Abstract
Background:
Microplastics are widespread in nature and have been detected in various human tissues and organs. They are thought to contribute to the occurrence and development of various diseases.
Objectives:
To explore the relationship between microplastic exposure and allergic rhinitis (AR).
Materials and Methods:
Thirty-three patients with AR and 22 individuals in the control group were included in this study. All the participants completed the total nasal symptom score (TNSS) and nasal irrigation. The nasal irrigation solution was under microplastic analysis.
Results:
There were no significant differences in age and gender between the AR group and the control group. A statistically significant difference was noted in the TNSS questionnaire scores between the groups (
Conclusions and Significance:
The concentration of microplastics in the nasal cavities of patients with AR was significantly higher than that in healthy individuals.
Introduction
Since the term “microplastics” was first introduced 2 decades ago, 1 public awareness of microplastic pollution has significantly increased, and various strategies to tackle microplastic pollution have been considered in international discussions. 2
Microplastics, defined as plastic particles smaller than 5 mm, are prominent environmental pollutants widely present in both natural ecosystems and the human body. 3 These particles, resulting from the fragmentation of larger plastic debris or as direct manufacturing byproducts, are now detected in various compartments of the environment, including air, water, and even within our tissues. 4 Recent studies have documented the presence of microplastics in various human tissues, such as the lungs, placental tissues (both maternal and fetal), breast milk, and blood, highlighting the alarming extent of their distribution.5 -8
The association between microplastics and human health is a growing concern, with evidence suggesting that these particles can be inhaled and lodged in the respiratory tract, potentially leading to inflammation and other adverse health effects. 9 Allergic rhinitis (AR), a common allergic disorder with a multitude of allergens, may have microplastics as an additional, yet underexplored factor contributing to its pathogenesis. 10
This study aimed to investigate the relationship between AR and microplastics, exploring the possibility that these ubiquitous particles could play a role in the development or exacerbation of allergic symptoms. Comprehending this relationship is essential for public health, as it may provide new insights into the etiology of allergic diseases and inform strategies for prevention and management.
To quantify microplastics in nasal irrigation fluid, we adopted a 2-step workflow: (i) alkaline digestion with KOH at 50 °C for 24 h to remove organic matter, followed by filtration through 50 μm nylon membranes; (ii) optical microscopy enumeration under a clean-room environment. This method was chosen for its simplicity and low cost, yet we acknowledge its limitations in polymer identification and particle-size resolution compared with spectroscopic or thermal techniques. A detailed comparison of alternative approaches is provided in the discussion section.
Materials and Methods
Clinical Materials
This study was approved by the Ethics Committee of the Peking University International Hospital. Patients aged 18 to 65 years with AR were recruited from the outpatient of otorhinolaryngology, between January 2024 and March 2024. AR was diagnosed by skin prick test or s-IgE (specific immunoglobulin E). Exclusion criteria were sinusitis with/without polyps, acute respiratory infection, or immunotherapy within the preceding 12 months. Also, outdoor workers were excluded from this study. Both the experimental and control groups were indoor workers who were not exposed to air pollution. All participants stopped the local nasal treatment for 2 weeks, including nasal irrigation and nasal sprays. A total of 33 AR patients were enrolled in this study.
The control group consisted of 22 healthy volunteers matched for age and sex and with no history of nasal disease or clinical manifestations. The other inclusion and exclusion criteria are the same as the observation group. After all participants signed the informed consent form, they completed the total nasal symptom score (TNSS; 0-4 points for each of the 4 major symptomatology scores of nasal obstruction, itchy nose, runny nose, and sneezing, for a total of 16 points). 11 Participants completed nasal irrigation under the guidance of a physician, using 40 mL of saline for the bilateral nasal cavity, and they were collected in sterile glass tubes. The saline solution for nasal irrigation is contained in a glass bottle, and the irrigated saline is collected in a glass container. The bottles and the saline are exactly the same. The sample collection process strictly avoided contamination from the plastic products.
