Abstract
We present a unique case of complete tongue necrosis caused by a compression of an endotracheal tube (ETT). A 39-year-old female underwent endotracheal intubation secondary to respiratory failure following sudden altered mental status. Tongue swallowing developed and worsened with obvious pallor on examination. Extensive ischemic changes with tongue necrosis developed dramatically due to the compression during her prolonged intubation. This case of tongue necrosis highlights the importance of proper ETT sizing and positioning during prolonged intubation in ICU patients.
Introduction
Endotracheal intubation is associated with many oral complications such as damage to the lips, tooth, gums, tongue, and oral mucosa. 1 The forceful insertion of the oral endotracheal tube (ETT) is a common cause of these injuries, but it can also occur when the tube has been properly placed. 2 The tongue is a well-vascularized end-organ with its primary blood supply coming from the bilateral lingual arteries with some contribution from both branches of the facial and pharyngeal arteries. 3 Tongue necrosis is a rare entity that has been frequently associated with various conditions, including temporal arthritis, 4 rheumatoid hyperviscosity syndrome, 5 and disseminated intravascular coagulation (DIC). 6 It may also occur in the setting of cardiogenic shock in which vascular compromise may occur with hypotensive state itself and with the use of vasoconstrictors such as vasopressin, especially when a high dose or continuous infusion is required to maintain blood pressure. 7 Tongue necrosis can be severely dysfunctional and rapidly progressive and could be ultimately fatal.
Case Presentation
A 39-year-old female without a significant past medical history presented to the emergency department with history of sudden loss of consciousness and cyanosis. Thirteen minutes after the patient arrived, a respiratory failure was developed, which required intubation with mechanical ventilation in the adult intensive care unit. Placement of the ETT was satisfactory after a chest X-ray was performed post-intubation. Her temperature was 37.8 C (100 F), blood pressure was 100/62 mm Hg which required some vasopressors use, pulse was 115/min, and respirations were 21/min on mechanical ventilation. Otherwise, her past medical and surgical history are unremarkable. She smokes only on occasions and is nonalcoholic. ECG showed sinus tachycardia. Computed tomography of the head, neck and chest showed no abnormalities.
Later, on day 15 of her admission, a massive gross swelling and pallor of the tongue was noted, which necessitated tracheostomy placement with concurrent extubation. The ischemia was managed by allowing the ischemic area to demarcate and slough off naturally then chlorhexidine oral solution was prescribed.
One day after tracheostomy, extensive ischemic changes in the dorsum of the tongue from the right to the left side were observed. Eventually, on day 18 of her admission, widespread tongue tissue necrosis has developed.
On oral examination, the anterior two-thirds of the tongue was completely black and nonviable (Figure 1). However, the excision procedure was not performed because the husband and parents declined to give their consent. A conservative strategy is selected and the necrotic tissue gradually established a distinct demarcation and ultimately underwent spontaneous amputation at her 23rd day of admission.
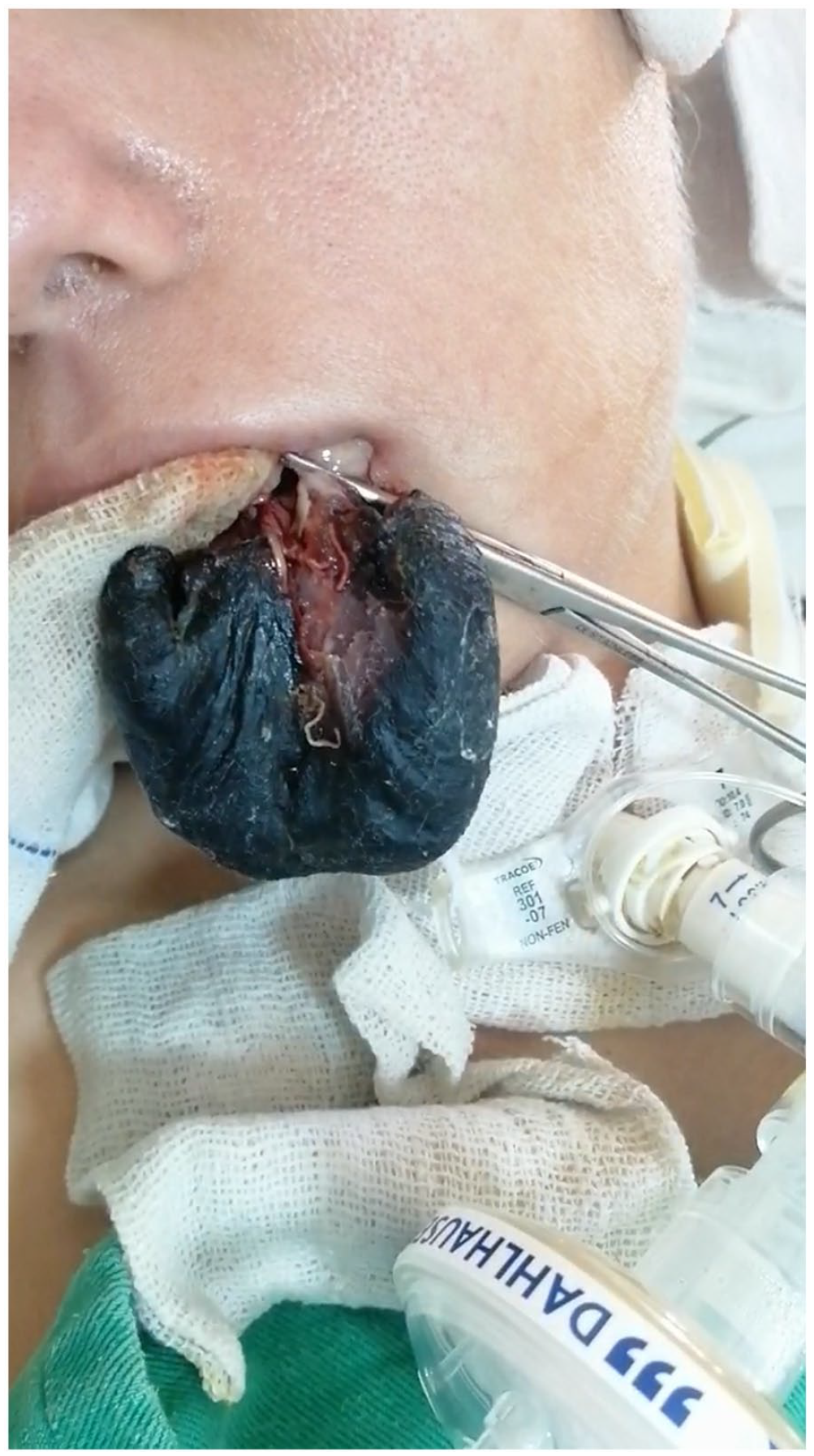
Bilateral tongue necrosis.
