Abstract
Highlights
High-energy, high-fat diet with the onset of chronic sinusitis.
Cucumber, rice, bread, and pork chops were associated with the onset of chronic sinusitis.
Promoting an anti-inflammatory dietary pattern be a valuable strategy for the prevention and treatment of chronic sinusitis.
Introduction
Chronic rhinosinusitis (CRS) is common in the field of otorhinolaryngology, as well as head and neck surgery. Its primary symptoms include nasal congestion, mucous or mucopurulent nasal discharge, head and facial swelling, and loss of sense of smell. 1 CRS has an overall prevalence of 5.5% to 28%.2,3 This condition is highly heterogeneous, with chronic inflammatory changes primarily affecting the nasal mucosa. It results from a complex inflammatory process, mediated by various factors, such as anatomical structure, genetics, and environment. 4 According to the 2020 European Position Paper on Rhinosinusitis and Nasal Polyps (EPOS) guidelines, sinusitis is divided into primary and secondary, localized and diffuse, or allergic and nonallergic types. 3 The sinus mucosa is a biomechanical barrier composed of an intact mucus-cilia system, epithelial cells, and neutrophils.5,6 Among these, epithelial cells are an important component of innate immunity and serve as the first line of defense against external stimuli.7,8 Researchers have identified at least 10 inflammatory endotypes associated with CRS, 9 which include 3 main endogenous types, usually associated with elevated levels of typical lymphocytic factors; the first type is influenced by interferon-gamma secreted by T helper type (TH) 1 cells, 10 the second is affected by interleukin (IL)-4, IL-5, and IL-13 secreted by TH2 cells, 11 and the third is affected by IL-17 secreted by TH17 cells. 12 The prevalence of these endotypes varies geographically worldwide, 13 with notable ethnic differences. 14 As a noninfectious inflammatory disease, CRS can be managed through various treatment approaches, including conventional glucocorticoid, antibiotic, and surgical treatments. 15 In addition, dietary modifications aimed at reducing pro-inflammatory factors can significantly benefit individuals with chronic sinusitis. 16
As the global economy continues to grow, Western dietary patterns, characterized by high-calorie and high-fat intake, is becoming more and more common in the world. 17 These Western dietary patterns are typically characterized by high consumption of red meat, processed meats, refined grains, added sugars, and saturated fats but a significantly low intake of fruits, vegetables, whole grains, and fish. 18 Such dietary choices have been linked to the growing prevalence of non-communicable diseases, and are associated with an elevated risk of various health issues, including obesity, type 2 diabetes, cardiovascular disease, inflammatory digestive disease, certain types of cancer. 19 Promoting healthy eating habits and encouraging individuals to adopt a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and low-fat dairy products is of utmost importance. The functioning of tissue-specific and systemic immune responses is intricately intertwined with metabolic regulation, and their normal functions are interdependent. It is worth noting that dietary structure and habits vary from country to country. 20 Understanding the impact of modern lifestyles and the Western Diet on the sinus mucosa’s inflammatory response is essential for developing prevention and treatment strategies for chronic sinusitis and improving the overall quality of life. 21 Accumulating studies have demonstrated the effectiveness of healthy dietary practices (eg, Mediterranean dietary patterns) in managing certain health conditions. 22 However, the connection between diet and sinusitis has not been extensively explored. Accordingly, using the 2012 Korean National Health and Nutrition Examination Survey (KNHANES) database, we analyzed the correlation of CRS with basic population information, dietary intake, individual dietary inflammatory index (DII), and food intake frequency to identify natural remedies for the prevention and treatment of sinusitis in Asians.
Materials and Methods
Study Design and Population
This study used data from the KNHANES 2012 cross-sectional survey, which was guided by EPOS 2012 and conducted jointly by the Korean Academy of Otolary-ngology—Head and Neck Surgery and the Korean Center for Disease Control and Prevention. The population for this survey was selected using stratified clustering methods. KNHANES data were collected through 3 main methodologies: health questionnaires, health examinations, and physical examinations. These datasets were derived from nutritional questionnaires evaluated by experienced ear, nose, and throat (ENT) specialists, registered nurses, and laboratory technicians. These questionnaires gathered essential information on the Korean national population, encompassing health surveys, nutritional surveys, ENT examinations, 24 hour food intake, and food intake frequency. Detailed information can be downloaded and accessed through the official website of KNHANES (https://knhanes.kdca.go.kr/).
