Abstract
Introduction
Pharyngeal fistula is a frequent complication of head and neck cancer surgery. It is a challenge to select appropriate flaps to repair penetrating pharyngeal fistulas. The use of supraclavicular flaps was first reported in 1979, and since then, has been greatly reformed. 1 Supraclavicular flaps have yielded encouraging results in the treatment of neck burn scars, oral and maxillofacial diseases, and head and neck tumors.1,2 In this study, double island folding of the supraclavicular flap and the supraclavicular flap combined with the pectoralis major flap were used to repair the pharyngeal fistula for the first time. We described the efficacy of pharyngeal fistula repair with supraclavicular flaps, preparation techniques, indications, and postoperative complications.
Patients and Methods
Patients
We analyzed the clinical data from patients treated with supraclavicular flaps to repair penetrating pharyngeal fistulas at the Northern Jiangsu People’s Hospital from January 2017 to December 2020. Included were 16 male patients aged 58 to 79 years, including 10 with postoperative pharyngeal fistula after hypopharyngeal cancer, 5 with postoperative pharyngeal fistula after laryngeal cancer, and 1 with postoperative pharyngeal fistula after laryngeal and esophageal cancer. Three of these patients had a history of radiation therapy prior to tumor resection. The pharyngeal fistula, once discovered during the healing process after tumor resection, was treated with antibiotics, dressing changes, debridement, negative pressure drainage, local sutures, and pressure bandages in the first 2 weeks. The surrounding necrotic tissue was removed during debridement to keep the wound fresh. All patients underwent second-stage reconstructive surgery, when the above methods failed (Table 1). Written consent was obtained from all the patients.
Clinical Data of the Patients and Prognosis of Pharyngeal Fistulas.
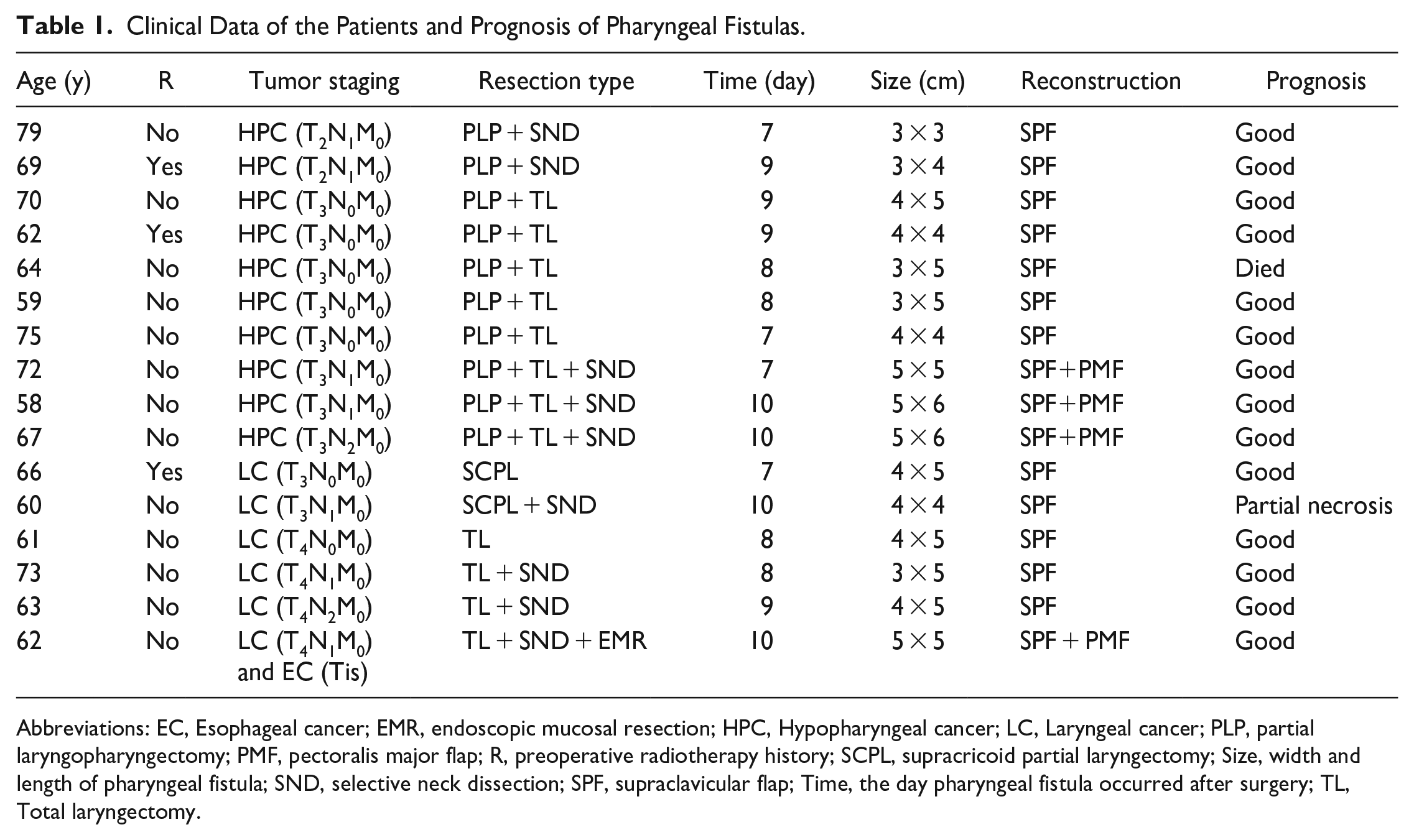
Abbreviations: EC, Esophageal cancer; EMR, endoscopic mucosal resection; HPC, Hypopharyngeal cancer; LC, Laryngeal cancer; PLP, partial laryngopharyngectomy; PMF, pectoralis major flap; R, preoperative radiotherapy history; SCPL, supracricoid partial laryngectomy; Size, width and length of pharyngeal fistula; SND, selective neck dissection; SPF, supraclavicular flap; Time, the day pharyngeal fistula occurred after surgery; TL, Total laryngectomy.
