Abstract

Significant Statement
Pseudo-continuous arterial spin labeling (pCASL) provides non-contrast perfusion imaging for hypervascular glomus tympanicum tumors, useful when gadolinium is contraindicated. This report details the first quantitative analysis of a small middle-ear glomus tumor. Its tumor blood flow was lower than values from larger skull base paragangliomas, likely due to its smaller size and distinct arterial supply. pCASL shows promise, but quantitative values may differ based on tumor characteristics.
Introduction
Paraganglioma of the middle ear, also known as a glomus tympanicum tumor, is a rare, highly vascular neoplasm that arises from paraganglionic cells associated with Jacobson’s nerve in the temporal bone. 1 Although generally benign, this tumor can grow insidiously and cause significant morbidity due to its anatomical location and potential involvement of adjacent neurovascular structures. Thus, early and accurate diagnosis is essential for optimal management.
Computed tomography (CT) is a preferred imaging modality, but it does not always provide sufficient specificity to distinguish glomus tympanicum from other middle-ear pathologies. Magnetic resonance imaging (MRI), including T1-weighted, T2-weighted, and contrast-enhanced imaging, is important for providing detailed anatomical information. However, these techniques mainly focus on structural features and may not fully capture the hemodynamic profile of the tumor. Given the hypervascular nature of glomus tumors, advanced functional imaging techniques can offer valuable diagnostic insights.
Pseudo-continuous arterial spin labeling (pCASL) is a noninvasive, noncontrast perfusion MRI technique that quantifies tissue blood flow by magnetically labeling arterial blood water as an endogenous tracer. 2 It provides quantitative perfusion maps without requiring a gadolinium-based contrast agent, making it particularly advantageous for patients with renal impairment or a contraindication to contrast media. Furthermore, fast spin-echo-based pCASL significantly reduces magnetic susceptibility artifacts in the temporal region, unlike some other perfusion techniques. 3
While pCASL has shown promise for hypervascular brain tumors and has been used to characterize various skull base lesions, including skull base paragangliomas, 4 its specific utility and quantitative findings for small glomus tumors confined to the tympanic cavity have not been well-described. In this report, we present a case of glomus tympanicum where pCASL provided valuable information that complemented standard imaging, aiding the preoperative diagnosis.
