Abstract
Objectives:
Children with genetic syndromes, especially Down syndrome (DS), are considered high-risk candidates for adenotonsillectomy (AT) due to anatomical abnormalities and comorbidities. This study aimed to evaluate the safety of AT in patients with DS and other genetic syndromes (OS).
Methods:
This retrospective study included 62 syndromic patients (46 DS, 16 OS) under 18 years of age who underwent tonsillectomy ± adenoidectomy ± ventilation tube (VT) insertion between 2010 and 2025. Demographics, comorbidities, surgical details, complications, and hospital stays were reviewed.
Results:
Indications included sleep-disordered breathing (51/62, 82.3%) and recurrent tonsillitis (16/62, 25.8%). Procedures performed were AT (51/62, 82.3%) or tonsillectomy alone (11/62, 17.7%) ± VT insertion (16/62, 25.8%). Median hospital stay was 1 day (IQR: 1-1), with 93.5% (58/62) discharged after 1 day. Two-day stays occurred in 18.75% of OS patients (3/16) and 2.2% of DS patients (1/46). Planned intensive care unit admission was required in 2 OS patients (3.2%). No emergency admissions or perioperative mortality occurred. Overall complication rate was 8.1% (5/62)—8.7% in DS and 6.3% in OS (P = 1.00)—including bleeding requiring reoperation (1/62, 1.6%), respiratory event (1/62, 1.6%), and insufficient oral intake (3/62, 4.8%).
Conclusion:
AT appears to be safe in children with genetic syndromes, with low rates of complications.
Keywords
Introduction
Down syndrome (DS) represents the most prevalent chromosomal disorder, with an incidence of 1 in 691 live births. 1 In individuals with DS, several anatomical and physiological factors contribute to the development of obstructive sleep apnea (OSA), including hypotonia, macroglossia, midface hypoplasia, narrow nasopharynx, lymphoid hyperplasia, and obesity.2-5 Moreover, OSA is commonly observed in other craniofacial syndromes characterized by features such as craniosynostosis, maxillomandibular hypoplasia, midfacial hypoplasia, micrognathia, and hypotonia.6,7 While the prevalence of OSA in the general pediatric population is reported to be 1%-4%, 8 it increases significantly in children with DS (40%-80%)3-5 and in several other syndromes such as syndromic craniosynostosis (40%-85%), 9 CHARGE syndrome (65%), 7 and Prader–Willi syndrome (80%). 10
In pediatric otolaryngology, recurrent tonsillitis and OSA are the main indications for adenotonsillectomy (AT), which is widely considered the first-line surgical treatment for both.11,12 If left untreated, OSA can lead to serious cardiovascular, metabolic, and neurocognitive complications, including systemic and pulmonary hypertension, cor pulmonale, cognitive dysfunction, and behavioral disturbances.13-16
Several studies have suggested that children with DS may carry a higher risk of morbidity following AT compared to the general pediatric population.17-20 Likewise, comorbidities such as craniofacial anomalies and other genetic syndromes have been associated with increased postoperative complication rates.21-23 As a result, patients with genetic syndromes often raise concern for clinicians and are commonly referred to tertiary care centers for surgical intervention.
The objective of this study was to evaluate the safety of AT in syndromic children and to compare postoperative outcomes between DS and other syndromic groups.
Materials and Methods
Protocol and Selection Criteria
Patient data from individuals who underwent tonsillectomy ± adenoidectomy ± ventilation tube (VT) insertion between January 2010 and January 2025 were retrospectively reviewed using medical records and archives. Inclusion criteria were as follows: children under 18 years of age with a diagnosis of DS or other genetic or congenital syndromes (OS); a history of tonsillectomy ± adenoidectomy ± VT insertion due to symptoms of OSA or recurrent tonsillitis; and availability of sufficient medical records, follow-up data, and contact information. Some of the included syndromes were related to chromosomal anomalies, while others were associated with genetic mutations or complex malformation syndromes.
Of the 78 patients initially identified, 16 (10 with DS, 6 with OS) were excluded due to missing data or inability to establish contact. The final study population included 62 patients: 46 with DS and 16 with OS. The study was approved by the institutional ethics committee of our university (Protocol No: 2024/2207).
Data Collection
Patient demographics and clinical data—including age, sex, type of syndrome, comorbidities, type of surgery, need for intensive care unit (ICU) admission and duration, perioperative and postoperative complications, length of hospital stay, emergency admissions, and need of readmission to the hospital or ICU within 1 month postoperatively—were collected from records and verified via telephone interviews with the families.
