Abstract
Using a nationally representative sample of older adults (age 65+, N = 7,547) and a path model, we examined the direct effects of dementia on social engagement, loneliness, and depressive/anxiety symptoms, and the mediation effects of loneliness and social engagement on the associations between dementia and depressive/anxiety symptoms. Of the study population, 7.7% and 5.5% had possible and probable dementia, respectively; 14.3% and 21.9% of those with possible and probable dementia had moderate to severe depressive/anxiety symptoms. The ratios of the indirect effects of social engagement and loneliness on a possible dementia to the total effect of possible dementia on depressive/anxiety symptoms were 0.26 and 0.28, respectively. The ratios in probable dementia were 0.11 and 0.21. The lack of social engagement and loneliness contribute substantially to depressive/anxiety symptoms in dementia. Strategies to increase social engagement and reduce social isolation are necessary to improve the psychological well-being of people living with dementia.
Introduction
The prevalence of depressive/anxiety symptoms among older adults with dementia, across all stages of the disease, is markedly higher than among their cognitively intact peers (Leung et al., 2021). Depression/anxiety exerts substantial adverse effects on individuals’ cognitive health and overall quality of life (Burks et al., 2021). Persistent or worsening depressive/anxiety symptoms are associated with accelerated dementia progression, affective and emotional dysregulation, and hastened functional decline (Botto et al., 2022; Defrancesco et al., 2017; Huang et al., 2022; Ismail et al., 2018; Lenze et al., 2005; Yin et al., 2024; Zhu et al., 2023). The comorbidity of dementia and depression/anxiety also complicates disease management, increases caregiver burden, and contributes to greater healthcare utilization (Chen et al., 2025; MacNeil-Vroomen et al., 2020; Xiang & An, 2015).
In addition to shared neurobiological mechanisms, depressive/anxiety symptoms among individuals with dementia likely reflect psychosocial responses to the awareness of cognitive decline (Botto et al., 2022; Brzezińska et al., 2020). In particular, the lack of social engagement and the experience of loneliness represent critical psychosocial stressors. During the early stages of dementia, individuals often feel shame, embarrassment, or frustration in social situations as cognitive, emotional, and functional impairments begin to interfere with their ability to maintain social roles and meaningful relationships (Aldridge et al., 2019; Honda et al., 2013; Kłosińska & Leszko, 2024; Singleton et al., 2017; Trindade et al., 2023). Dementia-related behavioral changes, such as apathy, disinhibition, and agitation, can further complicate interpersonal interactions and disrupt social integration (Hackett et al., 2019; Lozupone et al., 2024). Moreover, individuals with dementia may encounter social exclusion, discreditation, or discrimination in their social interactions (Biggs et al., 2019; Birt et al., 2020). Together, these challenges frequently lead to social withdrawal and reduced participation in community life, intensifying feelings of loneliness and depressive/anxiety symptoms and contributing to dementia progression (Penninkilampi et al., 2018; Wang et al., 2023).
Loneliness, defined as a subjective feeling of social disconnection or an unpleasant emotional experience resulting from a perceived deficiency in the quality of one’s social relationships (Perlman & Peplau, 1984), has increasingly been recognized as a critical biopsychosocial risk factor in later life. A substantial body of research has demonstrated its detrimental effects on the onset and progression of dementia (Htun et al., 2025; Lee et al., 2022, 2025; Luchetti et al., 2024; Oken et al., 2024; Rafnsson et al., 2020; Shen et al., 2022; Sundström et al., 2020), depression/anxiety (Lee et al., 2021), cardiovascular disease (Albasheer et al., 2024; Okeke et al., 2025), and increased risk of premature mortality (Holt-Lunstad et al., 2015; Wilson et al., 2019). Among individuals with dementia, loneliness may further precipitate or exacerbate depressive/anxiety symptoms by intensifying psychological distress, existential concerns, and feelings of worthlessness or hopelessness (Kotwal et al., 2024; Victor et al., 2020). Moreover, loneliness shares neurobiological and epigenetic mechanisms with both dementia and depression/anxiety, suggesting overlapping biological pathways that may heighten vulnerability to psychological decline (Bowirrat et al., 2023; Lam et al., 2021).
In contrast to the extensive body of research identifying a lack of social engagement and loneliness as risk factors for cognitive decline and dementia, their impact on the well-being of older adults already living with dementia remains relatively understudied. As discussed above, the limited existing studies, primarily based on convenience samples, suggest that reduced social engagement and heightened loneliness among individuals with dementia may contribute to increased depressive/anxiety symptoms. More population-based research is needed to examine the mediating role of social disengagement and loneliness in the relationship between dementia and depressive/anxiety symptoms. Such investigations could help disentangle the psychological pathways through which dementia affects mental health outcomes and identify key points of intervention.
Social health, including social participation and social networks, likely acts as a driver for the use of cognitive reserve, which can then slow cognitive impairment or maintain cognitive functioning (Vernooij-Dassen et al., 2022). Furthermore, depression/anxiety in dementia, whether they are a cause of cognitive impairment or a reaction to it, are important modifiable factors in dementia prevention, intervention, and care (Livingston et al., 2024). A better understanding of social engagement and loneliness as the mechanisms of the associations between dementia and depression/anxiety is essential for the development of targeted, person-centered interventions aimed at promoting social connection and emotional well-being among individuals with dementia.
