Abstract
Introduction
Instagram is among the leading social media platforms due to its rapid content delivery, condensed information, and numerous engagement features. 1 With its widespread appeal, physicians have begun using Instagram to share medical education with a broader audience, thus increasing its potential to influence health outcomes. Medical education sharing on social media is not just carried out by physicians but also by other health care providers such as nurses, naturopathic doctors, chiropractors, and midwives, who sometimes share treatments remedies for different health ailments that may not meet physician-standard guidelines and could be considered medical misinformation.
Although Instagram has measures in place to combat misinformation, 2 those mechanisms are typically used in response to widespread reports, usually due to major global events that draw significant media attention. Medical misinformation on social media, especially in the realm of otolaryngology, is an underexplored area. Given the increasing use of social media to share medical education and the accompanying risk of disseminating inaccurate information, our study aimed to examine the accuracy, engagement, and quality of otolaryngology-related educational videos produced by healthcare providers on Instagram.
Methods
A systematic search on Instagram was conducted to identify the top 150 video posts using the hashtags #Otolaryngology, #Otolaryngologist, and #ENTeducation. The criteria for selecting these posts included relevance to otolaryngology medical education. Exclusion criteria were applied, resulting in the exclusion of 96 videos. Among the excluded posts, 26 were due to non-English content, 20 were patient experience/narratives, 44 were unrelated to otolaryngology education, and 6 were entirely nonmedical content. The included posts were shared from September 2020 to January 2024. Engagement metrics such as likes, comments, shares, and views were used to quantify the reach of the content. Additionally, the duration of each video post was recorded. Physician otolaryngologists assessed medical education videos for accuracy using credibility and reputable medical sources, such as UpToDate, PubMed, and Cummings Otolaryngology: Head and Neck Surgery, 7th Edition. Furthermore, the Patient Education Materials Assessment Tool for Audiovisual Materials (PEMAT-A/V) was utilized to evaluate the understandability and actionability of medical educational videos. To minimize discrepancies, all video engagement metrics were extracted from Instagram on the same day.
Results
Video Demographics
Fifty-four Instagram videos were analyzed and categorized by content type based on their primary topic—ear (n = 15), nose (n = 20), and throat (n = 19). Figure 1 provides a brief description of topics within each category. 78% of the videos were created by otolaryngologists, 7% by plastic surgeons, and 15% by other health care providers such as a nurse, audiologist, dermatologist, neurologist, and emergency medicine physician.
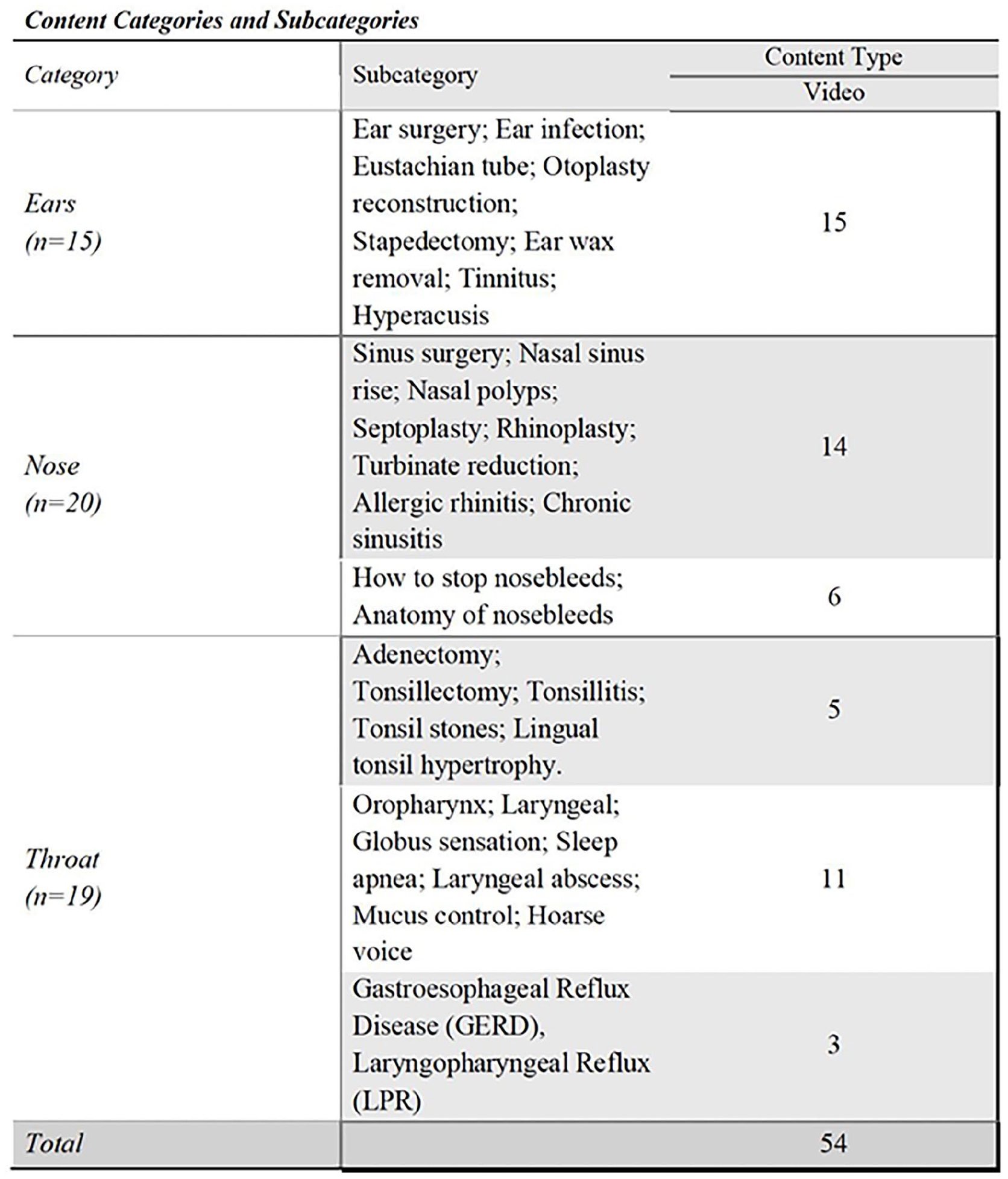
Categorization of medical education content videos.
Engagement Analysis and PEMAT-A/V for Medical Education Video