Microplastics Analysis
Digestion was performed using potassium hydroxide solution at 50°C for 24 h to eliminate organic substances from each collected sample. A potassium hydroxide solution was prepared by dissolving 150 g of potassium hydroxide in 500 mL of deionized water. First, 1 sample was placed in a 500 mL beaker. Next, 100 mL of potassium hydroxide solution was added to the breaker. The solution was covered with tin foil to prevent contamination and evaporation. The breaker was then placed on a constant heater to maintain a temperature of 50°C for 24 h. The solution was stirred using a magnetic stirrer at 160 rpm for complete digestion. After digestion, the digestive fluid was filtered through nylon Whatman filter paper with a pore size of 50 μm to remove any remaining microplastics. The filter paper was then rinsed with distilled pure water for 15 s. According to ISO standard 24187, 12 organic and inorganic matter are removed by digestion. The microplastics were left in the filter paper. The filter paper containing microplastics was transferred to a clean glass petri dish and dried for 24 h. Sample processing was conducted in a high efficiency particulate air (HEPA)-filtered environment, and blank control samples were used. The morphology and the amount of microplastics on the filter paper were directly examined and counted using an optical microscope (XSP-10C [Shanghai No.6 Optical Instruments Factory]). The laboratory personnel followed protocols to minimize plastic contamination during processing.
Statistical Analysis
Statistical analyses were performed using the SPSS (IBM) version 20.0. Variables following a normal distribution were reported as mean ± standard deviation, whereas those not following a normal distribution were described using the median (interquartile range). Intergroup comparisons were performed using the independent-samples Mann-Whitney
Results
Clinical Results
A total of 33 people were enrolled in the AR group and 22 people in the control group, and the clinical data are shown in Table 1. The ratio of males to females in the AR group was 1:1.2, and that in the control group was 1:1.4, and there was no statistically significant difference (
Demographic Characteristics and Microplastic Density.
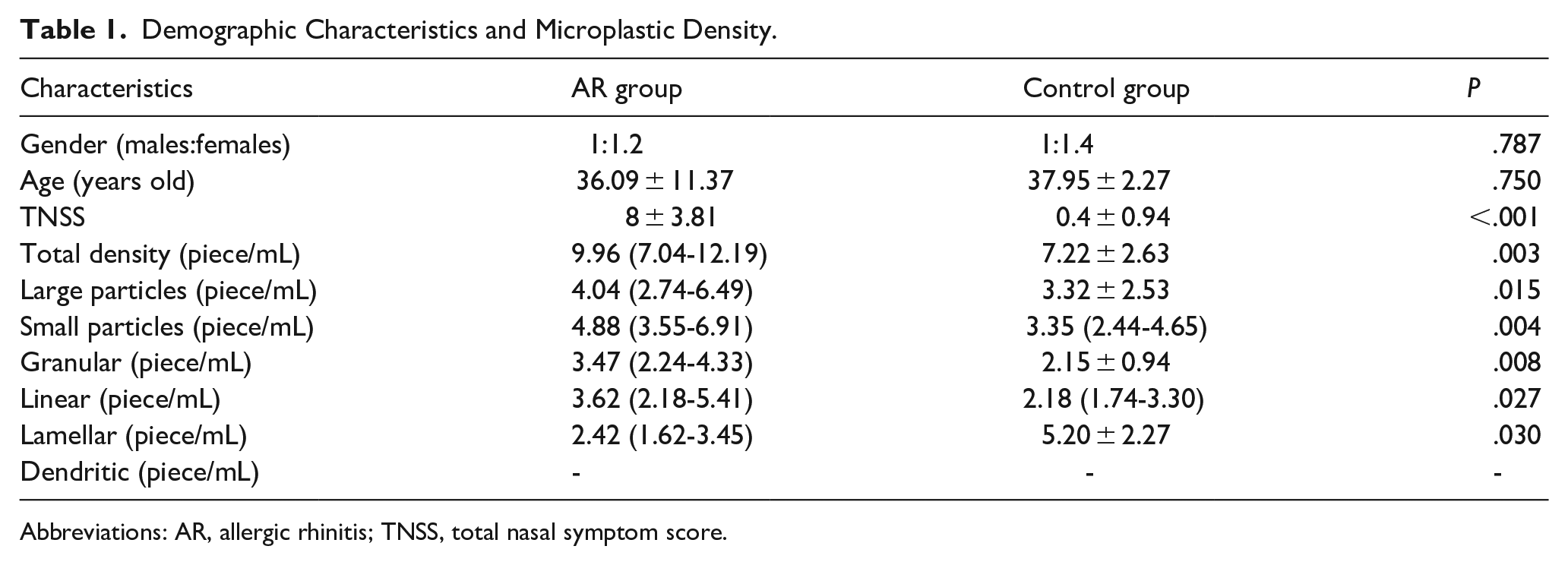
Abbreviations: AR, allergic rhinitis; TNSS, total nasal symptom score.