In this study, using a nationally representative sample of community-dwelling Medicare beneficiaries aged 65 and older, we examined the direct associations between dementia status (i.e., possible [less severe] or probable [more severe] dementia vs. no dementia) and social engagement (i.e., participation in social or community activities), loneliness, and depressive/anxiety symptoms. We then assessed the extent to which the relationship between dementia and depressive/anxiety symptoms was mediated by social engagement and loneliness. The study hypotheses were: (H1) depressive/anxiety symptoms would be positively associated with both possible and probable dementia and with loneliness, but negatively associated with social engagement; (H2a) dementia would be negatively associated with social engagement; (H2b) dementia would be positively associated with loneliness; (H3) social engagement would be negatively associated with loneliness; and (H4) the association between dementia and depressive/anxiety symptoms would be partially mediated by the influence of dementia on social engagement and loneliness. Given the higher psychosocial burden of probable than possible dementia, we further hypothesized that these mediation effects would be stronger for probable dementia than for possible dementia. Sociodemographic characteristics, chronic illness, activity-limiting pain, and social network size were included as covariates. Figure 1 shows the study’s conceptual and analytic framework. Findings are expected to provide new insights into the interrelationships among social engagement, loneliness, and depressive/anxiety symptoms among older adults living with dementia. Conceptual and Analytic Framework for the Direct and Indirect Effects of Dementia, Social Engagement, and Loneliness on Depressive/Anxiety Symptoms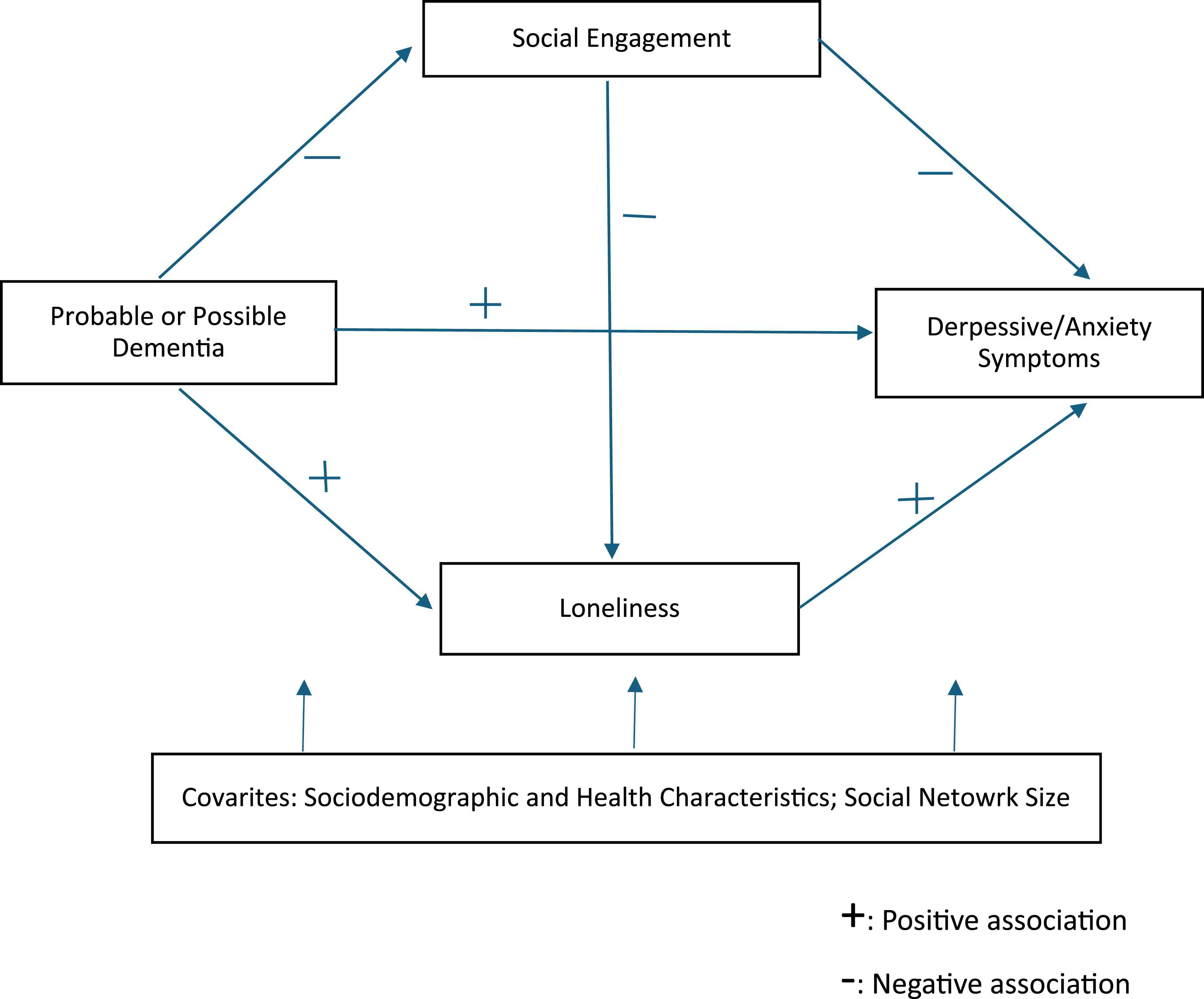
Methods
Data and Sample
Data came from the 2023 National Health and Aging Trends Study, which collects data annually from a nationally representative panel of Medicare beneficiaries ages 65 and older on their physical, functional, cognitive, and sensory capacities; social, physical, and technological environments; and participation in valued activities. In this study, after excluding 390 (of whom 16 had possible and 340 had probable dementia) sample persons who were proxy-interviewed, we focused on 7,547 sample persons who lived in their own homes or residential care communities (but not in nursing homes). The primary reason for including self-respondents only was that NHATS did not collect data on the sample persons’ loneliness (and other well-being indicators) from their proxy interviewees. This study, based on the analysis of de-identified public-use data, was exempt from the authors’ institutional review board review.
