Abstract
Keywords
Introduction
Arytenoid cartilage dislocation is considered a rare laryngeal injury and can occur following blunt trauma or intubation trauma from procedures such as endotracheal or gastric intubation. Intubation trauma is the most common cause of arytenoid dislocation. 1 Several methods have been used to treat arytenoid dislocation, including closed reduction using direct or indirect laryngoscopy under general anesthesia or local anesthesia, speech therapy, or the injection of botulinum toxin. 2 Closed reduction is commonly used as the first choice for the arytenoid dislocation. 3 Rubin et al. 4 used a special laryngoscope to perform reduction. In their procedure, anterior dislocation was reduced using a Hollinger laryngoscope and posterior dislocation using a Miller-3 laryngoscope placed into the ipsilateral pyriform sinus. However, some prefer to perform the reduction with laryngeal forceps or a laryngeal applicator. 1 Since the tools of closed reduction vary, and there is no dedicated tool for closed reduction, the treatment outcome varies from person to person. Therefore, we designed a modified laryngeal forceps, which has been registered as a China National Invention Patent (No.: ZL201711258763.6, authors: Zhihong Lin, Yaoshu Teng), based on the 3-dimensional structure of the arytenoid cartilage. This study uses retrospective controlled trials to compare the treatment outcome of the modified laryngeal forceps and traditional laryngeal forceps.
Materials and Methods
Patients
