Abstract
Cosmetic rhinoplasties are complex surgical procedures that can present with serious complications requiring revision surgeries. Septal graft difficulties are common complications in rhinoplasties, requiring surgeon awareness of the potential future need for corrective surgery. Here, we report a case of multiple revision cosmetic rhinoplasties due to recurrent complications. Additionally, a review of the literature regarding cosmetic rhinoplasty complications and risk factors was performed.
Introduction
Cosmetic rhinoplasty is a common yet complex plastic surgery procedure that is constantly evolving to improve long-term cosmetic results without compromising the function of the nose. 1 Due to the intricacy of the procedure, complications may arise resulting in multiple revision surgeries. We report a case of a 55-year-old female who presented with severe complications after rhinoplasty, requiring multiple revision surgeries.
Case Report
A 55-year-old female presented with debilitating pain and discomfort from a cosmetic rhinoplasty performed by another surgeon two months prior. Since surgery, the patient had green-brown foul-smelling mucus and crusting from the nose with worsening nasal obstruction. On physical examination, she had dorsal irregularities, a 1.5 cm septal perforation, caudal septal deviation, columellar deviation, bilateral nasal valve collapse, and a retrusive maxilla. The patient was advised to return to her original surgeon for follow-up but returned in three months, citing she was accused of cocaine usage. At the 3-month visit, her perforation increased to 3 cm, and breathing remained obstructed (Figure 1). Columellar deviation, caudal septal deviation, and valve collapse three months after primary rhinoplasty with an outside surgeon.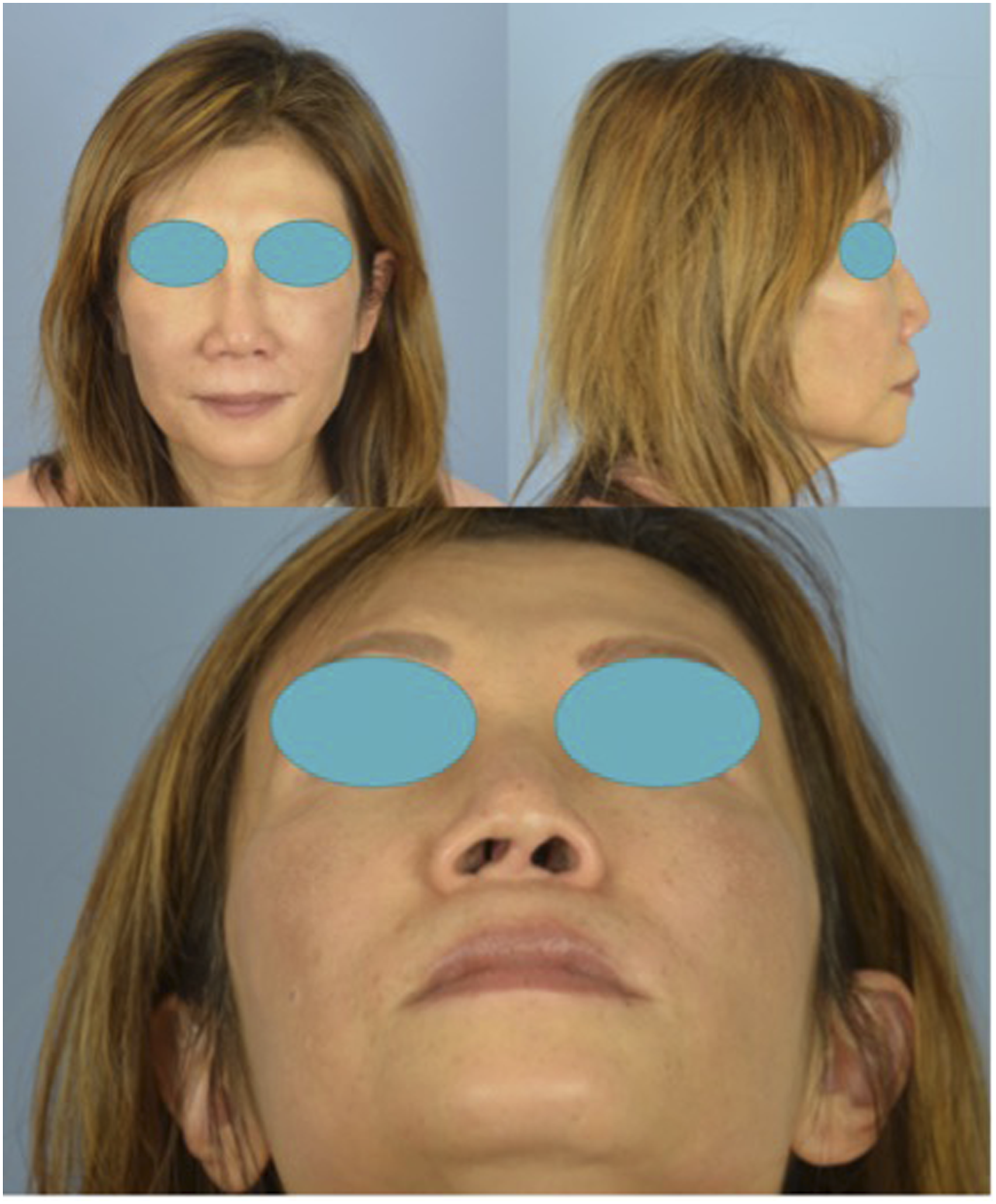
The patient was taken for revision surgery 6 months post-op. A revision septorhinoplasty with auricular cartilage grafting was performed. Severe fibrosis and scar tissue were encountered. The medial crura were fractured and knuckled, and her right lateral crus was truncated. Despite the patient’s septal perforation enlarging over time, there was still an adequate amount of septal cartilage posteriorly. Anteriorly, only 1 cm of the patient’s caudal strut still intact, though it deviated. Septal cartilage was harvested