Abstract
Introduction:
Burn injuries have been proven to carry long-term psychological and social consequences.
Objective:
To identify the mental and psychosocial impacts of facial burns on patients’ quality-of-life outcomes.
Methods:
The methods were developed in agreement with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis extensions for Scoping Review guidelines. A literature search utilizing the PubMed and Scopus databases was performed. Peer-reviewed, English-language studies examining psychological, social, or quality-of-life outcomes associated with facial burns were included.
Results:
Anxiety and depression were significantly worse in facial burn patients [Hospital Anxiety and Depression Scale (HADS) score: 2.5 ± 2.8, P < .002, HADS Score: 2.1 ± 2.7, P < .001, respectively]. Body image dissatisfaction was significantly higher in adolescent facial burn patients compared to those without facial burns, 1 year after the injury (P < .001). After undergoing augmented reality coupled rehabilitation, quality of life scores were improved compared to baseline (P < .001).
Conclusion:
This scoping review highlights the negative impacts of facial burns on mental health and psychosocial outcomes. Additional research is needed to further substantiate interventions, such as cognitive behavioral strategies and virtual reality-based rehabilitation, in the long-term management of individuals with facial burns.
Keywords
Introduction
Burn injuries remain a prominent global health issue, killing over 180,000 people annually. 1 Facial burns are a traumatic form of injury, not only due to their physical implications but also because of their profound impact on an individual’s psychological and social well-being. The scarring process for facial burn survivors marks a significant milestone in recovery, still facial burn survivors are likely to face a multitude of lifelong challenges. The visibility of facial burns poses unique challenges, such as social stigma, body image dissatisfaction, and significant mental health disorders. 2 A change in someone’s physical appearance due to facial burns can impact how comfortable they feel interacting and socializing in public. 3 Severe facial burns can diminish a person’s self-esteem and lead to depression. 4 Given these unique challenges, the recovery process for facial burns needs to integrate both the psychological and physical aspects of healing.
It is necessary to address how cultural and social stigma can negatively impact facial burn survivors’ mental health. 5 Facial burn survivors frequently face significant challenges due to the visible scars and disfigurements that result from their injuries. 6 These physical marks can be profound and often do not align with the conventional beauty standards upheld in various cultures around the world. 6 Confronting and mitigating stigma is an important factor in improving the quality of life (QoL) for facial burn survivors.
This scoping review aims to consolidate and examine existing research on the mental health outcomes and psychosocial impacts associated with facial burns. By identifying patterns and gaps in the current literature, this review seeks to highlight the complexities of recovery and inform more targeted, effective interventions for this vulnerable population. Understanding these dynamics is crucial for developing comprehensive care strategies that address both the physical and emotional needs of those affected by facial burns. A holistic review is needed to help implement strategies to address the visible and invisible wounds, such as altered self-esteem, that a facial burn survivor may face. This scoping review can potentially help healthcare providers design interventions that are proactive in addressing the psychological impact of facial burns.
Materials and Methods
A scoping review based on the Preferred Reporting Items for Systematic Reviews and Meta-Analysis Scoping Review guidelines was performed in January 2025.
Search Strategy
Articles were searched in the PubMed database with the following thread of keywords: [“Burns” (MeSH) OR “Facial Burns” OR “Facial burn injury” OR “Face burn” OR “Thermal injury” OR “Chemical burn” OR “Electrical burn”] AND [“Mental Health” (MeSH) OR “Psychosocial impact” OR “Psychological distress” OR “Depression” (MeSH) OR “Anxiety Disorders” (MeSH) OR “Post-Traumatic Stress Disorder” (MeSH) OR “PTSD” OR “Psychological resilience” OR “Coping mechanisms”]
Articles were also searched in Scopus with the following thread of keywords: [TITLE-ABS-KEY (“burns” OR “facial burns” OR “facial burn injury” OR “face burn” OR “thermal injury” OR “chemical burn” OR “electrical burn”)] AND [TITLE-ABS-KEY (“mental health” OR “psychosocial impact” OR “psychological distress” OR “depression” OR “anxiety disorders” OR “post-traumatic stress disorder” OR “PTSD” OR “psychological resilience” OR “coping mechanisms”)]
Eligibility Criteria
Inclusion criteria were peer-reviewed publications investigating the psychological, social, or quality-of-life outcomes associated with facial burns. The search was restricted to human studies published in English. Excluded studies were non-English publications and studies not examining psychosocial outcomes with burn treatment.
Selection of Sources of Evidence
Two reviewers (R.J.H. and J.K.) independently screened all abstracts to identify studies that fulfilled the eligibility criteria. Any disagreement between the reviewers was resolved by a third reviewer (J.E.L.). Qualitative data from each included study were extracted using standardization, including the study’s title, country of origin, study design and methods, population, patient sample size, and mental health outcome explored (Figure 1 and Table 1).
