Abstract
Our case study explores Bell’s palsy, a rare lower motor neuron facial nerve paralysis, particularly rare in newborns. While often idiopathic, it can stem from congenital or developmental factors. Unilateral facial paralysis is more prevalent, with Bell’s palsy accounting for more than 50%, while bilateral facial paralysis is exceptionally rare. We present a distinctive case of idiopathic Bell palsy in a 3.5-month-old infant, initially affecting the right side and spontaneously resolved within 30 days, followed by involvement on the left side a month later. Despite comprehensive evaluations and treatment, persistent facial weakness was observed on the left side. The patient initially responded well but faced ongoing challenges during the second attack. Our findings underscore the need for further research to improve the understanding and management of these cases.
Introduction
Bell’s palsy is a sudden onset, typically lower motor neuron facial nerve paralysis of unknown cause. It is uncommon in newborns. Facial paralysis can be congenital or developmental. Congenital palsy is the result of trauma during birth. Developmental palsy arises from developmental anomalies, such as the absence or underdevelopment of the nuclei of the cranial nerve, the lack of development of the nerve centers, and the absence or underdevelopment of the facial nerve itself. 1 Facial nerve palsy (cranial nerve seven) is a common neurological condition in children, often labeled Bell’s palsy when the cause is unclear. 2 Facial nerve paralysis in a newborn can stem from various causes beyond idiopathic Bell’s palsy. It is crucial to consider congenital, infectious, inflammatory, neoplastic, and traumatic factors before definitively diagnosing idiopathic Bell’s palsy. 3 Unilateral facial paralysis is quite common, with an incidence of 20 to 25 per 100,000 people, and the majority of cases (more than 50%) are ascribed to Bell’s palsy, also known as idiopathic facial paralysis.4,5 On the contrary, bilateral facial paralysis is extremely rare, accounting for only 0.3% to 2.0% of cases of facial paralysis.6,7 Bilateral facial palsy is defined by paralysis that affects both sides of the face, with symptoms appearing simultaneously or with the second side affected within 30 days of the first side. 8
In this article, we present an unusual case of Bell’s palsy idiopathic, in which the right side was initially affected, spontaneously recovering within 30 days, followed by involvement of the left side, which occurred a month after recovery of the right side.
Case Presentation
A 3.5-month-old girl was brought to the emergency center due to a sudden onset of facial asymmetry. The mother observed a change in the right corner of her mouth and an inability to close her right eye. The asymmetry was initially mild, worsened over a few hours, particularly when the baby cried, and was accompanied by excessive drooling from the right side of her mouth. The mother denied having any history of fever, feeding difficulties, or lethargy.
The mother had a urinary tract infection in the eighth month of pregnancy. The baby was delivered full-term via Cesarean section due to a breech presentation and a cord around the neck, with no signs of birth trauma. The baby weighed approximately 3.36 kg at birth and had normal Apgar scores. The mother confirmed that facial asymmetry was not present in the first months of her life. There was no family history of neurological diseases or a recent history of fever, cough, skin rashes, or trauma.
On general physical examination, the baby appeared active and alert, with a normal pulse and blood pressure. Her head circumference was 37 cm, showing a typical head shape. A positive red reflex was observed, along with reactive pupils, and no apparent restrictions in eye movements. However, her mouth exhibited deviation to the right side. Collectively, these observations indicated palsy of the right lower motor neuron facial nerve. The remainder of the neurological examination showed normal spontaneous movement in all limbs, intact deep tendon reflexes, symmetric neonatal reflexes, and no abnormal neurocutaneous stigmata.
Her basic diagnostic workup was largely noncontributory. She had normal complete blood count, serum Urinary creatinine excretion (UCE), lactic acid, C-reactive ammonia, protein, glucose, and arterial blood gases. The cerebrospinal fluid (CSF) analysis yielded negative results for gram stain, bacterial culture growth, and viral polymerase chain reaction (PCR) studies. Her CSF did not show abnormal findings, lactic acid and angiotensin-converting enzyme levels were also normal. Magnetic resonance imaging (MRI) of the brain was performed and normal was reported as shown in Figure 1. The diagnosis of idiopathic Bell palsy was then made.
