Abstract
Objectives:
Nasal septal surgery is one of the most common surgical procedure performed by otolaryngologists. Nasal packs are used for bleeding control, prevention of septal hematoma, replacement of mucoperichondrial flaps, and stabilization of the septum after nasal septal surgery. The aim of this study was to investigate the effects of albumin-glutaraldehyde–based tissue adhesive (Bioglue), which can be used as an alternative to nasal pack on the nasal septum after experimental nasal septum surgery.
Methods:
A total of 16 female Wistar albino rats were randomly separated into the study group (n = 10) and the control group (n = 6). After raising the mucoperichondrial flap on one side of the septum, Bioglue was used to fix the mucoperichondrial flap over the septal cartilage ın the study group and nasal packs (Merocel) were used for fixation in the control group. The rats were sacrificed at 2 and 4 weeks after septoplasty. All the tissue samples were evaluated under light microscope by the same pathologist in respect of foreign-body reaction, degree of inflammation, granulation tissue, fibrosis, cartilage damage, and cilia and goblet cell damage. In the control group, the Merocel packs were removed after 2 days and the groups were compared in terms of hematoma.
Results:
No hematoma was observed in any group. Septal perforation was determined in all the study group participants and loss of cilia and goblet cells and foreign-body reaction were found in 8 samples of the study group participants and in none of the control group.
Conclusions:
The results of this study show that Bioglue caused segmental cartilage injury; therefore, it may not suitable for use following septal surgery.
Introduction
Nasal septal surgery is one of the most common surgical procedure performed by otolaryngologists. Various nasal packs are used, such as Merocel, fingerstall packs, alginate, industrially medicated or impregnated gauze packs, Telfa, foam, polyethylene oxide gel, cellulose, absorbable gelatin sponges, Fucidin gauze wrapped in wax paper, and fatty tissue of slaughtered pigs for bleeding control, hemostasis, prevention of hematoma, synechiae, or restenosis, closure of dead space and stabilization of the cartilaginous-bony skeleton of nose after nasal septal surgery. Nasal packing may cause complications such as bleeding, mucosal injury, foreign-body reaction, removal and aspiration of the packing material, allergy, hypoxia, postoperative infection, toxic shock syndrome, and cardiovascular changes. 1,2 One of the most common problem encountered after septoplasty is discomfort during removal of the nasal packs. 3 Tissue adhesives, which may be synthetic or biological, are used in surgery to promote hemostasis, wound healing, and tissue adhesion. Synthetic tissue glues are mainly derived from cyanoacrylate and biological glues from fibrin adhesives. Cryolife BioGlue Surgical Adhesive (Cryolife, Inc) is the only tissue adhesive agent formed by combination of both synthetic and natural reagents. As it is made from bovine albumin and glutaraldehyde, it is classified as an animal-based sealant and has been used since 2001 with Food and Drug Administration approval. 4 The Bioglue is composed of 10% glutaraldehyde and 45% purified bovine serum albumin. Glutaraldehyde exposure binds lysine molecules of bovine serum albumin, cell-surface proteins, and extracellular matrix proteins to each other. The polymerization of this adhesive starts after 20 to 30 seconds, and full bonding strength is reached in 2 minutes. 5,6 Bioglue has both synthetic and biological features and has been used successfully in various fields. The aim of this study was to investigate the effectiveness of Bioglue as an alternative to nasal tampon in experimental septum surgery in rats.