Measures
Dementia status (no dementia, possible dementia, and probable dementia) was determined using the most recently updated NHATS dementia classification algorithm (Kasper et al., 2024) based on two types of information for self-respondents: (1) doctor diagnosis of dementia or AD (yes or no); and (2) scores from cognitive tests evaluating the sample person in the following three domains: memory (immediate and delayed 10-word recall), orientation (date, month, year, and day of the week; naming the President and Vice President), and executive function (clock drawing test). A possible dementia classification was assigned when the person scored ≤ 1.5 SD below the mean in one domain of the cognitive test. A probable dementia classification was assigned when the person was diagnosed with dementia or scored ≤1.5 standard deviations (SD) below the mean in at least two domains of the cognitive tests. Thus, possible dementia is a classification of less severe cognitive impairment than probable dementia. The score cut points for ≤1.5 SDs below the mean on NHATS cognitive domains were ≤3 for memory (score range 0 to 20), ≤3 for orientation (score range 0 to 8), and ≤1 for executive function (score range 0 to 5).
Depression/Anxiety Symptoms in the Past Month
In NHATS, depression/anxiety symptoms were assessed with the Patient Health Questionnaire-4 (PHQ-4) (Kroenke et al., 2009). The PHQ-4 includes the first two items (PHQ-2; had little interest or pleasure in doing things, and felt down, depressed, or hopeless) from the 9-item PHQ-9 for depression (Kroenke et al., 2003) and the first two items (GAD-2; felt nervous, anxious, or on edge, and have been unable to stop or control worrying) from the 7-item Generalized Anxiety Disorder Scale (Spitzer et al., 2006). Responses to each PHQ-4 item were based on a 4-point scale (0 = not at all; 1 = several days; 2 = more than half the days; 3 = nearly every day), with the total score ranging from 0 to 12. Depression and anxiety frequently coincide, with highly correlated symptoms, and act as mutual risk factors, regardless of age groups, resulting in comorbid depression and anxiety (Bian et al., 2024; Jacobson & Newman, 2017; King-Kallimanis et al., 2009). The unweighted Cronbach’s alpha for the PHQ-4 for the study sample was 0.77. The PHQ-4 scores were also used to categorize the symptom severity: no symptom (0-2), mild symptoms (3-5), and moderate/severe symptoms (6-12) for descriptive purposes (Kroenke et al., 2009).
Social Engagement
This was assessed by the number of the following six social or community activities that the sample persons participated in during the past month: a) visits with family/friends; (b) attendance in religious services; (c) participation in clubs, classes, or other organized activities aside from religious services (referred to as attendance in clubs/meetings hereafter); (d) working for pay; (e) volunteering; and (f) going out to dinner, a movie, gambling, or to hear music or see a play (i.e., going out for enjoyment). The number ranged from 0 to 6.
Loneliness
This was assessed with a question, “During the last month, how often did you feel lonely?” The response categories were every day (=5), most days (5–6 days a week) (=4), some days (2–4 days a week) (=3), rarely (once a week or less) (=2), and never (=1). We treated it as a continuous variable, with the score ranging from 1 to 5, and the higher score representing greater loneliness. For descriptive purposes, we also grouped them into three categories (never/rarely, some days, and five or more days).
Covariates included (1) sociodemographic factors: age (65–74 [reference], 75-84, 85+); gender (female vs. male); race/ethnicity (non-Hispanic White [reference], non-Hispanic Black, Hispanic, others); residential type (care community vs. own home); education (bachelor’s degree or higher vs. no degree); and income, defined as total annual income from all sources reported for the respondent and their spouse or partner (if any), including earnings, pensions, Social Security, retirement accounts, and other public or private benefits (<$43,000 vs. other); (2) health status: the number of chronic medical conditions (0-8: arthritis, cancer, hypertension, heart disease, stroke, diabetes, lung disease, osteoporosis), and activity-limiting chronic pain (yes or no); and (3) social network size: the number of people (up to five) with whom the sample person discussed important life matters, including positive or negative events and concerns. Social network size is considered a social environmental factor (Vernooij-Dassen et al., 2022) that may influence social engagement and help decrease loneliness among older adults with dementia.
