Abstract
Purpose:
This study aimed to explore the predictive factors of early-tracheostomy decannulation in patients with laryngeal cancer undergoing partial laryngectomy and to develop a nomogram for predicting the probability of early decannulation (within 1 month).
Materials and Methods:
This study conducted a retrospective analysis of patients with laryngeal cancer who underwent laryngeal function preservation surgery at the First Affiliated Hospital of Wenzhou Medical University from January 2012 to December 2021. Univariate analysis and multivariate logistic regression analysis were used to identify independent predictors factors, and the nomogram is constructed based on the results of multivariate logistic regression analysis. Receiver operating characteristic (ROC) curves, calibration curves, and decision curves were employed to validate the clinical utility of the model.
Results:
A total of 141 patients were analyzed. Among them, 82 patients successfully achieved early decannulation, while 59 patients failed to undergo early decannulation, the multivariate logistic regression analysis showed age (odds ratio [OR] 0.954, 95% CI 0.912-0.999), history of smoking (OR 0.975, 95% CI 0.951-0.998), surgical modality (OR 0.590, 95% CI 0.404-0.861), drainage tube (OR 0.216, 95% CI 0.08-0.580) is the independent risk factor for early-tracheostomy decannulation. The area under the curve of the ROC curve is 0.756 (95% CI 0.673-0.840) indicating good discriminative capacity. The calibration curve and the Hosmer-Lemeshow test (P = .138) demonstrate good model fitted and high calibration. The incidence of early decannulation was 58.2%, and at the threshold of 58.2%, the decision curve was above the none and all lines, so the model has clinical utility.
Conclusion:
A nomogram model based on age, history of smoking, surgical modality, and drainage tube was successfully developed to predict the probability of early-tracheostomy decannulation.
Introduction
The main treatment methods for laryngeal cancer include surgery (open surgery with or without preservation of laryngeal function, endoscopic surgery), radiotherapy, and chemotherapy. 1 In patients undergoing open surgery with preserved laryngeal function, although vocal function is retained, long-term retention of the tracheostomy tube often remains as a tough issue. Several reasons may lead to unsuccessful decannulation, such as laryngeal stenosis, deglutition disorders, follow-up treatment.2,3 Patients with these factors often require extended rehabilitation training to achieve tracheostomy decannulation, which is typically managed in outpatient settings. Meanwhile, the shortening of hospital stays has also forced some patients who could have early-tracheostomy decannulation to carry the tracheostomy tube for a more extended time. Decannulation of tracheostomy patients currently relies heavily on clinician judgment, but detailed guidelines and criteria from references can help standardize the process and determine the optimal timing for decannulation. Studies on tracheostomy tube decannulation have primarily focused on patients in intensive care units, with a significant emphasis on those with conditions such as stroke and traumatic brain injury. For instance, research has shown that early decannulation in elderly patients with craniocerebral injury can reduce complications and improve outcomes.4 -9 However, there are limited studies on predictors of early-tracheostomy decannulation in patients undergoing open partial laryngectomy. This study aimed to identify the predictive factors of early-tracheostomy decannulation in patients with laryngeal cancer who accept partial laryngectomy. Constructing a nomogram can conveniently predict the possibility of early decannulation. A nomogram model was subsequently developed to predict the probability of early-tracheostomy decannulation (with 1 month).
Materials and Methods
This study conducted a retrospective analysis of patients with laryngeal cancer who underwent laryngeal function preservation surgery at the First Affiliated Hospital of Wenzhou Medical University from January 2012 to December 2021. The study design was approved by the Ethics Review Committee of the First Affiliated Hospital of Wenzhou Medical University (KY2022-R166). The inclusion criteria were as follows: (1) Pathology confirms laryngeal squamous cell carcinoma; (2) patients with T1 to T3 classified by the eighth edition of the AJCC classification; (3) acceptance of open partial laryngeal resection; (4) no neoadjuvant chemotherapy or radiation therapy was administered prior to surgery. Exclusion criteria included were as follows: (1) concomitant with other malignancies; (2) previous history of tracheostomy surgery; (3) presence of chronic diseases; (4) patients with recurrent laryngeal carcinoma; (5) presence of distant metastasis; (6) the postoperative decannulation time exceeds 1 month; (7) patients who have not been able to decannulate due to treatment needs (chemoradiotherapy, etc) after surgery. A total of 141 patients were included in the study, which was divided into 2 groups according to whether the tracheostomy tubes had been decannulated within 1 month: (1) The early-tracheostomy decannulation group consists of 82 cases; (2) the prolonged tracheostomy dependence group consists of 59 cases. Although the postoperative care and intervention measures for laryngeal cancer have basically achieved homogeneous management, due to the failure of our hospital to achieve homogeneous management in the monitoring of postoperative hematological indicators of patients with laryngeal cancer, there may be errors in the relevant data. Therefore, only preoperative and surgical data of patients were collected, including gender, age, history of smoking, BMI, albumin, globulin, albumin/globulin, neutrophil, lymphocyte, monocytes, platelet, neutrophil/lymphocyte ratio (NLR), platelet/lymphocyte ratio (PLR), lymphocyte/monocyte ratio (LMR), T staging, the primary site of laryngeal cancer, surgical modality, neck dissection, and drainage tube.
