Abstract
Objective:
The reasons for short-term, incomplete recovery of some acute low-frequency sensorineural hearing loss (ALFHL) are unclear. We investigated the impact of endolymphatic hydrops and semicircular canal dysfunction on the incomplete recovery of ALFHL.
Methods:
The impact of electrocochleography (EcochG), caloric test, video head impulse test (vHIT), cervical vestibular-evoked myogenic potential (cVEMP), and ocular vestibular-evoked myogenic potential (oVEMP) results on the incomplete recovery of 86 patients with ALFHL was analyzed. The correlation between a high abnormal rate of vestibular-evoked myogenic potential (VEMP) and aural fullness, dizziness, and level of hearing loss was also examined.
Results:
Abnormal oVEMP with an odds ratio (OR) of 6.071 (P = .002) and EcochG with an OR of 5.919 (P = .005) were independent risk factors for incomplete recovery in ALFHL, but abnormal cVEMP, caloric test, and vHIT were not independent risk factors for ALFHL. There was no correlation between a high abnormal rate of VEMP and aural fullness, dizziness, or level of hearing loss in ALFHL.
Conclusion:
Abnormal oVEMP and EcochG values rather than caloric test and vHIT were risk factors for incomplete recovery of ALFHL, which may be related to the difficulty of successfully treating utricular and cochlear hydrops. High abnormal rate of VEMP was not correlated with hearing loss level, aural fullness, or dizziness in ALFHL. Abnormal oVEMP and EcochG values can indicate poor short-term prognosis of ALFHL.
Keywords
Introduction
Acute low-frequency sensorineural hearing loss (ALFHL) was initially classified as a subtype of idiopathic sudden sensorineural hearing loss, but is now recognized as a distinct condition. 1 While the exact pathophysiology of ALFHL remains unknown, previous study have suggested a potential association between ALFHL and cochlear hydrops or the early stages of Meniere’s disease (MD). 2 The condition of ALFHL is known to have a favorable prognosis with a high recurrence rate. 3 Previous reports indicated that the spontaneous recovery rate of untreated ALFHL ranged from 32% to 65%.4,5
Although studies have reported a good prognosis for acute ALFHL, some patients with ALFHL still have no improvement in their hearing or, despite some improvement, may not fully recover. 6 The cause of the poor prognosis of these patients and the pathophysiology is still unclear. It is not clear whether these patients cannot be quickly cured because the endolymphatic hydrops (EH) is not easy to resolve, or whether it progresses to MD. Inui et al 7 recently utilized 3-dimensional magnetic resonance imaging to discover a correlation between an increase in volume ratio of EH within the cochlea and non-cure of ALFHL. Furthermore, their study suggested that an increased volume ratio of EH in the vestibule and cochlea may contribute to the development of cochlear MD in patients with ALFHL. 7 Therefore, we speculate whether it is possible to predict the poor prognosis of ALFHL by assessing the EH in the cochlea and vestibule, as well as the function of the semicircular canals.
Electrocochleography (ECochG), a technique for recording cochlear electrical events, has evolved as an important tool in indication of EH in the cochlea. 8 The caloric test evaluates the low-frequency function of the horizontal semicircular canal, while the video head impulse test (vHIT) can assess the high-frequency function of all 3 pairs of semicircular canals. Vestibular-evoked myogenic potential (VEMP) is an objective method for assessing the otolithic apparatus and vestibular nerve conduction pathways in the vestibular system, such as the utricle and saccule, and is a myogenic potential recorded after stimulation of the otolithic apparatus by high-intensity acoustic signals. 9 Therefore, in this study, ECochG was used to detect cochlear EH, VEMP was used to detect EH in the utricle and saccule, while the caloric test and vHIT were employed to assess the function of the semicircular canals in patients with ALFHL. Furthermore, the correlation between the aforementioned results and incomplete recovery in ALFHL patients was analyzed.