Surgical Technique and Postoperative Follow-Up
All surgeries were performed under general anesthesia. All patients underwent total tonsillectomy using the classical cold dissection technique. Hemostasis was achieved by ligating the tonsillar inferior poles and bleeding areas with 3-0 Vicryl sutures. Adenoidectomy was performed transorally using cold curettage without the use of bipolar or monopolar cautery. In patients with adenoid hypertrophy and serous otitis media, who presented with symptoms such as snoring, apneic episodes during sleep, or hearing loss, adenoidectomy and/or VT insertion were also performed. All procedures were performed at our tertiary university hospital by experienced otolaryngologists.
All patients, including those transferred from the ICU, were routinely monitored in the inpatient unit for 1 day postoperatively. Oral hydration with water was encouraged starting at postoperative hour 2, followed by soft/liquid oral feeding by hour 4. In cases of insufficient oral intake, intravenous fluids were given. Oxygen saturation was monitored via pulse oximetry. Patients were routinely scheduled for follow-up visits at 1 week and 1 month after surgery.
Statistical Analysis
Statistical analyses were performed using IBM SPSS Statistics 30.0 (IBM Corp, Armonk, NY, USA). Normality of continuous variables was assessed via the Shapiro–Wilk test, Q–Q plots, and evaluation of skewness and kurtosis. Categorical variables were presented as counts and percentages (n, %) and were compared using the chi-square test or, when appropriate, Fisher’s exact test or Fisher–Freeman–Halton test. For continuous variables, independent t-test and Mann–Whitney U test were used. A P-value <.05 was considered statistically significant.
Results
Patient Characteristics
