Abstract
Background:
The measurement of olfaction in research has drawn significant attention due to its critical role in diagnosing and monitoring olfactory dysfunction (OD). Olfactory impairments are associated with various disorders, making accurate and reliable testing essential. Current assessment methods can be categorized into subjective and objective measures. Subjective tools provide information to evaluate an individual’s perception and awareness of smells. Conversely, psychophysical (objective) measures provide quantifiable data that can detect olfactory impairments with precision but prove to be time-consuming and costly. The reliability of subjective assessments compared with objective methods remains a topic of ongoing investigation. There is a growing need for a comprehensive and efficient approach to measuring olfaction that balances accuracy, cost, and practicality.
Methods:
This scholarly review examines and compares the outcomes of studies that have evaluated different olfactory assessment tools. Each study was chosen for its popularity among current otolaryngology providers. The effectiveness of these tests was analyzed based on sensitivity in detecting OD, ease of administration, and overall cost-efficiency.
Results:
Findings highlight the strengths and limitations of both subjective and objective methods. Subjective assessments, while convenient and cost-effective, exhibit variability in reliability due to individual differences in olfactory perception and cognitive biases. Objective tests provide precise and standardized results, but their practical application is limited due to cost, expertise, and duration of testing.
Conclusions:
Current olfactory assessments present a trade-off between cost, reliability, and practicality. Objective methods are currently the gold standard, but their limitations necessitate the development of more accessible testing. Future research should focus on refining hybrid models that integrate subjective self-reports with validated objective measures to achieve a comprehensive and cost-effective approach to olfactory assessment.
Keywords
Introduction
Olfaction is crucial for several vital functions, including safety, human health, and quality of life (QoL). The sense of smell is often the first sensory modality to detect changes in the external environment, even before sight, taste, or sound. 1 It plays a key role in nutrition, by influencing food preferences and appetite regulation. 2 Beyond its contribution to taste and enjoyment of food, the sense of smell is essential for detecting environmental hazards such as smoke, gas leaks, and spoiled food. It also influences memory, emotions, and social interactions. Olfaction has a neuroendocrine role in regulating food intake and energy balance, with the olfactory bulb being involved in these processes. Impairments in olfaction are associated with neurodegenerative diseases, mental health disorders, and metabolic conditions, highlighting its broader impact on overall well-being. 3
It is estimated that ~22% of the population has olfactory dysfunction (OD). OD refers to the impaired ability to smell, which can manifest as anosmia (complete loss of smell) or hyposmia (reduced sense of smell). This condition can arise from various etiologies, including post-viral infections, chronic rhinosinusitis (CRS), head trauma, and neurodegenerative diseases like Parkinson’s or Alzheimer’s. 4 OD can profoundly impact QoL. Reliable and accessible testing methods are crucial to help accurately diagnose and treat OD. In this manuscript, we highlight some of the main methods of olfactory testing in research and as part of a clinical examination.
Olfactory testing is generally broken down into 2 major categories: (1) Subjective Olfactory Assessment whereby an individual self-reports perception of their sense of smell and (2) Psychophysical Olfactory Testing (aka objective testing), which utilizes standardized tests that assess odor perception through structured stimuli. Factors such as personal preferences, cultural influences, and prior experiences can shape an individual’s subjective olfactory awareness. 5 Psychophysical olfactory testing can include odor threshold tests, odor discrimination tests, and odor identification tests. These tests are more sensitive to smell abnormalities than subjective tests, which are prone to underestimation. Subjective olfactory testing serves as a useful complementary technique to psychophysical testing to qualify and interpret olfactory-related perceptual responses.
Materials and Methods
This scholarly review examines and compares the outcomes of studies that have evaluated different olfactory assessment tools. Each study was chosen for its popularity among current otolaryngology providers, relative ease of use/administration, as well as prevalence in current research and practice. The effectiveness of these tests was reviewed based on sensitivity in detecting OD, ease of administration, and overall cost-efficiency.