Materials and Methods
The study was conducted in the Animal Research Laboratory of tertiary center clinic. Experiments were conducted in accordance with the principles of the Helsinki Declaration on the use of laboratory animals. A total of 16 female Wistar albino type rats aged 8 to 10 months and each weighing 220 to 275 g were used in the study, randomly separated as the study group (n = 10) and 6 rats as control group (n = 6). All the rats were kept under the same laboratory conditions and fed the same diet. Anesthesia was applied to all animals with an intramuscular injection of 30 mg/kg ketamine hydrochloride before the operation. Antibiotic prophylaxis of 10 mg/kg cefazolin Na was injected intramuscularly preoperatively. The operation site was wiped with povidone-iodine (Betadin). A surgical microscope (SHIN-NIPPON OP-2) was used for better visualization of the surgical field. First, an infiltration of 0.1 to 0.2 mL of 2% lidocaine hydrochloride + 1: 80-000 epinephrine (Jetokain) was applied to the columella and septum, and following the transcolumellar incision, the septum was visualized. Unilateral mucoperichondrial flap elevation was performed under the microscope. Since mucoperichondrial flaps are very thin in rats, those with severe mucosa and cartilage damage were excluded from the study. Bioglue was applied to the septum of the rats in the study group after unilateral mucoperichondrial elevation, and the mucoperichondrium was fixed to the septum. In the control group after unilateral mucoperichondrial elevation, the mucoperichondrium was laid on the septum and a Merocel pack was placed on it. All the operations were performed by the same surgeon. Transcolumellar incisions were sutured with 4-0 multifilament polyglactin 910 (Vicryl). In the control group, the Merocel packs were removed after 2 days. On postoperative day 2, the groups were compared in terms of hematoma. In the second week, 6 rats from the study group and 3 from the control group were sacrificed by high-dose intracardiac ketamine hydrochloride injection. At the end of week 4, the remaining 4 rats in the study group and 3 in the control group were sacrificed in the same way. Tissue samples were taken from the mucoperichondrium and septum for histopathological examination. The tissue samples were stored in formaldehyde solution, then stained with hematoxylin and eosin in the pathology laboratory. All the tissue samples were evaluated under light microscope by the same pathologist in respect of hematoma formation, foreign-body reaction, degree of inflammation, granulation