Techniques
The pharyngeal fistula was repaired by double island folding of the supraclavicular flap in 12 patients. The side of the neck without evident lymph nodes in regions V was selected to prepare the supraclavicular flap. In case 1, the distal skin island A was used to repair the cervical skin defect and the proximal skin island B to repair the mucosal surface of the pharyngeal fistula (Figures 1-4). In case 2, distal skin island A was used to repair the mucosal surface of the pharyngeal fistula and proximal skin island B to repair the cervical skin defect (Figures 5-8). The remaining 4 patients with larger pharyngeal fistulas were repaired with a supraclavicular flap combined with a pectoralis major flap (Figures 9-12). The skin side of the pectoralis major flap was directed medially to repair the mucosa of the pharyngeal fistula and close the laryngopharyngeal defect. The skin side of the supraclavicular flap was placed outward over the pectoralis major flap to repair the skin defect of the neck. All patients were treated with hormones and low molecular weight heparin for 3 days after surgery to facilitate blood circulation and reduce edema in distal skin islands. Flap survival was checked by electronic laryngoscopy and esophagogram 2 weeks later. Swallowing function was assessed after 1 month of nasal nutrition.
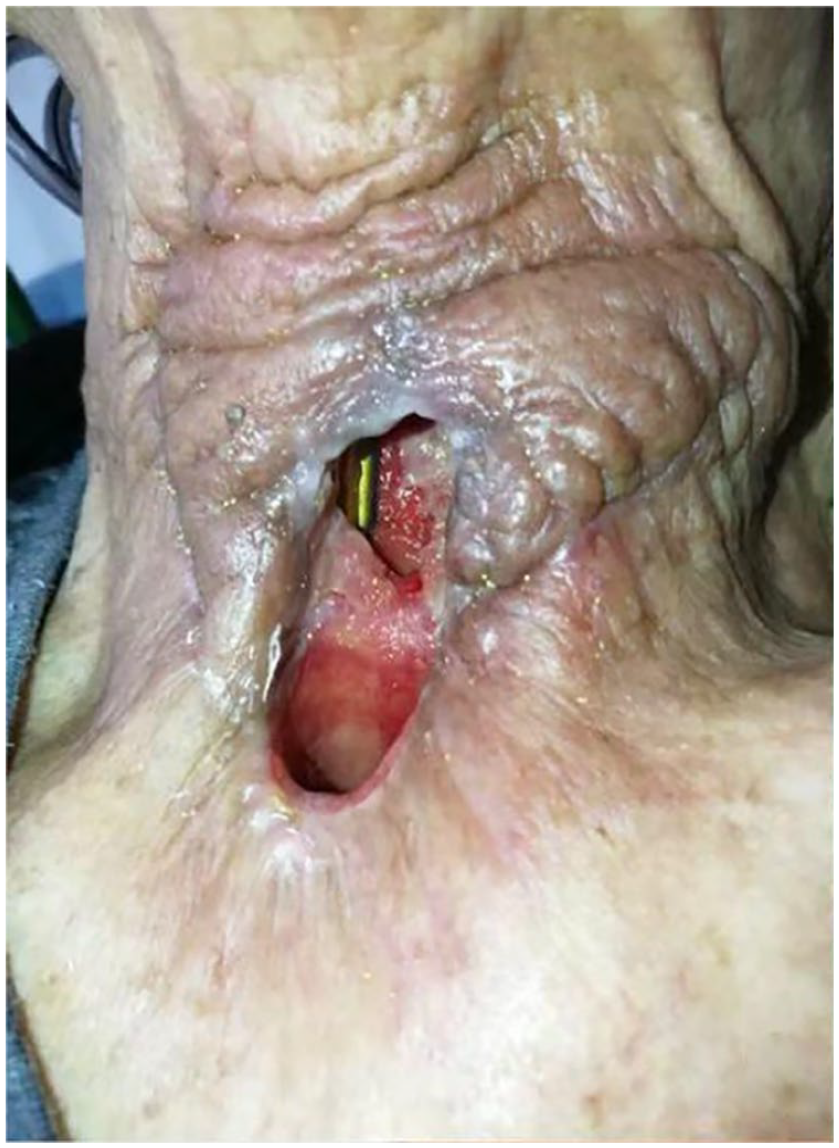
Size and shape of the preoperative pharyngeal fistula.
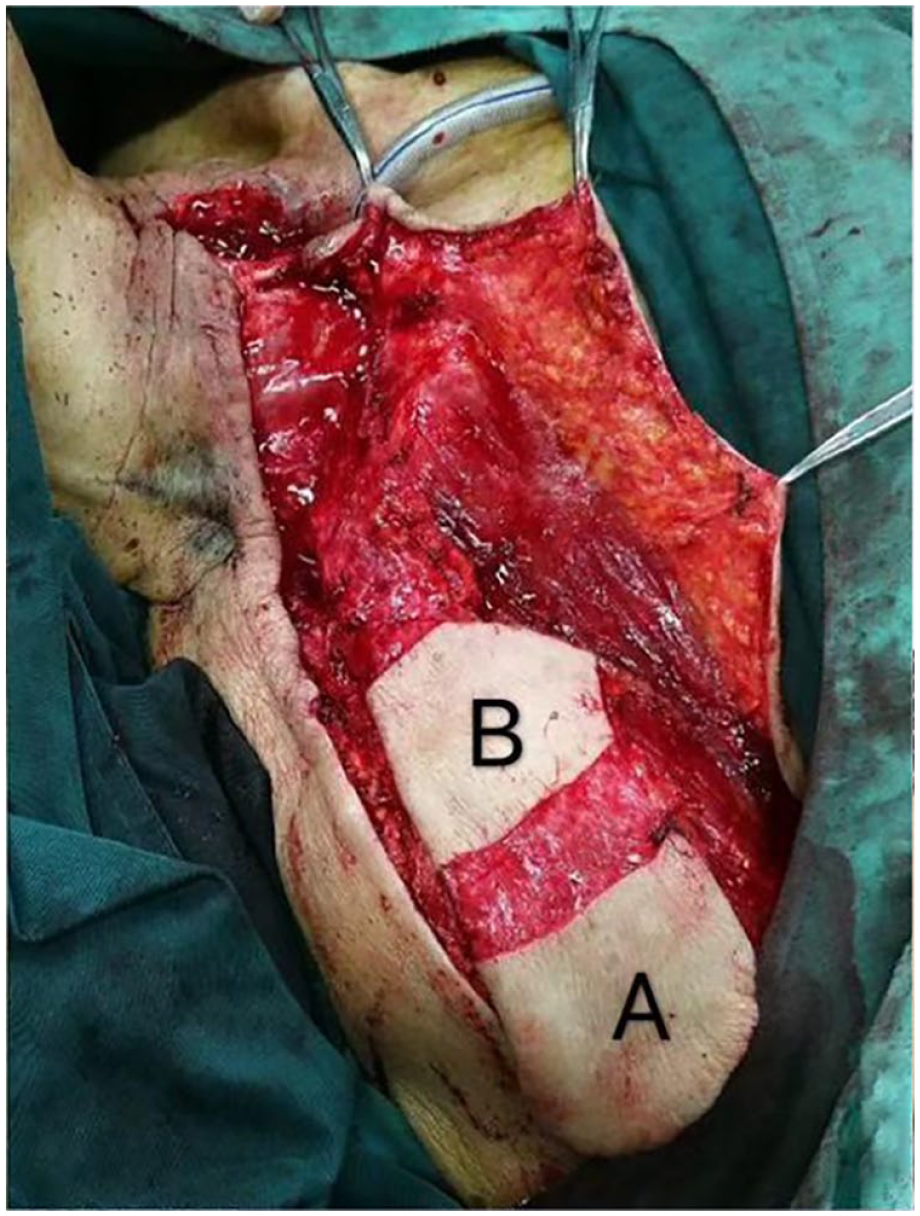
Size and position of the single-tipped double island supraclavicular flap. (A) The distal skin island and (B) The proximal skin island.