Microplastics Results
These microparticles were verified to be microplastics by microscopic infrared spectroscopy. The microplastics found in this study were categorized into large particles (maximum diameter >50 μm) and small particles (maximum diameter ≤50 μm) in terms of diameter, and granular, linear, lamellar, and dendritic (no distinction between large and small particles) in terms of morphology (Figure 1). The percentage of microplastics in the AR group is shown in Figure 2. The large and small particles were almost evenly distributed, accounting for approximately half each. Granular particles were the most common among the small particles, and linear particles were the most common among the large particles. The mean distributions of the AR group and control groups are shown in Figure 3. The density of microplastics in the AR group was significantly higher than that in the control group. All subgroups were statistically significant, except for dendritic microplastics (Table 1). Correlation analysis between microplastic density and TNSS revealed a positive association (ρ = 0.373,

Microscopic image of microplastics in nasal irrigation solution (a, small granular; b, large granular; c, small linear; d, large linear; e, small lamellar; f, large lamellar; g and h, dendritic). The arrows indicate various types of microplastics.
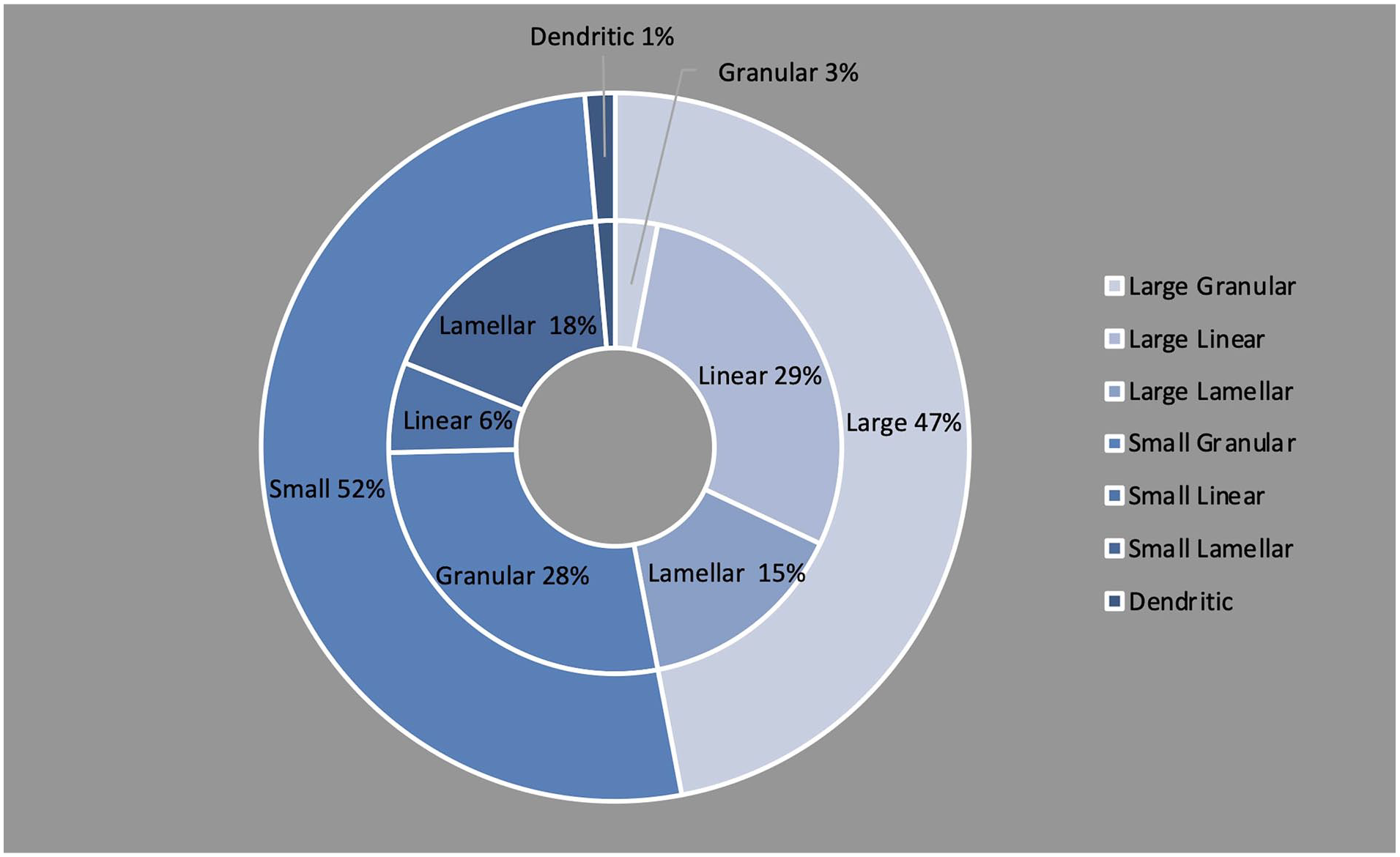
The proportion of microplastics in nasal irrigation fluid in the allergic rhinitis group.
