Abstract

Significance Statement
The incidence rate of anterior inferior cerebellar artery (AICA) aneurysms is less than 1% in intracranial aneurysms, and distal aneurysms are even rarer, accounting for about 0.1%. 1 When only present with cranial nerve symptoms, it may be misdiagnosed as vestibular neurilemmomas.
Here we report a case of an AICA aneurysm misdiagnosed as vestibular schwannoma with significant hemorrhage during the surgery. This case emphasizes the important role of Digital Subtraction Angiogra (DSA) in the diagnosis of AICA aneurysm.
A 62-year-old Chinese female patient sought medical attention from the neurology department with a complaint of “recurrent dizziness and headache for 3 months and hearing loss and tinnitus in the left ear for 2 months.” Her head MRI revealed a mass in the left internal auditory canal and no abnormalities were reported by MRA. She then came to our otolaryngology department for further treatment.
She had no special medical history before. Physical examination showed her left peripheral facial paralysis was Grade III, without other abnormalities. Her pure tone audiometry revealed normal hearing in the right ear and severe hearing loss in the left ear, while acoustic impedance test revealed “A” pattern in both ears (Figure 1). Computer tomography (CT) reconstruction of the internal auditory canal revealed a nodular, mildly high-density shadow in the left cerebellopontine angle region, and the left internal auditory canal was slightly enlarged compared to the opposite side (Figure 2A).The left internal auditory canal was enlarged, with nodular equal T1, short T2 signal shadows, and an ambiguous boundary, according to the MRI (Figure 2B). The mass was clearly and uniformly enhanced on the enhanced magnetic resonance imaging (MRI) with a size of approximately 5.7 mm × 5.2 mm and was estimated to be a vestibular schwannoma (Figure 2B).
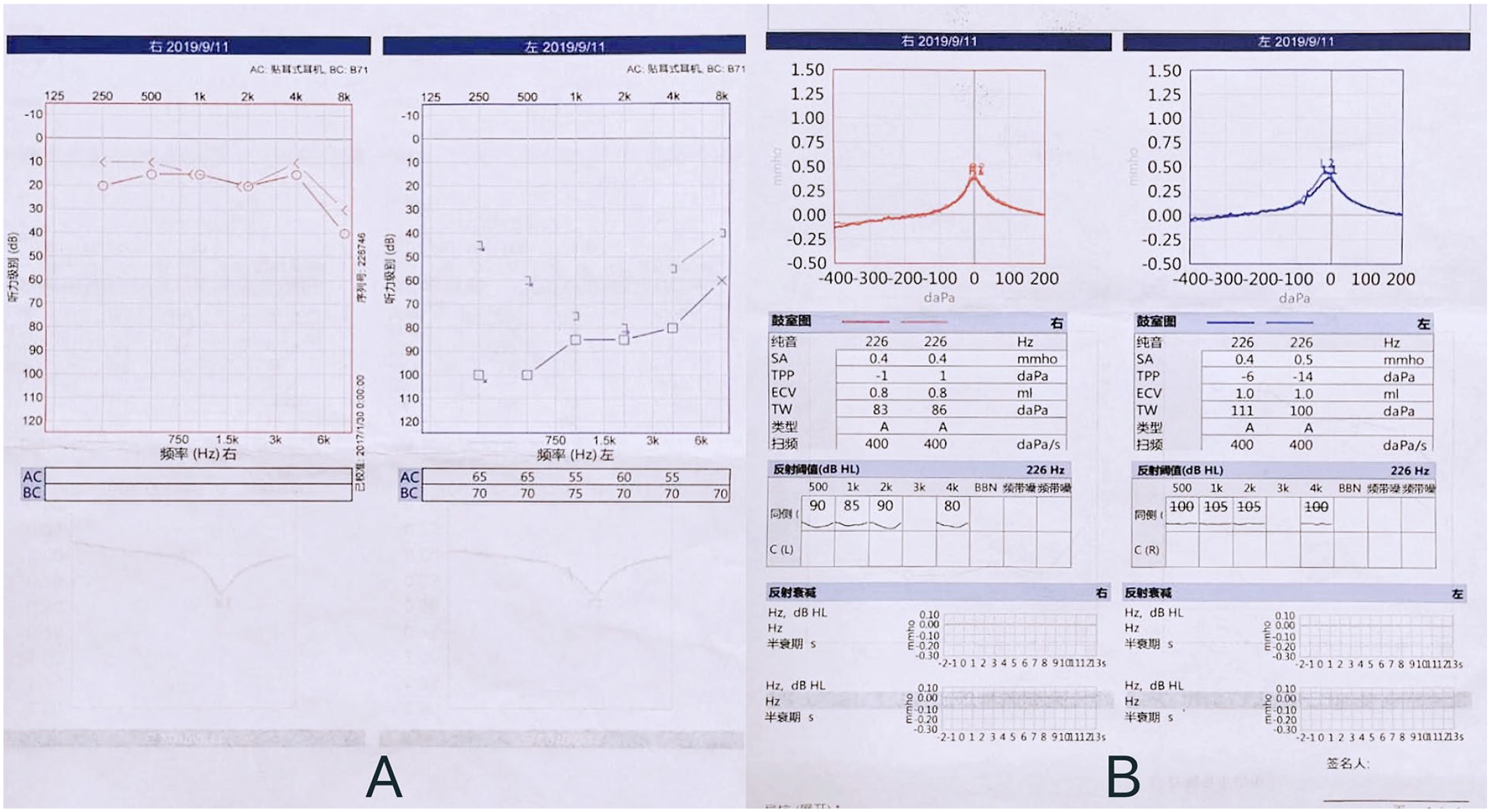
(A) The pure tone audiometry revealed severe hearing loss in the left ear. (B) The acoustic impedance test revealed “A” pattern in both ears.
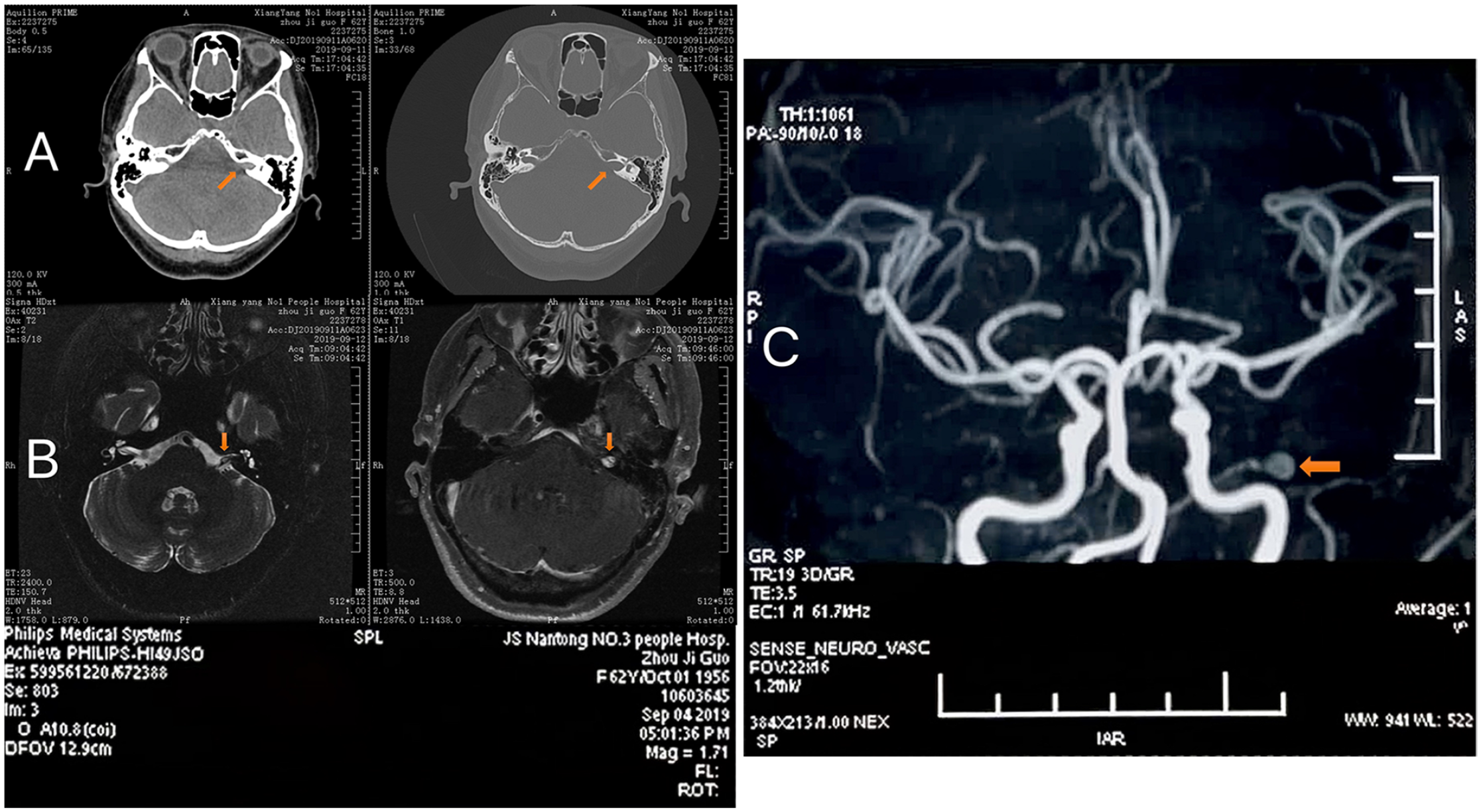
(A) CT reconstruction revealed a nodular, mildly high-density shadow in the left cerebellopontine angle region, and the left internal auditory canal was slightly enlarged. (B) MRI revealed a mass with equal T1, short T2 signal, the mass was clearly and uniformly enhanced on the enhanced MRI with a size of approximately 5.7 mm × 5.2 mm. (C) No abnormalities were reported by MRA, however as we re-read her MRA images, the final diagnosis was a distal AICA aneurysm.
The mass was identified as a left vestibular schwannoma based on the patient’s primary complaint, and translabyrinthine approach for left internal auditory canal neoplasm resection under general anesthesia was selected. Bright red neoplasm with a smooth surface could be