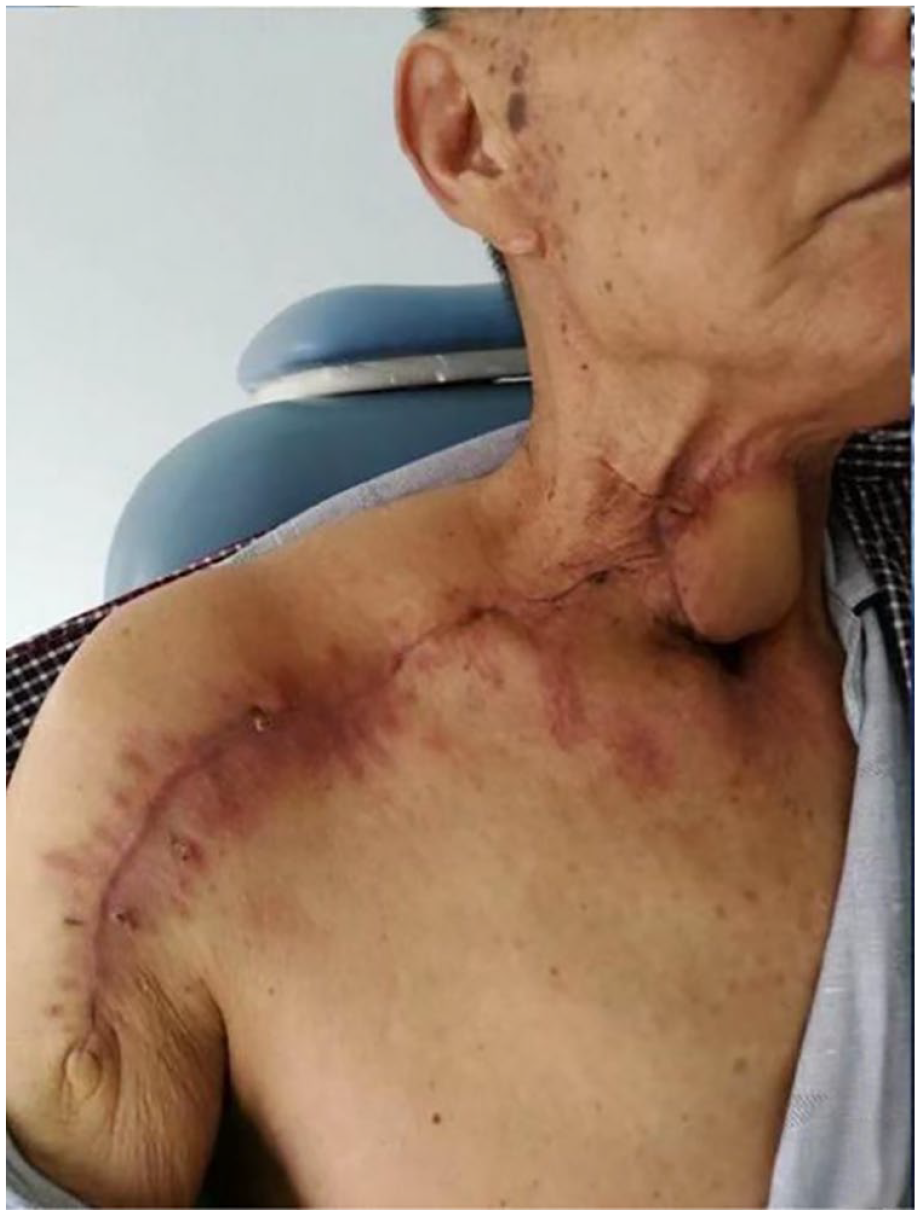
Postoperative flap condition.