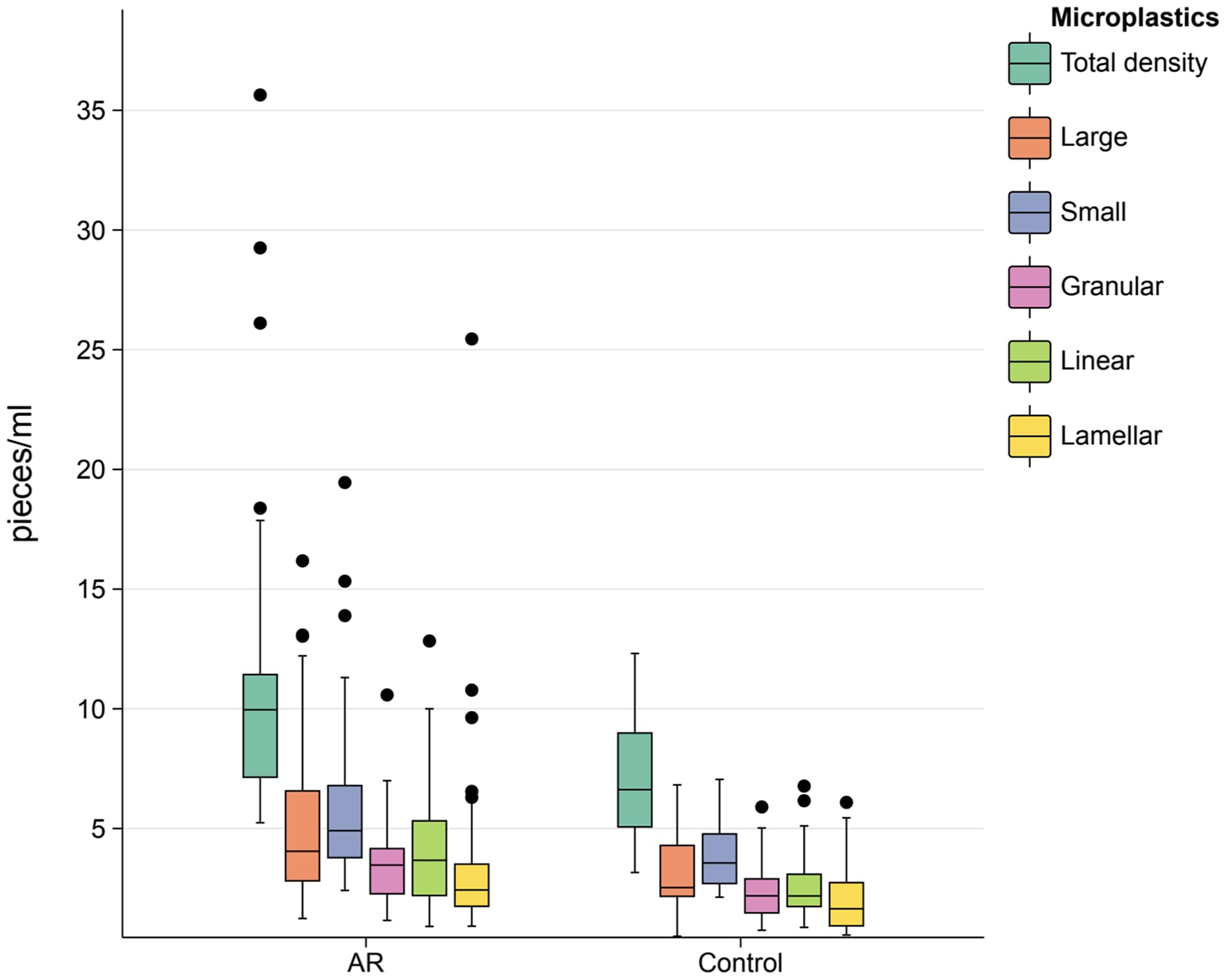
Comparison of microplastics in the allergic rhinitis and control groups.