Statistical analysis was performed using IBM SPSS Statistics (version 22.0; IBM Corp, Armonk, NY, USA) and the R software (version 4.2.0; R Foundation for Statistical Computing, Vienna, Austria). Categorical variables were compared using Pearson’s chi-squared test and Fisher’s exact test. Before analyzing continuous variables, the normality of the data was evaluated. Differences between groups were examined using Student’s t-test for normally-distributed variables and the Mann-Whitney U test for those that were not normally distributed. Univariate logistic regression analysis was performed to identify significant factors associated with early decannulation. Variables with P < .2 were included in the multivariate logistic regression. Two-sided P < .05 were deemed statistically significant.
A nomogram was constructed based on the results of multivariate logistic regression analysis. The model’s performance was evaluated by constructing a receiver operating characteristic (ROC) curve and its discrimination was assessed using the area under the curve (AUC). Calibration was performed using a plotted calibration curve and the Hosmer-Lemeshow test. A decision curve was generated to validate the clinical utility of the model.
Results
Among the 141 patients enrolled, 82 patients successfully achieved early decannulation, while the other 59 patients failed to undergo early decannulation. The results of the univariate statistical analysis are presented in Table 1. Statistically-significant differences between the 2 groups were observed in age, history of smoking, surgical modality, and drainage tube. Variables with P < .2, including globulin, LMR, T staging, and neck dissection, were considered. Based on clinical experience, early decannulation may be associated with T staging and neck dissection; consequently, age, smoking history, surgical approach, drainage tube, T staging, and neck dissection were incorporated into the multifactorial analysis. The results are displayed in Table 2. Notably, T staging and neck dissection were not significant in multifactorial analysis, while age, history of smoking, surgical modality, and drainage tube emerged as independent predictors of early-tracheostomy decannulation, and drainage tube was the strongest predictors.
Characteristics of the 2 Groups.
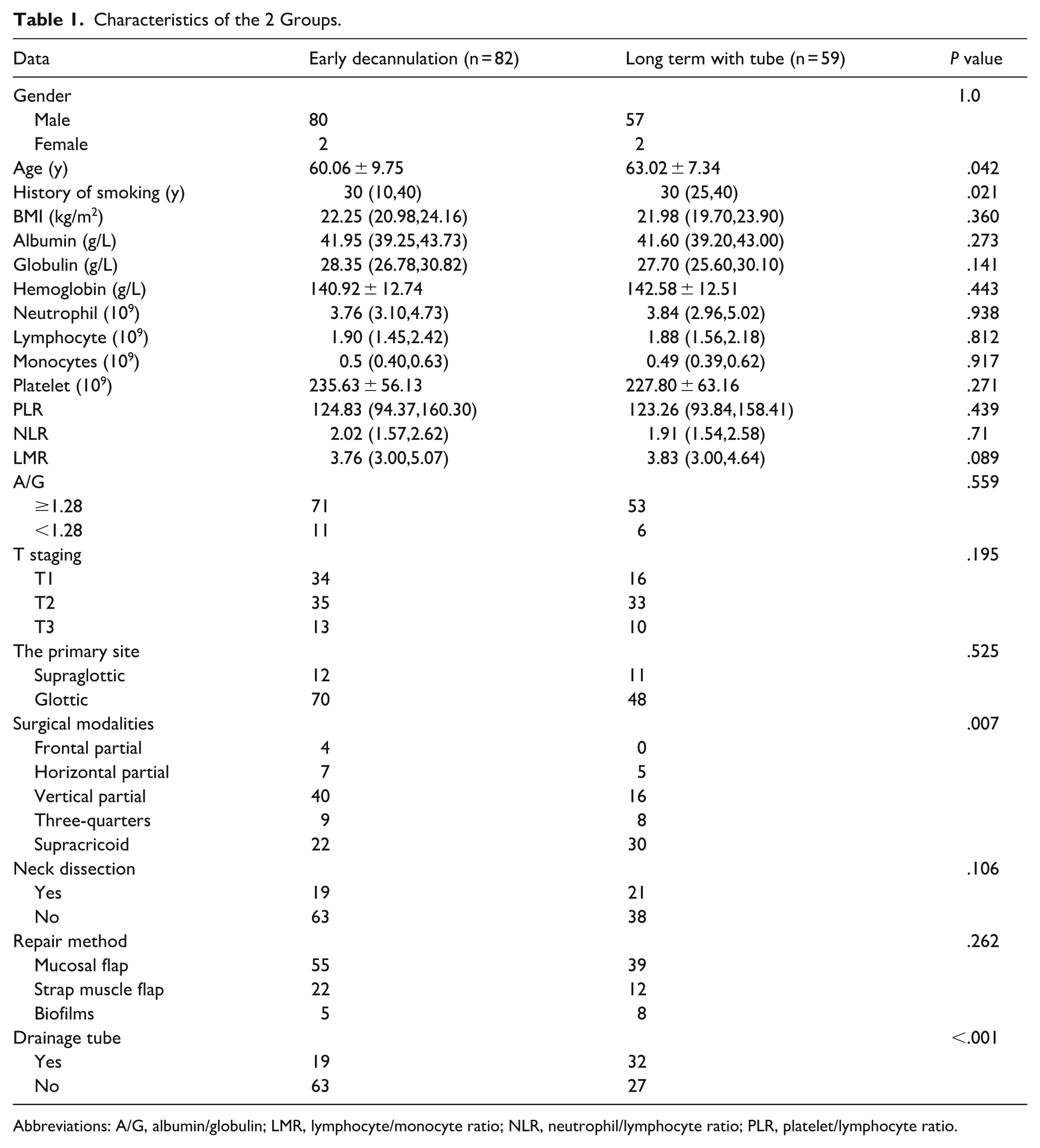
Abbreviations: A/G, albumin/globulin; LMR, lymphocyte/monocyte ratio; NLR, neutrophil/lymphocyte ratio; PLR, platelet/lymphocyte ratio.
Univariate and Multivariate Logistic Regression Analysis of Possible Variables in Predicting Early Decannulation.
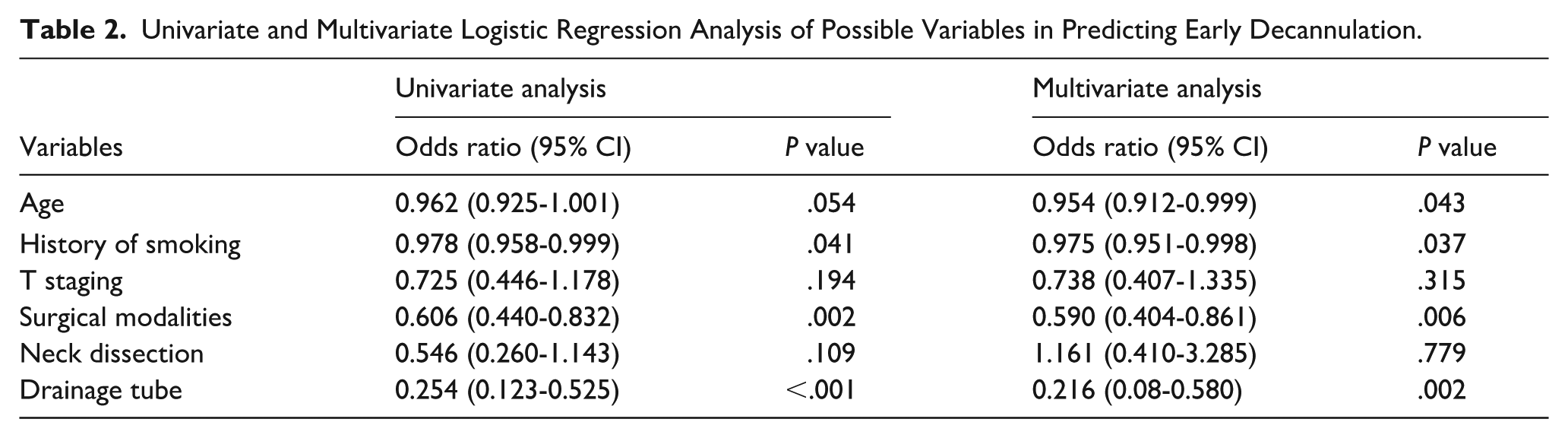
Therefore, we utilized the 4 factors to construct a nomogram for predicting the likelihood of early-tracheostomy decannulation (Figure 1). The nomogram consists of 7 rows. The score for each variable is determined based on the proportions indicated in the first row. The total score, as determined by