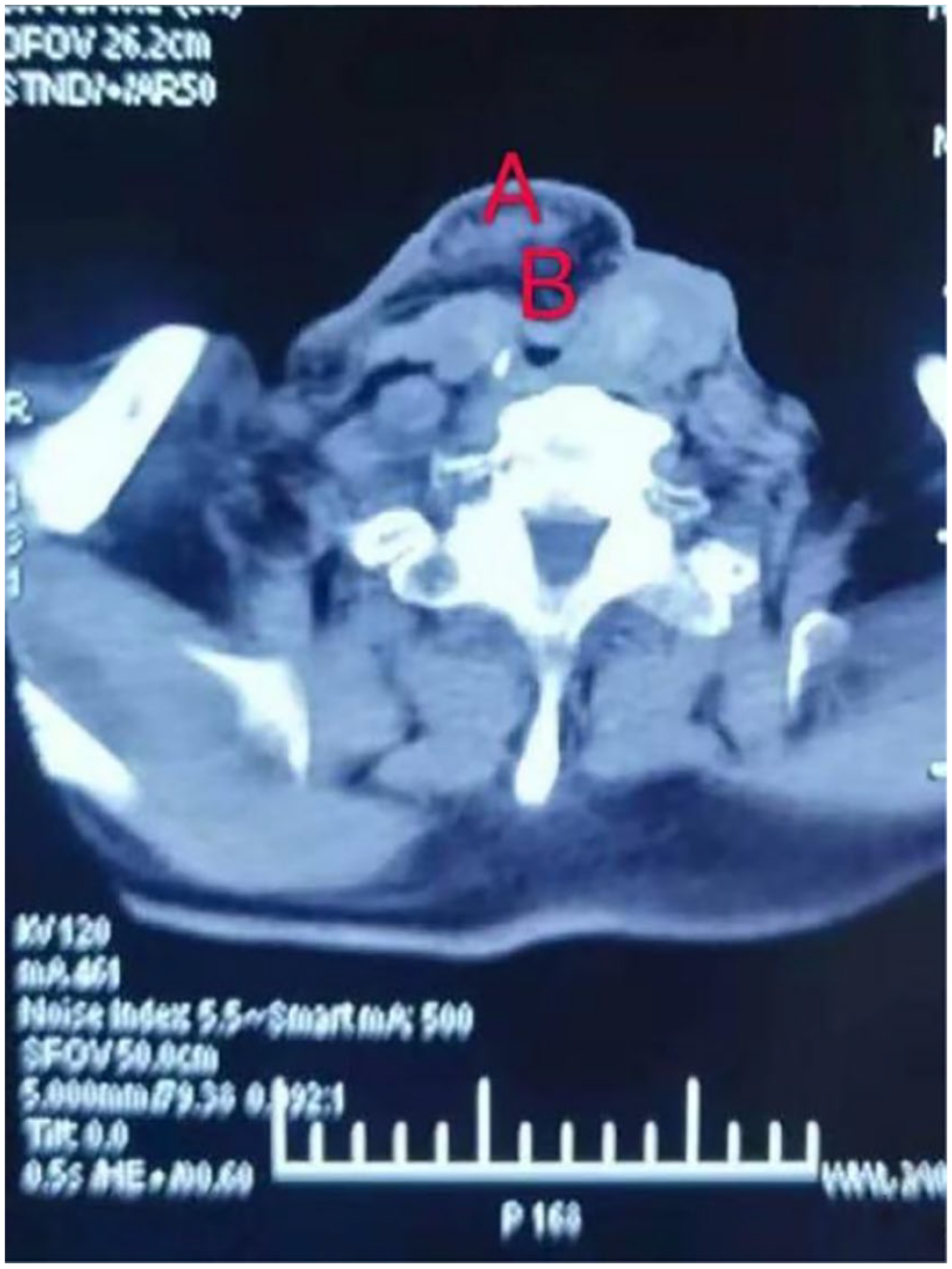
Postoperative neck CT examination. (A) The distal skin island and (B) The proximal skin island.
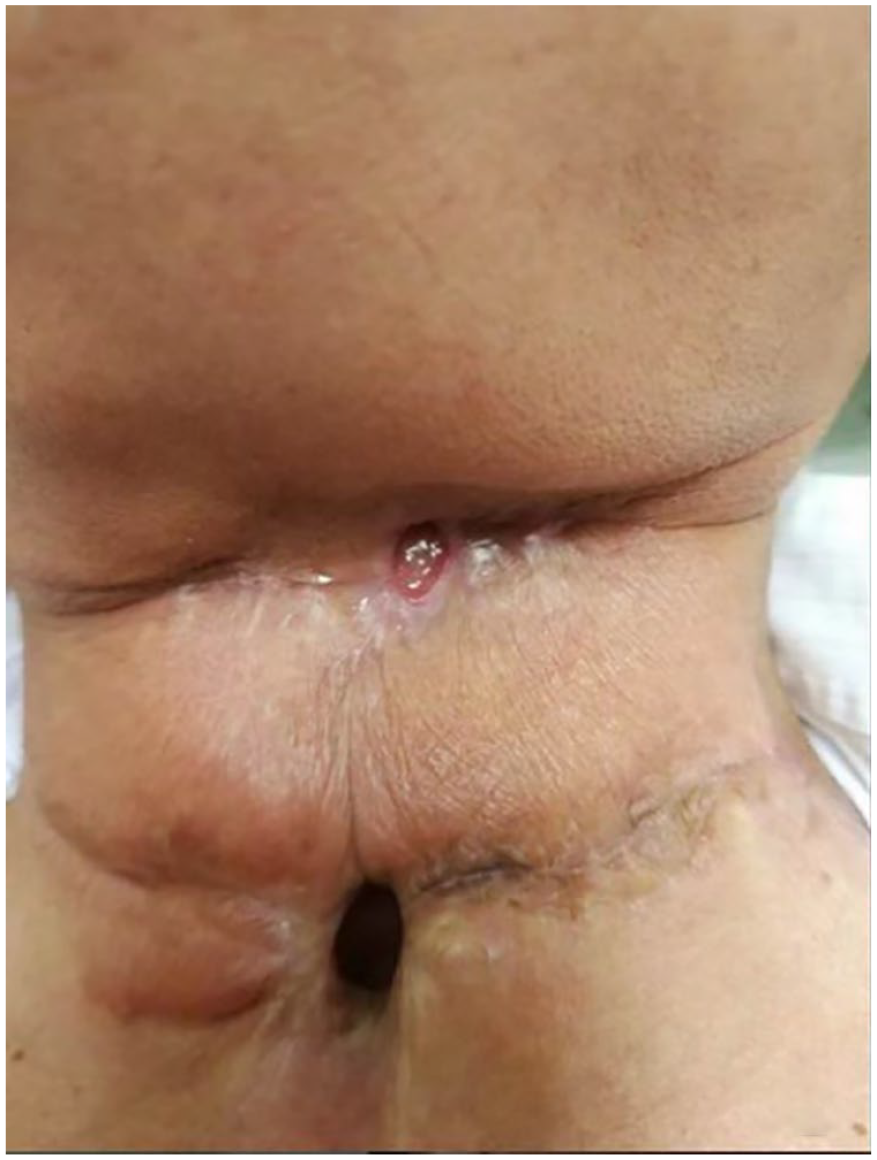
Size and shape of the preoperative pharyngeal fistula.