In this study, we selected 7421 participants who underwent ENT examinations from the 2012 KNHANES database. Participant inclusion was based on their responses to the question “Have you been diagnosed with chronic sinusitis” on an ENT questionnaire completed after an ENT interview and nasal endoscopy. Approximately 200 ENT physicians were involved in participant evaluations. Finally, 6342 participants were enrolled (2664 men and 3678 women), of whom 488 were adolescents (aged 13-19 years) and 5854 were of other ages. Subsequently, we conducted correlation analyses of the basic information, dietary intake, and food intake frequency data with CRS. Notably, the food intake frequency section excluded 3025 nonresponders, resulting in a final sample of 3317 participants for the statistical analysis (Figure 1).
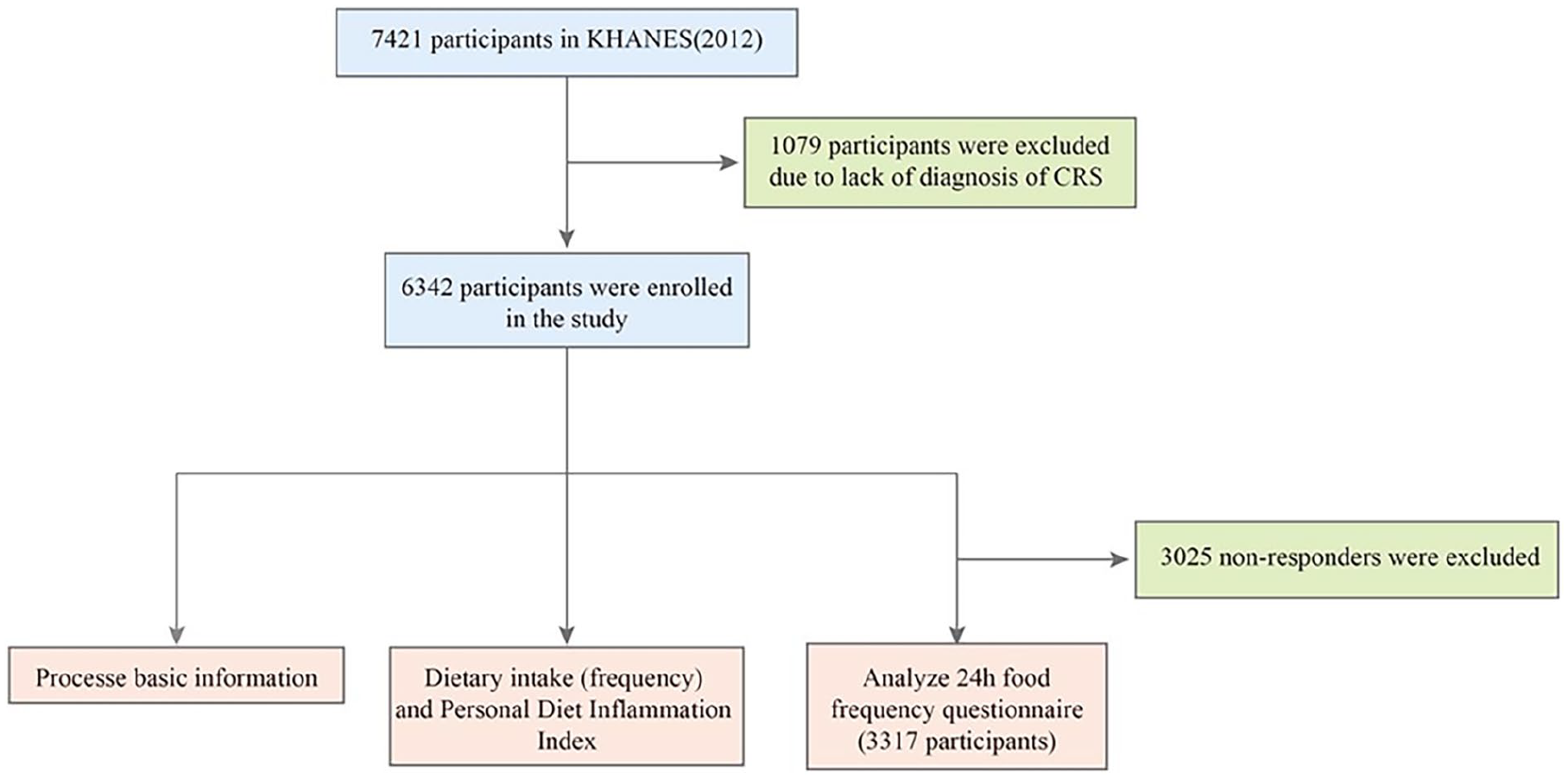
Study enrollment and process.