the sixth row, is employed to calculate the predicted probability of early-tracheostomy decannulation. For example, a 45 year-old patient who has never smoked, underwent vertical partial laryngectomy, and had an drainage tube, would score 75, 52.5, 50, and 0, respectively, with a total score of 177.5 and a 76% probability of early decannulation. To evaluate the predictive accuracy of the nomogram, an ROC curve was plotted, yielding an AUC of 0.756 (95% CI 0.673-0.840), which signifies a robust predictive capability (Figure 2). The calibration curve demonstrates that the nomogram is well-calibrated (Figure 3). The Hosmer-Lemeshow test yields a P value of .138, which is above the conventional threshold of .05, suggesting that the model’s predictions are consistent with the observed data, indicating a good fit. The incidence of early-tracheostomy decannulation was 58.2%, and at the threshold of 58.2%, the decision curve was above the “none” and “all lines,” suggesting that the model has clinical utility (Figure 4).
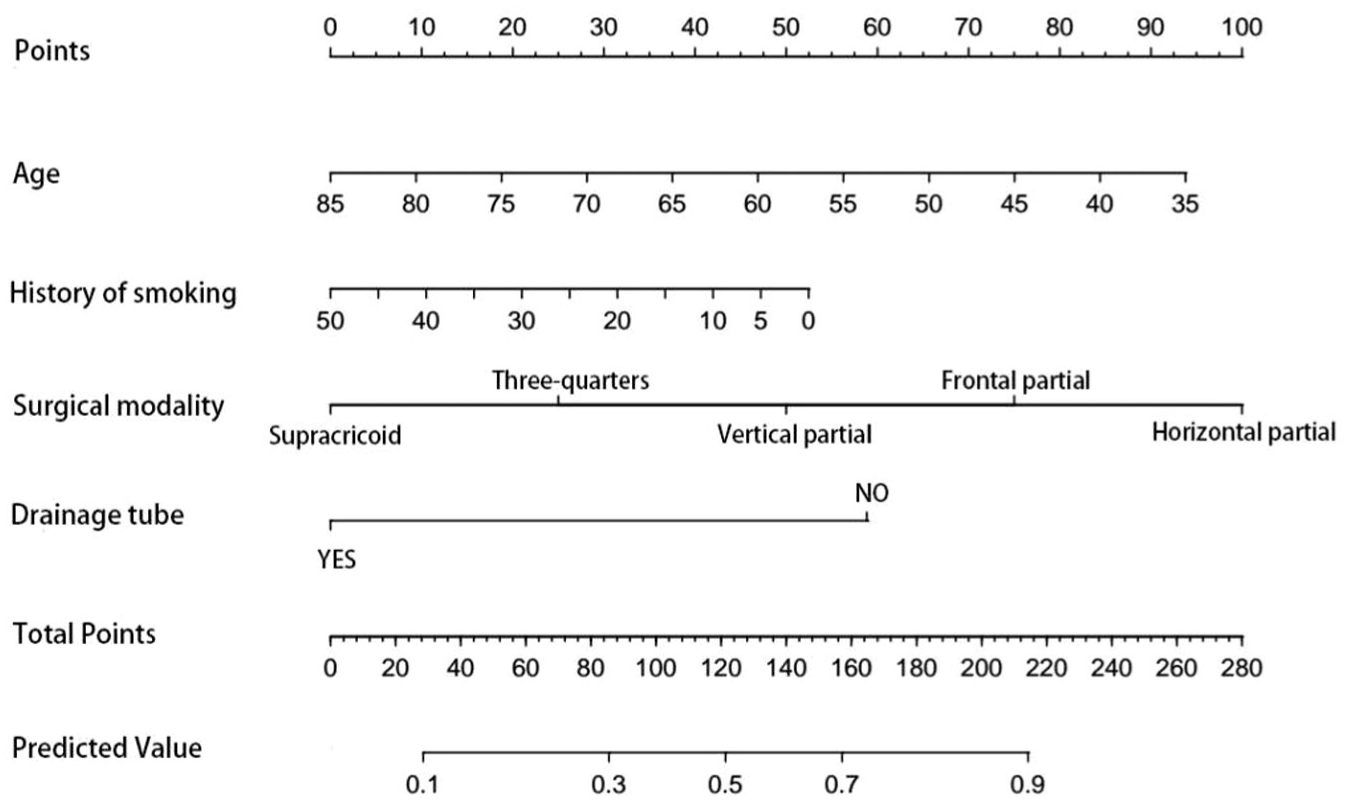
Nomogram for predicting early-tracheostomy decannulation in patients undergoing partial laryngectomy. The values represented by age, smoking history, surgical modality, and drainage tube can all be found in the “points” row to get the corresponding scores. Sum these scores to obtain the “total points,” and the predicted value corresponding to the number in this row is the possibility of decannulation.
