Abstract
Keywords
Introduction
Chronic cough refers to cough lasting for more than 8 weeks in adults. 1 It is very common in humans, with a prevalence rate of 2% to 18%. 2 The morbidity in China is 7.67%. 3 The etiology of chronic cough is complex and multicausal. The most frequent reasons in turn are upper airway cough syndrome (UACS), asthma, gastroesophageal reflux disease (GERD), nonasthmatic eosinophilic bronchitis, and combinations of these 4 conditions. 1 In China, the sequence is cough variant asthma (CVA), UACS, eosinophilic bronchitis, atopic cough, and GERD. 4 Therefore, GERD is one of the common causes of chronic cough. 1 Chronic cough induced by GERD is named gastroesophageal reflux cough, chronic cough due to gastroesophageal reflux disease, gastroesophageal reflux-induced chronic cough, reflux-cough syndrome, chronic cough associated with gastroesophageal reflux, gastroesophageal reflux-related chronic cough, and reflux-induced chronic cough in the literatures. Chronic cough is one of the extraesophageal symptoms of GERD. 5
GERD is a symptom and complication resulting from the reflux of gastric contents into the esophagus or beyond, into the oral cavity (including larynx) or lung. 5 GERD results in esophageal and extraesophageal symptoms. The phenomenon in which gastric contents backflow beyond the upper esophageal sphincter (UES) is defined as laryngopharyngeal reflux (LPR). 6 Symptoms and signs caused by LPR are called laryngopharyngeal reflux disease (LPRD).6,7 LPR and LPRD were defined in 2002 and quickly became a research focus in the otorhinolaryngopharyngeal field. There are few reports on whether patients with chronic cough induced by GERD have LPR and their LPR characteristics. In this article, we summarize the characteristics of LPR in 44 patients with chronic cough induced by GERD.
Materials and Methods
General Information
There were 44 patients who were referred from the Respiratory Department to the Otorhinolaryngology-Head and Neck Surgery Department at our hospital from October 2019 to January 2022. Their data were retrospectively summarized and analyzed. All patients conformed to the following requirements: (1) Their chief complaint was “cough for more than 8 weeks.” (2) They were all diagnosed with chronic cough induced by GERD, according to the recommendations of the CHEST Guideline and Expert Panel Report.8,9 (3) The patients denied cardiovascular disease history and use of angiotensin converting enzyme inhibitors. (4) The patients had not been exposed to irritative environments or tobacco. Exclusion criteria were as follows: (1) Patients with infection, allergy, throat wounds, throat surgery, spinal diseases, and radiation and acupuncture of the head and neck were excluded. (2) Patients with diseases of the lower respiratory tract were excluded. (3) Patients with rhinitis and rhinosinusitis were excluded.
In total, there were 21 (21/44, 47.7%) male and 23 (23/44, 52.3%) female patients. They were aged from 18 to 76 years, with an average age of 48.73 (48.73 ± 16.20) years. Their cough duration varied from 2 months to 10 years, with a mean duration of 29.6 (29.60 ± 37.60) months.
The symptoms of all patients were evaluated using the reflux symptom index (RSI). All patients were examined by a transnasal Rhino-laryngo Videoscope (OLYMPUS ENF TYPE VH) and had their reflux finding scores (RFSs) determined. Moreover, all of the patients underwent oropharyngeal pH monitoring (Dx-pH monitoring).
Consent was obtained from all of the above patients. The research was approved by the Ethics Committee of the China-Japan Friendship Hospital (2016-74).
Reflux symptom index and Reflux finding score
Recently, the RSI and RFS have become the most common scores used in clinical practice to evaluate the symptoms and signs of LPRD patients.10,11 In the present study, the same otorhinolaryngologist explained the meaning and method of RSI to all of the patients. After each patient understood the information completely, he or she scored his or her symptoms together with the otorhinolaryngologist. This score was the patient’s RSI. If the RSI was more than 13, it was abnormal. Otherwise, the score was considered normal.
Each patient was examined by the same laryngologist with an OLYMPUS ENF TYPE VH. Pictures of the throat were saved and analyzed by 2 senior laryngologists who were blinded to the patients’ information. These 2 laryngologists determined the RFS of each patient independently. The average of the RFSs determined by the 2 laryngologists for each patient was recorded as the patient’s RFS. If the RFS was more than 7, it was considered abnormal. Otherwise, it was normal.