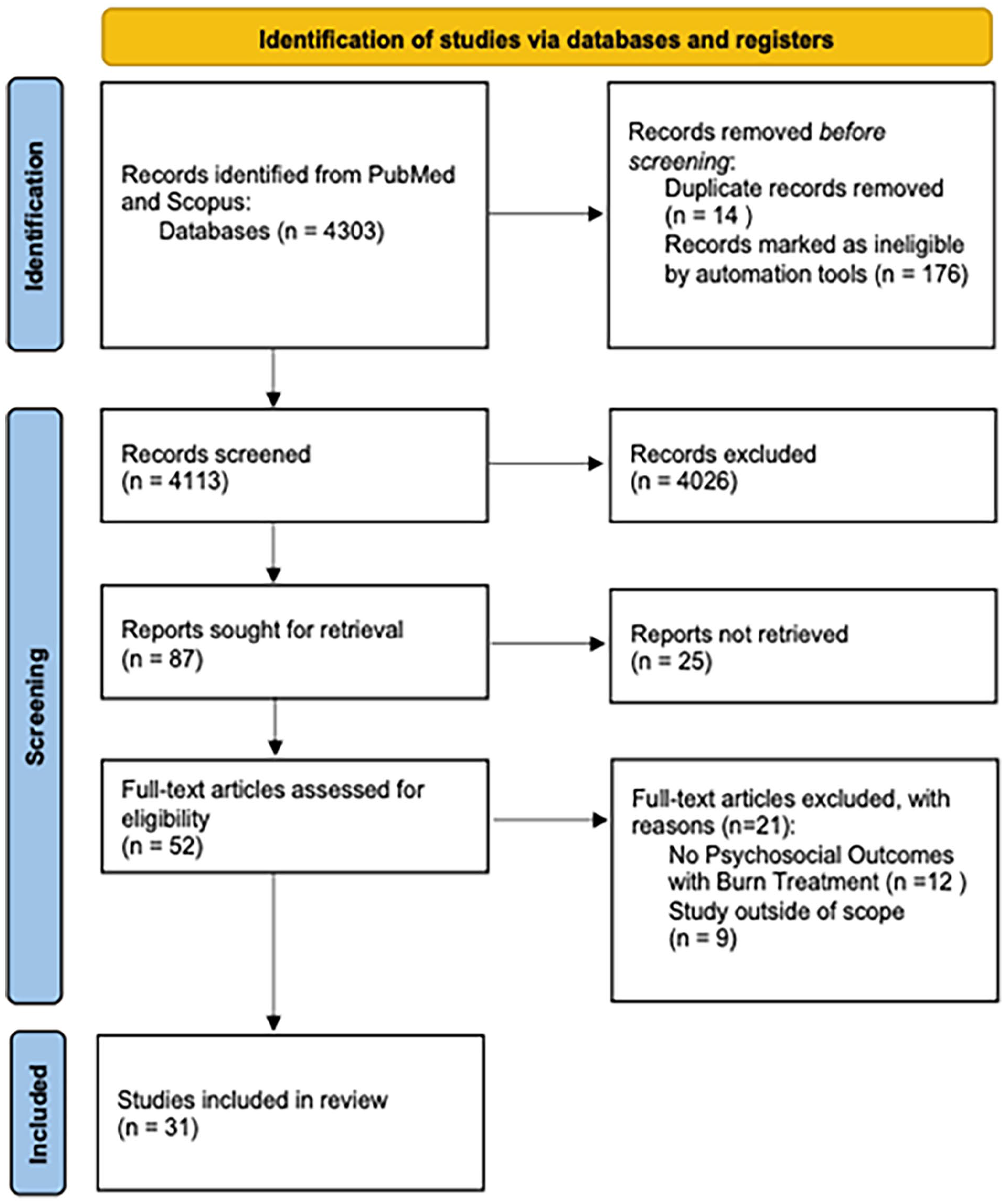
Preferred Reporting Items for Systematic Reviews and Meta-Analysis flow diagram.
Studies Included in Our Scoping Review.
