Abstract
Program evaluation is essential for medical schools to demonstrate social accountability and identify areas for improvement in medical education (MEd). Although stakeholder engagement is crucial in program evaluation, no previous review has specifically examined the stakeholders involved in MEd program evaluation. This scoping review addresses this gap by identifying the stakeholders, their roles, and their levels of engagement in evaluating MEd programs, along with the facilitators and barriers to their participation. Through a systematic search across four databases, we identified 53 relevant studies out of 7206 screened. Our findings reveal seven primary stakeholder groups, with students and program directors being the most frequent participants. However, a significant gap exists in the representation of community members and patients, indicating a need for greater inclusion of these key stakeholders. Additionally, we found that stakeholders are primarily engaged as passive participants providing feedback rather than actively shaping the evaluation process. Facilitators and barriers to participation were identified from the participants’ perspective, highlighting the need for further research to understand the viewpoints of active stakeholders, such as faculty and administrators. Future studies should also explore the impact of different evaluation approaches on stakeholder engagement to develop more inclusive and effective MEd program evaluations.
In today’s dynamic healthcare landscape, medical schools face the critical challenge of providing high-quality education while remaining socially accountable to their communities. The World Health Organization (WHO) defines social accountability for medical schools as ‘the obligation to direct their education, research, and service activities towards addressing the priority health concerns of the community, region, and/or nation they have a mandate to serve’ (Boelen et al., 1995, p. 3). This concept revolves around four core values: relevance, quality, cost-effectiveness, and equity in the healthcare system. The Global Consensus for Social Accountability of Medical Schools (2010) highlighted that the 21st Century presents medical schools with unique challenges, including improving quality, equity, relevance, and effectiveness in healthcare delivery.
Program evaluation is crucial in helping medical schools address these challenges, demonstrate progress on social accountability, and identify areas for improvement. The American Evaluation Association (AEA) defines program evaluation as ‘a systematic process to determine merit, worth, value, or significance’ (Patton et al., 2014, p. 1) aiming to make judgments about the program, improve its effectiveness, and inform decisions about future programming (Moreau, 2017; Patton, 1997). Evaluation allows medical schools to assess the effectiveness of their educational programs, identify areas for improvement, and ensure that their graduates are well-equipped to address community needs. Accreditation processes further emphasize the importance of program evaluation, mandating that medical schools regularly assess their educational programs and teaching methods (Santen et al., 2019; WFME, n.d; WFME & WHO, 2005).
Role of Stakeholder Engagement in Evaluation
Engaging diverse stakeholders in evaluation, including students, faculty, patients, and community representatives, is essential to maximize the benefits of evaluation (Moreau & Eady, 2023). Moreau and Eady (2023) identify three uses of evaluation findings in medical education (hereafter MEd): instrumental (direct action), conceptual (understanding without action), and symbolic (fulfilling requirements). Emphasizing the crucial role of diverse stakeholders in evaluation is pivotal to maximizing the benefits of these uses. Research suggests involving key stakeholders leads to more comprehensive and relevant assessments, greater program utilization, and increased stakeholder buy-in. This focus on stakeholder engagement is crucial for medical schools striving to fulfill their social accountability obligations. By incorporating diverse perspectives throughout the evaluation process, medical schools can ensure that their programs effectively address the specific health needs of their communities, ultimately leading to improved healthcare outcomes and a stronger connection with the community (Berk, 2009; Committee on Accredidation of Canadian Medical Schools [CACMS], 2024; WFME, 2020).
Research Gaps and Questions
However, the literature lacks clarity regarding the specific stakeholders currently engaged and the extent of their involvement in the evaluation process of MEd programs. To address this gap, the following research questions are proposed: RQ1 What are the different roles of stakeholders identified in the MEd program evaluations?; RQ2 How are these stakeholders engaged in MEd program evaluations, and what are the facilitators and barriers to their participation? By answering these research questions, we can gain a comprehensive understanding of stakeholder engagement in evaluating MEd programs. This will enable researchers and evaluators to design effective strategies for maximizing stakeholder participation and integrating diverse perspectives. This knowledge will empower medical schools to fulfill their social accountability obligations more effectively, improving MEd and healthcare delivery.
