Abstract
Background:
Sinonasal adenoid cystic carcinoma (ACC) is a rare, aggressive malignancy that commonly involves the nasal cavity and paranasal sinuses, with a propensity for perineural invasion and distant spread. Diffusion-weighted imaging (DWI) is a useful tool for evaluating tumor characteristics and monitoring treatment response. This case series aims to review the pre- and post-treatment diffusion characteristics of sinonasal ACC, focusing on the apparent diffusion coefficient (ADC) values.
Methods:
A series of 8 cases of sinonasal ACC that underwent pre- and post-treatment magnetic resonance imaging with DWI were retrospectively analyzed. Circular regions of interest were drawn on representative ADC images of the lesions.
Results:
Pre-treatment mean ADC values ranged from 651 to 1156 × 10−6 mm2/second, while the post-treatment average ADC values ranged from 1351 to 1879 × 10−6 mm2/second. Post-treatment changes in ADC values were observed in all cases, demonstrating an increase in ADC, indicative of positive treatment response.
Conclusion:
This case series suggests that DWI could serve as a non-invasive imaging tool for evaluating post-treatment response of sinonasal ADC. Post-treatment changes in ADC potentially correlate with treatment response and disease progression. Hence, DWI could play a supplemental role in monitoring therapy, highlighting its potential in guiding clinical management decisions for patients with sinonasal ACC.
Introduction
Sinonasal adenoid cystic carcinoma (ACC) is a rare and aggressive malignancy that arises from the epithelial structures of the sinonasal tract. 1 Although it accounts for a small percentage of head and neck cancers, ACC is notorious for its propensity for perineural invasion, local recurrence, and distant metastasis, particularly to the lungs and bones. 2 Due to its indolent growth pattern and late onset of symptoms, ACC is often diagnosed at an advanced stage, which complicates treatment and prognosis. 3 Surgical resection remains the primary treatment modality; however, the role of radiation therapy and chemotherapy, both in adjuvant and palliative settings, is becoming increasingly important for improving outcomes, especially in cases with extensive invasion or recurrence. 4
Accurate pre-treatment staging and post-treatment monitoring are crucial for effective management. 1 Traditionally, imaging modalities such as computed tomography and magnetic resonance imaging (MRI) have been used to assess tumor extent, local invasion, and distant metastasis. 5 While these methods are integral to the diagnostic process, they have limitations in detecting subtle perineural invasion and residual tumor, which is critical for determining the appropriate treatment approach and predicting outcomes. Furthermore, in advanced cases, these imaging modalities may not be sensitive enough to identify early signs of recurrence or treatment response.6,7
In recent years, diffusion-weighted imaging (DWI) has emerged as a promising non-invasive tool for evaluating tumor cellularity based on the movement of water molecules within tissues. 8 Malignant tumors, including ACC, often exhibit restricted diffusion and low apparent diffusion coefficient (ADC) values due to their higher cellularity,9,10 making DWI particularly useful in differentiating malignant from benign lesions. 11 This technique has shown potential in other head and neck cancers for assessing aggressiveness, detecting perineural spread, and monitoring therapeutic response.2,7 In sinonasal tumors such as ACC, DWI can help assess the aggressiveness of the lesion, detect perineural spread, and evaluate the efficacy of therapies such as chemotherapy, radiation, and surgery. 3 Changes in ADC values can be indicative of tumor necrosis, treatment-induced changes, or residual disease. However, the application of DWI in sinonasal ACC remains understudied, and its role in pre- and post-treatment assessment is not yet well defined. 8
There are only a few reports regarding ADC measurements of sinonasal ACC, and there is a paucity of data regarding post-treatment ADC values. Through the analysis of ADC values in a series of patients diagnosed with ACC, this study seeks to evaluate the potential of DWI in assessing both pretreatment and post-treatment cases. Thus, this study will contribute to the small but growing body of evidence supporting the use of advanced imaging techniques like DWI to improve the clinical management and outcomes of patients with sinonasal ACC.
