Abstract
Tapia’s syndrome is considered a neuropraxic injury of the recurrent laryngeal nerve and hypoglossal nerve which commonly presents after postoperative general anesthesia as hoarseness and dysphagia. Clinicians should consider this diagnosis in those presenting with symptoms of cranial nerve X and cranial nerve XII injury in the post-extubation setting for prompt diagnosis and management. Here, we report a rare case of Tapia’s syndrome following cardiac surgery which was then treated with carboxymethylcellulose gel implant injection.
Keywords
Introduction
Tapia’s syndrome was coined by Spanish Otolaryngologist Antonio Garcia Tapia in 1904 and describes symptoms of hoarseness and dysphagia believed to be caused by mechanical trauma to cranial nerves (CN) X and XII. 1 The theoretical etiology can be described as compression from intubation with flexion of the neck imposing the ramus of the mandible on the anterior branch of the recurrent laryngeal nerve and hypoglossal nerve.2-4 In Tapia’s syndrome, neuropraxia due to stretch or crush type injury is generally treated with steroids 4 ; multiple studies also suggest speech language therapy (SLT) improves prognosis within 3 to 6 months. 5
We present a unique case of Tapia’s syndrome following aortic valve replacement (AVR) and coronary artery bypass grafting (CABG) which was treated with SLT and vocal cord injection of carboxymethylcellulose gel implant, leading to partial recovery of function. We additionally provide a review of literature and previously documented cases of Tapia’s syndrome to summarize contemporary diagnosis and management of this condition.
Case Report
A 70-year-old male with a past medical history of aortic valve disease, coronary artery disease, hyperlipidemia, and hypertension underwent AVR and CABG. He was placed in supine position, was administered general anesthesia, and was intubated orotracheally. He tolerated the procedure well, and was transferred to the surgical intensive care unit (SICU) postoperatively in stable condition.
Upon admission to the SICU, his exam was notable for a normal neurologic exam with intact cough and gag reflexes and an endotracheal tube in place. He was quickly weaned off sedation and extubed to nasal cannula oxygen. Following extubation, the patient noted hoarseness in his voice. This hoarseness continued, and on postoperative day 4, Otolaryngology was consulted.