Subjective Olfactory Testing
Commonly-used subjective olfactory testing tools discussed in this review are summarized in Table 1.
Commonly-used Subjective Olfactory Tests.
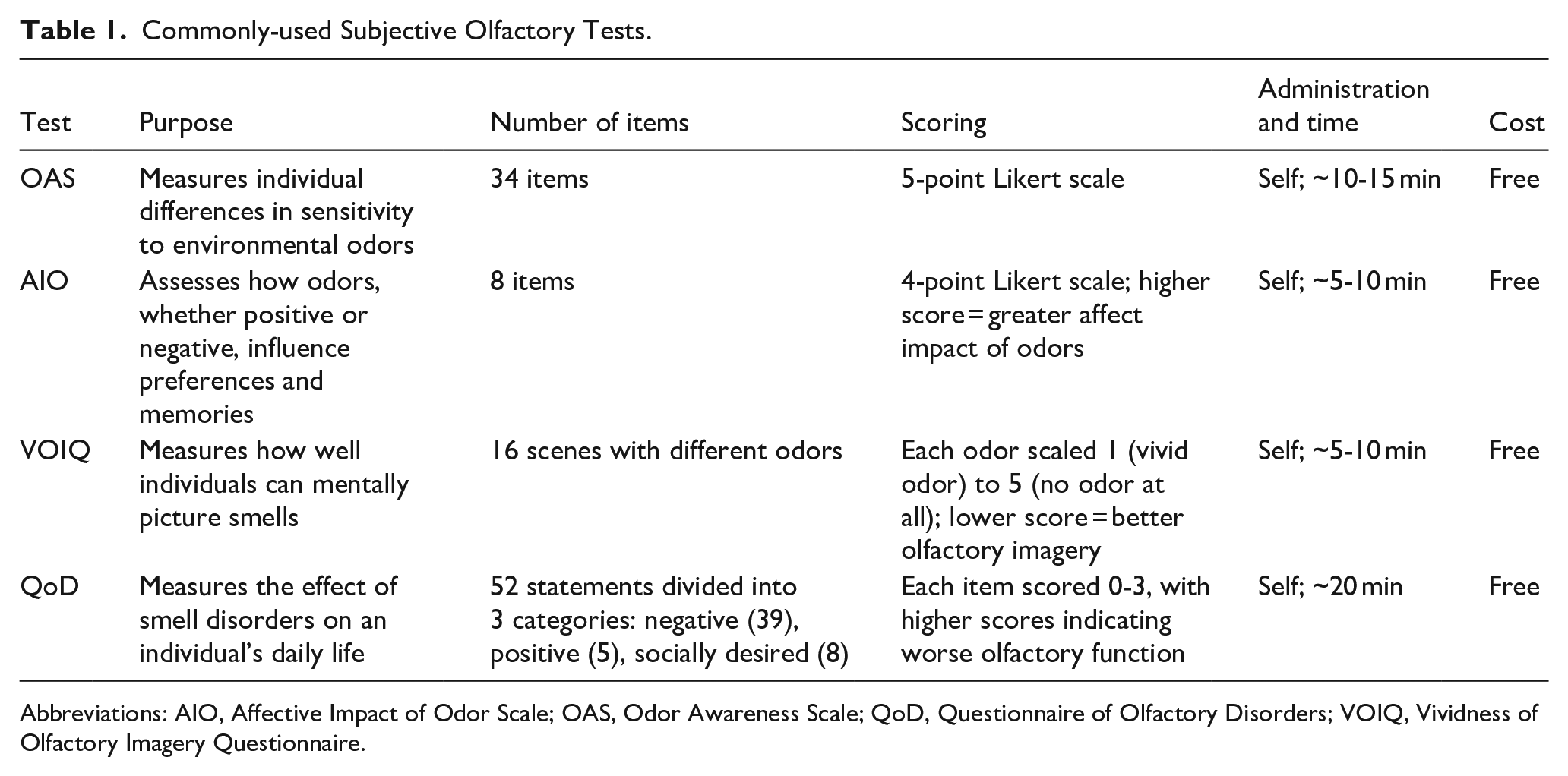
Abbreviations: AIO, Affective Impact of Odor Scale; OAS, Odor Awareness Scale; QoD, Questionnaire of Olfactory Disorders; VOIQ, Vividness of Olfactory Imagery Questionnaire.