tissue, fibrosis, cartilage damage, and cilia and goblet cell damage. The score of the degree of inflammation ranges from 0 to 3 (0: absent, 1: mild, 2: moderate, 3: severe), and all other parameters were score as 0 = no or 1 = yes.
Results
The Merocel packs were removed from the control group rats on postoperative day 2. The histopathological results obtained in week 2 are provided in Table 1, and those obtained in week 4 are given in Table 2.
Histopathological Examination Results of Both Groups in Week 2.a
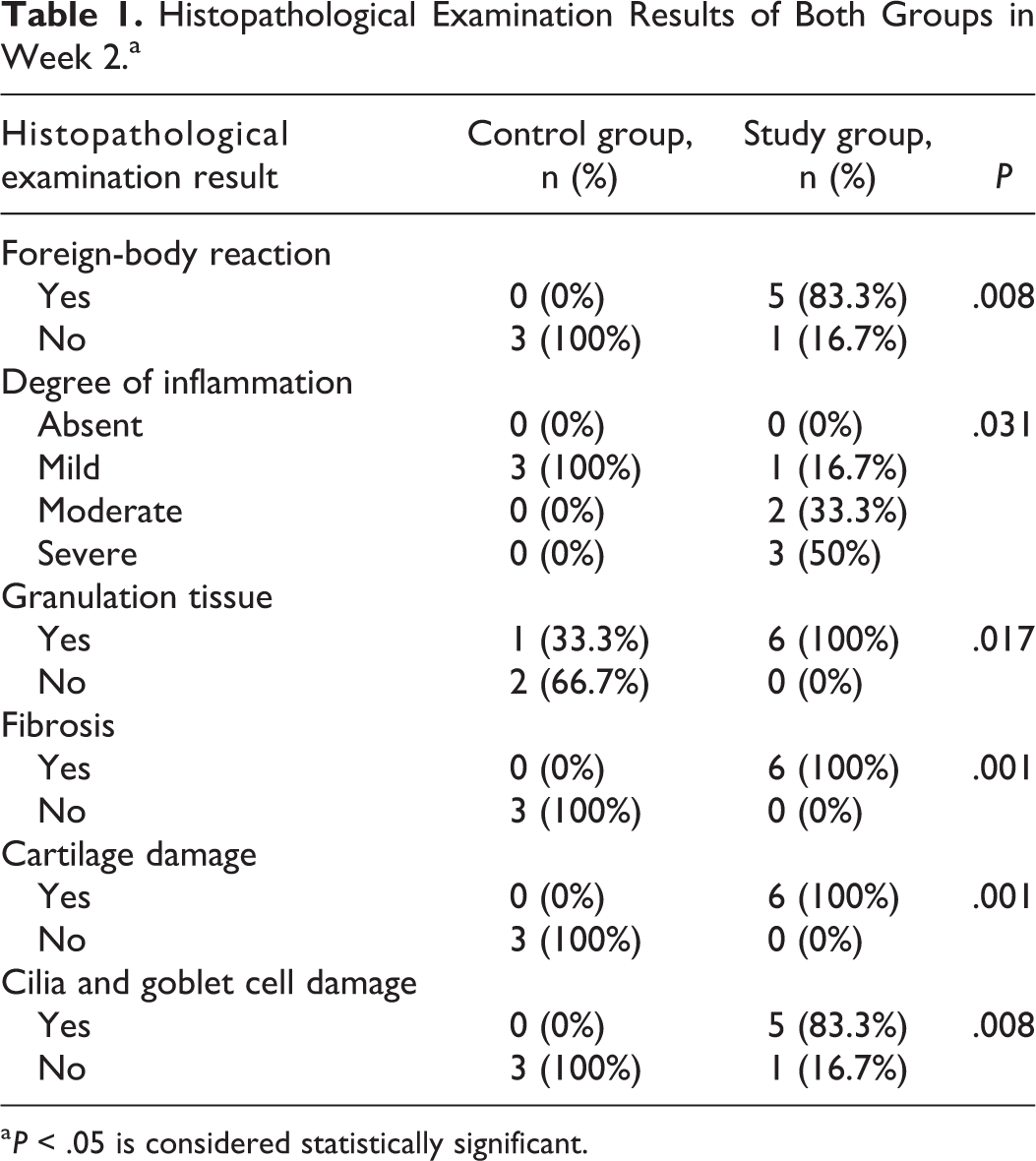
a
Week 4 Results.a
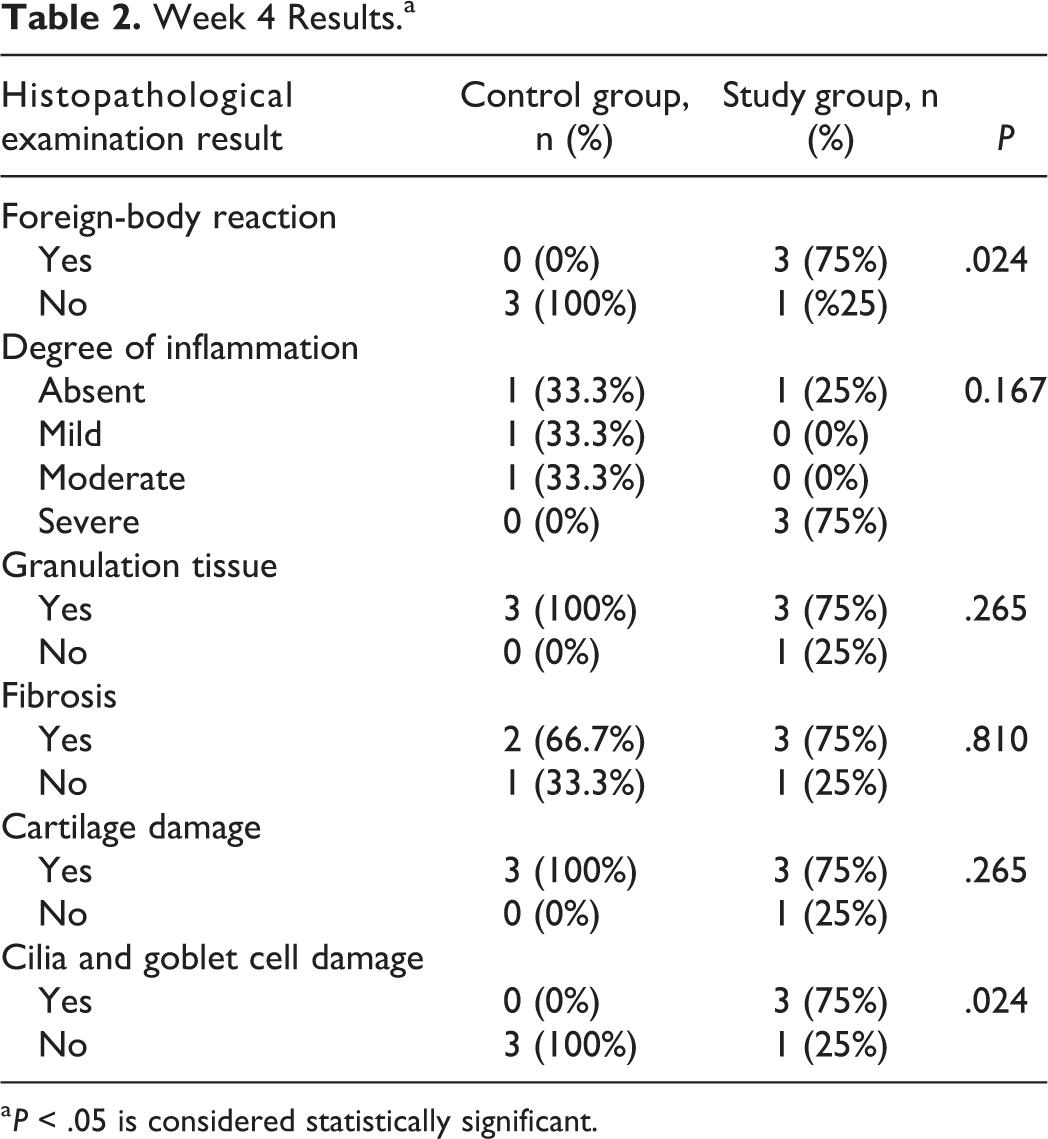
a
Hematoma
On postoperative day 2, all animals in both groups were examined and no hematoma was determined in any case.
Degree of Inflammation
In the samples taken in week 2, the degree of inflammation was significantly lower in the control group (
Granulation Tissue
Granulation tissue was observed in only 1 of the control group biopsies taken in week 2. Granulation tissue was observed in all the biopsies taken from the study group in week 2, and this difference between the 2 groups was statistically significant (
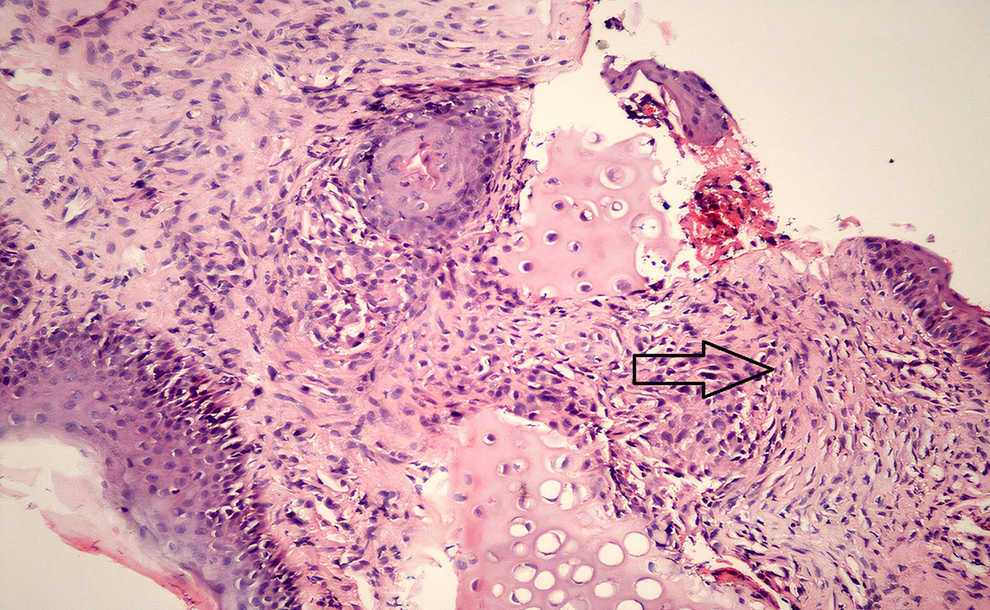
Study group: Tissue sample obtained at week 2. Histopathologic examination shows granulation tissue. Hematoxylin and eosin ×100.
