Abstract

Significance Statement
Here, we report a rare case of verrucous carcinoma (VC) of the palatine tonsils with neck metastases that was treated with surgical excision combined with chemotherapy and radiotherapy. Neck metastases of tonsil VC occur very rarely. If neck metastases are present, as in our patient’s case, surgical treatment with chemotherapy or radiotherapy is expected to have a positive effect. Additionally, it is crucial to confirm the absence of recurrence through continuous follow-up.
VC is a histologically malignant but relatively benign variant of squamous cell carcinoma (SCC) that proliferates slowly. 1 While the etiology of VC remains unknown, smoking, alcohol consumption, and betel nut chewing have been suggested as potential contributors. 2 VC primarily occurs in the oral cavity, especially at locations such as the buccal mucosa, retromolar trigone, anterior tongue, mucosa of the lower lip, and mucosa of the upper lip; minor lesions also occur in the larynx. 3 However, VC rarely occurs in the palatine tonsil, and neck metastases are extremely rare. Although the treatment of VC is still controversial, surgery, radiotherapy, and chemotherapy are used. 4 We present a rare case of VC of the palatine tonsil with neck metastases treated with surgical excision combined with chemotherapy and radiotherapy.
A 71-year-old male with a 1-month history of a neck mass on the right side was referred to the Department of Otolaryngology. He had a 30-pack-year smoking history with moderate alcohol consumption. He did not complain of any discomfort except for a mild sore throat. A gun biopsy of the neck mass was performed, and a microscopic examination revealed metastatic SCC (Figure 3B). Endoscopic examination revealed a slightly papillomatous mucosal surface at the lower pole of the right palatine tonsil (Figure 1). Computed tomography (CT) and positron emission tomography (PET) were performed. The PET/CT and neck CT findings were suggestive of metastatic level II neck mass in the right neck and malignancy involving the right palatine tonsil (Figure 2). The tonsil mass was excised through complete resection of the palatine tonsil under general anesthesia. Microscopic diagnosis of the palatine tonsil mass confirmed a verrucous SCC (Figure 3A). He underwent a combination of chemotherapy (cisplatin) and radiotherapy (66 Gy) and is being regularly followed up without recurrence.
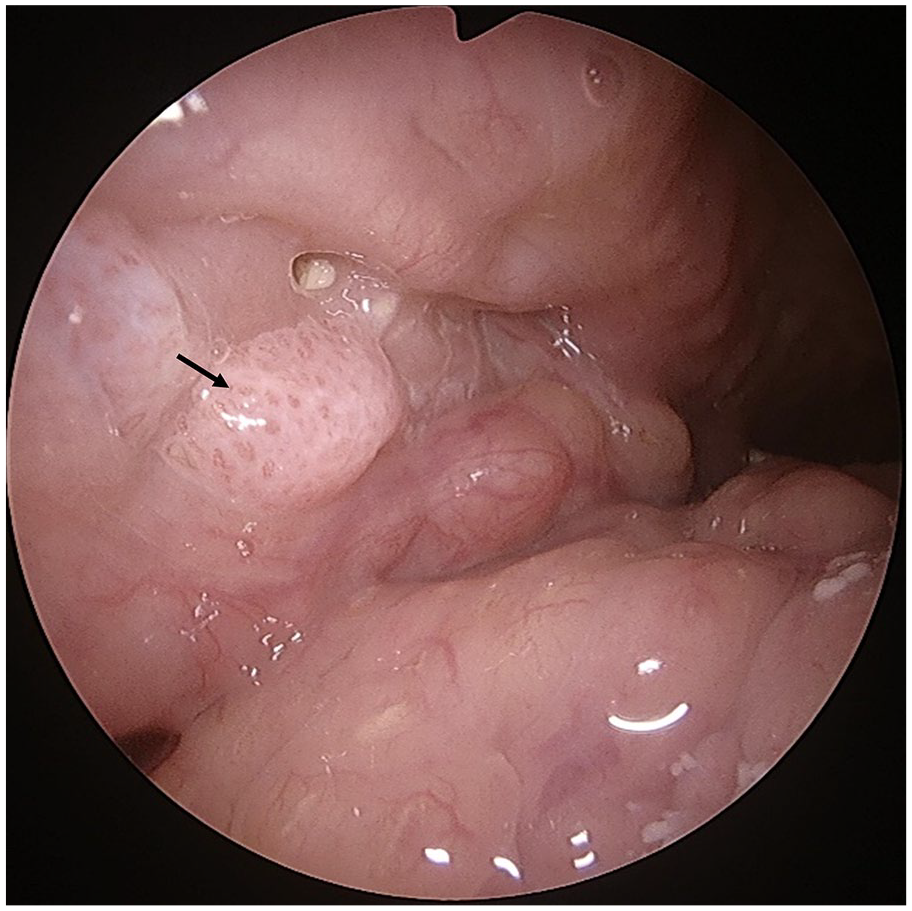
Endoscopic examination reveals a slightly papillomatous mucosal surface at the lower pole of the right side of the palatine tonsil (black arrow).