For Instagram video posts, the average number of likes per video post was 527 (±1170), comments 20 (±25), shares 169 (±484), views 20 725 (±43 856), and video length 44 seconds (±25). Ear-related content had the highest likes, shares, and views, while nose-related content had higher comments. The average understandability was high at 89%, and the average actionability was low at 39%. Across the content categories, understandability scores were similar ranging between 88% and 89%, while actionability was higher in nose-related content at 53% compared to ear (39%) and throat (28%) related content. Figure 2 illustrates the average engagement metrics (likes, comments, shares, and views), video duration, and PEMAT-A/V score for content categories: ears, nose, and throat.
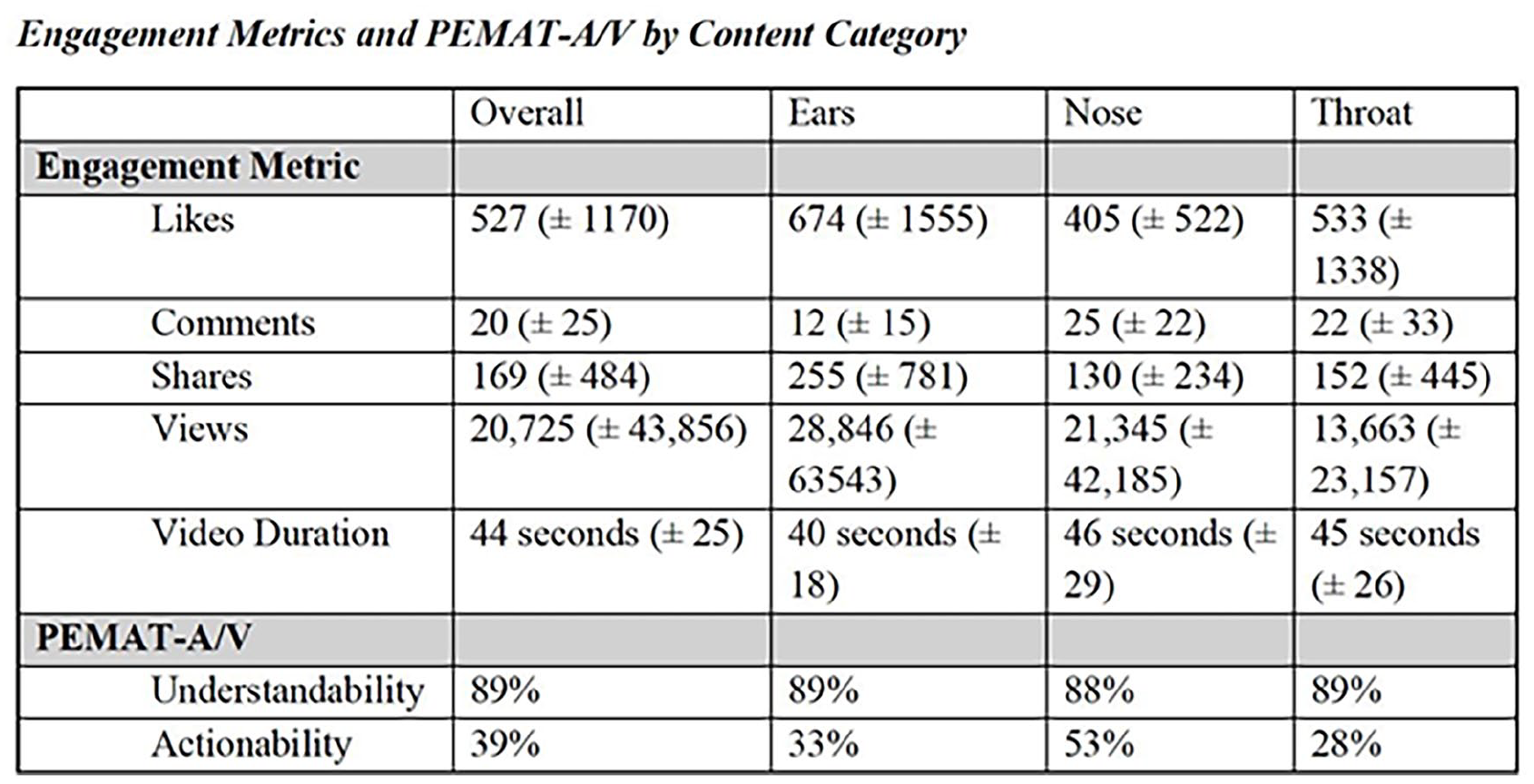
Engagement metrics and PEMAT-A/V by content category.
Accuracy Analysis
Overall, 85% of the content was completely accurate, 13% was incomplete/misleading, and 2% was completely inaccurate. Figure 3 shows the accuracy for all ENT educational videos. In the “Ears” category, 69% were completely accurate and 31% were incomplete or misleading (Figure 4). In the “Nose” category, 95% were completely accurate and 5% were inaccurate (Figure 5). In the “Throat” category, 84% were completely accurate and 16% were incomplete or misleading (Figure 6).
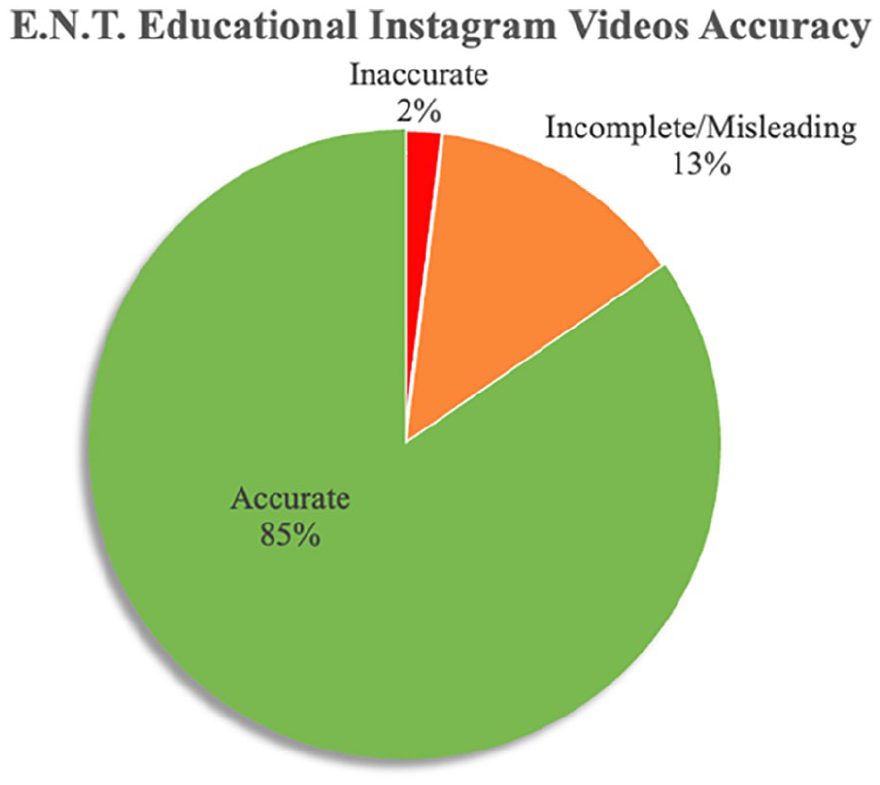
Accuracy percentage for all ENT Educational Instagram Videos: 85% of ENT medical educational videos were completely accurate, 13% were incomplete or misleading, and 2% completely inaccurate.
