Abstract

Significance Statement
Nasal septal abscess is a rare rhinosurgical emergency, often linked to nasal trauma but occasionally occurring unexpectedly. It requires immediate intervention to prevent functional sequelae, cosmetic disfigurement, and severe septic complications. This case report describes the unexpected development of a nasal septal abscess following routine electrocautery for anterior epistaxis, a common ear, nose, and throat procedure. The delayed onset of symptoms highlights the critical need for ongoing monitoring and follow-up care after nasal procedures.
Case Presentation
A 67-year-old male with asthma and gouty arthritis presented with three weeks of progressive bilateral nasal obstruction, nasal pain, and interorbital headache when in supine position. He reported a history of single episode of right anterior epistaxis treated with bipolar electrocoagulation one month in advance. He had presented to his attending physician five days ago and was prescribed a course of oral amoxicillin and clavulanic acid with minimal amelioration.
On initial assessment, patient was apyretic and the external nose was sensitive to pressure along its whole length with a slight erythema and marked tenderness of the peri-columella area. Anterior rhinoscopy revealed an obvious, dull purple tense and fluctuant to palpation bilateral bulging of the anterior nasal septum (Figure 1). Incision and drainage, under topical and local anesthesia after the first dose of intravenous amoxicillin-clavulanate, revealed a purulent discharge with loss of the central quadrilateral cartilage but preservation of caudal and dorsal struts. A gentle repeated irrigation of the cavity was performed, and the nose was packed bilaterally with bioresorbable nasal dressing.
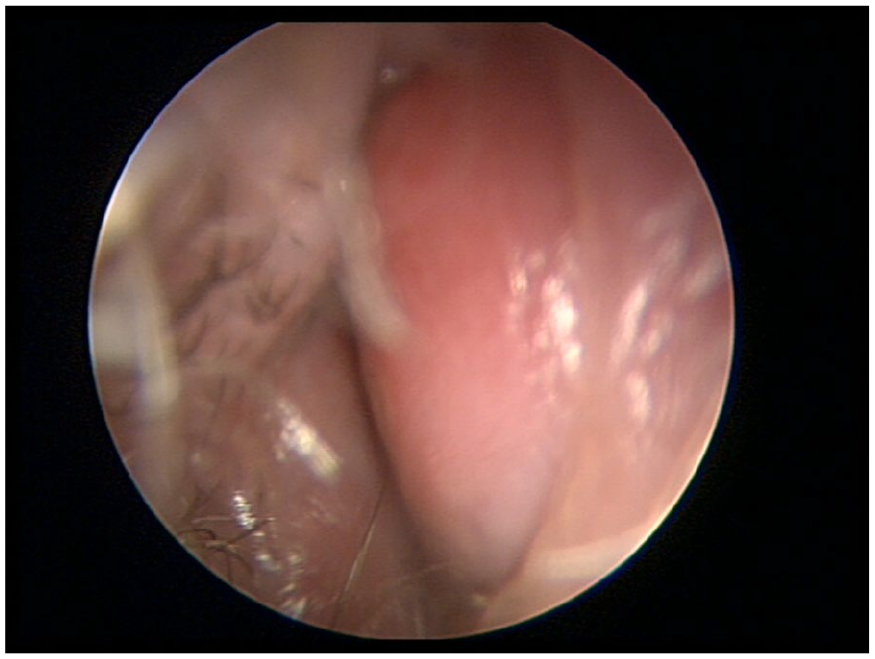
Clinical image. Physical examination revealed a healed septal mucosa over a cherry-like swelling of anterior nasal septum occluding right nostril.
Facial computed tomography failed to unveil an underlying etiology (Figure 2). Pus subsequently grew cutibacterium acnes, and the patient was discharged home the next day and was given a 10-day course of clindamycin. At the third day follow-up, there was no clinical evidence of abscess recurrence.