This is a retrospective study approved by the Institutional Review Board of the Second Affiliated Hospital, School of Medicine, Zhejiang University. The strengthening the reporting of observational studies in epidemiology guidelines for retrospective studies guided this report. A total of 28 patients with arytenoid cartilage dislocation caused by endotracheal intubation were recruited from May 2021 to February 2023. They were divided into the traditional group (n = 14) and the modified group (n = 14) by gender (Figure 1). Initial diagnosis of arytenoid dislocation was performed using a combination of clinical history and laryngoscopy (Figure 2), which showed a bowed and shorter vocal fold in cases of anteromedial dislocation, and a straight and longer vocal fold in cases of posterolateral dislocation. All patients had clinical histories of a traumatic laryngeal event associated with persistent hoarseness immediately following tracheal or gastric intubation. Video stroboscopy demonstrated arytenoid positional displacement, normal mucosal wave, and the absence of the jostle sign (a sign of vocal fold paralysis characterized by arytenoid movement on the immobile site during phonation, caused by contraction of the mobile site). High-resolution computed tomography (CT) and cricoarytenoid joint 3-dimensional reconstruction were performed in all patients (Figure 3A and B).
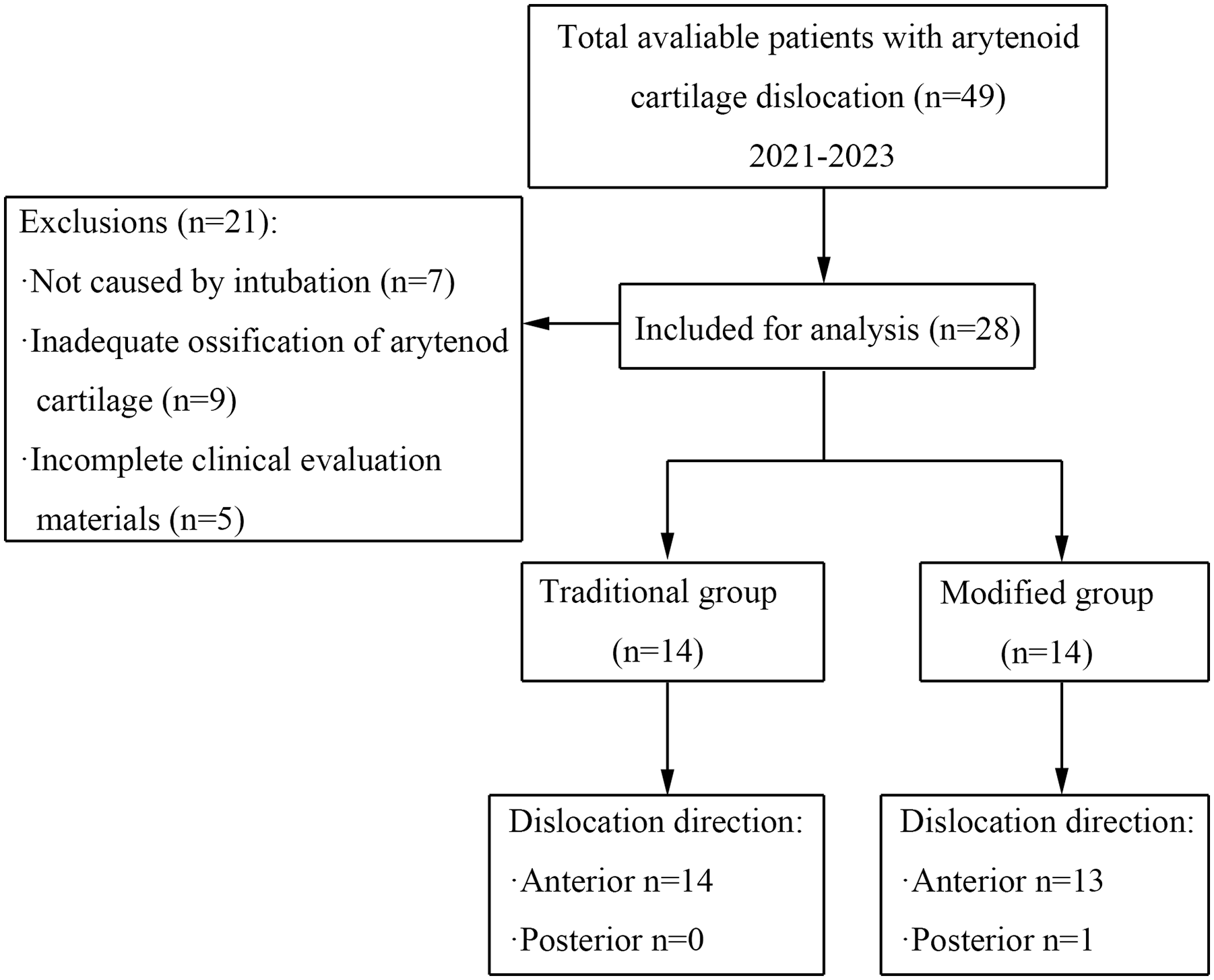
Strengthening the reporting of observational studies in epidemiology diagram.
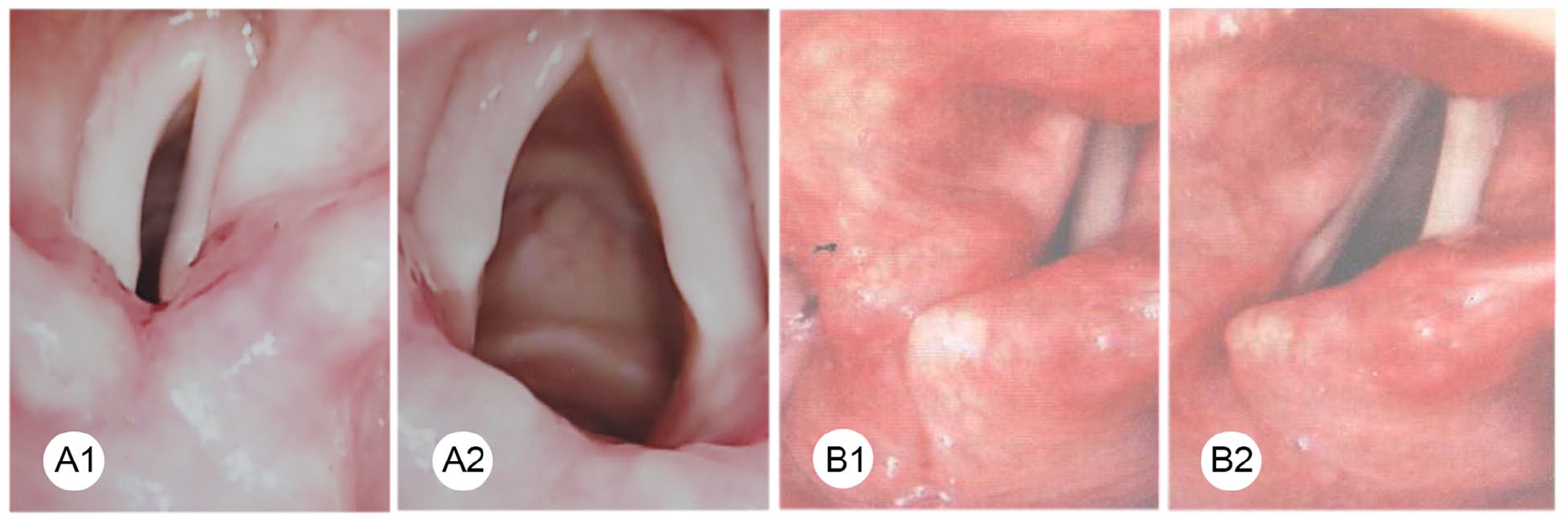
Left anteromedial dislocation, the affected side vocal cord was bowed and short during inspiration (A). Left posterolateral dislocation, the affected side vocal cord was straight and longer during inspiration (B).