If 1 patient had an abnormal RSI and/or abnormal RFS, he or she was diagnosed with suspect LPRD. Otherwise, the RSI and RFS of the patient were considered normal.7,10,11
Oropharyngeal pH Monitoring (Dx-pH Monitoring)
All patients underwent 24-hour oropharyngeal pH monitoring (Dx-pH monitoring) (Dx-pH monitor, Respiratory Technology Corporation, USA), as introduced in a previous article. 12 When the electrode detected an oropharyngeal pH lower than 5.5 (upright) and/or 5.0 (supine), the monitor recorded 1 LPR event. The decrease in oropharyngeal pH caused by drinking and eating was eliminated before data analysis. After 24-hour monitoring was completed, the monitor system summarized all the LPR events and calculated the final Ryan score. When the upright Ryan score was ≥9.41 and/or the supine Ryan score was ≥6.80, the score was considered abnormal and suggested severe acid reflux.
Then, the baseline of the monitor was changed to 6.5, and oropharyngeal pH values lower than 6.5 were calculated (the decrease in oropharyngeal pH caused by drinking and eating was eliminated).
Treatment
All patients were prescribed proton pump inhibitors (PPIs) (esomeprazole or rabeprazole, standard dose, bid) orally for 8 to 12 weeks after RSI, RFS, and Dx-pH monitoring.
Statistics
SPSS 18.0 (IBM, Armonk, NY) was used to analyze the results of all patients. The t-test was used to compare the scores of cough symptoms and total RSI.
Results
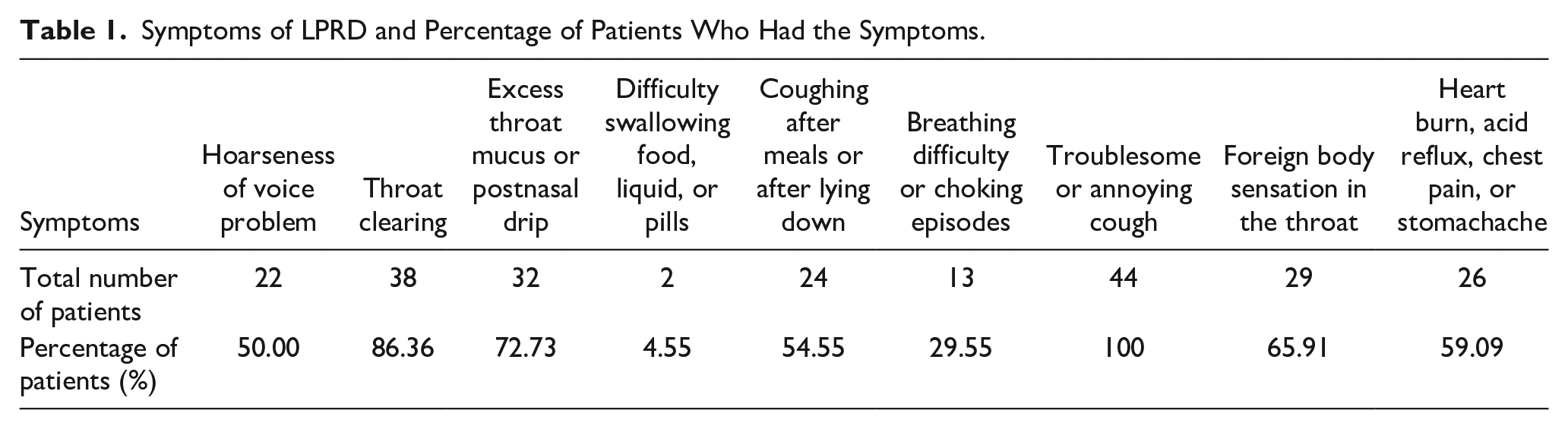
The RSIs of 44 patients were 4 to 27, with an average of 15.66 (15.66 ± 6.33). Among them, 25 patients (25/44, 56.82%) had abnormal RSIs. For the 9 symptoms listed in the RSI, all patients had at least 2 symptoms in addition to cough, which was the common symptom of all 44 patients. The percentage of patients with each symptom was listed in Table 1. According to the percentages, the symptoms in sequence were cough, throat clearing, excess throat mucus or postnasal drip, foreign body sensation of throat, heartburn/stomach acid coming up/chest pain/stomachache, cough after meals or after lying down, hoarseness, breathing difficulty, and swallowing difficulty. In total, 24 patients (24/44, 54.55%) had heartburn or stomach acid reflux, and 2 patients (2/44, 4.55%) had chest pain or stomachache.