Analysis
All analyses were conducted with Stata/MP 19.5’s svy function (College Station, TX) to account for NHATS’s stratified, multistage sampling design. First, we used χ2 and one-way ANOVA to compare all study variables by dementia status: No dementia, possible dementia, and probable dementia. We then used χ2 and t tests to compare the two dementia groups.
Second, we fitted a path model to test hypotheses regarding the direct effects of possible and probable dementia, loneliness, and social engagement on depressive/anxiety symptoms, as well as the mediating roles of loneliness and social engagement in the association between dementia status and depressive/anxiety symptoms. Path coefficients (B) and linearized standard errors (SE) with 95% confidence intervals (CIs) were estimated using the survey-adjusted SEM framework. To test whether the associations of possible and probable dementia with social engagement and loneliness differed significantly in strength, we conducted adjusted Wald tests comparing the corresponding path coefficients. To assess mediation, we estimated the indirect effects of possible and probable dementia on depressive/anxiety symptoms through each mediator. Indirect effects and their 95% CIs were computed using bootstrapping with 10,000 replications. We also bootstrapped the differences in indirect effects across dementia status (i.e., probable vs. possible dementia) for each mediator to formally test whether the magnitude of mediation differed significantly. In addition, we calculated the proportion of the total effect that was mediated (indirect effect divided by the sum of direct and indirect effects), and the ratio of indirect to direct effects, for each pathway. Note that, given the cross-sectional data, while we use terms such as direct and indirect effects from the mediation literature, we do not infer causal relationships, but the findings reflect associations.
Results
Prevalence of Depressive/Anxiety Symptoms, Social Engagement, and Loneliness
Prevalence of Depressive/Anxiety Symptoms, Social Engagement, and Loneliness, and the Sociodemographic and Other Characteristics by Dementia Status
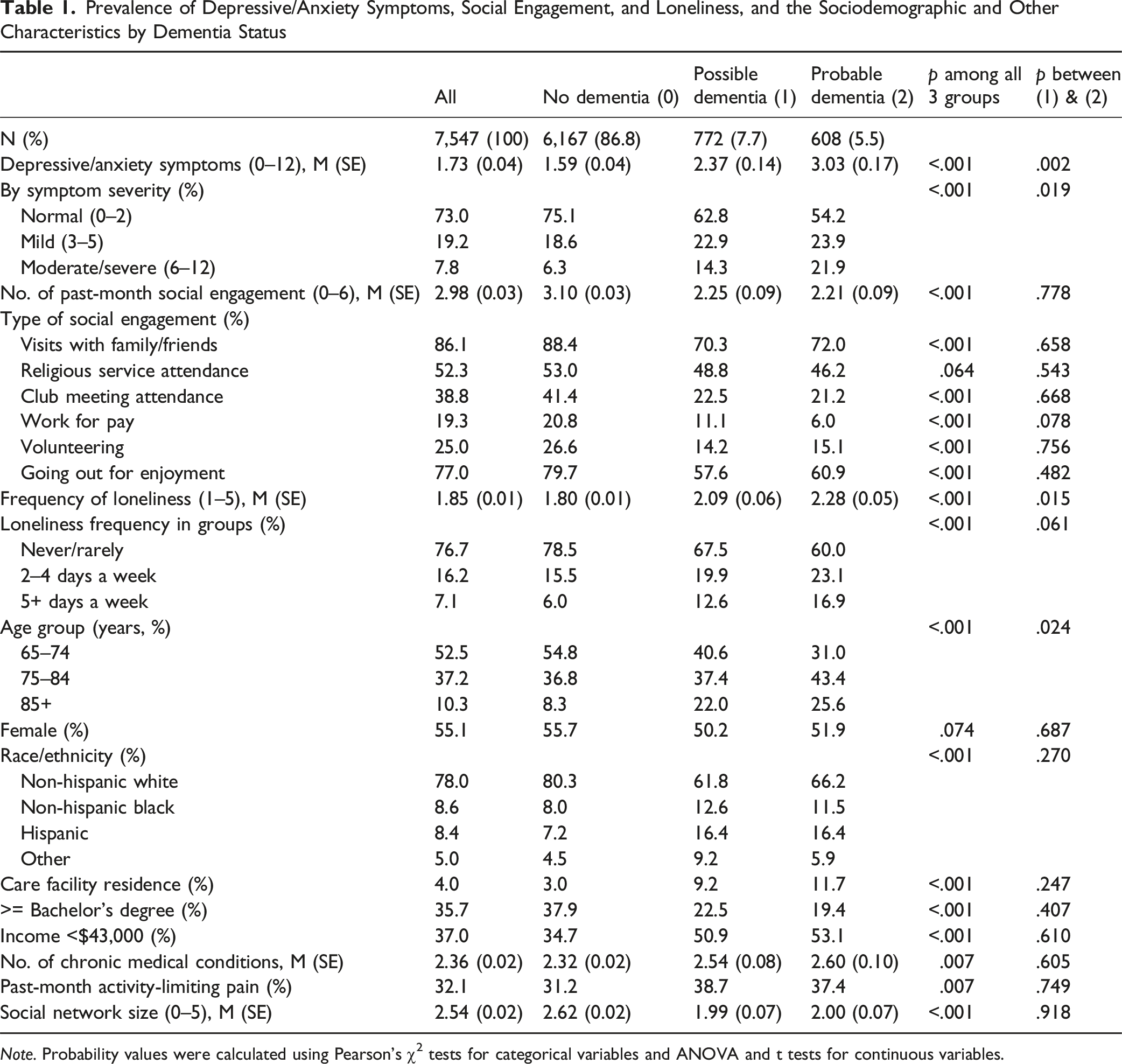
Note. Probability values were calculated using Pearson’s χ2 tests for categorical variables and ANOVA and t tests for continuous variables.