Case
A 35-year-old woman was referred to our hospital for diagnosis and treatment of a pulsatile reddish mass in the left tympanic cavity. A pure tone audiogram indicated mild conductive hearing loss of 30 dB in the left ear.
CT revealed a mass lesion in the left tympanic cavity that did not extend into the mastoid air cells and showed significant enhancement with contrast agent administration. The ossicles were involved, but there was no evidence of bony destruction (Figure 1A). On MRI, the lesion showed iso-intensity on T1-weighted (Figure 1B) and T2-weighted (Figure 1C) images and was strongly enhanced following gadolinium administration (Figure 1D). Images obtained using pCASL indicated high blood flow, suggesting hypervascularity of the lesion (Figure 2). Quantitative analysis revealed an absolute tumor blood flow (TBF) of 103.32 mL/100 g/min and a normalized TBF (relative to normal-appearing cerebellum) of 2.36.
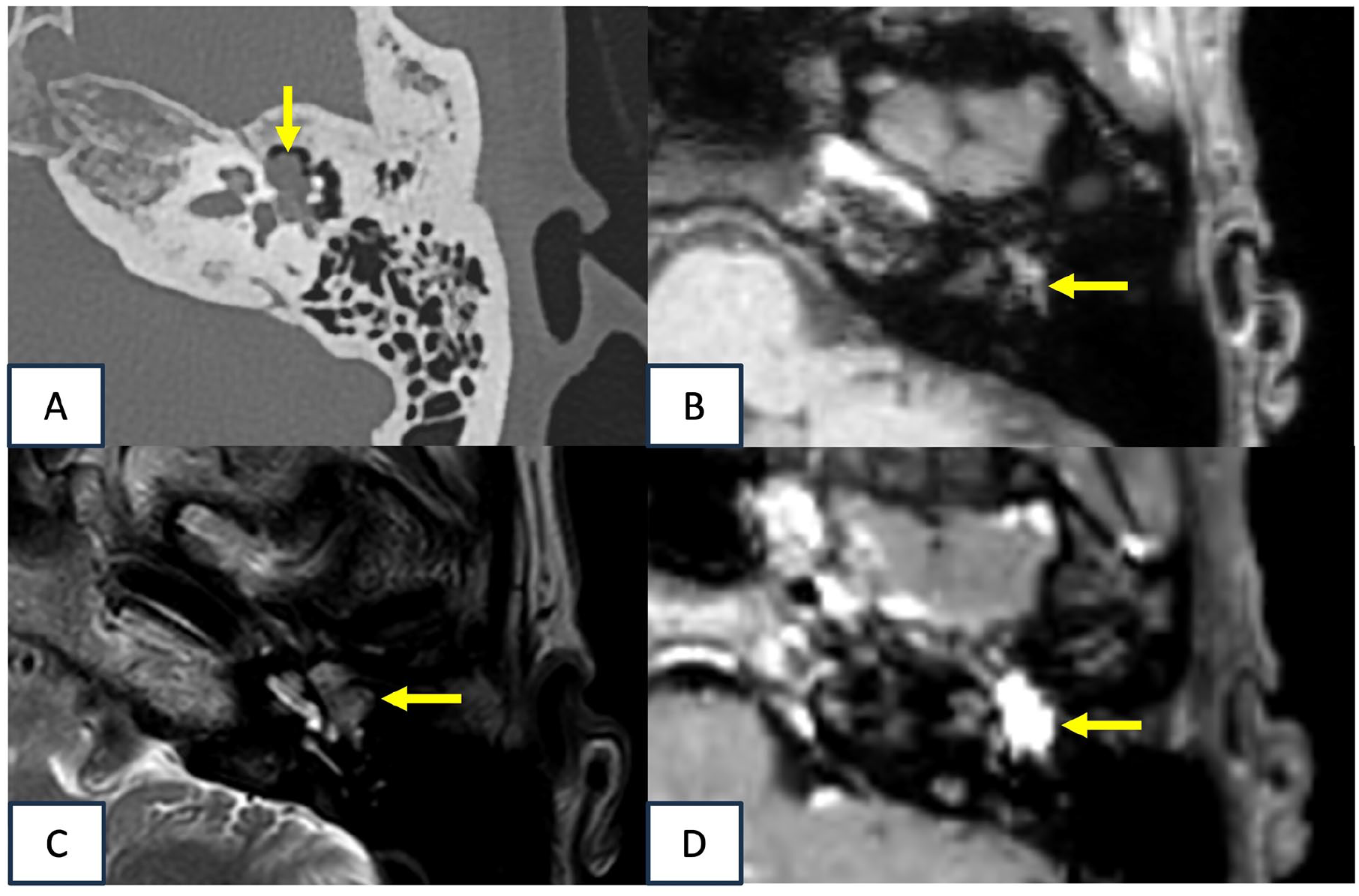
CT and MRI of the left temporal bone. (A) Noncontrast-enhanced CT of the left temporal bone revealed a tumor (arrow) in the left tympanic cavity that involved the ossicles, with no bony erosion. (B) The lesion in the left temporal bone (arrow) gave an iso-intense signal on T1-weighted MRI. (C) The lesion (arrow) also gave an iso-intense signal on T2-weighted MRI, and was located near the cochlea. (D) On contrast-enhanced T1-weighted MRI, the lesion gave a high-intensity signal (arrow). CT, computed tomography; MRI, magnetic resonance imaging.
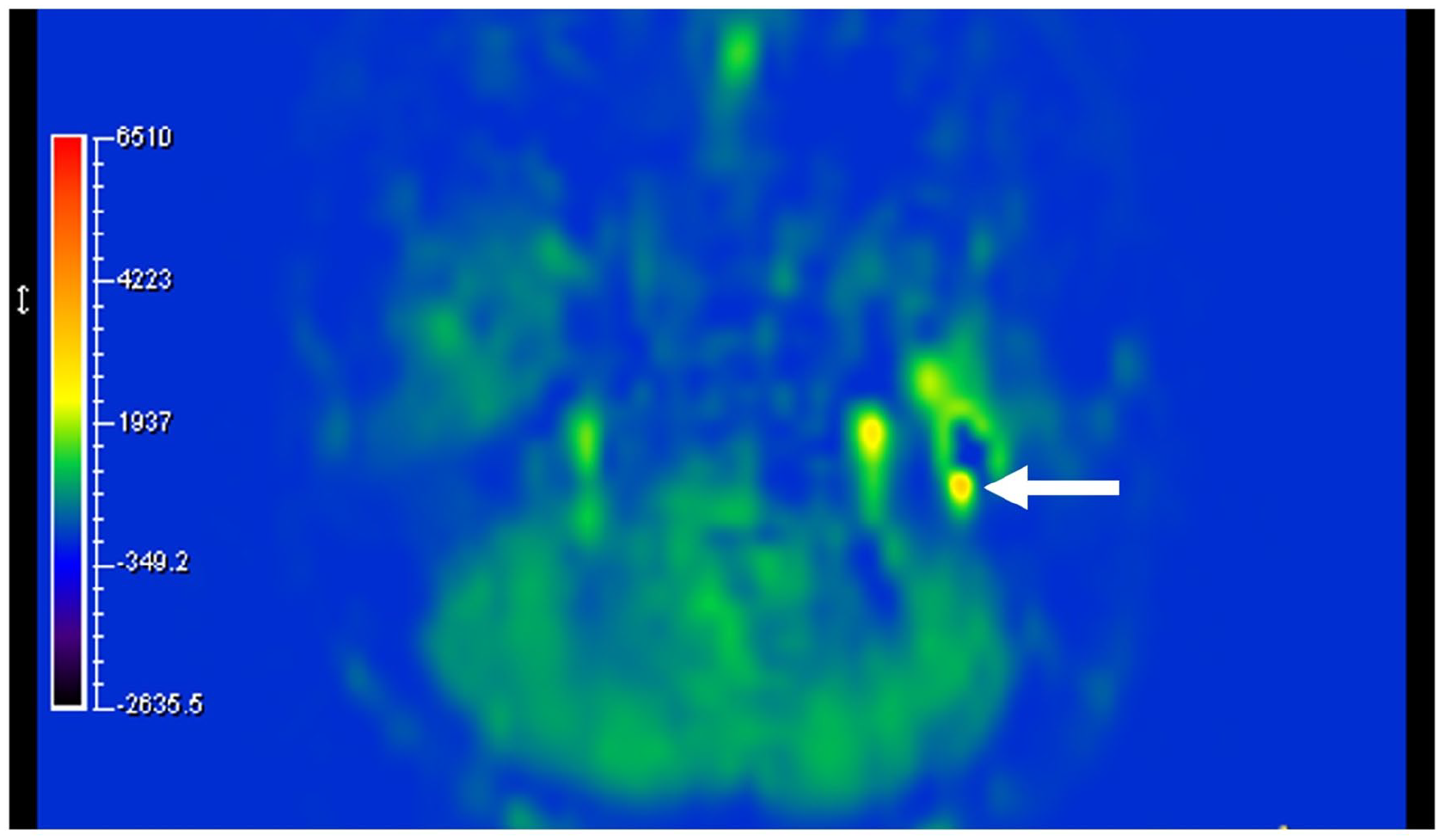
pCASL image of a layer of the skull base. The arrow indicates a tumor with high blood flow. pCASL, pseudo-continuous arterial spin labeling.
The primary differential diagnosis was paraganglioma. I-123 MIBG scintigraphy was negative, and serum catecholamine levels were normal. A biopsy was not performed due to the presumed hypervascularity and risk of bleeding. The patient underwent surgical tumor removal, during which the tumor was confirmed to be hypervascular, as anticipated from the imaging findings. The final histopathological diagnosis confirmed a glomus tumor.
Discussion