The Odor Awareness Scale
The Odor Awareness Scale (OAS) is a 34-item questionnaire developed to measure individual differences in sensitivity to environmental odors. The hypothesis that odor awareness can be categorized into awareness of negative (to be avoided/dislike) and positive (to be approached/enjoyed) odors was evaluated using confirmatory factor analysis on responses from 525 participants. 6 These questions were divided into 2 subscales: a 21-item negative subscale (focused on odors to avoid) and an 11-item positive subscale (focused on odors to seek out). Participants respond using a 5-point Likert scale ranging from “never” to “always.” Higher scores on the OAS indicate greater overall awareness of environmental smells. This test is often used in psychological and sensory research to study general olfactory awareness and its relation to health or environmental factors.
Affective Impact of Odor Scale
The Affective Impact of Odor Scale (AIO) is a test that assesses the ability to detect, identify, and recognize specific odors. It consists of 8 items, and participants are asked to name or describe them. This test focuses on sensory and cognitive abilities that are related to olfactory processing. AIO was developed to determine the impact of positive or negative smells in determining liking and memory of new persons, places, and foods. A higher score is proportional to a positive impact of odors and positive memories. AIO is often used in understanding how individuals react to odors in different contexts, including the role of smell in memory recall, personal preferences, and sensory sensitivities. This paper shows that the strengths of the AIO are that it is brief, and it is reliable among the US and Belgian samples (Cronbach’s α of .73 and .75, respectively). 7
Vividness of Olfactory Imagery Questionnaire
The Vividness of Olfactory Imagery Questionnaire (VOIQ) is a 16-item scenario test that assesses a person’s ability to mentally recall smells, also known as olfactory representation ability. It provides different odor scenarios, asking participants to rate the vividness of the imagined smell on a 5-point scale, ranging from “1—perfectly realistic and as vivid as the actual odor” to “5—no odor at all, only the thought of it.” The questionnaire explores the relationship between odor perception and its personal or contextual relevance. Questionnaire participants who scored higher on VOIQ (“good olfactory imagers”) were found to rate pleasant odors as more familiar and score lower on anhedonia questionnaires when compared to “poor olfactory imagers.” This finding suggests a connection between the vividness of olfactory imagery, emotions, and long-term olfactory memory. Individuals with strong olfactory representations are more likely to recall the enjoyment of sensory experiences, whereas those with weaker olfactory representations often report greater difficulty in remembering pleasant sensory perceptions. Additionally, individuals with higher olfactory imagery ability have a greater interest in olfaction. The ability to create and recognize olfactory images is linked to knowledge of odors and the ability to name specific scents. Olfactory experts, known for their extensive lexical knowledge of odors, frequently report having a well-developed ability to imagine odors. 7 VOIQ is useful in comparing olfactory imagery ability in different populations such as those with smell loss or neurological disorders.
Questionnaire of Olfactory Disorder
Questionnaire of Olfactory Disorder (QoD), developed in 2004 by Frasnelli et al, is a validated questionnaire specific for QoL measures specific to olfaction.8,9 It consists of 52 statements divided into 3 categories: negative statements (QoD-NS), positive statements (QoD-PS), and socially-desired statements (QoD-DS). Subjects then decide whether they agree (2 points), partly agree (1 point), or disagree (0 points) with each statement. NS indicate how much patients suffer from OD, PS indicate how well they are coping with it, and socially DS serve as a litmus test to their credibility. Hummel et al developed a shorter, modified version (17 QoD-NS, 2 QoD-PS, 6 QoD-DS) that makes administration less time-consuming. This version also measures patient’s responses on a 0 to 3 scale depending on whether they disagree, partly disagree, partly agree, or agree. The questionnaire is scored so that higher scores indicate better olfactory QoL. 10 QoD is useful in gauging the severity of olfactory problems and their impact on daily life. It has been used in olfactory-loss patients due to traumatic brain injury or CRS.