and used to make a caudal septal extension graft (CSEG), and this was fixated to the midline at the anterior nasal spine. To do this, 4-0 PDS was used to grab the periosteum of the nasal spine and then the CSEG. The native caudal septum was then fixated to the CSEG with a 5-0 PDS suture. The medial crura were secured to the CSEG via a tongue-in-groove maneuver to keep the tip midline.
At her 1-week post-op, the patient had improved breathing, symmetric nostrils, and a straight columella. At the 1-month post-op, the patient’s breathing remained good, but her columellar deviation and nostril asymmetry returned. The patient was adamant about having additional surgery to correct the deviation despite discussing the risks associated with poor blood supply at the base of the columella, including resorption of cartilage, loss of tip support, and poor healing.
Another revision surgery was performed 6 months after the first revision surgery. Intraoperatively, the patient’s old CSEG was noted to be thinner and more brittle compared to when it was first inserted. It was also no longer attached to the nasal spine. These likely occurred due to poor blood supply to the area, which most likely occurred after her initial surgery. The old CSEG was removed, and autologous rib was harvested and fashioned into bilateral extended spreader grafts with a new caudal septal replacement graft (CSRG). The graft was purposely made 5 mm longer than needed to account for any resorption that might occur. This time, a hole was drilled in the anterior nasal spine with K-wire. The CSRG was secured to this hole with 4-0 Prolene to ensure that it would not slip or move. The extended spreader grafts were secured on both sides of the CSRG so that the graft was fixated superiorly as well as inferiorly (Figure 2). Postoperatively, the patient had a straight caudal septum and columella and improved breathing. Intraoperative view showing bilateral extended spreader grafts and caudal septal replacement graft.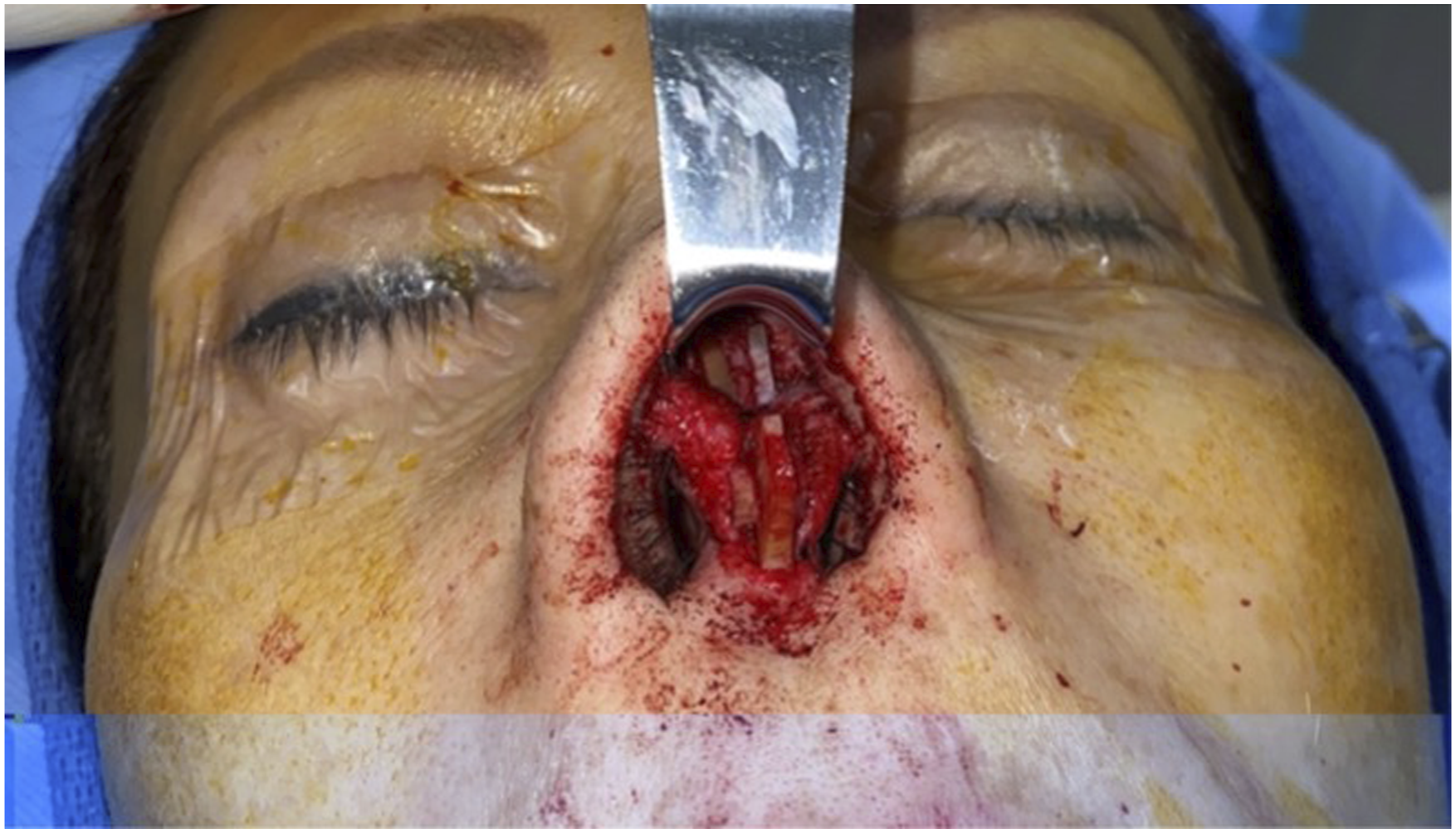
One month later, there was swelling and purulence along the left side of the columella leading to deviation. A culture was obtained, and the patient was placed on antibiotics. This grew methicillin-susceptible Staphylococcus aureus (MSSA), and fortunately, the infection resolved without negatively affecting her surgical results.