observed after the internal auditory canal was exposed during the operation. Since the diagnosis of vestibular schwannoma was not questioned, we directly incised the tumor. When the neoplasm was incised, bright red blood spurted out in columnar form (Figure 3). Based on the situation and her MRA images (Figure 2C), the final diagnosis was a distal AICA aneurysm. After sufficient hemostasis, the surgery was terminated. She was transferred to neurosurgery for further treatment.
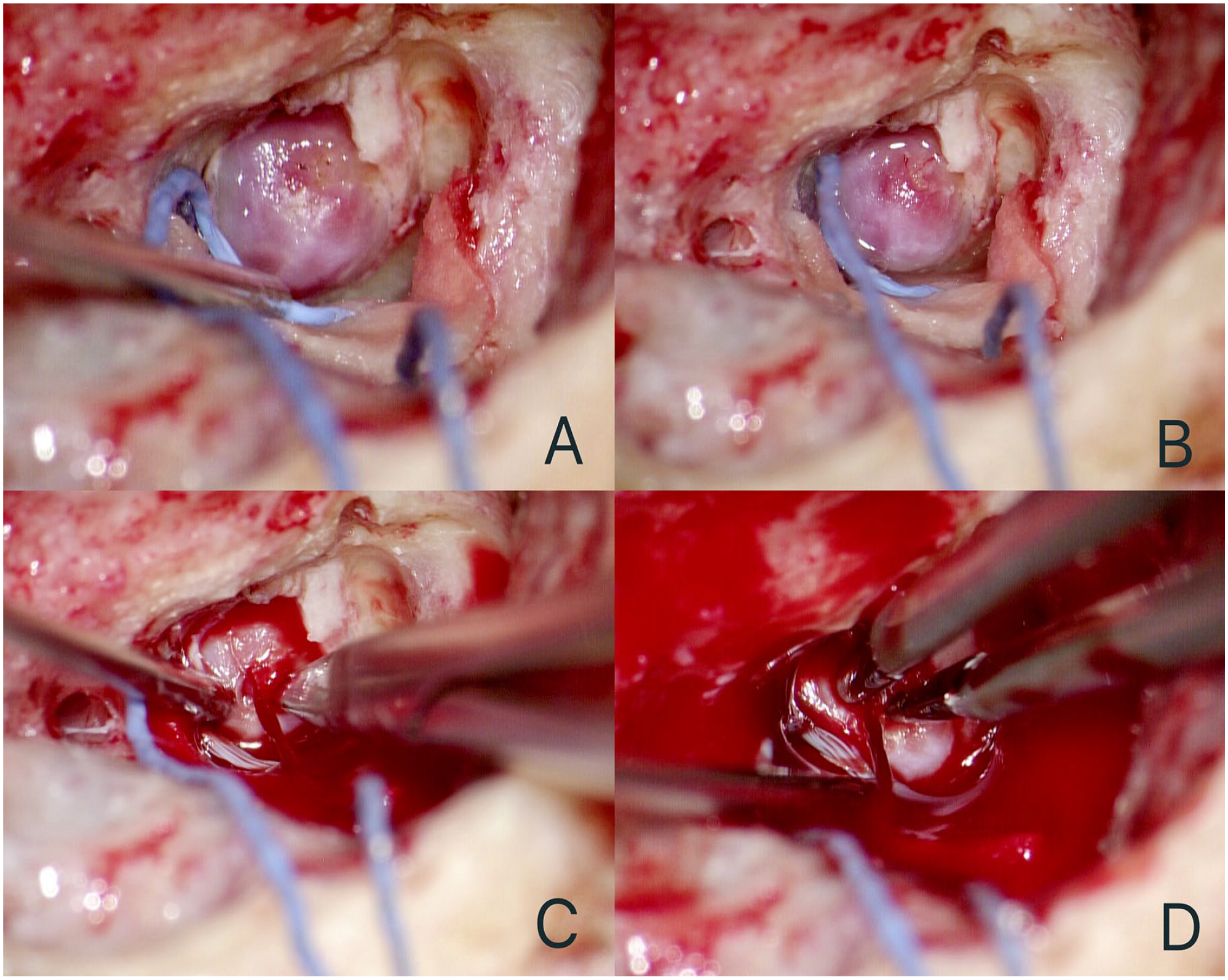
(A, B) Bright red neoplasm with a smooth surface could be observed. (C, D) When the neoplasm was incised, bright red blood spurted out in columnar form.
The incidence rate of AICA aneurysms is less than 1% in intracranial aneurysms, and distal aneurysms are even rarer, accounting for about 0.1%. 1 More than 80% of distal AICA aneurysms are diagnosed due to subarachnoid hemorrhage. 2 The majority of individuals exhibit facial and auditory nerve paralysis along with subarachnoid hemorrhage symptoms.2,3
When subarachnoid hemorrhage is caused by ruptured AICA aneurysms with cerebellopontine angle syndrome, it can be confirmed by CT and/or MRI. However, when only present with cranial nerve symptoms, the diagnosis of aneurysms lacks specificity by CT and/or MRI, and may be misdiagnosed as vestibular neurilemmomas, which are more common. 4 Aneurysms located in the internal auditory canal are prone to be missed by CT angiography (CTA). DSA is recommended to be improved as it can not only clearly display the size and location of the tumor, but also display the blood supply between various intracranial blood vessels, and can detect other coexisting cerebral vascular malformations. 5
The treatment of AICA aneurysms mainly includes surgical clipping and interventional embolization. Although interventional therapy has been reported, surgical clipping is still the best treatment, especially for aneurysms located at the distal end of AICA.4,5 The surgical approach depends on the location of the aneurysm. Aneurysms at the proximal end of AICA are generally treated through the middle cranial fossa or translabyrinthine approach. For aneurysms located at the distal end of AICA, the retrosigmoid approach is mostly chosen. 6 For some aneurysms located in the internal auditory canal, the 7th and 8th cranial nerves should be protected during the operation. There are many proficient vessels in AICA supplying the brainstem and auditory nerve which can lead to serious consequences once damaged. Careful preparation, proficient techniques, and resolute decisions are the guarantees of successful operations. In addition, multidisciplinary consultations are recommended to reduce the probability of misdiagnosis.
Footnotes
Acknowledgements
The authors thank Miss Rikee Liu for her edition of the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