Fibrosis
Fibrosis was observed in all the study group participants and in none of the control group in week 2. This difference between the 2 groups in terms of fibrosis formation was statistically significant (
Cilia and Goblet Cell Damage
Cilia and goblet cell damage was not observed in any of the control group participants in the 2- and 4-week biopsies in the control group. Cilia and goblet cell damage was observed in 8 cases in the study group. Cilia and goblet cell damage was determined to be significantly lower in the control group (
Foreign-Body Reaction
Foreign-body reaction was observed in 8 cases in the study group and in none of the control group in the 2- and 4-week biopsies (Figure 2). In terms of the frequency of foreign-body reaction, the difference between the control and study groups was found to be statistically significant (
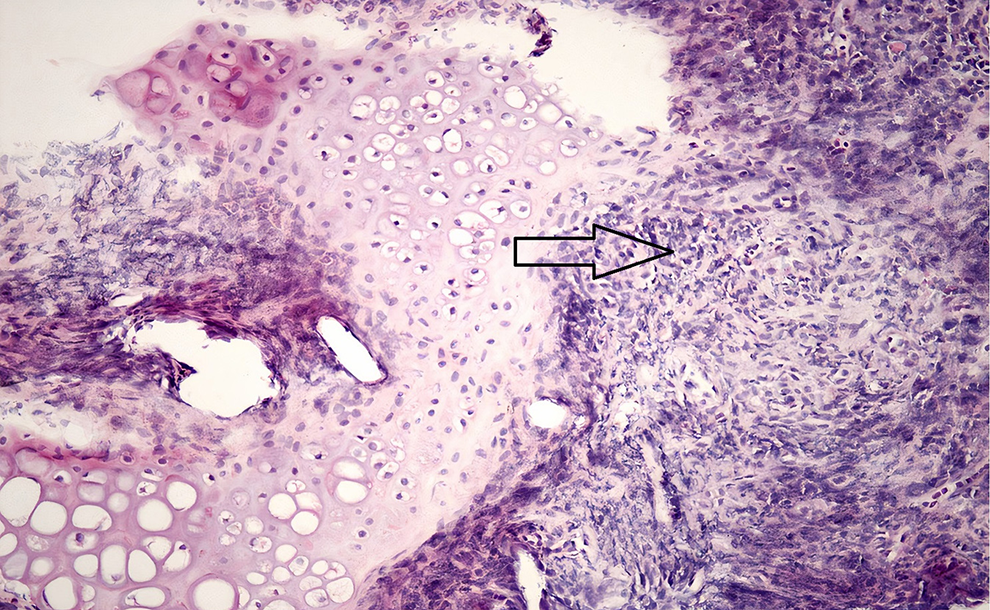
Study group: Tissue sample obtained at week 2. Histopathologic examination shows foreign-body reaction. Hematoxylin and eosin ×100.
Cartilage Damage
Cartilage damage was observed in all cases in the study group and in none of the control group in week 2 (Figure 3). Cartilage damage was significantly lower in the control group (
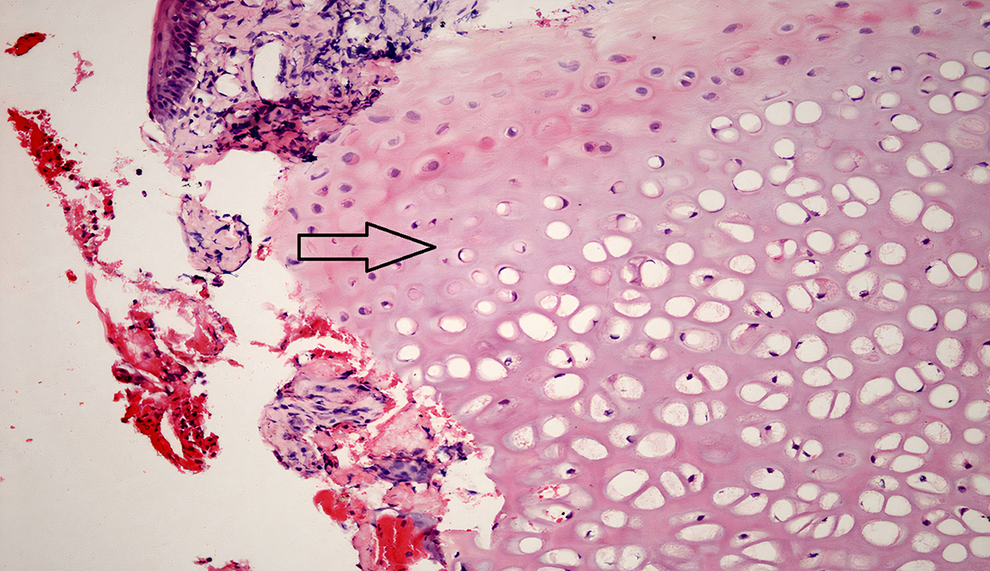
Study group: tissue sample obtained at week 2. Histopathologic examination shows cartilage damage. Hematoxylin and eosin ×100.