Symptoms of LPRD and Percentage of Patients Who Had the Symptoms.
All patients had LPRD signs when they were examined with the Rhino-laryngo Videoscope. Their RFSs ranged from 5.5 to 17, with an average of 10.89 (10.89 ± 2.81). There were 38 patients (38/44, 86.36%) whose RFSs were abnormal. According to the percentage of patients of each sign, the signs in turn were erythema/hyperemia/vocal fold edema, posterior commissure hypertrophy, diffuse laryngeal edema, subglottic edema, ventricular obliteration, thick endolaryngeal mucus, and granuloma (Table 2). In total, there were 42 patients (42/44, 95.45%) who had abnormal RSI and/or RFS.
LPRD Signs and Percentage of Patients With Each Sign.

Oropharyngeal pH monitoring found that 10 patients (10/44, 22.72%) had abnormal Ryan scores. Among them, 8 patients (8/10, 80%) had abnormal upright Ryan scores, ranging from 11.12 to 306.64 (140.00 ± 114.96). Their number of reflux episodes was 2 to 48 (18.75 ± 19.01), for a total of 150. Their percentage of time below baseline was 0.14% to 9.69% (4.25% ± 4.17%). There were 4 patients (4/10, 40%) who had abnormal supine Ryan scores, ranging from 8.56 to 15.86 (11.25 ± 3.59). Their number of reflux episodes was 1 to 17 (7.00 ± 6.93), which was 28 in total. Their percentage of time below baseline was 4.01% to 15.48% (7.25% ± 5.25%). When the baseline of the oropharyngeal pH monitor was changed to 6.5, there were 38 patients who had more than 3 reflux episodes. Their upright reflux episodes were 0 to 850 (207.56 ± 192.64) in number, for a total of 8510. Their supine reflux episodes were 0~537 (83.26 ± 101.32) in number, for a total of 3247.
For patients with abnormal Ryan scores, their RSI were 16.30 ± 6.48, which was not significantly different from that of patients with normal Ryan score (15.47 ± 6.37, P = 0.720), nor were their RFS (9.60 ± 2.37, 11.26 ± 2.84, P = 0.100).
Among these 44 patients, only 6 patients had gastroscopy reports. There were 3 patients with superficial gastritis, 2 with non-atrophic gastritis, 1 with atrophic gastritis. Two of them had reflux esophagitis.
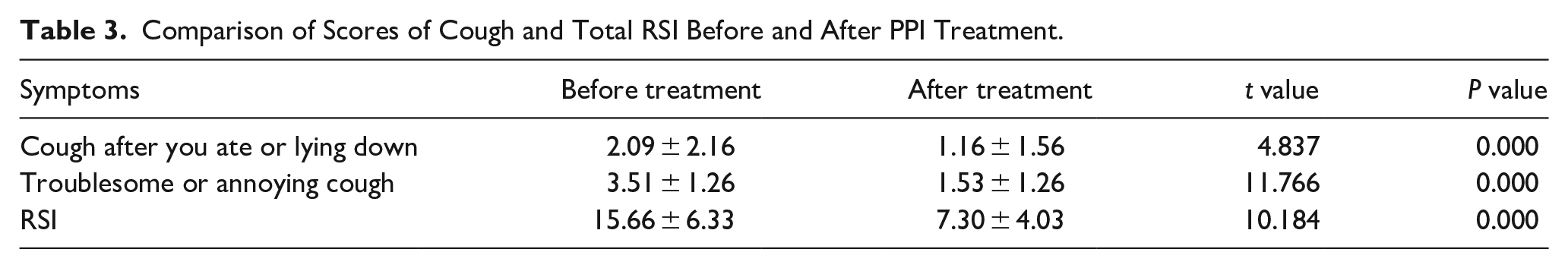
After PPI treatment, the chronic cough of most patients was relieved (only 3 patients had no obvious change in their cough), as were their LPRD symptoms (RSI of 3 patients had no change, while 1 patient had RSI increased). Their changes were listed in Table 3 (evaluation of chronic cough used the scores of the 5th and 7th items of the RSI).