Materials and Methods
The study was conducted in accordance with the Declaration of Helsinki, and was approved by the Ethics Committee. From January 2020 to December 2022, a total of 86 patients with ALFHL were included in this study. The inclusion criteria included acute onset sensorineural hearing loss exceeding 30 dB at 2 consecutive low frequencies of 250 and 500 Hz within a period of 3 days, 25 dB HL of normal hearing at hearing thresholds of 1, 2, 3, 4, and 8 kHz on the affected side, 25 dB HL of normal hearing at hearing thresholds of 0.25, 0.5, 1, 2, 4, and 8 kHz on the unaffected side and no history of episodic dizziness or spontaneous nystagmus. 6
The treatment protocol entailed oral administration of prednisone tablets at a dosage of 1 mg/kg/day, not exceeding 60 mg/day, for a continuous period of 5 days. Starting on the sixth day, 40 mg methylprednisolone was injected behind the ear every other day at a dose of 40 and 60 mg sodium aescinate tablets were taken orally twice a day, with 70 mg ginkgo biloba extract administered intravenously once a day. After 1 week of treatment, follow-up pure-tone audiometry was conducted. Patients who have fully recovered discontinued the treatment, while those who had not recovered continued for another week. After 2 weeks, only sodium aescinate tablets were administered orally.
ECochG Test
For the ECochG test, a Neuro-Audio system (Neurosoft, Ivanovo, Russia) was used in a sound-proof examination room. The EcochG silver ball electrode was placed on the upper wall of the deepest part of the ear canal near the eardrum and the extra tympanic ECochG was recorded bilaterally by averaging 1500 sweeps after alternating click stimuli of 7 per second at 95 dB nHL. This test was considered abnormal in this hospital when −SP/AP exceeded 0.40 and the SP/AP area ratio exceeded 1.92.
VEMP Test
For the VEMP test, the Neuro-Audio system (Neurosoft) was used to test patients in a sound-proof examination room. The VEMP waveforms were induced through ACS stimulation through inserted headphones with a 500-Hz short-tone burst of 1 ms-rise per fall time and 2 ms-plateau time, with 120 stimuli applied to each ear. The initial stimulus intensity was 95 dB nHL, which decreased incrementally by 5 dB nHL until the VEMP response disappeared and this process was repeated 3 times. Before applying the electrodes, the patient’s skin was disinfected and coated with a conductive paste. The resistance between the electrodes was controlled at less than 5 Ω. The cervical vestibular-evoked myogenic potential (cVEMP) and ocular vestibular-evoked myogenic potential (oVEMP) tests were described previously. 10
Caloric Test
For the caloric test, a 1068 nystagmograph (Otometrics, Taastrup, Denmark) was used to test patients in a dark examination room. The patient lay on their back, wore a nystagmograph, and tilted their head forward by 30°, placing the horizontal semicircular canal in a vertical position. During the examination, the patient had to keep their eyes open and blink as little as possible until the examination was completed. Hot air at 50°C and cold air at 24°C were injected into the ear in the order of cold first, then hot and then from left to right, with a flow rate of 8 L, lasting for 60 seconds each time. During the infusion process, the air nozzle was as close to the eardrum as possible and the next test was conducted after ensuring the subject has no nystagmus or dizziness. The nystagmograph was used to record and analyze nystagmus and the value of canal paresis (CP) was calculated. In this study, CP exceeding 25% was considered significant.
vHIT Test
For the vHIT test, an ICS Impulse system (GN Otometrics, Taastrup, Denmark) was used for patient testing in a regular examination room. Each patient wore a pair of lightweight, tightly fitting goggles equipped with a small video oculography camera to record and analyze eye movements. The patient was seated upright facing the wall 1.0 m away and instructed to focus on a static target on the wall. The examiner stood behind the patient and manually delivered 20 to 25 random, unpredictable, and passive head impulses of amplitude at 5° to 15°, peak velocity of 150° to 250° per second and a duration of 150 to 200 ms in the plane of each semicircular canal. Re-fixation corrective saccades (CS) were categorized by their appearance, as covert and overt. If the velocity of the CS exceeded 50° per second, they were considered significant. In this study, the cut-off values in VOR gain were 0.8 for the horizontal semicircular canal and 0.7 for the vertical semicircular canals. A pathological vHIT result referred to the combination of decreased gain and the presence of re-fixation saccades.
Pure-Tone Audiometry
Hearing tests were performed using air- and bone-conducted pure-tone audiometry (Otometrics, Taastrup, Denmark) at the start and 1 and 2 weeks and 1 month after treatment. The efficacy evaluation calculated the average at 250 and 500 Hz. Complete recovery was defined as hearing thresholds equal to or below 25 dB HL at all low frequencies below 500 Hz, while incomplete recovery was defined as hearing thresholds exceeding 25 dB HL at all low frequencies below 500 Hz.