Demographic Characteristics
In this study, some data were categorized, and the included population was divided into 2 distinct groups: a disease group and a healthy group. Basic information included sex, age (13-19 years vs other age groups), annual household income (lower vs middle/high income), occupation (managers, specialists, and related personnel vs other professionals), education (university and above vs below), residence (urban vs rural), body mass index (BMI; ≥25 vs <25 kg/m2), smoking (smoker vs nonsmoker), and alcohol consumption (drinker vs nondrinkers). To collect information on food intake frequency, we utilized food intake questionnaires that covered 63 common food items. Each food’s intake frequency was classified as either low frequency (less than the median) or high frequency (greater than the median).
Statistical Analysis
The data from the 2012 KNHANES were used for this study, and statistical analysis related to CRS was performed using SPSS version 26.0. We used chi-square tests to analyze the correlations between participants’ basic information (sex, age, annual household income, occupation, education, place of residence, BMI, smoking, and alcohol consumption) and CRS. To address the small amount of missing data in the basic information (annual household income: 39 missing data, and education: 244 missing data), we replaced the missing values with the series mean. The correlation between 24 hour dietary intake and CRS was assessed using 2 independent samples of nonparametric tests, and the calculated individual DII was compared using a chi-square test. Because of the large number of nonresponse samples for food intake frequency data, the sample size was adjusted to 3317 according to the number of responses received. The correlation between food intake frequency and CRS was evaluated using a chi-square test, followed by adjustments of P values, odds ratios (ORs), and 95% confidence intervals (CIs) using binary logistic regression models based on basic information such as sex, age, annual household income, occupation, education, and place of residence. All tests were 2-tailed, with a significance level of 0.05. The binary logistic regression models were performed using data with a P value of less than .20 in the 1-way analysis.
Results
Basic Demographic Information and CRS Onset