Those with probable dementia reported the highest frequency of loneliness, followed by those with possible dementia and those with no dementia. In terms of the percentages of those reporting loneliness, 40% of those with probable dementia and 32.5% of those with possible dementia, compared to 23.3% of those with no dementia, reported feeling lonely two or more days a week. Specifically, 16.9%, 12.6%, and 6.0% of individuals with probable dementia, possible dementia, and no dementia, respectively, reported feeling lonely five or more days a week. In these percentages, the two dementia groups were marginally significantly different from each other (F[1.92, 107.30] = 2.92, χ2 [df = 2] = 8.77, p = .061).
Sociodemographic and Health Characteristics and Social Network Size by Dementia Status
Table 1 also shows that both dementia groups did not significantly differ from each other in sociodemographic factors (except for older age among those with probable dementia), health status, or social network size. However, both dementia groups significantly differed from the no-dementia group in all other sociodemographic factors (except for gender distribution), health status, and social network size. Compared to the no-dementia group, both dementia groups included higher percentages of racial/ethnic minorities, residents of care facilities, individuals with an income <$43,000, and those experiencing activity-limiting pain, but included a lower percentage of individuals with a college degree. Both dementia groups also had more chronic medical conditions and smaller social networks.
Mediation Model Results
Effects of Social Engagement and Loneliness on the Association Between Dementia Status and Depression/Anxiety Symptoms: Model Parameters From the Mediation Model Using Path Analyses
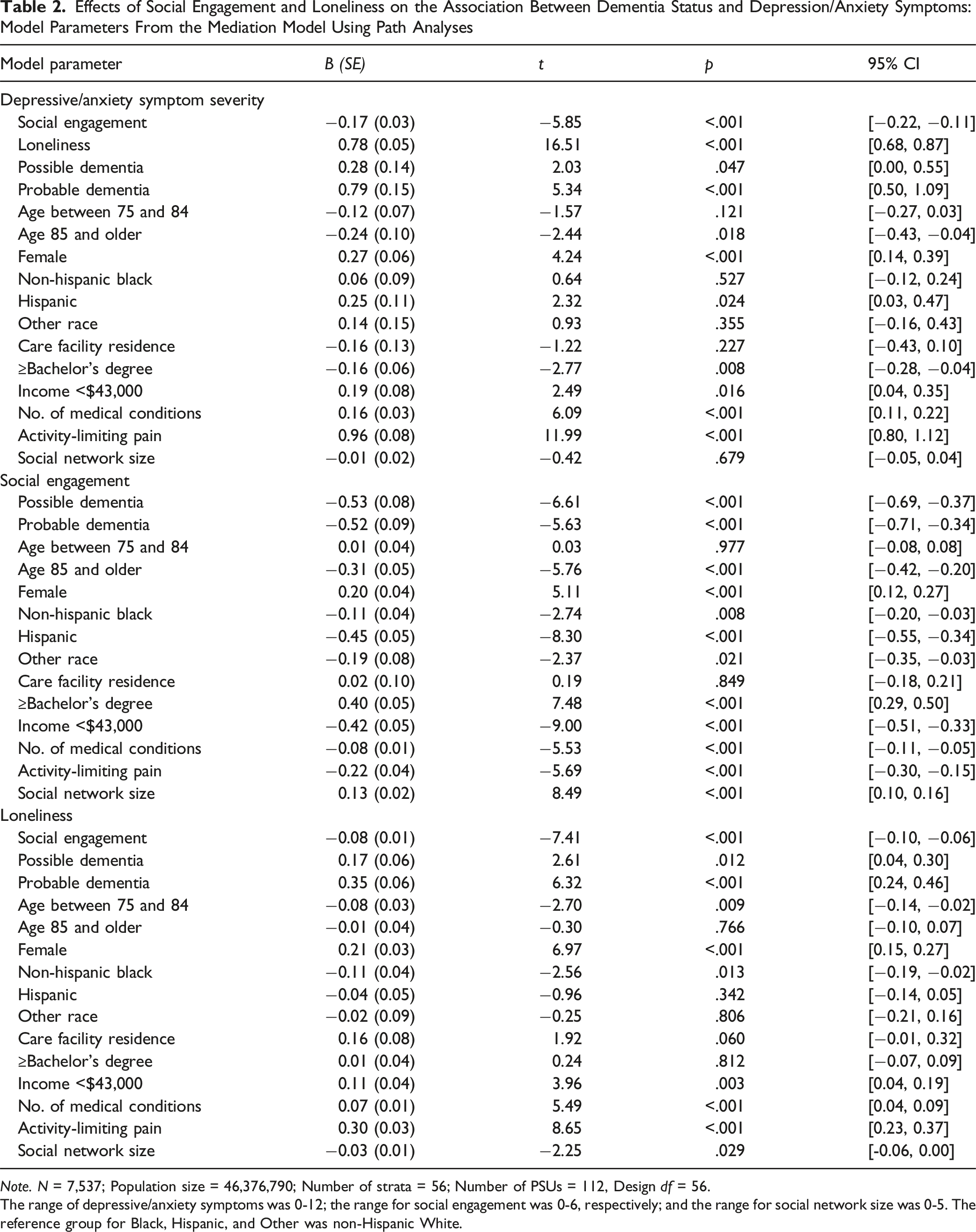
Note. N = 7,537; Population size = 46,376,790; Number of strata = 56; Number of PSUs = 112, Design df = 56.