Patient was found to have a tongue deviation to the left with protrusion (Figure 1A) and mild difficulty swallowing. Flexible laryngoscopy showed left vocal cord immobility lying in the paramedian position and a fair glottic gap with attempted adduction. Modified barium swallow was performed by SLT, which showed mild oral and moderate pharyngeal dysphagia with aspiration of thin and nectar thick liquids. A computerized tomography (CT) scan of the neck was performed and showed mild prominence of the left base of the tongue without discrete mass. Given the above symptoms and evaluation, the patient was diagnosed with Tapia’s Syndrome. Patient was discharged with follow-up of Otolaryngology and SLT. (A) Initial left sided hemiplegia of tongue on protrusion; (B) Left deviation of tongue with protrusion about 90% back to midline at 9 month follow-up.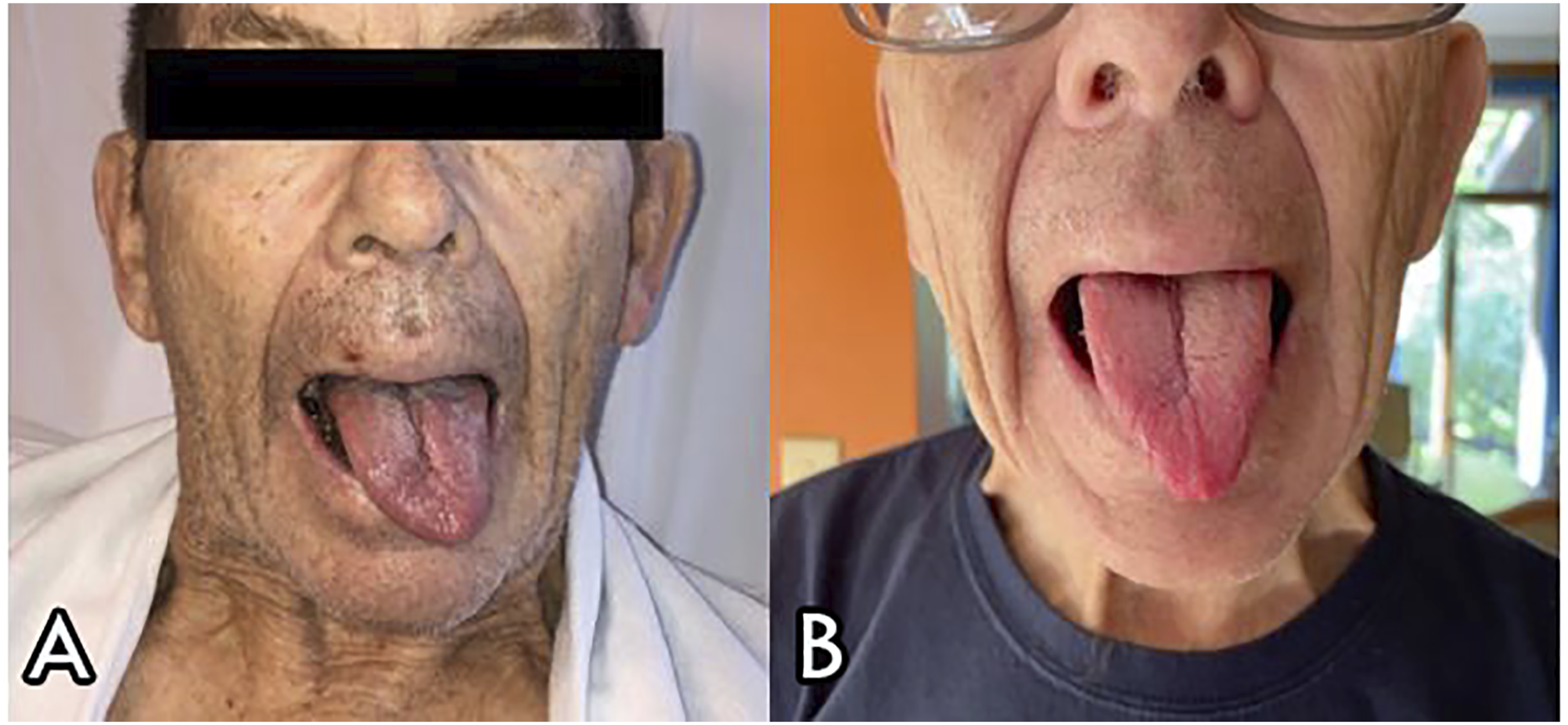
At a 3 week follow-up visit with Otolaryngology (postoperative day 29), the patient reported continued symptoms. Decision was made for vocal cord injection with carboxymethylcellulose gel implant which occurred 1 week later (on postoperative day 36). Patient was injected with 1.0 cm3 of the implant into the left vocal cord at the level of the vocal process and just anterior at the superior arcuate line (Figure 2A). (A) Post-operative carboxymethylcellulose gel implant injection and medialization of left true vocal cord; B & C) Slight weakness of left true cord along with mild atrophy at 9 month follow-up.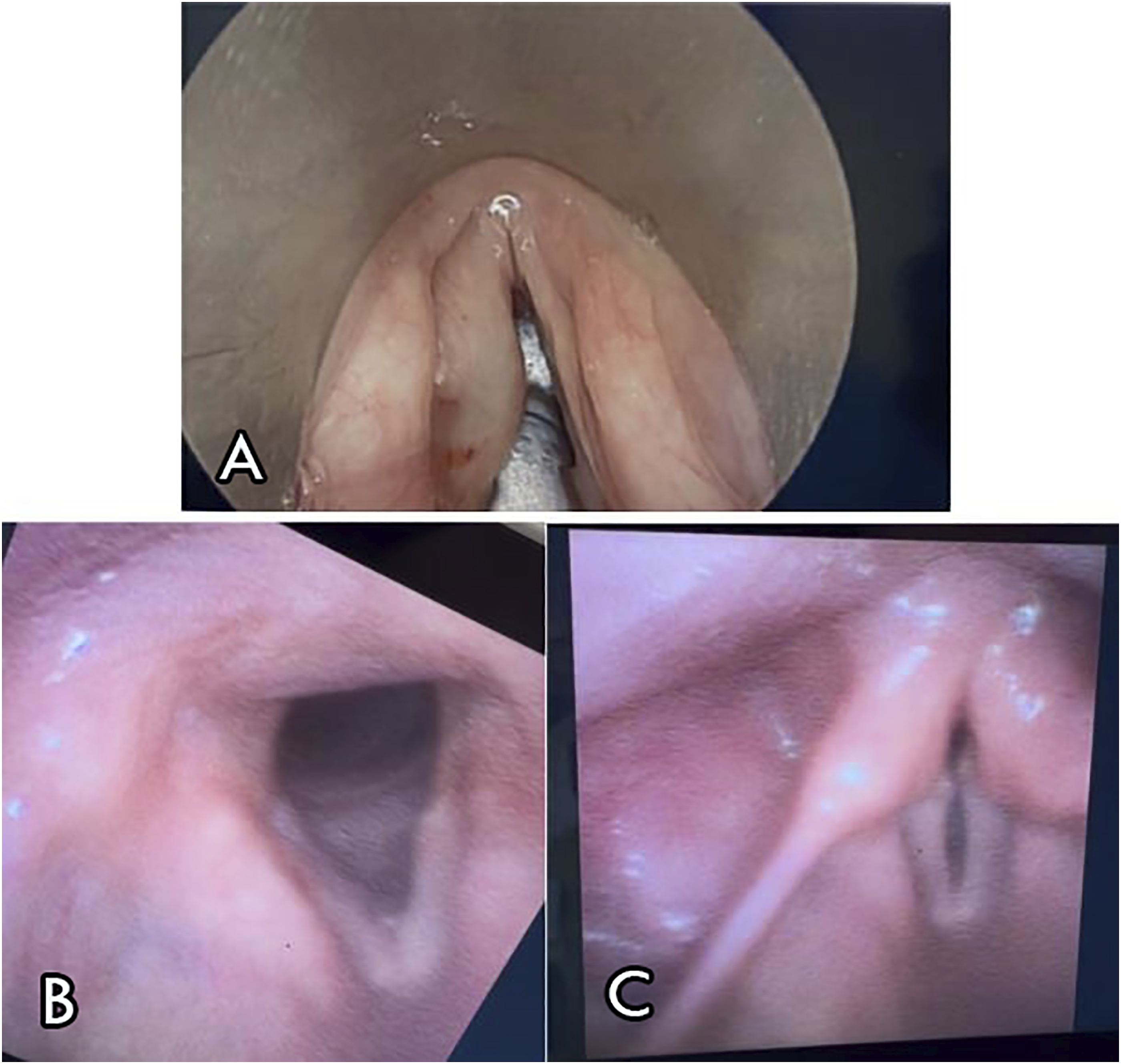
Modified barium swallow was re-performed 1 week following vocal cord injection, which showed no penetration or aspiration with independent swallow. He was then cleared by SLT for a regular diet with thin liquids, and continued with outpatient swallow and voice therapy.
The patient then followed up with Otolaryngology 6 months later, at which time he reported mild gradual improvement in his voice quality. Flexible laryngoscopy was performed, and showed continued left vocal cord paralysis with the vocal cord fixed in the near median position with near complete glottic closure, with no frank aspiration of saliva or pooled saliva. At this point, the patient elected for observation moving forward. Patient was again re-examined at 9 months postoperative with tongue protrusion about 90% back to midline (Figure 1B) and slight weakness of left true cord along with mild atrophy (Figure 2B and C).