Septal Perforation
Septal perforation was observed in all the study group participants and in none of the control group.
Fibrosis, cartilage damage, cilia goblet damage, and the degree of inflammation in only 1 tissue sample in the study group could not be evaluated because the tissue was insufficient and was considered absent. However, a foreign-body reaction was observed in this tissue sample, and a large perforation was detected in the septum while the tissue sample was taken.
Statistical Analysis
The results of the histopathological examination in both groups were examined with the likelihood ratio χ2 test. The results were evaluated in a 95% CI, and differences were considered statistically significant at
Discussion
Septal surgeries are common operations in otorhinolaryngology. Severe complications such as bleeding, hematoma, infection, abscess formation, and perforation can be seen after septal surgery. Nasal packing, septal splints, and quilting sutures are used to prevent these complications. Recently, tissue adhesives have been used to prevent complications in septal surgery. 7 There are reports ın the English literature of the successful use of tissue adhesives N-butyl cyanoacrylate and fibrin glue in septum surgery. Alkan et al 8 used N-2-butyl cyanoacrylate in the fixation of nasal septum to the anterior nasal spine in rabbits in experimental study. They demonstrated that N-2-butyl cyanoacrylate was successful in the fixation of the caudal edge of the nasal septum to the anterior nasal spine, with no serious infections, foreign-body reaction, necrosis, or histotoxicity. Aksoy et al 9 used N-butyl cyanoacrylate on nasal septal tissues after septal surgery in a rabbit model. They showed that the use of N-butyl cyanoacrylate resulted in hypocellularity and empty lacuna segments in newly formed cartilage tissue, at both week 4 and week 12. They suggested that in early period of surgery, N-butyl cyanoacrylate had minimal negative effect on cartilage cells and with time this negative effect decreased. They demonstrated that postoperative inflammation levels, granulation tissue formation, foreign-body reaction, cellular characteristics of bone and cartilage regrowth, and complication rates were acceptable.
Habesoglu et al 10 reported that fibrin glue had an adequate hemostatic effect and promoted the regeneration of mucociliary activity of the injured mucosa postoperatively and ıt can be used in septoplasty with no gross complications. Vaiman et al 11 showed that fibrin sealant by aerosol spray in endonasal surgery was more effective and convenient than nasal packing.