To explore the association between basic demographic factors and the onset of CRS, we used data from the 2012 KNHANES, involving 6342 participants. The prevalence rates of CRS were 0.87% among adolescents aged 13 to 19 years; 0.91% among the lower-income group; 0.91% among managers, specialists, and related personnel; and 1.96% among those with university-level education or higher. The univariate statistical analysis (Table 1) showed that adolescents (P < .001, OR = 1.760, 95% CI = 1.306-2.373); lower income groups (P = .007, OR = 0.678, 95% CI = 0.510-0.900); managers, specialists, and related personnel (P = .006, OR = 1.495, 95% CI = 1.119-1.997); and those with a university-level education or higher (P = .005, OR = 1.364, 95% CI = 1.099-1.693) exhibited statistically significant associations with CRS. Subsequent adjustment using binary logistic regression models revealed that adolescents [adjusted P value (aP) < .001, adjusted odds ratio (aOR) = 1.881, 95% CI = 1.380-2.564] and those with college-level education and higher (aP = .042, aOR = 1.298, 95% CI = 1.009-1.669) maintained their significant associations with CRS.
Correlations of Basic Demographic Information With CRS Onset.
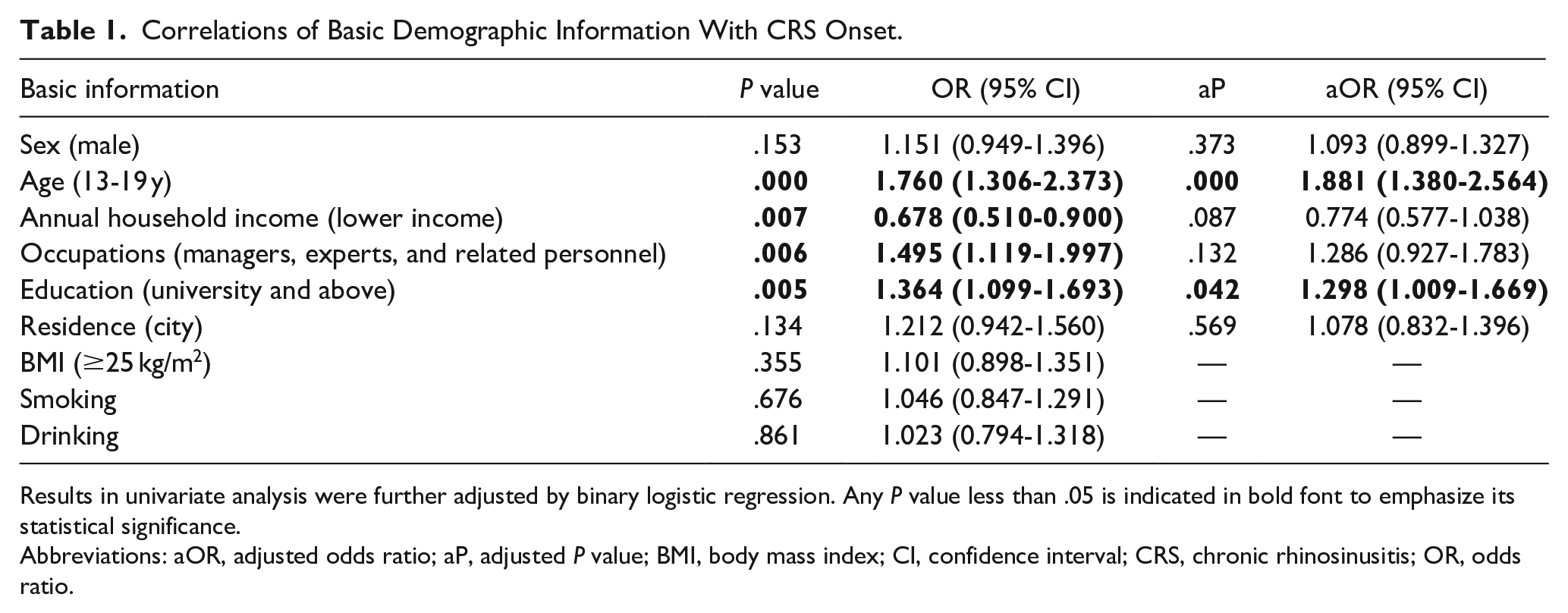
Results in univariate analysis were further adjusted by binary logistic regression. Any P value less than .05 is indicated in bold font to emphasize its statistical significance.
Abbreviations: aOR, adjusted odds ratio; aP, adjusted P value; BMI, body mass index; CI, confidence interval; CRS, chronic rhinosinusitis; OR, odds ratio.
Dietary Intake and Individual DII
To explore the correlation between dietary intake, individual DII, and the development of CRS, we used the 2012 KNHANES 24 hour dietary intake recall data, which provided discrete trends expressed in quartiles. A total of 6342 participants were included in this study. We identified 11 categories of dietary intake elements (fat, energy, carbohydrate, niacin, protein, riboflavin, thiamin, vitamin A, vitamin C, carotene, and iron) using reference food data. We found that fat (P = .001, IQR = 34.085) and energy (P = .004, IQR = 981.106) were significantly associated with the development of CRS (Table 2). For the purpose of comparison, we divided the individual DII into 4 subgroups based on quartiles, that is, Q1 (<1.15), Q2 (1.15-1.25), Q3 (1.25-1.50), and Q4 (>1.50) groups, with Q1 as the reference group (Table 3). Notably, we observed an increasing prevalence of CRS in the Q2, Q3, and Q4 groups, with the highest prevalence of 2.32% occurring in the Q4 group (P = .004, OR = 1.484, 95% CI = 1.132-1.946).
Correlation Between Dietary Intake and the Development of CRS.