The range of depressive/anxiety symptoms was 0-12; the range for social engagement was 0-6, respectively; and the range for social network size was 0-5. The reference group for Black, Hispanic, and Other was non-Hispanic White.
Direct Effects of Dementia, Social Engagement, and Loneliness
The top section of Table 2 shows that depressive/anxiety symptoms were significantly positively associated with possible dementia (B = 0.28, SE = 0.14, t = 2.03, p = .047), probable dementia (B = 0.79, SE = 0.15, t = 5.34, p < .001), and loneliness (B = 0.78, SE = 0.05, t = 16.51, p < .001), but they were significantly negatively associated with social engagement (B = −0.17, SE = 0.03, t = −5.85, p < .001). An adjusted Wald test comparing the two path coefficients indicated that the association between depressive/anxiety symptoms and probable dementia was significantly stronger than that for possible dementia (F[1,56] = 8.20, p = .006). In addition, depressive/anxiety symptoms were negatively associated with ages 85 and older and having a college degree, but they were positively associated with female gender, Hispanic ethnicity, having income <$43,000, having more chronic conditions, and having activity-limiting pain.
The middle and bottom sections in Table 2 show that after adjusting for sociodemographic and health characteristics and social network size, possible and probable dementia were negatively associated with social engagement (B = −0.53, SE = 0.08, t = −6.61, p < .001 for possible dementia; B = −0.52, SE = 0.09, t = −5.63, p < .001 for probable dementia), and significantly positively associated with loneliness (B = 0.17, SE = 0.06, t = 2.61, p = .012 for possible dementia; B = 0.35, SE = 0.06, t = 6.32, p < .001 for probable dementia). Adjusted Wald tests indicated no significant difference in the strengths of the associations between social engagement and possible and probable dementia (F(1,56) = 0.01, p = .921). However, the association between loneliness and probable dementia was significantly stronger than that for possible dementia (F(1,56) = 5.16, p = .027). Loneliness was also significantly negatively associated with social engagement (B = −0.08, SE = 0.01, t = −7.41, p < .001). These results largely support the study’s hypotheses on direct effects.
Indirect Effects of Social Engagement and Loneline ss on Depressive/Anxiety Symptoms
Indirect Effects of Social Engagement and Loneliness on the Relationship Between Possible and Probable Dementia and Depressive/Anxiety Symptoms
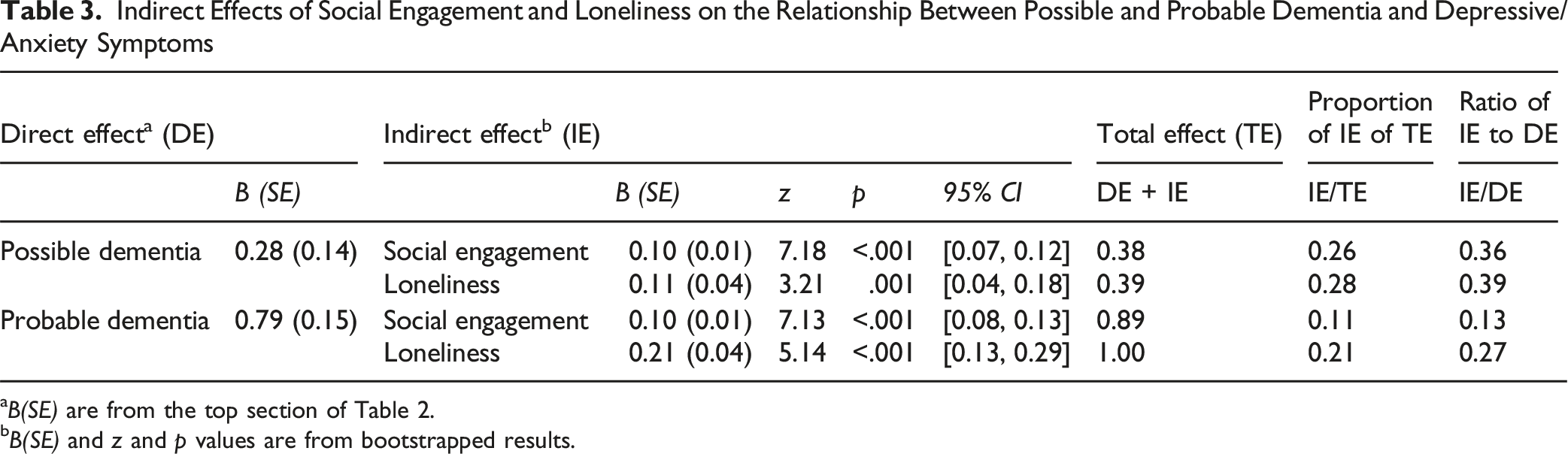
aB(SE) are from the top section of Table 2.