Of the 62 patients included in the study, 46 (74.2%) were diagnosed with DS, and 16 (25.8%) had OS. The types and characteristics of the syndromes in the OS group are summarized in Table 1.9,10,24-35
Distribution of Other Syndromes by Genetic Etiology.
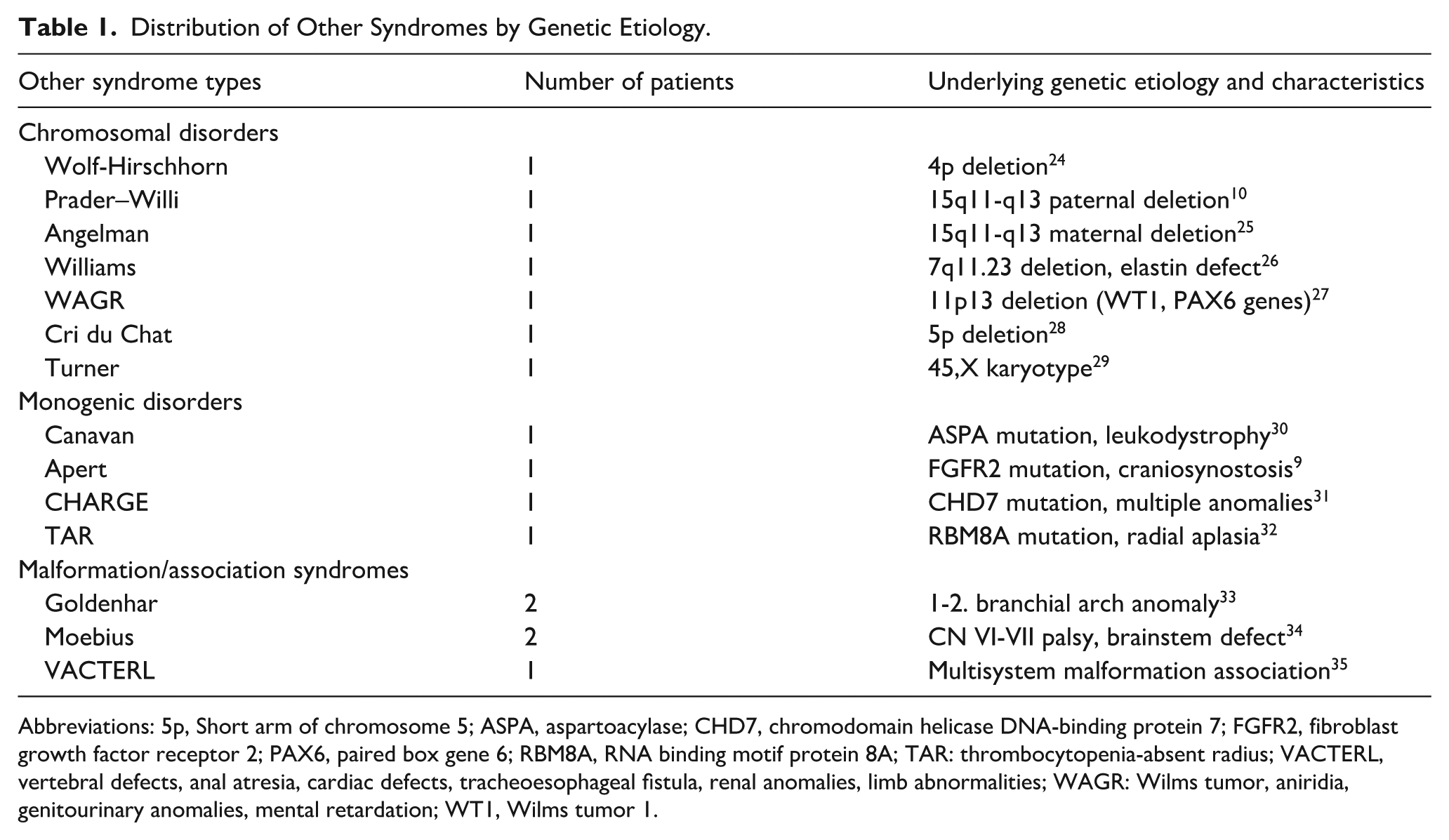
Abbreviations: 5p, Short arm of chromosome 5; ASPA, aspartoacylase; CHD7, chromodomain helicase DNA-binding protein 7; FGFR2, fibroblast growth factor receptor 2; PAX6, paired box gene 6; RBM8A, RNA binding motif protein 8A; TAR: thrombocytopenia-absent radius; VACTERL, vertebral defects, anal atresia, cardiac defects, tracheoesophageal fistula, renal anomalies, limb abnormalities; WAGR: Wilms tumor, aniridia, genitourinary anomalies, mental retardation; WT1, Wilms tumor 1.
Among all patients, 29 (46.7%) were male and 33 (53.2%) were female. Sex distribution was similar between groups: 47.8% male in DS and 43.7% in OS (P = .778). Median age was 6 years overall (IQR: 4-8), with no significant difference between DS (6 [IQR: 4-7]) and OS (6.5 [IQR: 4-8.5]) groups (P = .189). The main indications for surgery were sleep-disordered breathing (SDB) due to adenotonsillar hypertrophy (51 patients, 82.3%) and recurrent tonsillitis (16 patients, 25.8%), with 5 patients presenting with both conditions.
Comorbidities were observed in 90.3% (56/62) of all patients, with similar rates in DS (89.1%, 41/46) and OS (93.8%, 15/16) groups (P = 1.00). Cardiac comorbidities were the most common in the overall cohort (50%) and in the DS group (56.5%), whereas neurological comorbidities predominated in the OS group (68.8%). Endocrine comorbidities were significantly more frequent in DS (50.0% vs 12.5%, P = .009), whereas neurological comorbidities were more common in OS (68.8% vs 32.6%, P = .012). No significant differences were observed between groups for other comorbidity subtypes (Table 2).