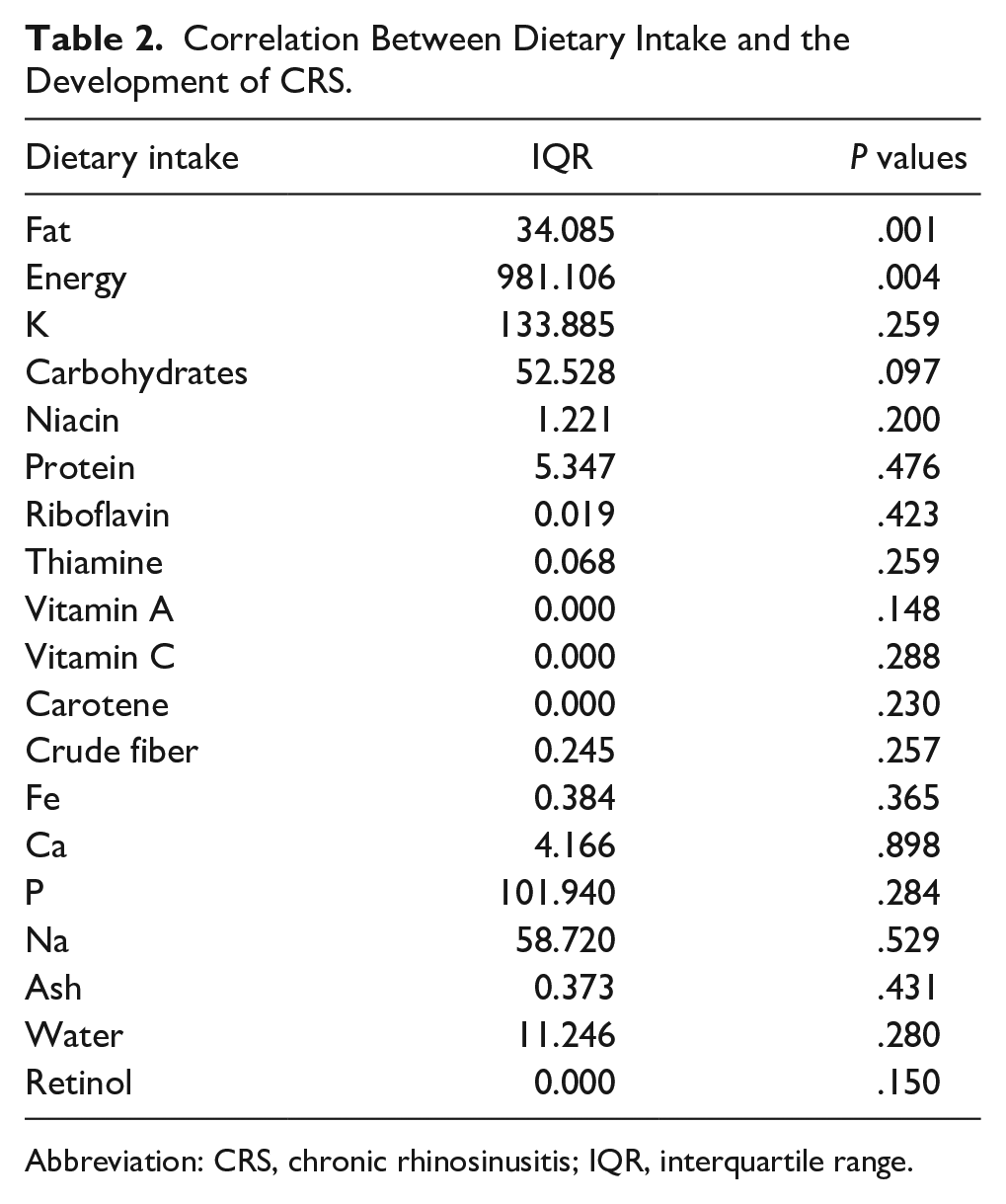
Abbreviation: CRS, chronic rhinosinusitis; IQR, interquartile range.
Correlation Between Dietary Inflammatory Index and the Development of CRS.
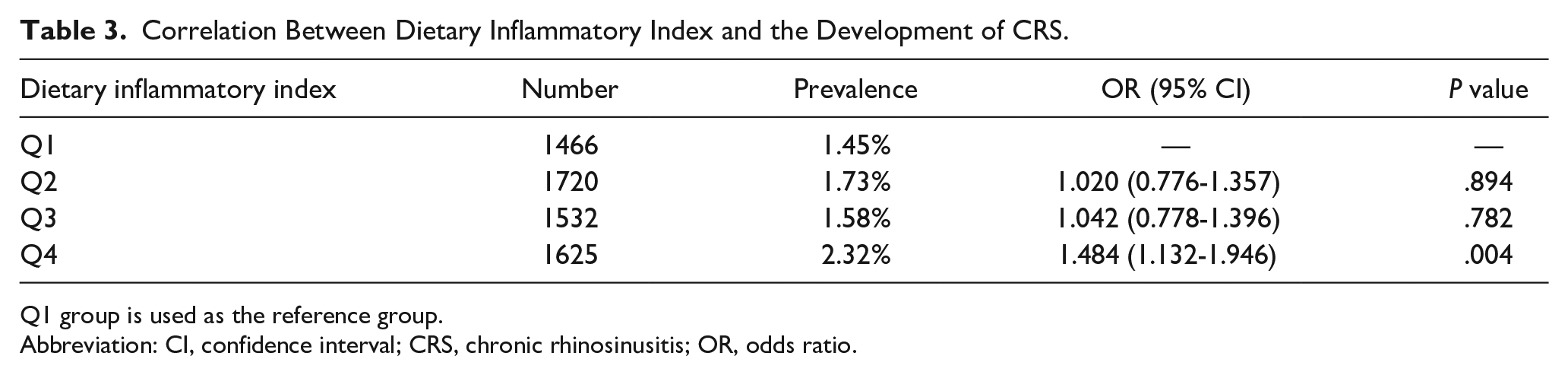
Q1 group is used as the reference group.