Discussion
Tapia’s Syndrome Literature Review of Cases.
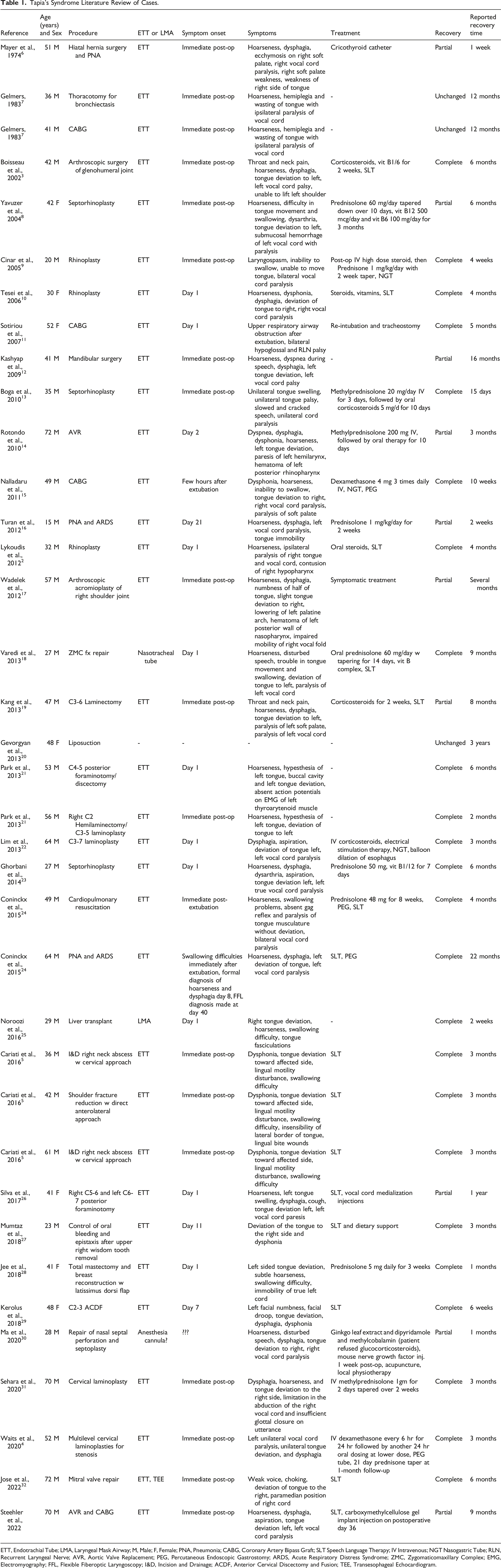
ETT, Endotrachial Tube; LMA, Laryngeal Mask Airway; M, Male; F, Female; PNA, Pneumonia; CABG, Coronary Artery Bipass Graft; SLT Speech Language Therapy; IV Intravenous; NGT Nasogastric Tube; RLN, Recurrent Laryngeal Nerve; AVR, Aortic Valve Replacement; PEG, Percutaneous Endoscopic Gastrostomy; ARDS, Acute Respiratory Distress Syndrome; ZMC, Zygomaticomaxillary Complex; EMG, Electromyography; FFL, Flexible Fiberoptic Laryngoscopy; I&D, Incision and Drainage; ACDF, Anterior Cervical Discectomy and Fusion; TEE, Transesophageal Echocardiogram.
The wide variety of cases in the literature in which Tapia Syndrome was found hints to multiple possible underlying etiologies. Incorrect laryngoscope use, overinflation of the endotracheal tube cuff, neck hyperextension, and prolonged packing of the throat. 27 Tapia’s syndrome has also been shown by use of a laryngeal mask airway (LMA) 25 and nasotracheal intubation. 18 Cranial nerve XII, in relation to LMA use, runs in close proximity to the greater horn of the hyoid, at the location of the superior portion of the LMA. 33 In addition, CN XII and CN X both course closely together at the level of the first cervical vertebra.17,34
Patients with Tapia Syndrome present in the acute postoperative setting. The initial evaluation of the patient should include a thorough head and neck physical exam to differentiate between central and peripheral lesions. Boga et al. described a classification system of Tapia syndrome, termed the Aktas and Boga Classification, that represents the array of symptomatology seen depending on the severity of nerve injury. Grade I (mild type) consists of unilateral cord and tongue paralysis, no uvula distortion, minimal slowdown in speaking, no tongue swelling and lack of dysphagia. Grade II (moderate type) consists of unilateral cord and tongue paralysis, no uvula distortion, mild slowdown in speaking, tongue swelling, pharynx dryness, dysphagia, cracked speech and normal feeding and drinking. The most severe type, grade III, consists of unilateral cord and tongue paralysis, uvula distortion, dysarthria, tongue swelling, dryness in the pharynx, dysphagia, and difficulties with both feeding and drinking. 13