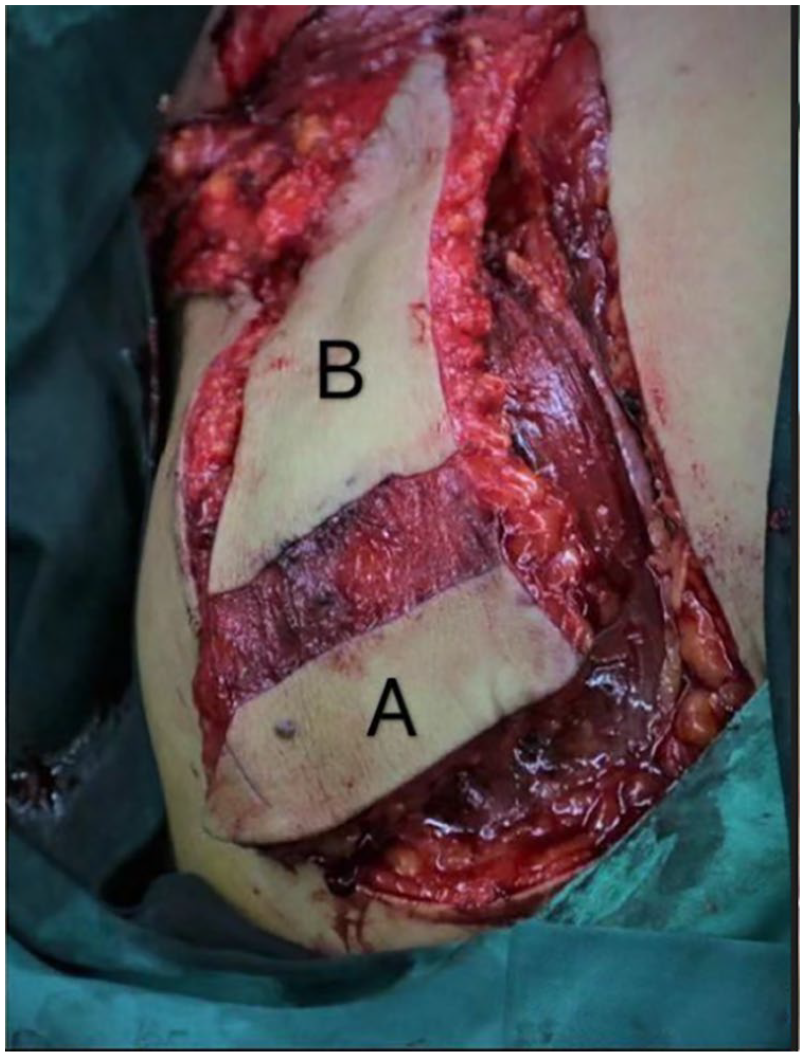
Size and position of the single-tipped double island supraclavicular flap. (A) The distal skin island and (B) The proximal skin island.
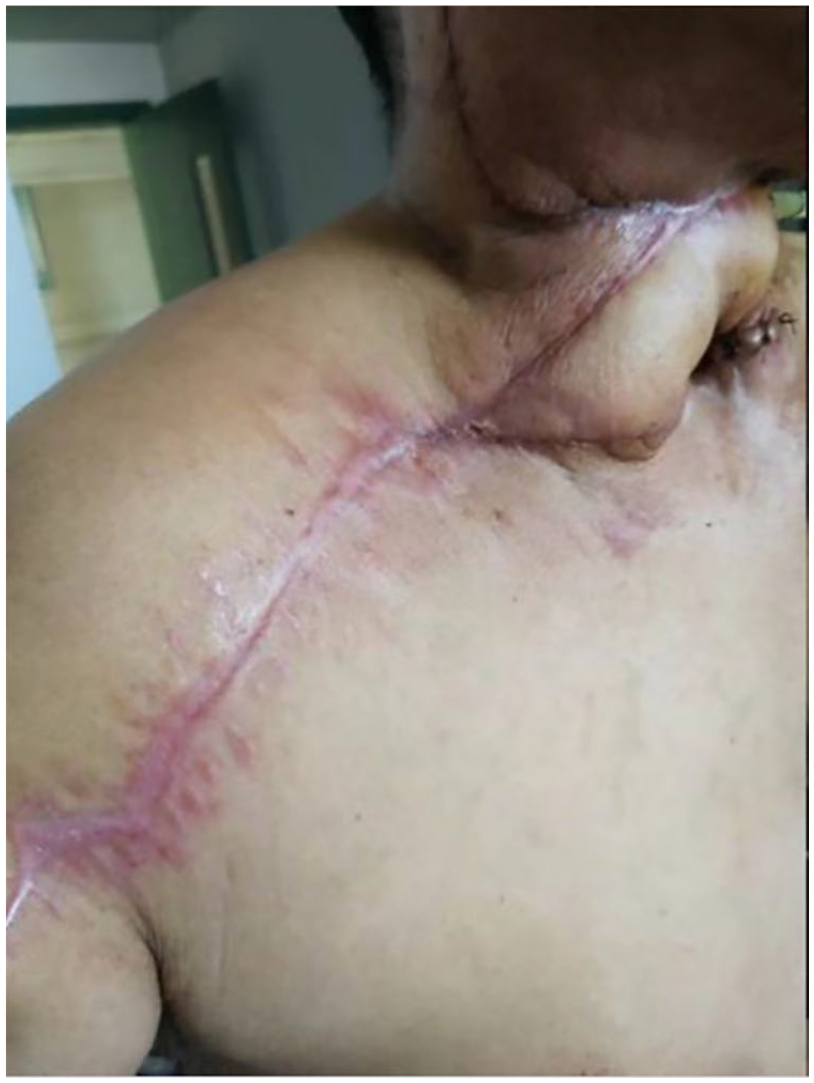
Postoperative flap.
