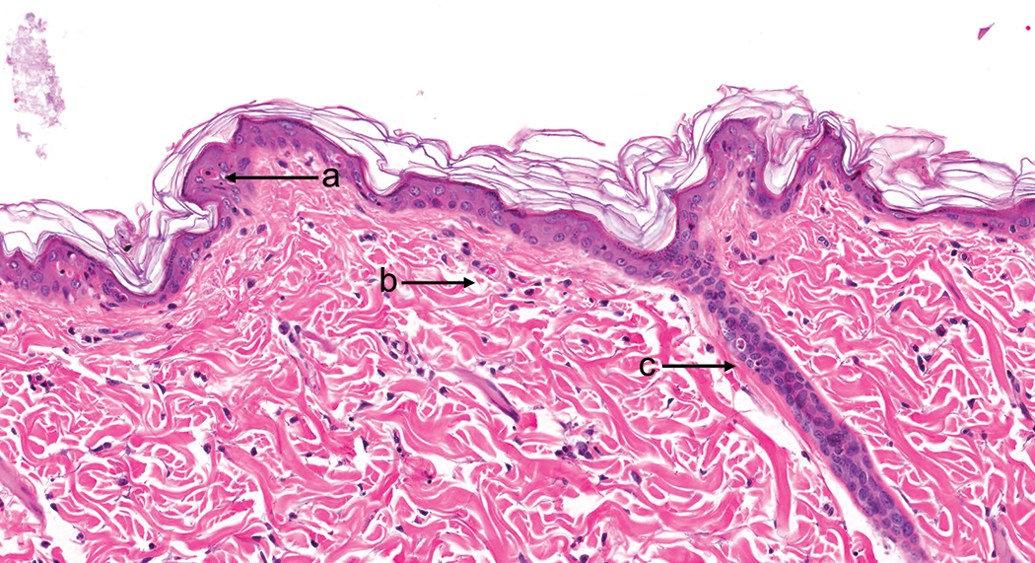
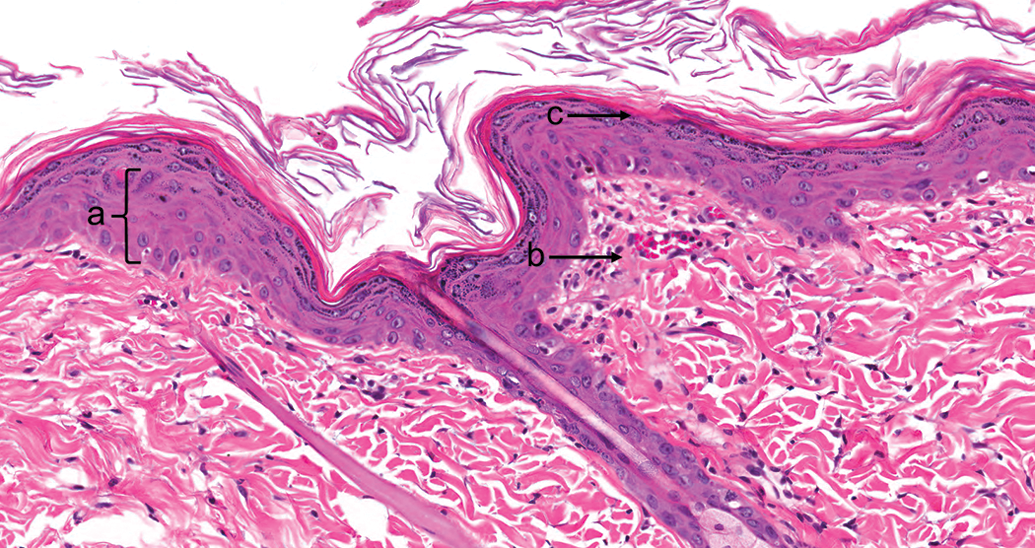
8-Methoxypsoralen, 24 hr after ultraviolet radiation exposure (nonpigmented skin). (a) “Sunburn cell” or apoptotic keratinocyte. (b) Dermal edema and congestion with minimal inflammatory cell infiltrate in the dermis. (c) Epidermal changes, including an apoptotic keratinocyte, extend down the hair follicle. Hematoxylin and eosin, original objective used was 20×.