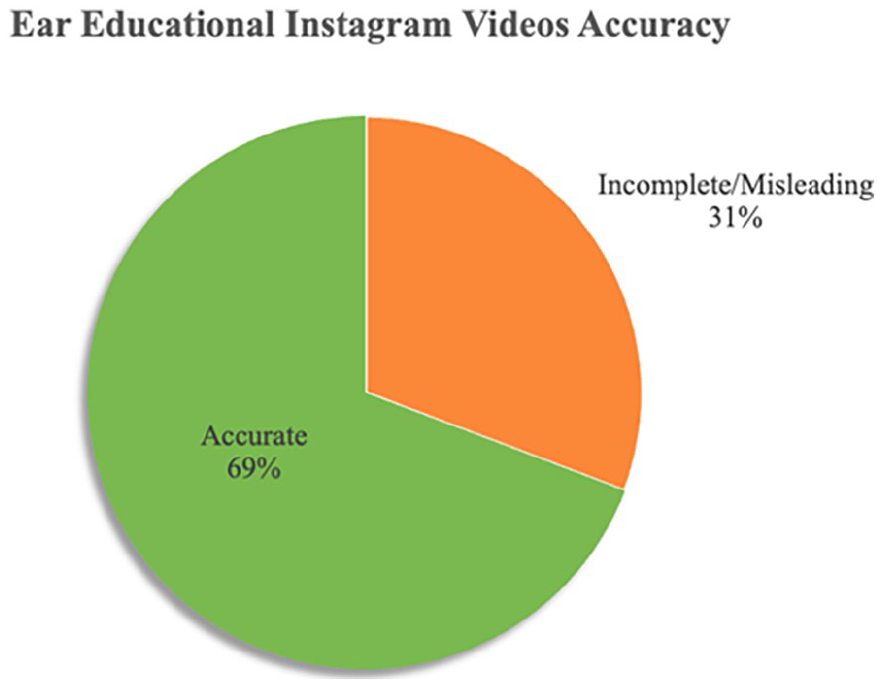
Accuracy percentage in “ears” educational Instagram videos: 69% of medical educational videos were completely accurate, 31% were incomplete or misleading, and no videos were completely inaccurate.
