Abstract
Introduction:
Leeches are freshwater ectoparasites that inhabit streams, pools, and springs. Internal infestation occurs by ingestion of contaminated water or direct exposure while swimming. This report presents a rare case of tracheal hirudiniasis.
Case Description:
A 34 year-old Nepalese woman presented with 1 week history of throat discomfort and dysphagia after the ingestion of river water. The initial clinical and endoscopic evaluations were unremarkable. Twelve hours after admission, a leech was visualized at the base of the tongue, but multiple failed extraction attempts led to its migration. Subsequently, rigid bronchoscopy under general anesthesia identified a leech in the trachea, 2 cm proximal to the carina. The parasite was successfully extracted with rigid bronchoscopy under general anesthesia, and the patient had a smooth recovery.
Discussion:
Internal hirudiniasis affects primarily the nasal cavity, oral cavity, pharynx, larynx, tracheobronchial tree, and esophagus, with rare cases in the abdomen, vagina, and eye. Symptoms depend on the site of infestation. Nasal cases present with epistaxis and obstruction, while tracheobronchial involvement may cause cough, dyspnea, and hemoptysis. Removal is challenging due to the mucosal attachment of the leech and its slippery nature. Various detachment techniques, including anesthetics, cryoprobes, and hypertonic solutions, have been described in the literature. In this case, general anesthesia likely facilitated detachment, enabling a successful extraction.
Conclusions:
Internal hirudiniasis should be considered in patients with freshwater exposure with relevant symptoms. Prompt recognition and appropriate extraction techniques are essential to prevent complications. Increased awareness among health care workers and the general population is essential for early diagnosis, prevention, and effective management.
Introduction
Leeches are freshwater ectoparasites commonly found in streams, pools, and springs. Humans may develop internal infestations by the ingestion of contaminated water or exposure while swimming in freshwater sources. 1 The nasal cavity is the most common site of internal infestation, followed by the oral cavity, pharynx, larynx, tracheobronchial tree, and esophagus. 2 A handful of cases of internal hirudiniasis have been reported involving the abdominal cavity, vagina, and eye.3-5
This case report presents a rare case of tracheal hirudiniasis, offering valuable information on the symptomatology of internal hirudiniasis, particularly tracheobronchial involvement. Additionally, we have briefly discussed the management challenges and techniques for aerodigestive hirudiniasis.
Case Presentation
A 34 year-old South Asian woman from northeast Nepal presented to the emergency department with 1 week history of foreign body sensation in her throat and dysphagia. She reported developing these symptoms shortly after drinking water from a nearby river. The patient denied experiencing blood-tinged saliva, drooling saliva, epistaxis, dyspnea, coughing, or hoarseness. She had no previous similar complaints, no known comorbidities, and an unremarkable family history. She consumed alcohol occasionally, with her last drink being 7 days earlier, but was a nonsmoker. She worked as a farmer and belonged to the lower middle class based on the modified Kuppuswami scale.
On examination, the patient was hemodynamically stable. Inspection of the oral cavity, pharynx, posterior rhinoscopy, and indirect laryngoscopy did not reveal the parasite or any signs of bleeding. She was kept nil per oral and initiated on intravenous fluids and antibiotics. However, nearly 12 hours after presentation, the parasite was visualized at the base of the tongue (Figure 1). Multiple forceps extraction attempts were unsuccessful. Repeated extraction attempts likely caused the parasite to migrate deeper, making it no longer visible at the base of the tongue.
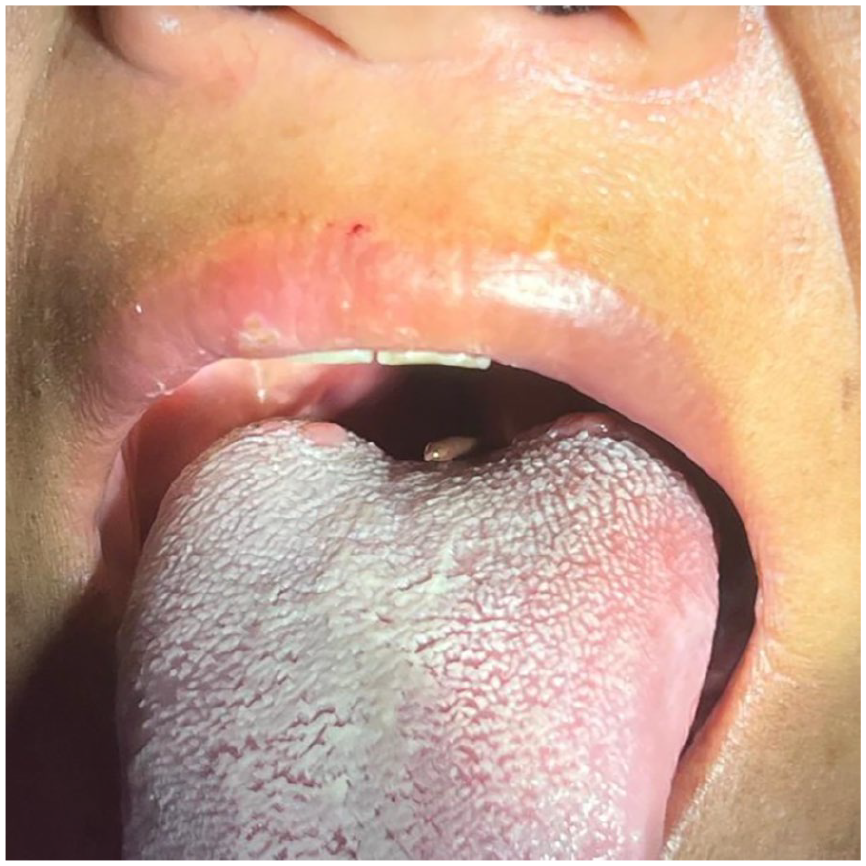
Leech seen at the base of the tongue.