Demographics. a
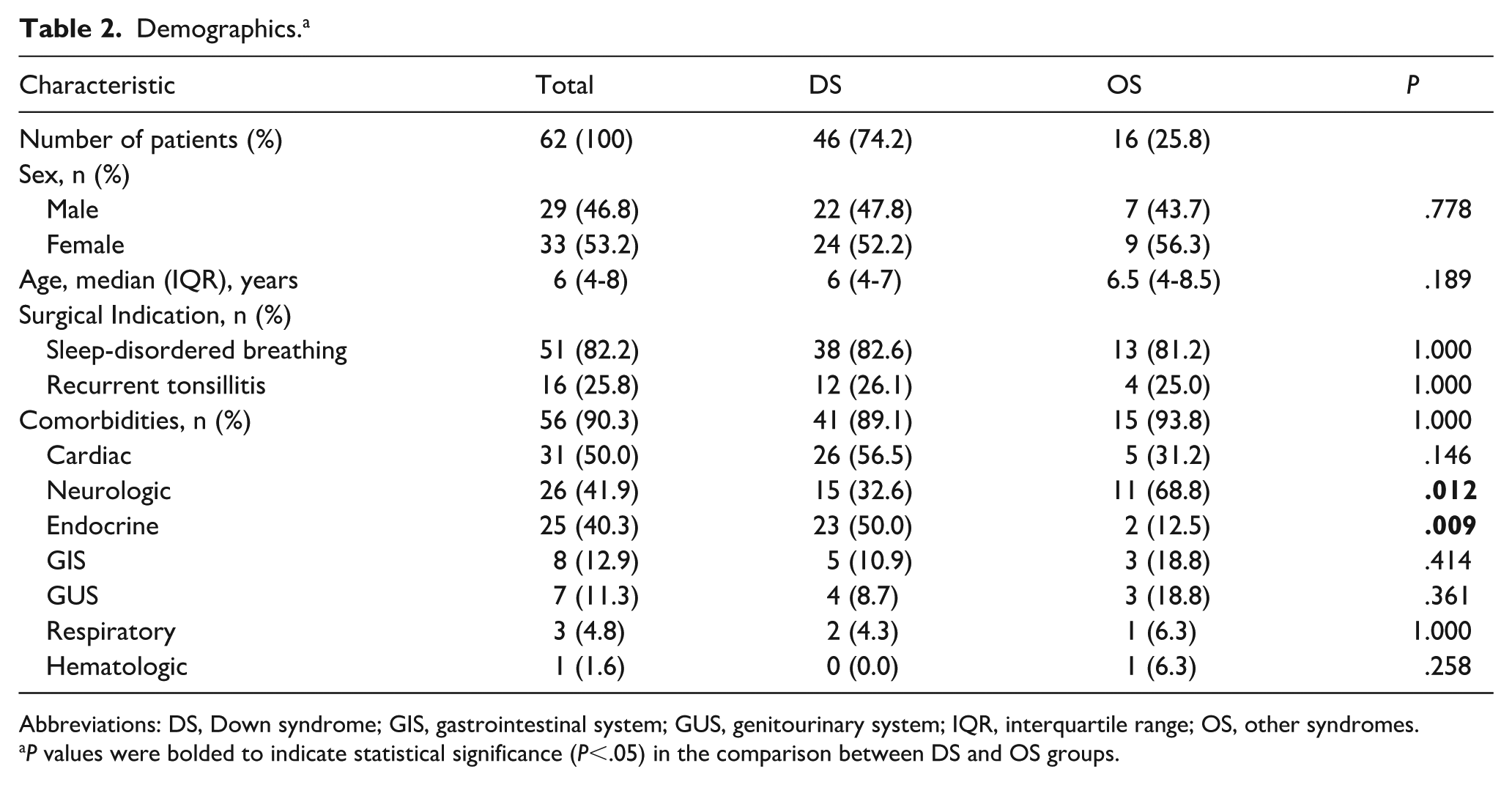
Abbreviations: DS, Down syndrome; GIS, gastrointestinal system; GUS, genitourinary system; IQR, interquartile range; OS, other syndromes.
P values were bolded to indicate statistical significance (P<.05) in the comparison between DS and OS groups.
Operative and Postoperative Findings
Operative and postoperative findings, along with 1-month follow-up data, are presented in Table 3. AT was performed in 82.3% of patients, while 17.7% underwent tonsillectomy alone. VT insertion was performed in 25.8% of cases.