Statistical Analysis
Statistical analysis was performed using statistical software SPSS version 22.0 (SPSS, Inc., Chicago, IL, USA). Univariate and multivariate binary logistic regression analysis was used to analyze the risk factors of incomplete recovery ALFHL. Chi-square tests and contingency coefficients were used to analyze the correlation between high abnormal VEMP and aural fullness, dizziness, and initial hearing loss. A P value <.05 was considered statistically significant.
Results
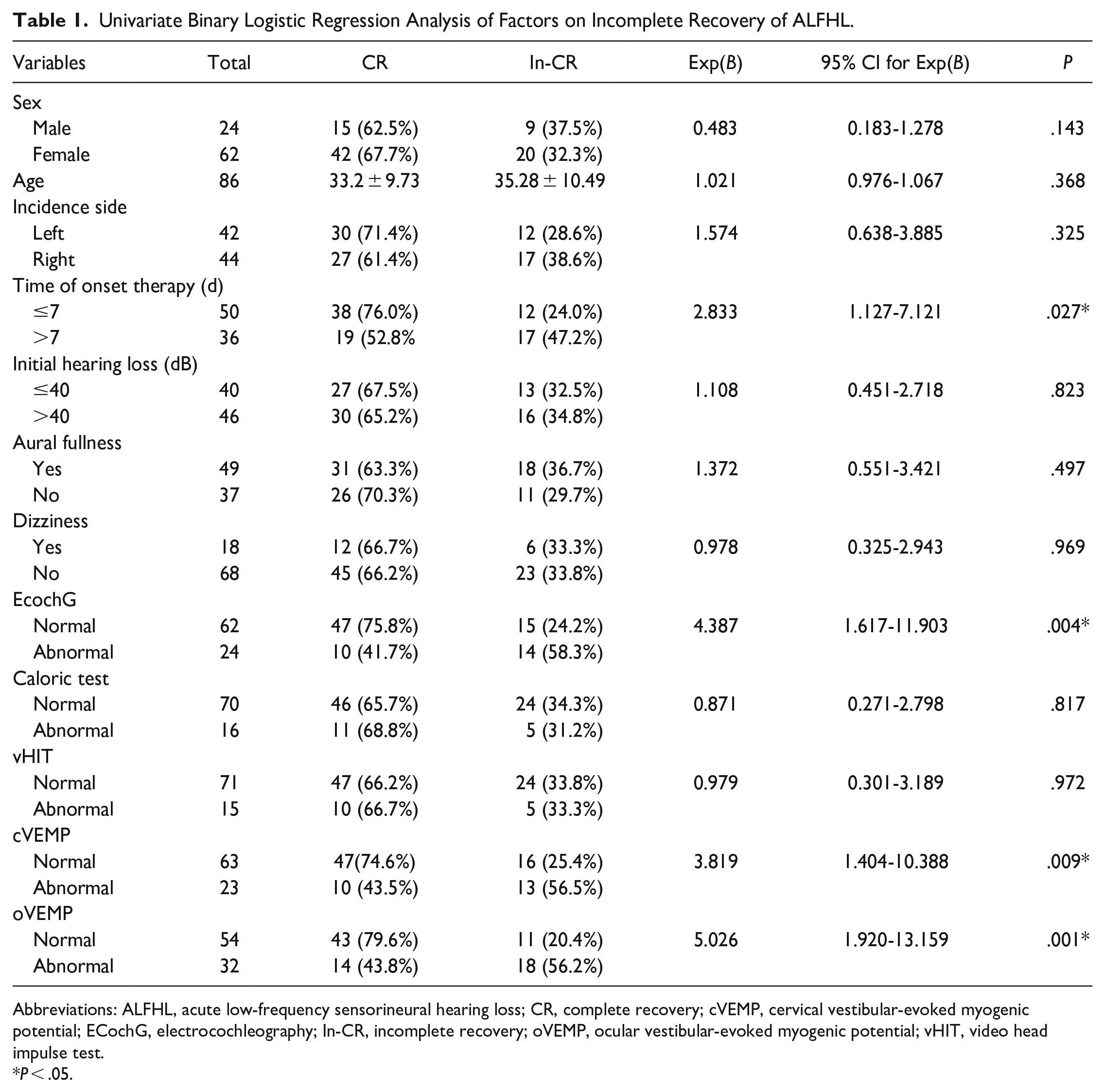
In this study, 57 out of 86 (66.2%) patients with ALFHL recovered completely, while 29 out of 86 (33.8%) did not fully recover. To investigate factors influencing adverse outcomes in ALFHL, variables such as EcochG, calorie test, vHIT, cVEMP, and oVEMP were analyzed, as well as sex, age, incidence side, time of onset therapy, initial hearing loss, aural fullness, and dizziness. Univariate logistic regression was used to analyze the prognostic factors affecting patients with ALFHL. The results showed that the incomplete recovery of ALFHL was not related to sex, age, incidence side, initial hearing loss level, aural fullness, and dizziness (Table 1).