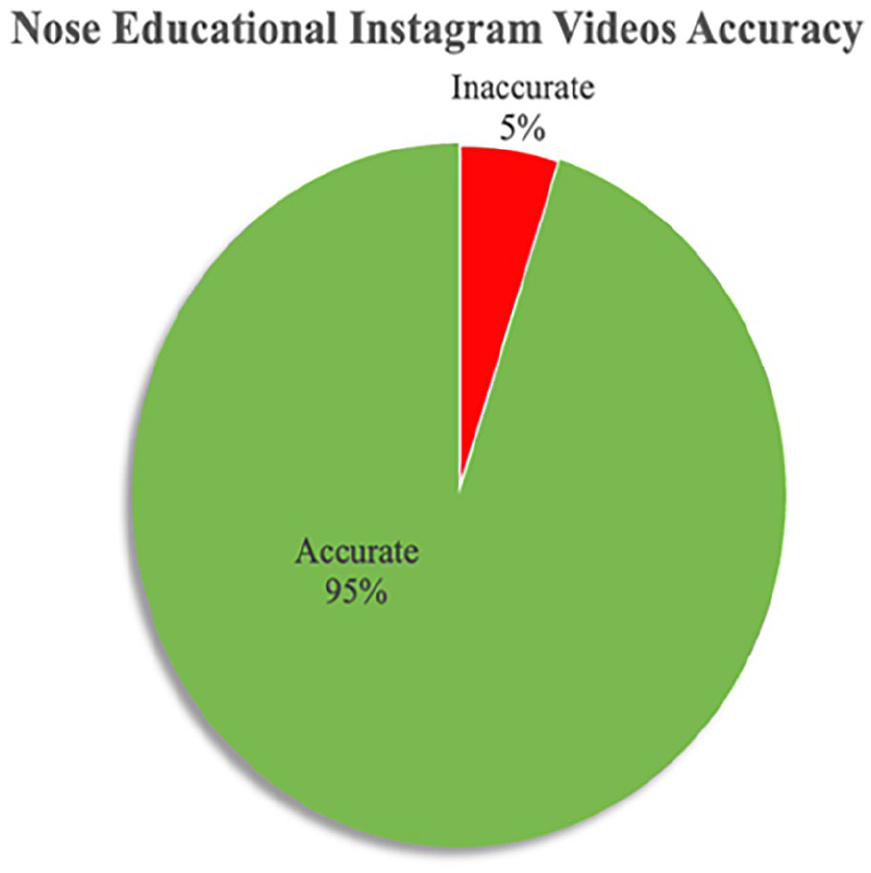
Accuracy percentage in “nose” educational Instagram videos: 95% of medical educational videos were completely accurate, 5% were completely inaccurate.
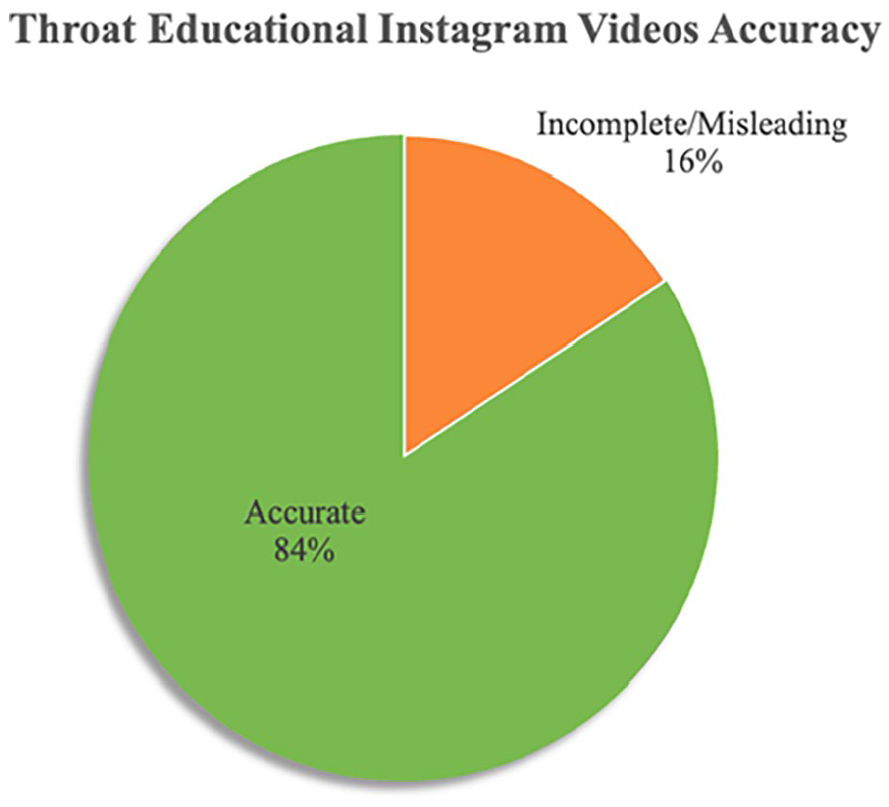
Accuracy percentage in “throat” educational Instagram videos: 84% of medical educational videos were completely accurate, 16% were incomplete or misleading, and no videos were completely inaccurate.
Hashtag Analysis
In assessing hashtag usage, six videos did not incorporate hashtags. Among the 48 Instagram videos that used hashtags, the top ones used hashtags were as follows: #otolaryngology (75%), #ent (56%), #nosebleeds (17%), #sinussurgery (17%), and #sinus (17%).