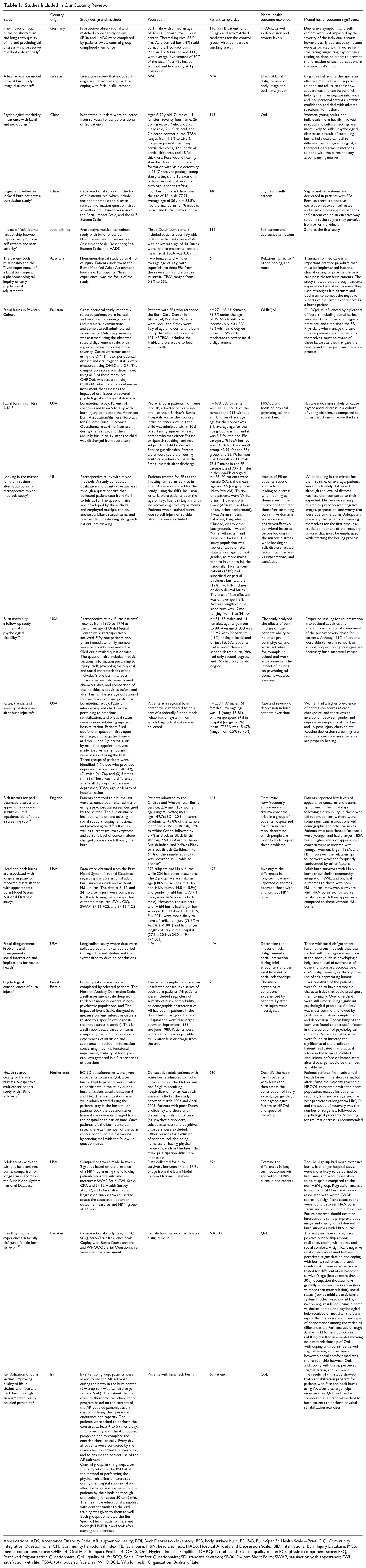
Abbreviations: ADS, Acceptance Disability Scale; AR, augmented reality; BDI, Beck Depression Inventory; BSB, body surface burn; BSHS-B, Burn-Specific Health Scale – Brief; CIQ, Community Integration Questionnaire; CPI, Community Periodontal Index; FB, facial burn; H&N, head and neck; HADS, Hospital Anxiety and Depression Scale; iBID, International Burn Injury Database; MCS, mental component score; OHIP-14, Oral Health Impact Profile-14; OHI-S, Oral Hygiene Index – Simplified; OHRQoL, oral health-related quality of life; PCS, physical component score; PSQ, Perceived Stigmatization Questionnaire; QoL, quality of life; SCQ, Social Comfort Questionnaire; SD, standard deviation; SF-36, 36-Item Short Form; SWAP, satisfaction with appearance; SWL, satisfaction with life; TBSA, total body surface area; WHOQOL, World Health Organization Quality of Life.
Results
Psychological Burden and Mental Health Outcomes
Facial burns impose an unparalleled psychological burden, with anxiety, depression, and post-traumatic stress disorder (PTSD) emerging as dominant outcomes. The visibility of facial burns amplifies emotional distress by continuously exposing survivors to altered self-perception and stigmatizing social interactions. Studies consistently show that individuals with facial burns experience significantly elevated levels of psychological distress compared to those without visible injuries. For instance, Hospital Anxiety and Depression Scale scores revealed heightened anxiety (4.8 ± 3.2) and depression (3.9 ± 3.5) in facial burn patients compared to controls (anxiety: 2.5 ± 2.8, P < .002; depression: 2.1 ± 2.7, P = .01). 1 These symptoms persisted even 1 year post-injury, underscoring the chronic nature of psychological distress.
The interplay between body image dissatisfaction and psychological outcomes is evident, with early depressive symptoms predicting worse self-esteem and higher scar severity 6 months post-burn. 7 Women and younger patients demonstrate greater vulnerability to PTSD and depression compared to their counterparts, as reflected in risk scores (P < .001). 8
Stigma, Body Image Dissatisfaction, and Their Interconnections
Medium-level stigma scores (58.01 ± 7.57) and low self-esteem scores (19.72 ± 2.43) were indicative of the challenges burns patients face, and the positive correlation between stigma and self-esteem (r = 0.286, P < .01) highlights the cyclical relationship between these factors. 4 In addition, socioeconomic factors such as income and education were shown to significantly predict stigma levels, accounting for 33.7% of its variation (F = 8.659, P < .01).
Body image dissatisfaction was a recurring theme across studies, with patients with facial burns frequently reporting lower satisfaction with appearance compared to those with non-facial burns. For example, SWAP scores were significantly worse among facial burn survivors (P < .01). 9 Adolescents with facial burns demonstrated persistent dissatisfaction with their appearance 1 year post-injury, further reinforcing the link between stigma, self-perception, and mental health. 10
Mirror exposure often serves as a pivotal moment in shaping survivors’ self-image and emotional response. Nearly half of the patients expressed apprehension before viewing their reflection, and 27% avoided mirrors altogether initially. 11 For this reason, Shepherd et al found that preparing patients for this experience was of paramount importance, as it mitigated stress, fostered resilience, and was an integral part of the healing process.