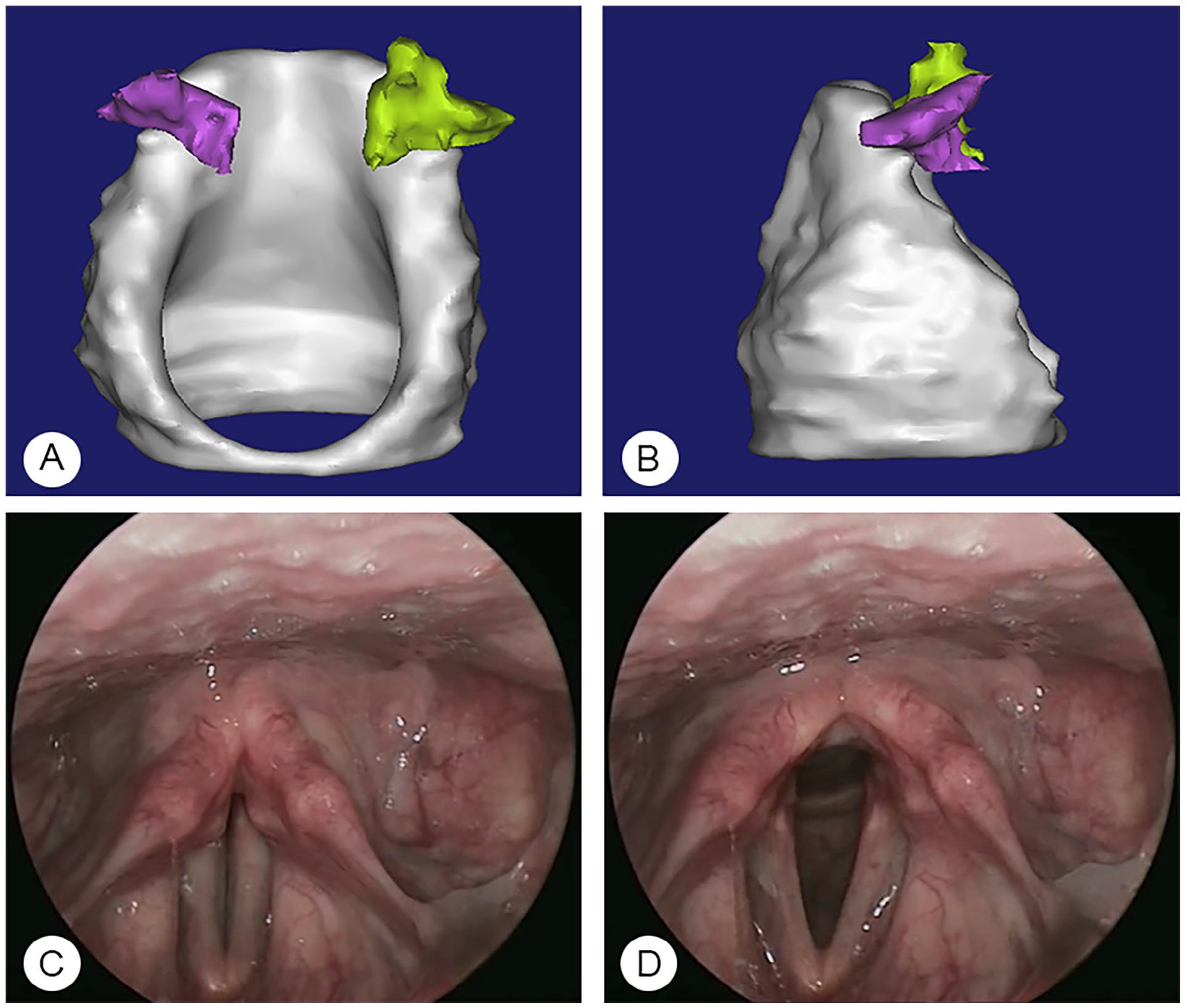
The high-fidelity 3-dimensional image of the arytenoid cartilage (A, B). Improved mobility of the vocal cord after the treatment (C, D).
Clinical Evaluation
Patients underwent a complete head and neck examination. Vocal function data, including voice handicap index (VHI) and maximum phonation time (MPT), were collected prior to closed reduction and 1 week after the last closed reduction. VHI is a self-assessment method for voice disorders and is divided into 3 subgroups used to score the physical (P), emotional (E), and functional (F) aspects of the voice. MPT was recorded when the patient produced a sustained /a/ vowel. Additionally, patient self-satisfaction evaluations were also recorded to assess the treatment outcome of closed reduction.