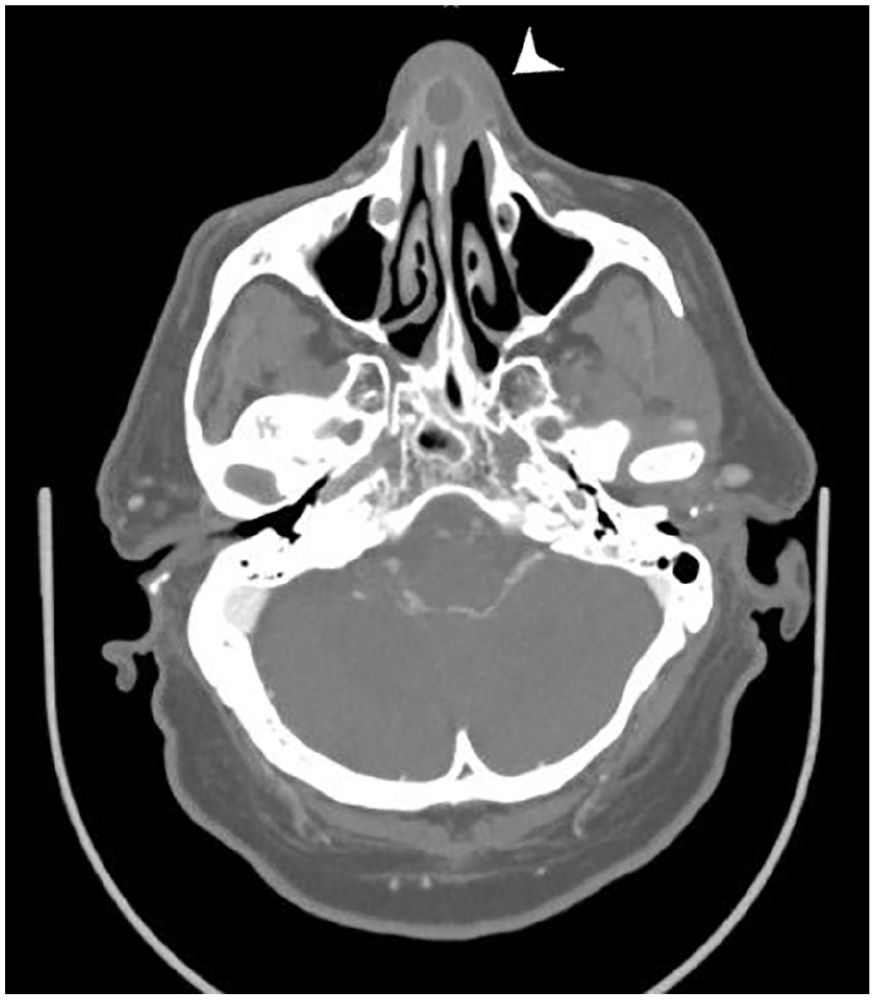
Computed tomographic image. Computed tomographic axial slice through the nasal cavity demonstrates a thin-walled, cystlike collection with peripheral enhancement involving the cartilaginous nasal septum (arrow) consistent with a nasal abscess.
Discussion
Nasal septal abscess (NSA) refers to an enclosed collection of pus in submucoperichondrial or submucoperiosteal leaflets potential space of nasal septum. It has an unknown actual incidence; however, men in their 50s and children are more commonly affected by this condition.1-7
Men are more likely than women to be involved in violent acts, aggressive behavior, and car accidents, which increases their risk of developing NSA.1,2 Nasal trauma is extremely common in pediatric population and often goes undiagnosed.1-3,6 Special attention is required for hematoma and NSA in young children, as these injuries could result from child abuse.2,3
NSA is most likely to occur after almost inevitable superimposed bacterial colonization of an untreated nasal septal hematoma as a result of minor nasal trauma.2,3,5,6,8 Nasal septal hematoma formation decollates mucoperichondrium from the relatively avascular quadrangular cartilage, compromises its vascular supply, and exerts increasing pressure. Quadrangular cartilage necrosis due to cartilage ischemia, avascular necrosis, and septal resorption usually takes place within 3 days.2,8 However, bacterial lysis can accelerate the process of cartilage degradation, liquefaction, and necrosis and lead to its total destruction in a 24 hour course.2,8
Other less frequently associated causative factors include septal and sinus surgery, acute ethmoiditis and sphenoiditis, odontogenic infection originating from maxillary incisors, and nasal vestibule furunculosis.1,2,9-12 In rare instances, NSA can appear secondary to nasogastric tube placement, nasotracheal intubation, nasopharyngeal swab test, rhinotillexomania, and intranasal drug abuse.2,9
The pus may be found in one or both sides of the cartilaginous or bony 3-layer divider of nasal fossae due to fragmentation or cartilage dissolution. The interval between nasal injury and symptoms is usually 5 to 7 days. 2 Typical clinical features include complete, usually bilateral, nasal congestion, throbbing nasal pain, fever, and headache in descending order of frequency.1-6 Anterior rhinoscopy reveals a bilateral nasal airway occlusion by a fluctuant septal swelling, which does not shrink after the application of topical decongestant.1-6
Permanent sequelae due to the widespread destruction of the supporting cartilaginous framework of the nose, unorganized asymmetric contractions, and loss of structural integrity of the lower two-thirds of the nose can be rapid and severe. These include columellar retraction and nasal valve collapse, widening of the nasal base, septal deformity and perforation, unaesthetic saddle-nose deformity, and maxillary hypoplasia in childhood.1-6 Nasal-oral fistula might sporadically form from dental or vestibular infection. 2 Delayed diagnosis or inadequate treatment may lead to ascending suppurative potentially life-threatening complications such as cavernous sinus thrombosis, meningitis, and cerebral abscess, due to valveless angular, ethmoidal, and ophthalmic venous tracts.1-6 Local extension through lymphatic pathways of the anterior skull base may involve the orbit, which can result in osteomyelitis, orbital abscess, and potentially sepsis and bacteriemia.1-6
The most common pathogen isolated is Staphylococcus aureus followed by Streptococcus pneumoniae and Klebsiella pneumoniae, while haemophilus influenzae is more likely in pediatric patients.1-6 NSA management should consider short-term effects including impaired breathing, sagging, and widening of the nasal infrastructure, and long-term consequences on nose and midface development. Prompt diagnosis, adequate parenteral antibiotherapy, wide unilateral or bilateral incisions with debridement of the infected cartilage, and effective drainage followed by quilting sutures or bilateral nasal packing remain the mainstay of treatment.1-6 In addition, immediate septal reconstruction using autologous cartilage graft is recommended, to avoid nasal deformities and severe impairment of nasal patency and growth.4,7
Footnotes
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Considerations
Our institution does not require ethics approval for reporting individual cases. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to Participate
Written informed consent was obtained from participant included in the report.