Operative and Postoperative Findings, 1-Month Follow-Up. a
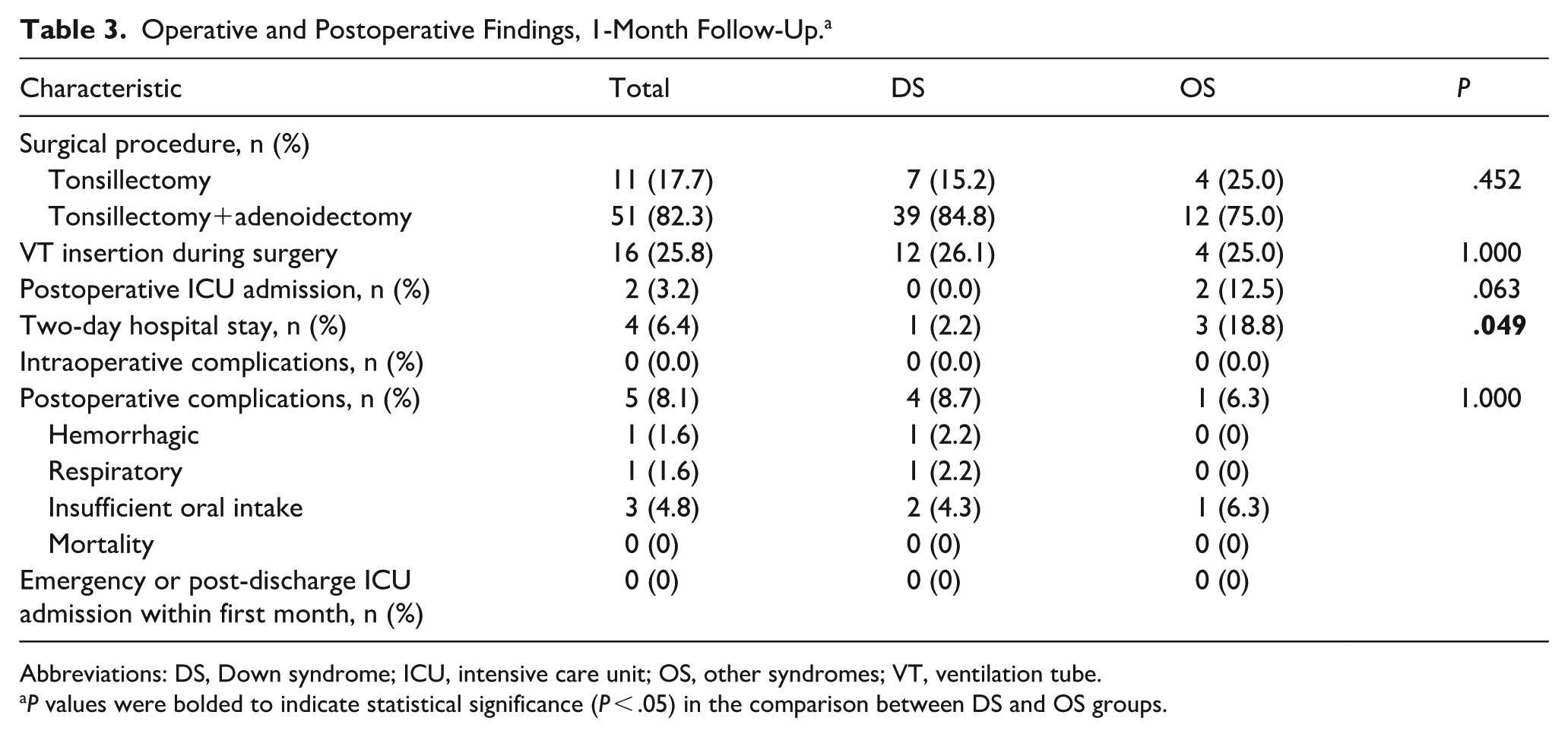
Abbreviations: DS, Down syndrome; ICU, intensive care unit; OS, other syndromes; VT, ventilation tube.
P values were bolded to indicate statistical significance (P < .05) in the comparison between DS and OS groups.
Two patients in the OS group (Prader–Willi and Turner syndromes) were admitted to the ICU postoperatively, as planned preoperatively, for close monitoring. In contrast, none of the patients in the DS group required ICU care.
The median length of hospital stay was 1 day in both groups (IQR: 1-1). Two-day hospital stay occurred in 18.75% of OS patients (3/16) and in 2.2% of DS patients (1/46). All other patients in both groups were discharged after 1 day. This difference was statistically significant (P = .049).
No intraoperative complications occurred in any of the patients. Postoperatively, complications were observed in 8.1% (5/62) of all patients: 8.7% (4/46) in the DS group and 6.3% (1/16) in the OS group, with no statistically significant difference between groups (P = 1.00).
One patient with DS required reoperation within the first 24 hours due to bleeding from the inferior pole of the tonsillar fossa, which was successfully managed by hemostasis using surgical ligation. Another patient with DS developed oxygen desaturation (<90%) and wheezing at postoperative hour 6; bronchospasm was suspected and treated with inhaled bronchodilators (salbutamol and ipratropium) along with 2 L/min nasal oxygen. The patient was monitored overnight with pulse oximetry and was discharged on postoperative day 1 in stable clinical condition. Three patients (2 DS and 1 Moebius syndrome) required intravenous fluid therapy with normal saline and dextrose-containing Ringer’s lactate due to insufficient oral intake. No patients required an emergency department visit or ICU admission after discharge, and no perioperative mortality was observed in the cohort.