Management of Tapia syndrome is theorized in some cases as treatment of neuropraxia (e.g., stretch or crush type injury)—often involving steroids. 4 Boga et al. grading scale suggests corticosteroids and IV corticosteroids for grades II and III, respectively. 13 For grade I cases, supportive treatment and close follow-up is recommended. Supportive treatment can be composed of anti-inflammatory drugs and warm air inhalation, with most cases resolving in 4–6 months. Literature also shows the advantages of interdisciplinary care and the role of speech language pathology to hasten recovery and prevent adverse outcomes. 5
Outside of our study, there is only 1 other case reported in the literature with follow-up of a patient that underwent vocal cord injection. Silva et al. had a partial recovery after 1 year with excellent vocal cord closure and normal voice despite continued paralysis of unilateral true cord. Our patient also did not experience a complete recovery; however, we believe the vocal cord injections assisted in resolving comorbidities associated with penetration and aspiration risk inherent to Tapia’s syndrome.
Lykoudis et al. described several preventive measures that have been discussed in previous reviews of Tapia Syndrome, including careful head and neck maneuvers during intubation, gentle intubation with the laryngoscope, proper cuff inflation, proper tube fixation to decrease excessive tube motion, and careful positioning of throat packing. 2
Conclusion
Reported cases of Tapia’s syndrome are rare; however, it is important to recognize the common presenting signs, symptoms, and management of Tapia syndrome, along with potential preventative techniques. The clinician should consider this diagnosis in those presenting with symptoms of CN XII and CN X neuropraxia in the postoperative or post-extubation setting as prompt diagnosis and management are warranted. Vocal cord injection is a safe procedure in managing Tapia’s syndrome to prevent comorbidities of vocal cord paralysis.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