Materials and Methods
Imaging Technique: All MRI examinations were performed on 1.5 or 3 Tesla clinical scanners. DWI was performed using a single-shot planar imaging technique with 2 different diffusion sensitivity coefficients, b-values of 50 and 800 mm2/second. Imaging parameters included a repetition time of 7500 ms and an echo time of 80 ms. The field of view was set at 17 cm, and automatically generated ADC maps were used for analysis.
Data Collection and Analysis: This retrospective study received institutional review board approval and was compliant with Health Insurance Portability and Accountability Act (HIPAA). The institutional database (mPower Radiology Search, Nuance) was searched for cases of pathology-proven ACC with available MRI, and the corresponding patient treatment history was referenced. Circular regions of interest were drawn manually on representative ADC images of the lesions by a neuro-radiologist with certification of added qualification in neuroradiology (Figure 1). The regions of interest were positioned in areas with the lowest mean ADC values in the lesions, while avoiding cystic or necrotic components.
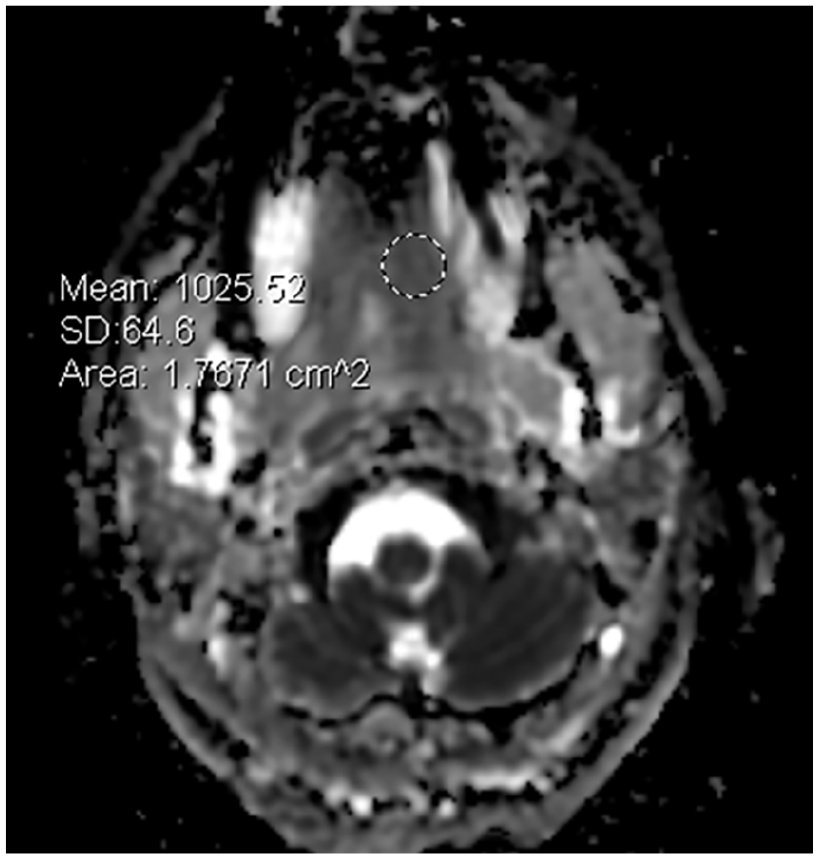
Axial ADC map of a pretreatment sinonasal adenoid cystic carcinoma (Case 1) with region of interest showing a mean ADC value of 1026 × 10−6 mm2/second. ADC, apparent diffusion coefficient.
Results
The ADC values in the evaluation of 8 sinonasal ACC cases, both before and after treatment, along with patient demographics, are listed in Table 1. In this case series, the pre-treatment ADC values ranged from 651 to 1156 × 10−6 mm2/second, with a mean of 928 × 10−6 mm2/second and standard deviation of 176 × 10−6 mm2/second, while the post-treatment average ADC values, after successful interventions such as induction chemotherapy, carbon ion therapy, and adjuvant TFHX therapy, ranged from 1351 to 1879 × 10−6 mm2/second, with a mean of 1659 × 10−6 mm2/second and standard deviation of 292 × 10−6 mm2/second (Figure 2).
ADC Measurements.