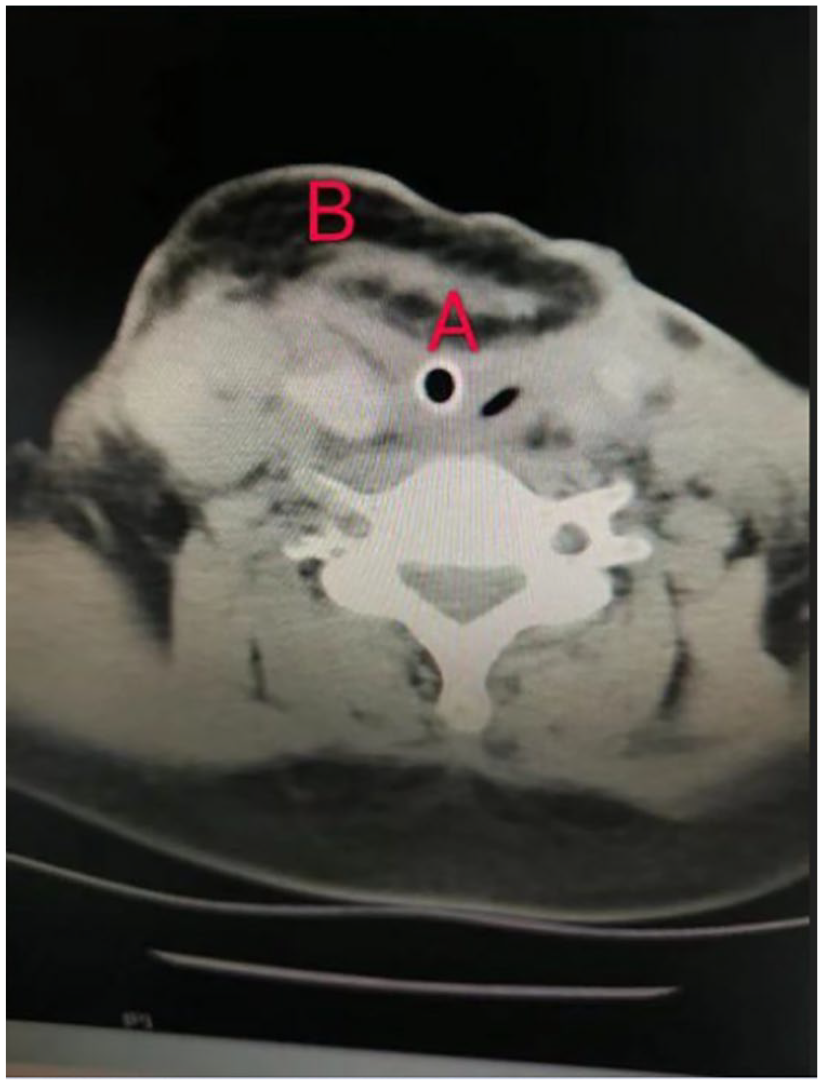
Postoperative neck CT examination. (A) The distal skin island and (B) The proximal skin island.
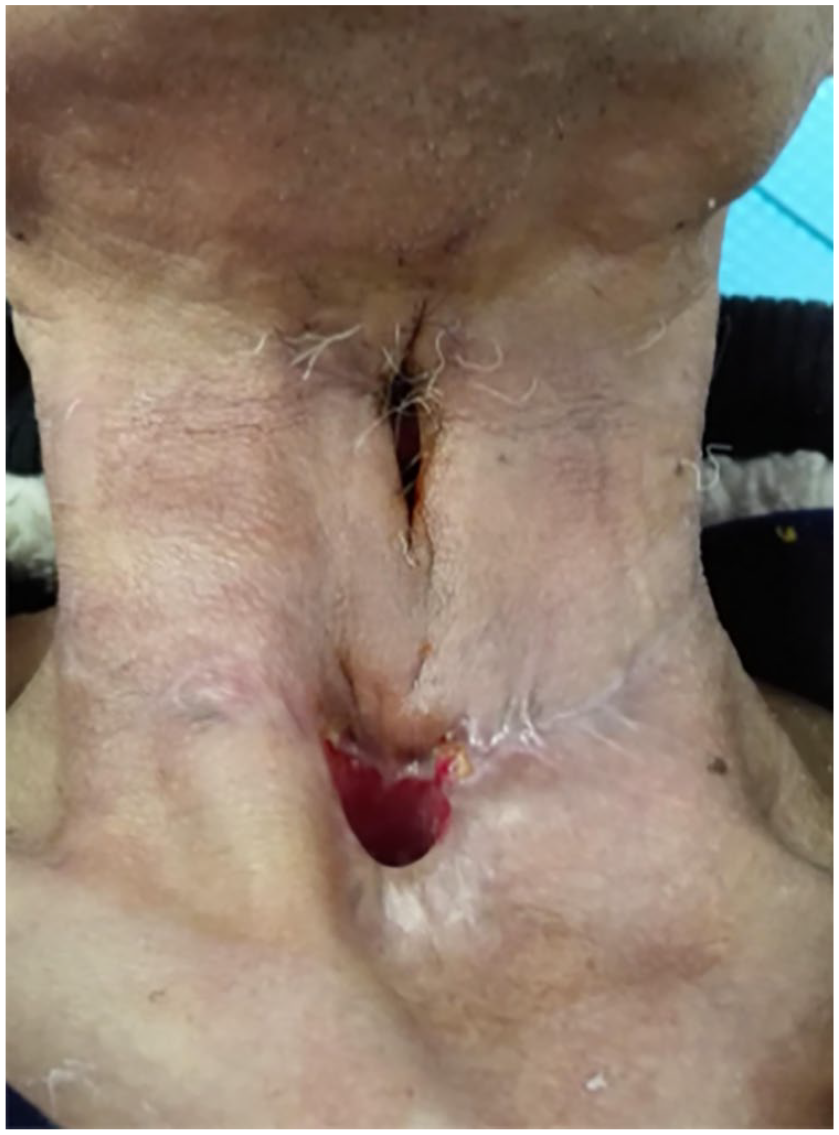
Size and shape of the preoperative pharyngeal fistula.
