Abstract
Cochlear implants have successfully improved hearing in severe and profoundly deaf patients in addition to improving their quality of life. Implant extrusion and wound infection of a cochlear implant are one of the most common postoperative complications, although it does not occur frequently (1.5%-5% of cases). 1,2 We present a case of an extruding cochlear implant with dehiscence that was successfully reimplanted, a procedure of which there have been few previous reports in the literature.
Introduction
Cochlear implants have become a standard treatment and are currently the only medical treatment to partially restore severe to profound hearing loss, which works by stimulating the cochlear nerve. Cochlear implantation is a generally safe procedure associated with minimal complications, one of which is extrusion of the implant. We present a case of an extruding cochlear implant with dehiscence.
Case
A 79-year-old rocket engineer experienced profound hearing loss and was implanted with a cochlear implant in 2010 and experienced no complications until he presented in 2014 with dehiscence. In the time between implantation and dehiscence, the patient experienced no immunosuppressive diseases, was on no immunosuppressive medication, and did not develop any new medical issues including diabetes. The patient was otherwise asymptomatic and had no pain or drainage from the wound or pain.
There is slot-like dehiscence of his scalp wound and the implant is extruding through the dehiscence (Figure 1). The surrounding skin is not unusually edematous or significantly erythematous. Although not obvious in the figure, the dehiscence is posterior to the healed surgical incision. The patient requested for the device to be reimplanted.
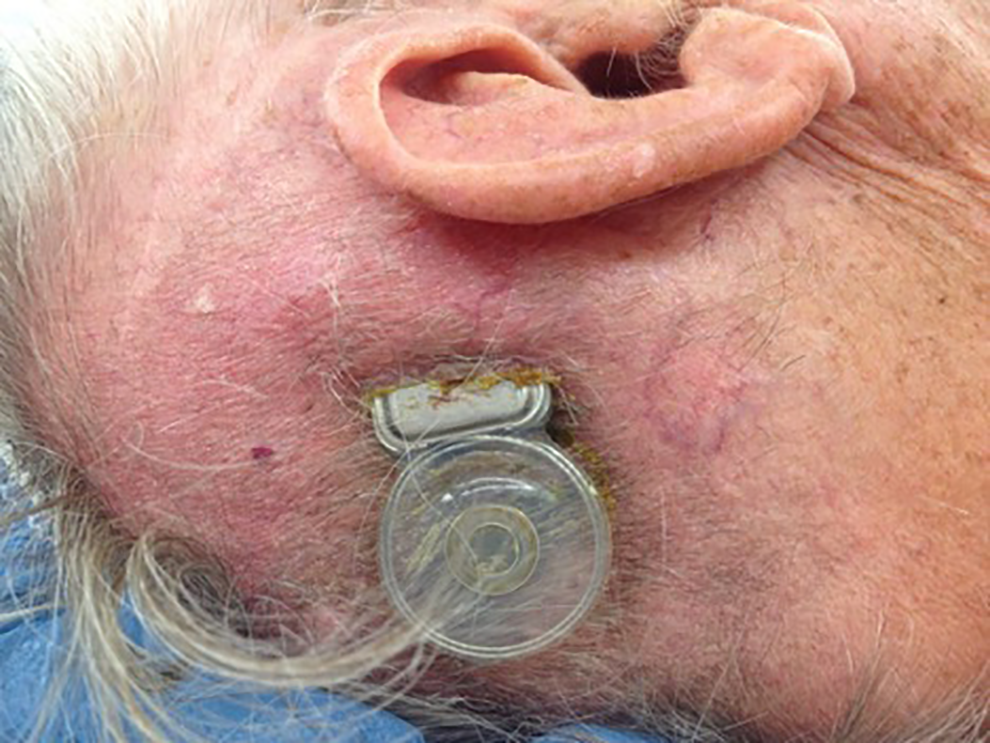
Extruding cochlear implant.
The wound over the implant was revised and debrided of infected tissue, and the implant was relocated superiorly through expansion of the soft tissue pocket. There was no granulation noted. Intraoperatively—after the implant was mobilized, it was soaked in betadine and fixated to the bone superiorly to where it is pictured. The patient was given perioperative cefozolin 1 gram pre- and postoperatively. Six years postoperatively, the patient is still benefitting from his implant with no wound complications.
Discussion
Skin complications following cochlear implant surgery make up a relatively small overall complication percentage. The global complication rate in a study of 403 adult and pediatric cochlear implant patients between 1993 and 2013 was 19.9%. This was divided into minor complications in 14.9% and major complications in 5%. Local skin complications such as ulcer, infection, or wound dehiscence were seen in 2.5% of their series, and most of these required medical care including surgical revision. 3
Consideration should be taken to see whether or not the implant is obviously infected. Much of the literature states that extruding implants should be explanted, although a literature review by Viol et al covering 1960 to 2009 of orthopedic implants found that important parameters in this case are location of hardware, obvious infection, implant removed if culture is positive in the extremities but retained if culture is positive in spine and hardware has maintained stability, duration of exposure—less than 2 weeks favorable, and hardware loosening. The article advocated for early cultures and soft tissue coverage of exposed hardware (local or free flaps). They found that many noninfected implants in the extremities and even some well-fixated, but culture-positive spine implants could be retained and overlying tissue reconstructed without sequelae. 4
Seo et al reported on 2 exposed cochlear implant patients one of whom had granulation and positive cultures of Staphylococcus aureus. Both had locally advanced skin flaps and both had retained their implant at 1-year follow-up. 5
Leach et al also advocated for the control of infection with antibiotics based on wound culture and sensitivity, local care to enforce control of infection and increased granulation, elimination of tobacco use, and eliminate sources of local trauma such as hats or glasses. 6 When appropriate, they advocated that the wound should be revised and debrided of infected tissue, the device relocated, use local tissue used for reconstruction, and HBO considered in patients with risk factors.
In the primary author’s experience, if the implant is grossly infected it is most likely going to extrude eventually. Noninfected implants in patients without risk factors have a good chance of surviving. The implant should be soaked in betadine in situ and reimplanted in a separate area. The implant should be fixated, and the use of local advancement flaps is preferred.
Footnotes
Authors’ Note
This manuscript is original and has not been submitted elsewhere in part or in whole.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