bB(SE) and z and p values are from bootstrapped results.
Table 3 also reports the proportion of each indirect effect relative to the total effect and the ratio of each indirect effect to the corresponding direct effect. For possible dementia, the proportions of the indirect effects via social engagement and loneliness to the total effect on depressive/anxiety symptoms were 0.26 and 0.28, respectively; the corresponding ratios to the direct effect were 0.36 and 0.39. For probable dementia, the proportions of the indirect effects via social engagement and loneliness to the total effect were 0.11 and 0.13, respectively, and the corresponding ratios to the direct effect were 0.13 and 0.27.
Discussion
In this study, we examined the prevalence of depressive/anxiety symptoms, social engagement, and loneliness among older adults living with dementia, and how social engagement (or the lack of it) and loneliness contribute to their depressive/anxiety symptoms. Our findings show that 13.2% of the Medicare beneficiaries aged 65 and older who were able to self-report their depressive/anxiety symptoms, social engagement, and loneliness had either possible or probable dementia. The prevalence of depressive/anxiety symptoms and loneliness was higher among those with probable than possible dementia, with a little more than one fifth of older adults with probable dementia experiencing moderate to severe depressive/anxiety symptoms and nearly one quarter reporting near-daily loneliness. The two dementia groups had fewer social engagements than the no-dementia group, but the two dementia groups did not significantly differ from each other.
The type of social engagement offers valuable insights. Older adults with and without dementia attended religious services at similar rates. The perceived and actual benefits of religious practice likely motivated both groups to participate. Systematic reviews of religious activities among older adults with dementia show that religion, faith, or spirituality helped them develop coping strategies to accept their condition, sustain relationships, maintain hope, and find meaning in life, which can slow cognitive decline and enhance quality of life (Agli et al., 2015; Daly et al., 2019). However, those with dementia were significantly less likely to engage in other activities, including visiting family and friends. As aforementioned, the lower social engagement in older adults with dementia may result from voluntary withdrawal due to shame, embarrassment, apathy, agitation, and involuntary social exclusion (Birt et al., 2020; Lozupone et al., 2024; Trindade et al., 2023). Reduced social engagement reflects disruptions in broader social and community activities, increasing social isolation. Past studies have also highlighted that a lack of enjoyable activities is a risk factor for declines in both mental and physical health (Bamonti & Fiske, 2021; Ong & Lee, 2023).
The path model confirmed significant direct associations between depressive/anxiety symptoms and both dementia statuses, social engagement, and loneliness, as well as a significant negative association between social engagement and loneliness. While the strength of the association between social engagement and dementia did not differ by dementia status, loneliness was more strongly associated with probable dementia than possible dementia. Bootstrap tests also showed that the indirect pathway through social engagement was comparable across dementia statuses. In contrast, loneliness was a significantly stronger mediator between probable dementia and depressive/anxiety symptoms than for possible dementia, despite lower proportion and ratio metrics for probable dementia. This discrepancy reflects the substantially larger total and direct effects of probable dementia, which reduce the relative contribution of the indirect effect via loneliness. Thus, although its relative share is smaller, loneliness plays a more prominent mediating role in the probable dementia pathway. The relationship between loneliness and depressive/anxiety symptoms may be bidirectional in cross-sectional studies; however, longitudinal research suggests a stronger effect from loneliness to mental health outcomes (Domènech-Abella et al., 2019). Loneliness is also a known risk factor for behavioral and psychological symptoms of dementia (Sun et al., 2021), highlighting the importance of addressing loneliness in dementia care.
Of the covariates, social network size was not significantly associated with depressive/anxiety symptoms but was positively associated with social engagement and negatively associated with loneliness. The directionality of the positive association with social engagement cannot be ascertained in cross-sectional data; however, having more supportive people was likely a motivating factor for engaging in activity, although social engagement may have also facilitated expanding one’s social network. The findings also show that physical and functional health problems played a significant role in depressive/anxiety symptoms, reduced social engagement, and increased loneliness. A previous longitudinal study showed that people with dementia generally had multiple health conditions, and those with more health conditions were lonelier and had poorer quality of life and poorer well-being; however, the number of health conditions had either minimal or no influence on cognition and social isolation over time (Sabatini et al., 2024).