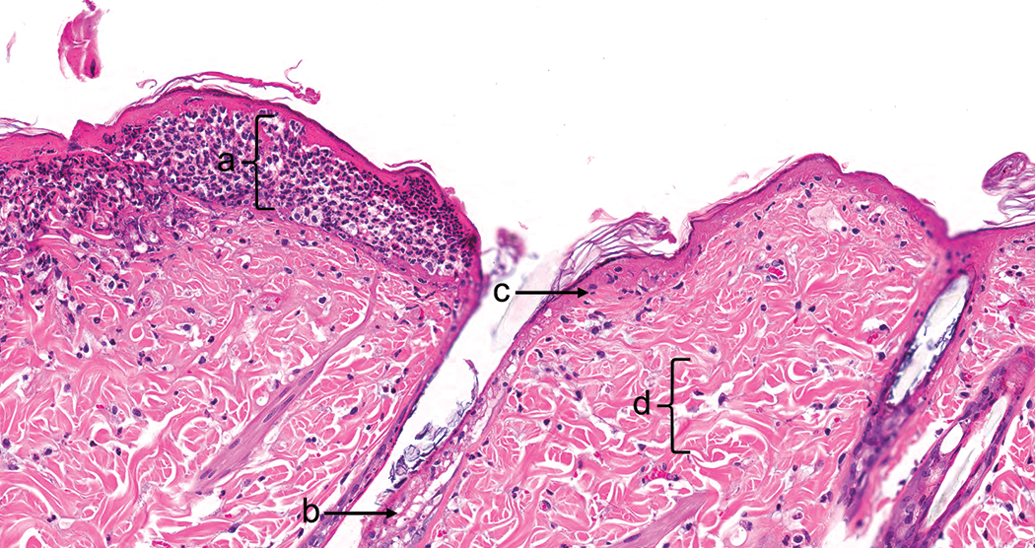
8-Methoxypsoralen, 48 hr after ultraviolet radiation exposure (pigmented skin). (a) Epidermal neutrophil aggregates. (b) Epidermal necrosis in the hair follicle. (c) Epidermal necrosis. (d) Dermal edema and congestion with minimal inflammatory cell infiltrate in the dermis. Hematoxylin and eosin, original objective used was 20×.
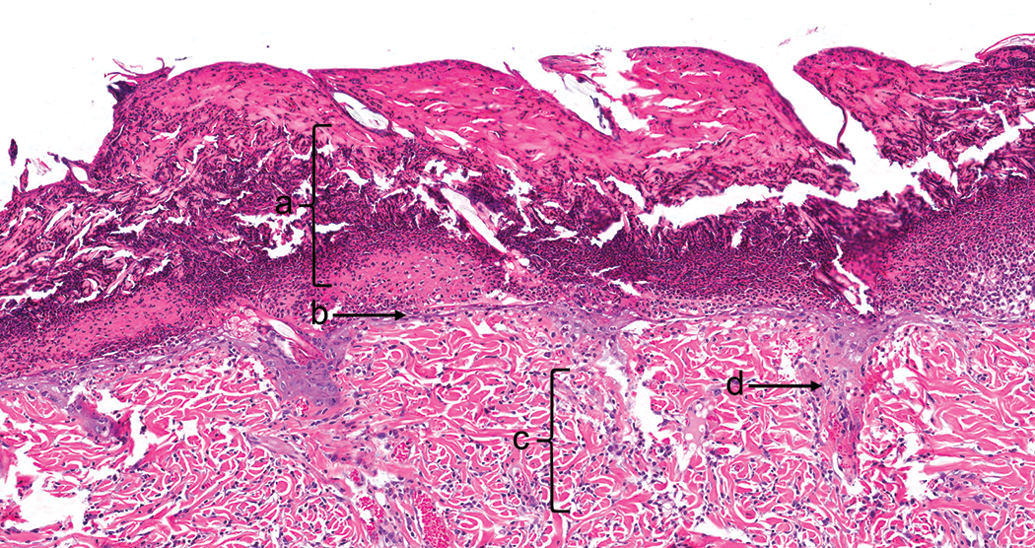
8-Methoxypsoralen, 72 hr after ultraviolet radiation exposure (pigmented skin). (a) Epidermal necrosis with sloughing and necrotic debris. (b) Epidermal regeneration. (c) Dermal edema, minimal inflammatory cell infiltrate, and congestion. (d) Epidermal proliferation extending into the dermis, presumed a hair follicle. Hematoxylin and eosin, original objective used was 20×.
In the group administered sparfloxacin, at 1 and 4 hr after UVR exposure, there were no pathological findings. Fluoroquinolones are known to elicit early reactions, as compared with other phototoxins (Testing Facility experience); however, the rats that showed erythema responses at 1 and 4 hr were not assigned for histopathological evaluation at these time points. Twenty-four hours after UVR exposure, mild epidermal hyperplasia and hyperkeratosis were observed, along with minimal edema, congestion, and mixed inflammatory cell infiltrates in the dermis (Figure 7). In one rat, minimal erosions, single cell necrosis, protein droplets in keratinocytes, and rare neutrophils in the epidermis were noted in the nonpigmented skin. Forty-eight hours after UVR exposure, minimal-to-mild epidermal hyperplasia, hyperkeratosis, and minimal mixed inflammatory cell dermal infiltrates with edema and congestion were observed (Figure 8). In one rat, minimal multifocal ulceration was noted in the nonpigmented skin. Seventy-two hours after UVR exposure, minimal epidermal hyperplasia and hyperkeratosis, edema and congestion in the dermis, and mixed inflammatory cell dermal infiltrates were observed (Figure 9).