We aimed to use Bioglue as a tissue adhesive in experimental septum surgery as an alternative to nasal tampon. Bioglue is mostly used successfully as a tissue sealant for thoracic, 12 -15 cardiovasculer, 16 -19 neuro, 20,21 plastic, 22 general, 23 -27 ophthalmological, 28 and urological 29 -31 surgery. As in the current study, there are also studies that have found Bioglue to be ineffective; LeMaire et al 32 used Bioglue in aortic anastomosis and observed severe fibrosis and stenosis in pathological examinations. They recommended that Bioglue should not be used on cardiovascular anastomoses in pediatric patients. In the present study, although all the study group had fibrosis, it was not observed in the control group in week 2. In the control group, fibrosis was observed to be minimal and the difference between the groups was not significant in week 4. Bernabeu et al 33 reported limb ischemia as a result of embolism in 2 cases after repair of aortic dissection with Bioglue. Fatal right ventricular infarction due to Bioglue embolization has been shown in the literature. 34 LeMaire et al 35 reported that acute nerve damage and diaphragm paralysis are due to Bioglue contact with the phrenic nerve in a pig model. Hurby et al 36 used Bioglue on the suture line in vesicourethral anastomosis and reported that it prolonged the operation time and did not increase the quality of anastomosis compared to suture only. In another clinical study, Bioglue was instilled into the fistula tract of a high transsphincteric fistula while transanal advancement flap operation was performed, but complications such as severe pain, purulent discharge, and abscess were observed. 37 Abbas and Tejirian 38 used Bioglue cases with complex anal fistula and reported acute sepsis in 4 of 6 patients and fistula was not closed in any of the patients. Rasul et al 39 reported that delayed spinal cord compression secondary to Bioglue induced granuloma and recommended judicious use of Bioglue. Woo et al 40 presented pulmonary artery rupture after 3 months of cardiac surgery is due to the cytotoxic effects of Bioglue. Singh et al 41 reported a case of sterile abscess formation 9 months after carotid endarterectomy following the use of Bioglue. Fife et al 42 used Bioglue for inferior vena cava repair during endometrial cancer staging in 2 cases. They detected foreign-body reaction to Bioglue may look like a cancer recurrence on imaging. They recommended that it is important to note prior use of vessel sealants in assessing para-aortic recurrence. No data could be found in the English literature related to Bioglue use in septum surgery. There is a limited number of studies on the use of Bioglue in otolaryngology practice. Friedman and Schalch 43 used Bioglue successfully in medialization of the middle turbinate. Sen et al 44 used Bioglue for dural and middle ear closure in translabyrinthine vestibular schwannoma surgery. However, an unacceptably high incidence of cerebrospinal fluid leakage (62.5%) was determined and ıt was recommended that Bioglue is not used in translabyrinthine vestibular schwannoma surgery. Chen et al 45 used Bioglue for vocal fold wound closure. They compared Tisseel, Bioglue, and Glubran 2 surgical adhesives for adhesive strength and the cytotoxicity. Tisseel was found to be the least toxic of the 3 adhesives, while Glubran 2 was the most toxic. They concluded that Bioglue’s biocompatibility was tissue specific and their viability results showed it may not be vocal-fold tissue friendly. In the current study, septal perforation was determined in all the study group participants and loss of cilia and goblet cells and foreign-body reaction were found in 8 samples of the study group participants.
Erkan et al 46 used fibrin glue in experimental septum surgery in rabbits. In the evaluation of histopathological tissue samples, complications such as cilia and goblet cell damage, mucosal damage, decreased perichondrium and cartilage thicknesses, distinctive inflammation, and segmental cartilage loss were observed. They found that it may be unwise to use fibrin glue in septal surgery to fix mucoperichondrial flaps in humans as well. The results of this study are similar to those of our study. In our study, ın the samples taken in week 2, granulation tissue, fibrosis formation, the degree of inflammation, cilia and goblet cell damage, foreign-body reaction, and cartilage damage were significantly higher in the study group. Inflammation, fibrosis, granulation tissue, and cartilage damage were observed minimally in the control group in the 4-week biopsies, and there was no statistical difference between the groups, since cilia and goblet damage and foreign-body reaction were not observed in these tissue samples. This may be due to the trauma that occurred with mucoperichondrial elevation. No hematoma was observed in any group. Septal perforation was determined in all the study group participants, and loss of cilia and goblet cells and foreign-body reaction were found in 8 samples of the study group participants and in none of the control group.
Conclusion
In conclusion when the literature is examined, it can be seen that although Bioglue has been applied successfully in many surgical fields, there are also serious risks and side effects and unsuccessful results as in the current study. It can be concluded that Bioglue may not an appropriate choice as a tissue adhesive in nasal septum surgery because it causes damage to the nasal cartilage septum and mucosa.
Footnotes
Authors’ Note
Each of the authors read and approved this manuscript. This manuscript is original and it, or any part of it, has not been previously published; nor is it under consideration for publication elsewhere. Experiments were conducted in accordance with the principles of the Helsinki Declaration on the use of laboratory animals.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