Methods
To answer our research questions, we conducted a scoping review of stakeholders’ participation in the MEd program evaluation, adhering to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guidelines (Peters et al., 2015; Tricco et al., 2018).
Search Strategy
We developed a comprehensive search strategy, incorporating best practices recommended by the university’s research support services. This strategy encompassed a broad range of keywords and synonyms related to stakeholder engagement in MEd program evaluation, including: stakeholder (participant, medical student, resident, teacher, patient, faculty), engagement (involvement, participation), and MEd (medicine, curriculum, program evaluation, course evaluation). We also incorporated relevant medical subject headings (MeSH terms). We searched four databases: Embase, Web of Science (WOS), CINAHL, and PsychInfo. To reflect current evaluation practices in medical schools, we limited our search to peer-reviewed studies published in English or French after 2013, excluding conference abstracts, letters, editorials, and review articles. The initial search occurred on February 17, 2023, with a final update on May 30, 2024. Appendix 1 provides detailed search equations for each database and article identification numbers. Identified articles were imported into the Covidence literature review management tool (Veritas Health Innovation) for further screening and analysis.
Study Selection
After removing duplicates, two authors independently reviewed titles, abstracts, and full-text articles based on the following inclusion criteria: focus on evaluating programs for undergraduate or graduate medical students, clearly identify the stakeholders involved in the program evaluation, and discuss methods for recruiting stakeholders, incentives for participation, and challenges faced during recruitment. We excluded studies where program evaluations involved students other than medical students (e.g., dental, osteopathic, or mixed student groups). We also excluded studies that evaluated teaching or assessment tools, as our aim was to highlight stakeholders’ participation in MEd program evaluations within faculty settings. Additionally, we excluded evaluations of programs in clinical settings to maintain a focus on faculty environments and evaluations of student performance, as these are typically assessed through standard course evaluations and do not directly address stakeholder participation in program evaluations. As a pilot, the two reviewing authors independently screened 15 randomly selected references to ensure consistent application of the eligibility criteria. This comprehensive review process aimed to ensure accuracy and minimize bias. Any disagreements regarding the inclusion or exclusion of articles were resolved through collaborative discussion between the two researchers at the end of each selection phase.
Data Extraction
The first and second authors independently extracted data from full-text articles using a standardized data extraction form within Covidence. The form developed and piloted a priori captured data on study characteristics (aim and design), program evaluation details (evaluation design, specific program evaluated, aim of the evaluation, and tools used), and stakeholder information (type and number of stakeholders engaged, recruitment methods, facilitators, and obstacles to participation). After independent extraction, the authors convened a consensus meeting to compare and discuss their findings. Any discrepancies were resolved through discussion and reference to the original articles, ensuring the accuracy and completeness of the final dataset.
Data Analysis and Presentation
We conducted a descriptive analysis, categorizing studies based on their goals, evaluation designs, and stakeholder characteristics. Given the diversity of included studies, we focused on identifying common factors that facilitated or hindered stakeholder participation in MEd program evaluations. Our findings, structured around our two main research questions, adhere to PRISMA-ScR guidelines for transparency and rigour (Tricco et al., 2018).