Psychophysical Olfactory Testing
Commonly-used psychophysical olfactory testing tools discussed in this review are summarized in Table 2.
Commonly-used Psychophysical Olfactory Function Tests.
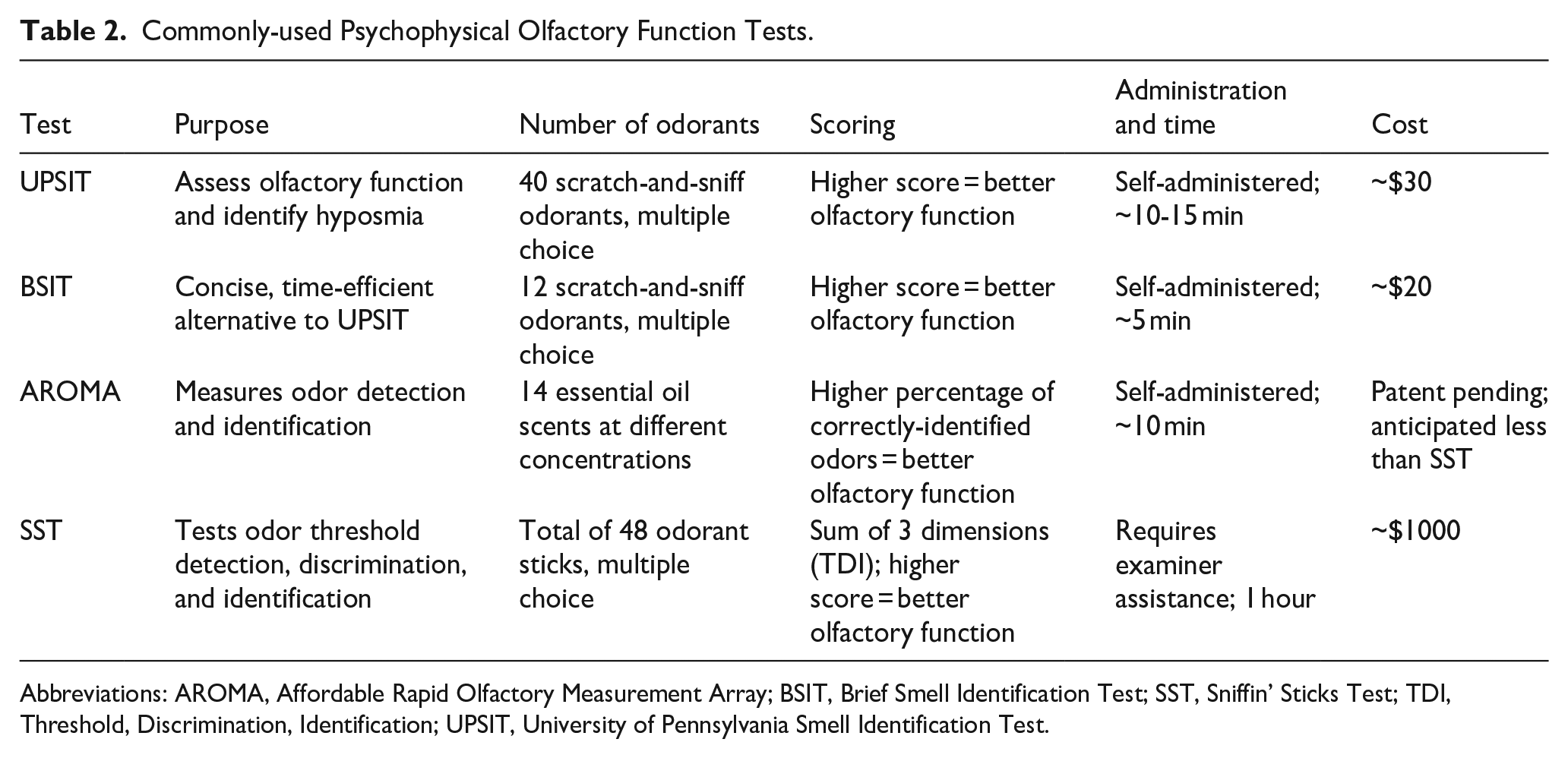
Abbreviations: AROMA, Affordable Rapid Olfactory Measurement Array; BSIT, Brief Smell Identification Test; SST, Sniffin’ Sticks Test; TDI, Threshold, Discrimination, Identification; UPSIT, University of Pennsylvania Smell Identification Test.