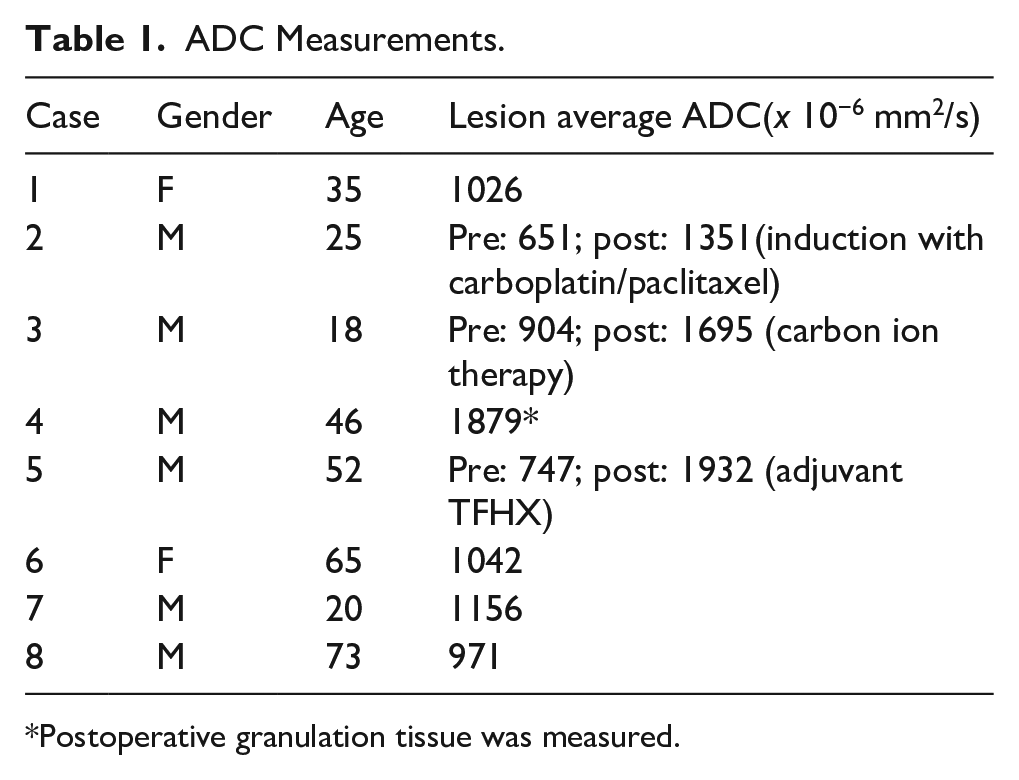
Postoperative granulation tissue was measured.
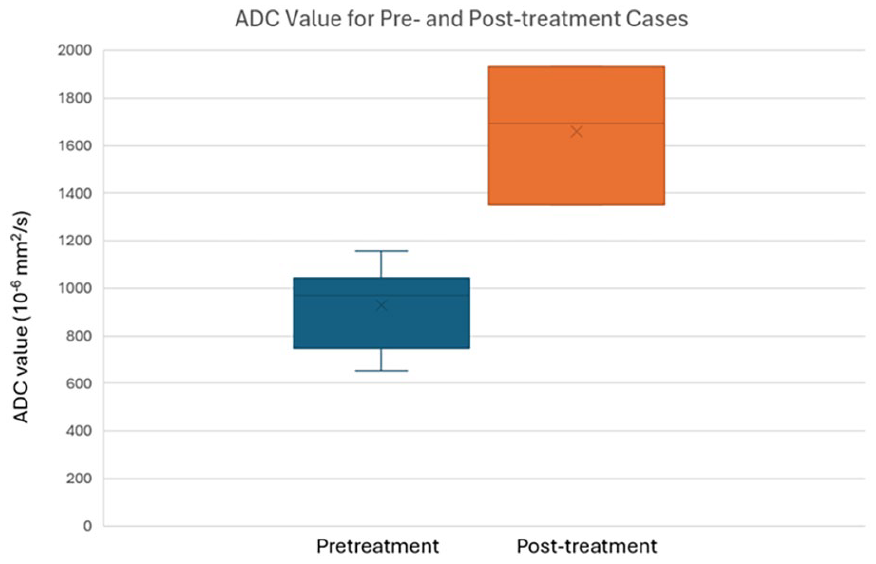
Box and whisker chart showing the ADC measurements for the pre-treatment and post-treatment groups of sinonasal adenoid cystic carcinoma. ADC, apparent diffusion coefficient.