Discussion
Our study found that most otolaryngology medical education content on Instagram was accurate. A majority of otolaryngology medical education came from physicians, predominately otolaryngologists (77%). Only 3.7% of the information came from nonphysician health care providers.
Of all the videos assessed, only one was considered inaccurate, and potentially dangerous by reviewing otolaryngologists. In the post, the creator advanced various cold treatments, such as inhalation via nebulizer with iodine, nasal spray with iodine, and inhalation of hydrogen peroxide. Specific doses and brands were discussed, and viewers were assured symptomatic relief in less than 24 hours. The post failed to mention important adverse effects such as asthmatic symptoms, iodine toxicity, or ciliary dysfunction that this regimen can cause. At the time of analysis, the video garnered 13 100 views, 1271 likes, and 660 shares. It had 76 comments, most of which expressed gratitude; some questioned the regimen’s safety, but many stated they would try the treatment.
Misinformation regarding medical topics on social media platforms remains prevalent in recent times. The increasing access to technology and social media provides further user engagement and unrestricted sharing of information that is not verified for accuracy.3-7 Depending on the medical content described, 80%+ of the posted material may contain some amount of misinformation.3,8 Furthermore, a sizeable number of individuals believe there is either no or little misinformation on social media; many adults do not feel confident determining the accuracy of the social media they consume. 3
A similar study assessing the quality of tinnitus-related videos on YouTube found that a substantial amount of content was low quality or contained incorrect information, 9 with the potential to negatively impact patients. The finding highlights the need for providers to create accurate, evidence-based, and high-quality content on such social platforms.
However, health care professionals’ attempts on social media to counter these inaccuracies have not been received well.3,5-8 In particular, since there is limited information available for health care providers on how to properly address patient misinformation on social media platforms. 10
Nonetheless, the health care sphere on social media platforms should still consider a different approach to stop the rapid spread of misinformation. One approach is to incorporate evidence-based literature along with content posted on social media. A few videos in our study incorporated evidence-based research literature in their video captions to demonstrate that the content they shared is evidence-based. We recommend this as a way for physician content creators to substantiate what they are discussing and provide the public with the confidence that the information they are receiving is supported by evidence.
Understanding the intentions behind creating educational content can aid in contextualizing the variability in the quality and accuracy of the information presented. In our analysis, the majority of videos (96.3%) appeared to stem from a genuine desire to educate and share specific topics within the creators’ specialty that they believed would interest the public. Only 3.7% of the videos appeared to have an educational purpose linked to product promotion, suggesting that commercial interests may have influenced the intent for content creation. In our analysis, those products featured included an “iodine nasal spray” as a suggested treatment remedy for nasal congestion and a medical device attachment for an ear endoscope.
Benefits of Medical Education on Social Media
Previous studies have highlighted that patients often retain only a fraction of the information provided during health care visits.8,10,11 Social media educational videos on medical topics offer a convenient way for patients to access and absorb important health information repeatedly. These videos can simplify complex medical techniques, enhance understanding, and allow for repeated viewing, potentially improving adherence to medical advice and patient outcomes.12,13 In our study, 30% of videos related to rhinology were on the topic of presentation and management of nosebleeds. Many videos taught viewers how to adequately stop a nosebleed by demonstrating different techniques and maneuvers. Another video in this category discussed the anatomy and arterial mechanisms behind nosebleeds. Notably, the videos also emphasized seeking professional medical help if symptoms persist. This dual approach—empowering patients with simple, effective techniques while advising professional consultation—can help manage symptoms, potentially slow disease progression, and reduce overall health care costs and treatment times.
Adapting to Social Media
Social media platforms are characterized by short video duration. Previous research has demonstrated that brief videos on social media can effectively convey information and engage audiences.14-16 In our study, the average video duration was 44 ± 25 seconds. Providers frequently utilized the caption feature to supplement their videos with detailed explanations. Instagram captions allow providers to define medical terms, present additional information, and cite relevant literature. 15 This added context can enhance the audience’s understanding and engagement with the content, compensating for the brevity of the videos and ensuring comprehensive information dissemination. Therefore, we recommend that providers increase utilization of the caption feature and encourage viewers at the end of videos to read the caption for more comprehensive information. This approach can allow for more detailed content to be shared on Instagram and helps reduce the risk of inaccurate or misinterpreted information.