The patient was immediately taken to the emergency operating room (OT) for a 70° diagnostic nasal endoscopy under local anesthesia (LA), but the parasite was not visualized. Subsequently, she was scheduled for diagnostic triple endoscopy and transferred to routine OT. Nasopharyngolaryngoscopy and esophageoscopy were unremarkable. However, rigid bronchoscopy under general anesthesia revealed a leech in the trachea, 2 cm proximal to the carina (Figure 2).
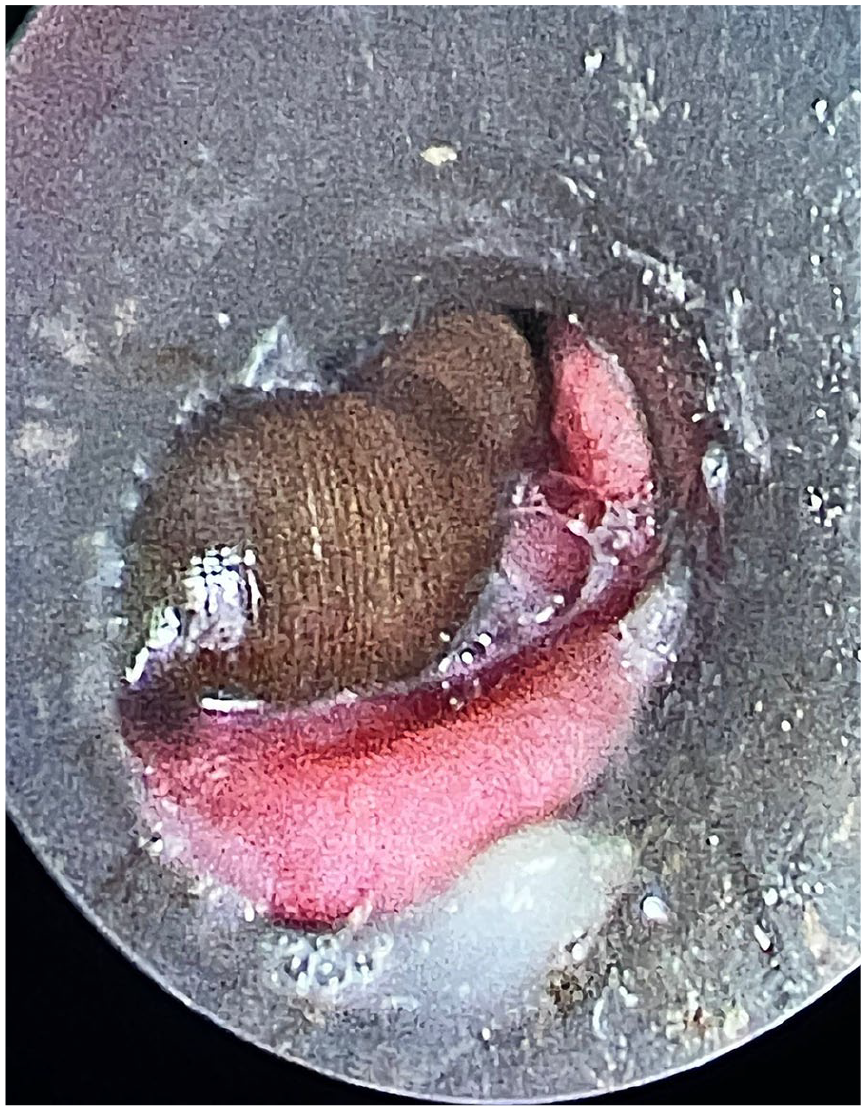
Leech visible leech in the trachea during rigid bronchoscopy.
The leech was successfully grasped with jaw forceps and secured using foreign body holding forceps. The foreign body, forceps, and bronchoscope were removed as a single unit. A 4 × 1 cm leech was extracted in 1 piece. Reevaluation with a rigid bronchoscope confirmed that there were no remaining leeches and that the bronchial mucosa appeared normal.
After the procedure, the patient reported significant symptomatic relief. She was monitored for 24 hours, during which her condition remained stable. On discharge, she was advised about safe drinking water practices and the potential risks of freshwater exposure. At the 1 week follow-up, the patient reported mild throat pain, likely due to the procedure, but denied any symptoms of leech infestation.