Results
The PRISMA diagram presents the results of the search in Figure 1. From the four databases, 7206 studies were screened, and 53 were included in the review. Most articles were excluded for not addressing the recruitment of evaluators nor how they are encouraged to participate in the evaluation and for not being concerned with a program evaluation as defined by our criteria. Specifically, 34 articles focused solely on students’ academic performance, 22 articles did not pertain to medical students, 2 articles were not in English or French, 3 were not original articles, and 1 article was excluded due to an error in the processing software. PRISMA Diagram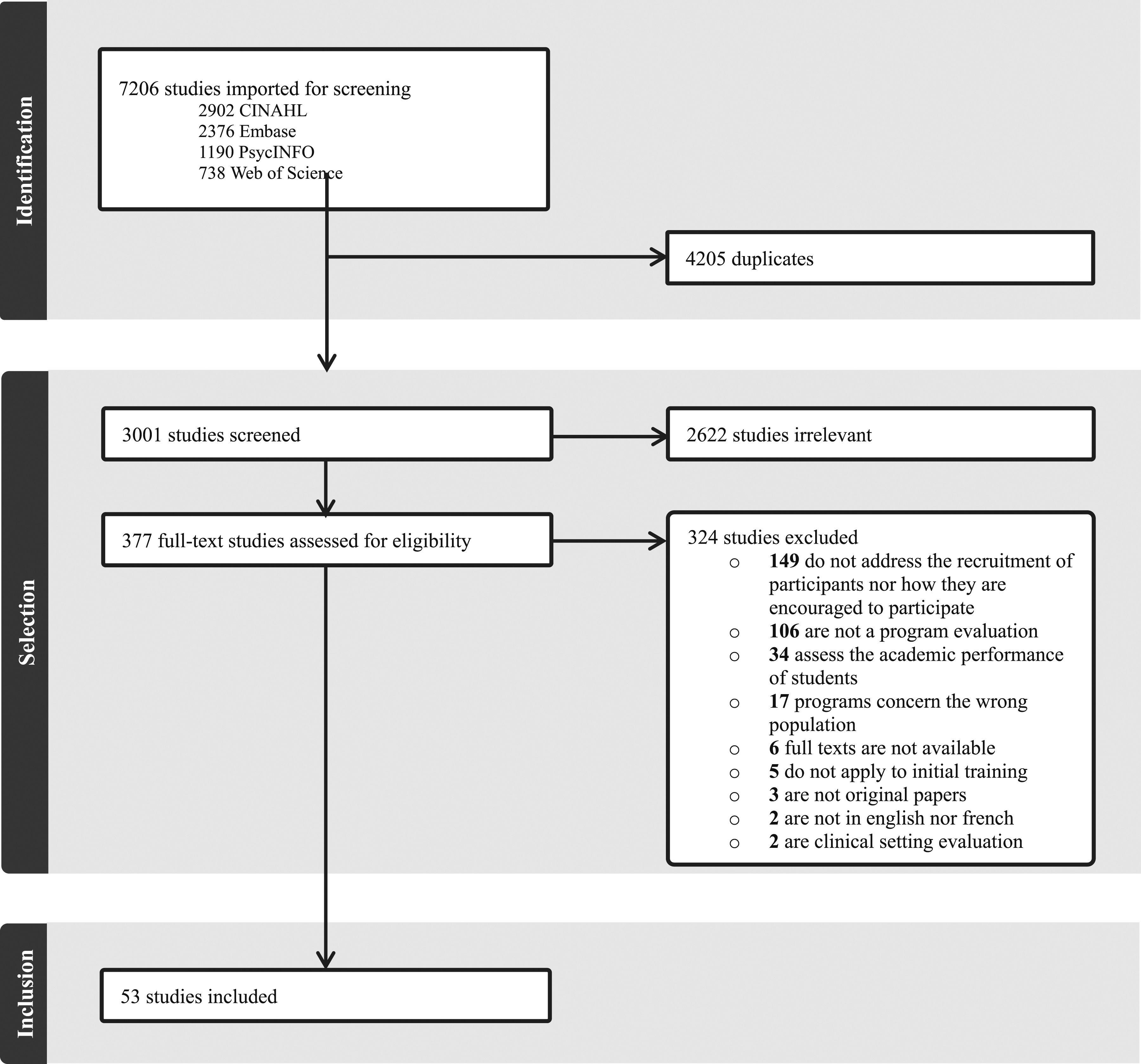
Studies Characteristics
Characteristics of Evaluations Included
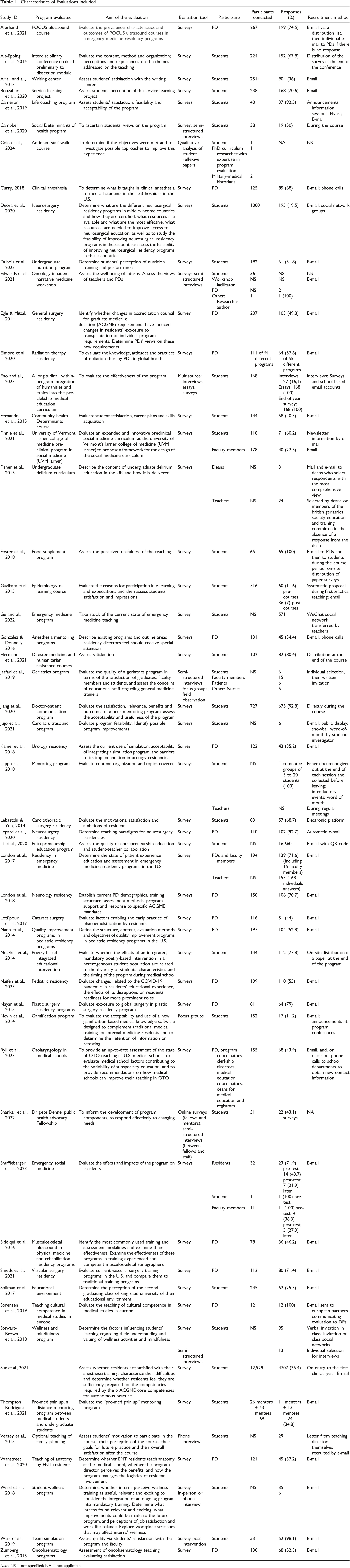
Note: NS = not specified; NA = not applicable.