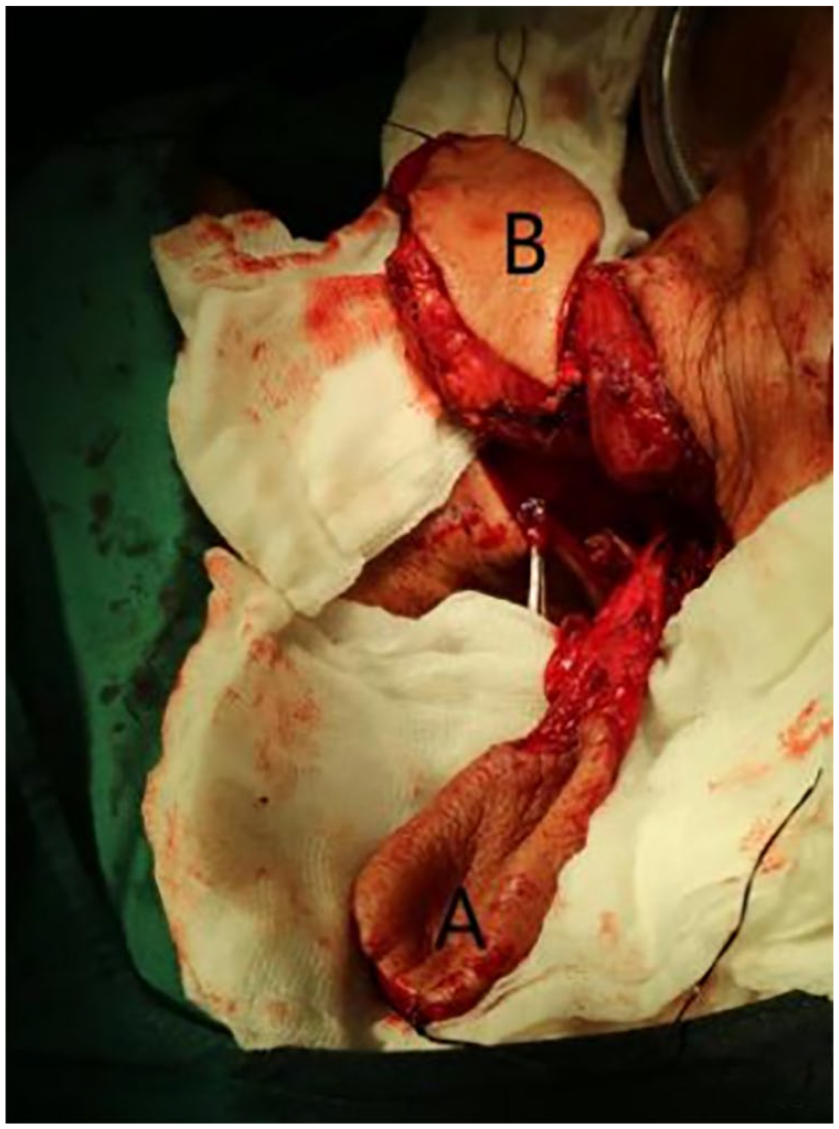
Intraoperative design of the supraclavicular flap (A) and the pectoralis major flap (B).
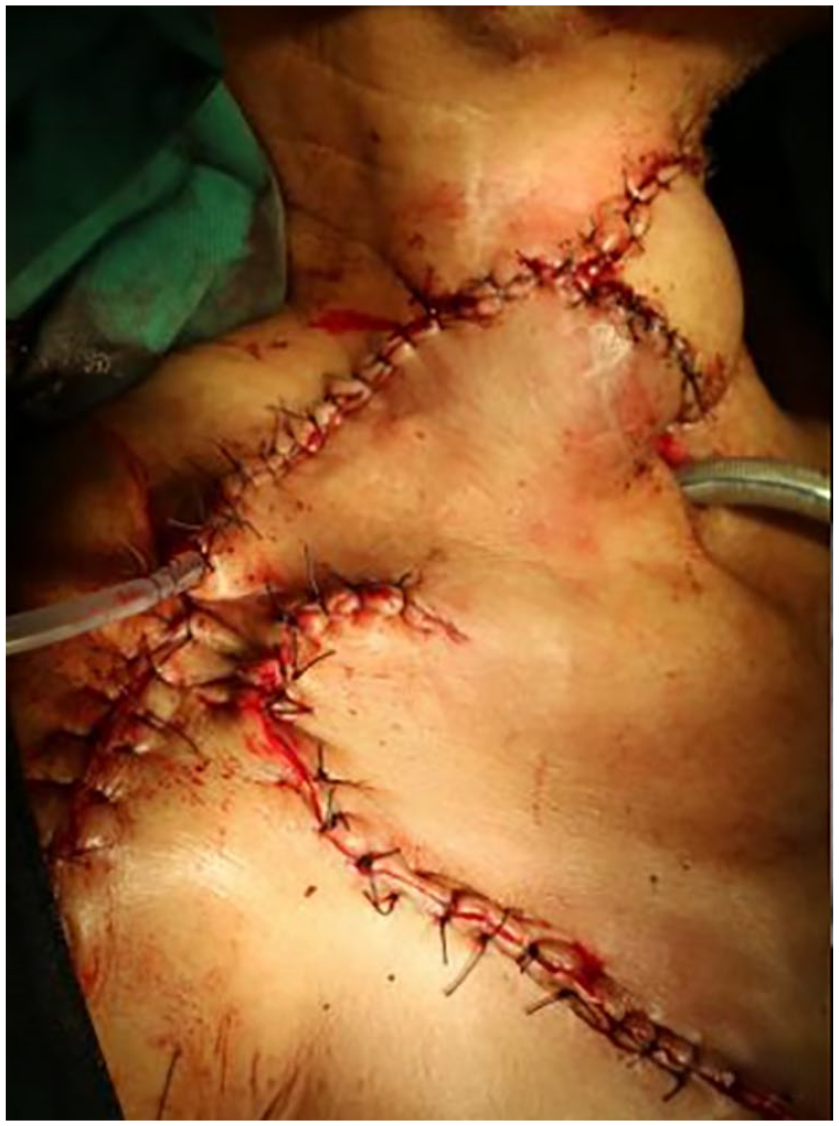
Postoperative flap.