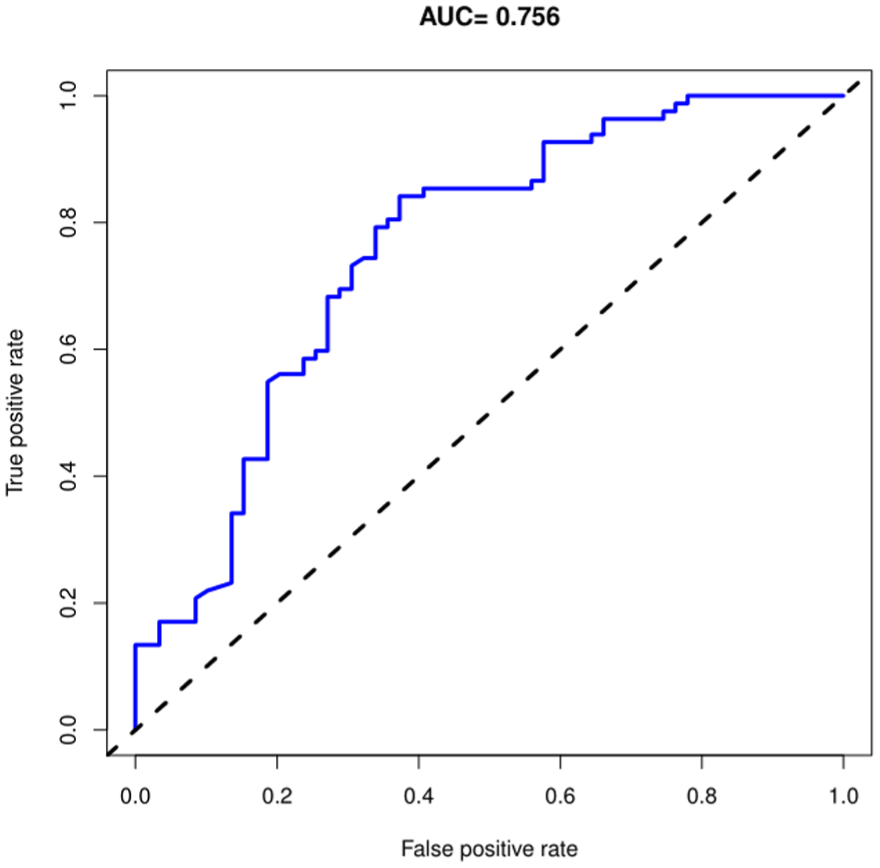
ROC curve of the multivariate logistic regression model which had an AUC of 0.756 (95% CI 0.673-0.840). AUC, area under the curve; ROC, receiver operating characteristic.