Content Discoverability on Social Media
Several factors, including the use of hashtags, influence content discoverability on platforms such as Instagram. Studies have shown that hashtags are beneficial in disseminating medical information on social media.17-20 However, the open nature of hashtags means that they can be used by anyone, leading to a mix of related and unrelated content. In our study, a search for #ENT revealed a broad range of unrelated posts. To improve the visibility of relevant content, we recommend using multiple, specific hashtags related to the topic. This strategy can target the intended audience more effectively and reduce the likelihood of losing educational videos amidst unrelated content.
PEMAT-A/V Analysis for Medical Education Video Category
Two independent graders assessed the understandability and actionability of Instagram videos by using the PEMAT-A/V grading system. 21 The low actionability of 39% observed in our study is attributed to the tendency of many providers on social media to avoid providing actionable medical advice. Providers recognize the importance of personalized medicine and prioritize safeguarding individuals by refraining from providing specific medical advice. Therefore, most of the videos are created for educational purposes rather than treatment advice. Furthermore, some providers go the extra mile by including a disclaimer in their video caption or at the beginning of the video, making individuals aware that the content is intended for educational purposes and not as medical advice.
Conclusions
Our analysis of the accuracy, quality, and engagement of otolaryngology-related educational material on Instagram revealed that most of the information is accurate, with some misleading and inaccurate content. Although the inaccurate video is small in comparison, it had moderate user engagement, indicating that even a single inaccurate video can adversely reach and influence many people.
Future research should analyze the accuracy, engagement metrics, understandability, and actionability of otolaryngology-related medical education content shared by health care providers on other social media platforms, such as TikTok and Facebook. Such a comparative analysis may help differentiate the accuracy between platforms and whether health care providers exhibit a higher engagement on one platform over another.
Study Limitations
While these metrics reflect the engagement data for otolaryngology-related content on Instagram, it is important to acknowledge an inherent potential limitation of utilizing this platform for analysis. Our analysis does not provide a comprehensive representation of all user interest and engagement on otolaryngology-related content on Instagram. We acknowledge that some algorithmic bias may exist, potentially affecting the generalizability of our findings. This study could have benefited from applying the same methodology across multiple different accounts to better assess and ensure generalizability. Therefore, our project offers a semi-personalized snapshot of video engagement on otolaryngology-related content on this platform. Furthermore, social media platforms are dynamic, and engagement metrics vary based on the time of analysis; therefore, results may vary if conducted by a different person at a different time point.
Although the term “otolaryngology” is rarely used in lay language, this may be a reason why people turn to social media to search for quick education about this specialty and what it entails. This potentially limits our study; however, our focus was to assess the quality and accuracy of these materials. In our preliminary study, we used “#ENT”, a more-commonly-used term, but using “#ENT” resulted in numerous unrelated contents. Expanding this study to include other social media platforms, such as the rapidly-growing TikTok, would be beneficial. The use of certain social media platforms varies between institutions review board. In our case, as a state-funded institution, our state legislation bans the access and use of TikTok data, thus precluded our ability to broaden our understanding of the quality and accuracy of otolaryngology-related medical educational content on this rapidly-growing platform.
Footnotes
Acknowledgements
The authors thank the content creators whose videos served as the basis of our research. Their commitment to spreading medical knowledge to the public not only enriched the platform of Instagram but also provided valuable information for academic research.
Author’s Contributions
Ogechukwu S. Anwaegbu: Conception, drafting, and editing of the article. Michel M. Adeniran, Adannaya C. Ihediwa, Joshua E. Lewis, Shobit D. Srivastava, and Tyler A. Janz: drafting and editing of the article. Brian J. McKinnon: Editing of article and study supervisor.
Data Availability
Data can be accessed by using Instagram platform to search for the relevant hashtags as outlined in the methods section of this study.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Brian J. McKinnon is an editorial board member. The authors Ogechukwu S. Anwaegbu, Michel M. Adeniran, Adannaya C. Ihediwa, Joshua E. Lewis, Shobit D. Srivastava, and Tyler A. Janz declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
The University of Texas Medical Branch Institutional Review Board (IRB) exempted this study (IRB protocol no.: 24-0008) from review in accordance with the review boards policy 45 CFR 46.104.