Abbreviation: CI, confidence interval; CRS, chronic rhinosinusitis; OR, odds ratio.
Food Intake Frequency
To investigate the correlation between different food intake frequencies and CRS, we utilized data from the 2012 KNHANES food intake frequency survey. To ensure the reliability of our analysis, we excluded 3025 participants who did not respond to this food intake frequency survey, resulting in a final sample of 3317 participants for data analysis. The binary logistic regression model was adjusted for sex, age, annual household income, occupation, education, and place of residence. Subsequently, we generated a forest plot (Figure 2). Among the various food items analyzed, cucumber consumption exhibited a significant association with the low risk of CRS (aP < .001, aOR = 0.547, 95% CI = 0.415-0.721). Conversely, fried pork chops (aP = .028, aOR = 1.335, 95% CI = 1.033-1.777), bread (aP = .024, aOR = 1.364, 95% CI = 1.042-1.786), and rice (aP = .021, aOR = 1.382, 95% CI = 1.051-1.818) were associated with a higher likelihood of CRS.
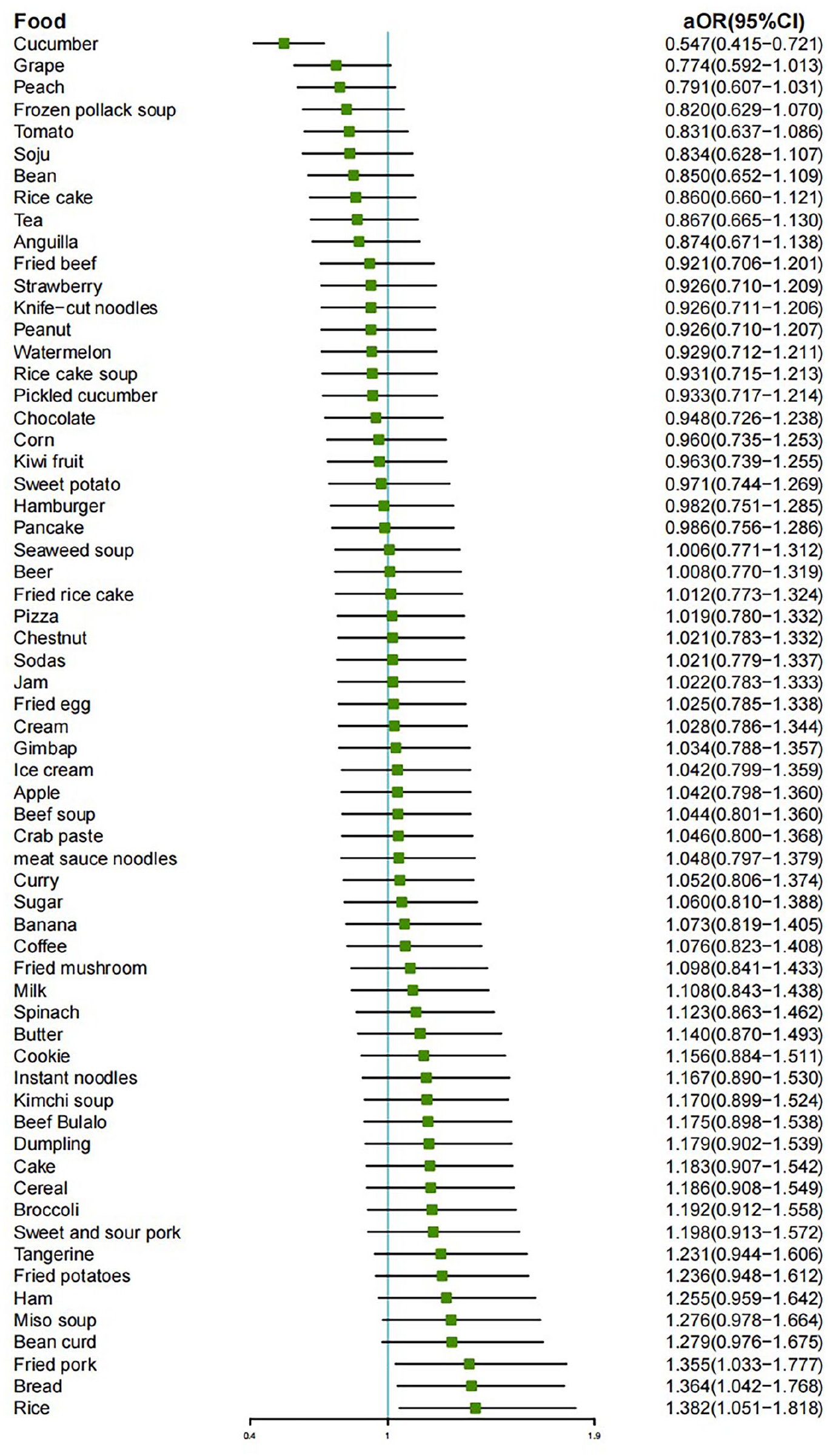
Forest plot of dietary intake. Adjusted odds ratios (ORs) and 95% confidence intervals (CIs) depict the associations between various dietary intake patterns and chronic rhinosinusitis (CRS) when compared to the healthy group. Binary regression models were adjusted for sex, age, annual household income, occupation, education, and place of residence.