Discussion
Microplastics are present in the natural world and even in the human body. 7 Microplastics can enter the respiratory tract and lungs, from which we can infer that they also adhere to the nasal cavity.7,9,13,14 This study aimed to investigate the relationship between AR and nasal microplastics. We analyzed the microplastic content in the nasal irrigation of patients with AR, which was statistically significant when compared to the control group. The particle size distribution was relatively balanced, with approximately equal proportions of larger and smaller particles, each accounting for ~50%. Granular particles were the most common among the small particles, and linear particles were the most common among the large particles.
Several techniques exist for analyzing microplastics in nasal secretions. Density separation plus gravimetry, as used here, is inexpensive and rapid but lacks polymer specificity and is prone to false positives from organic debris. Fourier-transform infrared spectroscopy (FT-IR) and μ-Raman offer unequivocal polymer identification with detection limits of 20 to 50 and <1 µm, respectively, yet are equipment-intensive and susceptible to biological-matrix interference. Thermal desorption-gas chromatography-mass spectrometry (GC/MS) provides quantitative mass data with high sensitivity (<1 µg) but cannot size particles <50 µm and demands specialist pyrolysis setups. Scanning electron microscopy with energy dispersive X-ray spectroscopy (SEM-EDS) supplies high-resolution morphology and elemental mapping but is labor-intensive and costly. We therefore combined density separation with random FT-IR spot-checks (25% of particles) to balance throughput, cost, and reliability, and propose full spectroscopic validation in future larger studies.
Jiang et al 15 reported that microplastic particles were detected in the nasal lavage and sputum of both delivery personnel and office workers, and the content in delivery workers is much higher than that of office workers. Taş et al 16 first found microplastics in the nasal lavage of patients with chronic rhinosinusitis without nasal polyps, which was significantly higher than that in controls. Subsequently, microplastics were detected in the nasal lavage fluid of patients with AR. 17 Therefore, they deduced a correlation between microplastics and the development of chronic rhinosinusitis and AR. This is consistent with our finding that microplastics were found in the nasal cavities of healthy individuals and that the number of microplastics in the nasal cavities of AR patients was markedly higher than that in healthy individuals. Given the cross-sectional nature of this pilot study, we cannot establish whether microplastics precede AR onset or merely reflect increased deposition in inflamed mucosa.
Prata et al 4 concluded that larger particles of microplastics are retained in the upper respiratory tract, and that the nasal cavity is the first barrier in the respiratory tract, blocking large microplastic particles. However, in our study, the nasal cavity contained almost equal proportions of large and small microplastic particles. Jenner et al 18 found a variety of microplastics in lung tissue, with maximum diameters ranging from 12 to 2475 μm. This shows that the size of the microplastics is not an influential factor in their entry into the respiratory tract. In addition to respiratory exposure, Dzierżyński et al 5 summarized other ways in which microplastics have the potential to enter the human body, including gastrointestinal and skin contact exposure.
Based on the pathogenesis of microplastics in the lungs, 18 we hypothesized that the pathogenesis of microplastics in AR is as follows.11,19 After entering the nasal cavity, microplastic particles may act as foreign bodies or adsorbed substances on the surface of microplastics, causing physical stimulation of the nasal mucosa and triggering local inflammatory reactions. Second, microplastic particles may be recognized and phagocytosed by the immune cells of the nasal mucosa, which activates the immune system. Finally, exposure to microplastics may change the structure of microbial communities in the nasal cavity, destroying the original microbial balance, which may trigger or exacerbate AR. 7
The present study has limitations that should be acknowledged. The achieved sample size (n = 33 in the experimental group and n = 22 in controls) fell short of the 52 participants per arm indicated by our post hoc power calculation (α = .05, power = 0.80, effect size
Conclusion
In conclusion, this study preliminarily revealed an association between microplastic exposure and AR. However, the limited sample size restricts the broader applicability of the findings. Future studies should focus on expanding the sample size to validate this association and elucidate the specific mechanisms by which microplastics affect nasal immunity and microbiota. These efforts will contribute to a deeper understanding of the interaction between microplastics and respiratory health.
Footnotes
Ethical Considerations
This study was approved by the Ethics Committee of the Peking University International Hospital.
Consent to Participate
Written informed consent was obtained from all participants.
Consent for Publication
All data were obtained with written informed consent to publish.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data can be available in the paper.