Stakeholders Role Identified in MEd Program Evaluations Our review identified seven distinct groups of stakeholders involved in MEd program evaluations. Students (n = 33, 62%) and program directors (n = 20, 38%) were the most frequently included stakeholders. Other stakeholder groups identified included teachers (n = 4, 8%), faculty members (n = 5, 9%), patients (n = 1, 2%), and nurses (n = 1, 2%). A few studies included a broader category of stakeholders encompassing deans, program evaluation experts, military medical historians, and researchers (n = 4, 8%). Notably, nine studies (17%) intentionally incorporated multiple perspectives by gathering input from various combinations of students, teachers, program directors, researchers, faculty members, patients, and nursing paramedics. These results are presented in Table 2.
Stakeholders Identified in MEd Program Evaluations
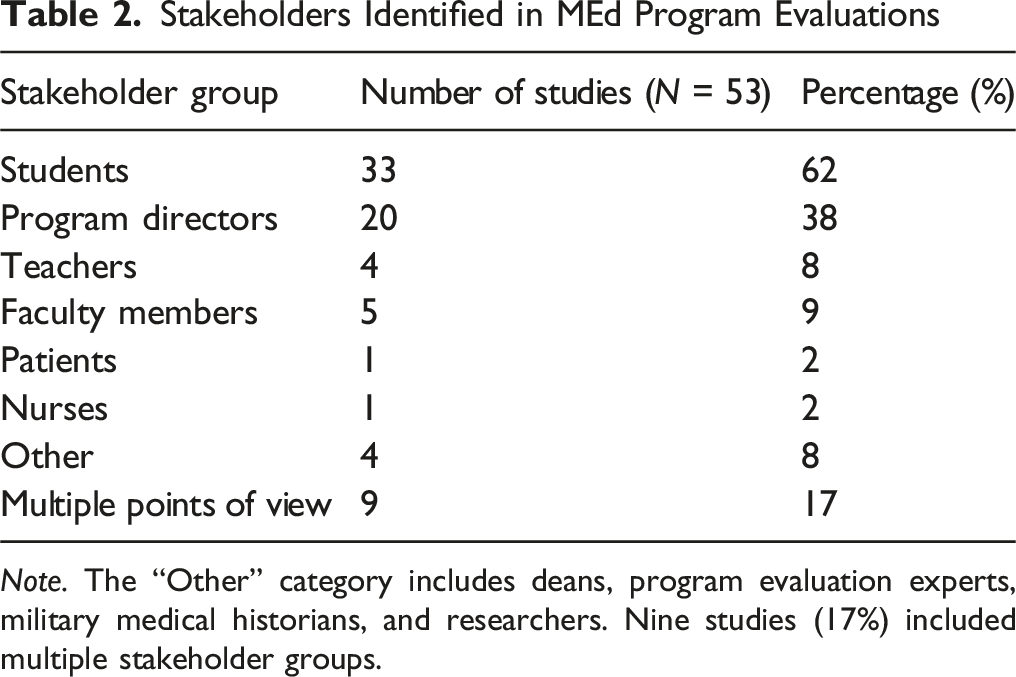

Note. The “Other” category includes deans, program evaluation experts, military medical historians, and researchers. Nine studies (17%) included multiple stakeholder groups.