Scratch-and-Sniff Olfactory Testing
The University of Pennsylvania Smell Identification Test (UPSIT) is a tool for the assessment of olfactory function. It is 40 multiple choice questions with scratch-and-sniff odorants. The patient/participant can self-administer this test, and it can be mailed to individuals. A higher score correlates with better olfactory function. The score is based on age and sex nomogram. It is commonly used to assess OD secondary to workplace injury and has the potential to detect anosmic malingering. While attempts have been made to develop methods to differentiate between anosmic and anosmic malingering individuals, further research is needed. 11 The Brief Smell Identification Test (BSIT) is a streamlined alternative (12 questions) to the more comprehensive UPSIT. 12 The BSIT can be administered in under 5 minutes, making it particularly advantageous in clinical settings where time and resources are limited.
In a study of 183 participants with CRS, the BSIT, and the Smell Identification Test (SIT), each participant was assigned scores for both tests, allowing for direct comparison. The study revealed a strong bivariate linear association between BSIT and SIT scores for all participants (r = 0.893; P < .001), showing that BSIT scores closely correlate with SIT results. However, the BSIT identified a significantly-lower proportion of patients with abnormal olfaction than the SIT (47% vs 68%; P < .001), indicating that the BSIT underestimates the prevalence of OD when using the suggested cut-point of ≤8. However, if the cut-point is changed to ≤9, there is improved sensitivity and overall accuracy of the BSIT, making it a more reliable tool for detecting olfactory impairment in patients with CRS.
Sniffin’ Sticks Test
Sniffin’ Sticks are a set of marker-like devices that dispense odors and are used to evaluate 3 aspects of olfaction: odor threshold, discrimination, and identification in contrast to the SIT that only measures identification. This test is administered by a trained clinician or research coordinator. The odor threshold test determines the lowest concentration of an odorant (usually n-butanol) that an individual can detect. The concentration of the odorant is gradually increased until the subject can reliably detect it. 13 In Europe, the most utilized psychophysical test is the Sniffin’ Sticks Test (SST). 14
The odor discrimination test assesses the ability to distinguish between different odors. Subjects receive 16 pairs of odorants, and they must identify the one that differs from the other 2 in a triple forced-choice format. The odor identification test evaluates the ability to identify common odors. Subjects are presented with 16 different odorants and must choose the correct one from 4 verbal options provided for each odorant. The results from these 3 tests are calculated to create a score known as the Threshold, Discrimination, Identification score, which provides a comprehensive measure of an individual’s olfactory function. 15 Each test is scored out of 16 and then added together. The score is then categorized into functional anosmia (≤16.5), hyposmia (16.5-30.5), and normosmia (>30.5).
A study by Mai et al 3 aimed to determine whether the assessment of olfactory function using the SST could be adapted for self-assessment, offering a solution for diagnosing OD in clinical and research settings. The report notes that self-assessment Sniffin’ Sticks may be a reliable method for distinguishing between healthy individuals and patients with OD, when compared to examiner-assisted assessments. However, the lower reliability and weaker correlations for the threshold and discrimination tests highlight limitations in these components when self-administered, suggesting areas for improvement.