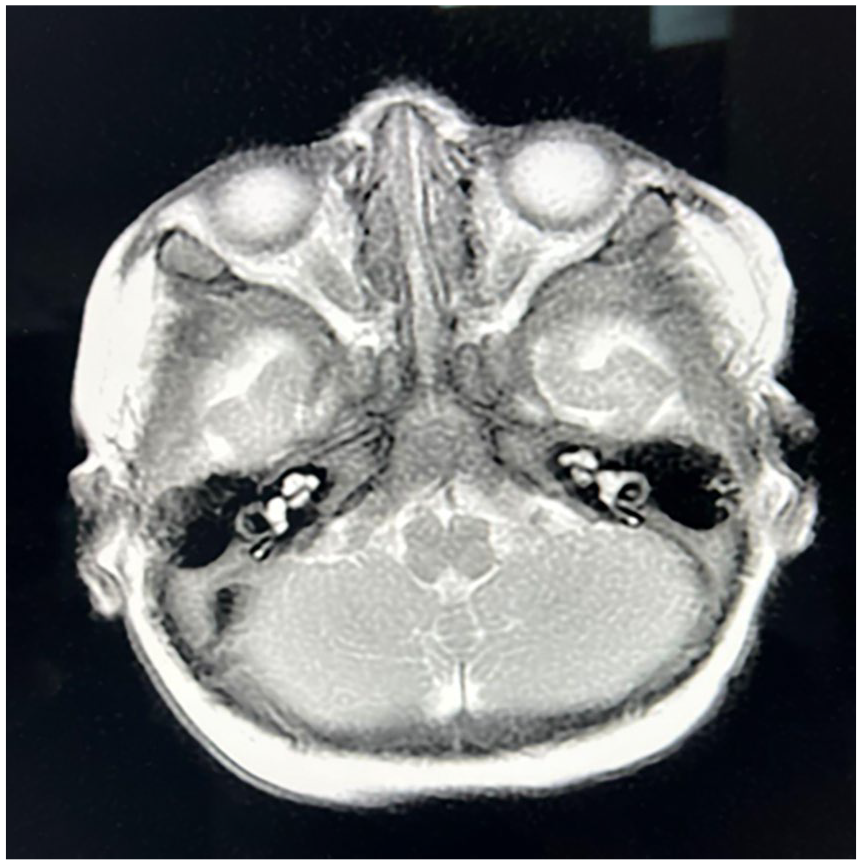
Shows the magnetic resonance imaging of the brain with the normal trajectory of the bilateral facial nerves.
Neurological examination revealed the bilateral Bell sign, indicating the inability to close the eyes or raise the eyebrows. These findings suggest a bilateral complete lower motor neuron type of facial palsy, classified as grade 4 on the House-Brackmann scale. This indicates moderate to severe weakness, with incomplete eye closure.
The patient started with soluble oral prednisolone at a dose of 0.5 mg/kg/day for 7 days, 2.5 ml of vitamin D and ossein mineral complex syrup once a day, and 3 drops of iron between feeds.
A month later, the mother noticed a change: the left corner of the mouth was now noticeably deviated and the inability to close the left eye seemed compromised, despite previous exhaustive evaluations, including an MRI with unremarkable findings. The patient underwent the same treatment protocol as in her initial attack.
Following her initial attack, the patient showed remarkable and rapid improvement, achieving complete recovery in 2 weeks. Subsequent neurological examinations revealed complete symmetry on eye and mouth closure, even during crying. However, during the second attack, despite ongoing physical therapy and oral prednisolone at a dose of 0.5 mg/kg/day for 7 days. The patient’s facial weakness persisted. However, he remains active, meets developmental milestones appropriate for her age, and continues to experience healthy weight gain.