A small remaining tag of necrotic tissue attached to the gangrenous tongue was excised with healing by secondary intention. Her admission was further complicated by ventilator-associated pneumonia and distal limb ischemia with ulceration. Additionally, erosion and ulceration of the pinnae with some tissue loss was noted, which was basically attributed to prolonged pressure on the pinna. However, on day 33 of her admission she expired suddenly.
Discussion
To our best knowledge, this is one of the very rare reported cases of bilateral tongue necrosis in a young patient secondary to prolonged endotracheal intubation with no previous significant medical or surgical history. Tongue necrosis is a rare entity that has been frequently associated with various conditions, including temporal arthritis, 4 rheumatoid hyperviscosity syndrome, 5 DIC, 6 Kawasaki disease, 7 Wegener granulomatosis, 7 and essential thrombocytosis. 7 The occurrence of necrosis affecting two-thirds of the tongue in a young female due to prolonged oral intubation represents a highly atypical presentation. 8 In our patient, increased intraoral pressure was a big contributor to the necrosis. Our patient was not severely hypotensive on admission, and thus did not require extensive use of vasopressors. However, there is maybe a possible minor role to the poor peripheral perfusion due to vasopressor agents used during her ICU admission, as the literature reveals that vasopressin has some link with reported cases of tongue necrosis. 9 Ad-ditionally, the vasospastic effects of noradrenaline may magnify the effect of the pressure caused by oral intubation. 10 Ischemic necrosis of the tongue in intubated patients is rare and has previously been reported in patients with cardiogenic shock requiring pressor support, or those undergoing prolonged neurosurgical procedures that require flexed thoracic-cervical positioning during spinal surgeries or head and neck surgeries.11,12 However, our patient has no signs of cardiogenic shock or any past surgical history.
A number of other potential causes of tongue necrosis was reasonably excluded from the patient past medical history, physical examination, and laboratory findings.
Prolonged intubation, which refers to intubation lasting beyond 7 days, is typically linked with mild, yet potentially serious complications. One of these complications is tongue swelling, which is a common occurrence following surgical procedures and has been reported previously. In addition to these mild complications, patients may also encounter difficulties with speaking and swallowing after extubation. However, more severe complications such as laryngeal injury and upper airway distress that require advanced airway management have also been documented.13,14
Factors that contribute to tongue necrosis in ICU patients include local pressure from ETT, deep sedation, and hemodynamic instability. 15
Necrosis of the tongue in this case is unique because it was probably due to the prolonged oral intubation with compression by an anesthetic tube. The necrosis of the dorsum of the tongue was progressive from the left to the right side to involve the side not compressed by the tube.
Conservative management is typically used for tongue necrosis, with the necrotic tissue eventually demarcating and auto-amputating over time which can lead to functional deficits and deformity. 16 Surgical treatment may be an option, involving debridement to aid with healing and rehabilitation.
To avoid the potential development of tongue necrosis, it is crucial to take special care in orienting and securing ETTs properly in intubated patients. In cases where the ETT is compressed, repositioning, resizing, orienting, and securing the tube, along with regular checks of the tongue’s size, color, and consistency, can help prevent or limit the occurrence of tongue necrosis. 17 It is important to be aware of this potential complication in patients requiring prolonged oral intubation, and if tongue edema is detected, attempts should be made to reposition the ETT or other transoral devices. 18 These simple measures may prevent the progression of tissue necrosis, thereby avoiding potential morbidity and mortality. In addition, the amount of vasopressor agents should be reduced to the lowest recommended dosage once a necrosis is suspected. 19 Ultimately, the correlation between extensive tongue necrosis and other extensive comorbidities, resulting in end-organ damage, may highlight a poor overall prognosis and a high mortality.
Conclusion
Tongue necrosis can result in severe functional deficits. It is important to be aware of the risk factors and symptoms of tongue necrosis, especially in patients requiring prolonged oral intubation or other procedures that increase intraoral pressure. Regular monitoring and repositioning of the ETT or other transoral devices are mandatory in suspected cases. Surgical intervention may be necessary. By making prompt diagnosis and taking appropriate preventive measures, healthcare professionals can help reduce the risk of tongue necrosis and prevent further tissue damage with improvement in associated morbidity, mortality, and patient outcomes.
Footnotes
Acknowledgements
The authors are grateful for their colleges in Al-Mouwasat Hospital in the ENT-HNS department.
Data Availability statements
The data that support the findings of this study are available from the author or corresponding author upon reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Our institution does not require ethical approval for reporting individual cases. Written informed consent was obtained from the patient for publication of this article.