Regarding sociodemographic covariates, our findings indicate that low income (<$43,000) was associated with lower levels of social engagement and higher levels of loneliness and depressive/anxiety symptoms, suggesting that financial insecurity poses a significant barrier to psychosocial well-being in later life. We also found that Hispanic ethnicity was associated with higher depressive/anxiety symptoms, and all minoritized older adults reported significantly lower social engagement; however, this was not associated with greater loneliness. Notably, being Black was linked to a lower likelihood of loneliness, but being Hispanic was no different from being White. Higher levels of depressive symptoms without having a higher level of loneliness among Hispanic older adults may reflect a complex interplay of social support and structural disadvantages. While familism and strong intergenerational ties may protect against loneliness, barriers such as limited access to culturally and linguistically appropriate mental health care, underinsurance, and stigma toward psychological distress may lead to under-recognition or undertreatment of depressive symptoms (Sadule-Rios, 2012). The observed decoupling of lower social engagement from greater loneliness among minoritized older adults might be due to limitations in how social engagement is measured. Conventional indicators, such as participation in clubs, recreational outings, or classes, may not fully capture the culturally salient forms of interaction common in Black and Hispanic older adults. These may include extended family interactions, religious involvement, and multigenerational co-residence. Such informal and family-centered connections may help buffer against loneliness despite limited broader community participation (Taylor & Nguyen, 2020). Further research is needed to explore the complex relationships among social engagement, loneliness, and depressive/anxiety symptoms in minoritized older adults living with dementia.
This study had some limitations related to data constraints. Depressive/anxiety symptoms were assessed using only four items each, loneliness was measured with a single item, and social engagement was not captured in terms of frequency. Since only self-respondents were included, the findings are primarily applicable to individuals with relatively high functioning. Additionally, the cross-sectional nature of the survey data limits the ability to infer causality, and self-reports of depression/anxiety, social engagement, and loneliness may have been affected by recall or social desirability bias. Social networks in NHATS included only those providing emotional support, which may have excluded individuals offering instrumental support to older adults with dementia. As symptoms of dementia can fluctuate over short periods, particularly in terms of mood, behavior, and cognitive clarity, such variability may also influence how older adults experience and report psychosocial constructs such as loneliness and social engagement. Given that the NHATS measures of social engagement and loneliness assess behavior and perception over short reference periods (e.g., “in the past month” and “in the past week,” respectively), these indicators may reflect transient cognitive or emotional states rather than stable patterns. While these short-term measures provide valuable snapshots of lived experiences, they may also introduce measurement variability, particularly among respondents with dementia.
Despite these limitations, this study was the first to examine the interrelationships among dementia, social engagement, loneliness, and depressive/anxiety symptoms in late life. The findings offer valuable insights into the types of potential interventions needed to enhance the emotional well-being and quality of life of older adults living with dementia. Specifically, this study highlights the essential roles of enhancing social engagement and reducing loneliness in improving the mental health of older adults living with dementia. Targeted interventions that promote meaningful engagement, alleviate loneliness, and reduce depressive/anxiety symptoms are needed. Routine clinical assessments should incorporate evaluations of social engagement and loneliness to identify at-risk individuals. Training caregivers to recognize and respond to signs of loneliness and emotional distress is also critical. Although the evidence base remains limited, growing research supports the effectiveness of interventions such as cognitive stimulation, music therapy, and psychological approaches—including cognitive behavioral therapy, pleasant events therapy, and problem-solving therapy—in reducing loneliness and depressive/anxiety symptoms among older adults with dementia (Kishita et al., 2020; Noone et al., 2019; Orrell et al., 2017; Rai et al., 2021). Technology-based interventions, including social robots and multimedia systems, have also shown promise (Budak et al., 2023; Sun et al., 2024). Facilitated small-group activities in settings such as senior centers and other community spaces, and individualized volunteer befriending (Sun et al., 2022) can help foster and preserve social connections among older adults with dementia. Finally, building dementia-friendly communities with accessible public spaces and transportation can further promote social inclusion and community participation (Hung et al., 2021).
Footnotes
Ethical Approval
The University of Texas at Austin’s Institutional Review Board exempted this study based on de-identified public-domain data.
Author Contributions
Study concept and design: Namkee G. Choi, Yuanjin Zhou, C. Nathan Marti. Acquisition of data: Namkee G. Choi. Data analysis: Namkee G. Choi, C. Nathan Marti. Interpretation: Namkee G. Choi, Yuanjin Zhou, C. Nathan Marti. Drafting of the paper: Namkee G. Choi. All authors reviewed and revised it critically for important intellectual content and gave final approval of the version to be submitted.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by grant P30AG066614, awarded to the Center on Aging and Population Sciences at The University of Texas at Austin by the National Institute on Aging.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data used in this study (The National Aging and Health Trends Study) are in the public domain.