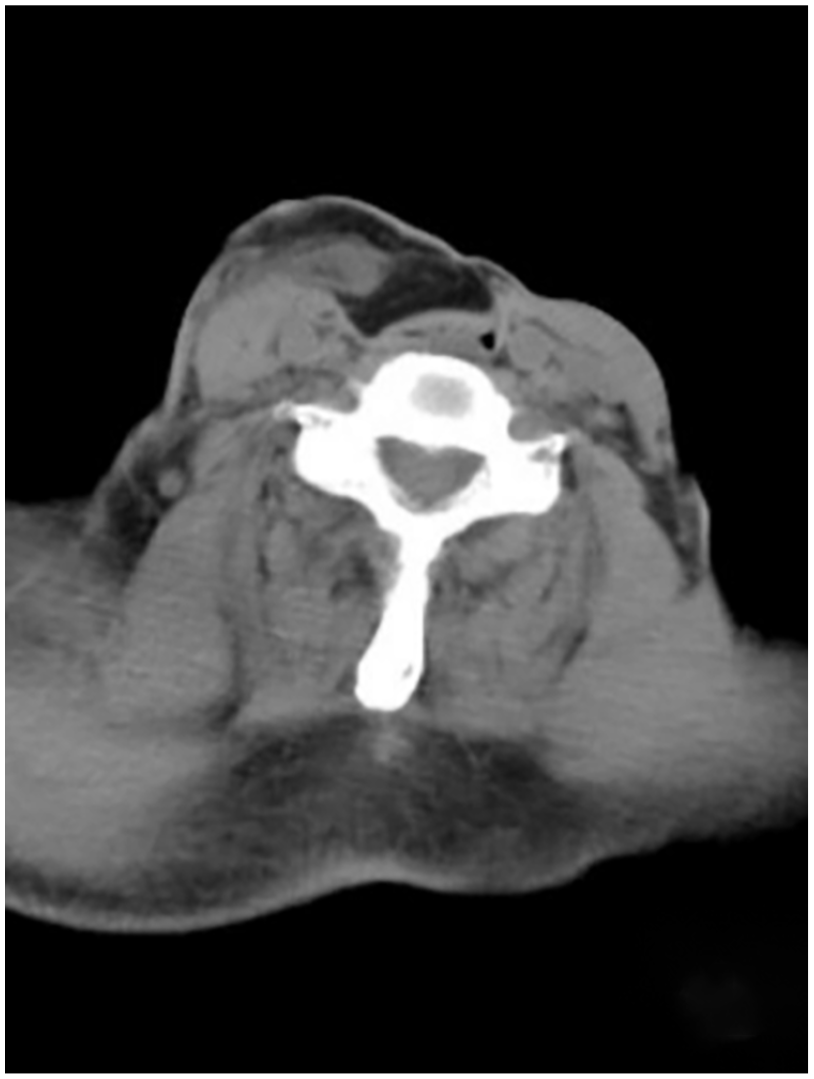
Postoperative CT examination of the neck.
Results
The supraclavicular flap was taken from the left shoulder in 7 patients and from the right shoulder in the remaining 9 patients. The size of the supraclavicular flap taken was 6 to 8 cm in width and 6 to 15 cm in length. One patient had partial necrosis at the distal end of the flap, which was successfully treated after debridement and dressing. The flaps grew well in the remaining 15 patients. Among them, a patient with a postoperative pharyngeal fistula after hypopharyngeal carcinoma was implanted with radioactive particles for tumor recurrence at the entrance of the esophageal, and died in the 11th month after surgery (Table 1).
Discussion
The supraclavicular flap is a fascial tissue flap tipped with a supraclavicular arteriovenous penetrating branch and its surrounding fatty connective tissue. Its reparative potential for fistulas has been highlighted in recent years. Since Lamberty first reported it in 1979, its anatomy has been clarified. 3 The supraclavicular artery originates mainly from the branch of the transverse cervical artery to the deltoid region of the shoulder, and to a lesser extent from the suprascapular artery. 4 The anatomical variation of supraclavicular arteries and veins is relatively prominent. The veins are particularly thin and anatomically variable. The supraclavicular flap was initially used for cervicofacial skin repair after burns. But today it is widely used for the repair of postoperative defects resulting from head and neck tumors, such as oral cancer, tongue cancer, and hypopharyngeal cancer.5,6 Other pedicled flaps, such as the pectoralis major muscle flap, are too bulky and hypertrophic, and the latissimus dorsi muscle flap requires changing its position during surgery. Compared to other flaps, the supraclavicular flap does not contain a muscle layer and has the advantages of moderate thickness, high tissue flexibility, rich blood supply, proximity to the defect site, simple preparation, and minimal trauma. The donor area should only be pulled together and sutured without additional skin grafting.7,8
In this study, double island folding of the supraclavicular flap and the supraclavicular flap combined with the pectoralis major flap were used to repair pharyngeal fistula for the first time. All patients were confirmed to have Grade 3 pharyngeal fistula with localized penetrating fistula formation. A total of 12 patients with small pharyngeal fistulas were repaired by folding the double island of a supraclavicular flap. The remaining 4 patients with large pharyngeal fistulas were repaired with a supraclavicular flap combined with a pectoralis major flap.
Previous literature reported that Doppler ultrasound or Digital Subtraction Angiography (DSA) should be used to pinpoint the transverse cervical artery and supraclavicular artery before surgery. 9 However, in practice, we found that this method is not suitable for all patients. The supraclavicular artery is too thin to be displayed by ultrasound. As shown in the present study, the posterior cervical triangle, which was delineated by the posterior border of the sternocleidomastoid muscle, the external jugular vein, and the superior clavicular border, could be referred to as the tip of the flap, without deliberately dissecting the transverse cervical artery. In addition, the flap should be turned intraoperatively with a clear anatomical hierarchy, separated with a blade, and coagulated by bipolar electrocoagulation. This treatment can reduce damage to the flap vessels. Recently, we have recognized that indocyanine green achieves a high accuracy in assessing the intraoperative blood supply into the flap.
In our study, we also found that supraclavicular flaps often bruise postoperatively, which may be related to the thinness or absence of supraclavicular veins. Therefore, the external jugular vein should be preserved as much as possible to ensure adequate venous return of the flap. If the disconnection position is low, the distal end of the external jugular vein can be injected directly into the internal jugular vein by performing a microvascular anastomosis. When the flap is sutured, the flap tip should not be twisted and the stitches should not be too dense. Otherwise, the flap anastomosis may split due to excessive tension or poor blood supply. In addition, patients with lymph node metastases in lateral cervical regions V and those with a history of surgery and radical radiotherapy in the clavicular region are not suitable candidates for supraclavicular flap transfer surgery. 10
Conclusions
The supraclavicular flap has the advantages of simple preparation, small trauma, few postoperative complications, and anatomical proximity to the defect site, all of which make it clinically recommended for the repair of pharyngeal fistula.
Footnotes
Acknowledgements
I would like to express my gratitude to Mr. Yongke Cao for English language editing. I also want to thank the research team for their collaboration and help during gathering data for my research project.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
This study was approved by the Ethics Committee of the Institutional Review Board of Northern Jiangsu People’s Hospital.
Statement of Human and Animal Rights
In our study, the procedures followed were in accordance with the ethical standards of the Ethics Committee of the Institutional Review Board of Northern Jiangsu People’s Hospital on human experimentation and with the Helsinki Declaration of 1975, as revised in 2000.
Statement of Informed Consents
Written consent was obtained from the patients.