Univariate Binary Logistic Regression Analysis of Factors on Incomplete Recovery of ALFHL.
Abbreviations: ALFHL, acute low-frequency sensorineural hearing loss; CR, complete recovery; cVEMP, cervical vestibular-evoked myogenic potential; ECochG, electrocochleography; In-CR, incomplete recovery; oVEMP, ocular vestibular-evoked myogenic potential; vHIT, video head impulse test.
P < .05.
The rate of incomplete recovery in ALFHL patients with initial treatment after 7 days (47.2%) was significantly higher than that of patients with initial treatment within 7 days (24.0%) (P = .027). The rate of abnormal EcochG in patients with ALFHL was 27.9% (24/86). In patients with abnormal EcochG, the rate of incomplete recovery was 58.3%, which was significantly higher than the rate of 24.2% observed in patients with normal EcochG (P = .004) (Table 1). The rate of abnormal caloric test in ALFHL patients was 18.6% (16/86), while the rate of incomplete recovery in ALFHL patients with abnormal caloric test (31.2%) was not significantly higher than the rate of 34.3% in ALFHL patients with a normal caloric test (P = .817) (Table 1).
The rate of abnormal vHIT in ALFHL patients was 17.4% (15/86), and the rate of incomplete recovery in ALFHL patients with abnormal vHIT (33.3%) was not significantly higher than that in ALFHL patients with normal vHIT (33.8%) (P = .972) (Table 1). The rates of abnormal cVEMP and oVEMP in patients with ALFHL were 26.7% (23/86) and 37.2% (32/86), respectively. In patients with abnormal cVEMP and oVEMP, the rates of incomplete recovery were 56.5% and 56.2%, respectively, which were significantly higher than the rates of 25.4% and 20.4% observed in patients with normal cVEMP (P = .009) and oVEMP (P = .001) (Table 1).