Discussion
The variability in ADC values across cases could reflect differences in tumor differentiation, extent of invasion, and overall aggressiveness. 10 Tumors with more infiltrative characteristics, such as the cavernous sinus invasion seen in Case 2, exhibited lower ADC values, indicating higher cellularity. Conversely, Case 4 (postoperative granulation tissue) had a much higher ADC value, consistent with the lower cellularity of granulation tissue. A cutoff on the order of 1200 to 1300 × 10−6 mm2/second could be used to differentiate the pre-treatment and post-treatment groups based on this small case series. This highlights DWI’s potential not only in detecting malignancy but also in distinguishing tumor from non-tumor tissue post-surgery.6,11 The overall lower ADC measurements in this study versus other reports (1380-1600 × 10−6 mm2/second)12,13 for pretreatment tumors are likely related to the technique in which the lowest ADC values were recorded and perhaps due to differences in tumor grade.
The increase in ADC following induction chemotherapy (Case 2) and carbon ion therapy (Case 3) aligns with known effects of these therapies, which induce tumor necrosis and apoptosis, thereby decreasing cellularity. 7 Notably, Case 5, which received adjuvant TFHX (a combination of chemotherapy and radiotherapy), also demonstrated an increase in ADC post-treatment, further supporting the role of DWI in evaluating therapeutic efficacy.12,14 The ADC value of 1932 × 10−6 mm2/second post-treatment is considerably higher than the pre-treatment value of 747 × 10−6 mm2/second, indicating a decrease in tumor cellularity after adjuvant therapy.
In Case 4, the post-surgical granulation tissue exhibited a higher ADC value (1879 × 10−6 mm2/second) compared to the pre-treatment ADC, which was in the lower range for malignancy. This illustrates the ability of DWI to differentiate between viable tumor tissue and non-tumor tissues, such as postoperative changes like granulation tissue, which typically has lower cellularity and thus higher ADC values. This finding reinforces the importance of DWI in distinguishing between recurrent tumors and benign post-treatment changes, thus aiding in clinical decision-making. In this case series, the difference between pretreatment ADC measurements was lower than the post-treatment measurement.
The overall lower ADC measurements in this study versus other reports (1380-1600 × 10−6 mm2/second)12,13 for pretreatment tumors are likely related to the technique in which the lowest ADC values were recorded, and perhaps due to differences in tumor grade. While DWI can help identify early signs of recurrence and treatment failure, it is important to recognize its limitations.7,10 DWI alone may not be sufficient to differentiate between residual tumor and post-treatment changes, and further histopathological correlation is often necessary. 12 In addition, as the clinical experience with DWI in sinonasal ACC grows, it will be important to establish standardized ADC measurement techniques and ADC thresholds for distinguishing benign from malignant tissues and for evaluating treatment response.
Future studies with larger cohorts and prospective designs are needed to further validate these findings and to investigate the potential of DWI as part of a multimodal imaging strategy for managing sinonasal ACC. Further exploration into the role of DWI in assessing molecular features of ACC and its ability to predict long-term outcomes, such as survival and recurrence, will also be valuable.
Conclusion
This study suggests that DWI can provide insights regarding the pre- and post-treatment assessment of sinonasal ACC. The low pre-treatment ADC values of ACC are consistent with those typically encountered with malignant neoplasms, while post-treatment increases in ADC values might indicate a reduction in tumor cellularity and suggesting a positive treatment response or the presence of granulation tissue. The findings of this study underscore the potential of DWI as a non-invasive imaging modality to monitor treatment efficacy and detect recurrence in patients with sinonasal ACC.
Footnotes
Consent for Publication
Written informed consent for information published in this article was not obtained because it was waived by the IRB.
Author Contributions
M.M.: draft; D.T.G.: data collection, editing, supervision; N.C.: approval of final version.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