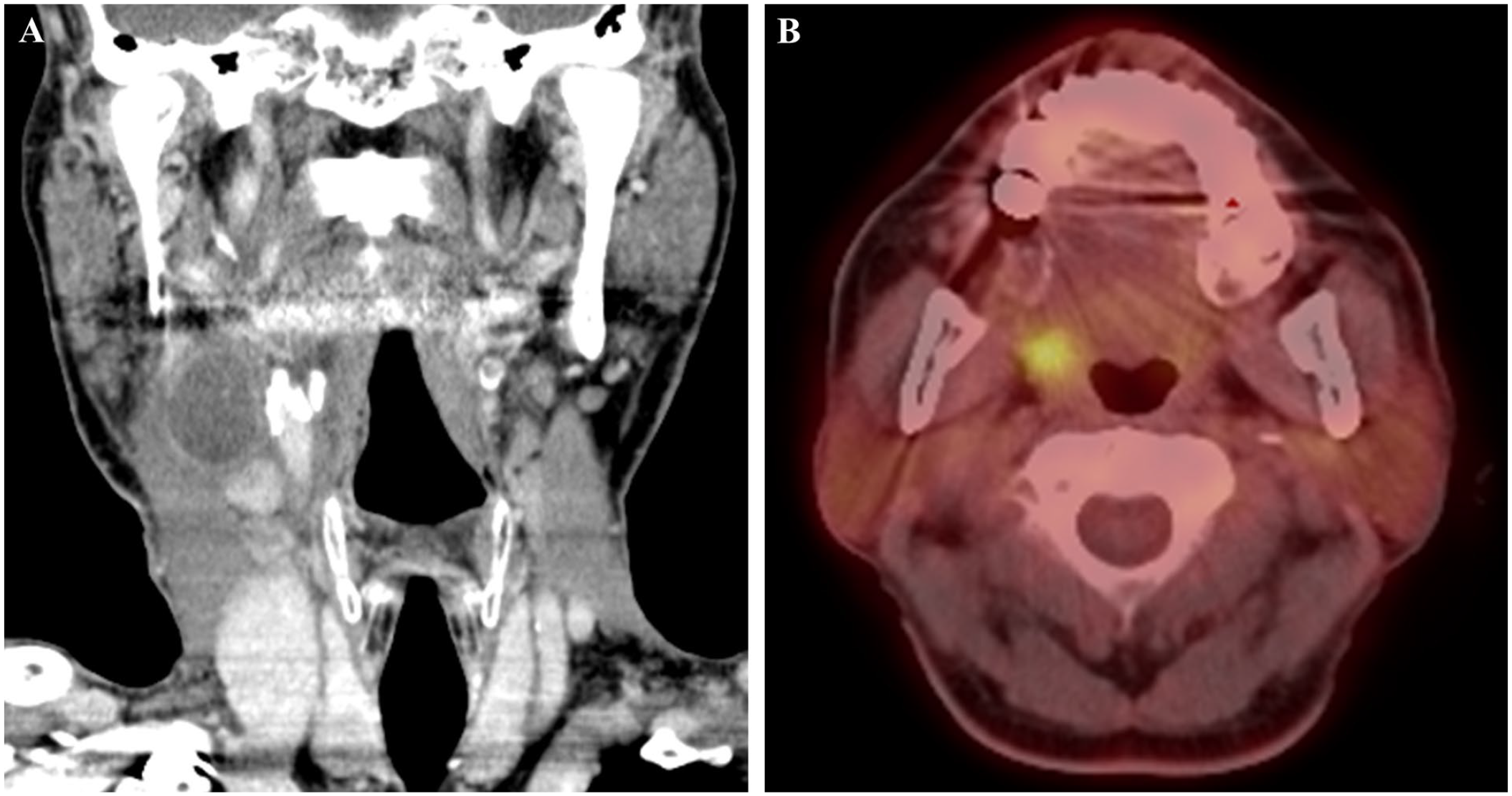
(A) CT scan showing multiple metastatic level II neck masses in the right neck. (B) PET/CT scan showing malignancy in the right palatine tonsil with a high FDG uptake.
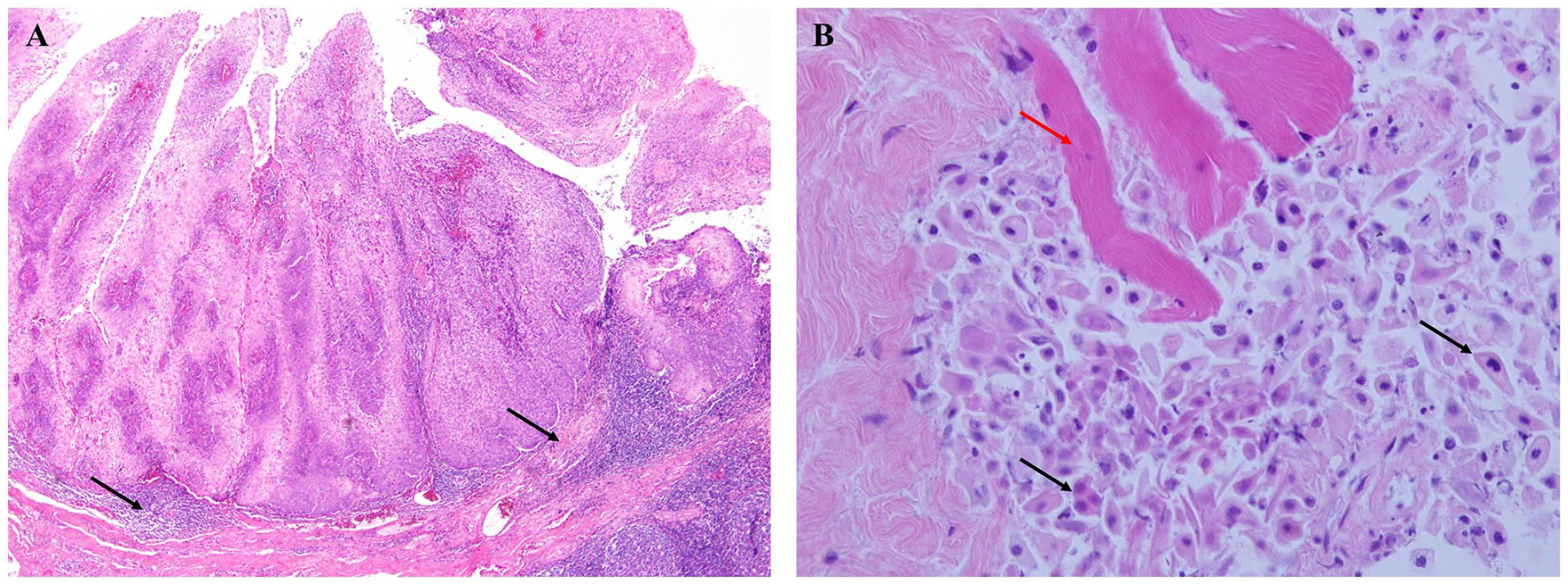
(A) Microscopic examination reveals superficial keratosis and a broad-pushing border of infiltration and dense inflammatory response (black arrow) with thickened rete ridges. The tumor has multiple filiform and finger-like projections of well-differentiated squamous epithelium that mature toward the surface (hematoxylin and eosin, original magnification ×40). (B) The neck mass shows atypical squamous cells (black arrow) infiltrating into fibromuscular tissues. Polygonal-shaped tumor cells show hyperchromatic and pleomorphic nuclei with abundant skeletal muscle bundles (red arrow) (hematoxylin and eosin, original magnification ×400).