Comparison of Scores of Cough and Total RSI Before and After PPI Treatment.
Discussion
The etiology of chronic cough is complex. GERD is the most frequent etiology in addition to respiratory diseases.1,4 Chronic cough induced by GERD has been identified in 4.6% of cases in China. 4 In this article, we summarized the characteristics of LPR in patients with chronic cough due to GERD only.
First, we evaluated the characteristics of the symptoms. In this study, cough was not the only symptom of patients with chronic cough induced by GERD. They all had other LPRD symptoms, most frequently throat clearing (86.3%) and excess throat mucus/postnasal drip (72.7%). There were 56.82% patients whose RSIs were abnormal, which indicated that more than half of patients with chronic cough caused by GERD had LPRD symptoms and could be diagnosed with suspect LPRD. More than half of the patients had symptoms of GERD simultaneously, which included acid reflux, heartburn, chest pain, stomachache, and others. Chronic cough caused by GERD has been considered an extraesophageal symptom of GERD for a long time.5,13 With further knowledge of LPR and LPRD, “extraesophageal symptoms of GERD,” “extraesophageal reflux,” and “supraesophageal reflux” are now considered LPRD. 6 According to the definition of GERD and LPRD, such chronic cough is not only one of the extraesophageal symptoms of GERD, 13 but also one symptom of LPR. 6 This indicates that for patients with chronic cough, doctors should pay attention to the symptoms and case history of GERD and LPRD, in addition to respiratory tract factors, to reduce misdiagnosis and missed diagnosis.
Second, we identified characteristics of the signs. Laryngoscopy revealed edema, hyperemia, hypertrophy, and other inflammatory features of the laryngeal mucosa to various degrees. Most patients (86.36%) had abnormal RFSs and reached the criterion for diagnosing suspect LPRD.7,11 Considering the RSI and RFS, 95.45% of patients could be diagnosed with suspect LPRD. This indicated that laryngoscopy should be performed routinely in chronic cough patients to evaluate the condition of the pharynx and larynx, especially for patients without GERD symptoms.
Third, we analyzed the results of pH monitoring. Dx-pH monitoring found only a small proportion of patients (22.72%) with abnormal Ryan scores, which indicated that they had more severe acid reflux. Most acid reflux events occurred in the upright position, which is in accordance with the characteristics of LPR. However, Ryan scores only calculated pH events below upright 5.5/supine 5.0,12,14 while the normal oropharyngeal pH is 7.03. 15 Therefore, some reflux events with pH above upright 5.5/supine 5.0 may have been omitted. This may be one of the reasons why neither the RSIs nor the RFSs of patients with abnormal Ryan scores were significantly different from those of patients with normal Ryan scores. In this study, the baseline of the pH monitor was changed to 6.5, and pH events below 6.5 were calculated. We found that 86.36% of patients had more than 3 oropharyngeal pH events below 6.5, most of which occurred in the upright position. Transient pH decreases were mainly caused by reflux events, except for salivary secretion, bacteria, eating, and drinking. 14 The results supported that most patients in this study had an obvious weak acid reflux, which was in accordance with the results of Herregods. 16 Herregods found that more important factors for patients with chronic cough due to GERD were the volume of refluxate, the proximal extent of reach of the refluxate, and the duration of reflux episodes, not the acidity of the reflux. This may be related to the pathogenesis of chronic cough caused by GERD, which will be discussed in the following paragraph.
Fourth, we considered the relationship between the mechanism of chronic cough caused by GERD and LPR. The pathophysiology of chronic cough caused by GERD has not been clarified until now. In addition to high reactivity and poor defense function of the respiratory tract, a decrease in the pressure of the esophageal sphincter, and insufficient esophageal motility,17-20 there are 2 theories: (1) Reflex theory. This means that reflux causes cough through the esophagus–trachea reflex mediated by the vagus nerve.8,21 This can be supported by cough caused by acid instillation into the distal esophagus.22,23 (2) Reflux theory. In this theory, cough is caused by direct stimulation of the upper respiratory tract by the refluxate or stimulation of the lower respiratory tract by microaspiration or macroaspiration.8,21 This can be supported by more lipid-laden macrophages in bronchoalveolar lavage. 24 However, some studies have noted that the function of this mechanism is limited.25,26 Chronic cough due to GERD may mainly be caused by the reflex theory. However, Li’s research indicated that proximal acid reflux (reflux theory) and distal reflux-reflex (reflex theory) may act in coordination in chronic cough due to GERD, in which the latter may play a greater role. 27 In addition, Li also found that cough caused by GERD can cause reflux conversely to form a vicious cycle of reflux-cough-reflux. 27 This in turn aggravates cough and reflux, resulting in intractable cough.