This case demonstrates the potential utility of pCASL in the diagnostic workup of glomus tympanicum tumors. While contrast-enhanced CT and MRI are standard for evaluating middle-ear masses, pCASL can offer complementary information about tumor hemodynamics without the need for gadolinium. This is a key advantage in patients where contrast agents are contraindicated. pCASL provides a noninvasive method to confirm the hypervascular nature of a lesion, which can increase diagnostic confidence and aid in differentiating it from less vascular pathologies like cholesteatomas or schwannomas.
An important finding in our case was the quantitative TBF value. The absolute TBF of 103.32 mL/100 g/min, while indicating hyperperfusion relative to surrounding tissue, was lower than the minimum TBF reported for skull base paragangliomas in a previous study by Geerts et al. 4 We speculate this discrepancy is due to 2 factors. First, our patient’s tumor was small and confined to the tympanic cavity. Second, the primary feeding vessel for a glomus tympanicum is the inferior tympanic artery, which may result in different perfusion dynamics compared to larger glomus jugulare tumors that recruit a more extensive arterial supply. This suggests that while pCASL is valuable, clinicians should be aware that TBF values in small, purely tympanic glomus tumors may be lower than those of their larger skull base counterparts.
The question of whether pCASL should be a routine sequence for imaging a middle-ear mass is pertinent. As an additional sequence, it can be feasibly integrated into standard MRI protocols. While it may not replace contrast-enhanced imaging, it serves as a valuable adjunct, particularly for confirming vascularity in ambiguous cases or when contrast cannot be administered.
This case report suggests that pCASL offers valuable information on blood perfusion that can complement the diagnostic capability of preoperative MRI for glomus tumors. Although this is a single case, it highlights a novel application and provides the first quantitative TBF data for a small glomus tympanicum. Further studies are needed to establish normative pCASL values for glomus tumors of varying sizes and to clarify its overall diagnostic value in a broader clinical context.
Footnotes
Informed Consent
Written informed consent was obtained from the patient for publication of this report. Our institution does not require ethical approval for reporting individual cases.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author, HS, upon reasonable request.