The prevalence of VC is lower than that of total carcinoma in the oral cavity and oropharynx and is reported to be 2% to 12%. 5 The buccal mucosa is the most common site of occurrence reported by studies, and the lower lip, alveolar ridge, gingiva, and larynx are common specific locations. However, it is extremely rare for VC to occur in the palatine tonsil with lymph node involvement and distant metastases.1,6,7 VC proliferates slowly, often with long-term leukoplakia, and is accompanied by leukoplakia in approximately 13% of cases. 8 It is histologically malignant but relatively benign. Adjacent lymph node invasion by VC is rarely reported, with a prevalence of approximately 2% to 5% in Western countries.1,8
VC is a low-grade variant of SCC, with a rare presence of lymph nodes and distant metastases at any stage. 9 Additionally, accurate pathological evaluation is necessary for enlarged lymph nodes draining from the VC as it may be misinterpreted as indicating metastatic disease, despite not metastasizing. 10 In our patient, pathological evaluation was performed on the neck mass for accurate metastases evaluation. The neck mass did not have an anatomical structure that could develop primary SCC around it, and it was confirmed that the apoptotic shrinkage in tumor cells seen in the neck mass was also observed in the tonsil mass. Therefore, we concluded that VC originating in the tonsil was the cause of neck metastases.
In another study, metastases accompanied by primary verrucous carcinoma can be explained by an inaccurate pathological diagnosis or occult SCC presence in lesions with VC characteristics. 11 Moreover, among VCs recorded as regional or distant metastases, there is a possibility that they will be reclassified as “hybrid” verrucous carcinoma, a papillary SCC, or SCC with verrucous features by histological review. 10 Therefore, accurate pathological findings for metastases are essential in VC.
Wide surgical excision should be considered the primary treatment for VC, and radiotherapy should be considered a secondary treatment if complete resection is impossible. Surgical treatment is recommended first because distant metastases are extremely rare, and most VCs show good differentiation, although they can cause local invasion. Chemotherapy can also be administered, and a study reported that chemotherapy is effective against advanced VC. 12 The 5-year survival rate of VC was reported to be 88.9% for surgical treatment alone, 57.6% for radiotherapy alone, and 73.4% for the combination of surgical treatment and radiotherapy. 9 Other studies have reported VC survival rates of 100% for stage I, 68% for stage I, 35% for stage II, and 26% for stage III. 8 The overall recurrence rate of VC after surgical treatment has been reported to be approximately 30% to 50%, necessitating continuous follow-up. 3
Footnotes
Authors’ Note
We declare that this article is original, has not been published before, and is not currently being considered for publication elsewhere. We confirm that the article has been read and approved by all named authors and all authors contributed. There are no other persons who satisfied the criteria for authorship but are not listed. We further confirm that the order of authors listed in the article has been approved by all authors.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Institutional Review Board of Jeju National University Hospital approved this study.