Discussion
This case, apart from the patient’s unusual age at the time of symptom onset, is a typical instance of idiopathic Bell’s palsy. Numerous instances of seventh nerve palsy have been documented in newborns, with the vast majority attributed to birth trauma, which is also the primary cause of most cases of congenital facial palsy. 9 The risk factors for such trauma include pre- and post-maturity, being the firstborn, overweight, and the use of forceps or Cesarean sections during delivery.10,11 Manzouri et al reported a case of a 3-month-old baby with acute unilateral facial nerve paralysis, presumed to be Bell’s palsy after excluding other causes, who showed partial response to oral steroids. 12 Although facial nerve palsy is not the most prevalent neurological disorder in the pediatric population, its clinical impact is substantial. 13 It significantly affects functional and aesthetic aspects, compromising the quality of life of affected children. 14 Despite the relatively favorable natural progression of the disorder, it is often considered a pediatric neurological emergency by many caregivers, especially as it can disrupt breastfeeding, a crucial activity at that age. 15 Children with Bell’s palsy often experience remarkable natural healing. Approximately 90% of them show significant improvement in 6 months and nearly all, close to 100%, recover fully within 1 year. 3
Bilateral facial palsy is extremely rare, accounting for only 0.3% to 2% of all facial palsies, with an incidence of just 1 in 5,000,000 people. 16 Lyme disease, caused by the Borrelia burgdorferi spirochete infection carried by common ticks, accounts for 50% of bilateral facial palsy cases in children.17-19
The illness typically unfolds in 3 stages: starting with fever and headaches, progressing to meningitis and encephalitis, and finally leading to severe arthritis and persistent central nervous system problems. Therefore, it is critical to pinpoint the cause of facial paralysis in children. Jairath et al documented a series of cases in India where Lyme disease manifested with various skin symptoms. 19 A thorough assessment is necessary to uncover any central lesions responsible for bilateral facial nerve paralysis. Instances of bilateral transient facial paralysis in young people are extremely rare. Siwula et al recounted a similar scenario in which a 6-year-old child experienced a sudden onset of facial paralysis. 16
In this case, the differential diagnosis of Lyme disease, Moebius syndrome, was excluded based on clinical signs and symptoms. Blood cultures test was also negative and real-time PCR analysis did not show any reaction for Herpes Simplex Virus (HSV-1 and HSV-2), Enterovirus, varicella zoster, and paramyxovirus, all of which could potentially cause transient bilateral facial weakness. Brain MRI was normal, effectively eliminating the possibility of central lesions as the cause of facial palsy. Therefore, after a comprehensive investigation, we have excluded all other potential causes of bilateral facial palsy by correlating with clinical, laboratory, and radiological findings; therefore, it was hypothesized that the present case was a positive diagnosis of idiopathic bilateral Bell’s palsy. This case is exceptionally unique, as it marks the first reported worldwide instance of Bell’s palsy affecting both sides of the face, with a 1 month interval between occurrences.
Footnotes
Acknowledgements
The authors are very appreciative of the patient for the opportunity to learn and thankful to the hospital for providing support for completing this report.
Author Contributions
Fnu Yogeeta: contributed to the conceptualization, writing—original draft, final approval, and agreeing to the accuracy of the work. Muskan Devi: contributed to the conceptualization, writing—original draft, final approval, and agreeing to the accuracy of the work. Sameer Abdul Rauf: contributed to writing—original draft, final approval, and agreeing to the accuracy of the work. Sanam Bano Rajper: contributed to writing—original draft, final approval, and agreeing to the accuracy of the work. All authors approved the final version to be published.
Data Availability Statement
The data that support the findings of this article are available from the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Patient Consent
Written informed consent was obtained from the individual(s) for the publication of any potentially identifiable images or data included in this article.