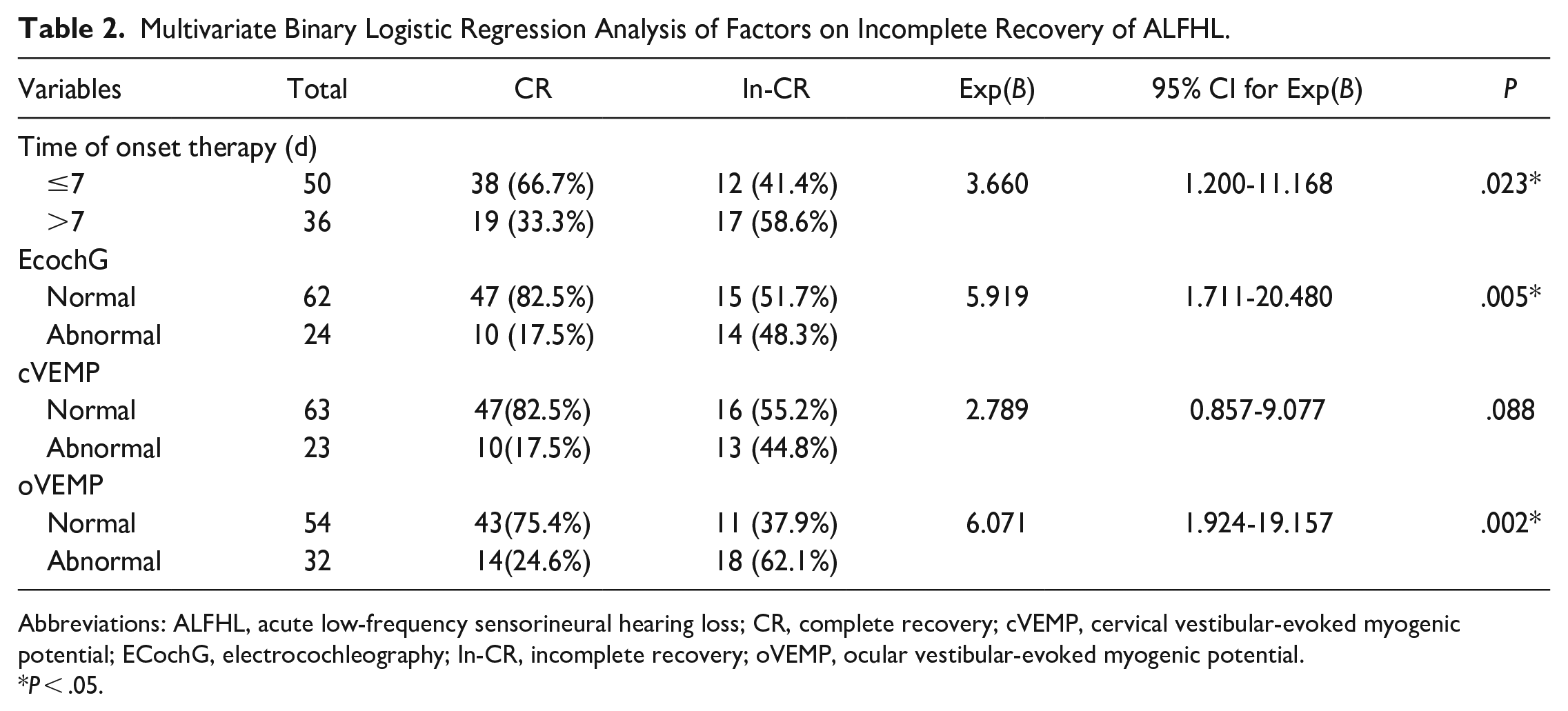
Time of onset therapy, cVEMP, oVEMP, and EcochG were next included in a multivariate binary logistic regression analysis. The results indicated that time of onset therapy, oVEMP, and EcochG were independent risk factors for incomplete recovery in ALFHL patients (Table 2). The risk of incomplete recovery in ALFHL patients with initial treatment after 7 days was 3.7 times higher than in patients with initial treatment within 7 days (Table 2). The risk of incomplete recovery in patients with abnormal oVEMP was 6.1 times higher than in patients with normal oVEMP (Table 2). The risk of incomplete recovery in patients with abnormal EcochG was 5.9 times higher than in patients with normal EcochG (Table 2).
Multivariate Binary Logistic Regression Analysis of Factors on Incomplete Recovery of ALFHL.
Abbreviations: ALFHL, acute low-frequency sensorineural hearing loss; CR, complete recovery; cVEMP, cervical vestibular-evoked myogenic potential; ECochG, electrocochleography; In-CR, incomplete recovery; oVEMP, ocular vestibular-evoked myogenic potential.
P < .05.
The high abnormal rate of VEMP as abnormal cVEMP or oVEMP in patients with ALFHL was analyzed for its correlation with initial hearing loss level, aural fullness, and dizziness. The results showed that there was no difference in the distribution of abnormal VEMP in ALFHL patients with or without aural fullness, dizziness, and different initial hearing levels (Table 3). A contingency coefficient test also showed that there was no correlation between abnormal VEMP and initial hearing level, or whether it was accompanied by aural fullness or dizziness (Table 3).
Distribution of Abnormal rate of VEMP in Initial Hearing Loss, Aural Fullness, or Dizziness.