Discussion
This study explored CRS based on the latest version of the EPOS 2020 guidelines, which are different from the EPOS 2012 guidelines used in the KNHANES 2012 database; notably, CRS is no longer simply divided into CRS with and without nasal polyps. The updated guidelines offer more nuanced insights into the cellular and molecular pathophysiological mechanisms. 23 Despite evidence indicating variations in CRS prevalence across different ethnic groups, most current studies have predominantly focused on European and American populations. 24 It is also possible that recent studies have found an increase in the prevalence of CRS compared to 10 due to modern technological advances and environmental degradation, which have made the diagnosis of CRS more accurate. An innovative aspect of this study is that it investigated the CRS prevalence in Korean populations using the KNHANES database, which better represents the characteristics of the onset of CRS in an Asian population, thereby contributing to a more comprehensive understanding of CRS. Furthermore, the decision to utilize data from the most recent year, despite potential limitations in the sample size, is commendable. This approach ensures that the study’s findings align more closely with the current living environment and dietary habits, enhancing its representativeness. In addition, the database is curated and maintained by professionals in diagnosing CRS and conducting nutritional analysis of ingested foods, thus strengthening the study’s credibility.
While analyzing the correlation between the onset of CRS and dietary factors, we were surprised to find that the onset of CRS was also correlated with age, household income, occupation, and education levels. These findings are aligned with the guidance provided by the EPOS 2012 guidelines and the existing literature. 25 In addition, we found that adolescent groups were more prone to developing chronic sinusitis, a trend in line with prior research. In terms of sex, some studies suggest that men are more likely to develop CRS. 26 However, given our study’s focus on data from 2012 and its relatively small sample size, we did not observe this sex-related correlation in our analysis. Interestingly, while one epidemiological study of São Paulo residents showed a significant association between the prevalence of CRS and low household income, 27 our adjusted and processed data did not reveal such a correlation. Moreover, in a study on the relationship between socioeconomic status and the onset of CRS, Kilty et al concluded that the lower the education level, the more significant the CRS symptoms. 28 Similarly, another study also found that a lower education level was correlated with socioeconomic status and might trigger chronic inflammation due to poor access to medical care, which might be associated with the development of CRS. However, in our current study, we observed the opposite pattern: there was a significant association between college and higher education levels and the development of CRS.29,30 These contrasting conclusions could be attributed to differences in social structures, economic conditions, and healthcare access among various countries and ethnic groups. Such factors can have varying effects on the onset of CRS, as highlighted in previous research. 31
The most significant finding in this study is that the onset of CRS is correlated with dietary factors, particularly the consumption of high-fat, high-energy foods, such as pork chops, bread, and rice. This finding aligns with the existing literature demonstrating that dietary factors have an effect on the development of rhinitis. 32 Although the disease examined in the aforementioned study is different from that in our study, the finding also reflects the influence of dietary factors on the development of otorhinolaryngological diseases. Furthermore, our study reaffirms the notion that chronic high-fat intake can alter microbial composition and mucosal structure and function, ultimately resulting in inflammation. 33 This observation is consistent with the existing body of knowledge: High-fat, high-energy diets contribute to inflammation. These findings highlight that an anti-inflammatory diet is particularly important in preventing and treating CRS. 34 A study conducted on a mouse model demonstrated that a high-fat diet led to increased plasma concentrations of the inflammatory reagent bacterial lipopolysaccharide, thereby increasing the risk of obesity and diabetes. 35 In this context, the DII is widely used to assess the overall inflammatory potential of a diet and its relevance to various diseases. In our study, the individual DII calculated from each participant’s dietary intake data provides further evidence that an anti-inflammatory diet is beneficial in reducing the incidence of CRS, and higher DII scores indicate a greater pro-inflammatory capacity of the diet. 36 In addition, a moderate negative correlation between the DII and the Healthy Eating Index has been documented. 37 Notably, our study indicated that the Q4 group was significantly correlated with the development of CRS compared to the Q1 group. This finding emphasizes the potential of advocating an anti-inflammatory diet and guiding healthy eating habits in reducing inflammatory markers and improving CRS outcomes. 38 In addition to conventional treatments for CRS, such as glucocorticoids, 39 antibiotics, 40 and surgical treatment, 41 our findings suggest that an anti-inflammatory diet is also a complementary approach for managing CRS. We believe that promoting an anti-inflammatory diet has the potential to reduce the incidence of CRS and enhance the efficacy of its treatment.