The mechanism of chronic cough induced by GERD is almost the same as that of LPRD,28-30 which may be related to the definition of GERD and LPRD.5,6 GERD is a disease comprising symptoms, end-organ effects, and complications related to the reflux of gastric contents into the esophagus, oral cavity, and/or the lung. 5 LPRD involves a series of symptoms and signs caused by backflow of gastric contents above the UES. 6 According to the definitions, LPRD is GERD that occurs above the UES. Cough can not only be an extraesophageal or supraesophageal symptom of GERD but also be a symptom of LPRD, which depends on the height of the gastric refluxate. When gastric reflux reaches beyond the UES, chronic cough is both an extraesophageal (supraesophageal) symptom of GERD and a symptom of LPRD. Otherwise, chronic cough is only an extraesophageal (supraesophageal) symptom of GERD. In the former condition, chronic cough may be caused by coordination of the reflex theory and the reflux theory. In the latter condition, chronic cough may only be caused by the reflex theory. In this study, as most patients (95.45%) had abnormal RSI and/or RFS and LPR events, chronic cough in these patients was a symptom of both LPRD and GERD and may be resulted from both gastric content reflux and the reflux-reflex.
Although most patients in this study could have been diagnosed with LPRD according to their RSI, RFS, and Dx-pH monitoring results, there were still some patients whose RSI, RFS, and Dx-pH monitoring findings did not fit the profile of LPRD. The reasons may be as follows: (1) Some patients may have only distal GERD. Their gastric refluxate did not reach the level of UES. (2) Although gastric content reached the UES, the symptoms and signs may not be severe enough to result in an abnormal RSI, RFS, and Dx-pH monitoring. (3) The number of LPR events was less, or the oropharyngeal pH was not below 6.5, which could not be detected by Dx-pH monitoring. What is detected by Dx-pH monitoring is the change in oropharyngeal pH, not the LPR event itself. If the gastric refluxate contains pepsin, bile acid, or other nonacid substances, the oropharyngeal pH will not change much and will result in false negativity. (4) The RSI does not include all symptoms of LPRD, nor does the RFS. This may be another reason for false negativity. (5) The patient’s chronic cough may not be caused by GERD or LPRD. However, chronic cough cannot be excluded as a result of GERD, although there were no GERD symptoms or pathological gastroesophageal reflux, according to the CHEST Guideline and Expert Panel Report. 8 In the same way, chronic cough cannot be ruled out from LPRD symptoms, even if the RSI, RFS, and Ryan scores are in the normal range.
There are few reports regarding LPRD and chronic cough. Suzuki et al. described 2 LPRD patients who had gas reflux. 31 Their chronic cough was cured by antireflux surgery after invalid antireflux treatment. This suggests that gas reflux can cause chronic cough. The main refluxate of LPRD is gas.6,28-30 which can only slightly reduce the oropharyngeal pH. 31 This may be the reason why only a small portion of patients in this study had abnormal Ryan scores.
Certainly, there were some shortcomings of this study: (1) the size of the sample in this study was not large enough; (2) the indices evaluating LPRD in this study had limitations (the RSI and RFS only contain some of the symptoms and signs of LPRD, and the Ryan score only calculates reflux events of pH lower than upright 5.5/supine 5.0); and (3) chronic cough caused by GERD is an exclusive diagnosis without a gold standard.
Conclusion
Patients with chronic cough induced by GERD all had symptoms and signs of LPRD. Most of them had an abnormal RSI and/or RFS and could be diagnosed with suspect LPRD. Dx-pH monitoring revealed that most of them had abnormal reflux events, most of which were weak acid and occurred in upright position. These findings suggest that most patients with chronic cough induced by GERD have LPRD and that chronic cough is a common symptom of LPRD. LPR is an important reason for chronic cough induced by GERD, which cannot be ignored.
Footnotes
Data accessibility statement
The data of this research can be accessed through legal and optimal process.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