Operative Technique
Fourteen patients were treated by closed reduction under local anesthesia using traditional laryngeal forceps, and 14 patients were treated by closed reduction using modified laryngeal forceps. Anterior dislocations were reduced with posterior-upward force applied to the arytenoids and posterior dislocations with anterior-upward force (Figure 4). Each procedure was performed no more than 3 times. After each closed reduction manipulation, patients were encouraged to speak as much as they were able to and perform a strong laryngeal contraction similar to clearing the throat while holding and shaking the laryngeal body. There were no major complications resulting from closed reduction using indirect laryngoscopy. All patients tolerated the procedure well.
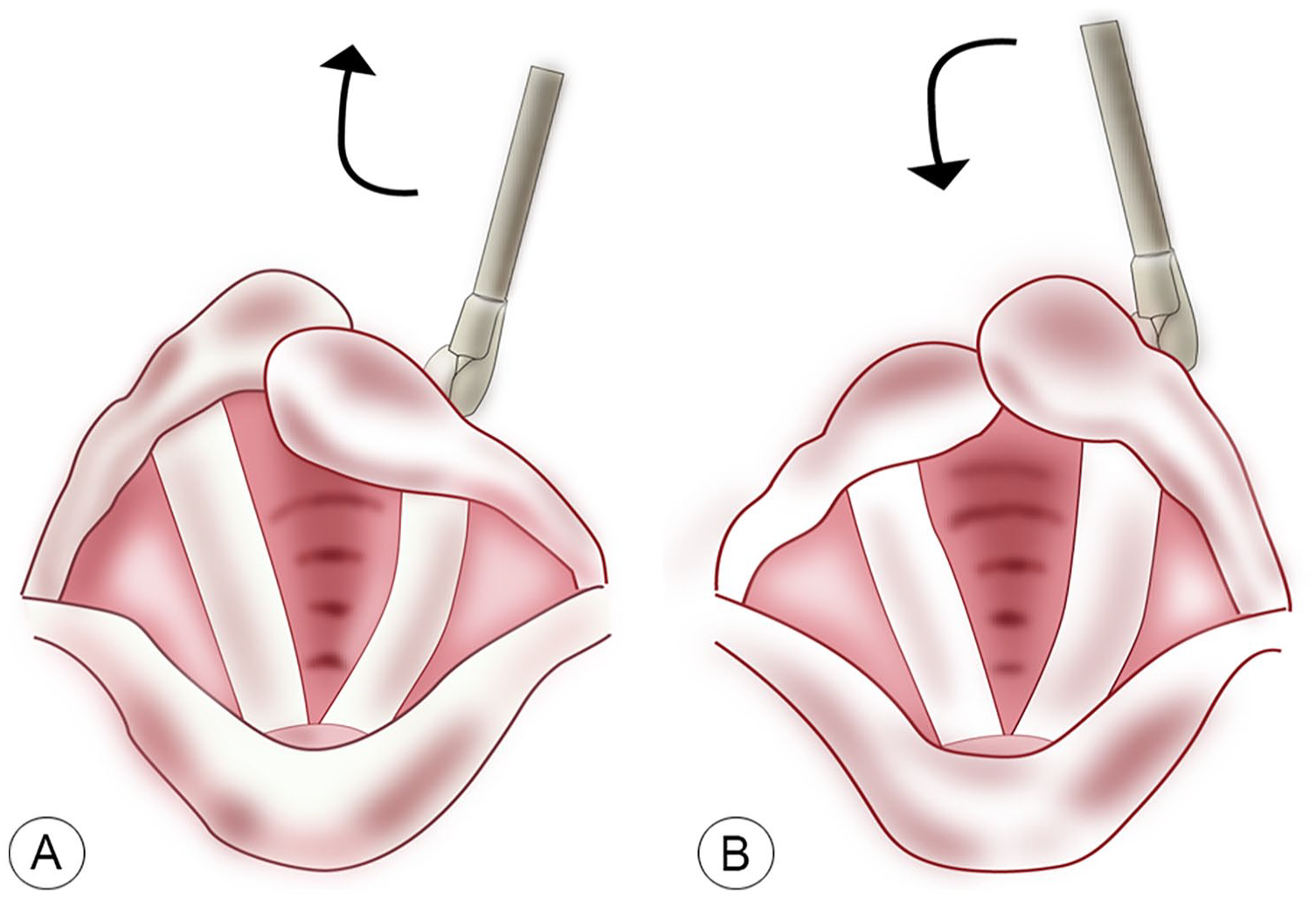
The diagram of closed reduction using modified laryngeal forceps. Anterior dislocations were reduced with posterior-upward force on the arytenoids (A). Posterior dislocations were reduced with anterior-upward force (B).