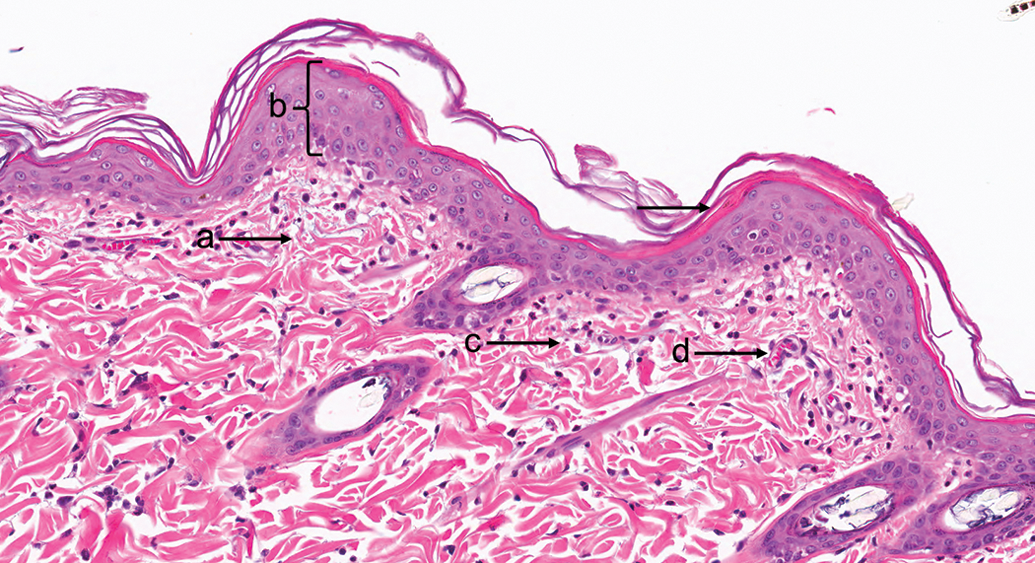
Sparfloxacin, 24 hr after ultraviolet radiation exposure (pigmented skin). (a) and (c) Dermal edema and congestion. (b) Epidermal hyperplasia. (d) Capillary congestion. Hematoxylin and eosin, original objective used was 20×.
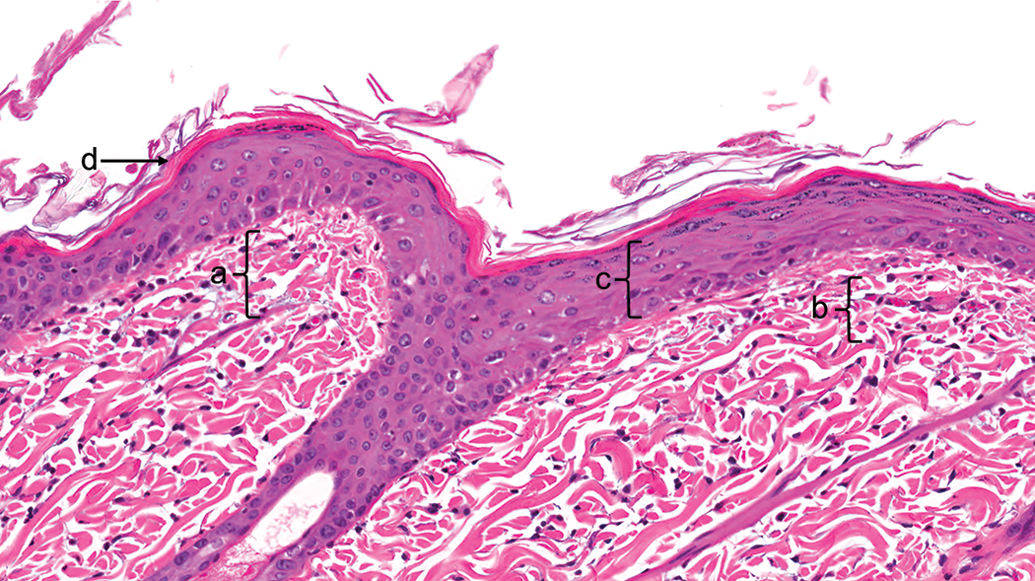
Sparfloxacin, 48 hr after ultraviolet radiation exposure (nonpigmented skin). (a) Dermal edema and minimal inflammatory cell infiltrate. (b) Capillary congestion. (c) Epidermal hyperplasia. (d) Hyperkeratosis. Hematoxylin and eosin, original objective used was 20×.