Discussion
Syndrome Groups
The majority of our cohort consisted of patients with DS (n = 46), while the remainder were classified as OS (n = 16). Although conditions such as VACTERL, Moebius, and Goldenhar do not meet the classical definition of genetic syndromes, they were included in the OS group due to their multisystem congenital anomalies and the increased perioperative risk perceived by clinicians.
Surgical Indications and OSA Management
In our cohort, surgical indications were SDB due to adenotonsillar hypertrophy in 82.3%, recurrent tonsillitis in 25.8%, and both conditions in 8.1%. These proportions are similar to previous reports, where SDB accounted for 82.5% and recurrent tonsillitis for 20.3% of indications, 36 and are also in line with another series in which upper airway obstruction represented 61.7% and recurrent tonsillitis 18.1%. 37 Although polysomnography (PSG) is considered the gold standard for diagnosing OSA, preoperative PSG data were unavailable in our study. The diagnosis of SDB was instead based on symptoms, history, physical examination, and in some cases, video documentation of apneic episodes during sleep.
The treatment of OSA in pediatric populations, particularly in syndromic patients, is of critical importance due to its association with growth retardation and behavioral disorders.38,39 For patients with mild OSA, anti-inflammatory therapies such as intranasal steroids may serve as a first-line treatment.40,41 AT is the primary surgical treatment when medical therapy is insufficient. AT has consistently been shown to improve OSA symptoms in DS and other syndromic patients such as Prader–Willi, CHARGE, and Apert syndromes, although complete resolution is uncommon.9,11,31,42 In our study, syndromic patients with mild OSA symptoms were initially managed preoperatively with intranasal corticosteroids and nasal irrigation. Surgical intervention was reserved for those who did not respond to this conservative approach. Therefore, when determining surgical indications in syndromic patients, clinicians must carefully weigh the risks and benefits and consider multidisciplinary consultation when necessary.
Postoperative Complications and Mortality
In our cohort, the overall postoperative complication rate was 8.1% (5/62), including 1 respiratory event (1.6%), 1 case of bleeding (1.6%), and 3 cases of insufficient oral intake (4.8%). No perioperative complications were observed. None of our patients required noninvasive or invasive respiratory interventions, including mechanical ventilation and tracheostomy, which is similar to the findings of Goldstein et al 17 Only one DS patient developed bronchospasm 6 hours postoperatively, which resolved with inhaled bronchodilators. Notably, one patient with insufficient oral intake had Moebius syndrome, whereas the remaining complications occurred in DS patients.
Baker et al 20 analyzed 353 DS patients and 7159 non-DS patients who underwent tonsillectomy with or without adenoidectomy. In the large control group, the respiratory complication rate was 1.5% and the bleeding rate was 1.2%. They reported a higher incidence of postoperative bleeding (2.8%) in the DS group, while respiratory complication rates (1.4%) did not significantly differ from those in the control group. Our findings regarding respiratory and hemorrhagic complication rates are comparable to both groups in this study, but are particularly consistent with the rates observed in the healthy control group. However, unlike our series, this study did not provide data on insufficient oral intake, which represents a clinically relevant complication in syndromic patients.
Due to heterogeneity in the definitions of complications and differences in retrospective analysis methodologies across studies, varying incidence rates have been reported in the literature. In the DS cohort reported by Cottrell et al, 36 the postoperative complication rate was 31.5%, including respiratory (17%), hemorrhagic (5.6%), and insufficient oral intake (11.6%) events. In contrast to our findings and other reports, the high complication rates in that study likely reflect the combination of several factors: low thresholds for complications, the retrospective analysis spanning 27 years, and practice changes over that period, including earlier opioid use that may have contributed to higher respiratory morbidity.