Statistical Analysis
Data are presented as mean ± standard deviation. The means were compared using paired t-tests, Wilcoxon match-pair signed-ranks tests, or Mann–Whitney U-tests. Statistical significance was indicated by P < .05. All analyses were performed using SPSS 21.0 statistical software (SPSS Inc., Chicago, IL).
Results
Among the 28 patients included in the study, 18 of them were male (64.3%) and 10 were female (35.7%). The clinical features of all patients are summarized in Table 1. They were divided into the traditional group (n = 14) and the modified group (n = 14) by gender. The ages of the groups were 49.71 ± 11.79 years and 53.79 ± 14.91 years for traditional and modified, respectively, with no statistically significant difference between them (P > .05). There were 27 anteromedial dislocations (96.4%) and 1 posterolateral dislocation (3.6%). The incidence difference between the anteromedial dislocation and posterolateral dislocation was statistically significant (P < .05), but there was no significant difference between the traditional group and the modified group. There were 7 patients with left-sided dislocations (50.0%) and 7 with right-sided dislocations (50.0%) in the traditional group, 8 patients with left-sided dislocations (57.1%) and 6 with right-sided dislocations (42.9%) in the modified group, indicating no statistically significant difference between the 2 in the incidence of left versus right dislocation (P > .05). To evaluate the treatment outcome of closed reduction, patient self-satisfaction evaluations were also recorded. In the traditional group, 13 patients reported satisfied outcomes and only 1 patient felt dissatisfied. In the modified group, 12 patients reported satisfied outcomes and 2 patients felt dissatisfied. There was no significant difference in the treatment effects between the traditional group and the modified group (Table 2). However, we found the median time interval between closed reduction and the return of normal voice in the traditional group was 31.08 ± 10.56 days, which was significantly longer than the median time of 17.92 ± 3.83 days in the modified group (P < .05).
Clinical Features of All Patients in the Study.
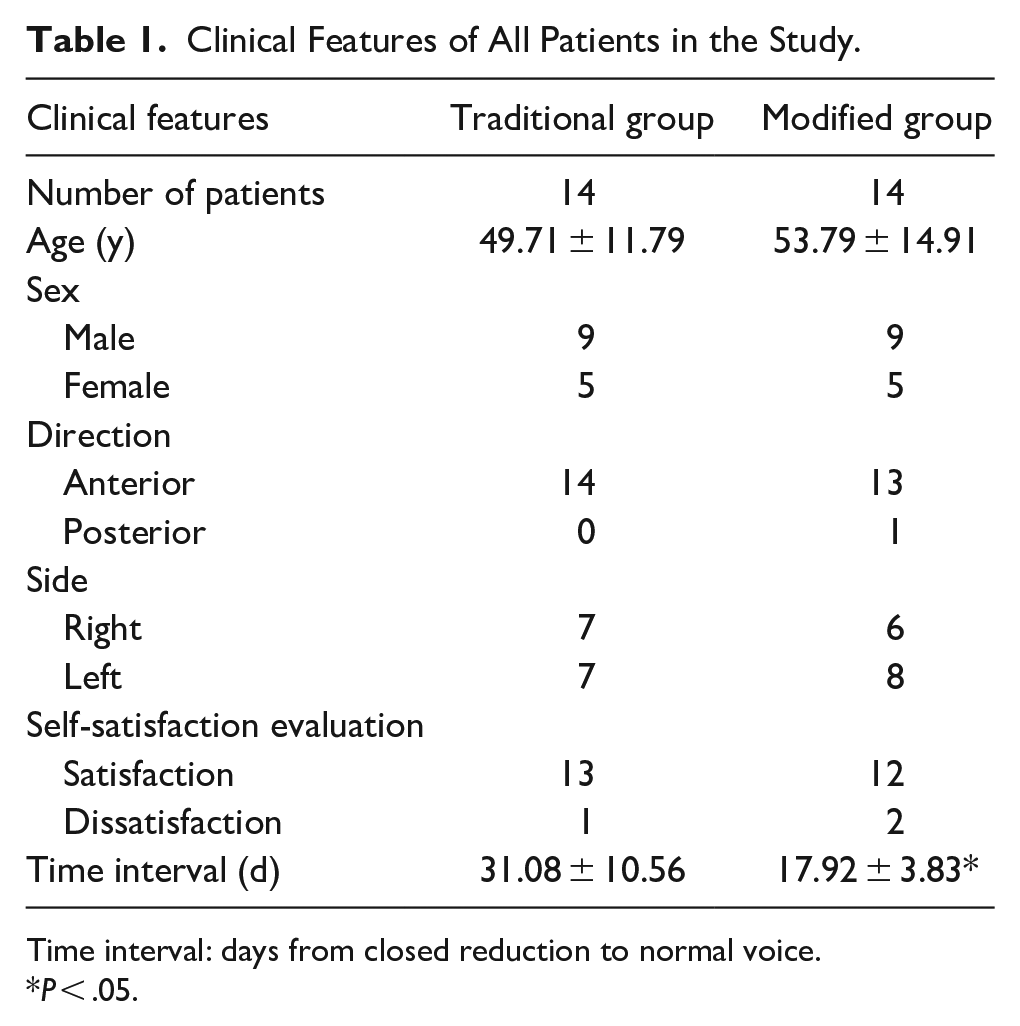
Time interval: days from closed reduction to normal voice.