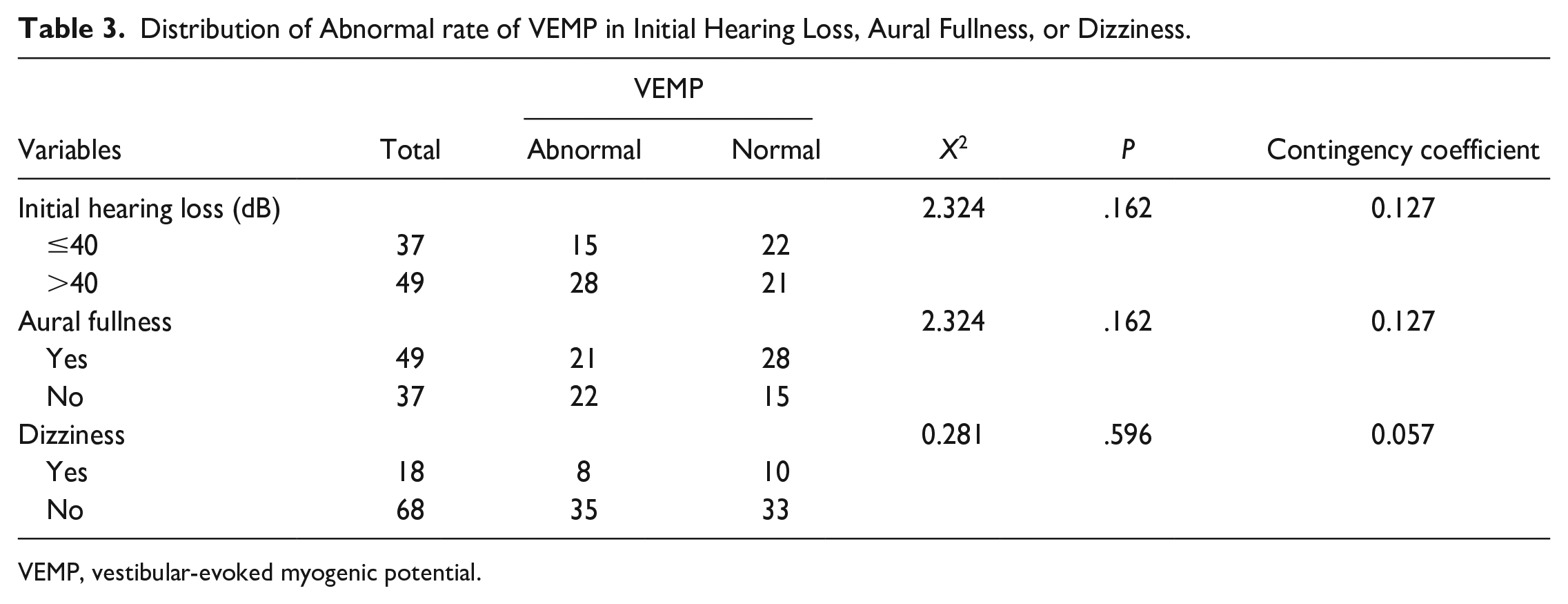

VEMP, vestibular-evoked myogenic potential.
Discussion
The condition of ALFHL shows a trend of either spontaneous recovery, or the majority of cases can completely recover after short-term treatment, 1 but approximately one-third of ALFHL do not completely recover within a short period.11,12 The potential pathophysiological mechanism leading to the incomplete recovery of this part of patients with ALFHL is still unclear. There is limited research on whether it is related to EH in the cochlea, sacs, and vestibule or related to impaired semicircular canal function. Therefore, this study investigated the relationship between the poor short-term prognosis of ALFHL and EH in the cochlea and vestibule, and semicircular canal dysfunction.
Fushiki et al 13 reported that the incomplete recovery rate of ALFHL after initial treatment was 37.1% and this study found that 33.8% of ALFHL patients did not completely recover after initial treatment. Previous studies have reported that age, hearing loss level, and initial treatment time influenced the prognosis of ALFHL, whereas sex, aural fullness, and dizziness do not have an impact on the prognosis of ALFHL,6,12 so these influencing factors were included in this analysis. This study found that there was no correlation between sex, age, hearing loss level, presence of aural fullness, dizziness, and incomplete recovery, but a significantly higher rate of incomplete recovery was found in ALFHL patients who received initial treatment after 7 days, as compared to those who underwent treatment within 7 days.
Im et al 14 reported that the ratio of EcochG abnormal values was 35.5% in patients with ALFHL, but Choi et al 12 found that EcochG values that were close to normal with only 1.6% abnormal values in patients with ALFHL. In this study, abnormal EcochG values were found in 27.9% of patients with ALFHL. It was reported that abnormal EcochG values were associated with an increased risk of progression to hearing fluctuation or MD. 15 Im et al 14 also reported a higher ratio of EcochG abnormality with increasing low-tone hearing loss. This study found that in ALFHL patients with abnormal EcochG values, the incomplete recovery rate of 58.3% was significantly higher than that in patients with normal EcochG at 24.2%. The risk of incomplete recovery in ALFHL patients with abnormal EcochG values was also 5.9 times higher than in patients with normal EcochG values. It has been reported that there is a correlation between an increase in the volume ratio of EH in the cochlea and the failure to cure ALFHL. 7 Additionally, abnormal EcochG indicated the presence of EH in the cochlea.8,14 Therefore, we speculate that the increased risk of incomplete short-term hearing recovery in ALFHL patients with abnormal EcochG may be associated with the difficulty of resolving EH in the cochlea.