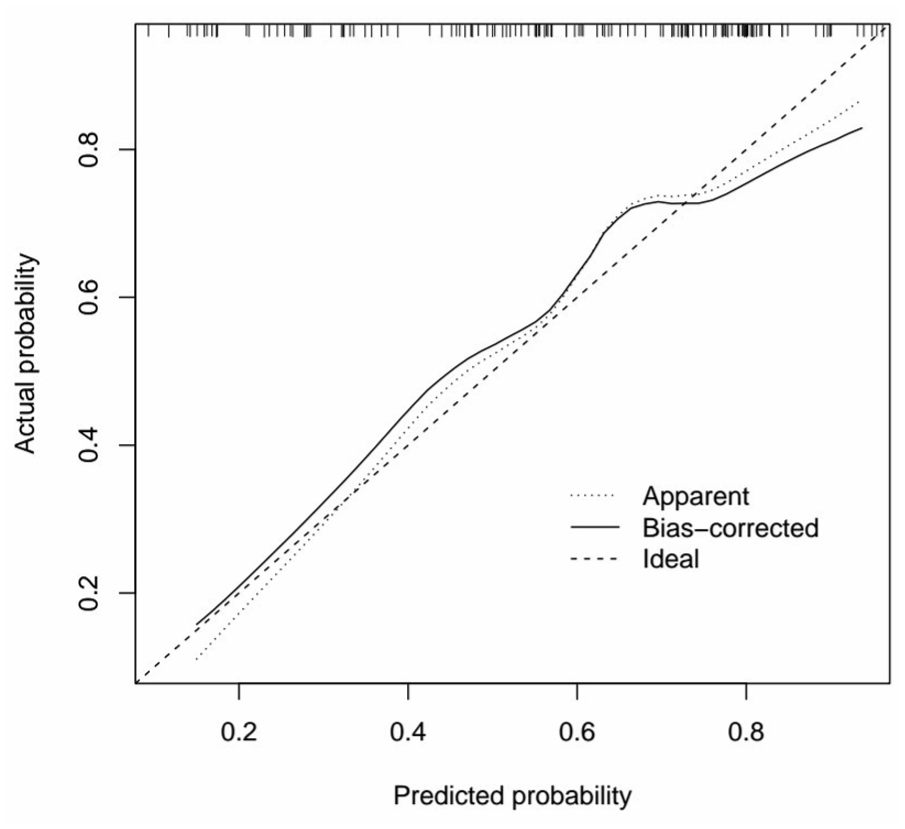
Calibration curve of the nomogram.
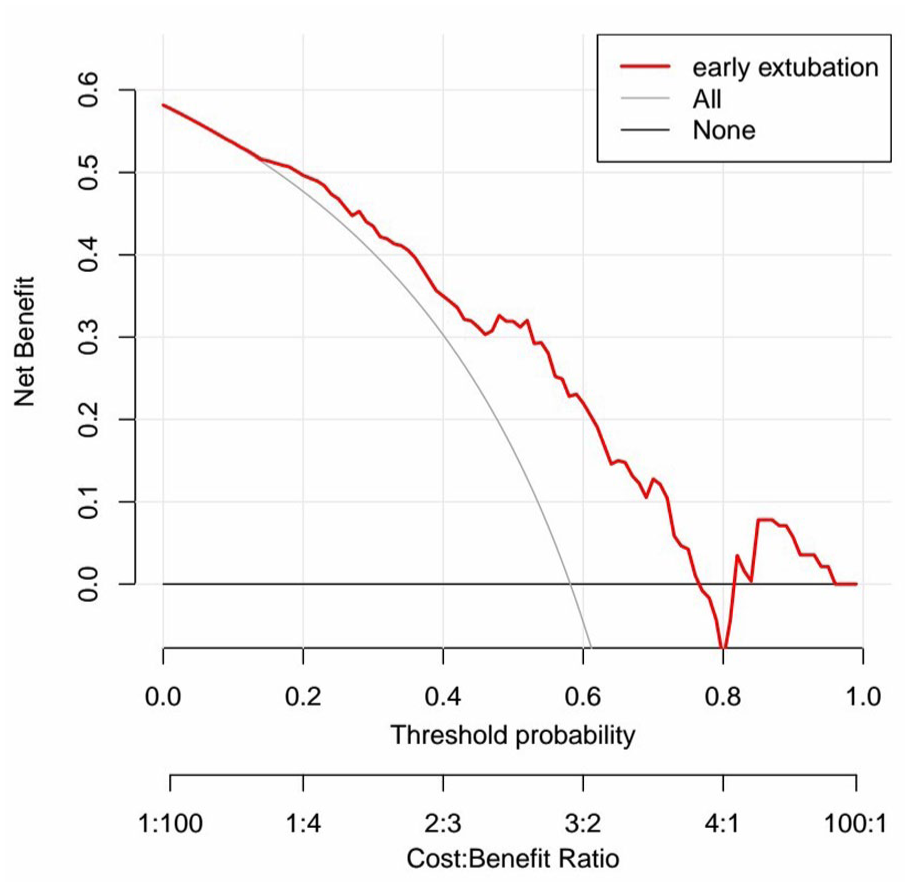
Decision curve of the nomogram.