P < .05.
The VHI Scores and MPT at the Different Time Points for Each Group.
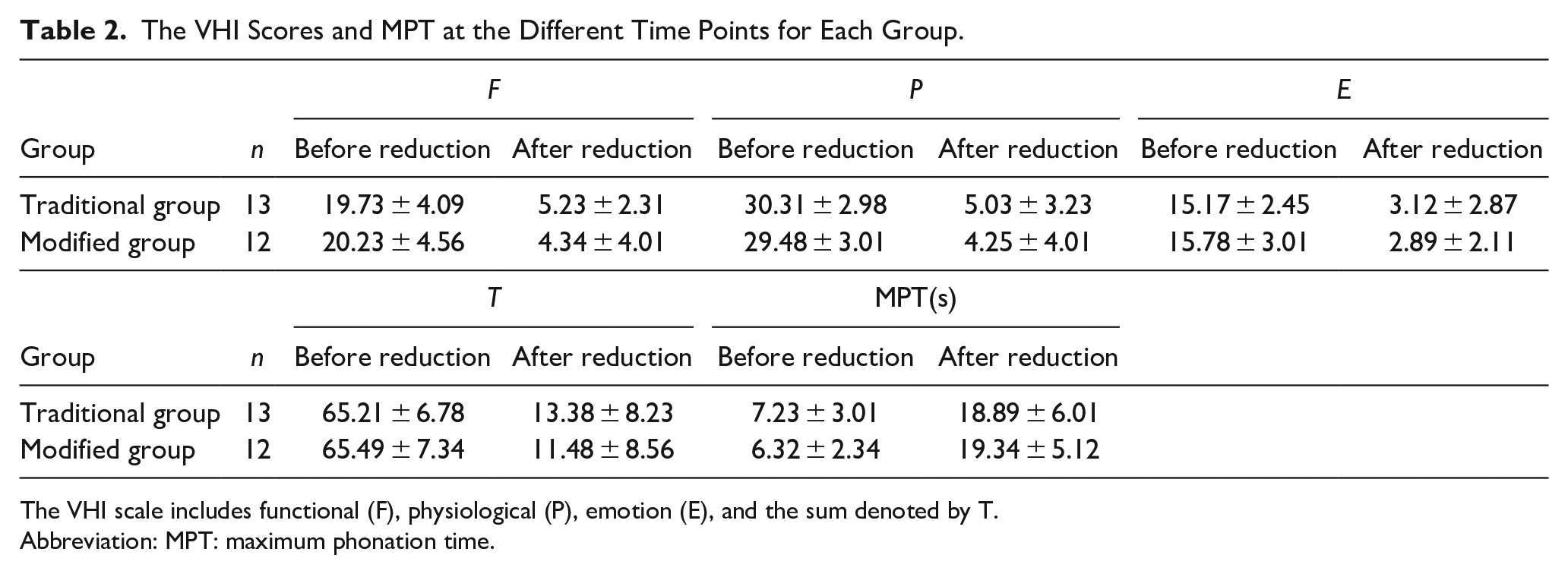
The VHI scale includes functional (F), physiological (P), emotion (E), and the sum denoted by T.
Abbreviation: MPT: maximum phonation time.
Discussion
Arytenoid dislocation was first reported in 1973 and is a rare clinical entity. 5 Diagnosis for arytenoids dislocation is usually made following a thorough check of patient medical history, especially those involving recent intubation and physical examination. 6 The diagnosis in this study was based on medical history, laryngeal endoscopy, voice analysis, high-resolution CT examination, and the cricoarytenoid joint 3-dimensional reconstruction. As we have previously reported,7,8 the cricoarytenoid joint 3-dimensional reconstruction is a new approach that can diagnose vocal cord paralysis and arytenoid dislocation more directly. Some researchers have used laryngeal electromyography (LEMG); 9 however, LEMG has its limitations. Rubin et al. 4 found that 39.7% of their patients with arytenoid cartilage dislocation displayed abnormalities on LEMG. This is possibly due to the co-occurrence of denervation and a joint dislocation, nerve susceptibility to inflammatory mediators infiltrating after trauma, or hematoma and scarring in the posterior portion of the thyroarytenoid muscle. These cases can lead to the appearance of denervation on LEMG. Furthermore, LEMG requires special equipment, training, and considerable experience. For this reason, it is still not commonly used in many clinics and hospitals in China, including our hospital.