Stakeholder Engagement, and Facilitators and Barriers in MEd Program Evaluations
Stakeholder Engagement
Our review found that stakeholders were predominantly engaged as participants providing feedback rather than actively shaping the evaluation process itself. Most studies utilized email (n = 43, 81%) to recruit participants, while other methods such as phone calls (n = 3, 6%), direct recruitment during class (n = 11, 21%), and individual recruitment or social media (n = 3, 6%) were less common. The specific methods used to engage stakeholders varied across groups. Students (n = 33) primarily participated through surveys (n = 29, 87.9%), with fewer instances of interviews (n = 9, 27.3%), focus groups (n = 2, 6.1%), or activity analysis (essays or clinical practice) (n = 3, 9%). Program directors, teachers, and faculty members were consistently engaged through surveys in all relevant studies. The response rate varied widely from one study to another, especially for those using questionnaires: 11.2% to 100%. Eighteen (34%) authors who used questionnaires achieved a minimum response rate of 60%. Among the authors’ objectives, fifteen (28%) are concerned with student satisfaction. One study also interviewed program directors, while another utilized semi-structured interviews, focus groups, and field observations with faculty members. Patients and paramedics were involved in only one study, participating through semi-structured interviews and focus groups. Two studies employed unique approaches to stakeholder engagement. Cole et al. (2024) utilized a diverse evaluation team and student reflexive essays, while Shankar et al. (2022) commissioned an independent evaluation organization. Additionally, six studies combined various methods, such as surveys, interviews, focus groups, and field observations, to better understand stakeholder perspectives.
Facilitators and Barriers to Participation in MEd Program Evaluations
Appendix 3 provides an overview of the facilitators and barriers identified in the reviewed studies regarding participation in MEd program evaluations. It is important to note that these facilitators and barriers primarily pertain to participants in the evaluation process, rather than active stakeholders, as most studies engaged them as such.
Facilitators to Participation
Most studies (64%, n = 34) reported multiple facilitators to participation in MEd evaluations. Anonymity was highlighted as a significant factor favouring participation in many studies (45%, n = 24). Additionally, the voluntary (11%, n = 6), optional (2%, n = 1), or confidential (6%, n = 3) nature of participation, as well as the right to refuse to answer any question (2%, n = 1), were also considered encouraging. To maintain anonymity and confidentiality, some studies chose not to use official channels or avoided evaluating the presence of teachers, preferring independent researchers. Another key facilitator was the use of reminders, which were sent via email (42%, n = 22), phone (4%, n = 2), orally (2%, n = 1), or through unspecified methods (2%, n = 1).
Some studies aimed to systematize the recruitment process to enhance response rates. In 19% of the studies (n = 10), researchers utilized a national database of program directors’ email addresses. Additional dissemination channels included newsletters and the country’s most popular social network. Some studies also sent requests to more people than initially anticipated or involved third parties. Others took advantage of students' presence in class to distribute questionnaires (9%, n = 5). Limiting the number of questions or ensuring a short duration was also beneficial.
Some studies adopted a targeted approach. One team used personalized emails, either directly or through departmental channels. Another study specified that the person most involved in the program should complete the questionnaire. In another case, a student investigator was employed to recruit other students for the evaluation.
In some instances, program evaluation was integrated into a regular, protocolized process, such as allocating time away from teaching for evaluation, habitual program evaluation by students, or making it part of the teachers’ mission. In terms of incentives, some studies mentioned that access to further education was conditional on completing the evaluation. In contrast, others (15%, n = 8) offered material incentives like gifts, prizes, and compensation, all targeting students.
Barriers to Participation
The barriers to participation in MEd program evaluations were less frequently specified in studies (72%, n = 38). Some studies faced recruitment difficulties due to invalid or unavailable email addresses (6%, n = 3). Using social network groups as dissemination channels did not reach all potential reviewers. Similarly, relying on program directors to disseminate evaluations reduced information transfer and student involvement. Collecting responses was challenging due to evaluators’ lack of time, as they were preoccupied with faculty and personal obligations, or because the evaluation took place far from the program being evaluated. Repeated requests for responses led to student fatigue. One study reported a loss of responses due to a questionnaire not suited for residency programs with different organizational structures. While most studies viewed voluntary participation as beneficial, one study found that it did not motivate participants to engage in program evaluation. Finally, three studies (6%) mentioned the lack of incentives, especially material ones, as a barrier.