Discussion
In follow-up interviews with patients who could not decannulate tracheostomy early, it was found that almost all of them shared the same desire: to have the tracheostomy tube removed. 10 Therefore, a model capable of predicting early-tracheostomy decannulation is of utmost importance, as it greatly encourages patients and fosters a more optimistic outlook for postoperative recovery. According to Simone Thomas et al, underlying medical conditions directly influence the timing of decannulation. 11 Consequently, patients with concurrent chronic underlying conditions were excluded from the inclusion criteria.
The indicators considered in this study were all preoperative and surgery-related, designed to predict the likelihood of early-tracheostomy decannulation in patients with laryngeal cancer following surgery. We identified that the variables predicting early-tracheostomy decannulation included age, history of smoking, surgical modality, and drainage tube.
Survival studies on cancer populations in Europe and the United States indicate that younger patients generally enjoy a higher quality of life and longer survival periods than their elder counterparts.12,13 It can be inferred that for patients with cancer, age is a crucial factor influencing prognosis and quality of life. As individuals age, their cells undergo senescence, bodily functions (including the heart, lungs, and muscles) gradually deteriorate, and the capacity to tolerate surgical stress also diminishes over time. In this study, we found that the probability of early-tracheostomy decannulation decreased as age increased. It has also been confirmed in Wehbi et al’s research that age is a significant predictor. 14 A study led by Ishizaki et al also showed that age was an important factor associated with decannulation. 15 Our study corroborated Ishizaki et al’s findings, revealing that the probability of early decannulation decreased with increasing age. In this model, the likelihood of early decannulation at age 85 was observed to be 40% lower than that at age 35, which aligns with findings that elderly patients over 80 may face increased risks and complications post-tracheotomy.
Numerous studies have confirmed that smoking is a significant independent risk factor for the development of laryngeal cancer.16 -18 Our research indicates that the length of a patient’s smoking history plays a significant role in the success of early decannulation following surgery. Beyond the carcinogenic risk, smoking impairs lung function, and prolonged smoking exacerbates this damage. 19 We believe that impaired lung function due to smoking is a significant factor in delayed decannulation. After undergoing partial laryngeal resection, a patient’s short-term respiration depends entirely on the tracheostomy, which suggests that the primary lung function governs the patient’s breathing capacity. With identical airway conditions, superior lung function leads to more effortless breathing.
In addition to potential damage to lung function, smoking can also affect the amount of respiratory secretions in patients. Studies have demonstrated that long-term smokers undergoing partial laryngectomy prone to produce increased phlegm, which impairing airway patency. The clearance capacity of airway secretions serves as a critical factor influencing decannulation. 20 Among patients with comparable coughing ability, those with fewer airway secretions can expel phlegm more easily, maintain unobstructed airways, and prevent mucus crust blockage in the respiratory tract. Smoking has a multifaceted impact on patients with laryngeal cancer; it not only impairs lung function, a known risk factor for carcinogenesis, but also significantly increases the risk of developing laryngeal cancer. Furthermore, it may affect early decannulation.
Laryngeal partial resection surgery, commonly categorized into partial frontal laryngectomy, horizontal partial laryngectomy, vertical partial laryngectomy, three-quarters (near-total or Pearson) laryngectomy, and supracricoid laryngectomy, has been shown to improve patient quality of life and reduce the impact on laryngeal function, as evidenced by clinical studies comparing it to total laryngectomy.21 -23 Different surgical methods, such as partial laryngectomy, require varying amounts of reserved laryngeal space to ensure the preservation of specific functions like speech and breathing. In the surgical modality described above, the horizontal partial laryngectomy does not destroy the thyroid cartilage. Consequently, the postoperative laryngeal space is larger than that in other surgical modalities, thereby effectively preserving respiratory and pronunciation functions. In contrast, other surgical modalities involve removing part of the thyroid cartilage plate, which results in varying degrees of laryngeal cavity narrowing and stenosis. Our study revealed that retaining more thyroid cartilage is beneficial for early decannulation. The greater the amount of thyroid cartilage retained, the larger the laryngeal space. After surgery on the laryngeal cavity, there is an increase in airflow with each breath.