Among various types of procedures available for the treatment of arytenoid dislocation, 10 closed reduction is one of the most commonly used. 3 At present, there are multiple reports about the choice of reduction tools. Rubin et al. 4 used the laryngoscope to perform reduction. In their procedure, anterior dislocation was reduced using a Hollinger laryngoscope and posterior dislocation using a Miller-3 laryngoscope placed into the ipsilateral pyriform sinus. However, this method requires special equipment, making it difficult to be widely applied. In 1966, Wang et al. 11 first performed closed reduction to arytenoid dislocation using laryngeal applicator with indirect laryngoscopy. In 1984, Yu et al. 12 reported 102 cases of vocal cord movement disorder treated by closed reduction in which only 22 cases recovered to normal voice with unsatisfactory treatment effect. Currently, the most common tools for closed reduction are laryngeal forceps and laryngeal applicator in China. In both cases there is poor operation stability, making it difficult to fix and control the reduction direction. Furthermore, the arytenoid cartilage is so small and irregular, limiting the surface area for which to apply force. This will ultimately affect the success rate of closed reduction. We used cricoarytenoid joint 3-dimensional reconstruction technology to reconstruct high-fidelity 3-dimensional images of the arytenoid cartilage successfully (Figure 3A and B). On the basis of this 3-dimensional imaging, the head of the laryngeal forceps were designed according to the lateral aspect of the arytenoid cartilage (Figure 5). Compared with the traditional laryngeal forceps or laryngeal applicators, the modified laryngeal forceps have a groove fit to the arytenoid cartilage, which greatly improves the consistency and stability of the distal contact surface between the arytenoid cartilage and the forceps. Additionally, the head of the modified laryngeal forceps can be rotated which corrects the limitation of unidirectional force present in traditional laryngeal forceps and allows for application with both anterior and posterior dislocations. In this study, 28 patients with a history of postoperative arytenoid dislocation were reviewed; 12 of the 14 patients treated by modified laryngeal forceps regained normal voice and vocal fold shape (Figure 3C and D). We found that using modified laryngeal forceps is an effective procedure and can shorten the treatment duration.
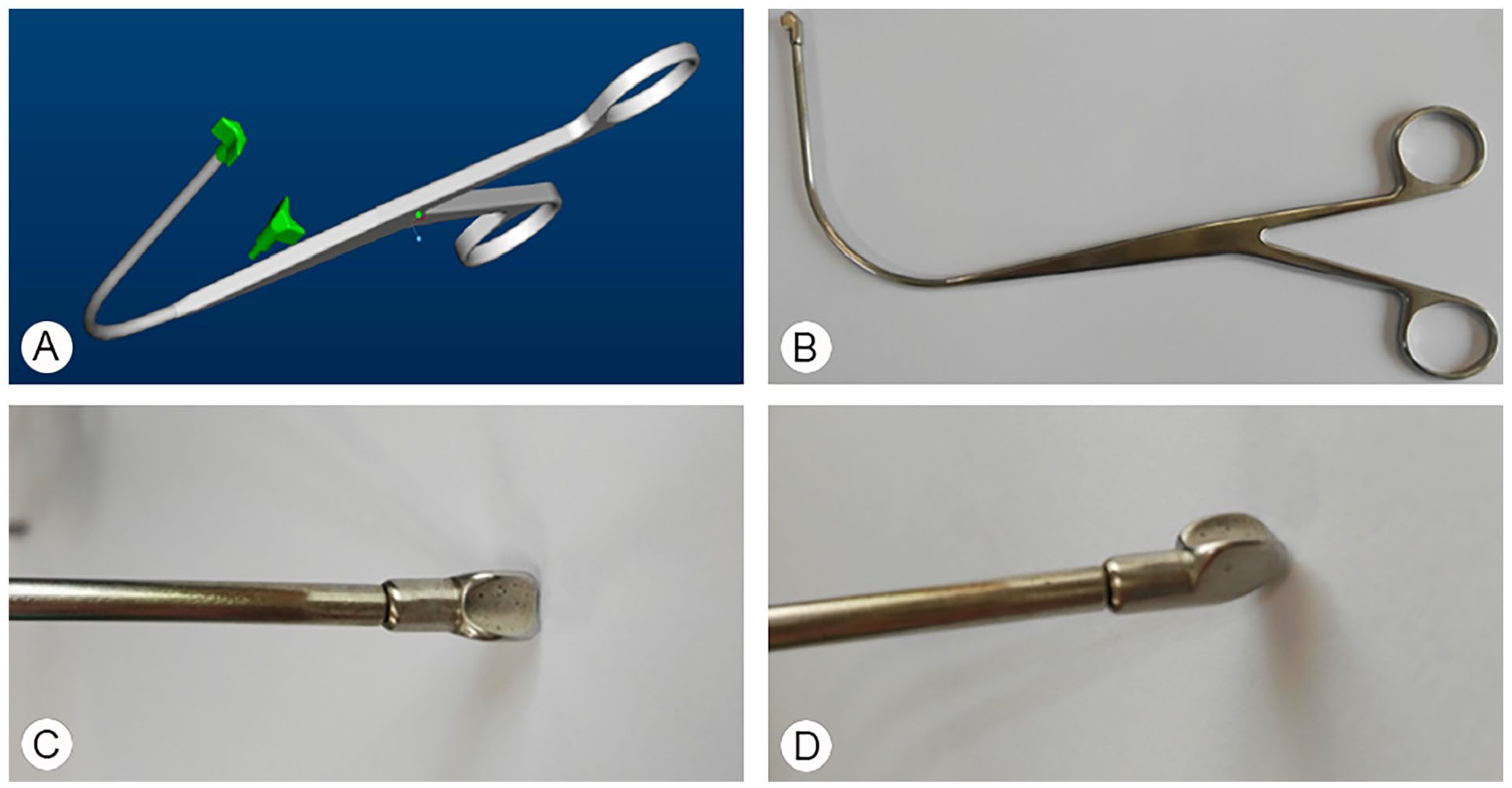
Based on the high-fidelity 3-dimensional image of the arytenoid cartilage, the head end of the laryngeal forceps was designed (A). The overall view of modified laryngeal forceps (B). The frontal view of modified laryngeal forceps (C). The right-sided view of modified laryngeal forceps (D).