Discussion
The symptoms of internal hirudiniasis vary depending on the site of infestation. When a leech is present in the nasal cavity or nasopharynx, patients may present with epistaxis, nasal obstruction, and foreign body sensation in the nasal cavity. 6 Oral cavity and oropharynx infestation typically presents with a foreign body sensation, odynophagia, and dysphagia. The presence of a leech in the larynx causes airway obstruction and a change in voice. 7 Infestation of the trachea and bronchus typically manifests as cough and dyspnea.8,9 These symptoms are often painless due to the anesthetic properties of the leech’s saliva.1,2
Furthermore, these parasites secrete hirudin, an anticoagulant that can cause bleeding manifestations such as hemooptysis, hematemesis, epistaxis, and blood-tinged saliva.1,10 In chronic cases, patients may develop anemia. Moslehi et al reported a case of bronchial leech infestation in which the patient presented 7 months of intermittent hemooptysis, hematemesis, cough, vomiting, epistaxis, and melena. 8 In the stool exam, the occult blood was 3+, while the occult parasite was negative. Similarly, Yang et al reported endobronchial leech in 49 year-old female with a history of cough, rusty brown sputum with hemoptysis and hoarseness for 6 weeks and ground glass opacity in the medial basal segment of the right lobe of the lung. 9
In our case, initially, the patient presented with 1 week of foreign body sensation and dysphagia, suggesting an infestation in the oral cavity or pharynx. Unlike most reports of internal hirudiniasis, our patient did not develop signs of bleeding manifestations, which could be attributed to the early presentation.
During the initial examination, the parasite was not observed, suggesting that it was hidden within the oral cavity or pharynx or had already migrated to the trachea. However, nearly 24 hours later, the parasite was visualized at the base of the tongue. Following multiple failed attempts to extract the parasite using forceps, it migrated to the trachea. Despite this, the patient did not show typical symptoms such as cough, dyspnea, or hemoptysis, possibly due to the small size of the parasite.
The extraction of a leech is challenging for several reasons. First, leeches attach firmly to the mucous membrane using their anterior and posterior suckers; applying excessive force may cause the parasite to rupture. The presence of hirudin in saliva may cause uncontrollable bleeding at the attachment site. In the case reported by Moslehi et al, the parasite ruptured during extraction, leaving its suckers attached to the bronchial mucosa. 8 The remaining parasite fragments were removed using a Dormia basket. Therefore, the parasite should be removed from the mucosa prior to attempting extraction.
In our case, the parasite probably detached due to the general anesthetic administered during the procedure. Zhang et al also attributed parasite detachment to sevoflurane administration. 10 Other studies have reported the use of hypertonic sodium chloride solution, 11 glycerin phenic, 12 and lidocaine 6 to facilitate leech detachment from the mucosa. However, these methods must be used with extreme caution in the respiratory tract to prevent bronchospasm, mucosal chemical injury, and even suffocation. In addition, the parasite should be gently grasped before administering these agents to prevent its dislodgment into the distal airway. Leeches have a slippery body, making them difficult to grasp. We used blunt forceps with transverse serrations to ensure a firm grip during extraction.
A newer method of extracting living foreign bodies involves the use of a cryoprobe. Li and Sun successfully removed a leech in 1 piece using intrabronchial cryotherapy under LA. 13 However, these advanced techniques require specialized equipment and are not yet accessible in resource-limited settings such as ours.
Lastly, the management of internal hirudiniasis is incomplete without advocating for behavioral changes: Drinking impure water and exposure to freshwater remain major risk factors for parasitic infestations. While the dangers of consuming contaminated water are well documented, including infections and infestations such as cholera, typhoid fever, giardiasis, and hirudiniasis, as well as noninfectious conditions such as fluorosis and arsenicosis, the risks associated with direct freshwater exposure are often overlooked. Swimming or bathing in untreated water bodies increases the risk of bacterial infections such as leptospirosis and parasitic manifestations such as internal hirudiniasis and schistosomiasis. Addressing these issues requires an integrated approach that not only focuses on clinical management but also considers preventive strategies, including improving sanitation, ensuring access to safe drinking water, and promoting awareness of the health hazards of unprotected contact with freshwater.
Conclusions
Internal hirudiniasis should be considered in patients with a history of freshwater exposure who present pertinent symptoms. Prompt recognition and appropriate extraction techniques are essential to prevent complications. This case underscores the importance of considering parasitic infestations in endemic regions and highlights the need for increased awareness among health care professionals and the general population.
Footnotes
Ethical Considerations
Clearance from institutional review committee (IRC) approval is not required to publish a case report at our institute.
Consent to Participate
The patient and the patient party were explained about the use of their clinical scenario and images in a depersonalized form, for report writing and publication purposes, both verbally and followed by obtaining written consent for the same.
Consent for Publication
Written consent obtained from the patient covered consent for publication.
Author Contributions
S.B. and Su.B. conceptualized the study, were associated with patient care, and reviewed the report. S.P. and S.S.K. performed background research, reviewed the literature, and prepared the manuscript. GP was associated with patient care and manuscript preparation.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
No datasets were generated or analyzed during the study.