Discussion
This scoping review examined the roles and participation levels of stakeholders in MEd program evaluations, including the facilitators and barriers to their participation. We found 53 studies that addressed these questions, and our review yielded several interesting findings.
First, we found a growing number of publications in MEd program evaluation during the last decade. Indeed, there has been a notable increase in publications on MEd program evaluation, with 45% of these works published between 2020 and 2024 and 30% between 2016 and 2019. This trend reflects a growing interest in the field of MEd program evaluation. This reflects the need to develop such evaluation to respond to social accountability and the accreditation process of medical schools (Santen et al., 2019; WFME & WHO, 2005). It is also found in a number of publications guiding to develop this evaluation (Balmer et al., 2020, 2023; Cook, 2010; S. R. Shrivastava & P. S. Shrivastava, 2023).
Secondly, we identified seven primary stakeholder groups involved in MEd program evaluation: students, program directors, teachers, faculty members, patients, nurses, and other healthcare professionals. While students (n = 33, 62%) and program directors (n = 20, 38%) were the most frequently included, the near absence of community members and patients underscores a critical gap in current evaluation practices. This underrepresentation is particularly concerning given their unique perspective as the primary beneficiaries of medical training and their central role in social accountability (Boelen et al., 2016). Engaging these stakeholders more meaningfully could offer invaluable insights into program effectiveness and relevance to community needs (Moreau & Eady, 2023).
Third, we found that stakeholders were predominantly engaged as participants providing feedback rather than actively shaping the evaluation process. This represents a missed opportunity to empower them to contribute to the design and interpretation of evaluations. Strategies to actively engage these groups should be prioritized. One of the first strategies would be reflections on the evaluation approach as a first step in developing a program evaluation by considering, for example, design thinking (Fish et al., 2022; Sandars & Goh, 2020), utilization-focused approach (Patton, 2012), or empowerment evaluation (Fetterman, 1996; Fetterman et al., 2010). Another would be diversifying data collection methods and incorporating a wider range of perspectives that could lead to more comprehensive and meaningful evaluations.
Finally, several factors were identified that influence participation in MEd program evaluations. Facilitators included anonymity, reminders, convenience, targeted communication, and incentives. Conversely, recruitment difficulties, challenges in collecting responses, the inadequacy of voluntary participation alone, and lack of incentives were barriers to participation. It is crucial to note that these factors primarily relate to participants in the evaluation process, not active stakeholders, as most studies engaged them as such. Therefore, future studies should prioritize investigating the perspectives of active stakeholders, such as program administrators, faculty, and employers, to gain a more comprehensive understanding of the factors that influence their engagement in MEd program evaluations.
Strengths and Limitations of the Study
This study is the first to review the participation of stakeholders in medical education program evaluation. The research carried out in this work is targeted and structured. Several databases were searched, with a reading by two independent practitioners supported by a program evaluation expert. The large number of articles included lends power to the literature review, but it could have benefited from two more independent reviewers for more validity to the results. Due to limited publication of medical program evaluations, future scoping reviews should include grey literature, such as unpublished reports and non-peer-reviewed sources, to gain valuable insights into stakeholder engagement in practice settings. The method does not allow us to understand the individual reasons behind stakeholder participation in evaluation.
Conclusion
Evaluating medical programs and teaching is essential to the medical school accreditation process. Many MEd publications reflect a growing interest in program evaluation, which aligns with the importance of medical schools’ social responsibility. The evaluation depends on the participation of its stakeholders: students, program directors, teachers, and faculty members. It should systematically involve patients and paramedics. This participation could be considered an involvement in the evaluation process instead of mere feedback. To encourage stakeholder participation in program evaluation processes, consideration could be given to the choice of evaluative approaches before the implementation of evaluations. This work could be completed to understand better and perceive stakeholders' motivations for participating in the evaluation of medical programs and teaching.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors thank the financial support from the Région Auvergne Rhône-Alpes, France, with the Pack Ambition Internationale for the publication of this article (22PACK-CHANELIERE-3303). The authors reveiced no financial support for the research and authorship.