Our future research endeavors will focus on identifying which endotypes respond more favorably to the anti-inflammatory diet. This approach will enable us to provide more precise clinical recommendations, thereby enhancing the effectiveness of dietary interventions in managing CRS. This direction represents a crucial avenue for our future work.
While our study has provided valuable insights, there are areas that could benefit from improvement. First, the limited number of statistics available in the KNHANES 2012 dataset may not fully represent the diverse Asian population. Second, the world standard reference database used to calculate DII only contains dietary data from the general adult population, and most of them are from Europe and the United States. Therefore, the DII values we calculated may not fully reflect the dietary inflammation levels across different age groups in Asia.
In summary, we analyzed data from the 2012 KNHANES and found that age (13-19 years) and education levels (university and above) were risk factors for CRS, and dietary factors and fat and energy intake were closely correlated with the development of CRS. Particularly, high DII, as well as high consumption of fried pork chops, bread, and rice, were risk factors for CRS, while high cucumber consumption was a protective factor for CRS. These findings reinforce the intricate relationship between dietary habits and the occurrence of CRS. They underscore the potential significance of adopting an anti-inflammatory diet as a valuable strategy for preventing and treating CRS, not only in Korea but also on a global scale.
Supplemental Material
sj-zip-1-ear-10.1177_01455613241254281 – Supplemental material for Association Between Dietary Factors and Chronic Sinusitis Among Korean Individuals: Insights From a Large Population-Based Study in Asia
Supplemental material, sj-zip-1-ear-10.1177_01455613241254281 for Association Between Dietary Factors and Chronic Sinusitis Among Korean Individuals: Insights From a Large Population-Based Study in Asia by Jiao-Jiao Chen, Jing-Chao Sun, Zhu-Jun Yu and Zhi-Min Tan in Ear, Nose & Throat Journal
Supplemental Material
sj-zip-2-ear-10.1177_01455613241254281 – Supplemental material for Association Between Dietary Factors and Chronic Sinusitis Among Korean Individuals: Insights From a Large Population-Based Study in Asia
Supplemental material, sj-zip-2-ear-10.1177_01455613241254281 for Association Between Dietary Factors and Chronic Sinusitis Among Korean Individuals: Insights From a Large Population-Based Study in Asia by Jiao-Jiao Chen, Jing-Chao Sun, Zhu-Jun Yu and Zhi-Min Tan in Ear, Nose & Throat Journal
Footnotes
Acknowledgements
We appreciate the Korean Society of Otorhinolaryngology—Head and Neck Surgery and the members of the Division of Chronic Disease Surveillance in the Korea Centers for Disease Control and Prevention for participating in this survey and their dedicated work.
Author Contributions
J.J.C.: Data acquisition, visualization, data analysis, original draft preparation; J.C.S.: Software, methodology, visualization, data analysis, reviewing and editing; Z.J.Y.: Software, methodology, data acquisition, data analysis; Z.M.T.: Conceptualization, reviewing and editing, supervision.
Data Availability Statement
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Statement
Our study did not require further ethics committee approval as it did not involve animal or human clinical trials and was not unethical. In accordance with the ethical principles outlined in the Declaration of Helsinki, all participants provided informed consent before participating in the study. The anonymity and confidentiality of the participants were guaranteed, and participation was completely voluntary.
Institutional Review Board Statement
The KNHANES was approved by the Institutional Review Board (IRB) of the Korea Centers for Disease Control (IRB No. 1401-047-547).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