A study reported that abnormal rates of caloric test and vHIT were 66.7% and 21.7% in ALFHL patients, respectively. 16 This study found that abnormal caloric test and vHIT existed in 31.4% and 17.4% of the patients with ALFHL, respectively and that the incomplete recovery rate in ALFHL patients with abnormal caloric test or vHIT was not significantly higher than that in ALFHL patients with a normal caloric test or vHIT. These results suggested that the incomplete recovery of ALFHL was not related to abnormal semicircular canal function.
A study of VEMP in ALFHL showed that the majority of patients with ALFHL exhibited normal VEMPs, with only 8% of abnormal values. 17 Im et al 14 also reported that the mean amplitude of VEMP on the low-tone sensorineural hearing loss side was not significantly different from the normal hearing side, but in this study, the abnormal rates of cVEMP and oVEMP in patients with ALFHL were 26.7% and 37.2%, respectively and the abnormal rate of VEMP either cVEMP or oVEMP was 50.0%. The abnormal rate of VEMP in ALFHL patients in this study was much higher than the reported abnormal rate of VEMP in the previous studies, which may be due to the smaller number of patients in these studies and the lack of analysis of the VEMP amplitude ratio and asymmetry.
Many studies on MD reported that EH was significantly associated with the disappearance of cVEMP.18,19 It had been reported that 54% of MD patients had an absence of cVEMP response to clicks on the affected side. 18 This study observed that absence of responses or a decreased VEMP amplitude existed in 50.0% of patients with ALFHL, which indicated that 50% of ALFHL patients may suffer from EH in the utricle or saccule.
A study of ALFHL reported that there was no significant correlation between the raw and corrected amplitudes of cVEMP and the hearing recovery of ALFHL. 20 This study observed that the incomplete recovery rates in ALFHL patients with abnormal cVEMP or oVEMP were significantly higher than that in patients with normal cVEMP or oVEMP and that the risk of incomplete recovery in ALFHL patients with abnormal oVEMP was 6.1 times higher than in patients with normal oVEMP. It has been reported that abnormal oVEMP indicates the presence of EH and degree of EH in the utricle in MD.21,22 Therefore, we speculate that ALFHL patients with abnormal oVEMP have a higher risk of short-term incomplete hearing recovery, which may be associated with severe and difficult-to-resolve EH in the utricle.
A previous study reported a correlation between aural fullness and high abnormal rates of VEMP 10 and another study also indicated that severe sensorineural hearing loss and dizziness were associated with abnormal VEMP. 23 This study further examined whether the high abnormal rate of VEMP in patients with ALFHL was correlated with the level of hearing loss, accompanied by aural fullness or dizziness. It was found that the high abnormal rate of VEMP in ALFHL patients was not correlated with level of hearing loss, accompanied by aural fullness or dizziness.
Conclusion
Our study suggested that abnormal oVEMP and EcochG value were the independent risk factors that affected the incomplete recovery of ALFHL, which may be related to the difficulty of successfully treating utricular and cochlear hydrops in patients with ALFHL. It was also concluded that the incomplete recovery of patients with ALFHL was not correlated with abnormal caloric test and vHIT, indicating that the incomplete recovery of ALFHL was not correlated with semicircular canal dysfunction. Moreover, abnormal VEMP was found in half of the patients with ALFHL, and a high abnormal rate of VEMP was not correlated with hearing loss level, aural fullness, or dizziness.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by Hospital Cultivation Program funded by the First Affiliated Hospital of Chongqing Medical University (2018PYJJ-02).
Ethics Statement
The study protocol was approved by the Ethics Committee of the First Affiliated Hospital of Chongqing Medical University. Informed consent was waived due to the retrospective nature of this study.
Data Availability Statement
All data from this study are available for retrieval and access.