When to perform closed reduction to achieve the best treatment outcome is still controversial. Several studies have suggested that 24 to 48 hours after arytenoid dislocation is the appropriate time, as waiting too long may lead to fibrosis on the surface of the traumatic arytenoid cartilage. This causes a certain extent of stiffness of the joint, affecting the overall efficacy of closed reduction. 13 Sataloff et al. 3 have reported that closed reduction 10 weeks after arytenoid dislocation still provides a stable and effective treatment outcome. It has also been reported that performing closed reduction 1 year after dislocation is still valid. 14 However, in the study we have reported previously, 8 we state that 2 to 4 weeks as an appropriate time window to perform closed reduction. In this study, we performed reduction during this time window, and the majority of patients showed positive treatment outcomes.
Of course, there are some limitations in this study. First, the sample size was small. In this study, we reviewed only 28 patients with arytenoid cartilage dislocation, which may be caused by the decrease in the incidence of dislocation due to the improvement of intubation techniques in recent years. In the future, high-quality and large-sample clinical studies are needed. Furthermore, the diagnosis in this study was based on the history, laryngeal endoscopy, voice analysis, high-resolution CT examination, and the cricoarytenoid joint 3-dimensional reconstruction. The cricoarytenoid joint 3-dimensional reconstruction as a new approach can diagnose vocal cord paralysis and arytenoid dislocation more directly. However, the cricoarytenoid joint 3-dimensional reconstruction also has its limitations; that the quality of the reconstruction is insufficient for diagnosis in the patient with an inadequate ossification of arytenoid cartilage. Despite these limitations, we will continue our further research in this field.
Conclusion
Based on the treatment outcomes from 28 patients with arytenoid dislocation, we have confirmed that closed reduction with the modified laryngeal forceps under local anesthesia is an effective and safe procedure. Compared with traditional laryngeal forceps, it can shorten the treatment duration.
Footnotes
Acknowledgements
The authors thank all of the members of Department of Otorhinolaryngology—Head and Neck Surgery, the Second Affiliated Hospital, School of Medicine, Zhejiang University, for their invaluable help.
Data Availability Statement
The authors declare that all data supporting the findings of this study are available within the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Statement
This is a retrospective study approved by the Institutional Review Board (IRB) of the Second Affiliated Hospital, School of Medicine, Zhejiang University (IRB number: IR2019001254).
Statement of Informed Consent
Written informed consent was obtained from the subjects for their anonymized information to be published in this article.