QoL and Interventions
Facial burns adversely affect QoL across physical, psychological, and social domains. QoL scores were significantly lower among facial burn survivors, with scar severity negatively correlating with physical and psychological well-being. 12 Rehabilitation strategies, such as augmented reality (AR)-based interventions, have shown promise in improving outcomes. A randomized clinical trial demonstrated significant gains in QoL scores after 6 weeks of AR-coupled rehabilitation compared to baseline (P < .001). 13
Discussion
This scoping review assessed the impact of facial burns on affected individuals and the psychological burden and challenges that these patients faced. By analyzing the included studies, we uncovered important connections between the psychological impacts that facial burns have on individuals as well as the detriment they serve to the QoL of these patients. These findings accentuate the negative implications associated with facial burns and provide a framework for improving the problem. Despite being a scoping review, this study offers significance by providing a comprehensive overview of the current psychological impacts of facial burns. It offers healthcare professionals, researchers, and policymakers a consolidated foundation on which to build more targeted and evidence-based interventions against this problem.
Anxiety, depression, and PTSD were greatly increased in this population, underscoring the importance of integrating mental healthcare into burn treatment.8,14 The heightened vulnerability of women and younger patients indicates that targeted psychological interventions toward those populations may be beneficial in diminishing long-term distress. 8 Importantly, the integration of trauma-informed care, psychological screening, and reconstructive surgery into routine burn management can enhance recovery. Early identification of high-risk individuals, particularly women and adolescents, is critical. Studies underscore the necessity of holistic approaches that address the psychological, social, and physical dimensions of recovery. These findings highlight the need for a multidisciplinary approach to provide comprehensive mental health support. One of the most striking findings within the literature is the impact of facial burns on body image and self-esteem. Body image dissatisfaction and stigma contribute to a persistent state of psychological distress. Social stigma remains a detriment to the recovery process within patients, as the perception that society has on physical appearance significantly affects self-worth and body image.4,15 The positive relationship between body image and self-esteem suggests that addressing societal attitudes and providing psychosocial support can be crucial in treating facial burn patients, leading to more favorable outcomes psychologically. In addition to this, mirror exposure also presents as a potential aid in the recovery process as it unveils the psychological challenges that patients face while confronting their distorted appearance. Many patients experienced apprehension or avoidance when seeing their reflections post-burn, leading to the integration of structured mirror exposure therapy to ease the transition. 11 Another therapy that proved to be particularly effective for facial burn patients was cognitive-behavioral therapy (CBT). The use of the Newell CBT model targeted the fears of these patients by encouraging gradual confrontation of the social anxieties that these individuals suffer, leading to the development of adaptive coping strategies. 15 Psychological preparation and support during these critical moments aid in alleviating distress and promoting acceptance of one’s new appearance.
While this scoping review provides valuable insight into the psychosocial impacts of facial burns, several limitations must be addressed. The librarian at our institution suggested to data from Scopus and PubMed. This provided the study with valuable insights, but a more comprehensive review incorporating additional databases such as MEDLINE and Embase would be beneficial for capturing a more diverse range of literature on facial burns and mental health. The inclusion of only peer-reviewed, English-language studies may have been impacted by selection bias, leading to the potential omission of relevant research papers from non-English sources. Furthermore, variability in study designs, patient populations, and measurement tools across the included studies may have affected the standardization of the reported outcomes. Many studies relied on self-reported psychological measures, which may introduce a level of response bias. In addition, many of these studies were conducted in high-income countries, limiting the broadness of findings to low- and middle-income countries where access to facial burn care may differ drastically.
Further research should aim to validate and expand upon the findings presented in this paper. Future studies should utilize longitudinal designs to assess the long-term psychological effects of facial burns, as most current literature lacks follow-up beyond 1 year post-injury. In addition, the design of randomized controlled trials to evaluate the efficacy of structured mirror exposure therapy in reducing body image distress and self-esteem to improve QoL. The role of social support networks and peer mentorship programs should also be explored to determine the efficacy in treating the psychological issues within facial burn survivors.
Conclusion
This study aimed to assess the impact of Mental Health Outcomes and The Psychosocial Consequences of Facial Burns. The results indicate a significant association between facial disfigurement and increased risk of obstacles surrounding self-esteem and QoL. Facial burns present a multifaceted challenge, profoundly affecting not only physical health but also mental and psychosocial well-being. This scoping review underscores the significant psychological burden associated with facial burn injuries, including heightened anxiety, depression, PTSD, and body image dissatisfaction. The cyclical relationship between stigma, self-esteem, and QoL highlights the need for comprehensive, patient-centered care. While emerging interventions such as cognitive behavioral strategies and AR-based rehabilitation show promise, further high-quality longitudinal studies are necessary to validate their efficacy. Integrating psychological screening, trauma-informed care, and tailored interventions into routine burn management can promote holistic recovery. Prioritizing mental health support alongside rehabilitation is essential in improving outcomes and enhancing the overall QoL for facial burn survivors.
Footnotes
Acknowledgements
We would like to thank the University of Texas Medical Branch for helping with the systematic review process.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