When performing neck dissection or when surgical wounds are extensive, a drainage tube is inserted to prevent potential complications, such as infection and wound dehiscence, caused by the accumulation of exudates in the surgical cavity.24,25 The model we have developed indicates that patients with a drainage tube are less likely to have their tracheostomy tube removed at an earlier time. There is no statistically difference compared with patients who have undergone neck dissection, which may be related to the fact that these patients undergo more traumatic surgery and have a relatively slower postoperative recovery. There may also be a correlation with the extent of laryngeal tumor invasion (involving neurovascular structures).
This study incorporated preoperative indicators such as the NLR, which has been identified as an independent prognostic factor for laryngeal cancer survival rates. However, contrary to the findings of other studies, this research found that indicators such as NLR, PLR, and LMR were not predictive of a negative outcome.26 -29 There may be no direct correlation between long-term survival and early decannulation; long-term survival involves not only respiratory and swallowing functions but also immune, circulatory, and other systems, reflecting the patient’s overall health status. In contrast, decannulation is a short-term local condition. T staging plays a pivotal role in guiding the treatment of laryngeal cancer; however, there is no direct correspondence between T staging and surgical approaches. Surgical techniques are limited by the surgeon’s skill proficiency and the patient’s condition. Patients at the same cancer stage may undergo different surgical approaches, and their postoperative recovery can differ. Therefore, indicators that are meaningful for treating laryngeal cancer may not hold significant value in predicting early decannulation.
Before decannulation of a tracheostomy, an electronic nasopharyngolaryngoscopy is typically performed to clearly assess the degree of glottic stenosis. However, this method is indeed insufficient for evaluating granulation tissue formation and stenosis at the tracheostomy site. As a novel approach, fiberoptic bronchoscope (FOB)-guided decannulation of a tracheostomy can effectively address this deficiency and increase the success rate of decannulation.6,14,30 This study may assist in identifying patients eligible for the FOB-guided protocol. Specifically, patients with a high probability of early decannulation can be considered for the FOB-guided protocol, potentially enhancing the success rate of this procedure.
In this study, we successfully developed a nomogram to predict the probability of early decannulation in patients who have undergone partial laryngectomy, taking into account the risk factors for delayed decannulation and the potential complications as discussed in the literature. It is noteworthy that this is the first nomogram study focused on facilitating early-tracheostomy decannulation in patients with laryngeal cancer; we identified a total of 4 factors to predict outcomes. Overall, we are of the opinion that the 4 factors selected in the nomogram are theoretically and clinically well-grounded for predicting outcomes.
Given that our study was retrospective, the model construction, though relatively successful, exhibited certain limitations. These limitations encompassed insufficient preoperative data, the omission of postoperative data, and a limited number of cases. Smoking often causes impairment of lung function, and early decannulation may be closely associated with lung function. Due to lack of lung function data in some patients, this study failed to include such data in the analysis, which to a certain extent reduced the predictive ability of the model. In future studies, lung function will be considered for inclusion. This study excluded chronic diseases to eliminate confounding factors, but this has limited the application scope of the study. In future research, a predictive model incorporating more elements will be constructed. We attempted to use preoperative and surgical data to construct this model, aiming to offer substantial assistance in clinical work and to play a positive role in the physiological rehabilitation of laryngeal cancer patients after surgery. In future studies, we expect to identify additional indicators to enrich our research. This study was carried out at a single hospital, thus representing only the situation in Wenzhou. We anticipate subsequent multicenter collaboration to develop a more comprehensive forecasting model.
Conclusion
In summary, the nomogram model, incorporating age, history of smoking, surgical modality, and the presence of a drainage tube, has been successfully developed to predict the probability of early decannulation after partial laryngeal resection in patients with laryngeal cancer. This model can guide treatment strategies and facilitate doctor-patient communication.
Footnotes
Acknowledgements
This work has been carried out thanks to the Medical and Health Research Project of Zhejiang Province (CN; no. 2024KY1687).
Ethical Considerations
The ethics review committee approved the study design of the First Affiliated Hospital of Wenzhou Medical University.
Consent to Participate
This study was reviewed and approved by the Ethics Committee in Clinical Research of the First Affiliated Hospital of Wenzhou Medical University, which granted a waiver of informed consent in accordance with relevant regulations.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Medical and Health Research Project of Zhejiang Province (CN; no. 2024KY1687).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