The complication rates in the OS and DS groups were comparable (6.3% vs 8.7%). Due to the limited number of events, statistical comparison based on complication type was not feasible. In addition, 90.3% (56/62) of our patients had comorbidities, either as components of their syndrome or as additional conditions, most commonly cardiac (50.0%), neurological (41.9%), and endocrine (40.3%) disorders. Given the low complication rates in our series despite the high prevalence of comorbidities, our study was not designed to specifically assess the potential impact of comorbidities on postoperative outcomes. Several studies in the literature have investigated the influence of syndromic and non-syndromic comorbidities on postoperative complications following AT. In a large retrospective study conducted by Gehrke et al, 43 children with craniofacial or syndromic abnormalities had increased susceptibility to postoperative complications following AT. Similarly, multiple studies have shown that children with DS are at increased risk of postoperative respiratory complications and may require support ranging from oxygen therapy to invasive interventions.11,17,44 However, one study reported that comorbidities did not significantly impact perioperative risk. 45
The reported mortality rates following tonsillectomy in pediatric patients range from 0.04% (1/2360) in hospitalized patients 46 to 0.0055% (1/18,111) during a 2-week follow-up period. 47 In our series, no mortality was observed. The literature supports that mortality remains low even in high-risk pediatric populations. 36 However, in a large population-based study, the overall mortality rate for AT in children was 0.007%, while in those with complex chronic conditions it was markedly higher at 0.117%. 48 Although rare, a case of postoperative death due to arrhythmia in a patient with Williams syndrome has also been documented. 26
Our findings indicate that AT can be safely performed in this pediatric population, which is generally considered high-risk, when comprehensive precautions are taken. These include careful evaluation, appropriate surgical indication, preoperative multidisciplinary consultation, postoperative ICU admission when necessary, and close postoperative monitoring with early intervention, all of which contribute to achieving low complication rates.
ICU Admission and Length of Hospital Stay
In our cohort, 2 patients (3.2%), 1 with Prader–Willi and 1 with Turner syndrome, were admitted to the ICU based on preoperative planning and were transferred to the inpatient unit the following day. No patients required emergency care or unplanned ICU admission within the first postoperative month. In the literature, Lavin et al 23 reported a 2.3% postoperative ICU admission rate following tonsillectomy at a tertiary care center. Even among high-risk pediatric AT populations, only 18.2% of ICU admissions required ICU-specific interventions. Their study emphasized that extended monitoring in the post-anesthesia care unit during the first 2 postoperative hours had a 93.8% negative predictive value for ICU necessity. Consistent with these findings, we also closely monitored high-risk patients in the post-anesthesia care unit during the early postoperative period.
The mean length of stay in our cohort was notably short at 1.06 days. Four patients required a 2-day hospitalization: 1 DS patient due to postoperative bleeding, 1 Goldenhar patient due to recent epilepsy and cardiology-initiated ECG monitoring, and 2 OS patients with planned ICU admissions. Previous studies have reported prolonged hospital stays in DS patients, often attributed to delayed oral intake and respiratory complications.17,44 Bower and Richmond 44 reported a mean length of stay of 2.1 days, Goldstein et al 17 reported 1.6 days, and Yumusakhuylu et al 19 reported 1.26 days. Compared with these reports, our shorter duration may be attributed to the low complication and ICU admission rates in our cohort. Although the OS group had a statistically significantly higher rate of 2-day hospital stay compared to the DS group (18.8% vs 2.2%), this finding should be interpreted with caution due to the limited sample size, borderline statistical significance, and the influence of 2 planned ICU admissions in the OS group.
Strengths and Limitations
The strengths of our study include the use of a uniform surgical technique, procedures performed at a single tertiary care center, and the inclusion of patients with rare or previously unreported syndromes. However, some limitations should be noted. These include the retrospective design, involvement of multiple surgeons (despite a standardized approach), the heterogeneity of the OS group, absence of PSG-confirmed diagnosis of OSA, and a relatively small sample size. Despite its limitations, this study offers important insights into the safety of AT in syndromic children, who are often considered high-risk surgical candidates and are thus commonly referred to tertiary care centers.
Conclusions
In syndromic patients, no severe postoperative complications or mortality were observed after AT, and the complication rates were comparable between the patients with DS and patients with other syndromes (OS). In the vast majority of patients, a 1-day hospital stay was sufficient, and postoperative ICU care was required only in a very limited number of cases.
This study demonstrates that AT can be performed safely not only in children with DS, but also in those with less commonly studied syndromes, when performed with careful patient selection and appropriate perioperative management. Our findings highlight the need for larger, prospective studies to further clarify outcomes in this high-risk population.
Footnotes
Ethical Considerations
This article received approval from the Istanbul University Istanbul Faculty of Medicine Ethics Committee (Protocol Number: 2024/2207).
Consent to Participate
Written informed consent was obtained from the legal guardians of all participants.
Author Contributions
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