SST requires 30 to 60 minutes to complete, which is time-consuming. A more time-efficient test has been developed—SST-12—which is a screening version of the SST. It involves only 12 scents and can be completed in 5 minutes. This test provides a quick assessment on odor identification. 14
Affordable Rapid Olfactory Measurement Array
The Affordable Rapid Olfactory Measurement Array (AROMA) is a simple, reusable smell test that uses essential oils. Patients can use this test easily, as it can be self-administered, and conveniently, as it can be mailed. This test consists of 14 different scents of varying strengths and has been found to closely match results from well-known smell tests like the UPSIT. AROMA can test both an individual’s ability to identify smells and has proven to give consistent results (ρ = 0.85, P < .001). 16 This is a cost-effective alternative to traditional smell tests, which is shown by a prospective cross-sectional study by Li et al.
In 2020, Li et al studied 50 individuals without sinonasal disease. All participants completed the AROMA, SST, Sino-Nasal Outcome Test (SNOT-22), and the QoD. The AROMA test was enhanced with 2 higher concentrations to better assess olfactory reserve. The AROMA test demonstrated strong test-retest reliability (r = 0.757, P < .01) and showed a moderate correlation with SST-12 (ρ = 0.412, P < .01). Age and SNOT-22 scores were significantly correlated with AROMA results (ρ = −0.547 and −0.331, respectively, P < .05), and age showed a weaker correlation with SST-12 (ρ = −0.377, P < .01). Median correct identification rates were 92% for SST-12, 90% for AROMA detection, and 81% for AROMA identification.
AROMA offers a potential low-cost alternative. It showed comparable accuracy to the SST-12 test in identifying scents (r = 0.412, P < .01), reinforcing its validity. 17 The use of varying odorant concentrations could help distinguish between impairments in scent detection and identification, which are linked to different diseases. AROMA can be the future of olfaction testing in clinical care. 17
Psychophysical Versus Subjective Olfactory Testing
A study by Monk et al 18 investigated the correlation between subjective and objective/psychophysical olfactory tests. They found a moderate positive correlation between OAS and UPSIT scores, suggesting that individuals who scored higher on the OAS tended to perform better on the UPSIT. 18 Similarly, the AIO showed a moderate correlation with UPSIT, linking the emotional significance individuals place on odors with their objective olfactory abilities. In stark contrast, VOIQ did not exhibit a significant correlation with SIT, indicating that the ability to vividly imagine smells does not necessarily translate to better olfactory function. Notably, subjective testing was highly correlated with the SIT. These findings underscore the complexity of olfactory perception and highlight the challenges in using subjective measurements to predict objective/psychophysical olfactory capabilities.
The results highlight the necessity of integrating both subjective and objective measures in finding the perfect test for olfaction. Future research should focus on refining subjective measures to enhance their predictive capabilities and exploring novel methodologies that could help bridge the gap between subjective and objective/psychophysical assessments. Additionally, expanding the study’s sample size and diversifying participant recruitment can provide more comprehensive insights into olfactory function across different populations.
Conclusion
The current diagnostic assessments that test olfaction are complicated, rely on fixed scent concentrations, and come with high costs. This limits their use in clinical settings and self-assessments. There is no test that fully assesses the nuances of subjective and psychophysical olfactory awareness. Subjective tests such as OAS and AIO show correlations with psychophysical measures such as UPSIT, while VOIQ does not. Rapid and cheaper psychophysical tests such as BSIT and AROMA have limitations compared with SIT and Sniffin’ Sticks, which are more comprehensive. These findings highlight the need for a “gold standard” in olfactory testing, which efficiently and effectively assesses both subjective and objective measures. Future research should attempt to develop new tests, improve existing ones, and establish a consensus on reliable assessment of OD.
Footnotes
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