Discussion
Cosmetic rhinoplasties are multifaceted surgeries that may have serious complications that require revision procedures. Many complications may arise due to surgical error, improper diagnosis, variation in patients’ anatomy, overaggressive surgical removal, or poor patient post-operative compliance. 2 According to a study conducted by Neaman et al., of their 369 patients who had cosmetic rhinoplasty, 7.9% developed post-surgical complications and 9.8% required surgical revision. 3
Moreover, nasal tip reconstruction is crucial in many revision rhinoplasties but can have the potential for high rates of complications. Caudal septal extension grafts (CSEG) can be used in patients with a contracted nose to provide nasal tip support and projection. A retrospective review of 44 consecutive patients who underwent nasal tip reconstruction with a septal extension graft showed 45.5% of patients developing nasal tip stiffness and decreased projection, 11.4% developed nasal deviation, and 4.5% developed infections. 4
In this case, the patient’s retrusive maxilla and septal perforation from her first surgery most likely contributed to her poor baseline blood supply to the caudal septum. This then predisposed her to resorption of her CSEG after her first revision surgery and infection after the second revision. What is unique about this case is the degree to which the blood supply of the caudal septum and columella (septal and columellar branches of the superior labial artery) was compromised from her initial rhinoplasty. Thus, surgeons must be vigilant of this and other possible complications during cosmetic rhinoplasties, inform patients of the potential need for revision procedures and be prepared to address these complications appropriately.
Conclusion
Rhinoplasties are complex procedures in plastic surgery that require the preservation of functionality of the nose while improving cosmetic outcomes. Complications are common and can result in detrimental effects on form and function. As such, revision surgeries are frequently performed but present unique challenges based on the results and sequelae of prior surgery. Surgeons need to be adept at recognizing and addressing multiple issues and complications that can result from rhinoplasty.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