Sparfloxacin, 72 hr after ultraviolet radiation exposure (pigmented skin). (a) Epidermal hyperplasia. (b) Dermal edema, minimal inflammatory cell infiltrate, and congestion. (c) Hyperkeratosis. Hematoxylin and eosin, original objective used was 20×.
These findings correlate with the visual observations, in that the effects in the group administered 8-MOP were most severe as measured by both MSS and microscopic changes. Some level of regeneration of epidermal epithelium was present in the skin of rats administered 8-MOP at 72 hr, reflecting a possible healing process and suggesting, even with the degree of damage observed, that recovery was possible. The histopathological changes in the skin of rats administered sparfloxacin presumably reflected a different mechanism of phototoxic damage, as compared with the 8-MOP damage, most prominently the degree of epidermal necrosis elicited by 8-MOP, as compared with the epidermal hyperplasia and hyperkeratosis elicited by sparfloxacin. Further evaluation of dose response and/or cellular markers of damage is needed to better evaluate these differences.
Discussion
The work presented here demonstrates that, though histopathologic evaluation of phototoxic skin reactions is useful for the overall description of the reactions and mechanistic interpretation, it does not provide additional information in defining these reactions for safety assessment over and above that which is provided by visual evaluation alone. Along with standard histopathologic evaluation of hematoxylin and eosin–stained skin, any of the well-described markers of cellular and genetic damage (e.g., apoptosis, scheduled and unscheduled DNA repair, p53 activation, comet assay, etc.) have utility in determining mechanisms of UVR damage and recovery, and any resultant exacerbation and/or changes wrought by test materials. While these tools are useful when investigating the mechanisms of this damage and recovery, they lend little to the interpretation of a phototoxic response over that provided by visual evaluation alone. The two phototoxins chosen were based on the Testing Facility’s experience with them as positive control articles in regulated studies. Both of these phototoxins have been well defined as both preclinical and clinical literature that document their clinical and mechanistic background based on visual observation. For example, the publications that established preclinical photosafety testing (e.g., Sambuco et al. 1984), as did work ranking the relative clinical photosafety risk of fluoroquinolones (Dawe et al. 2003), used clinical observations without microscopic evaluation of the induced lesions. That the current U.S. Department of Health and Human Services, Food and Drug Administration. Notice (2010a), U.S. Department of Health and Human Services, Food and Drug Administration. Notice (2010b), and U.S. Department of Health and Human Services, Food and Drug Administration. Notice (2015) guidances, along with the preceding European Medicines Agency (2002) and FDA (2003) photosafety guidance documents, do not mention histopathologic evaluation as part of either preclinical or clinical assessment of phototoxic skin, further argues against the use of histopathologic evaluations for safety assessments intended for regulatory submissions. While the omission of histopathological end points from these guidance documents does not preclude their use, the results reported here provide a scientific basis that inclusion of histopathologic evaluation of the skin for safety assessment purposes does not provide information over that provided by clinical observation.
While histopathologic evaluation of phototoxicity is not required for photosafety evaluation, what is the possible consequence in including this evaluation in a safety study? One possible scenario is as follows. In a preclinical phototoxicity study, based on visual evaluation, no test material-induced phototoxicity is evident. However, histopathologic evaluation of the irradiated skin reveals changes that are not present in the skin in the group administered the vehicle formulation. A large body of background data would be required to allow interpretation of these results, and considering the potential mechanisms of phototoxicity elicited by different phototoxins (and potential confounding non-phototoxic changes in the skin), these data will in most cases not be available. The study director would have to interpret these results and the sponsor include this work in the regulatory submission, most likely without data to properly interpret the safety impact of these findings, placing both in an untenable position. In addition, it is feasible that under different UVR exposure conditions, either of dose or spectral distribution of the UVR source used, subvisual effects of UVR exposure alone will be identified by microscopic evaluation, complicating interpretation of any effect that a test material may have on that response. Even without test material effect, the hallmark of previous photosafety assessment, lack of visual effect, has now been questioned by any such microscopic finding. Again, how is this interpreted in a regulatory submission and put in context of any possible safety effect, especially if the groups administered the test material show equivocal or positive results?
In conclusion, based on current regulatory guidance and historical precedent, visual evaluation of skin reactions in response to the administration of a test material and UVR exposure is the defining criterion for evaluation of phototoxic reactions. Although histopathologic evaluation of the skin may provide valuable mechanistic information on the phototoxic reactions observed, the inclusion of histopathologic evaluation in photosafety studies intended for regulatory submission is not recommended.
Footnotes
Author Contribution
All authors (DL, ME) contributed to conception or design, data acquisition, analysis, or interpretation; drafting the manuscript; and critically revising the manuscript. All authors gave final approval and agreed to be accountable for all aspects of work in ensuring that questions relating to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
